Contents
What is latex
Over 90% of natural rubber comes from the latex or milky sap of the rubber tree – Hevea brasiliensis. The sap is blended with chemicals during manufacturing to give latex its elastic quality. Latex is used in a large number of products including adhesives, foam, carpet backing and in a number of “dipped” products. Dipped products include surgical gloves, household gloves, catheters, condoms, balloons, etc. Natural latex rubber is also found in toys, erasers, sports equipment, clothing, elastic bands, and many medical and dental devices. Latex can also be in bottle nipples and pacifiers. Synthetic products, including latex house paints, have not been shown to pose any hazard to latex-sensitive individuals. Certain fruits and vegetables (such as bananas, chestnuts, kiwi, avocado and tomato) can cause allergic symptoms in approximately 50% of latex-sensitive individuals.
For reasons not yet clearly understood, some individuals can become allergic to certain constituents of the latex molecule. If you are allergic to latex your body treats latex as an allergen and sets off an allergic reaction.
Latex allergy occurs when your body’s immune system overreacts to proteins found in natural rubber latex, through contact with your skin, mucous membranes, parenteral, intravenous and inhalation. If you have a latex allergy, your immune system identifies something that is typically harmless as an invader or allergen. With latex allergy, it overreacts by producing antibodies called Immunoglobulin E (IgE) that can react with contaminating proteins found in the natural rubber latex. These antibodies travel to cells that release chemicals, causing an allergic reaction. This reaction usually appears in the nose, lungs, throat, sinuses, ears, lining of the stomach or on the skin.
Once allergic, you may remain sensitive for the rest of your life. Latex allergies are most common in people who have regular exposure to latex products such as rubber gloves. That is why this allergy is most common among healthcare workers and people who have undergone multiple surgeries.
Growth in the latex allergy problem has been related to the rising demand and use for latex products. The onset of recommendations for universal precautions resulted in increased use of latex gloves – to meet the increased demand, manufacturing processes may have changed resulting in a more highly allergic product.
Latex allergy may cause mild itchy skin and hives to very severe anaphylaxis, a potentially life-threatening condition that can cause throat swelling and severe difficulty breathing. Every year, there are hundreds of cases of anaphylaxis. The severity of allergic reactions to latex can worsen with repeated exposure to the substance.
Other chemicals used to make latex gloves can cause a delayed onset rash which only forms where the material touches the skin. This is called contact dermatitis. Red, itchy bumps or blisters usually appear within 12 to 48 hours. These symptoms are irritating, but not life-threatening.
Latex can also become airborne and cause respiratory symptoms. For example, latex proteins can attach to the cornstarch powder used in latex gloves. As powdered latex gloves are used, the starch particles and latex allergens become airborne, where they can be inhaled or come into contact with your nose or eyes and cause symptoms. High concentrations of this allergenic powder have been measured in intensive care units and operating rooms. Using non-powdered latex gloves, or synthetic (vinyl, nitrile) gloves reduces the risk of these reactions. The capacity of latex products – especially gloves – to cause allergic reactions varies enormously by brand and by production lot.
Given the potential for a very serious allergic reaction, proper diagnosis of latex allergy is important. Your doctor / allergist / immunologist has specialized training and expertise to accurately diagnose your condition and provide relief for your symptoms.
Understanding latex allergy and knowing common sources of latex can help you prevent allergic reactions.
- People who react to latex typically develop a skin rash. This is irritating, but not life-threatening.
- However, if you have trouble breathing when you are around latex, or if you get a combination of symptoms, get immediate medical attention. These symptoms include hives, itching or flushing, swelling, sneezing, runny nose, cough, wheeze, shortness of breath, chest tightness, nausea, dizziness or lightheadedness.
- There is no cure for latex allergy. People with severe reactions must avoid latex.
- An allergist is the best physician to determine if you are allergic to latex and help you develop a treatment plan.
Anaphylaxis Life-threatening symptoms:
- trouble breathing or noisy breathing
- difficulty talking more than a few words and/or hoarse voice
- wheeze
- cough
- swelling and tightness of the throat
- collapse
- light-headedness or dizziness
- diarrhea
- tingling in the hands, feet, lips or scalp
- swelling of tongue
- pale and floppy (in young children)
A severe allergic reaction (anaphylaxis) is a medical emergency. Call your local emergency immediately. Lay the person down. If they have an adrenaline injector and you are able to administer it, do so.
Who is at risk of latex allergy?
Anyone who is exposed to latex may become sensitized – fortunately, the majority of individuals do not. However, certain populations are more at risk:
- rubber-industry workers
- healthcare workers (from wearing rubber gloves)
- individuals with congenital urinary anomalies (from use of catheters and other latex devices) e.g. children with spina bifida.
- individuals with a history of sensitivity to certain foods i.e. banana, avocado, chestnut, tomato, peach or kiwifruit
- individuals who have undergone multiple medical/surgical procedures
- individuals with a history of non-medication related anaphylactic reactions during anesthesia.
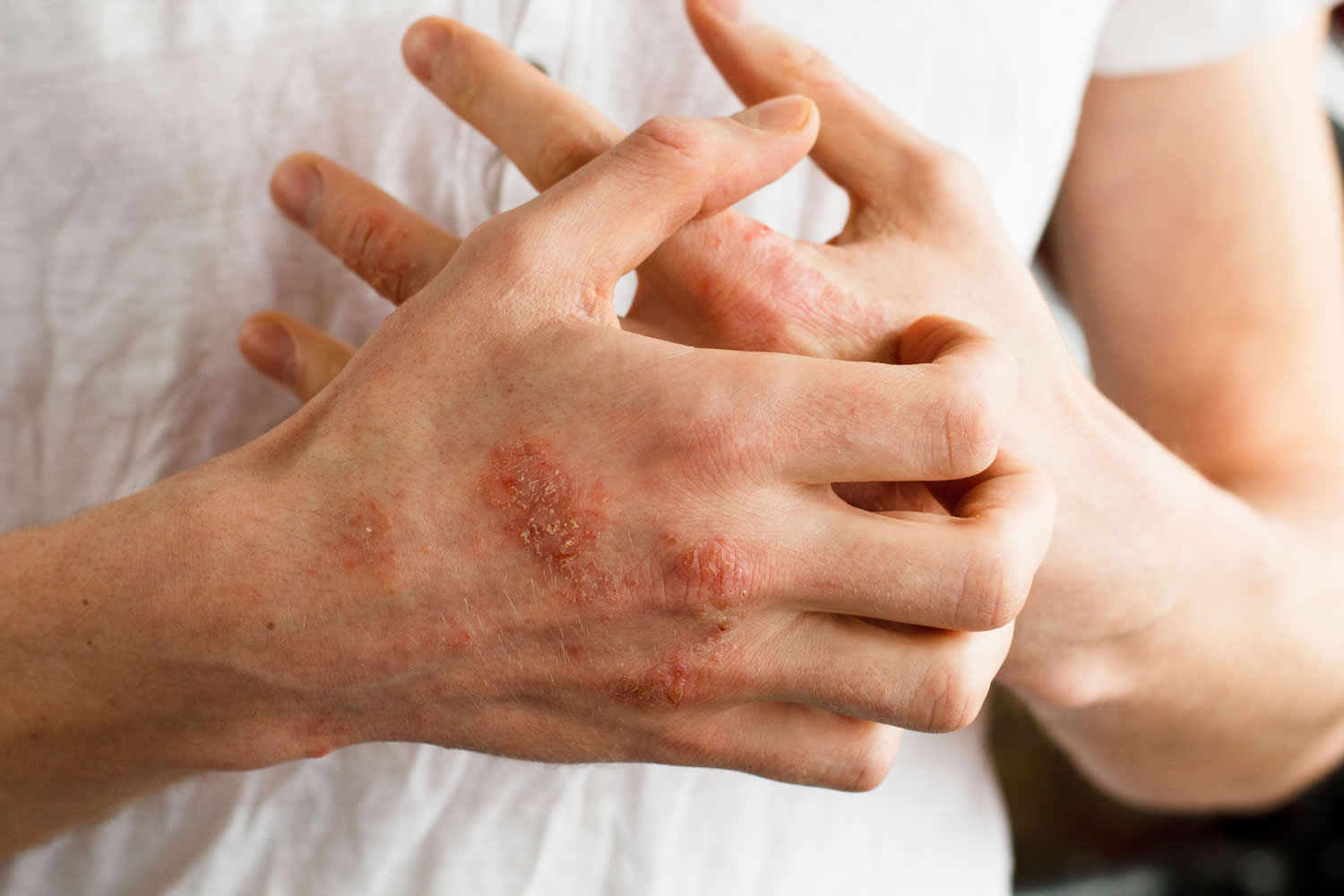
Figure 1. Latex allergy rash
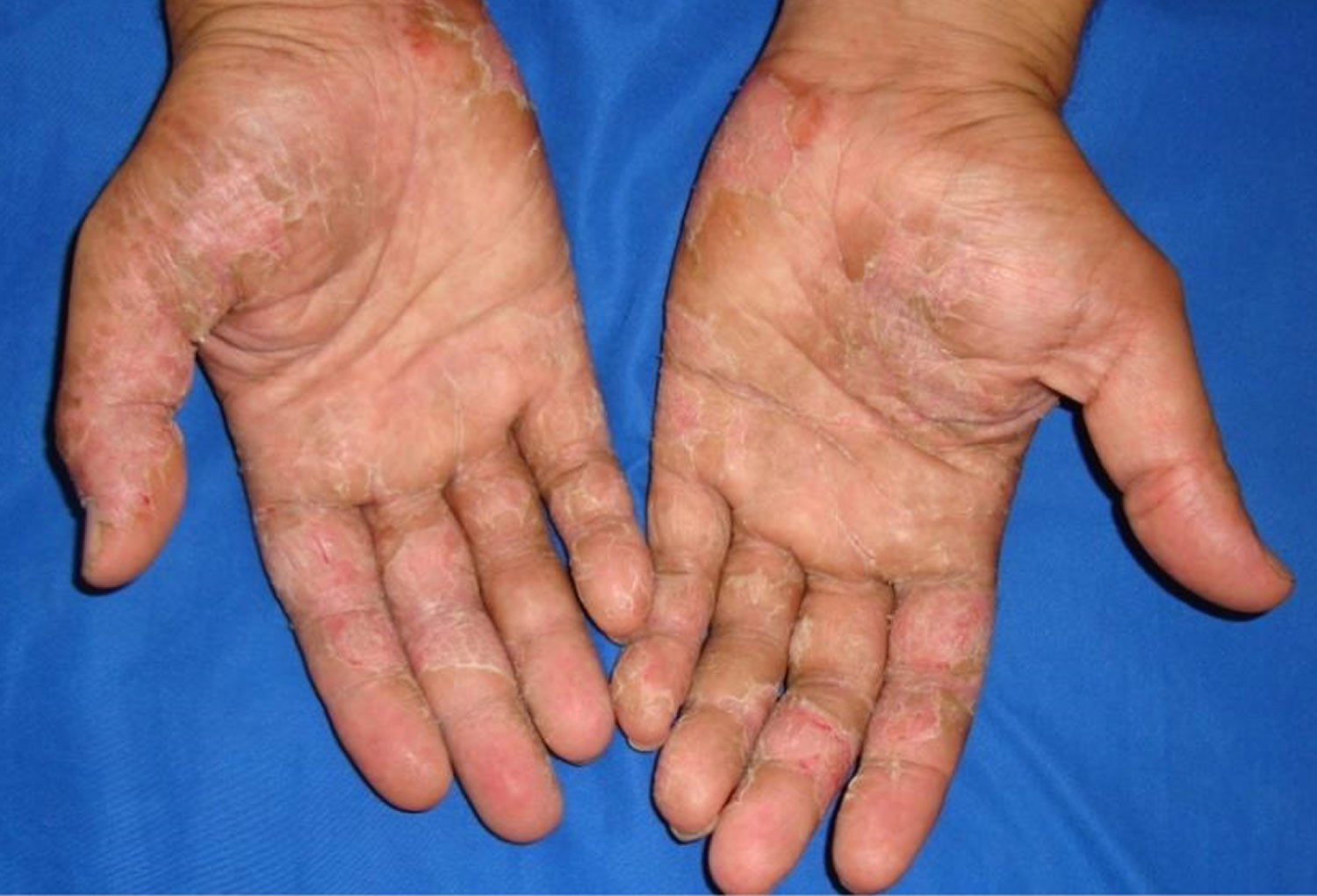
Figure 2. Latex glove allergy rash
Types of reactions to latex
The common reactions of latex sensitive individuals exposed to latex are contact urticaria, dermatitis and asthma.
- Contact urticaria usually presents with itching and swelling of the skin at the site of contact with latex. This may, for example, be hands from wearing gloves, genitals from contact with condoms, etc. The symptoms usually start within 5 – 15 minutes after coming into contact with the latex article, although it can be delayed for several hours. Symptoms can continue for a variable period, from several hours to days after the latex contact has ceased.
- Delayed-type Contact Dermatitis from latex may take several days to appear. It presents with an itchy, scaly rash, although there may be small blisters if the reaction is acute. The rash will usually last several days to weeks but if exposure to latex continues, the rash will last longer. Contact dermatitis is not generally caused by sensitivity to latex protein but rather to the chemicals used in the manufacture of the latex product, including antioxidants and rubber accelerators e.g. thiuram, carbamates, MBT, etc.
- Immediate-type hypersensitivity requires previous sensitization and is the most potentially dangerous reaction to latex. Clinical presentations vary but may include contact urticaria, coryza (sneezing or runny nose due to irritation and swelling of the mucous membrane in the nose), conjunctivitis (swollen or irritation of the conjunctiva), stinging or burning, asthma, and, with mucosal or parenteral exposure, anaphylaxis. A common cause for the asthmatic reaction is powdered gloves. The starch powder picks up the latex proteins and when the gloves are removed the powders can then be inhaled or come into contact with the skin on the face where it can cause an allergic reaction. In the most serious allergic reaction, symptoms occur within minutes and involve multiple systems in the body. This life threatening condition is called anaphylaxis.
Latex allergy symptoms
If you’re allergic to latex, you’re likely to have symptoms after touching latex rubber products, such as gloves or balloons. You can also have symptoms if you breathe in latex particles that are released into the air when someone removes latex gloves.
Latex allergy symptoms range from mild to severe. A reaction depends on how sensitive you are to latex and the amount of latex you touch or inhale. Your reaction can become worse with each additional latex exposure.
Mild symptoms
Mild latex allergy symptoms include:
- Itching
- Skin redness
- Hives or rash
More-severe symptoms
These include:
- Sneezing
- Runny nose
- Itchy, watery eyes
- Scratchy throat
- Difficulty breathing
- Wheezing
- Cough
Life-threatening symptoms: Anaphylaxis
The most serious allergic reaction to latex is anaphylaxis, which can be deadly. An anaphylactic reaction develops immediately after latex exposure in highly sensitive people, but it rarely happens the first time you’re exposed.
Symptoms of severe allergy (anaphylaxis) may include:
- trouble breathing or noisy breathing
- difficulty talking more than a few words and/or hoarse voice
- wheeze
- cough
- swelling and tightness of the throat
- collapse
- light-headedness or dizziness
- diarrhea
- tingling in the hands, feet, lips or scalp
- swelling of tongue
- pale and floppy (in young children)
A severe allergic reaction (anaphylaxis) is a medical emergency. Call your local emergency immediately. Lay the person down. If they have an adrenaline injector and you are able to administer it, do so.
Figure 2. Anaphylaxis Emergency Action Plan
 Causes of latex allergy
Causes of latex allergy
In a latex allergy, your immune system identifies latex as a harmful substance and triggers certain antibodies to fight it off. The next time you’re exposed to latex, these antibodies tell your immune system to release histamine and other chemicals into your bloodstream, producing a range of allergy signs and symptoms. The more times you are exposed to latex, the more strongly your immune system is likely to respond. This is called sensitization.
Latex allergy can occur in these ways:
- Direct contact. The most common cause of latex allergy involves touching latex-containing products, including latex gloves, condoms and balloons.
- Inhalation. Latex products, especially gloves, release latex particles, which you can breathe in when they become airborne. The amount of airborne latex from gloves differs greatly depending on the brand of glove used.
It’s possible to have other skin reactions when using latex. They include:
- Allergic contact dermatitis. This reaction results from the chemical additives used during manufacturing. The main sign is a skin rash with formation of blisters 24 to 48 hours after exposure, similar to poison ivy.
- Irritant contact dermatitis. Not an allergy, this skin irritation is caused by wearing rubber gloves or exposure to the powder inside them. Signs and symptoms include dry, itchy, irritated areas, usually on the hands.
Not all latex products are made from natural sources. Products containing man-made (synthetic) latex, such as latex paint, are unlikely to cause a reaction.
Risk factors for latex allergy
Certain people are at greater risk of developing a latex allergy:
- People with spina bifida. The risk of latex allergy is highest in people with spina bifida — a birth defect that affects the development of the spine. People with this disorder often are exposed to latex products through early and frequent health care. People with spina bifida should always avoid latex products.
- People who undergo multiple surgeries or medical procedures. Repeated exposure to latex gloves and medical products increases your risk of developing latex allergy.
- Health care workers. If you work in health care, you’re at increased risk of developing a latex allergy.
- Rubber industry workers. Repeated exposure to latex may increase sensitivity.
- People with a personal or family history of allergies. You’re at increased risk of latex allergy if you have other allergies — such as hay fever or a food allergy — or they’re common in your family.
Connection between food allergy and latex allergy
Certain fruits contain the same allergens found in latex. They include:
- Avocado
- Banana
- Chestnut
- Kiwi
- Passion fruit
If you’re allergic to latex, you have a greater chance of also being allergic to these foods.
Prevention of latex allergy
The only way to prevent an allergic reaction to latex is to avoid the substance. A new, natural rubber latex from the desert plant guayule is now being used for many products. This product is thought to be a safer alternative for people with latex allergy and healthcare workers.
Synthetic products are also safe. Substitutes for latex gloves, such as vinyl or nitrile gloves, should be used at all times by people with latex allergy.
Natural skin condoms are available, but while they protect against pregnancy, they do not shield against HIV or other sexually-transmitted diseases.
If you have mild skin reactions from latex, anti-inflammatory medications may help relieve symptoms.
People at risk of a serious, anaphylactic reaction to latex should carry autoinjectible epinephrine everywhere in case of emergency. Be sure to seek medial attention immediately in the event of a serious reaction.
Many common products contain latex, but you can usually find a suitable option. Prevent an allergic reaction to latex by avoiding these products:
- Dishwashing gloves
- Some types of carpeting
- Balloons
- Rubber toys
- Hot water bottles
- Baby bottle nipples
- Some disposable diapers
- Rubber bands
- Erasers
- Condoms
- Diaphragms
- Swim goggles
- Racket handles
- Motorcycle and bicycle handgrips
- Blood pressure cuffs
- Stethoscopes
- Intravenous tubing
- Syringes
- Respirators
- Electrode pads
- Surgical masks
- Dental dams
Many health care facilities use nonlatex gloves. However, because other medical products may contain latex or rubber, be sure to tell doctors, nurses, dentists and other health care workers about your allergy before all exams or procedures.
Wearing a medical alert bracelet can inform others of your latex allergy.
Latex Allergy – Guidelines for Health Care Workers
Help prevent latex sensitivity
- Use appropriate work practices to reduce chance of reactions to latex. When wearing latex gloves, use only approved barrier cream. After removing latex gloves, wash hands thoroughly and dry thoroughly.
- Practice good housekeeping: frequently clean areas and equipment contaminated with latex-containing dust.
- Learn to recognize the symptoms of latex allergy: skin rash; hives; flushing; itching; nasal, eye or sinus symptoms; asthma; and (rarely) shock.
- Care should be exercised when removing latex gloves to reduce the risk of exposure of latex allergens to self and/or colleagues.
Latex allergy in the health care worker
- Avoid contact with latex gloves and products. Commonly used latex medical products include: rubber gloves; elastic bandages; adhesive tape; urinary catheters; electrode pads; wound drains; stomach and intestinal tubes; urinary collection devices; protective sheets; enema tubing and tips; dental cofferdams; rubber pads; and fluid circulating warming blankets. Equipment containing latex includes: haemodialysis and anaesthesia equipment; rubber masks; electrode pads; head straps; rubber tourniquets; rubber nasal-pharyngeal airways; rubber oral-pharyngeal airways; teeth protectors; bite blocks; blood pressure cuffs; rubber breathing circuits; reservoir breathing bags; rubber ventilator hoses and bellows; rubber endotracheal tubes; latex cuffs on plastic tracheal tubes; latex injection ports on intravenous tubing; and certain epidural catheter injection adaptors.
- Avoid areas where you might inhale the powder from latex gloves worn by other workers.
- Tell your employer and health providers (physicians, nurses, dentists, etc) that you have latex allergy.
- Wear a medical alert bracelet.
- Consult with your doctor to determine whether you should carry an emergency adrenaline (epinephrine) kit in case of accidental exposure to latex and/or in the event of anaphylactic shock (adrenaline immediately counteracts the shock).
Patients with latex sensitivity
The following guidelines are summarized U.S. Food and Drug Administration (FDA) advice to health professionals to ensure a patient’s latex allergy is not overlooked 1:
- Include questions about latex sensitivity when taking a patient’s health history – asking patients whether they have ever experienced itching, rash or wheezing after wearing latex gloves or inflating a toy balloon may be useful. Spina bifida patients are at higher risk for acquiring latex allergy, as are others who have undergone numerous medical procedures. As well, patients with sensitivity to certain foods (chestnuts, kiwifruit, bananas, avocado, peaches, figs, passion fruit) should be considered high risk for latex allergy.
- Those patients who report signs of latex allergy should have the allergy recorded in the clinical notes.
- Ensure patients are informed when they have had a suspected latex-related allergic reaction while under the professional’s care, and recommend a latex allergy test to those individuals.
- A latex-safe environment should be offered to patients with latex allergy:
- no-one in the area should wear powdered natural rubber gloves
- only non-latex gloves should be used to directly examine the patient
- do not inject or withdraw fluid through rubber ports or intravenous lines
- all natural rubber latex products that routinely directly or indirectly come into contact with mucosa, non-intact skin, and internal bodily spaces (e.g. catheters, endotracheal tubes) should be removed or made latex -safe (e.g. covering – blood pressure cuffs used over clothing, stethoscope tubing covered with stockinette)
- products made of dry-moulded rubber (e.g. wheelchair tyres, tool handles) do not need to be removed from the area but if direct contact with such objects is routine, precautions should be taken to minimise direct exposure by covering the object or body part exposed (i.e. having the patient wear nonlatex gloves while wheeling self in wheelchair)
- hospital dietary services should have latex-safe meals that lack food known to cross-react with antibodies to natural rubber latex (e.g. avocado, banana, potato, tomato, papaya, chestnut or kiwifruit)
- if a latex-safe operating room is not always available, patients should be scheduled as the first procedure of the day so that latex-allergens can not build up in the environment
- For patients with an identified latex allergy e.g. alert in clinical notes, medical alert bracelet, etc. staff will need to have latex-free products available. It is recommended that each ward/department consider which of their patients are likely to be “high risk” and develop an emergency kit of latex-free products for use (acknowledging that there may be other patients not identified as “high risk” who may develop a latex allergy). The equipment required will vary and will need to be identified by the clinical area.
Latex allergy diagnosis
Diagnosis is sometimes a challenge. Your doctor will examine your skin and ask questions about your symptoms and medical history. Tell your doctor about your reactions to latex and if you’ve had any other allergy signs and symptoms. Your doctor will also ask questions to rule out other reasons for your symptoms.
- In most cases, a diagnosis of latex allergy can be made from an accurate history and clinical examination.
There are a number of skin tests which can confirm latex sensitivity, including patch tests (for allergic contact dermatitis type reactions), skin prick test (for contact urticaria type reactions) and radioallergosorbent assay blood test (RAST) which is not as accurate as the skin tests.
A skin test can help determine if your skin reacts to the latex protein. The doctor will use a tiny needle to place a small amount of latex below the surface of the skin on your forearm or back. If you’re allergic to latex, you develop a raised bump. Only an allergist or other doctor experienced in skin testing should perform this test.
Blood tests (RAST) also may be done to check for latex sensitivity.
Latex allergy treatment
Although medications are available to reduce the symptoms of latex allergy, there is no cure for latex allergy. The only way to prevent a latex allergic reaction is to avoid products that contain latex.
The first step in living with a latex allergy is being aware of the problem. An allergist / immunologist, often referred to as an allergist, has the knowledge and experience to diagnose the problem and develop a treatment plan.
If your allergy is severe, it is important to tell your family, employer, school personnel and healthcare providers about your allergy and have an Anaphylaxis Emergency Action Plan (see Figure 2 above).
If you need surgery, ask that everything be latex-free.
If you have trouble breathing when you are around latex, stay away from areas where powdered gloves are used and avoid all direct contact with latex.
If you must wear gloves, try substituting vinyl or nitrile gloves for latex. Synthetic latex gloves do not contain natural latex and are another option. These work in nearly all situations, including surgery, but they may be more expensive. If you tend to get a skin rash reaction to latex, latex gloves made without additional chemicals may be a good choice.
Latex condoms may cause serious allergic reactions in some people. If either partner has a latex allergy, synthetic rubber condoms are the best choice, although natural skin condoms may be used.
Despite your best efforts to avoid latex, you may come into contact with it. If you’ve had a severe allergic reaction to latex, you may need to carry injectable epinephrine with you at all times. If you have an anaphylactic reaction, you will need to go to the emergency room for an immediate injection of adrenaline (epinephrine).
For less severe reactions, your doctor may prescribe antihistamines or corticosteroids, which you can take after exposure to latex to control your reaction and help relieve discomfort.
- https://www.fda.gov/RegulatoryInformation/Guidances/default.htm[↩]