Contents
What is neurodermatitis
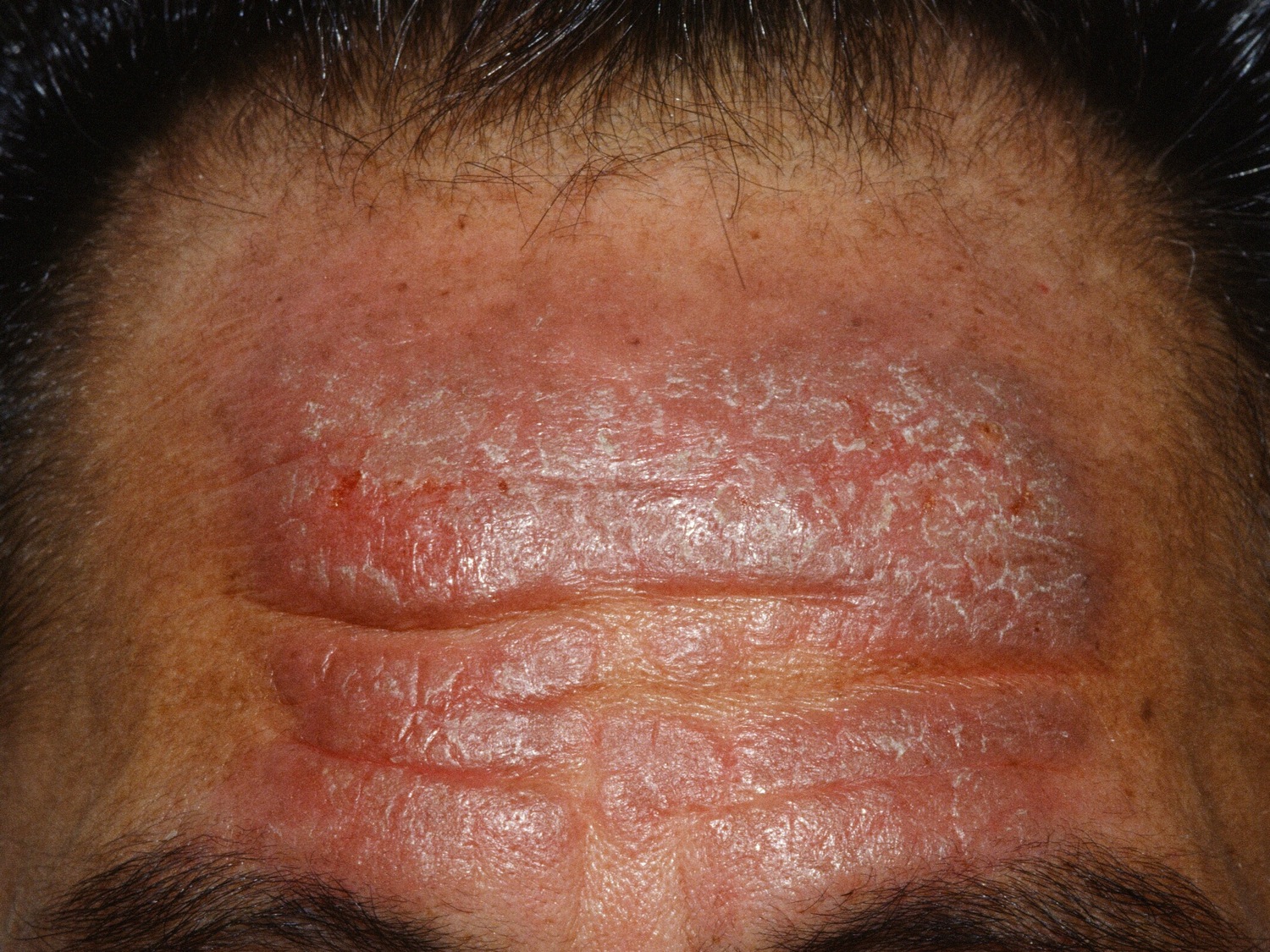
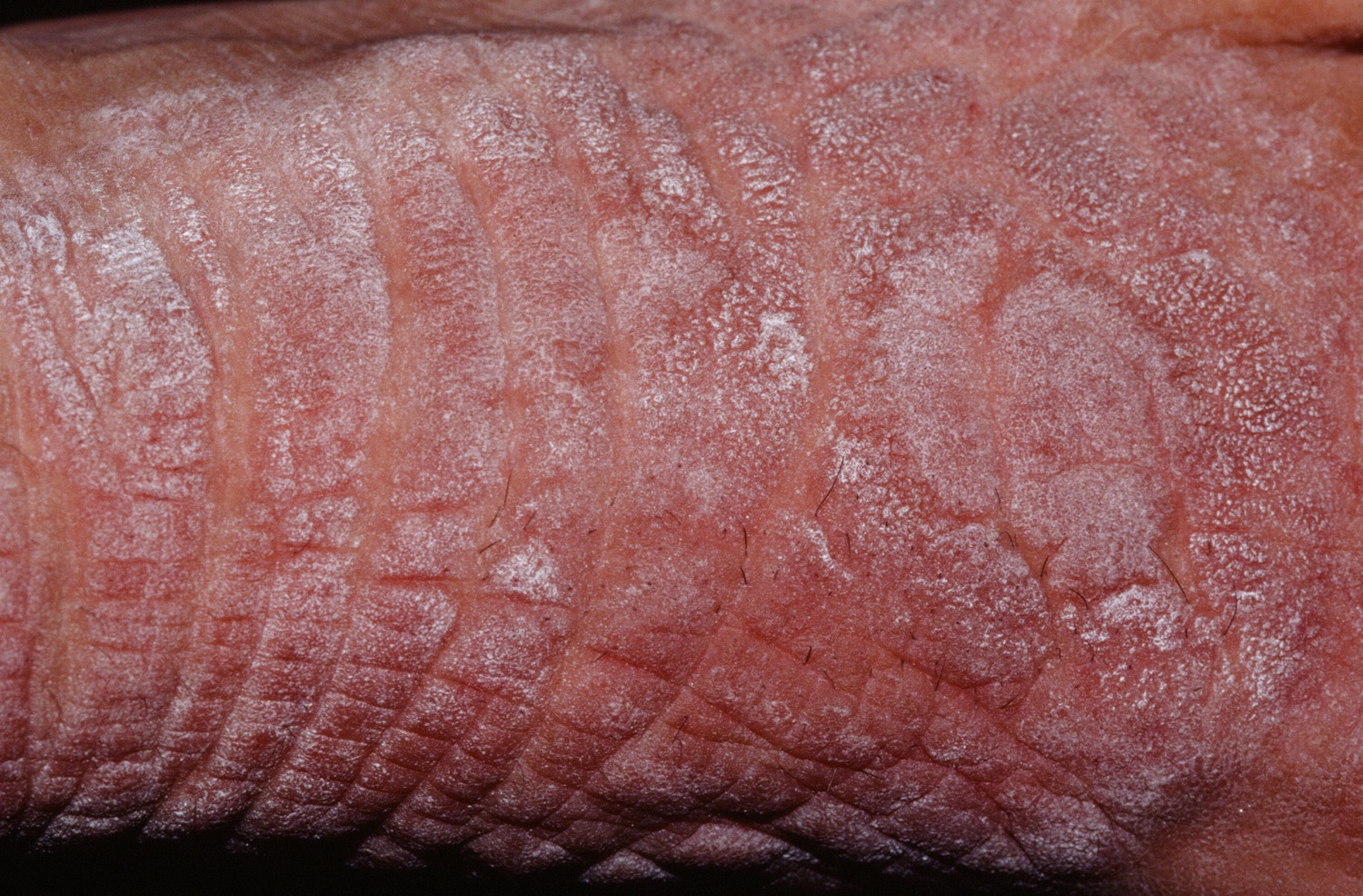
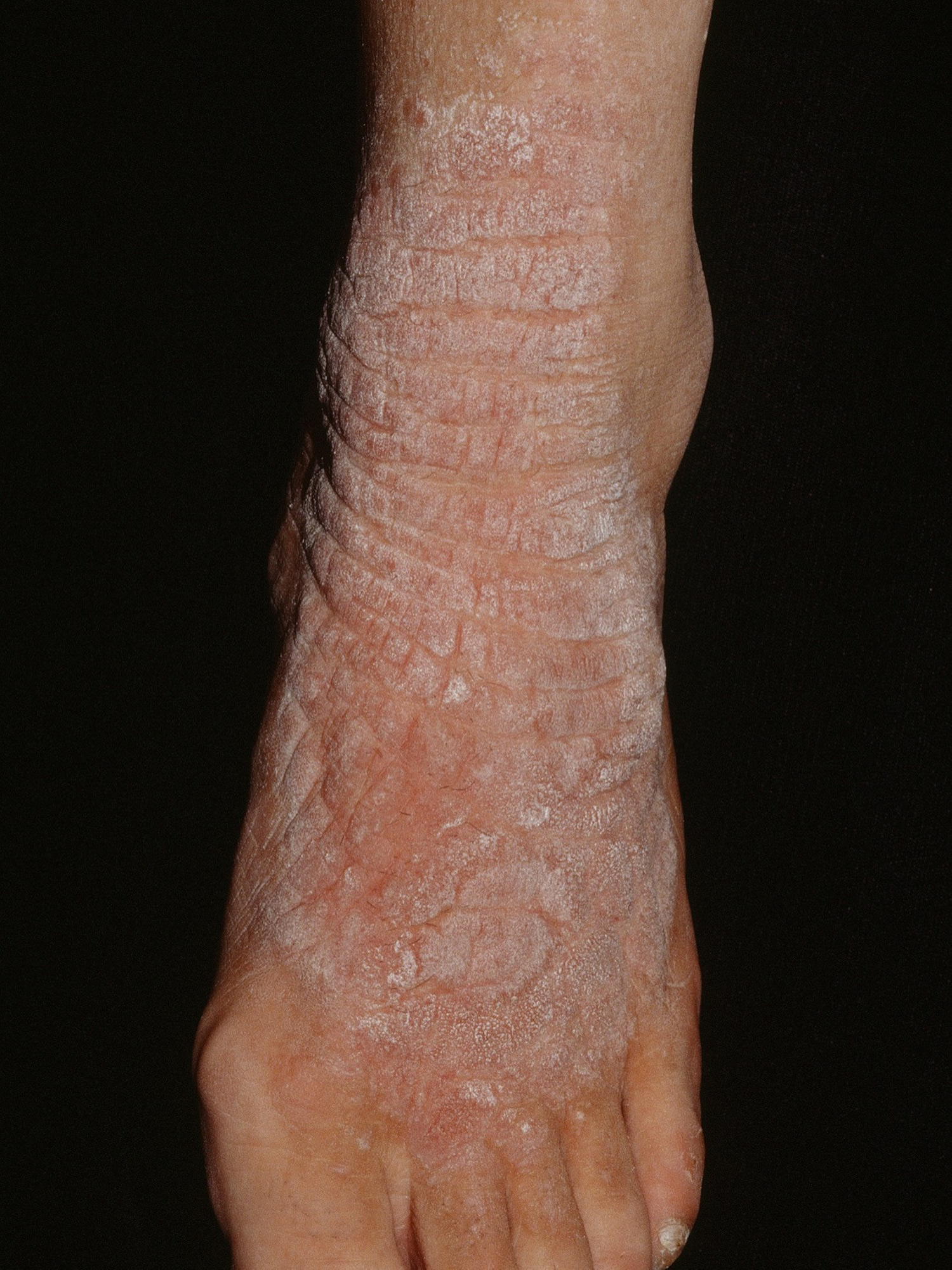
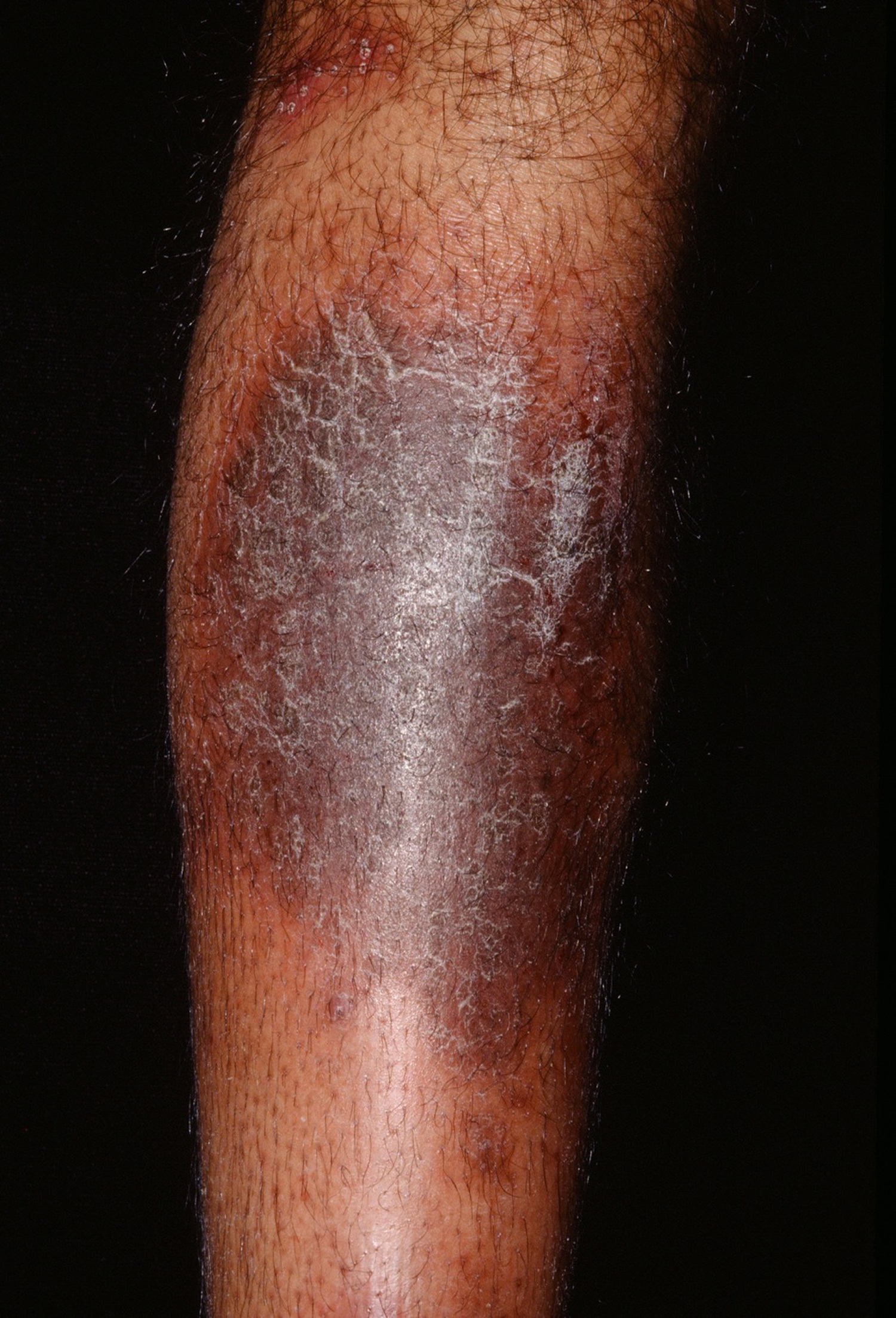
Neurodermatitis also known as lichen simplex, is a skin condition characterized by a localized area of chronic, lichenified eczema/dermatitis (see Figures 1 to 5 below). Neurodermatitis starts with a patch of itchy skin. Scratching makes it even itchier. This itch-scratch cycle causes the affected skin to become thick and leathery. The term lichenified refers to skin thickening with accentuation of the skin markings. You may develop several itchy spots, typically on the neck, wrist, forearm, thigh or ankle.
Neurodermatitis occurs in adult males and females. Women are more likely to develop neurodermatitis than are men. The condition is most common between ages 30 and 50. Neurodermatitis is unusual in children. However, some children who have eczema (atopic dermatitis) can develop neurodermatitis. Neurodermatitis is more common in people with anxiety and/or obsessive compulsive disorder.
Neurodermatitis is not life-threatening or contagious. But the itching can be so intense or recurrent that it disrupts your sleep, sexual function and quality of life.
Breaking the itch-scratch cycle of neurodermatitis is challenging. Treatment success depends on resisting the urge to rub or scratch the affected areas. Over-the-counter and prescription creams can help ease the itching. You’ll also need to identify and eliminate factors that may be aggravating the problem.
Figure 1. Neurodermatitis (lichen simplex chronicus)
Figure 2. Neurodermatitis (lichen simplex)
Figure 3. Neurodermatitis (lichen simplex) leg
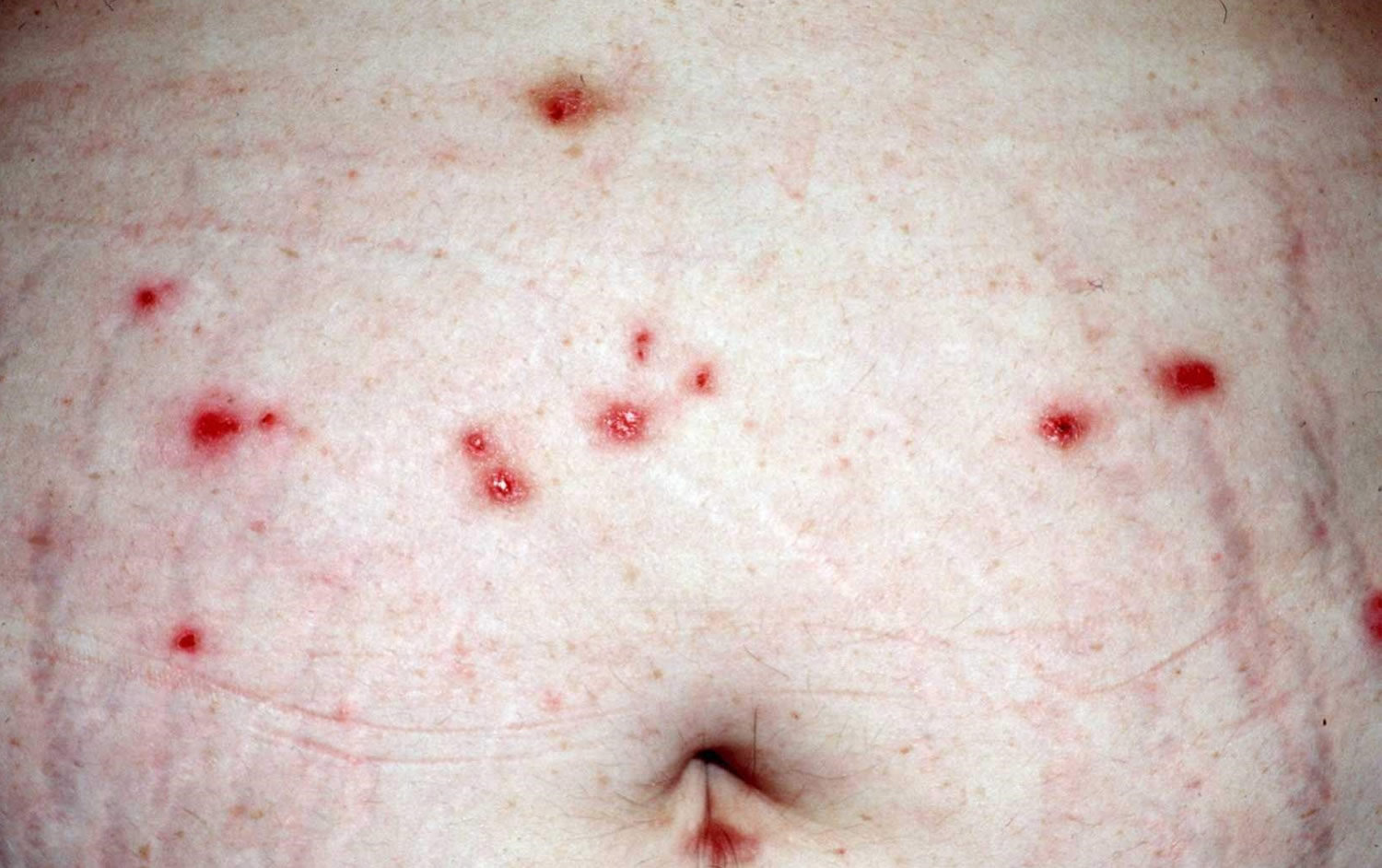
Figure 4. Neurodermatitis (lichen simplex) abdomen
Figure 5. Neurodermatitis (lichen simplex chronicus) face
Neurodermatitis causes
Although the exact cause of neurodermatitis isn’t known, neurodermatitis (lichen simplex chronicus) follows repetitive scratching and rubbing, which arises because of chronic localized itch.
Sometimes neurodermatitis begins with something that simply rubs or irritates the skin, such as tight clothing or a bug bite. As you rub or scratch the area, it gets itchier. The more you scratch, the more it itches.
In some cases, neurodermatitis is associated with other skin conditions, such as dry skin, eczema or psoriasis. Stress and anxiety can trigger itching too.
The primary itch can be due to:
- Atopic eczema (atopic dermatitis)
- Contact eczema
- Venous eczema
- Psoriasis
- Lichen planus
- Fungal infection
Researchers have discovered that a trigger can increase the risk of developing neurodermatitis. Things that can trigger neurodermatitis include:
- Injury to a nerve – neuropathy (radiculopathy) e.g., brachioradial pruritus. Itch due to neuropathy appears to be due to hyperexcitable sensory nerve fibers following nerve injury or entrapment.
- Period of intense stress or emotional trauma
- Insect bite
- Bug bite
- Tight clothing, especially clothing made of wool or a synthetic fabric like rayon or polyester
- Dry skin
Traffic exhaust, allergens, sweat, heat, and poor blood flow can also be a trigger.
Risk factors for developing neurodermatitis
Certain factors may affect your risk of neurodermatitis, including:
- Your sex and age. Women are more likely to develop neurodermatitis than are men. The condition is most common between ages 30 and 50.
- Other skin conditions. People with a personal or family history of dermatitis, eczema, psoriasis or similar skin conditions are more likely to develop neurodermatitis.
- Anxiety disorders. Anxiety (especially obsessive-compulsive disorder) and stress can trigger the itch associated with neurodermatitis.
Neurodermatitis complications
Persistent scratching can lead to a wound, a bacterial skin infection, or permanent scars and changes in skin color. Scratching may also disrupt your sleep.
Neurodermatitis symptoms
Signs and symptoms of neurodermatitis include:
- An itchy skin patch or patches
- Leathery or scaly texture on the affected areas
- A raised, rough patch or patches that are red or darker than the rest of your skin
The condition involves areas that can be reached for scratching — the head, neck, wrist, forearm, ankle, vulva, scrotum or anus. The itchiness, which can be intense, may come and go or be nonstop. You may scratch out of habit and while sleeping.
When a person has neurodermatitis, the person is likely to notice several of these signs and symptoms:
Itch
Neurodermatitis causes an itchy patch on the surface of the body. Unlike eczema, psoriasis, and other itchy skin conditions, people tend to develop just 1 or 2 patches that itch. While rare, neurodermatitis can cause several itchy patches.
When people develop neurodermatitis, they often find themselves:
- Scratching or rubbing the itchy patch(es), either frequently or sporadically
- Thinking that the patch(es) itches for no apparent reason
- Feeling itchiest while relaxing
- Feeling especially itchy when life becomes stressful
Pain
Some people feel pain. One study found that when neurodermatitis appears on the scalp, it may cause pain, itch, or both.
Raised, rough patch that is red to violet-colored
As the person continues to scratch or rub the itchy patch, a scaly, reddish to violet-colored patch appears.
Skin thickens and looks leathery
With frequent scratching or rubbing, the skin can thicken. The patch may look leathery and turn a brownish color. Very thick skin can have a grayish hue.
Hair loss
The scratching (or rubbing) can cause hair loss on areas like the scalp.
Open sore that bleeds
Repeatedly scratching or rubbing can wound the skin, leading to an open sore that bleeds. If this happens, the person has an increased risk of developing an infection.
Scarring
If a wound is deep, the skin may scar as it heals.
Infection
Signs of infection include honey-colored crusts and fluid leaking from the area. You may also see pus-filled bumps.
Neurodermatitis diagnosis
Your doctor may diagnose neurodermatitis by examining the affected skin and determining whether you’ve been itching and scratching. To rule out other causes, he or she may take a small sample of the affected skin (skin biopsy) for testing and skin scrapings for possible tinea infection.
Neurodermatitis treatment
It is important to understand that the itchy patch of skin is, at least in part, due to scratching and rubbing. Treatment needs to address the symptoms and any underlying cause.
It is of vital importance that the patient be told not to scratch, because it doesn’t matter how strong a steroid your doctor give you, if you continue to scratch, you’ll continue to have neurodermatitis.
Treatment is aimed at controlling the itching, preventing scratching and addressing underlying causes.
- Anti-inflammatory medicated creams. If over-the-counter corticosteroid cream isn’t helping, your doctor may prescribe a stronger version of this drug. Potent topical steroids until the plaque is resolved (4–6 weeks) — occlusion for a few hours after application may enhance efficacy. Reduce potency or frequency of topical steroids once lichenification has resolved. A calcineurin inhibitor (tacrolimus) ointment may help if the vulva is involved.
- Corticosteroid injections. Your doctor may inject corticosteroids directly into the affected skin every 4–6 weeks to help it heal.
- Anti-itch medications. Prescription antihistamines help relieve itching in many people with neurodermatitis. Some of these drugs may cause drowsiness and help with alleviating scratching while you sleep.
- Coal tar preparations
- Anti-anxiety drugs. Because anxiety and stress can trigger neurodermatitis, anti-anxiety drugs may help prevent the itchiness.
- Tricyclic antidepressant (eg, amitriptyline or nortriptyline), to help sleep.
- Light therapy. Exposing the affected skin to particular types of light is sometimes helpful.
- Psychotherapy. Talking with a counselor can help you learn how your emotions and behaviors can fuel — or prevent — itching and scratching.
- Moisturizers to relieve dryness and reduce desire to scratch.
- Capsaicin cream or doxepin cream: These may decrease the itch.
- Cooling creams containing menthol.
- Tacrolimus ointment (approved to treat atopic dermatitis), which you would apply to the itchy area.
Treating the primary underlying condition; for example:
- Antifungal agents for dermatophyte infection
- Phototherapy and immunomodulatory medications for inflammatory dermatoses (oral corticosteroids, methotrexate, azathioprine or ciclosporin)
- Tricyclic antidepressants (amitriptyline, nortriptyline, doxepin), other antidepressants (eg, duloxetine) or antiepileptic medications (valproate, lamotrigine, gabapentin) for radiculopathy.
- If stress or anxiety is a constant in your life, the following may be necessary to get rid of the itch:
- An anti-anxiety medicine
- Psychotherapy, so you can talk about stress or anxiety and find ways to manage these effectively.
Emerging therapies
Further study is needed, but some small studies have reported success with the following treatments:
- Botulinum toxin (Botox) injection. In one study of 3 patients, all the patients had noticeably less itch within 1 week. Within 2 to 4 weeks, everyone’s patches of neurodermatitis had cleared.
- Aspirin solution. Applying a solution combining aspirin and dichloromethane has been effective for some people with neurodermatitis.
Lifestyle and home remedies
These self-care measures can help you manage neurodermatitis:
- Stop rubbing and scratching. The itching may be intense, but rubbing and scratching worsen the situation.
- Apply cool, wet compresses. These may soothe the skin and relieve the itch. Putting a cool, wet compress on the affected skin for 5 minutes before you apply a corticosteroid can help the medicine penetrate thickened skin more easily — and reduce the itchiness.
- Try over-the-counter medications. Apply an anti-itch cream or lotion to the affected area. A hydrocortisone cream can temporarily relieve the itch. An oral antihistamine, such as diphenhydramine (Benadryl, others) can relieve severe itching and help you sleep. Some people have had success with capsaicin cream, but it may sting at first.
- Antihistamine: This can relieve the itch and help you sleep.
- Cover the affected area. Bandages or dressings can help protect the skin and prevent scratching. These may be especially useful if you scratch during your sleep.
- Moisturizer: This reduces dryness, which can reduce the itch.
- Keep your nails trimmed. Short nails may do less damage to the skin, especially if you tend to scratch while you’re asleep.
- Take warm baths and moisturize your skin. Prepare your bath with warm — not hot — water. Sprinkle in baking soda, uncooked oatmeal or colloidal oatmeal (Aveeno, others). Use mild soaps without dyes or perfumes. After washing, apply unscented moisturizer to protect your skin.
- Avoid triggers. Notice what seems to bring on a recurrence and avoid it. For example, use stress management techniques and wear clothing that isn’t itchy.