Contents
What is papular urticaria
Papular urticaria is a common and often annoying disorder manifested by chronic or recurrent papules caused by a hypersensitivity reaction to the bites of mosquitoes, fleas, bedbugs and other insects 1. Individual papules may surround a wheal and display a central punctum 2. Despite the name, papular urticaria is not a true urticaria, which implies temporary whealing that resolves within hours. Papular urticaria bumps last days to weeks.
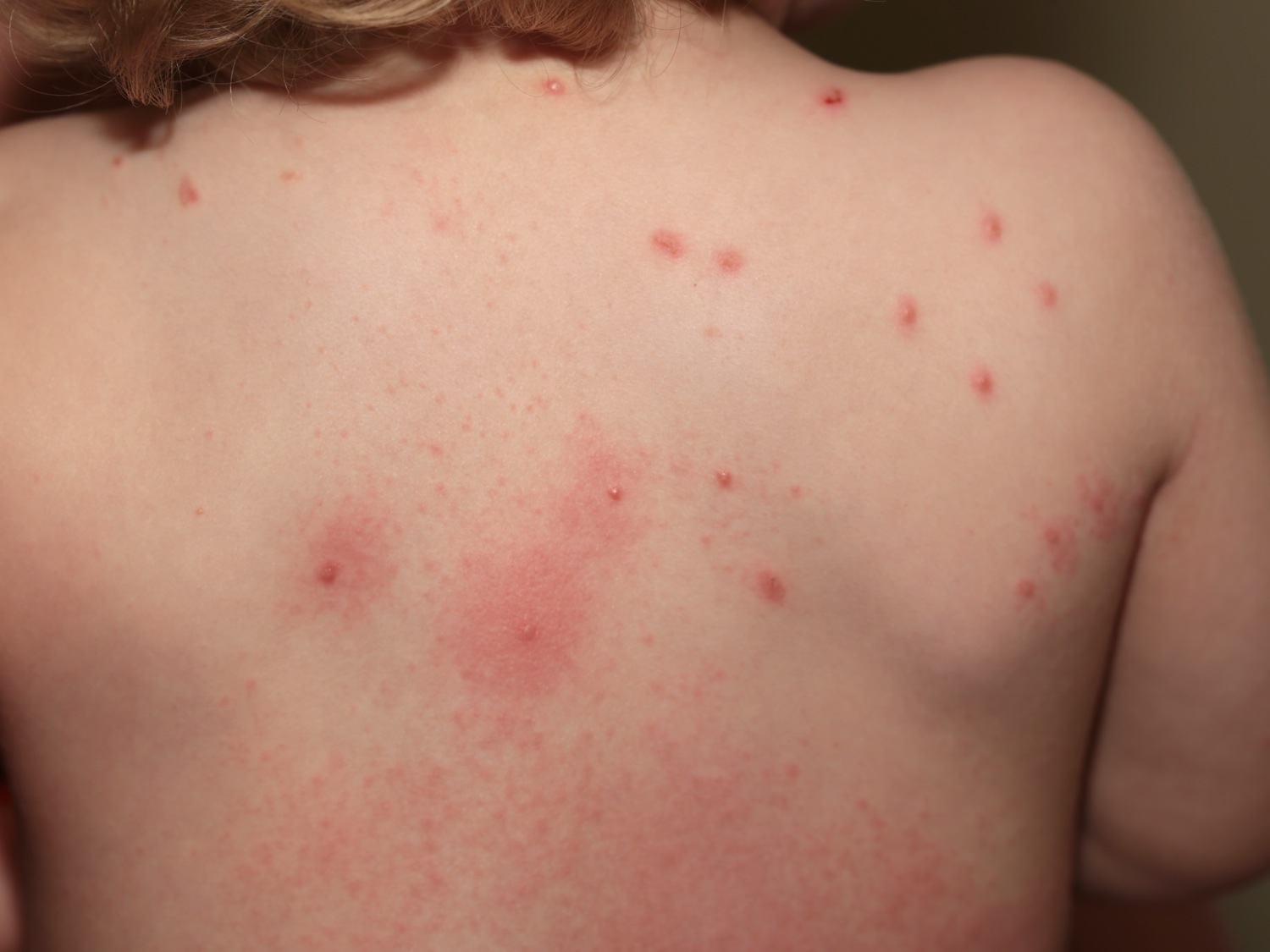
Crops of very itchy red bumps, 0.2 to 2 cm in diameter, appear every few days during the summer or autumn months. Sometimes each spot develops a fluid-filled blister up to one centimeter in diameter. They are most often on the legs and other uncovered areas such as forearms and face, but sometimes they are scattered in small groups all over the body.
It is difficult not to scratch papular urticaria, so the spots become crusted and may get infected – they are then pussy and sore. Sometimes one new spot provokes old ones to come up again and itch intensely.
The spots remain for a few days to a few weeks and can leave persistent marks or scars, especially if they have been scratched deeply.
Papular urticaria may clear up on holiday or on moving house. One or several members of the family may be affected. Occasionally the eruption can clear up for years and then recur unexpectedly. It is not associated with any internal complaint.
Figure 1. Papular urticaria (insect bites)
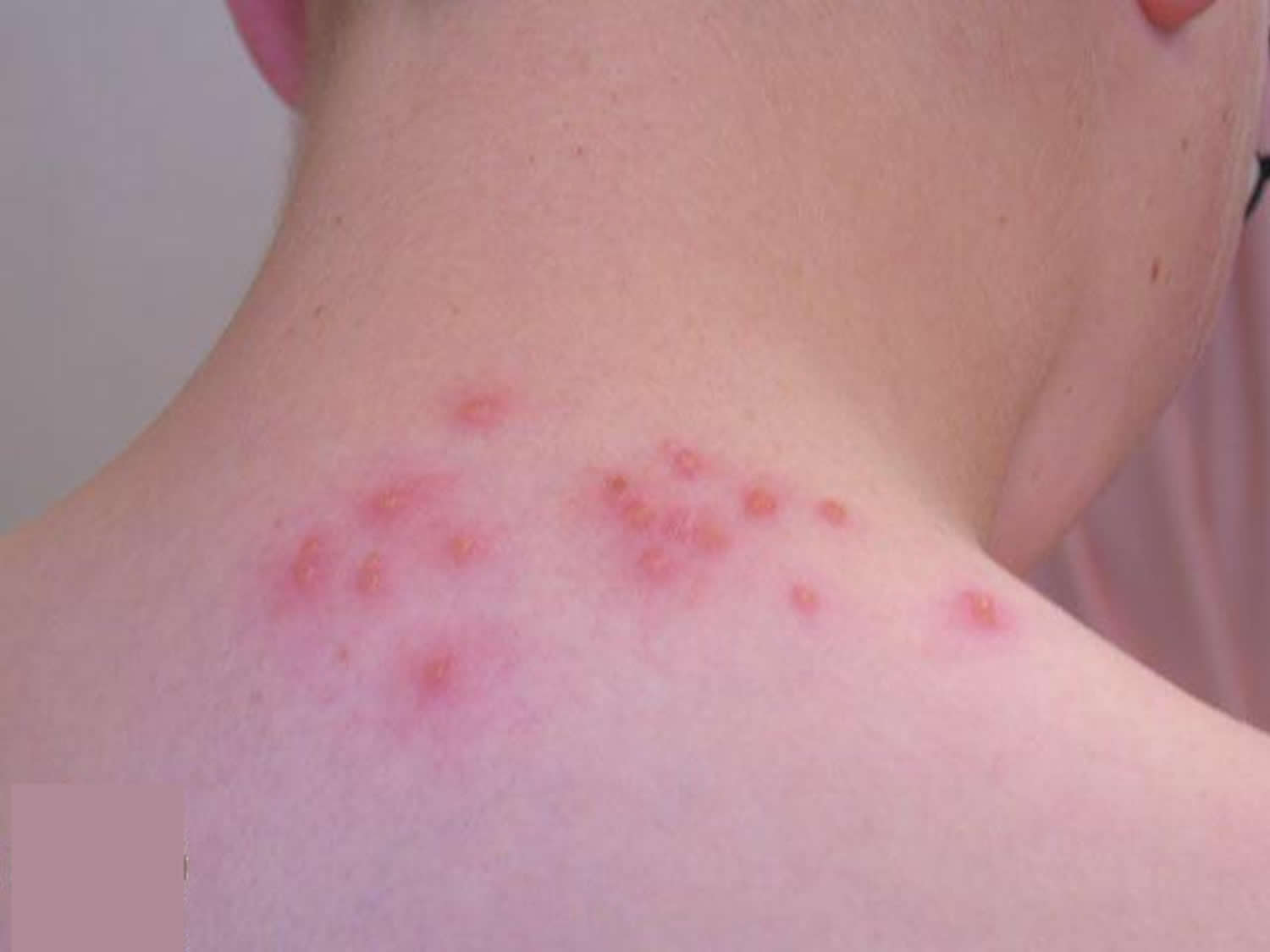
Although the overall incidence rate is unknown, papular urticaria tends to be evident during spring and summer months; in some climates, such as that in San Francisco, California, this condition may affect children throughout the year. In addition, despite no known racial or sex predisposition, certain ethnic groups (specifically Asians) may be more predisposed to more intense reactions, and a small Nigerian study reported a slight female predominance for skin diseases such as papular urticaria and atopic dermatitis 3. Papular urticaria was evident in 2.24% of 5250 first-time pediatric patients, with 6029 diagnoses in one pediatric dermatology service survey 4. A survey of skin disorders in more than a 1000 new pediatric patients at a hospital in Bangalore, India found insect bite reactions and papular urticaria in 5.1% 5. A Nigerian survey of 491 pediatric dermatoses in 441 patients found papular urticaria in 6.7% of them 6. Papular urticaria is also common in Colombia, linked with exposure to indoor fleas and poverty 7.
This eruption is primarily self-limited, and children eventually outgrow this disease, probably through desensitization after multiple arthropod exposures 8. However, adults can be affected, albeit at a much lower rate.
Causes of Papular urticaria
Papular urticaria is generally regarded to be the result of a hypersensitivity or allergic reaction reaction to bites from insects 9, such as mosquitoes, gnats, fleas 10, mites 11, bedbugs 12, caterpillars 13 and moths. The most common identified causes are insects that live on cats and dogs, particularly fleas and mites. Fleas are easily seen with the naked eye but can be difficult to get rid of. Mites are too small to see but are equally common. Animals get repeatedly infested and have to be treated with flea powder or a leave-on preparation such as fipronil every few weeks. Unfortunately flea collars are not very effective. Fleas produce many eggs, which become larvae and pupae. The average cat has only twenty fleas, but is surrounded by 20,000!
Often after a few months or years the person becomes desensitized to these insects and the reaction dies down. Affected individuals rarely notice the initial bite. Varicella vaccines have also been implicated 14. Not everyone with papular urticaria has pets, and it can be nearly impossible to work out what a patient is reacting to 15. One specific mite causing it is Peymotes ventricosus and it is also known as the “grain itch”, “barley itch”, “straw itch”, “hay itch”, “prairie itch”, “mattress itch”, and “cotton seed itch”, sometimes evident occupationally in farmers, bakers, dock workers, packers, and indoor workers. These mites are invisible to the naked eye 16.
The histopathologic pattern in papular urticaria consists of mild subepidermal edema, extravasation of erythrocytes, interstitial eosinophils, and exocytosis of lymphocytes. These findings suggest a pathophysiologic process that is immunologically based 2.
Morphologic and immunohistochemical evidence suggest that a type I hypersensitivity reaction plays a central role in the pathogenesis of papular urticaria. The reaction is thought to be caused by a hematogenously disseminated antigen deposited by an arthropod bite in a patient who is sensitive. This theory is supported by the fact that these lesions can and often do occur in areas away from the bites. The putative antigen is unknown.
The presence of immunoglobulin and complement deposits in the skin of some patients with papular urticaria suggests that the lesions may be due to a cutaneous vasculitis 17. The deposits were most frequently seen in lesions within 24 hours of their development. The presence of granular deposits of Clq, C3, and immunoglobulin M (IgM) in superficial dermal blood vessel walls suggests that immune complexes (IgM aggregates) may be primarily involved in the pathogenesis, with complement activation initiated by Clq through the classic pathway. A T helper 2 (Th2) shift may be present, similar to what is observed in atopy 10.
In a study of the specific pattern of flea antigen recognition by IgG subclass and IgE during the progression of papular urticaria caused by flea bite, variations in the antibody responses of both subclasses to flea antigens were identified 18. Among these 25 patients, those with 2-5 years of papular urticaria had more IgE bands than patients with shorter or longer durations of symptoms. Thus, the predominant specific antibody isotypes appear to vary according to the time elapsed from the onset of fleabite-induced papular urticaria 18. The cellular immune response against whole-flea antigen in patients with papular urticaria by flea bites may be the result of an impaired dendritic cell population 19.
Papular urticaria diagnosis
Children, adult males, nonlocal inhabitants, and those belonging to urban or periurban areas may be more vulnerable to papular urticaria 20. Patients usually report chronic or recurrent episodes of a papular eruption that tends to occur in groups or clusters associated with intense pruritus. The most common first appearance is of papules and urticarial plaques in clusters over exposed and covered parts of the body.
The eruption is characterized by crops of symmetrically distributed pruritic papules and papulovesicles. The lesions can also appear in an area localized to the site of insect bites, but they occur on any body part. The lesions tend to be grouped on exposed areas (see the image below), particularly the extensor surfaces of the extremities. Sometimes, a central hemorrhagic punctum may be evident with ecchymoses and brownish pigmentation persisting after resolution 16. Scratching may produce erosions and ulcerations. Secondary impetigo or pyoderma is common. Having pets and the use of colognes were identified as predisposing factors for insect bite dermatitis in one large study, whereas atopy was not 21.
Papular urticaria treatment
The treatment of papular urticaria should be conservative and is symptomatic in most cases. Mild topical steroids and systemic antihistamines for relief of the itching that often accompanies this condition may be used. On occasion, papular urticaria may be severe enough to warrant the use of short-term systemic corticosteroids. If secondary impetigo occurs, topical or systemic antibiotics may be needed. Note that the use of insect repellents while the patient is outside and the use of flea and tick control on indoor pets are necessary when these individuals are being treated for papular urticaria.
Rigorous use of an effective insecticide may prevent insect bites and, accordingly, papular urticaria. Insecticides containing diethyltoluamide (DEET) are among the most beneficial. For safety purposes, topical insecticides used on infants and children should be in accordance with their age. DEET, picaridin, PMD (para-menthane-3,8-diol), and IR3535 are suitable for protection against arthropod bites; IR3535 is not suitable for Anopheles mosquitoes 22. Use of protective clothing, insecticide-treated bed nets, and insecticide-treated clothing is desirable.
An oral desensitization vaccine has been attempted, but the vaccine was deemed ineffective and the study sample size was too small for statistical significance 23.
Home remedies of papular urticaria include:
- Topical steroid cream – this should be applied as soon as the itchy spots appear.
- Antihistamine tablets – these may reduce the spots and reduce itching.
- Antiseptic cream to reduce or avoid secondary infection.
- Insecticides to rid the house, work place or school, of insects.
- Kennel and carpet spray containing a pyrethroid – this should be followed by vacuuming.
- Long lasting insect growth regulator.
- Keeping pets outside.
- Wearing fully covering clothing.
- Insect repellents applied to exposed skin to prevent insect bites when outdoors.
- Papular Urticaria. https://emedicine.medscape.com/article/1051461-overview[↩]
- Stibich AS, Schwartz RA. Papular urticaria. Cutis. 2001 Aug. 68(2):89-91.[↩][↩]
- Altraide DD, George IO, Frank-Briggs AI. Prevalence of skin diseases in Nigerian children–(the University of Port Harcourt Teaching Hospital) experience. Niger J Med. 2008 Oct-Dec. 17(4):417-9.[↩]
- Del Pozzo-Magaña BR, Lazo-Langner A, Gutiérrez-Castrellón P, Ruiz-Maldonado R. Common Dermatoses in Children Referred to a Specialized Pediatric Dermatology Service in Mexico: A Comparative Study between Two Decades. ISRN Dermatol. 2012. 2012:351603.[↩]
- Sacchidanand S, Sahana MS, Asha GS, Shilpa K. Pattern of pediatric dermatoses at a referral centre. Indian J Pediatr. 2014 Apr. 81(4):375-80.[↩]
- Oninla OA, Oninla SO, Onayemi O, Olasode OA. Pattern of paediatric dermatoses at dermatology clinics in Ile-Ife and Ilesha, Nigeria. Paediatr Int Child Health. 2016 May. 36 (2):106-12.[↩]
- Lozano AM, López JF, Zakzuk J, García E. Papular urticaria: A review of causal agents in Colombia. Biomedica. 2016 Dec 1. 36 (4):632-645.[↩]
- Steen CJ, Carbonaro PA, Schwartz RA. Arthropods in dermatology. J Am Acad Dermatol. 2004 Jun. 50(6):819-42, quiz 842-4.[↩]
- Lewis-Jones MS. Papular urticaria caused by Dermestes maculatus Degeer. Clin Exp Dermatol. 1985 Mar. 10(2):181.[↩]
- Cuellar A, Rodriguez A, Rojas F, Halpert E, Gomez A, Garcia E. Differential Th1/Th2 balance in peripheral blood lymphocytes from patients suffering from flea bite-induced papular urticaria. Allergol Immunopathol (Madr). 2009 Jan-Feb. 37(1):7-10.[↩][↩]
- Burns DA. Papular urticaria produced by the mite Listrophorus gibbus. Clin Exp Dermatol. 1987 May. 12(3):200-1.[↩]
- Demain JG. Papular urticaria and things that bite in the night. Curr Allergy Asthma Rep. 2003 Jul. 3(4):291-303.[↩]
- Hossler EW. Caterpillars and moths: Part II. Dermatologic manifestations of encounters with Lepidoptera. J Am Acad Dermatol. 2010 Jan. 62(1):13-28; quiz 29-30.[↩]
- Bronstein DE, Cotliar J, Votava-Smith JK, Powell MZ, Miller MJ, Cherry JD. Recurrent papular urticaria after varicella immunization in a fifteen-month-old girl. Pediatr Infect Dis J. 2005 Mar. 24(3):269-70.[↩]
- Lembo S, Panariello L, d’Errico FP, Lembo G. Professional’s and non-professional’s papular urticaria caused by Scleroderma domesticum. Contact Dermatitis. 2008 Jan. 58(1):58-9.[↩]
- Corazza M, Tassinari M, Pezzi M, Ricci M, Borghi A, Minghetti S, et al. Multidisciplinary Approach to Pyemotes ventricosus Papular Urticaria Dermatitis. Acta Derm Venereol. 2014 Feb 26. 94(2):248-249.[↩][↩]
- Heng MC, Kloss SG, Haberfelde GC. Pathogenesis of papular urticaria. J Am Acad Dermatol. 1984 Jun. 10(6):1030-4.[↩]
- Cuellar A, Rodriguez A, Halpert E, et al. Specific pattern of flea antigen recognition by IgG subclass and IgE during the progression of papular urticaria caused by flea bite. Allergol Immunopathol (Madr). 2010 Mar 11.[↩][↩]
- Dominguez-Amorocho O, Duarte S, González JM, Halpert E, Ortega MC, Rodríguez A, et al. Differences in Systemic and Skin Migrating-Specific CD4 T Cells in Papular Urticaria by Flea Bite. Int Arch Allergy Immunol. 2012 Sep 25. 160(2):165-172.[↩]
- Raza N, Lodhi MS, Ahmed S, Dar NR, Ali L. Clinical study of papular urticaria. J Coll Physicians Surg Pak. 2008 Mar. 18(3):147-50.[↩]
- Kar S, Dongre A, Krishnan A, Godse S, Singh N. Epidemiological study of insect bite reactions from central India. Indian J Dermatol. 2013 Sep. 58(5):337-41.[↩]
- Alpern JD, Dunlop SJ, Dolan BJ, Stauffer WM, Boulware DR. Personal Protection Measures Against Mosquitoes, Ticks, and Other Arthropods. Med Clin North Am. 2016 Mar. 100 (2):303-16.[↩]
- Giraldi S, Ruiz-Maldonado R, Tamayo L, Sosa-de-Martinez C. Oral desensitization in papular urticaria in children. Trop Doct. 2002 Jul. 32(3):142-5.[↩]