Contents
- What is lichen planus
- What are the clinical features of lichen planus?
- Lichen planus outlook (prognosis)
- Lichen planus possible complications
- Lichen planus causes
- Lichen planus symptoms
- Lichen planus diagnosis
- Lichen planus treatment
What is lichen planus
Lichen planus is a chronic inflammatory and non-infectious skin condition that forms itchy rash on the skin, scalp, nails, genital, vulva and/or mucosal surfaces. Lichen planus affects up to 1-2% of the population, which generally occurs in middle-aged adults (adults over the age of 40 years). About half those affected have oral lichen planus, which is more common in women than in men. About 10% have lichen planus of the nails. Lichen planus is less common in children. A history of lichen planus in family members is sometimes present.
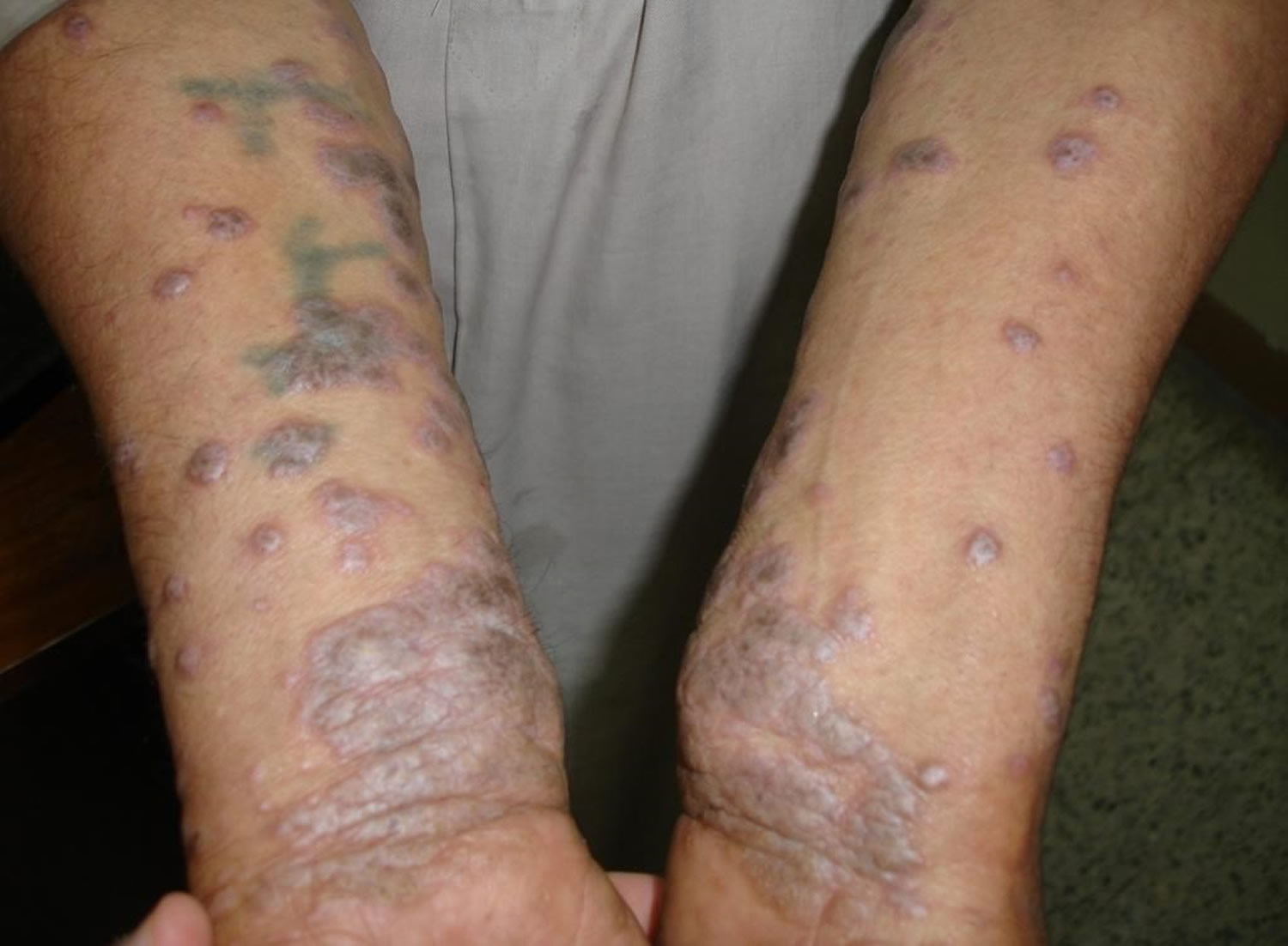
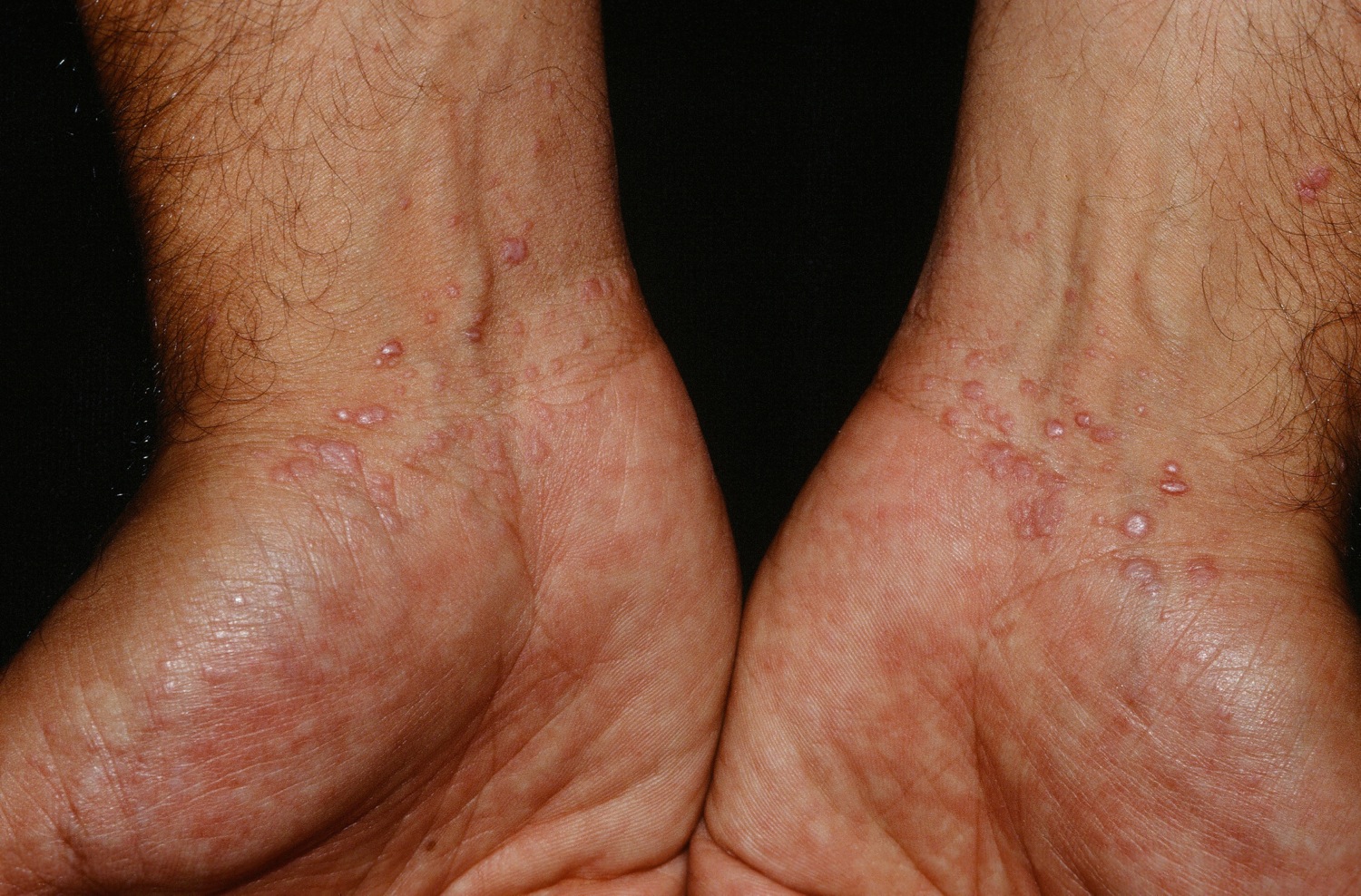
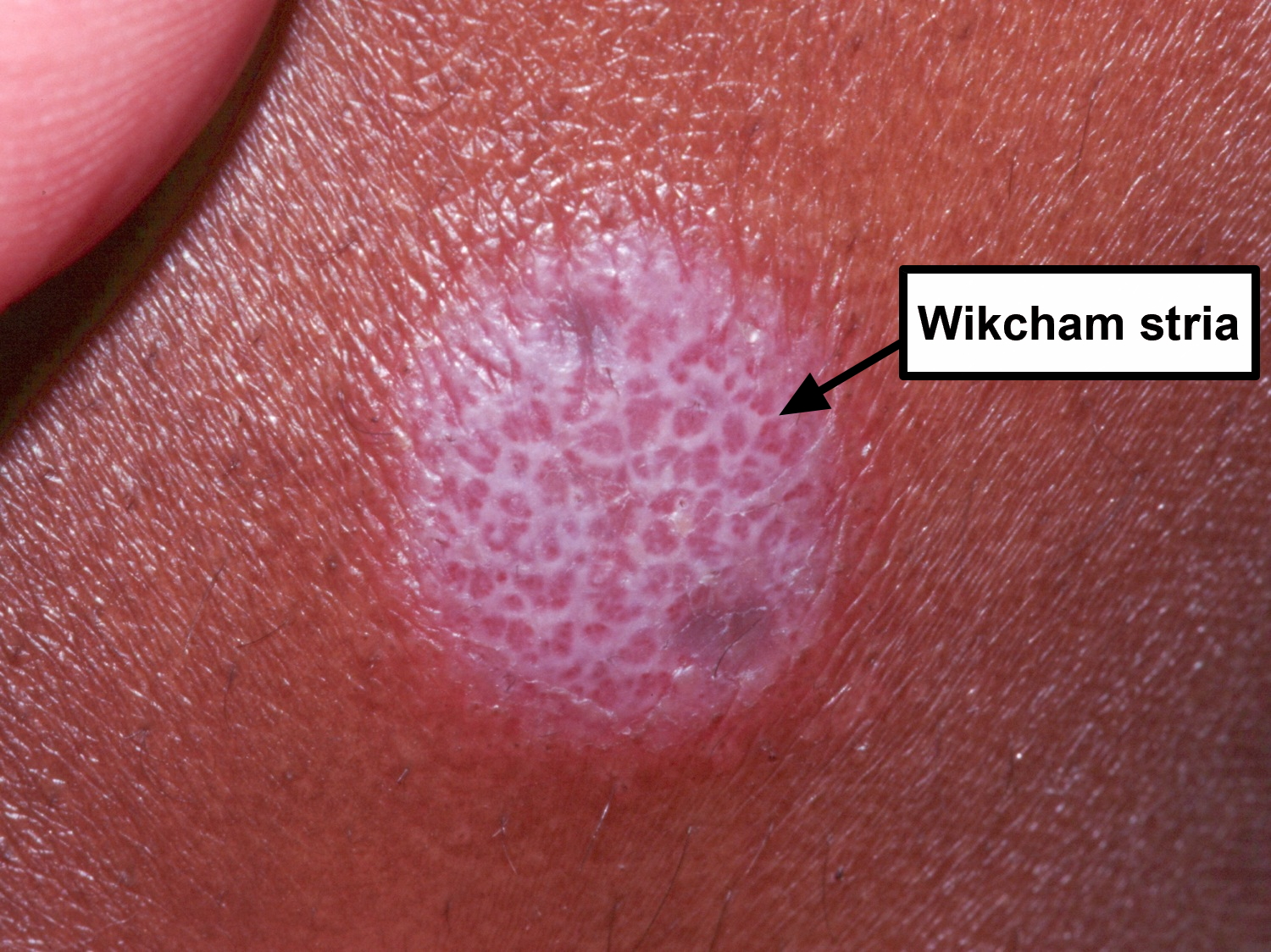
On the skin, the most common form of lichen planus presents with 3 to 5 mm diameter, itchy, purple, flat-topped spots (papules) which when looked at closely, have irregular fine white streaks visible on the surface called “Wickham’s striae”. The number of lesions can vary from a few to many, developing over several weeks. Lichen planus can join together to form lesions many centimeters in size called “plaques”. The areas typically affected are the fronts of the wrists, ankles and lower back although they can affect any part of the body surface. Skin trauma can promote formation of new lichen planus lesions. This is called “the Koebner phenomenon”. When the spots resolve they generally leave brown stains called post-inflammatory hyperpigmentation which take months to resolve.
In the mouth, vagina and other areas covered by a mucous membrane, lichen planus forms lacy white patches, sometimes with painful sores.
Figure 1. Lichen planus
Figure 2. Lichen planus with a white, reticulated pattern on the surface–classic Wickham’s stria
There are several clinical types of lichen planus that share similar features on histopathology. They can involve areas beyond the skin as listed below.
- Cutaneous lichen planus
- Erosive lichen planus (Mucosal lichen planus)
- Oral lichen planus
- Genital lichen planus
- Lichen planopilaris
- Lichen planus of the nails
- Lichen planus pigmentosus
- Lichenoid drug eruption
- Lichen planus scalp
- Actinic lichen planus
- Annular lichen planus
- Inverse lichen planus
- Bullous lichen planus
- Linear lichen planus
Annular lichen planus
Lichen planus papules form a ring with a central clearing, most commonly on the penis.
Inverse lichen planus
This form of lichen planus tends to occur in the groin, armpits and under the breasts.
Bullous lichen planus
This form of lichen planus is surmounted by blisters.
Linear lichen planus
Linear lichen planus occurs in straight lines, possibly due to trauma (Koebner phenomenon) or it may occur in isolation.
Most people can manage typical, mild cases of lichen planus at home, without medical care. If the condition causes pain or significant itching, you may need prescription drugs.
Treatment helps control lichen planus but does not cure it. Most cases are self-resolving over 1 to 2 years regardless of treatment. Even after the lichen planus has cleared, it leaves brown stains which can take many months to resolve. Oral, scalp and nail disease tends to be more persistent.
Drug induced lichen planus can take months to resolve after the medication causing the condition has been stopped.
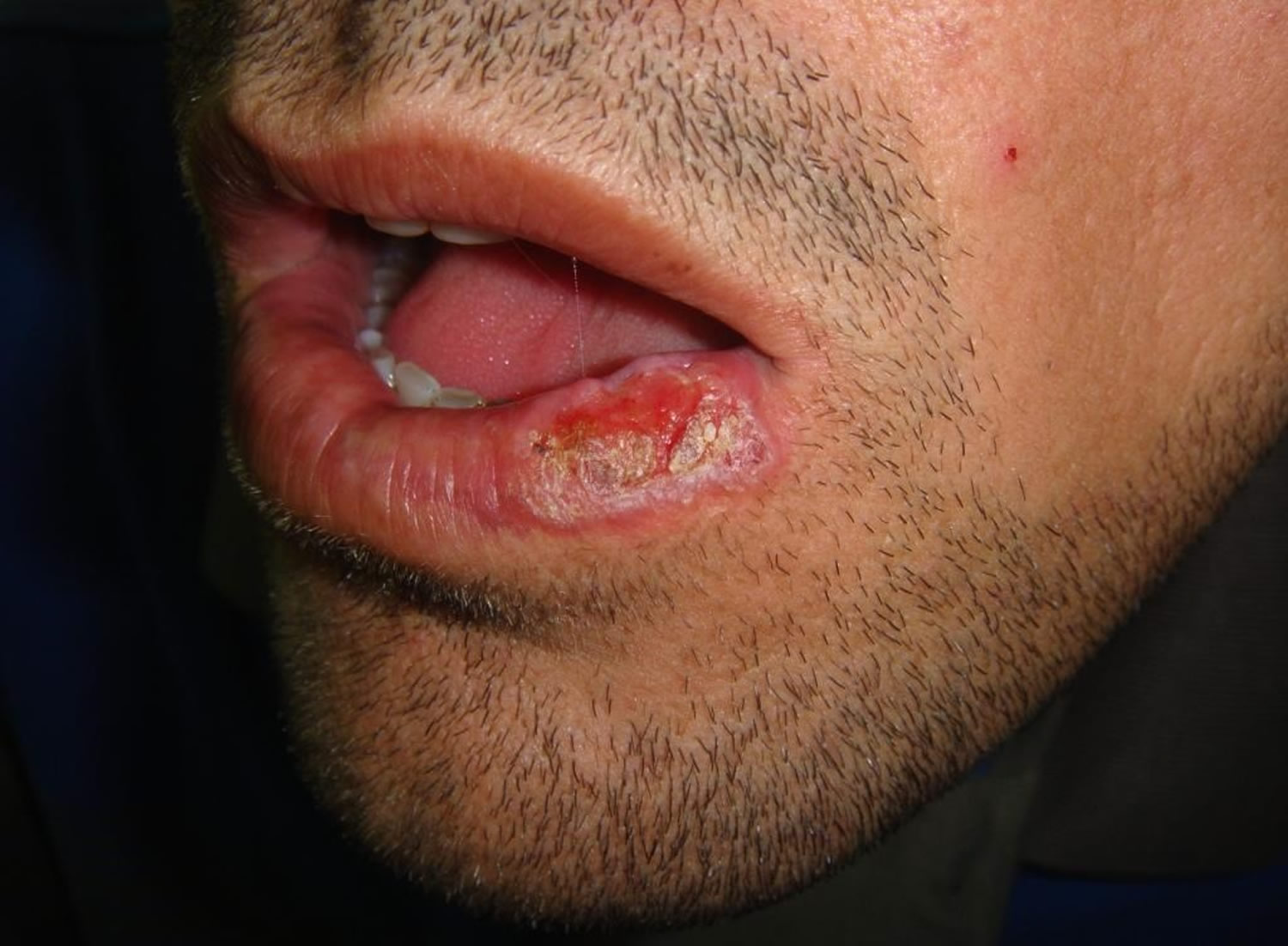
Erosive lichen planus
Erosive lichen planus is a painful, ulcerative form of lichen planus can affect the inside of the cheek, side of the tongue, gums and inside of the lips (oral lichen planus), vulva, vagina and penis (genital lichen planus). Erosive lichen planus rarely affects the eyelids, external ear canal, oesophagus, larynx, bladder and anus. Long standing erosive lichen planus can be complicated by squamous cell carcinoma.
A severe variant of erosive lichen planus in women is known as the vulvovaginal gingival syndrome. Ulceration occurs in the mouth and gums as well as on the vulva and in the vagina. Peno-gingival syndrome is the equivalent condition in men.
Erosive lichen planus is sometimes associated with classical cutaneous lichen planus or other forms of mucosal lichen planus. Erosive lichen planus causes painful and persistent ulcers. These heal with scarring.
Erosive lichen planus most often affects people in their 40s to 70s and is rare in children. It is at least twice as common in women than in men.
Erosive lichen planus is a destructive autoimmune disorder of unknown cause involving T lymphocytes .
- Occasionally, it is drug-induced, and will resolve on withdrawal of the responsible drug.
- Partial response to antifungal agents and antibiotics indicates an abnormal response to local microflora may be involved, especially Candida albicans.
- Cytokine expression profiling has found increased levels of the interleukins, IL 17 and IL 23.
Erosive lichen planus is not due to infection or allergy.
Erosive lichen planus complications
Squamous cell carcinoma
In about 1–3% of cases, longstanding erosive lichen planus can result in cancer (squamous cell carcinoma, SCC) of the mouth (oral cancer), vulva (vulval cancer) and penis (penile cancer). This should be suspected if there is an enlarging lump or an ulcer with thickened edges.
Some patients with erosive lichen planus have a particularly high risk of squamous cell carcinoma.
- Smokers
- Patients that are immune suppressed due to disease or drugs
- Patients infected with oncogenic types of human papilloma virus (HPV, see genital warts).
Scarring
Erosive lichen planus is a destructive disorder. Even when the inflammatory component has resolved, scarring may interfere with eating or sexual function.
Erosive lichen planus treatment
The management of erosive lichen planus may be very challenging. As it is a chronic complaint, topical and systemic treatment may be required intermittently or continuously, long-term.
General measures
For oral disease, it is important to practice good oral hygiene, and to have regular dental check-ups. Avoid foods that make the mouth sore.
The genitals should be gently washed using water alone or with a non-soap cleanser such as aqueous cream. A non-irritating emollient such as petrolatum may be applied as desired.
Ultrapotent topical steroids
Topical steroids generally applied daily for 4–6 week courses. They are the mainstay of therapy in most patients but maintenance treatment 1–3 times per week or more often may be necessary long term.
- In the mouth, topical steroids may be supplied as a paste, nasal spray (intended for rhinitis) or asthma-preventive puffer. These should be applied to the eroded areas two or three times daily.
- For genital erosions, ultrapotent steroid ointment (e.g., clobetasol proprionate) should be applied to the affected area as a thin smear once daily. Cream may be preferred, but is more likely to sting on application.
- Hydrocortisone foam can be used inside the vagina or anus.
Calcineurin inhibitors
Calcineurin inhibitors such as pimecrolimus cream or tacrolimus ointment have proven very effective for some patients with erosive lichen planus. These are applied once or twice daily for several weeks. Treatment may be repeated as required.
Mouthwashes containing ciclosporin or tacrolimus have been found to help oral disease.
Systemic steroids
Systemic steroids such as prednisone may be prescribed for a few weeks or longer, usually at a dose of 0.5–1 mg/kg/day. Once the erosions have healed, the dose is tailed off. Longterm use of systemic steroids may have serious side effects. In many patients, calcium and vitamin D should also be prescribe to reduce the chance of corticosteroid-induced bone thinning.
Methotrexate
Methotrexate is taken in a dose of 10–20mg once weekly. Folic acid is often added to reduce the chance of potential adverse effects. This may be very effective for erosive lichen planus, with improvement or healing occurring within one to three months. It may be continued long term if required. Blood count, liver function and procollagen levels should be monitored. Alcohol intake should be minimized. It must not be taken during pregnancy.
Other oral treatments
Other drugs that sometimes help include:
- Antibiotics
- Oral antifungal agents
- Acitretin
- Hydroxychloroquine
- Azathioprine
- Thalidomide
Surgery
Surgical release of vulval and vaginal adhesions and scarring from lichen planus may occasionally be performed to reduce urination difficulties and allow intercourse. Procedures may include:
- Simple perineotomy (division of adhesions)
- Fenton procedure (an incision that is repaired transversely)
- Perineoplasty (excision of involved tissue and vaginal mucosal advancement)
Lichen planus vulva
Lichen planus may affect labia majora, labia minora and vaginal introitus. Presentation includes:
- Painless white streaks in a lacy or fern-like pattern
- Painful and persistent erosions and ulcers (erosive lichen planus )
- Scarring, resulting in adhesions, resorption of labia minora and introital stenosis
- Painful desquamative vaginitis, preventing intercourse, and causing a mucky discharge. The eroded vagina may bleed easily on contact
- Overlap with vulval lichen sclerosus, an inflammatory skin disorder that most commonly affects women over 50 years of age.
Rarely, squamous cell carcinoma may arise in vulval lichen planus. In one study 1, 1/3 occurred in erosive lichen planus and 2/3 in non-erosive. All squamous cell carcinoma were located in non-hair bearing vulvar mucosa, most common between the clitoris and the urethra. These cancers are aggressive malignancies with disease-related death in over 30% within the first 1-3 years. Given the risk of vulvar squamous cell carcinoma, any woman with vulvar lichen planus needs close follow-up.
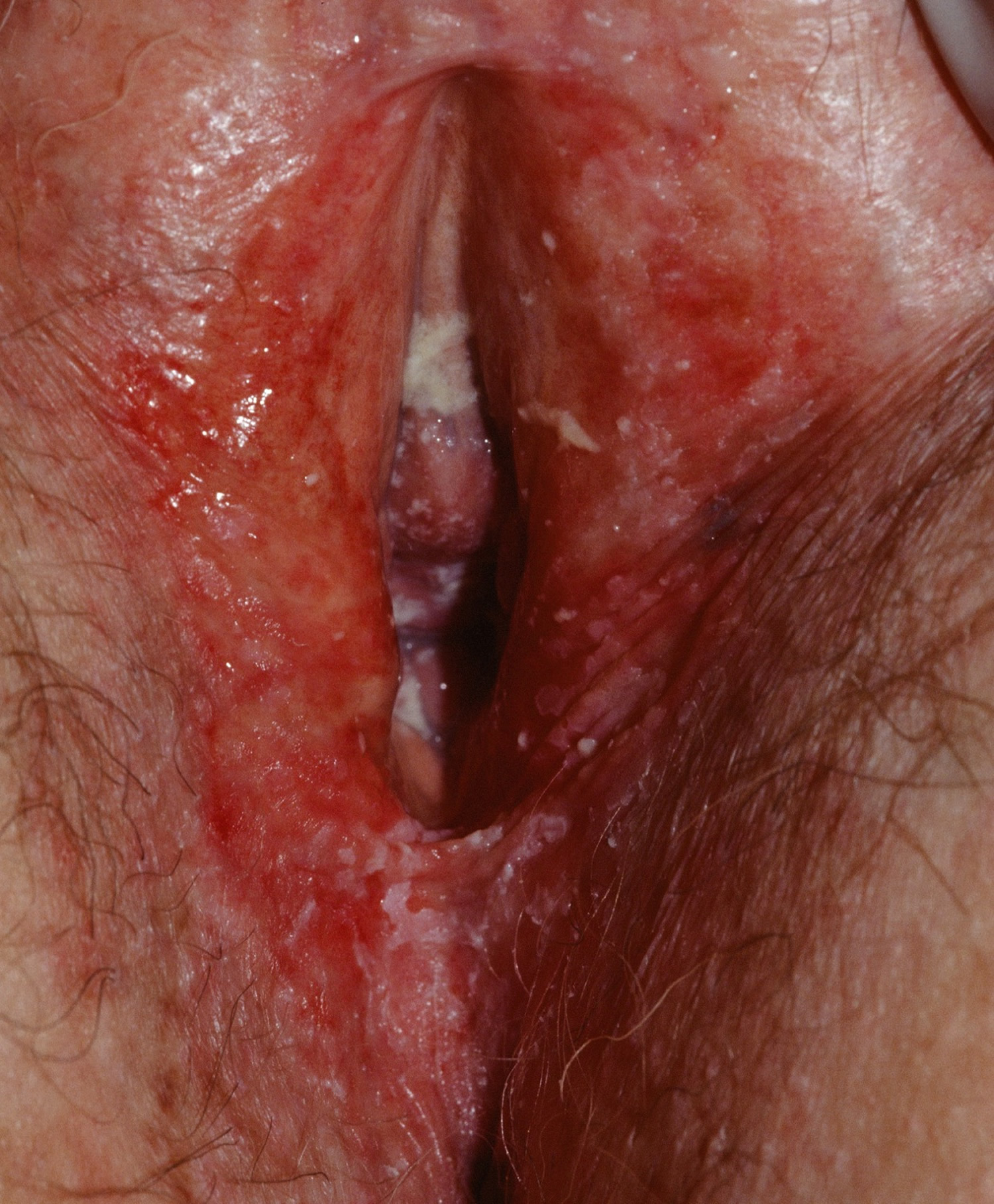
Genital erosive lichen planus
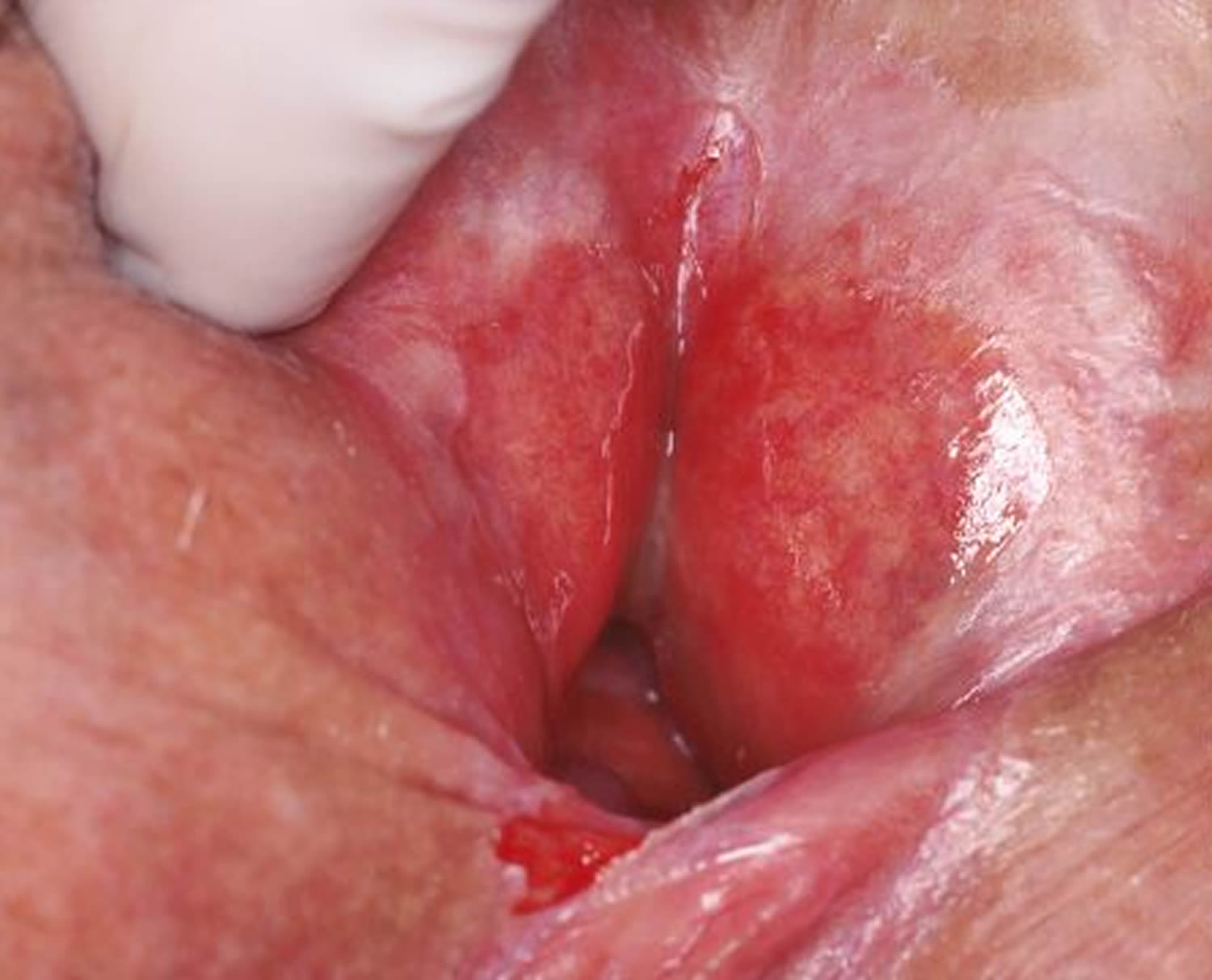
In women, erosive lichen planus affects the labia minora (inner lips) and introitus (entrance to the vagina). The affected mucosa is bright red and raw. Erosive lichen planus can be very painful, stinging when passing urine and preventing sexual intercourse. It is one cause of vulvodynia (burning discomfort of the vulva). Erosive lichen planus may also result in very severe itch.
The clitoral hood may disappear, and the labia minora can shrink and stick to each other or to the labia majora (the outer lips). It can also scar, closing over the vagina.
Sometimes erosive lichen planus affects deep within the vagina where it causes inflammation and superficial ulceration (desquamative vaginitis). The surface cells in the vagina peel off and cause a mucky discharge. The eroded vagina may bleed easily on contact.
Erosive lichen planus in men affects the end of the penis (the glans), which becomes red, raw and tender.
Figure 3. Lichen planus vulva (erosive lichen planus)
Erosive vulvar lichen planus treatment
- Topical steroid ointments
- Topical tacrolimus
- Hydroxychloroquine
- Rituximab
- Cyclosporin, topical or oral
- Tacrolimus, topical or oral
- Photodynamic therapy
A strong topical steroid ointment may be tried initially. If this fails, topical tacrolimus may be tried, as tacrolimus 0.1% ointment applied twice daily has been very effective in several studies. Systemic tacrolimus has been used 2.
Other options include intralesional kenalog (e.g. 10 mg/cc) for localized areas. Systemic steroids are almost always effective but cannot be continued long term because of side effects. Oral hydroxychloroquine may be very effective. An oral and a vaginal prosthesis allowing occlusion of a class II topical steroid has been used effectively. Cyclosporin topically three times daily (1:1 ratio oral cyclosporin and olive oil in a gauze applied for 10-15 minutes) was effective in one patient 3. Systemic cyclosporin (e.g. 1-2 mg/kg/day) was very effective in 2 patients 4. Adalimumab has been used 5.
Vulvovaginal hexyl 5-aminolevulinate-hydrocloride photodynamic therapy seems to be an effective and safe treatment for erosive vulvar lichen planus 6. In this study of 40 women, there was similar benefit with one session with vulvovaginal hexyl 5-aminolevulinate-hydrocloride photodynamic therapy compared with daily application of topical clobetasol for 6 weeks.
Rituximab
Two women with intractable vulvovaginal lichen planus cleared within 4 weeks with rituximab 7.
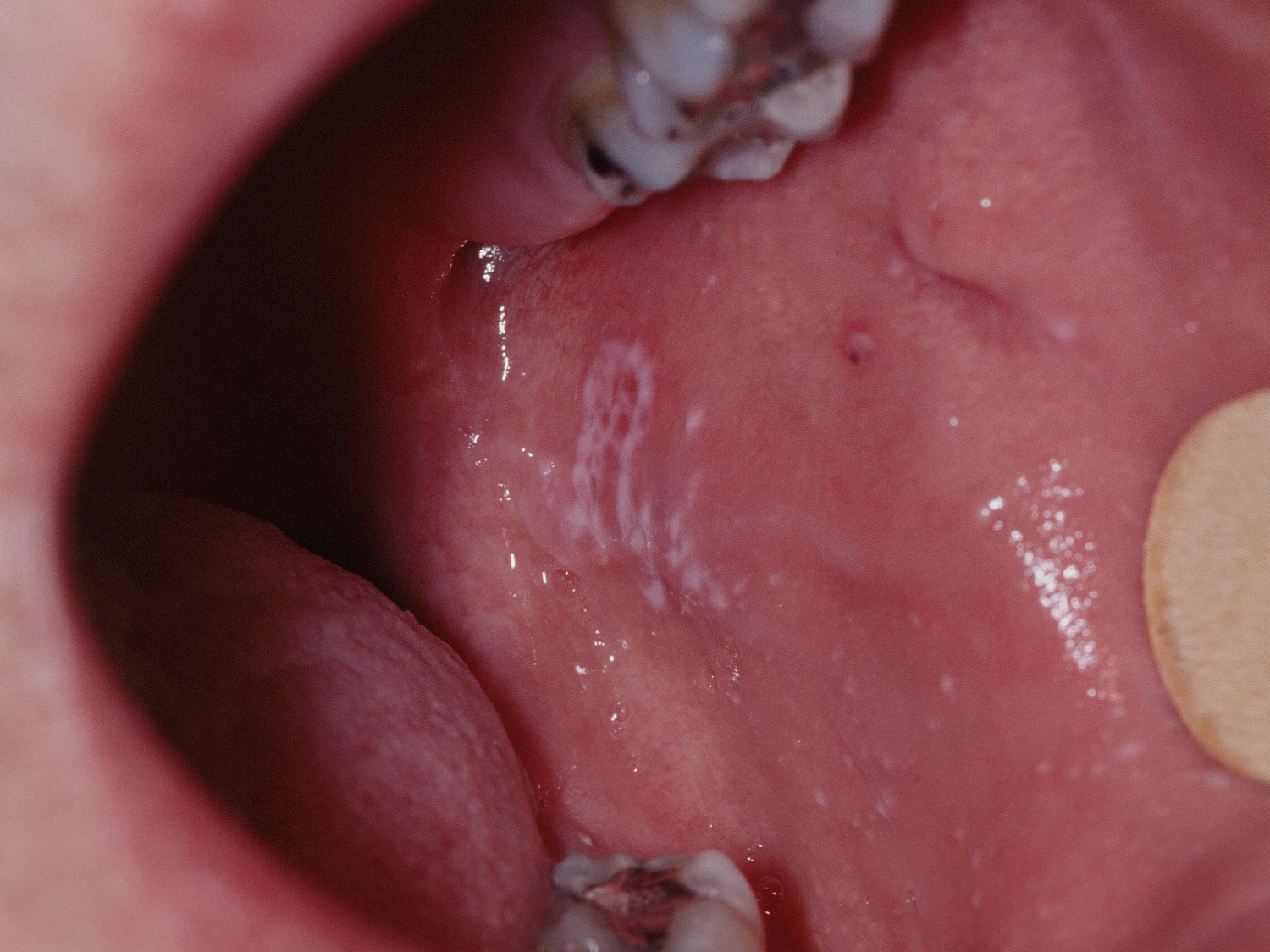
Oral lichen planus
Oral lesions occur in 50% of those with cutaneous lichen planus. In some cases, it is the only site of involvement. Oral lesions typically appear as lace-like white streaks on the inside of the cheeks (reticular pattern) but they can also affect the side of the tongue, gums and lips. An erosive form of oral lichen planus results in pain and ulceration which may lead to scarring. Some oral lesions may result from sensitivity to dental restorative materials or toothpaste. Oral lichen planus is a risk factor for oral squamous cell carcinoma, particularly the ulcerative type. In rare cases, it can involve other mucosal sites such as the eyes, nasal mucosa, larynx, esophagus and anus.
Oral lichen planus can be very painful and ulceration may lead to scarring. Sometimes eating is so uncomfortable that affected person is unable to maintain adequate nutrition.
Lichen planus, particularly the erosive form, may rarely lead to oral cancer (squamous cell carcinoma). Persistent ulcers and enlarging nodules should undergo biopsy.
The prognosis for oral lichen planus is uncertain. It can clear up within a few months or persist (with or without treatment) for decades. There are often periods of remission and relapse.
The mouth is often the only affected area. Oral lichen planus often involves the inside of the cheeks and the sides of the tongue, but the gums and lips may also be involved. The most common patterns are:
- Painless white streaks in a lacy or fern-like pattern
- Painful and persistent erosions and ulcers (erosive lichen planus)
- Diffuse redness and peeling of the gums (desquamative gingivitis)
- Localised inflammation of the gums adjacent to amalgam fillings
The precise cause of oral lichen planus is not fully understood. It involves cytotoxic CD8+ T lymphocytes and pro-inflammatory cytokines, which attack the oral epithelial cells — resulting in their death. The immune response is mediated by antigen-specific cells.
In most cases oral lichen planus is idiopathic, when the reaction is thought to be against autoantigens. In other cases, it may be precipitated by exogenous antigens described below.
- Drugs — this is called oral lichenoid drug reaction. It is most often due to gold therapy. Other medications include some antibiotics, nonsteroidal anti-inflammatory drugs, antimalarials, drugs used for treating hypertension and heart disease, and antiretroviral medicines. These drugs more commonly cause a lichenoid skin eruption, with the mouth being affected less often.
- Contact allergens in dental restorative materials (mercury, nickel, gold, resins, acrylates) or toothpaste, particularly spearmint. These may be identified by careful patch testing.
- Viral infection, particularly Hepatitis C
Oral lichenoid lesions are also part of the spectrum of chronic graft-versus-host disease that occurs after bone marrow transplantation.
Figure 4. Oral lichen planus
Oral lichen planus treatment
It is important to identify and remove or avoid any potential agent that might have caused a lichenoid reaction, such as drugs that have been started in recent months and contact allergens identified by patch testing.
Most people get satisfactory control of symptoms with the following measures.
- Meticulous oral hygiene: brushing teeth and gums, regular visits to dentist, once-weekly mouthwash with diluted chlorhexidine
- If standard toothpaste irritates, try products that do not contain sodium lauryl sulfate
- Stop smoking
- Topical chamomile gel
- Topical retinoid, for example tretinoin or isotretinoin gel
- Topical steroids as drops, pastes, gels or sprays, for example, triamcinolone in an emollient dental paste, fluticasone nasal preparations, and clobetasol propionate in various forms.
- Steroid injections (intralesional triamcinolone)
- Mouth rinse containing a calcineurin inhibitor: ciclosporin or tacrolimus
In severe cases systemic corticosteroids may be used.
Other possible therapeutic agents may include:
- Thalidomide
- Systemic retinoids (acitretin or isotretinoin)
- Griseofulvin
- Azathioprine
- Cyclophosphamide
- Methotrexate
- Dapsone
- Metronidazole
- Low molecular weight heparin.
Targeted molecular medicines are under investigation for the treatment or recalcitrant disease, with apremilast reported effective in a few patients.
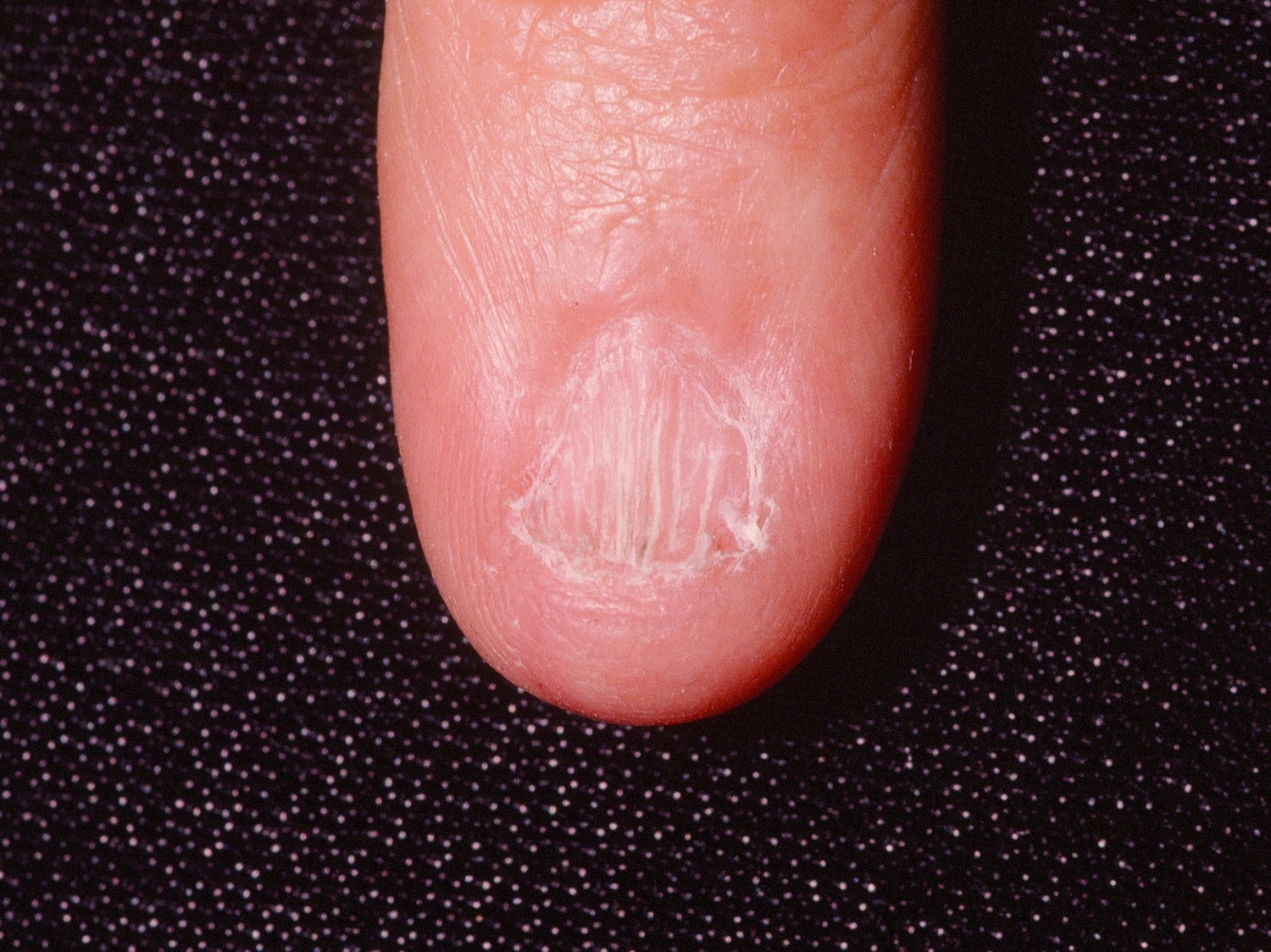
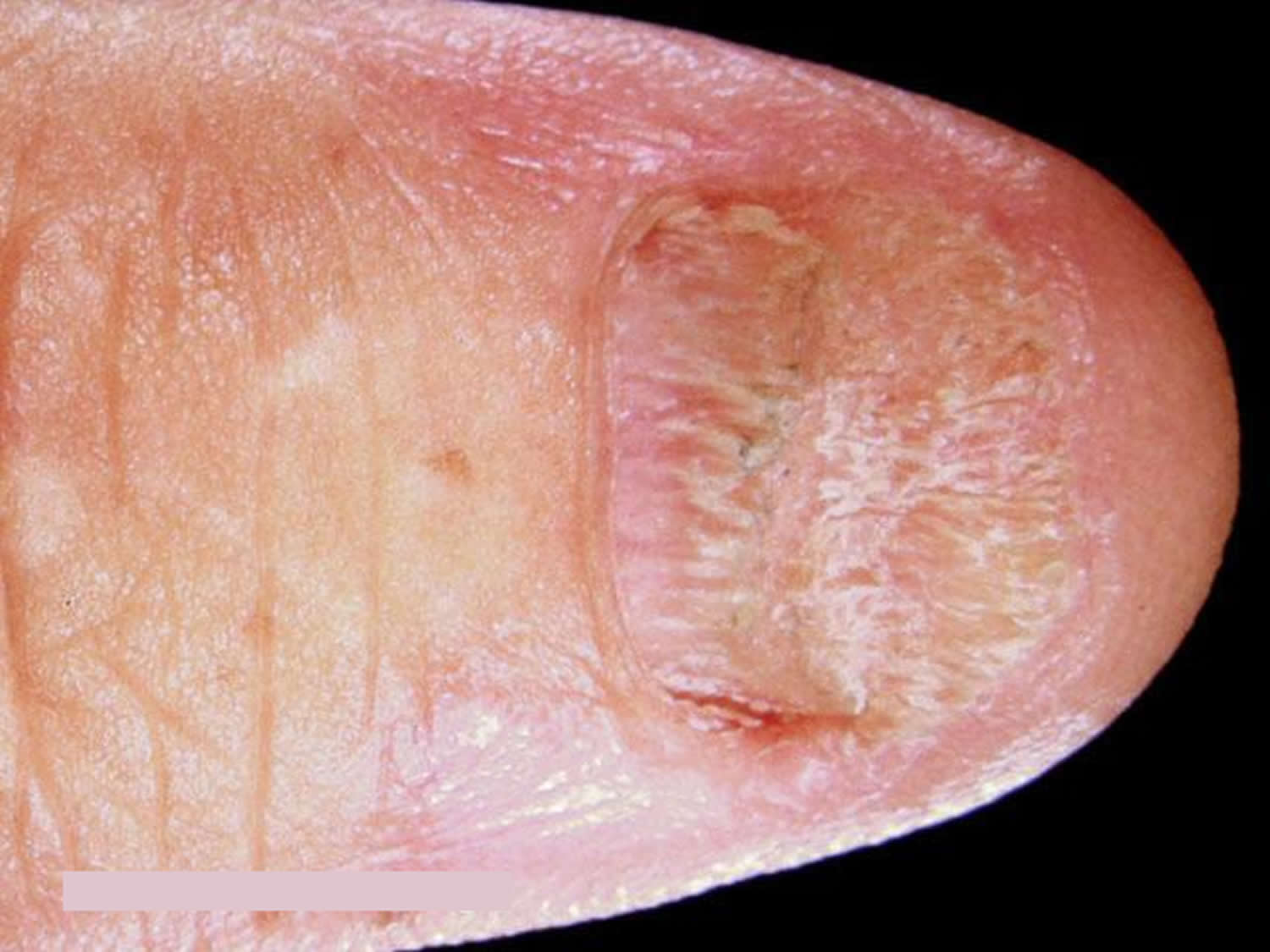
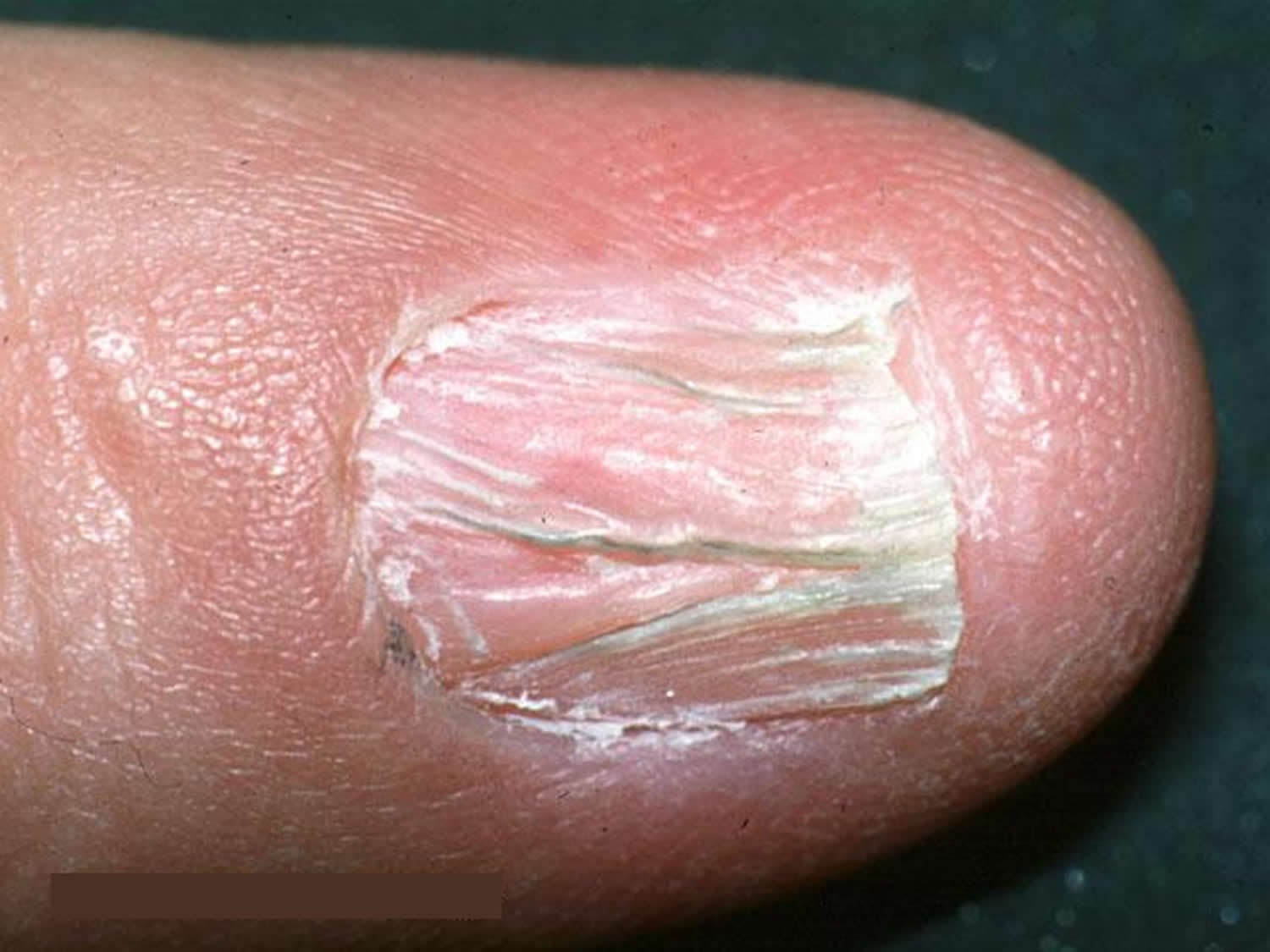
Lichen planus nails
Lichen planus affects one or more nails, sometimes without involving the skin surface. It is called twenty-nail dystrophy if all nails are abnormal and nowhere else is affected. Nail changes such as longitudinal grooves, ridges, nail plate thinning, thickening, roughness, nail lifting off the nail bed (onycholysis), nail loss (temporary or permanent) and nail bed scarring (pterygium) occur in 10% of those with skin lesions.
Lichen planus nails may shed or stop growing altogether, and they may rarely, completely disappear (anonychia).
Figure 5. Lichen planus nails
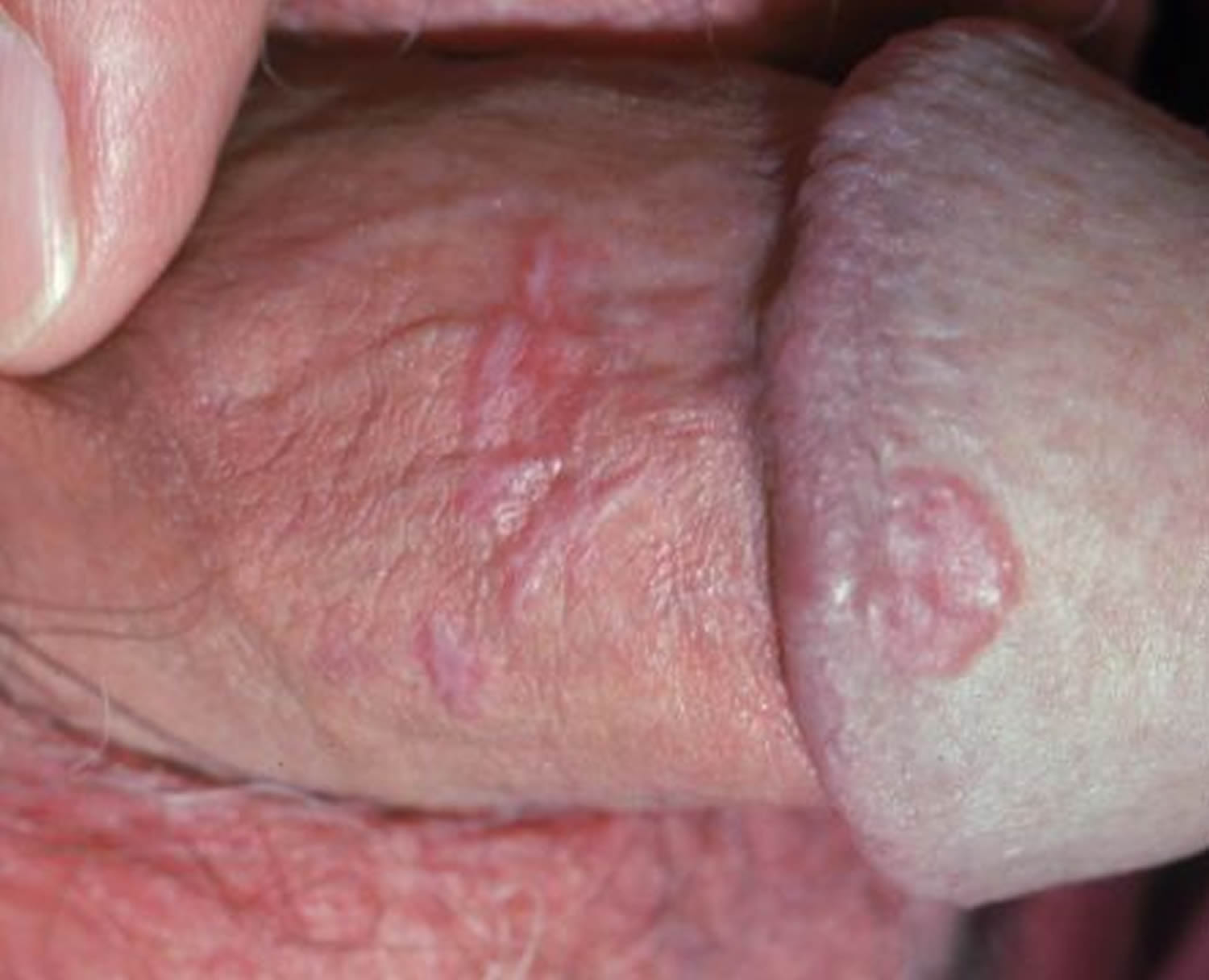
Genital lichen planus
Lesions can involve the glans penis in men and the vulva and vagina in women. Open sores called erosions can develop at these sites sometimes leading to ulceration, pain and scarring.
Penile lichen planus usually presents with classical papules in a ring around the glans. White streaks and erosive lichen planus may occur but are less common.
Figure 6. Genital lichen planus
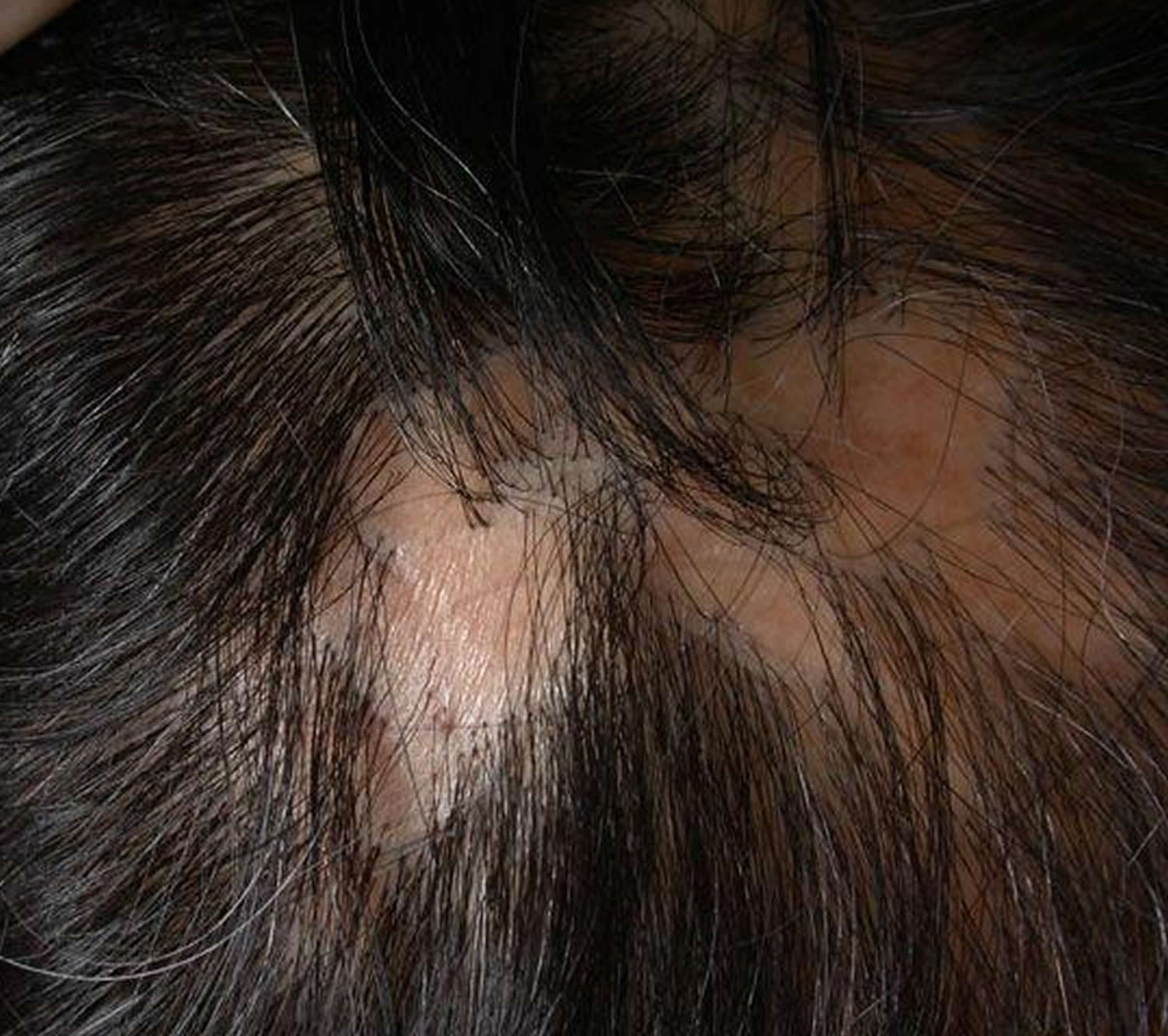
Lichen planus scalp
Lichen planus of the scalp and hair follicles can lead to permanent hair loss.
Lichen planopilaris presents as tiny red spiny follicular papules on the scalp or less often, elsewhere on the body. Rarely, blistering occurs in the lesions. Destruction of the hair follicles leads to permanently bald patches characterised by sparse “lonely hairs”.
Frontal fibrosing alopecia is a form of lichen planopilaris that affects the anterior scalp, forehead and eyebrows.
Pseudopelade of Brocq is probably a variant of lichen planus without inflammation or scaling. Areas of scarring without hair slowly appear, described as “like footprints in the snow”.
Figure 7. Lichen planus scalp
Lichen planus pigmentosus
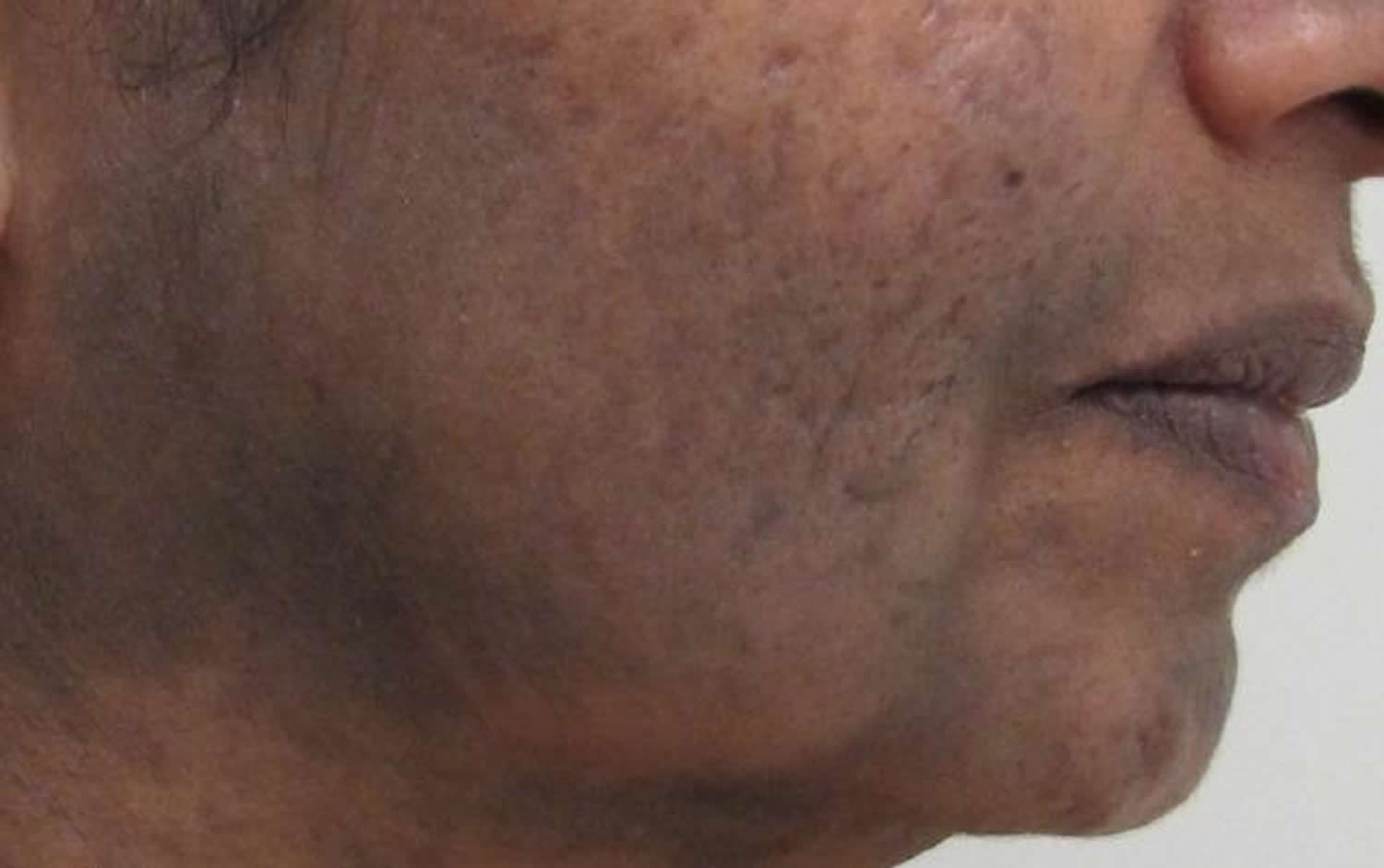
Lichen planus pigmentosus also called actinic lichen planus, describes ill-defined oval, greyish brown marks on the face and neck or trunk and limbs without an inflammatory phase. Lichen planus pigmentosus is most common in middle-aged individuals with darker skin. This form of lichen planus is seen more commonly in the Middle East, India and East Africa. Brown patches with a surrounding white halo typically occur on the face, neck and upper limbs with some cases showing a tendency to affect the armpits. It can be provoked by sun exposure but can also arise in sun-protected sites such as the armpits. It has diffuse, reticulate and diffuse patterns. Lichen planus pigmentosus is similar to erythema dyschromicum perstans and may be the same disease.
Lichen planus pigmentosus may rarely affect the lips, resulting in a patchy dark pigmentation on upper and lower lips.
Figure 8. Lichen planus pigmentosus
Lichen planus pigmentosus treatment
Sun avoidance and sunscreen should be recommended in cases where the pigmentation is sun-related, e.g., of the head and neck. Initial therapy should be directed at controlling the inflammation, thus allowing the pigmentation to fade. Any therapy that ignores the inflammatory component (e.g., laser alone, hydroquinone alone) is destined to fail. Since the darker skin and pigmentation can obscure the true amount of inflammation present, periodic biopsies can aid in assessing response to treatment. Sunscreen, oral hydroxychloroquine, and topical tacrolimus may be given for 2-3 months. If they fail to suppress the inflammation, cyclosporin may be considered. Once the inflammation has been suppressed, topical hydroquinone and/or laser therapy may be considered 8.
What are the clinical features of lichen planus?
Lichen planus may cause a small number or many lesions on the skin and/or mucosal surfaces.
Cutaneous lichen planus
The usual presentation of the disease is classical lichen planus. Symptoms can range from none (uncommon) to intense itch.
- Papules and polygonal plaques are shiny, flat-topped and firm on palpation.
- The plaques are crossed by fine white lines called Wickham stria.
- Hypertrophic lichen planus can be scaly.
- Bullous lichen planus is rare.
- Size ranges from pinpoint to larger than a centimeter.
- Distribution may be scattered, clustered, linear, annular or actinic (sun-exposed sites such as face, neck and backs of the hands).
- Location can be anywhere, but most often front of the wrists, lower back, and ankles.
- Color depends on the patient’s skin type. New papules and plaques often have a purple or violet hue, except on palms and soles where they are yellowish brown.
- Plaques resolve after some months to leave greyish-brown post-inflammatory macules that can take a year or longer to fade.
Lichen planus outlook (prognosis)
Lichen planus is usually not harmful. Most often it gets better with treatment. The condition often clears up within 18 months, but may come and go for years.
If lichen planus is caused by a medicine you are taking, the rash should go away once you stop the medicine.
Lichen planus possible complications
Mouth ulcers that are present for a long time may develop into oral cancer.
There is some evidence that lichen planus may increase your risk of a skin cancer known as squamous cell carcinoma, though the risk is small. Your doctor may recommend routine screening for evidence of cancerous cells in tissues affected by lichen planus.
Lichen planus can be difficult to manage on the vulva and in the vagina, causing severe pain and sometimes leaving scars. Sexual dysfunction can become a long-term complication.
For many people the affected skin might stay slightly darker even after the rash clears up.
Lichen planus causes
The cause of lichen planus is unknown but is thought to be due to an allergic or an abnormal T cell-mediated autoimmune disease. Lichen planus is believed to occur when your immune system mistakenly attacks an unknown protein within skin and mucosal keratinocytes. No one knows the exact cause of this abnormal immune response. The condition isn’t contagious.
Lichen planus occurs more frequently in those who are infected with hepatitis C; however, most people with lichen planus do not have hepatitis C.
Other rarer medical conditions that may be associated with lichen planus include: viruses such as human herpes virus 6 or 7 (HHV-6 or -7), herpes simplex virus (HSV), varicella zoster virus (VZV); bacteria such as the helicobacter pilori that can affect the stomach; vaccines and contact allergens such as amalgam teeth fillings; or other metals such as gold or copper.
A similar skin condition can be triggered by certain medications such as diuretics, ACE inhibitors, beta blockers, non steroidal anti-inflammatories, antimalarials and gold. The time interval from medication exposure to the appearance of the condition can vary from months to more than a year.
Risks factors for lichen planus
Risk factors for triggering lichen planus include:
- Middle aged adults (adults over the age of 40 years)
- Genetic predisposition
- Physical and emotional stress
- Injury to the skin; lichen planus often appears where the skin has been scratched—isomorphic response (koebnerisation)
- Localized skin disease such as herpes zoster—isotopic response
- Exposure to certain medicines, dyes, and other chemicals (including gold, antibiotics, arsenic, iodides, chloroquine, quinacrine, quinidine, phenothiazines, and diuretics)
- Systemic viral infection, such as hepatitis C (which might modify self-antigens on the surface of basal keratinocytes)
- Flu vaccine
- Nonsteroidal anti-inflammatory drugs (NSAIDs), such as ibuprofen (Advil, Motrin IB, others) and naproxen (Aleve, others)
- Contact allergy, such as to metal fillings in oral lichen planus (rare)
- People who take certain medications may develop a rash that looks like lichen planus (drug-induced lichen planus). These medications include:
- High blood pressure (hypertension) medicines, including diuretics, ACE inhibitors, and calcium channel blockers
- Diabetes medications, including the sulfonylureas
- Ibuprofen or naproxen
- Antimalarial medications
- Gold
- Penicillamine
- Ketoconazole
A lichenoid inflammation is also notable in graft-versus-host disease, a complication of bone marrow transplant.
Lichen planus symptoms
The signs and symptoms of lichen planus vary depending on the areas affected.
Mouth sores are one symptom of lichen planus. They:
- May be tender or painful (mild cases may not cause pain)
- Are located on the sides of the tongue, inside of the cheek, or on the gums
- Look like bluish-white spots or pimples
- Lacy white patches in the mouth — inside the cheeks or on the gums, lips or tongue
- Gradually increase in size
- Sometimes form painful ulcers
Skin sores are another symptom of lichen planus. They:
- Usually appear on the inner wrist, legs, torso, or genitals
- Painful oral or vaginal ulcers
- Are itchy
- Have even sides (symmetrical) and sharp borders
- Occur alone or in clusters, often at the site of a skin injury
- May be covered with thin white streaks or scratch marks
- Are shiny or scaly looking
- Have a dark, violet color
- May develop blisters or ulcers
Other symptoms of lichen planus are:
- Dry mouth
- Hair loss and scalp discoloration
- Metallic taste in the mouth
- Ridges in the nails
- Nail damage or loss
- Purplish, flat-topped bumps, most often on the inner forearm, wrist or ankle, but sometimes on the external genitals
- Blisters that may break to form scabs or crusts
Lichen planus diagnosis
Your health care provider may make the diagnosis based on the appearance of your skin or mouth lesions. However, a small sample of skin (skin biopsy) may be necessary in some cases to confirm the diagnosis.
Patients with chronic liver disease (e.g. primary biliary cirrhosis, chronic active hepatitis) have twice the risk of developing lichen planus compared with the general population. Some of these patients are infected with Hepatitis B and some with Hepatitis C virus. Lichen planus has developed after Hepatitis B vaccination and in association with hepatocellular carcinoma (liver cancer).
In a recent meta study, lichen planus was significantly associated with an increased risk of dyslipidemia and higher triglyceride levels 9.
And, if necessary, the results of lab tests. These tests may include:
- Hepatitis B and C test. You may have your blood drawn to test for hepatitis B and hepatitis C, which is a possible trigger for lichen planus.
- Liver function test
- Blood lipid profile
- Allergy tests. Your doctor may refer you to an allergy specialist (allergist) or dermatologist for skin patch testing to identify agents to which you may be allergic and that may act as triggers for your condition.
Other tests may be needed if your doctor suspects you have any of the several variations of lichen planus, such as the type that affects the esophagus, genitals, ears or mouth.
Lichen planus treatment
Lichen planus on the skin often clears up on its own in a couple years or less. If the disease affects your mucous membranes, it tends to be more resistant to treatment and prone to recur.
Medications and other treatments might help relieve itching, reduce discomfort and promote healing. Talk with your doctor to weigh the potential benefits against possible side effects of treatment.
How to get rid of lichen planus
Mild cases may require no treatment.
Lichen planus treatments may include:
- Antihistamines
- Medicines that calm down the immune system (in severe cases)
- Lidocaine mouthwashes to numb the area and make eating more comfortable (for mouth sores)
- Topical corticosteroids or oral corticosteroids to reduce swelling and lower immune responses
- Corticosteroid shots into a sore
- Vitamin A as a cream or taken by mouth
- Other medicines that are applied to the skin
- Dressings placed over your skin with medicines to keep you from scratching
- Ultraviolet light therapy
Corticosteroids
The first choice for treatment of lichen planus is usually a prescription corticosteroid cream or ointment, to help reduce inflammation. They should be used as directed by your dermatologist as incorrect use can cause side effects. Creams should be applied to the itchy red/purple spots rather than the brown stains. If that doesn’t help and your condition is severe or widespread, your doctor might suggest a corticosteroid pill, either alone or with the cream or ointment. If you still don’t see improvement, your doctor might suggest a corticosteroid injection. Intralesional corticosteroids may be used for thick and stubborn lesions.
Common side effects of topical corticosteroids include skin irritation or thinning where the cream is applied, oral thrush and upset stomach. Short term use of oral corticosteroids over a 6 week period may be used when lichen planus affects many areas of the body or oral lichen planus. Corticosteroids are considered safe when taken as directed and for short-term use.
Immune response medicines
Medications that suppress or modify your body’s immune response may be used as ointments, gels or oral medication. For example, topical calcineurin inhibitors can be particularly helpful in managing lichen planus of mucous membranes. Examples include tacrolimus (Protopic) and pimecrolimus (Elidel).
Antihistamines
Antihistamines act against a protein called histamine that is involved in inflammation. An oral or topical antihistamine may relieve itching or pain associated with lichen planus.
Light therapy
Light therapy (phototherapy) may help clear up lichen planus affecting the skin. The most common phototherapy for lichen planus uses ultraviolet B (UVB) light, which penetrates only the upper layer of skin (epidermis).
There is some risk of “sunburn” with this treatment. Phototherapy using ultraviolet A (UVA) light in combination with the medication psoralen also may be effective, though it carries a small long-term risk of skin cancer and cataracts.
Light therapy usually requires two to three treatments a week for several weeks.
Retinoids
If your condition doesn’t respond to corticosteroids or light therapy, your doctor might prescribe a retinoid (acitretin). Retinoids are synthetic versions of vitamin A that can be applied to the skin or taken by mouth. Retinoid lotion may be an effective treatment, but it can irritate the skin, causing dryness, redness and peeling.
Retinoids can cause birth defects, so these drugs aren’t recommended for women who are pregnant or may become pregnant. If you’re pregnant or nursing, your doctor may opt to delay topical retinoid therapy or choose a different treatment.
Other medicines
Oral medications such as hydroxychloroquine, methotrexate, cyclosporin and mycophenolate mofetil are sometimes used in particular cases.
Dealing with triggers
If your doctor suspects that your lichen planus is related to hepatitis C infection, an allergen or a drug you take, he or she will recommend steps to address the trigger. For example, you may need to switch medications or avoid offending allergens. Your doctor may refer you to an allergist or, in the case of a hepatitis C infection, a specialist in liver disease (hepatologist) for further treatment.
Home remedies
Self-care measures can help reduce the itching and discomfort caused by lichen planus. These include:
- Tub soaks with colloidal oatmeal (Aveeno, others), followed by moisturizing lotion
- Cool compresses
- Over-the-counter hydrocortisone cream or ointment, containing at least 1 percent hydrocortisone (if you’re not using a prescription topical corticosteroid)
- Not scratching
For oral lichen planus, good oral hygiene and regular dentist visits are important. You can help reduce the pain of mouth sores by avoiding:
- Smoking
- Drinking alcohol
- Consuming spicy or acidic food and drink
Alternative medicine
A number of small studies indicate the possible benefit of vitamins A and B in treating lichen planus of the skin, but further research is needed.
A couple of small clinical trials have suggested the benefit of aloe vera gel for treating lichen planus of the mouth and vulva.
Talk with your doctor before trying an alternative treatment for lichen planus. Some alternative medicines or vitamin supplements result in serious adverse reactions when combined with prescription medicines.