Contents
What is a hiatal hernia
A hiatal hernia is a condition in which the upper part of the stomach pushes upward through an opening in the diaphragm 1. The diaphragm is the muscle wall that separates the stomach from the chest. The diaphragm helps keep acid from coming up into the esophagus. Your diaphragm normally has a small opening (hiatus) through which your food tube (esophagus) passes on its way to connect to your stomach. The stomach can push up through this opening and cause a hiatal hernia. When you have a hiatal hernia, it’s easier for the acid to come up.
The prevalence of sliding hiatal hernias ranges from 10% to 60%. Sliding hiatal hernias represent 95% of all hiatal hernias with paraesophageal hernias making the remaining. Hiatal hernias are common, especially in people over age 50.
In most cases, a small hiatal hernia doesn’t cause problems, and you may never know you have a hiatal hernia unless your doctor discovers it when checking for another condition.
But a large hiatal hernia can allow food and acid to back up into your esophagus, leading to heartburn. Self-care measures or medications can usually relieve these symptoms, although a very large hiatal hernia sometimes requires surgery.
If you have symptoms, eating small meals, avoiding certain foods, not smoking or drinking alcohol, and losing weight may help. Your doctor may recommend antacids or other medicines. If these don’t help, you may need surgery.
The leaking of acid from the stomach into the esophagus is called gastroesophageal reflux disease (GERD). Gastroesophageal reflux disease (GERD) may cause symptoms such as:
- Heartburn
- Problems swallowing
- A dry cough
- Bad breath.
What is a diaphragm
The diaphragm is the major muscles of respiration. And the other respiratory muscles are the intercostal muscles.
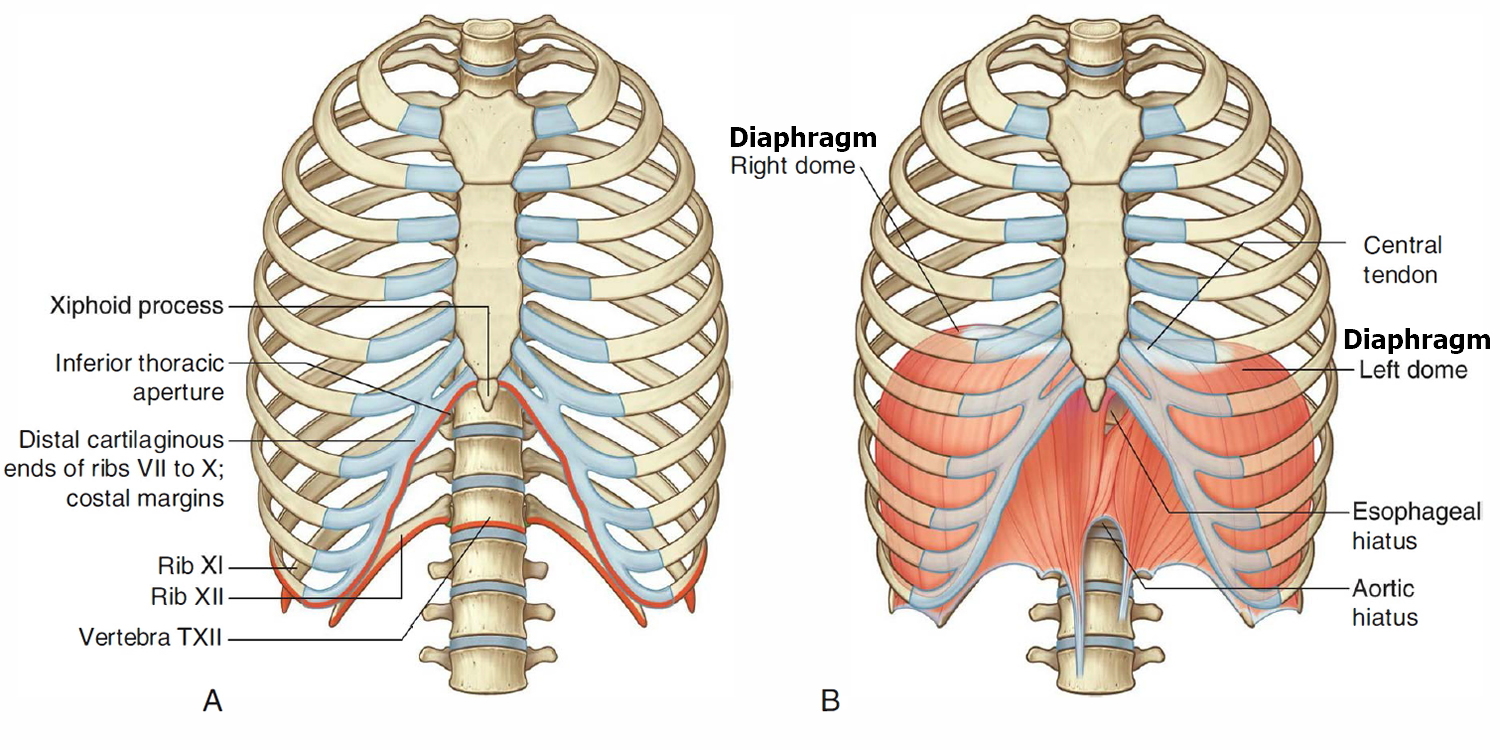
Figure 1. Diaphragm muscle
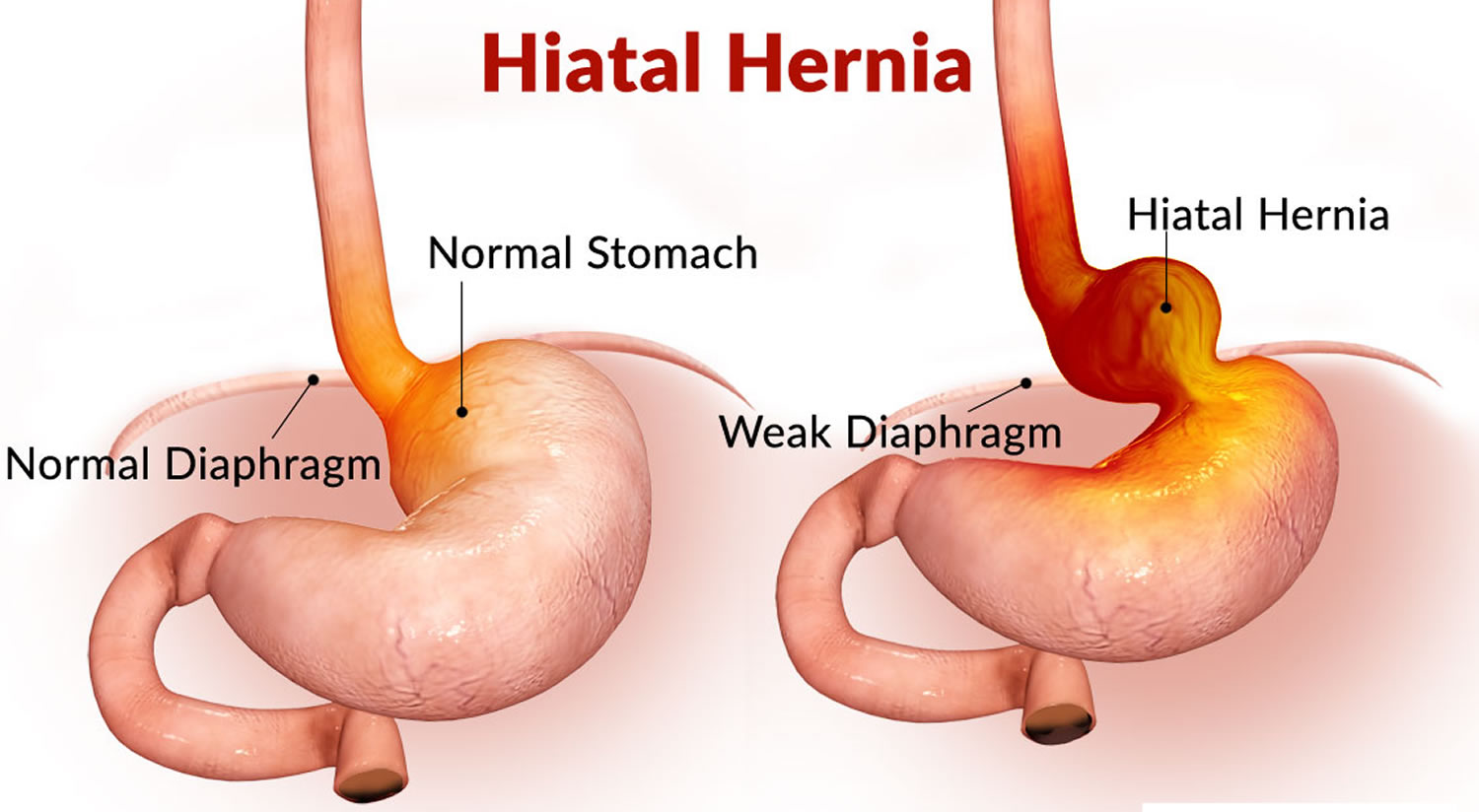
Figure 2. Hiatal hernia
Hiatal hernia types
There are four types of hiatal hernias. However, the sliding hiatal hernia (type 1) is the most common and accounts for up to 95% of all hiatal hernias 2.
- Type 1 hiatal hernias solely involve “sliding” of the gastroesophageal junction into the thoracic cavity.
Type 2 to 4 hiatal hernias are true paraesophageal hernias and are classified based upon on location of the gastroesophageal junction as well as what has herniated into the thoracic cavity.
- A type 2 hiatal hernia has a gastroesophageal junction in the normal anatomic position, but a portion of the stomach, most often the fundus, has herniated through the hiatus.
- Type 3, like type 2, have a portion of the stomach that has herniated through the hiatus, but also have an abnormal position of the gastroesophageal junction in the thoracic cavity.
- Type 4 has an abnormal GE junction position like type 1 and 3. However, another organ, most often a portion of the colon, has herniated into the thoracic cavity.
Hiatal hernia symptoms
Most patients with sliding hernias (type 1) are generally asymptomatic. However, larger hiatal hernias can cause signs and symptoms such as:
- Heartburn
- Belching
- Difficulty swallowing
- Chest or abdominal pain
- Feeling especially full after meals
- Vomiting blood or passing black stools, which may indicate gastrointestinal bleeding.
Patients with paraesophageal hernias can develop symptoms of obstruction. If the obstruction occurs at the level of the gastroesophageal junction, then dysphagia is the most common symptom. If any contents remain in the distal esophagus, then regurgitation will occur. However, if the distal stomach becomes obstructed, the resulting proximal gastric distention will lead to nausea and vomiting and in some cases chest pain that radiates to the back.
When to see a doctor
Make an appointment with your doctor if you have any persistent signs or symptoms that worry you.
Hiatal hernia causes
A hiatal hernia occurs when weakened muscle tissue allows your stomach to bulge up through your diaphragm. It’s not always clear why this happens, but pressure on your stomach and age-related changes in your diaphragm may contribute to the formation of a hiatal hernia.
How a hiatal hernia forms
Your diaphragm is a large, dome-shaped muscle that separates your chest cavity from your abdomen. Normally, your esophagus passes into your stomach through an opening in the diaphragm called the hiatus.
Hiatal hernias occur when the muscle tissue surrounding this opening becomes weak, and the upper part of your stomach bulges up through the diaphragm into your chest cavity.
Possible causes of hiatal hernia
Hiatal hernia could be caused by:
- Injury to the area
- Being born with an unusually large hiatus
- Persistent and intense pressure on the surrounding muscles, such as when coughing, vomiting or straining during a bowel movement, or while lifting heavy objects
Risk factors of hiatal hernia
Hiatal hernia is most common in people who are:
- Age 50 or older
- Obese
Hiatal hernia diagnosis
A hiatal hernia is often discovered during a test or procedure to determine the cause of heartburn or chest or upper abdominal pain. Such tests or procedures include:
- Blood testing. Your doctor may recommend a complete blood count to check for anemia due to blood loss.
- An esophagram (barium swallow). During this procedure, you drink a chalky liquid containing barium that coats your upper digestive tract. This provides a clear silhouette of your esophagus, stomach and the upper part of your small intestine (duodenum) on an X-ray.
- Endoscopy. During an endoscopy exam, your doctor passes a thin, flexible tube equipped with a light and video camera (endoscope) down your throat and into your esophagus and stomach to check for inflammation.
- Manometry. During this test, a thin, pressure-sensitive tube (catheter) is passed through your nose, down through the esophagus and into the stomach. The catheter then measures pressure and movement inside the esophagus.
Hiatal hernia treatment
Most people with a hiatal hernia don’t experience any signs or symptoms and won’t need treatment. If you experience signs and symptoms, such as recurrent heartburn and acid reflux, you may require treatment, which can include medications or surgery.
Medications for heartburn
If you experience heartburn and acid reflux, your doctor may recommend medications, such as:
- Antacids that neutralize stomach acid. Over-the-counter antacids, such as Gelusil, Maalox, Mylanta, Rolaids and Tums, may provide quick relief.
- Medications to reduce acid production. Called H-2-receptor blockers, these medications include cimetidine (Tagamet HB), famotidine (Pepcid AC), nizatidine (Axid AR) and ranitidine (Zantac 75). Stronger versions of these medications are available in prescription form.
Medications that block acid production and heal the esophagus. Proton pump inhibitors block acid production and allow time for damaged esophageal tissue to heal.
Over-the-counter proton pump inhibitors include lansoprazole (Prevacid 24HR) and omeprazole (Prilosec OTC). Stronger versions of these medications are available in prescription form.
Surgery to repair a hiatal hernia
In a small number of cases, a hiatal hernia may require surgery. Surgery is generally reserved for emergency situations, which are rare, and for people who aren’t helped by medications to relieve heartburn and acid reflux.
An operation for a hiatal hernia may involve pulling your stomach down into your abdomen and making the opening in your diaphragm smaller, reconstructing a weak esophageal sphincter, or removing the hernia sac.
In some cases, surgery is done using a single incision in your chest wall (thoracotomy) or abdomen (laparotomy). In other cases, your surgeon may insert a tiny camera and special surgical tools through several small incisions in your abdomen. The operation is then performed while your surgeon views images from inside your body that are displayed on a video monitor (laparoscopic surgery).
The laparoscopic approach for the surgical treatment of giant hiatal hernia is effective with limited morbidity and negligible mortality. However, it is technically demanding that requires advanced skills in upper gastrointestinal laparoscopic surgery and recurrence rates are high. Robotic technology with the stereoscopic vision might help the surgeon perform a more precise dissection of the sac and the esophagus, reduction of the herniated organs into the abdomen, and cruroplasty 3. To date, very few studies have specifically assessed the impact of the robotic technologies on the outcomes in patients undergoing minimally invasive repair of a giant hiatal hernia, showing no real clear benefits to the patients. No long-term follow-up are available. Gehrig et al. 4 conducted a case-control study comparing 12 patients operated with the aid of the robot and 17 patients undergoing laparoscopic hiatal hernia repair. No advantages were found in operative time, intraoperative complications and early postoperative course.
Home remedies for hiatal hernia
Making a few lifestyle changes may help control the signs and symptoms of acid reflux caused by a hiatal hernia.
- Eat several smaller meals throughout the day rather than a few large meals.
- Avoid foods that trigger heartburn, such as chocolate, onions, spicy foods, greasy foods, citrus fruits and tomato-based foods.
- Avoid alcohol.
- Eat at least two to three hours before bedtime 5, 6.
- Lose weight if you’re overweight or obese 7, 8, 9.
- Stop smoking and avoiding secondhand smoke 10, 11, 12.
- Elevate the head of your bed 6 inches (about 15 centimeters) 13, 14, 15.
- Hiatal Hernia. Medline Plus. https://medlineplus.gov/hiatalhernia.html[↩]
- Watson TJ, Moritz T. Hernia, Sliding (Paraesophageal) [Updated 2017 Oct 10]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2017 Jun-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK459270/[↩]
- Mid-term results of robot-assisted laparoscopic repair of large hiatal hernia: a symptomatic and radiological prospective cohort study. Draaisma WA, Gooszen HG, Consten EC, Broeders IA. Surg Technol Int. 2008; 17():165-70. https://www.ncbi.nlm.nih.gov/pubmed/18802897[↩]
- Robotic-assisted paraesophageal hernia repair–a case-control study. Gehrig T, Mehrabi A, Fischer L, Kenngott H, Hinz U, Gutt CN, Müller-Stich BP. Langenbecks Arch Surg. 2013 Jun; 398(5):691-6. https://www.ncbi.nlm.nih.gov/pubmed/22846911/[↩]
- Duroux P, Bauerfeind P, Emde C et al. Early dinner reduces nocturnal gastric acidity. Gut 1989;30:1063–1067.[↩]
- Orr WC, Harnish MJ. Sleep-related gastro-oesophageal reflux: provocation with a late evening meal and treatment with acid suppression. Aliment Pharmacol Ther 1998;12:1033–1038.[↩]
- Jacobson BC, Somers SC, Fuchs CS et al. Body-mass index and symptoms of gastroesophageal reflux in women. N Engl J Med 2006;354:2340–2348.[↩]
- Fraser-Moodie CA, Norton B, Gornall C et al. Weight loss has an independent beneficial effect on symptoms of gastro-oesophageal reflux in patients who are overweight. Scand J Gastroenterol 1999;34:337–340.[↩]
- Mathus-Vliegen LM, Tytgat GN. Twenty-four-hour pH measurements in morbid obesity: effects of massive overweight, weight loss and gastric distension. Eur J Gastroenterol Hepatol 1996;8:635–640.[↩]
- Schindlbeck NE, Heinrich C, Dendorfer A et al. Influence of smoking and esophageal intubation on esophageal pH-metry. Gastroenterology 1987;92:1994–1997.[↩]
- Waring JP, Eastwood TF, Austin JM et al. The immediate effects of cessation of cigarette smoking on gastroesophageal reflux. Am J Gastroenterol 1989;84:1076–1078.[↩]
- Kadakia SC, Kikendall JW, Maydonovitch C et al. Effect of cigarette smoking on gastroesophageal reflux measured by 24-h ambulatory esophageal pH monitoring. Am J Gastroenterol 1995;90:1785–1790.[↩]
- Stanciu C, Bennett JR. Effects of posture on gastro-oesophageal reflux. Digestion 1977;15:104–109.[↩]
- Hamilton JW, Boisen RJ, Yamamoto DT et al. Sleeping on a wedge diminishes exposure of the esophagus to refluxed acid. Dig Dis Sci 1988;33:518–522.[↩]
- Pollmann H, Zillessen E, Pohl J et al. Effect of elevated head position in bed in therapy of gastroesophageal reflux. Z Gastroenterol 1996;34(Suppl 2): 93–99.[↩]