Contents
What is metatarsalgia
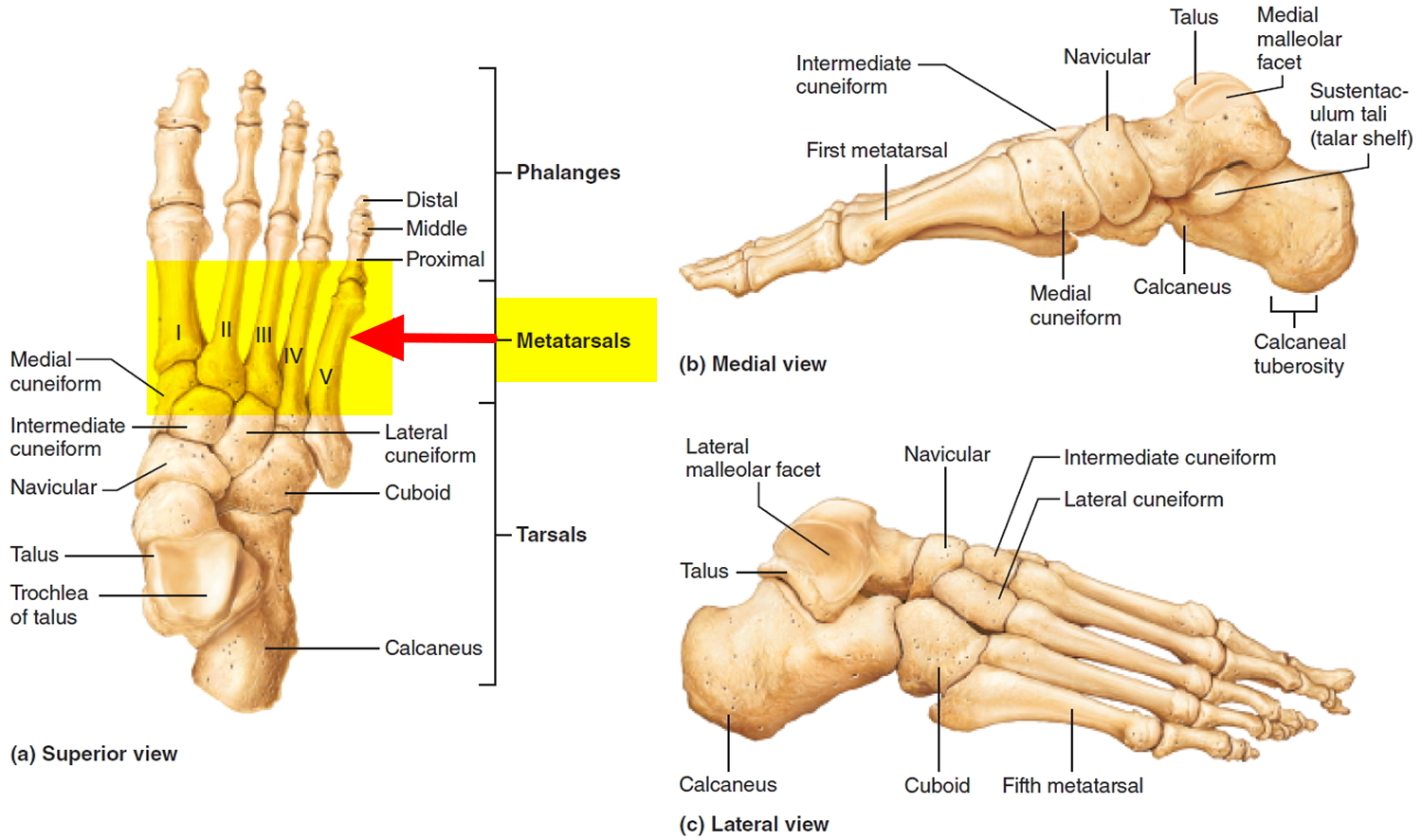
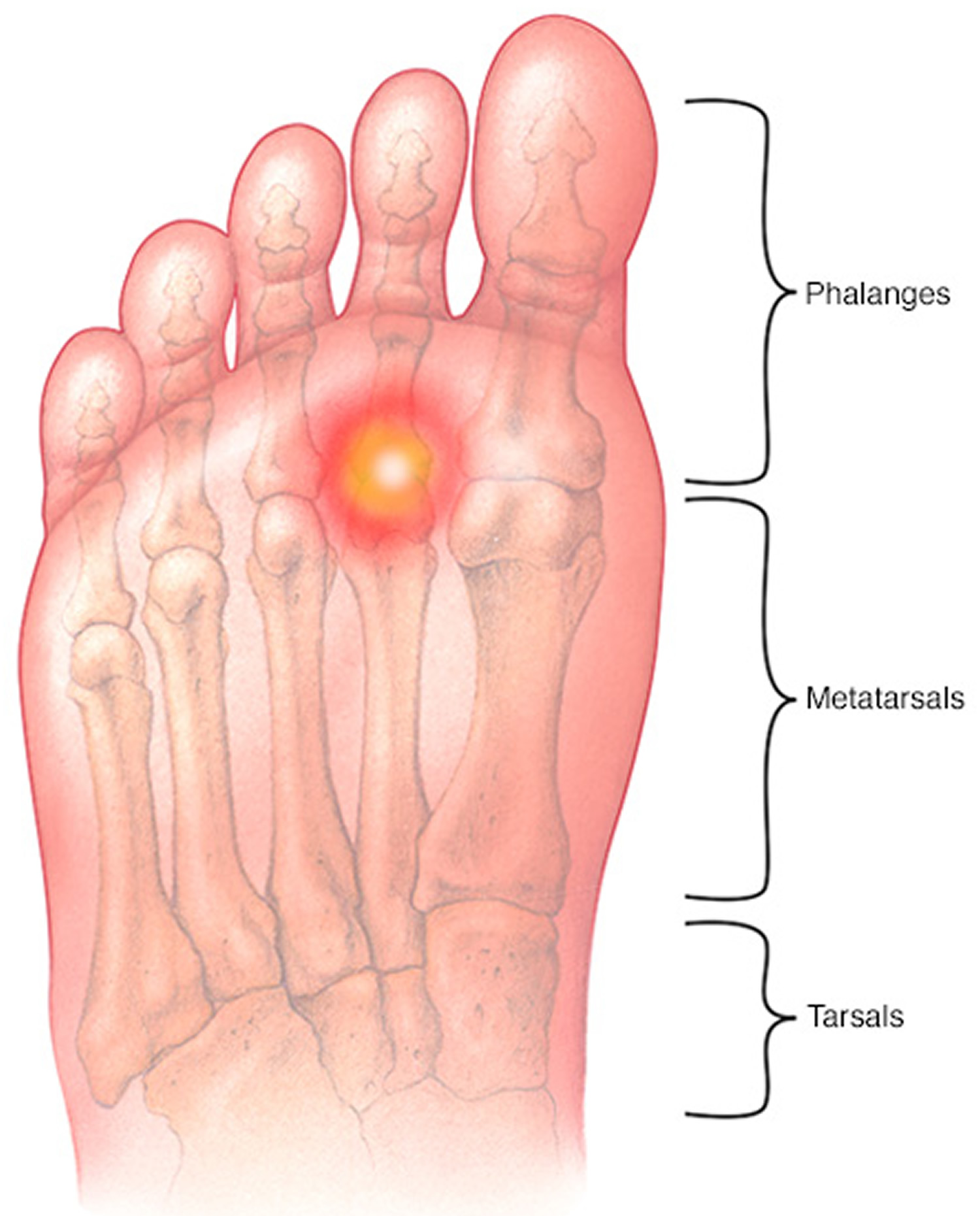
Metatarsalgia (metatarsal pain) is the name for pain in the ball of the foot. Metatarsalgia affects the metatarsals, the bones connecting the ankle bones to the toes (see Figures 1 and 2). Metatarsalgia is one of the most common reports in patients with foot problems. This pain is confined to the area across the plantar region of the forefoot under the metatarsal heads, including the second through fourth metatarsal heads. However, it is frequently accompanied by deformity of the first and fifth rays as well as of the toes. Metatarsalgia is a common source of pain because metatarsals support your weight when you’re standing, walking and running 1. Nearly 80% of the normal population present some form of pain in the metatarsal region over their lifetime 2. The main etiological factors are biomechanical alterations, which make up 92% of the total 3.
Symptoms of metatarsalgia can include:
- Sharp, aching or burning pain in the ball of your foot — the part of the sole just behind your toes
- Pain that worsens when you stand, run, flex your feet or walk — especially barefoot on a hard surface — and improves when you rest
- Sharp or shooting pain, numbness, or tingling in your toes
- A feeling of having a pebble in your shoe
Metatarsalgia can have a number of different causes, including wearing unsupportive footwear (shoes that are too tight or too loose), conditions such as arthritis, and doing high-impact sports. There is great variability in possible causative factors, but all of them seem to be related to gait mechanics, foot anatomy, and foot and ankle deformity. Primary metatarsalgia is mainly related to repetitive pressure loading under the metatarsal head, which exceeds the focal tissue tolerance and leads to inflammation and pain 4.
Some common causes of metatarsalgia include:
- Badly fitting footwear – high-heeled or restrictive shoes can force the ball of the foot into a small amount of space, which puts more pressure on that area
- High-impact sports – sports like running or tennis put extra pressure on the feet
- Being overweight or obese – this can also increase the pressure on the feet
- An unusual bone structure in the feet – having narrow, high-arched or flat feet can increase the chances of metatarsalgia
- Joint and foot conditions – including arthritis, gout, bunions, bursitis, Morton’s neuroma, hammer toes,and stress fractures
Metatarsalgia can be very uncomfortable and interfere with your normal activities, but will often improve with some simple self-help measures, such as ice and rest, often relieve symptoms.
Wearing proper footwear with shock-absorbing insoles or arch supports might prevent or minimize future problems with metatarsalgia.
You can usually treat metatarsalgia at home without seeing your doctor.
However, you should get medical advice if:
- The pain doesn’t improve despite trying self-help measures
- The pain significantly interferes with your normal activities
- You develop sudden and very severe foot pain or a change in the shape of your foot – this could be a sign of a more serious problem that requires immediate treatment
- Talk to your doctor if you have a burning pain in the ball of your foot that doesn’t improve after changing your shoes and modifying your activities.
Figure 1. Metatarsals
Metatarsalgia complications
Left untreated, metatarsalgia might lead to pain in other parts of the same or opposite foot and pain elsewhere in the body, such as the low back or hip, due to limping (altered gait) from foot pain.
Metatarsalgia causes
Metatarsalgia is usually the result of increased pressure on the ball of the foot.
Sometimes a single factor can lead to metatarsalgia. More often, several factors are involved, including:
- Intense training or activity. Distance runners are at risk of metatarsalgia, primarily because the front of the foot absorbs significant force when a person runs. But anyone who participates in a high-impact sport is at risk, especially if your shoes fit poorly or are worn.
- Certain foot shapes. A high arch can put extra pressure on the metatarsals. So can having a second toe that’s longer than the big toe, which causes more weight than normal to be shifted to the second metatarsal head.
- Foot deformities. Wearing too-small shoes or high heels can cause your foot to be misshapen. A downward-curling toe (hammertoe) and swollen, painful bumps at the base of your big toes (bunions) can cause metatarsalgia.
- Excess weight. Because most of your body weight transfers to your forefoot when you move, extra pounds mean more pressure on your metatarsals. Losing weight might reduce or eliminate symptoms.
- Poorly fitting shoes. High heels, which transfer extra weight to the front of your foot, are a common cause of metatarsalgia in women. Shoes with a narrow toe box or athletic shoes that lack support and padding also can contribute to the problem.
- Stress fractures. Small breaks in the metatarsals or toe bones can be painful and change the way you put weight on your foot.
- Morton’s neuroma. This noncancerous growth of fibrous tissue around a nerve usually occurs between the third and fourth metatarsal heads. It causes symptoms that are similar to metatarsalgia and can also contribute to metatarsal stress.
Risk factors for metatarsalgia
Almost anyone can develop metatarsalgia, but you’re at higher risk if you:
- Participate in high-impact sports that involve running and jumping
- Wear high heels, shoes that don’t fit properly or shoes with spikes, such as cleats
- Are overweight or obese
- Have other foot problems, including hammertoe and calluses on the bottom of your feet
- Have inflammatory arthritis, such as rheumatoid arthritis or gout
Metatarsalgia is also more common in older people and people with diabetes.
Metatarsalgia symptoms
Metatarsalgia tends to develop gradually over time.
It may be felt in a small area of the foot, or across the whole width of it. One or both feet may be affected.
The pain of metatarsalgia is sometimes described as:
- a burning or aching sensation
- a shooting pain
- tingling or numbness in the toes
- a feeling like there’s a small stone stuck under the foot
Metatarsalgia tends to be worse when you’re standing, walking or running.
Metatarsalgia diagnosis
Various foot problems can cause symptoms similar to those of metatarsalgia. To help pinpoint the source of your pain, your doctor will examine your foot while you stand and while you sit and ask about your lifestyle and activity level. You might need an X-ray to identify or rule out a stress fracture or other foot problems.
Metatarsalgia treatment
How to treat metatarsalgia
The following measures will often help improve metatarsalgia and stop it coming back:
- Rest your feet – put your feet up regularly and avoid activities that make the pain worse; try low-impact activities such as cycling or swimming instead of sports that involve a lot of running or jumping
- Use an ice pack – apply an ice pack to the affected area for about 20 minutes several times a day (a bag of frozen peas will also work); make sure you wrap it in a towel so it doesn’t damage your skin
- Change your footwear – try flat shoes that have plenty of room for your feet and have a well-cushioned sole; replace any worn out shoes as they could make things worse (read more about choosing sports shoes and trainers)
- Use shock-absorbing pads or insoles – these can fit inside your shoes to help cushion your feet; they’re available from pharmacies and sports shops, or can be bought online
- Maintain a healthy weight – adopting a healthy, balanced diet and doing regular low-impact exercises can help you lose weight if you’re overweight
- Take paracetamol or ibuprofen to help relieve pain and swelling if necessary
Try these measures for a few weeks to see if your symptoms improve.
In rare cases, when conservative measures don’t relieve your pain and your metatarsalgia is complicated by foot conditions such as hammertoe, surgery to realign the metatarsal bones might be an option.
Home remedies
To help ease your metatarsalgia pain, try these tips:
- Rest. Protect your foot from further injury by not stressing it. Elevate your foot after standing or walking. You might need to avoid your favorite sport for a while, but you can stay fit with low-impact exercises, such as swimming or cycling.
- Ice the affected area. Apply ice packs to the affected area for about 20 minutes at a time several times a day. To protect your skin, wrap the ice packs in a thin towel.
- Take an over-the-counter pain reliever. Try ibuprofen (Advil, Motrin IB, others), naproxen sodium (Aleve) or aspirin to reduce pain and inflammation.
- Wear proper shoes. Avoid too-tight or too-loose shoes and limit your wearing of high heels. Wear shoes appropriate to the sports you play.
- Use metatarsal pads. These off-the-shelf pads are placed in your shoes just ahead of the metatarsal bone to help deflect stress from the painful area.
- Consider arch supports. If insoles don’t help, your doctor might recommend arch supports to minimize stress on the metatarsal bones and improve foot function. You can buy arch supports over-the-counter, or they can be custom fitted.
- Espinosa N., Brodsky J.W., Maceira E. Metatarsalgia. J Am Acad Orthop Surg. 2010;18:474–485. https://www.ncbi.nlm.nih.gov/pubmed/20675640[↩]
- Viladot-Perice A. 4th ed. Springer-Verlag Ibérica; Barcelona: 2001. Metatarsalgias, patología del antepié[↩]
- Nery C.A.S. Metatarsalgias. In: Hebert S., Xavier R., Pardini Júnior A.G., Barros Filho T.E.P., editors. Ortopedia e traumatologia: princípios e prática. 4th ed. Artmed; Porto Alegre: 2009. pp. 616–639[↩]
- Wu KK. Morton neuroma and metatarsalgia. Curr Opin Rheumatol. 2000;12:131–142. doi: 10.1097/00002281-200003000-00007. https://www.ncbi.nlm.nih.gov/pubmed/10751016[↩]