Contents
What is impetigo
Impetigo is a contagious skin infection caused by bacteria 1. Impetigo is characterised by pustules and honey-coloured crusted erosions (“school sores”). More than 90 percent of impetigo cases are caused by Staphylococcus aureus or “staph,” bacteria, while the rest are caused by Streptococcus pyogenes (group A beta-haemolytic streptococcus) bacteria (which also are responsible for “strep” throat and scarlet fever) 2. If staph bacteria are to blame, the infection may cause blisters filled with clear fluid. These can break easily, leaving a raw, glistening area that soon forms a scab with a honey colored crust. By contrast, infections with strep bacteria usually are not associated with blisters, but they do cause crusts over larger sores and ulcers. Methicillin-resistant Staphylococcus aureus (MRSA) bacteria is also becoming an important cause of impetigo.
It is most common in children between the ages of two and six. It usually starts when bacteria get into a break in the skin, such as a cut, scratch, or insect bite.
Symptoms start with red or pimple-like sores surrounded by red skin. These sores can be anywhere, but usually they occur on your face (around the nose, mouth, and ears), arms and legs. The sores fill with pus, then break open after a few days and form a thick crust. They are often itchy, but scratching them can spread the sores to other parts of their body. Impetigo can spread to anyone who touches infected skin or items that have been touched by infected skin (such as clothing, towels, and bed linens).
There are more than 3 million cases of impetigo in the United States every year. Doctors typically see impetigo with kids 2 to 6 years old, probably because they get more cuts and scrapes and scratch more.
Impetigo is contagious and it can spread by contact with sores or nasal discharge from an infected person. You can treat impetigo with antibiotics.
Types of impetigo
The three types of impetigo are non-bullous (crusted), bullous (large blisters) and ecthyma (ulcers):
- Non-bullous or crusted impetigo is most common. It begins as tiny blisters that eventually burst and leave small wet patches of red skin that may weep fluid. Gradually, a yellowish-brown or tan crust covers the area, making it look like it has been coated with honey or brown sugar.
- Bullous impetigo causes larger fluid-containing blisters that look clear, then cloudy. These blisters are more likely to stay longer on the skin without bursting.
- Ecthyma or ulcerated impetigo is usually due to Streptococcus pyogenes, but co-infection with Staphylococcus aureus may occur.
Who gets impetigo ?
Impetigo is most common in children (especially boys), but may also affect adults if they have low immunity to the bacteria. It is prevalent worldwide. Peak onset is during summer and it is more prevalent in developing countries.
The following factors predispose to impetigo.
- Atopic dermatitis or eczema
- Scabies
- Skin trauma: chickenpox, insect bite, abrasion, laceration, thermal burn, dermatitis, surgical wound.
How long is impetigo contagious
Impetigo is contagious until the rash clears, or until at least two days of antibiotics have been given and there is evidence of improvement 2. Your child should avoid close contact with other children during this period, and you should avoid touching the rash. If you or other family members do come in contact with it, wash your hands and the exposed site thoroughly with soap and water. Also, keep the infected child’s washcloths and towels separate from those of other family members.
Prevention of impetigo
The bacteria that cause impetigo thrive in breaks in the skin. The best ways to prevent this rash are to keep your child’s fingernails clipped and clean and to teach him not to scratch minor skin irritations. When he does have a scrape, cleanse it with soap and water, and apply an antibiotic cream or ointment. Be careful not to use washcloths or towels that have been used by someone else who has an active skin infection.
When certain types of strep bacteria cause impetigo, a rare but serious complication called glomerulonephritis can develop. This disease injures the kidney and may cause high blood pressure and blood to pass in the urine. Therefore, if you notice any blood or dark brown color in your child’s urine, let your pediatrician know so he can evaluate it and order further tests if needed.
Prevent the spread of impetigo.
- If you have impetigo, always use a clean washcloth and towel each time you wash.
- DO NOT share towels, clothing, razors, and other personal care products with anyone.
- Avoid touching blisters that are oozing.
- Wash your hands thoroughly after touching infected skin.
Keep your skin clean to prevent getting the infection. Wash minor cuts and scrapes well with soap and clean water. You can use a mild antibacterial soap.
Causes of impetigo
Impetigo is caused by streptococcus (strep) or staphylococcus (staph) bacteria. Methicillin-resistant staph aureus (MRSA) is becoming a common cause.
Skin normally has many types of bacteria on it. When there is a break in the skin, bacteria can enter the body and grow there. This causes inflammation and infection. Breaks in the skin may occur from injury or trauma to the skin or from insect, animal, or human bites.
Impetigo may also occur on skin where there is no visible break.
Impetigo is most common in children who live in unhealthy conditions.
In adults, it may occur following another skin problem. It may also develop after a cold or other virus.
Impetigo can spread to others. You can catch the infection from someone who has it if the fluid that oozes from their skin blisters touches an open area on your skin.
Because impetigo spreads by skin-to-skin contact, there often are small outbreaks within a family or a classroom. Avoid touching objects that someone with impetigo has used, such as utensils, towels, sheets, clothing and toys. If you have impetigo, keep your fingernails short so the bacteria can’t live under your nails and spread. Also, don’t scratch the sores.
See your health care provider if the symptoms don’t go away or if there are signs the infection has worsened, such as fever, pain, or increased swelling.
Risk factors for impetigo
Factors that increase the risk of impetigo include:
- Age. Impetigo most commonly occurs in children ages 2 to 5.
- Crowded conditions. Impetigo spreads easily in schools and child care settings.
- Warm, humid weather. Impetigo infections are more common in summer.
- Certain sports. Participation in sports that involve skin-to-skin contact, such as football or wrestling, increases your risk of developing impetigo.
- Broken skin. The bacteria that cause impetigo often enter your skin through a small skin injury, insect bite or rash.
Adults and people with diabetes or a weakened immune system are more likely to develop ecthyma.
Symptoms of impetigo
Symptoms of impetigo are:
- One or many blisters that are filled with pus and easy to pop. In infants, the skin is reddish or raw-looking where a blister has broken.
- Blisters that itch, are filled with yellow or honey-colored fluid, and ooze and crust over. Rash that may begin as a single spot, but spreads to other areas with scratching.
- Skin sores on the face, lips, arms, or legs that spread to other areas.
- Swollen lymph nodes near the infection.
- Patches of impetigo on the body (in children).
What are the clinical features of impetigo
Primary impetigo mainly affects exposed areas such as the face and hands, but may also affect trunk, perineum and other body sites. It presents with single or multiple, irregular crops of irritable superficial plaques. These extend as they heal, forming annular or arcuate lesions.
Although many children are otherwise well, lymphadenopathy, mild fever and malaise may occur.
Nonbullous impetigo
Nonbullous impetigo starts as a pink macule that evolves into a vesicle or pustule and then into crusted erosions. Untreated impetigo usually resolves within 2 to 4 weeks without scarring.
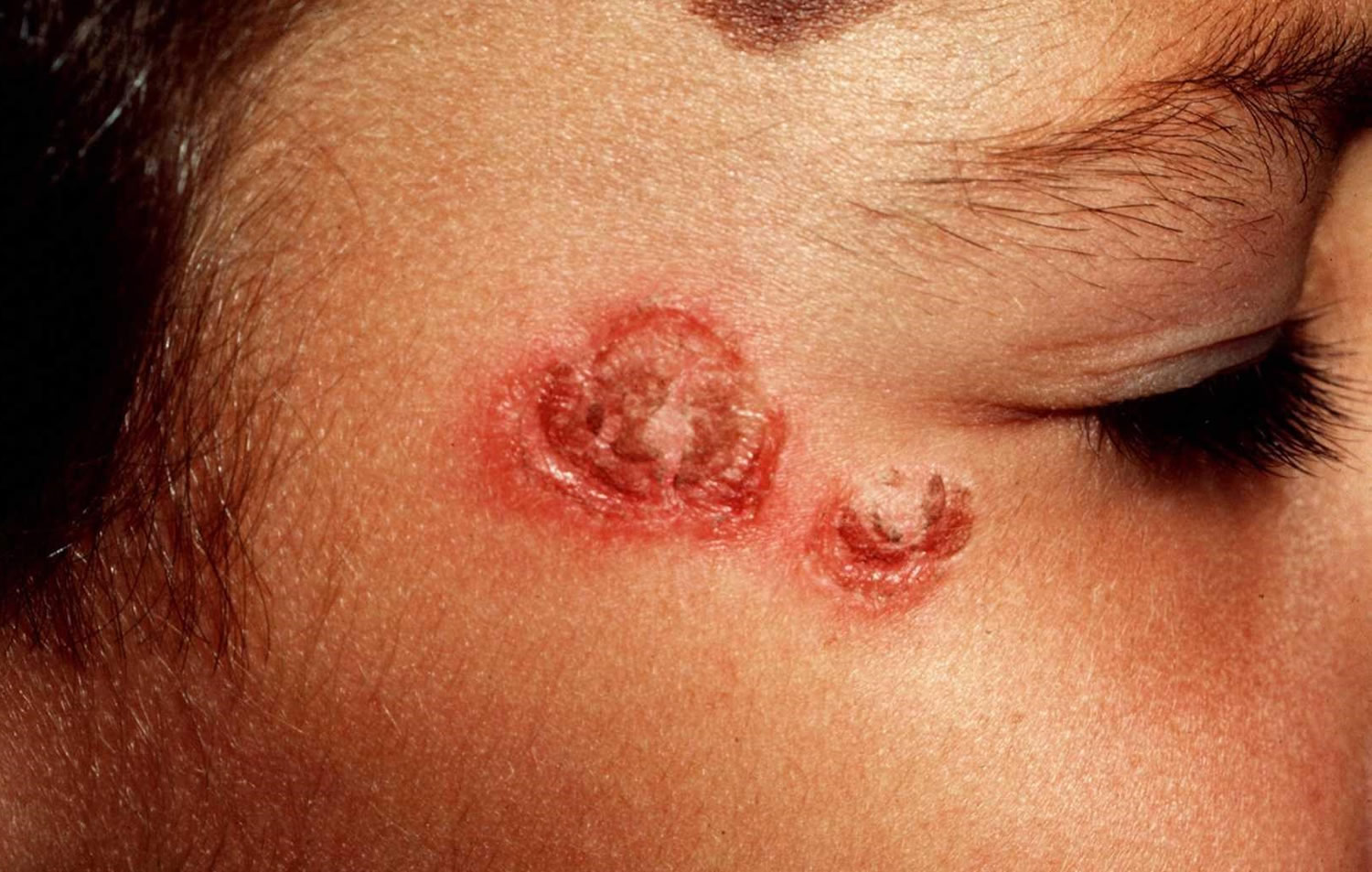
Ecthyma
Ecthyma starts as nonbullous impetigo but develops into a punched-out necrotic ulcer. This heals slowly, leaving a scar.
Bullous impetigo
Bullous impetigo presents with small vesicles that evolve into flaccid transparent bullae. It heals without scarring.
Exams and Tests
Your health care provider will look at your skin to determine if you have impetigo.
Your provider may take a sample of bacteria from your skin to grow in the lab. This can help determine if MRSA is the cause. Specific antibiotics are needed to treat this type of bacteria.
Figure 1. Impetigo on nose
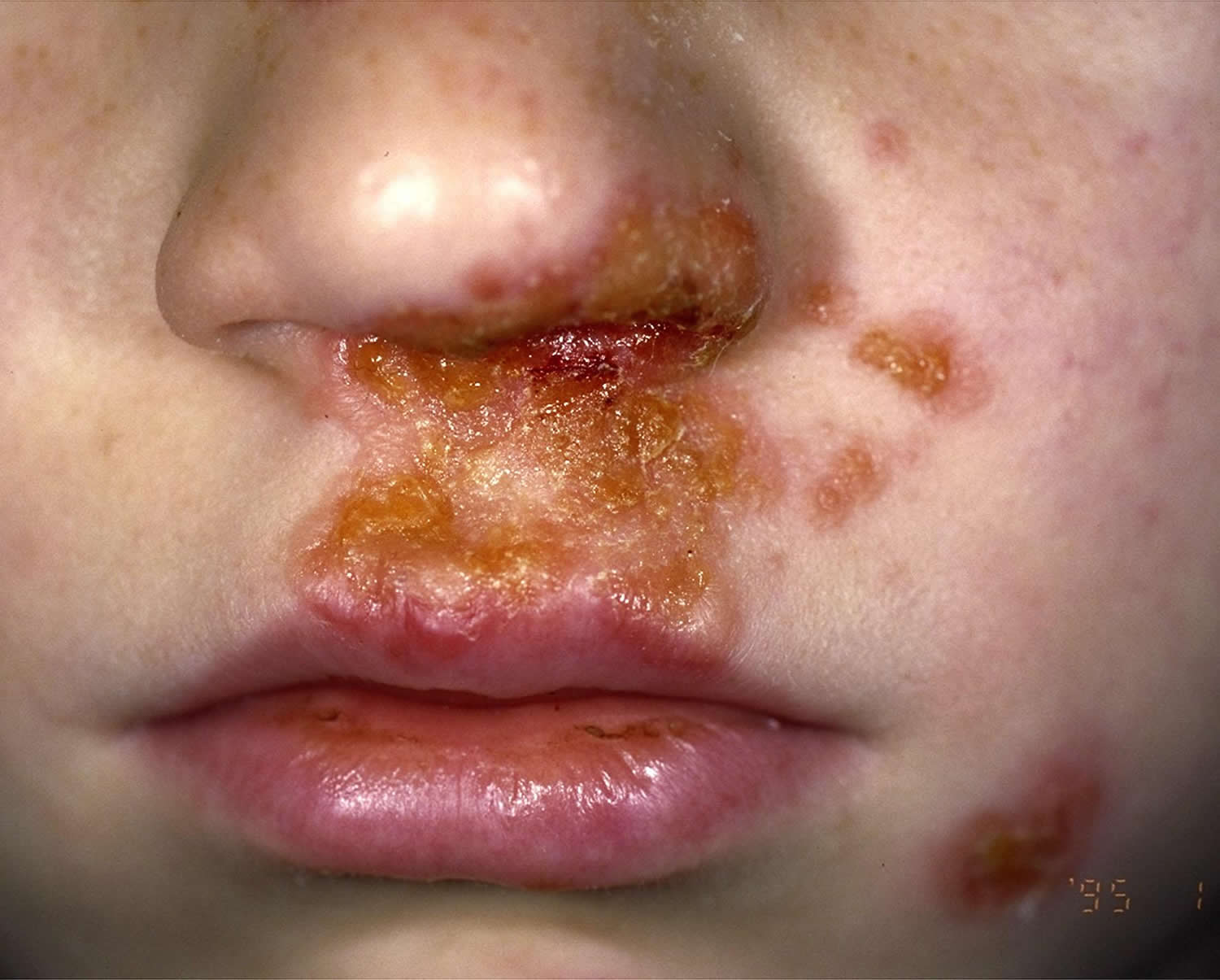
Figure 2. Impetigo on face
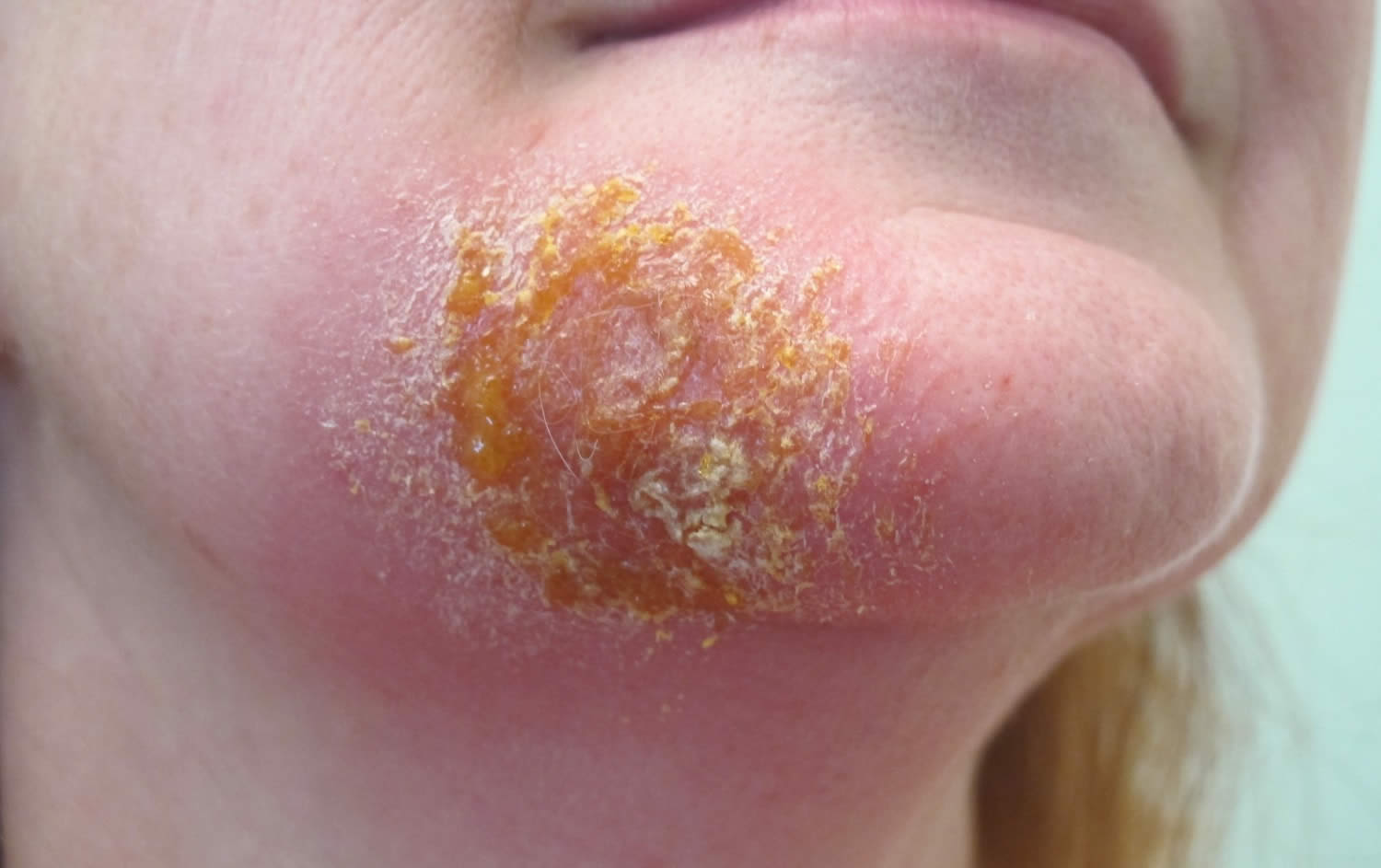
Figure 3. Impetigo on legs
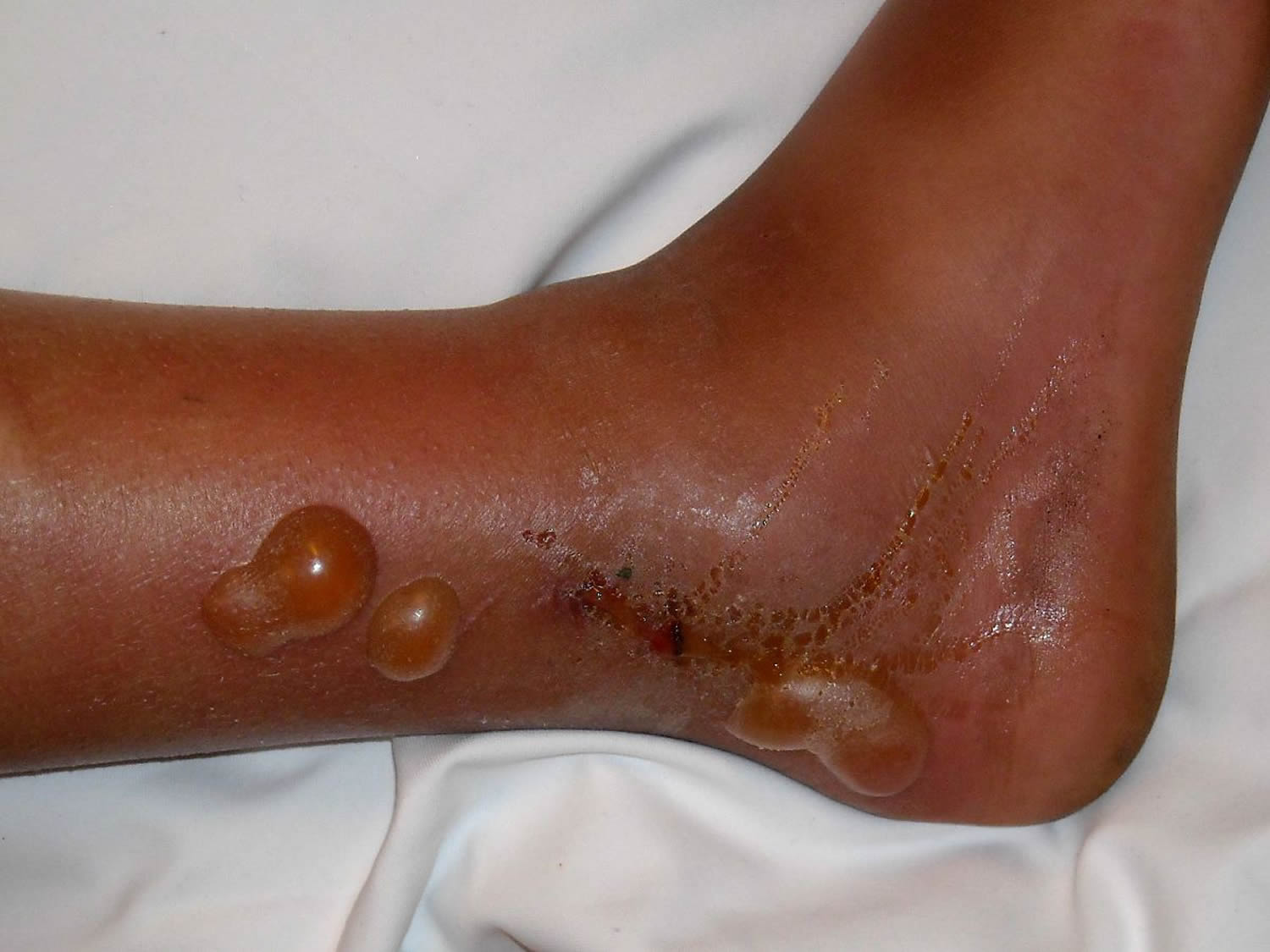
Figure 4. Impetigo on scalp
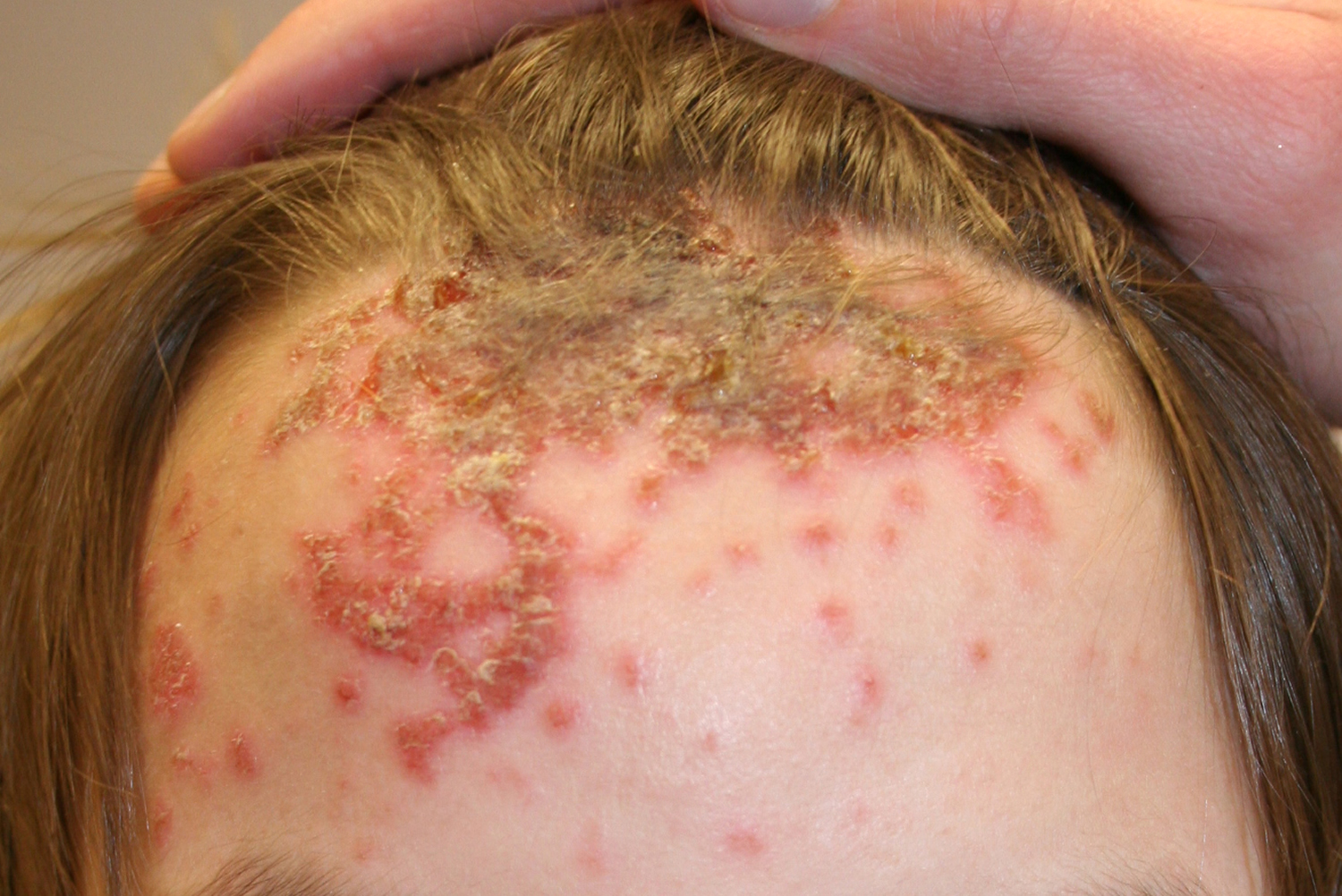
Figure 5. Impetigo in children
Figure 6. Impetigo rash
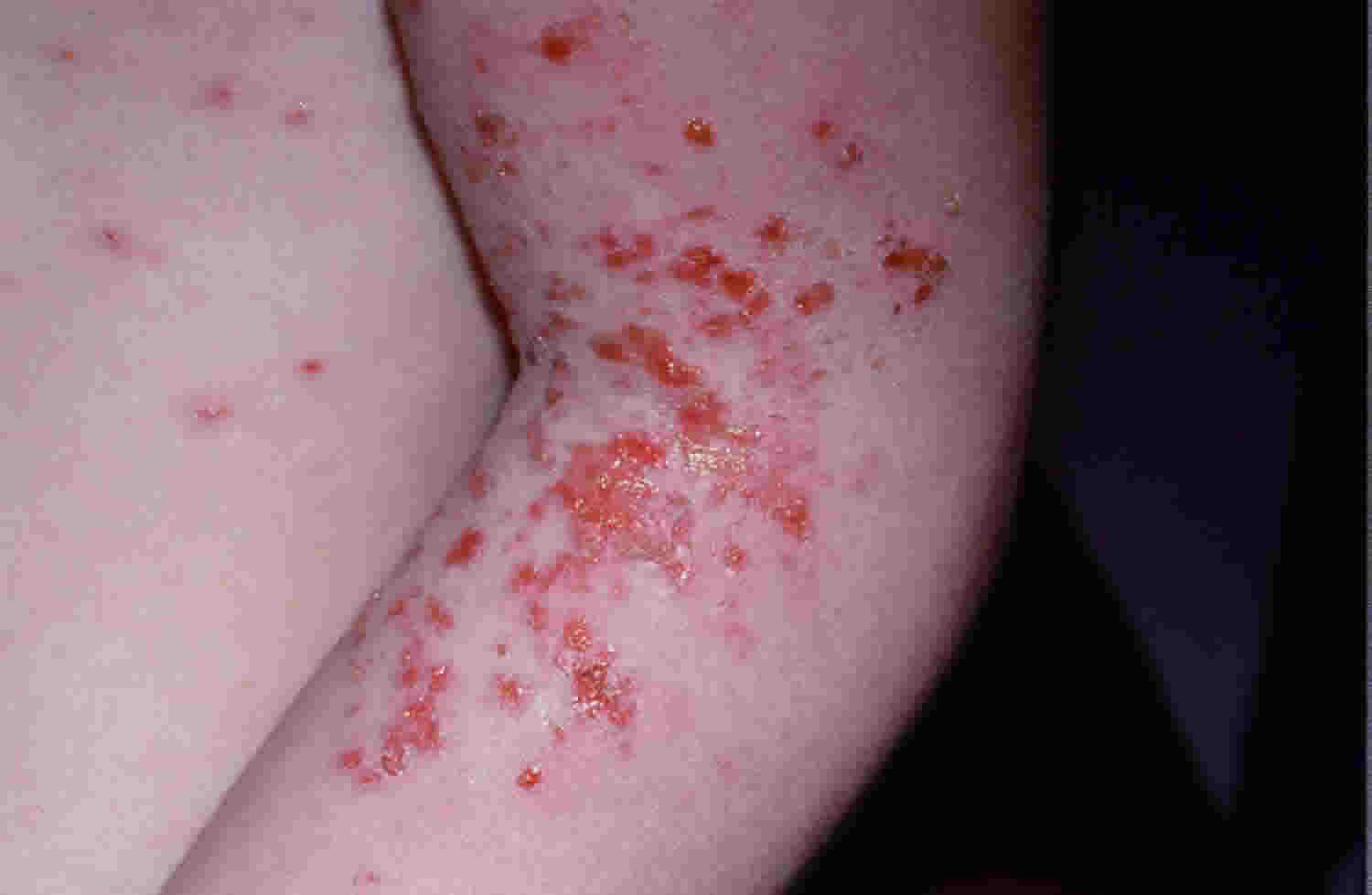
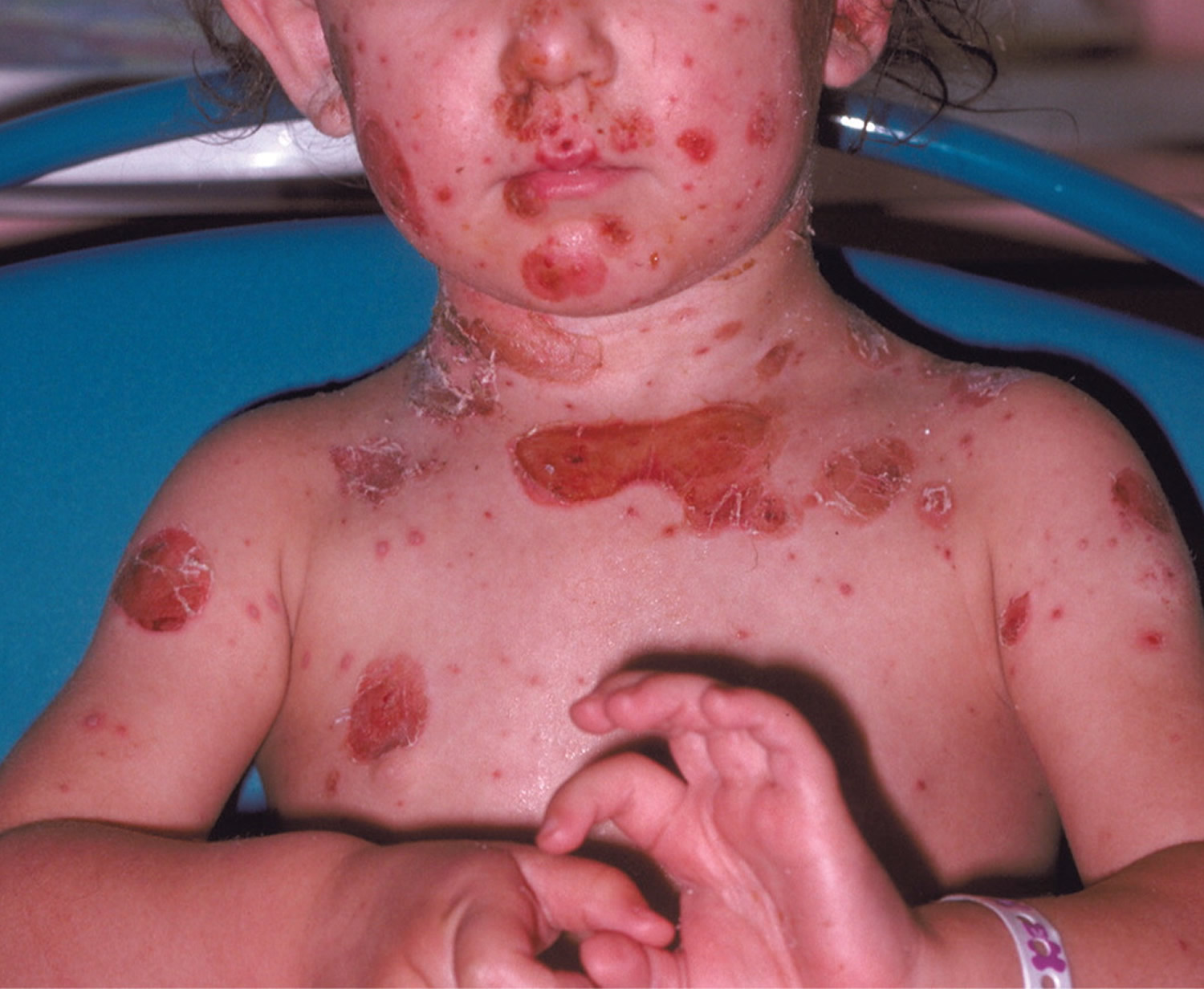
Figure 7. Bullous impetigo
How is impetigo diagnosed ?
Impetigo is usually diagnosed clinically but can be confirmed by bacterial swabs sent for microscopy (gram positive cocci are observed), culture and sensitivity.
Blood count may reveal neutrophil leucocytosis when impetigo is widespread.
Skin biopsy is rarely necessary. Histological features are characteristic.
Non-bullous impetigo
- Gram-positive cocci
- Intraepidermal neutrophilic pustules,
- Dense inflammatory infiltrate in upper dermis
Bullous impetigo
- Split through granular layer of epidermis without inflammation or bacteria
- Acantholytic cells
- Minimal inflammatory infiltrate in upper dermis
- Resembles pemphigus foliaceus
Ecthyma
- Full thickness skin ulceration
- Gram stain shows cocci within dermis
Impetigo treatment
Impetigo needs to be treated with antibiotics, either topically or by mouth, and your doctor may order a culture in the lab to determine which bacteria are causing the rash. Make sure your child takes the medication for the full prescribed course or the impetigo could return.
- When it just affects a small area of the skin (and especially if it’s the non-bullous form), impetigo is treated with antibiotic ointment.
- If the infection has spread to other areas of the body or the ointment isn’t working, the doctor may prescribe an antibiotic pill or liquid to be taken for 7–10 days.
There is no over-the-counter (OTC) treatment for impetigo 3.
Quality evidence-based research for the most effective treatment of impetigo is lacking 4. In 2012, an updated Cochrane review on impetigo interventions evaluated 68 randomized controlled trials, including 26 on oral treatments and 24 on topical treatments. There was no clear evidence as to which intervention is most effective 5. Topical antibiotics are more effective than placebo and preferable to oral antibiotics for limited impetigo 4. Systemic antibiotics are often reserved for more generalized or severe infections in which topical therapy is not practical. Clinicians sometimes may choose both topical and systemic therapy 5. The ideal treatment should be effective, be inexpensive, have limited adverse effects, and should not promote bacterial resistance 6.
Table 1. Topical Antibiotics for Impetigo
| Medication | Instructions | Cost* |
|---|---|---|
Fusidic acid 2% ointment† |
|
|
Mupirocin 2% cream (Bactroban)‡ |
|
|
Mupirocin 2% ointment‡ |
|
|
Retapamulin 1% ointment (Altabax)§ |
|
|
NA = not available.
*—Estimated retail price based on information obtained at http://www.goodrx.com. Generic price listed first; brand listed in parentheses.
†—Coverage for Staphylococcus aureus (methicillin-susceptible) and streptococcus.
‡—Coverage for S. aureus (methicillin-susceptible) and streptococcus. Mupirocin–resistant streptococcus has now been documented.
§—First member of the pleuromutilin class of antibiotics. Coverage for S. aureus (methicillin-susceptible) and streptococcus.
Table 2. Systemic Antibiotics for Impetigo
| Drug | Adult seven-day dose | Cost (for a typical course of treatment)* | Children seven-day dose | Cost* |
|---|---|---|---|---|
Amoxicillin/clavulanate (Augmentin)† | 875/125 mg every 12 hours | $19 ($193) |
| 1 bottle, 400/57 mg per 5 mL (100-mL oral suspension): $30 ($125) |
Cephalexin (Keflex) | 250 mg every six hours or 500 mg every 12 hours | $5 ($90) |
| 1 bottle, 250 mg per 5 mL (100-mL oral suspension): $14 (NA) |
Clindamycin‡ | 300 to 600 mg every six to eight hours | $18 ($200) |
| 1 bottle, 75 mg per 5 mL (100-mL oral solution): $47 (pricing varies by region) |
Dicloxacillin | 250 mg every six hours | $14 (NA) |
| See adult pricing: no liquid formulation available |
Doxycycline§ | 50 to 100 mg every 12 hours | $15 ($95) |
| 1 bottle, 25 mg per 5 mL (60-mL oral suspension): $20 (pricing varies by region) |
Minocycline (Minocin)§ | 100 mg every 12 hours | $36 ($185) |
| See adult pricing: no liquid formulation available |
Trimethoprim/sulfamethoxazole§ | 160/800 mg every 12 hours | $4 (NA) |
| 1 bottle, 40/200 mg per 5 mL (100-mL oral suspension): $4 (pricing varies by region) |
note: Because of emerging resistance, penicillin and erythromycin are no longer recommended treatments.
NA = not available.
*—Estimated retail price based on information obtained at http://www.goodrx.com. Generic price listed first; brand listed in parentheses.
†—Good coverage for Staphylococcus aureus (methicillin-susceptible) and streptococcus.
‡—If methicillin-resistant S. aureus is suspected or proven.
§—If methicillin-resistant S. aureus is suspected or proven. There is no activity against streptococcus.
Untreated, impetigo often clears up on its own after a few days or weeks 8. The key is to keep the infected area clean with soap and water and not to scratch it. The downside of not treating impetigo is that some people might develop more lesions that spread to other areas of their body.
And you can infect others. To spread impetigo, you need fairly close contact — not casual contact — with the infected person or the objects they touched. Avoid spreading impetigo to other people or other parts of your body by:
- Cleaning the infected areas with soap and water (DO NOT scrub).
- Loosely covering scabs and sores until they heal.
- Gently removing crusty scabs.
- Washing your hands with soap and water after touching infected areas or infected persons.
- To prevent impetigo from spreading among family members, make sure everyone uses their own clothing, sheets, razors, soaps, and towels. Separate the bed linens, towels, and clothing of anyone with impetigo, and wash them in hot water. Keep the surfaces of your kitchen and household clean.
Complications from impetigo
Impetigo may lead to:
- Spread of the infection to other parts of the body (common)
- Kidney inflammation or failure (rare)
- Cellulitis. This potentially serious infection affects the tissues underlying your skin and eventually may spread to your lymph nodes and bloodstream. Untreated cellulitis can quickly become life-threatening.
- Permanent skin damage and scarring (very rare)
Soft tissue infection
The bacteria causing impetigo can become invasive, leading to cellulitis and lymphangiitis; subsequent bacteraemia might result in osteomyelitis, septic arthritis or pneumonia.
Staphylococcal scalded skin syndrome
In infants under 6 years of age or adults with renal insufficiency, localised bullous impetigo due to certain staphylococcal serotypes can lead to a sick child with generalised staphylococcal scalded skin syndrome (SSSS). Superficial crusting then tender cutaneous denudation on face, in flexures, and elsewhere is due to circulating exfoliatin/epidermolysin, rather than direct skin infection. It does not scar.
Toxic shock syndrome
Toxic shock syndrome is rare and rarely preceded by impetigo. It causes fever, diffuse erythematous then desquamating rash, hypotension and involvement of other organs.
Post-streptococcal glomerulonephritis
Group A streptococcal infection may rarely lead to acute post-streptococcal glomerulonephritis 3–6 weeks after the skin infection. It is associated with anti-DNase B and antistreptolysin O (ASO) antibodies.
Rheumatic fever
Group A streptococcal skin infections have rarely been linked to cases of rheumatic fever and rheumatic heart disease. It is thought that this occurs because strains of group A streptococci usually found on the skin have moved to the throat (the more usual site for rheumatic fever-associated infection).
Home remedies for impetigo
TOPICAL DISINFECTANTS
There are some studies on the benefits of nonantibiotic treatments, such as disinfectant soaps, but they lack statistical power 4. Disinfectants appear to be less effective than topical antibiotics and are not recommended 5. Studies comparing hexachlorophene (not available in the United States) with bacitracin and hydrogen peroxide with topical fusidic acid found the topical antibiotic to be more effective 9.
NATURAL THERAPIES
The evidence is insufficient to recommend or dismiss popular herbal treatments for impetigo 10. Natural remedies such as tea tree oil; tea effusions; olive, garlic, and coconut oils; and Manuka honey have been anecdotally successful. The fact that impetigo is self-limited means that many “cures” could appear to be helpful without being superior to placebo. In one study, tea leaf ointment and oral cephalexin (Keflex) were similarly effective, with a cure rate of 81% vs. 79% 11. Tea tree oil (derived from Melaleuca alternifolia) appeared to be equivalent to mupirocin 2% for topical decolonization of MRSA 12.
- Impetigo. Medline Plus. https://medlineplus.gov/impetigo.html[↩]
- Impetigo Care. American Academy of Pediatrics. https://www.healthychildren.org/English/health-issues/conditions/skin/pages/Impetigo-Care.aspx[↩][↩]
- How to Treat Impetigo and Control This Common Skin Infection. U.S. Food and Drug Administration. https://www.fda.gov/forconsumers/consumerupdates/ucm048837.htm[↩]
- George A, Rubin G. A systematic review and meta-analysis of treatments for impetigo. Br J Gen Pract. 2003;53(491):480–487.[↩][↩][↩]
- Koning S, van der Sande R, Verhagen AP, et al. Interventions for impetigo. Cochrane Database Syst Rev. 2012;(1):CD003261.[↩][↩][↩]
- Feaster T, Singer JI. Topical therapies for impetigo. Pediatr Emerg Care. 2010;26(3):222–227, quiz 228–231.[↩]
- Impetigo: Diagnosis and Treatment. Am Fam Physician. 2014 Aug 15;90(4):229-235. http://www.aafp.org/afp/2014/0815/p229.html[↩][↩]
- How to Treat Impetigo and Control This Common Skin Infection. U.S. Food and Drug Administration. https://www.fda.gov/ForConsumers/ConsumerUpdates/ucm048837.htm[↩]
- Christensen OB, Anehus S. Hydrogen peroxide cream: an alternative to topical antibiotics in the treatment of impetigo contagiosa. Acta Derm Venereol. 1994;74(6):460–462.[↩]
- Martin KW, Ernst E. Herbal medicines for treatment of bacterial infections: a review of controlled clinical trials. J Antimicrob Chemother. 2003;51(2):241–246.[↩]
- Sharquie KE, al-Turfi IA, al-Salloum SM. The antibacterial activity of tea in vitro and in vivo (in patients with impetigo contagiosa). J Dermatol. 2000;27(11):706–710.[↩]
- Caelli M, Porteous J, Carson CF, Heller R, Riley TV. Tea tree oil as an alternative topical decolonization agent for methicillin-resistant Staphylococcus aureus. J Hosp Infect. 2000;46(3):236–237.[↩]