Contents
What are causes of itchy anus
An itchy anus, also called pruritus ani, is a common complaint affecting both men and women. The itch, in or around the anus, can be extremely intense and persistent, causing a constant urge to scratch. Itchy anus most commonly affects adults, affecting from 1% to 5% of people in the general population. Men are more commonly affected than women with a 4:1 ratio. The condition is most common in people age 40s to 60s. There are many causes of itchy anus and an accurate diagnosis is important in order to treat the specific cause. Medical management of itchy anus often provides patients with relief of their symptoms and improves their quality of life.
There are many different possible causes for having an itchy anus, such as:
- Leakage of poo (feces) from the rectum as a result of diarrhea, fecal incontinence, constipation, diet, food intolerance or tears in the rectum
- Infections such as herpes, bacteria (streptococcal and staphylococcal infections, erythrasma), tinea, Candida
- Sexually transmitted infections (+ if you have anal sex)
- Genital warts,
- Genital herpes,
- Syphilis,
- Gonorrhea,
- Chlamydia,
- Molluscum contagiosum,
- Scabies,
- Pubic lice
- Intestinal parasites such as threadworms (pinworms)
- Hemorrhoids (piles), anal warts, and in extremely rare cases, cancer of the anus
- Anal fissures (painful clefts or grooves)
- Anal abscesses
- Anal fistulae (abnormal passageways between the bowel and an organ or skin surface)
- Crohn’s disease
- Celiac disease
- Excessive sweating
- Skin conditions
- Psoriasis
- Contact dermatitis, which occurs when your skin is irritated by soaps, creams or perfumed or bleached toilet paper.
- Hidradenitis suppurativa
- Seborrhoeic dermatitis, atopic dermatitis
- Psoriasis
- Lichen simplex chronicus, lichen sclerosus et atrophicus, lichen planus
- Connective tissue disease
- Drug eruptions
- Trauma (e.g. waxing burns, shaving injuries and injuries secondary to anal insertion of foreign bodies)
- Medical diseases that affect the entire body may also cause itchy anus. The examples include:
- Diabetes mellitus,
- Leukemia
- Lymphoma,
- Kidney failure,
- Liver diseases (obstructive jaundice),
- Iron deficiency anemia
- Hyperthyroidism
- Hypovitaminosis (deficiencies of vitamin A, B and D have been associated with itchy anus)
- Dietary factors:
- More common: coffee (caffeinated and decaffeinated), tea, cola, alcohol, chocolate, tomato, including tomato sauce
(histamine) - Less common: milk, peanuts, citrus fruits, grapes, spicy foods, prunes, figs
- More common: coffee (caffeinated and decaffeinated), tea, cola, alcohol, chocolate, tomato, including tomato sauce
- Benign tumors
- Seborrhoeic keratoses
- Angiokeratomas
- Anal intraepithelial neoplasia (rarely causes pruritus, generally asymptomatic)
- Bowenoid papulosis (may contribute to fecal soiling)
- Malignant tumors
- Squamous cell carcinoma
- Extramammary Paget disease
- Melanoma
- Chemotherapy
- Psychological
- Anxiety
- Sexual abuse
- Fear of STI or cancer
- Delusional parasitosis
- Idiopathic
- Up to 25% of cases
Studies have shown that the relief of itchy anus symptoms can occur promptly after the feces (stool) has been cleansed from the perianal area, indicating that feces (stool) is likely an irritant causing of itching. In addition to difficult or inadequate hygiene, overzealous or aggressive overcleaning with the use of many irritating soaps, scents, and lotions may cause itchy anus, resulting in this condition occasionally being referred to as “polished anus syndrome.” Overzealous cleaning, in addition to the use of topical steroids, can destroy natural skin barriers and cause trauma to the anal skin, making the problem worse. In a way, trying to keep it “too clean” may worsen the problem. Try to avoid using soap, shampoo or bubble baths in this area as they remove the natural protective oils. Long hot baths or showers can also be problematic.
Dietary factors may also play a role with itchy anus, although there are not definitive studies implicating particular food items or diets. Coffee, either caffeinated or decaffeinated, is thought to be a major contributing factor. Coffee consumption may lower the anal resting pressure (normal strength of muscle contraction at rest) and contribute to anal leakage of stool. Other dietary agents which are possible causes of itchy anus include tea, cola, energy drinks, chocolate, citrus fruits, tomatoes, spicy foods, beer, dairy products and nuts.
Infectious processes may also result in pruritis ani. Examples include bacterial skin infections, fungal infection (although a common fungus, Candida albicans, appears to be a normal inhabitant of the perianal skin), parasitic infections with pinworms or scabies, and viral infections with anal warts.
Numerous skin conditions also cause secondary itchy anus. Conditions that are potential causes of pruritus ani include psoriasis, seborrheic dermatitis, atopic dermatitis, contact dermatitis, lichen planus, lichen simplex, and lichen sclerosis. Local cancers such as Bowen’s disease or extra mammary Paget’s disease are also potential causes of itchy anus.
Medical diseases that affect the entire body may also cause itchy anus. The examples include diabetes mellitus, leukemia and lymphoma, kidney failure, liver diseases (obstructive jaundice), iron deficiency anemia, or hyperthyroidism.
It’s unusual for an itchy anus on its own to be related to something more serious. But in rare cases, it may be a sign of something like anal or bowel cancer, so it’s important to get it checked by your doctor.
While itchy anus has a wide variety of potential causes, it is important to understand that in many cases the itching has no identifiable source.
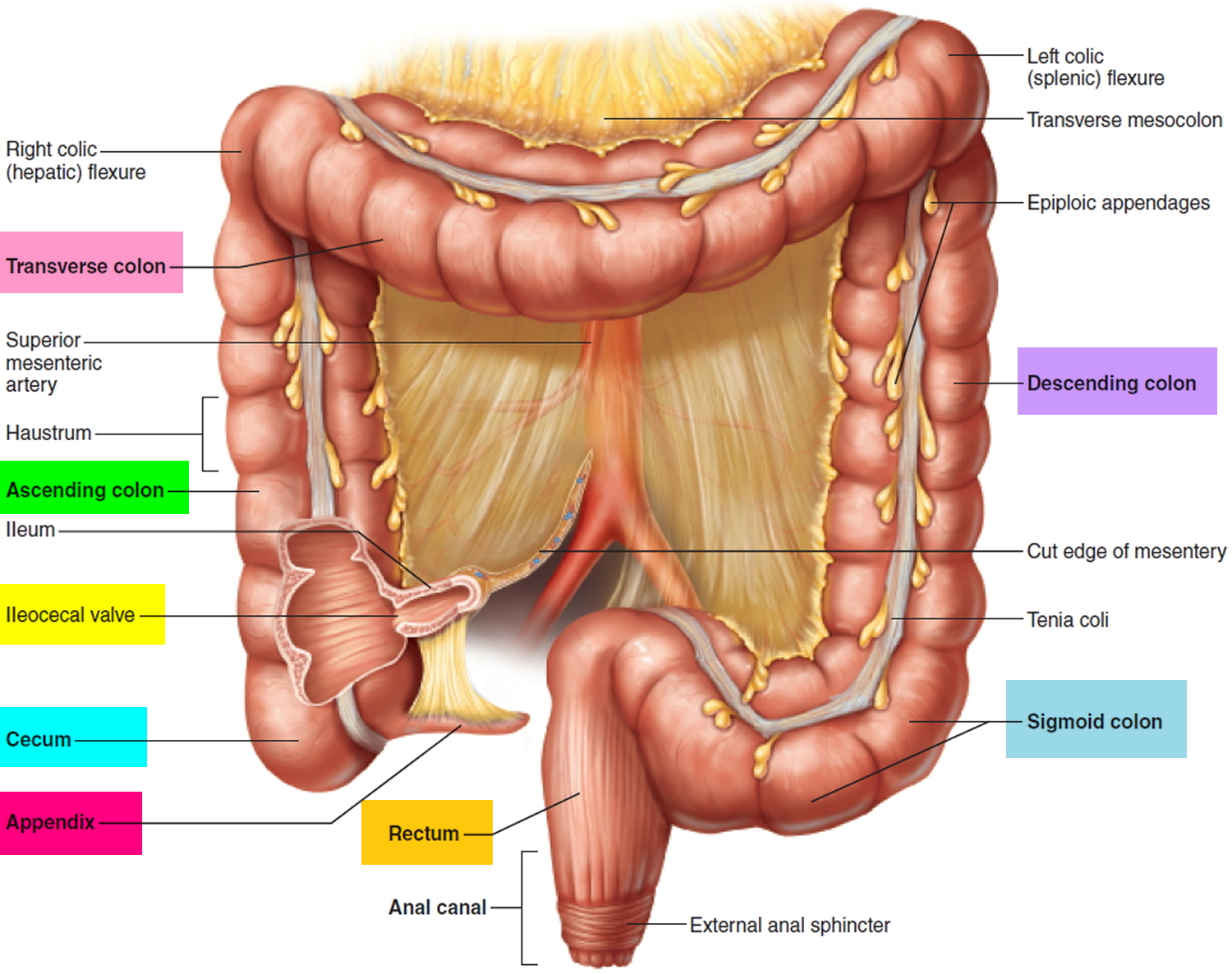
Figure 1. Rectum
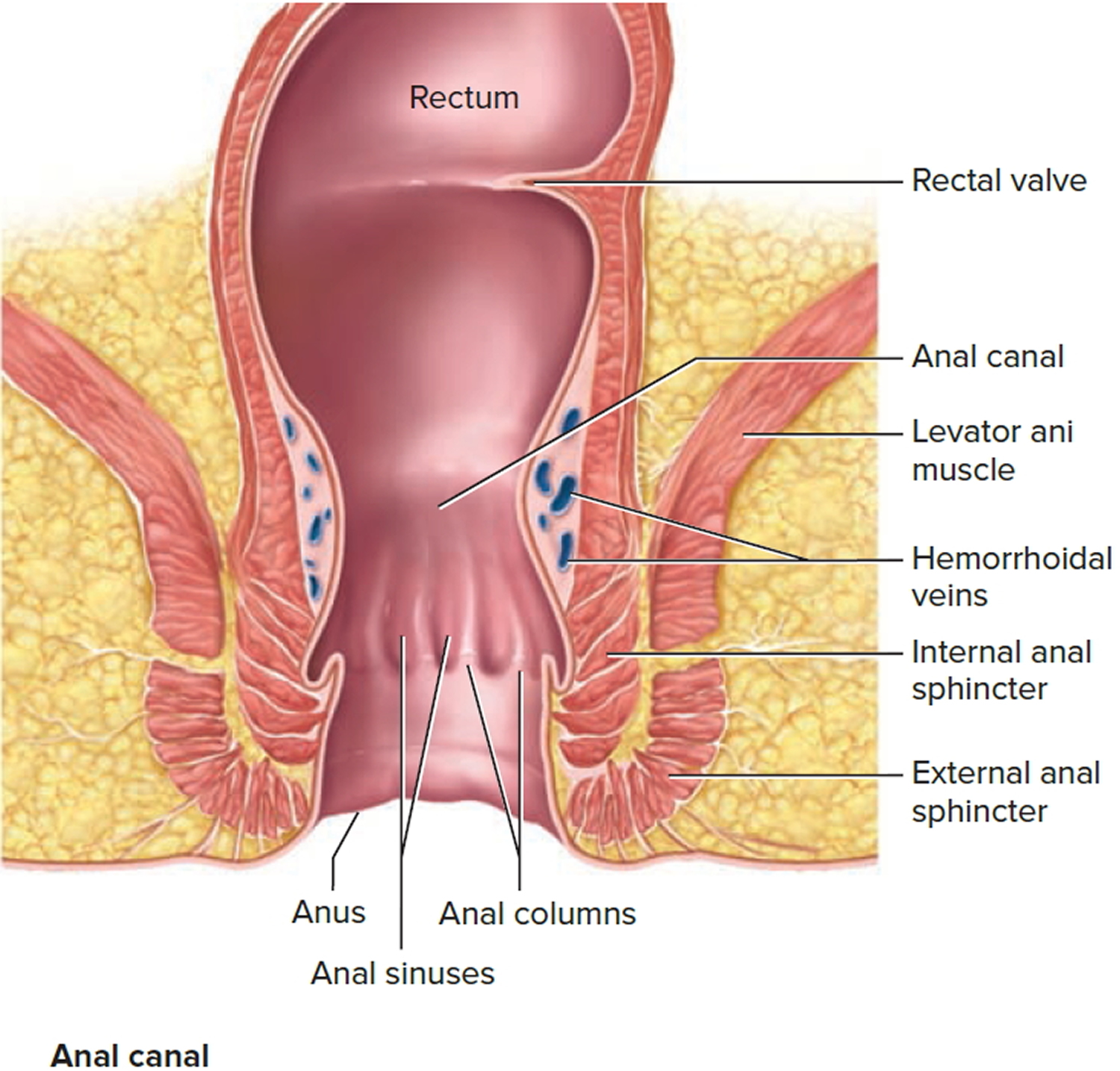
Figure 2. Rectum anatomy and Anus (anal canal)
It’s important to see your doctor if:
- you have any anal bleeding
- you don’t know what’s causing the itchy anus
- the itching is intense
- the itching lasts longer than 3 or 4 days
- keeps coming back
- worries you or makes it hard to sleep
- comes with itching elsewhere on the body.
Your doctor can ensure that rare and specific conditions (such as worms and anal cancer) aren’t overlooked, and can prescribe treatments for the cause of the itchy anus.
Itchy anus at night
An itchy anus that’s worse at night is often caused by threadworms (pinworms), especially in children and are spread easily.
Pinworm is an intestinal infection caused by tiny parasitic worms. It’s a common infection that affects millions of people each year, particularly school-age kids.
You can spot worms in your feces. They look like pieces of white thread. You might also see them around your child’s bottom (anus). The worms usually come out at night while your child is sleeping.
If your child has a pinworm infection, you can see worms in the anal region, especially if you look about 2 or 3 hours after your child has fallen asleep. You also might see the worms in the toilet after your child goes to the bathroom. They look like tiny pieces of white thread and are really small — about as long as a staple. You might also see them on your child’s underwear in the morning.
If your child develops a pinworm infection, try not to worry. Pinworms don’t cause any harm (just itching and restless sleep), and it won’t take long to get rid of them.
Other symptoms can include:
- extreme itching around the anus or vagina, particularly at night
- irritability and waking up during the night
The itching is usually worse at night because the worms move to the area around the rectum to lay their eggs. In girls, pinworm infection can spread to the vagina and cause a vaginal discharge. If the itching leads to broken skin, it can also lead to a bacterial skin infection.
Less common signs of worms include:
- weight loss
- wetting the bed
- irritated skin around the anus
You can buy medicine for threadworms (pinworms) from pharmacies. Many anti-worm preparations, for example pyrantel and mebendazole can be bought over-the-counter at pharmacies. Suspensions are available for children not old enough to take tablets. Your doctor will advise you on the most appropriate treatment for you. This is given in one dose and repeated in 2 weeks.
Treat everyone in your household, even if they don’t have symptoms.
Although medicine takes care of the worm infection, the itching may continue for about a week. So the doctor also might give your child a cream or other medicine to help stop the itching.
Note: Children under 2, and pregnant and breastfeeding women, can’t usually take medicine for threadworms (pinworms) – see your doctor instead.
Medicine kills the threadworms (pinworms), but it doesn’t kill the eggs. Eggs can live for up to 2 weeks outside your body.
There are things you can do to stop becoming infected again.
DO
- wash hands and scrub under fingernails – particularly before eating, after using the toilet or changing nappies
- encourage children to wash hands regularly
- bathe or shower every morning
- rinse toothbrushes before using them
- keep fingernails short
- wash sleepwear, sheets, towels and soft toys (at normal temperature)
- disinfect kitchen and bathroom surfaces
- vacuum and dust with a damp cloth
- make sure children wear underwear at night – change it in the morning
Here are a few ways to prevent pinworm infections in your family:
- Remind kids to wash their hands often, especially after using the toilet, after playing outside, and before eating.
- Make sure your kids shower or bathe every day and change underwear and swimsuits daily.
- Keep kids’ fingernails short and clean.
- Tell kids not to scratch around their bottom or bite their nails.
- Wash your kids’ pajamas every few days.
DON’T
- shake clothing or bedding, to prevent eggs landing on other surfaces
- share towels or flannels
- bite nails or suck thumbs and fingers
How threadworms (pinworms) spread
Threadworms (pinworms) spread when their eggs are swallowed. They lay eggs around your anus, which make it itchy. The eggs get stuck on your fingers when you scratch. They can then pass on to anything you touch, including:
- clothes
- toys
- toothbrushes
- kitchen or bathroom surfaces
- bedding
- food
- pets
Eggs can then pass to other people when they touch these surfaces and touch their mouth. The eggs pass into the digestive system and hatch in the small intestine. They take around 2 weeks to hatch. From the small intestine, pinworm larvae go to the large intestine, where they live as parasites (with their heads attached to the inside wall of the bowel).
About 1 to 2 months later, adult female pinworms travel from the large intestine to the area around the rectum. There, they will lay new pinworm eggs, which trigger itching around the anus.
When someone scratches the itchy area, microscopic pinworm eggs transfer to their fingers. Contaminated fingers can then carry pinworm eggs to the mouth, where they go back into the body, or stay on various surfaces, where they can live for 2 to 3 weeks.
If you’re wondering if your family pet could give your child a pinworm infection, it can’t. Pinworms don’t come from animals.
Children can get worms again after they’ve been treated for them if they get the eggs in their mouth. This is why it’s important to encourage children to wash their hands regularly.
Itchy anus symptoms
Anal itching may be associated with redness, burning and soreness. The itching and irritation may be temporary or more persistent, depending on the cause.
Primary or idiopathic itchy anus is classified by a staging system used at Washington Hospital Center, and is based on the physical features of the skin. Stage 0 is normal skin, stage 1 is red and inflamed skin, stage 2 has thickened skin, and stage 3 has thickened skin, coarse ridges, and often ulcerations.
Itchy anus diagnosis
Your doctor may be able to diagnose the cause of your itching simply by asking you questions about your symptoms, medical history and personal habits. Toileting behaviors must be evaluated, including the frequency and quality of stools, possible feces or mucus leakage, perianal moisture sensation, or the sensation of incomplete evacuation of stool. In addition, hygiene rituals or cleansing methods after a bowel movement must be evaluated.
Travel history and current medications, including all topical agents used, must be reviewed. A detailed diet history should be taken with close attention to known dietary agents suspected of causing itchy anus. Often a heavy consumption of caffeine with coffee, tea, cola, or energy drinks is present. Lastly, investigation regarding possible infectious agents, such as threadworms (pinworms) in children, should also be considered. Adults rarely harbor threadworms (pinworms).
Your doctor will perform an office physical examination to provide information regarding a possible cause of the symptoms. Examination should include a thorough inspection of the skin around the anus. The skin may appear normal or may have findings such as open wounds or cracks, redness, or possible characteristic changes of thickened skin due to repeated scratching and irritation.
In addition to inspection of the perianal region, your doctor may place a finger through the anus into the rectum (digital rectal exam). Part of the evaluation of the anal canal may be completed with a small instrument or anoscope which is referred to as “anoscopy.” An office biopsy with a small 3 or 4 mm piece of tissue may also be obtained to help with diagnosis and decision-making regarding treatment. Skin swabs or scrapings may also be obtained. Physical examination may also involve inspection of other sites of involvement.
The detailed anal examination is necessary, but brief, and patients should not feel embarrassed. The examination may have some feelings of discomfort but should not be painful.
If the cause of your itching isn’t obvious, your doctor may refer you to a skin specialist (dermatologist) or a doctor who specializes in treating rectal and anal problems (proctologist). He or she may do other tests, such as proctoscopy or colonoscopy to view more of the digestive tract. But it’s possible the cause of the itching may never be identified.
Itchy anus treatment
The goal of therapy is to restore clean, dry, and intact skin. Treatment can be challenging, as many cases have no clear identifiable cause.
Normalisation of bowel motions
Additional fiber and an adequate fluid intake should be directed toward achieving the perfect stool, said to be that which is formed yet so smooth that it barely requires the use of toilet paper. It is important to use bowel medications to thicken stool and create a formed bowel movement to minimize leakage or seepage and also to allow for complete evacuation. The goal is a soft, bulky, easy to clean stool. Most people can benefit from taking a fiber supplement (Citrucel®, Metamucil®, Fibercon®, Benefiber®, and Konsyl® are examples). This can be taken in powder or capsule/tablet form and is usually taken once or twice daily. The fiber serves to absorb the moisture from the stool, adding bulk and allowing for complete evacuation of stool during bowel movements.
If stools still remain loose, additional medications may be helpful. Imodium® is an antidiarrheal medication which can thicken or firm stool and help decrease seepage. In more difficult cases, prescription medications such as Lomotil® may be needed to thicken the stool. Your physician can help decide which medications may be best for you.
Dietary changes are often necessary for treatment. There are several common foods which may be related to itchy anus. These foods and beverages include coffee, colas, tea, chocolate, tomatoes and beer. These items may possibly decrease your sphincter tone which can cause some seepage or leakage. Avoiding overuse of these items may improve symptoms. It may be helpful to remove one item at a time from your diet for several weeks. If your symptoms improve, you could try reintroduction of the item in smaller volume and see if there is a limit to which you may have that item without producing symptoms.
Cleaning after defecation
It will also be important to modify bowel hygiene or cleaning habits. It must be stressed that the anus does not need to be scrubbed or sterilized. Cleaning with plain water rinses is quite helpful. Soaps, perfumes, dyes in tissue or clothing, and baby wipes containing deodorants should be avoided because they can act as irritants. Alcohol and witch hazel agents should similarly be avoided. Bathing with Dove® soap is recommended, as it is free of conventional soap. Also, handheld detachable shower heads can be used to clean and wash away any remaining soap residue. The same effect can also be created with a bidet, although they are not common in the U.S.
Balneol® is a gentle and soothing cleaning agent. It is commercially available mineral oil-based preparation that can be used at home or taken along in a pocket or a purse for use in public facilities. Another possible cleaning agent is dilute white vinegar. One tablespoon in an 8 ounce glass of water can be kept in the bathroom and applied with a cotton ball. Burrow’s solution, diluted at 1:40 (one Domeboro® tablet in 12 ounces of water or one tablet in six ounces of water for 1:20 solution) is also a gentle and non-irritating cleanser. It can be kept in a plastic squeeze bottle in the refrigerator and used in place of soap and water.
The ultimate goal of treatment is to create dry, healthy, and intact skin. The skin can be dried after cleansing using a hair dryer on low setting. An athlete’s foot powder or Zeasorb®, a lubricating and drying agent in powder form can also be used to absorb moisture. After drying, the athlete’s foot powder or Zeasorb® can be applied, and a small piece of cotton can be placed between the buttocks and against the anus to help absorb the moisture. Tight fitting, synthetic undergarments should be avoided.
Do not scratch!
One of the most important, but often most difficult, aspects of the management of itchy anus, is to avoid trauma to the skin. This means no scratching with hands or dry toilet paper. Behavioral modification is often very difficult to achieve, due to the intense desire to scratch. Many people also scratch during sleep and are not aware of it until they wake to find themselves scratching. It is often recommended to have patients cut their nails and wear a pair of light, soft, cotton gloves on their hands at night so they are not able to scratch.
Itchy anus cream
In order to control symptoms, a short course of a steroid ointment may be tried. A weak topical steroid such as 1% hydrocortisone cream used two to three times a day for a short period of time can be effective in relieving symptoms of pruritis 1. A long-acting topical steroid such as betamethasone may also be effective. Strong steroids or prolonged use can lead to skin atrophy (weakness and thinning) which sometimes worsens itchy anus. High potency steroids should not be used for more than four to eight weeks. If there is thinned or denuded skin, topical antibiotics may occasionally be helpful. It should be noted that cream forms of medication cause more thinning or atrophy than ointment forms.
A skin barrier cream such as zinc oxide may also be helpful in protecting the skin around the anus from irritants. Additional topical agents such as numbing medications, menthol, phenol, camphor, or a combination of them may be helpful. Calmoseptine® is used frequently, with a combination of zinc oxide and menthol and can be very beneficial at relieving patients’ symptoms. If there is any concern that there may be an infection, topical antibiotics (gentamicin, clindamycin, or bacitracin) or antifungals (clotrimazole, nystatin) may be added in conjunction with other therapies. They can be applied at nighttime before bed and again in the morning after bathing.
Other treatments for intractable pruritus
Patients coming to the doctor for evaluation of itchy anus with moderate to severe changes of the skin, may be treated by application of Berwick’s dye (which is a combination of gentian violet and brilliant green pigment) with alcohol. It can relieve itching but will sting if there are open wounds. Your physician can dry the dye with a hair dryer and it can be sealed in place with Benzoin tincture and then again dried in place. This dye can stay in place for several days and will often give great relief while the skin is able to regenerate or re-epithelialize. This treatment is performed in an office setting, but is not used in the home setting.
You may notice that your problems will improve for some time with treatment but then recur. For a small number of patients, itchy anus can be quite difficult to manage, and it may be difficult to completely relieve their symptoms. In these patients, it may be beneficial to try topical capsaicin 2. Capsaicin comes from Capsicum chili peppers. It is believed to work by depressing the feelings or desensitizing certain nerves. This medicine has been studied with a small number of patients, and up to 70% of patients had relief of their symptoms for up to almost 11 months. The medicine is applied with a very low concentration of 0.006%.
A very small number of patients find only minimal relief from all attempted treatment options. These individuals may benefit from injectable therapy. This particular therapy is saved for patients with persistent and intense itchy anus. Methylene blue is a dye which can be injected into the skin and may relieve symptoms by causing destruction of the nerve endings 3. The methylene blue can be mixed with topical anesthetics and injected into and below the affected perianal region. Many patients do experience a change in sensation in the injected area. It may feel somewhat numb like a local anesthetic for a dental procedure. It also will turn the skin in the area blue. In very rare cases, this may be injected too close to the surface of the skin and may cause some skin breakdown or ulcerations.
How to stop anal itching yourself
DO
- gently wash and dry your anus after pooing and before bed
- wear loose-fitting cotton underwear
- keep cool – avoid clothing and bedding that makes you overheat
- have cooler, shorter showers or baths (under 20 minutes)
- eat plenty of fiber – such as fruit and vegetables, wholegrain bread, pasta and cereal – to avoid runny poo or constipation
- avoid prolonged sitting
DON’T
- wipe your bottom after pooing – instead, wash with water or pat clean with moist toilet paper, then pat dry
- scratch – if you can’t stop, keep fingernails short and wear cotton gloves at night
- strain when you go to the toilet
- use scented soaps, bubble bath or bath oil
- use perfumes or powders near your anus
- eat spicy food or drink lots of alcohol and caffeine – these can make itching worse
Using creams and ointments for an itchy anus
Don’t use:
- more than one cream or ointment at the same time
- any cream or ointment for longer than a week – they can irritate your skin and make things worse
Lifestyle and home remedies
Prevention of anal itching mainly involves washing properly, keeping the area clean, cool and dry, and avoiding irritants. If you already have anal itching, try these self-care measures:
- Cleanse gently. After bowel movements, clean the area with plain water or mild soap. It may help to use moist cotton balls or a small squeeze bottle of water. Don’t scrub. The goal is to keep the area clean without further irritating the skin.When traveling by air, take an empty squeeze bottle that you can readily fill with water in bathrooms.
- Dry thoroughly. After cleansing, pat the area dry with toilet paper or a towel. Or use a hair dryer set on low. Unmedicated talcum can help keep the area dry. Avoid cornstarch powder, which can foster bacterial growth. You could place a moistened or dry cotton ball against the anus to help absorb moisture. Replace it as needed.
- Don’t scratch. Scratching further irritates your skin and leads to persistent inflammation. You may find some relief by applying a cold compress to the area or taking a lukewarm bath. Trim your nails short and wear cotton gloves while you’re sleeping to help prevent scratching.
- Wear cotton underwear and loose clothing. This helps keep the area dry. Avoid wearing pantyhose and other tightfitting garments because these can trap moisture.
- Avoid irritants. Avoid bubble baths, genital deodorants, perfumed soaps, moist wipes, witch hazel products and other items that might irritate the anal area. Cut back on or avoid coffee, cola, alcohol, citrus fruits, chocolate, spicy foods, tomatoes and foods that may cause diarrhea. Avoid overuse of laxatives.
- Apply ointments or gels. Protect your skin from moisture by applying a thin layer of a zinc oxide ointment (Desitin, Balmex) or petroleum jelly. You could also use a 1 percent corticosteroid cream (Cortaid, Preparation H Anti-Itch Cream) two or three times a day to relieve itching. But don’t use this type of cream for more than two weeks because of possible side effects, such as thinning of the skin.
- Maintain regular, firm bowel movements. If soft stools or frequent bowel movements are a problem, gradually adding fiber to your diet may help. Fiber supplements, such a Metamucil or Citrucel, also may help.
- Siddiqi S, Vijay V, Ward M, Mahendran R, Warren S. Pruritus ani. Ann R. Coll Surg Engl 2008;90:457–63.[↩]
- Lysy J, Sistiery-Ittah MJ, Israelit Y, et al. Topical capsaicin – a novel and effective treatment for idiopathic intractable pruritus ani: a randomised, placebo controlled, crossover study. Gut 2003;52:1323–6.[↩]
- Jones D. ABC of colorectal diseases: Pruritus ani. BMJ 1992;305:575–7.[↩]