Contents
What is patent foramen ovale
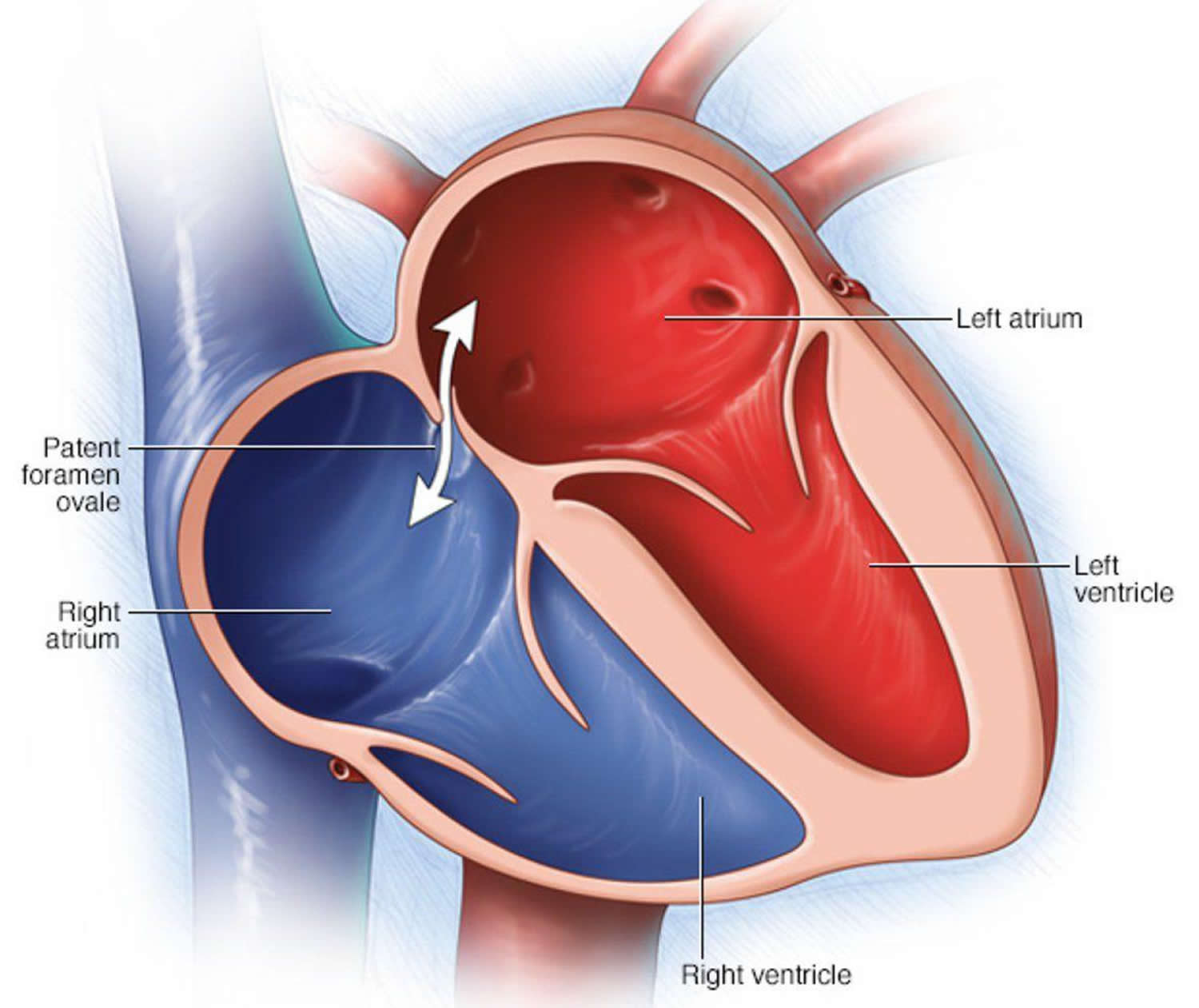
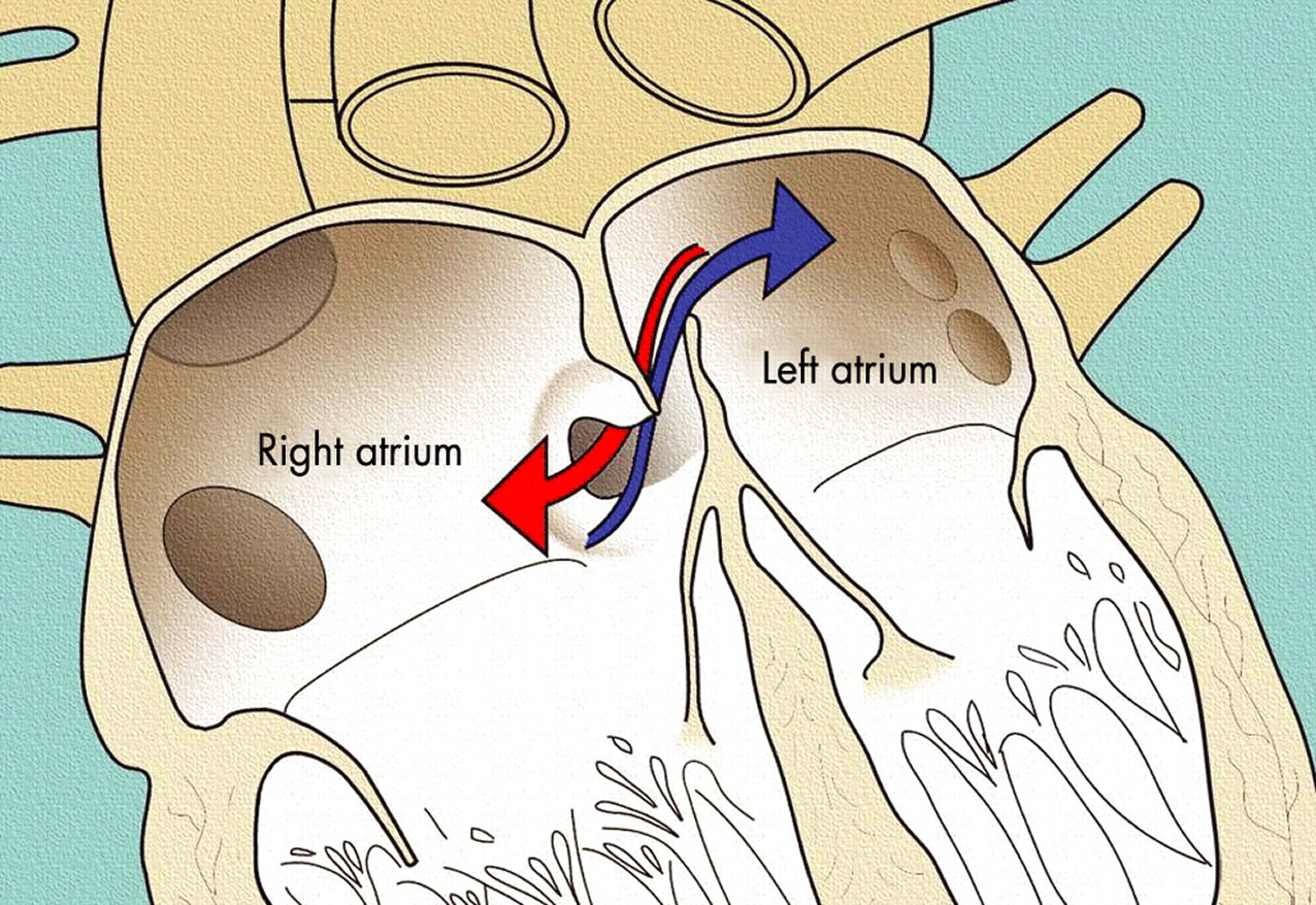
A patent foramen ovale is a small flap-like opening between the top two chambers of the heart, the right and the left atrium. This is part of the fetal circulation when you’re in the womb, allowing blood to bypass the lungs and take oxygen straight to the brain and body.
In most people, this closes when they’re very young, but for some, it stays fully or partially open. This usually doesn’t cause any symptoms or problems with the function of your heart, so it often isn’t picked up until you have tests for other conditions.
There are two kinds of holes in the heart. One is called an atrial septal defect (ASD), and the other is a patent foramen ovale (PFO). Although both are holes in the wall of tissue (septum) between the left and right upper chambers of the heart (atria), their causes are quite different. An atrial septal defect (ASD) is a failure of the septal tissue to form between the atria, and as such it is considered a congenital (present at birth) heart defect, something that you are born with. Generally an ASD hole is larger than that of a patent foramen ovale. The larger the hole, the more likely there are to be symptoms.
Patent foramen ovales, on the other hand, can only occur after birth when the foramen ovale fails to close. The foramen ovale is a hole in the wall between the left and right atria of every human fetus. This hole allows blood to bypass the fetal lungs, which cannot work until they are exposed to air. When a newborn enters the world and takes its first breath, the foramen ovale closes, and within a few months it has sealed completely in about 75 percent of us. When it remains open in about 25 percent of the normal population, it is called a patent foramen ovale, patent meaning open. For the vast majority of the millions of people with a patent foramen ovale, it is not a problem, even though blood is leaking from the right atrium to the left. Problems can arise when that blood contains a blood clot.
Most people with patent foramen ovale never know they have it. An infant who has no other heart defects will have normal health and life span.
Most patent foramen ovales do not cause any symptoms. These do not need any treatment, that is most people will not require surgery to close it or medications. But sometimes patent foramen ovales can lead to complications. The most significant of these is stroke. This happens when a traveling blood clot blocks a blood vessel in the brain. Though patent foramen ovales do not cause most strokes, having a patent foramen ovale plus having a high risk of developing blood clots may slightly raise the risk for stroke in some people.
If you have no risk factors for stroke or any history of traveling blood clots, you usually will not get treatment. But if you have had such problems, your healthcare provider may want to treat your patent foramen ovale.
Treatment for patent foramen ovales varies. In some cases, your healthcare provider may still choose not to treat the patent foramen ovale. Another choice is medicine that helps prevent blood clots, such as aspirin or warfarin. Sometimes your healthcare provider will suggest closing the patent foramen ovale by using a catheter. Closing the patent foramen ovale during traditional heart surgery is another possible route.
Compared with a traditional surgical repair, a robotic-assisted minimally invasive repair may ease your pain after surgery. It may also allow you to recover more quickly. Plus it may give your surgeon more exact control compared with other types of minimally invasive patent foramen ovale repair. It may decrease your risk for complications. Ask your healthcare provider what treatment makes sense for you.
Some research shows a possible link between patent foramen ovale and suffering with certain types of migraine, but more studies are needed before scientists can confirm this.
Human heart
Normal heart function after birth
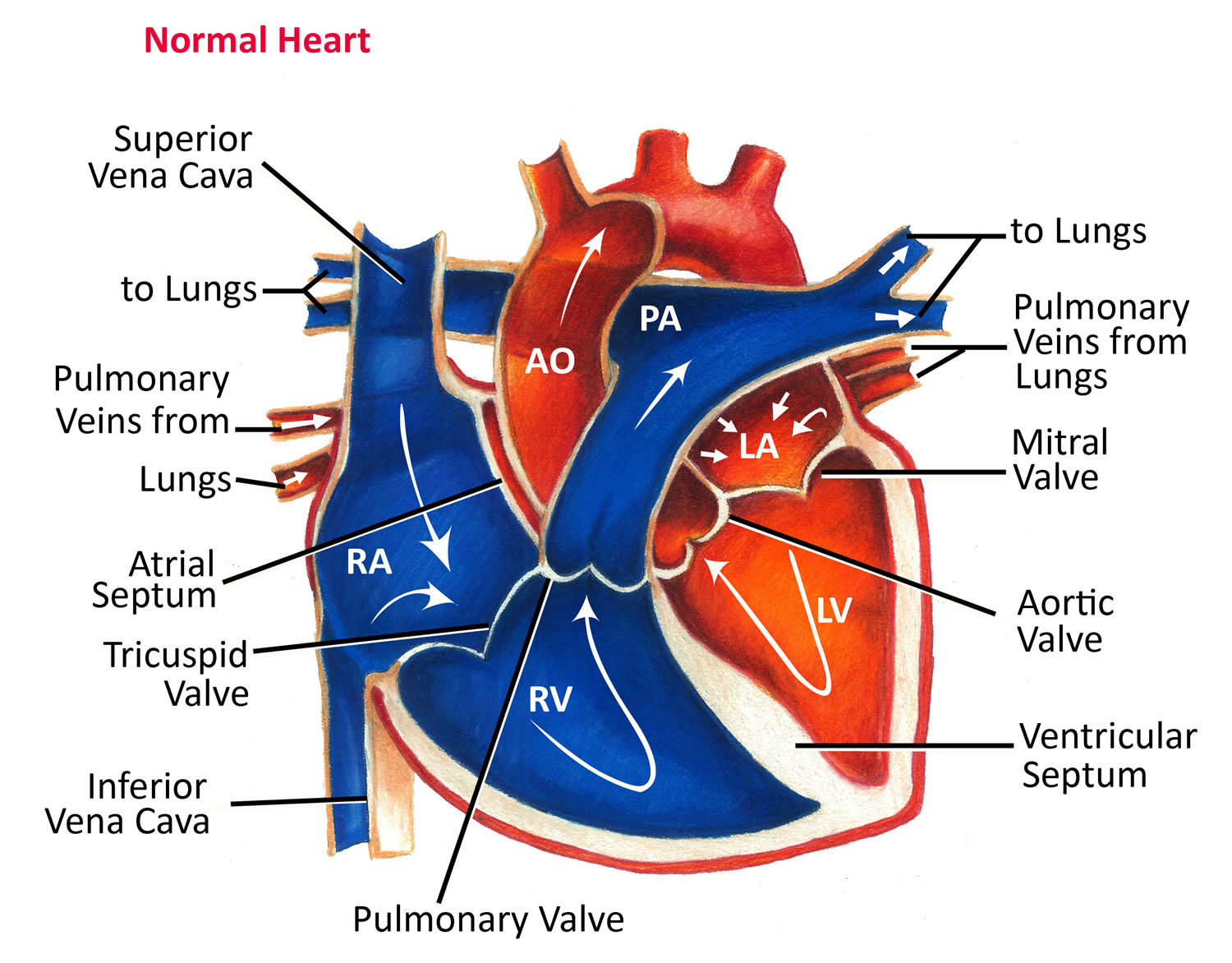
Your heart has four pumping chambers that circulate your blood:
- The right atrium. The upper right chamber (right atrium) receives oxygen-poor blood from your body and pumps it into the right ventricle through the tricuspid valve.
- The right ventricle. The lower right chamber (right ventricle) pumps the blood through a large vessel called the pulmonary artery and into the lungs, where the blood is resupplied with oxygen and carbon dioxide is removed from the blood. The blood is pumped through the pulmonary valve, which closes when the right ventricle relaxes between beats.
- The left atrium. The upper left chamber (left atrium) receives the oxygen-rich blood from the lungs through the pulmonary veins and pumps it into the left ventricle through the mitral valve.
- The left ventricle. The lower left chamber (left ventricle) pumps the oxygen-rich blood through a large vessel called the aorta and on to the rest of the body. The blood passes through the aortic valve, which also closes when the left ventricle relaxes.
Baby’s heart in the womb
Because a baby in the womb isn’t breathing, the lungs aren’t functioning yet. That means there’s no need to pump blood to the lungs. At this stage, it’s more efficient for blood to bypass the lungs and use a different route to circulate oxygen-rich blood from the mother to the baby’s body.
The umbilical cord delivers oxygen-rich blood to the baby’s right atrium. Most of this blood travels through the foramen ovale and into the left atrium. From there the blood goes to the left ventricle, which pumps it throughout the body. Blood also travels from the right atrium to the right ventricle, which also pumps blood to the body via another bypass system.
Newborn baby’s heart
When a baby’s lungs begin functioning, the circulation of blood through the heart changes. Now the oxygen-rich blood comes from the lungs and enters the left atrium. At this point, blood circulation follows the normal circulatory route.
The pressure of the blood pumping through the heart usually forces the flap opening of the foramen ovale closed. In most people, the opening fuses shut, usually sometime during infancy. No blood can flow between them. If a patent foramen ovale exists, a little blood can flow between the atria, the right and the left atrium. This hole is normal in the heart before birth, as part of the fetal circulation. But in most people, it closes soon after birth. If it doesn’t close, you have a patent foramen ovale. A patent foramen ovale is often discovered during tests for other problems. Learning that you have a patent foramen ovale is understandably concerning, but most people never need treatment for this disorder.
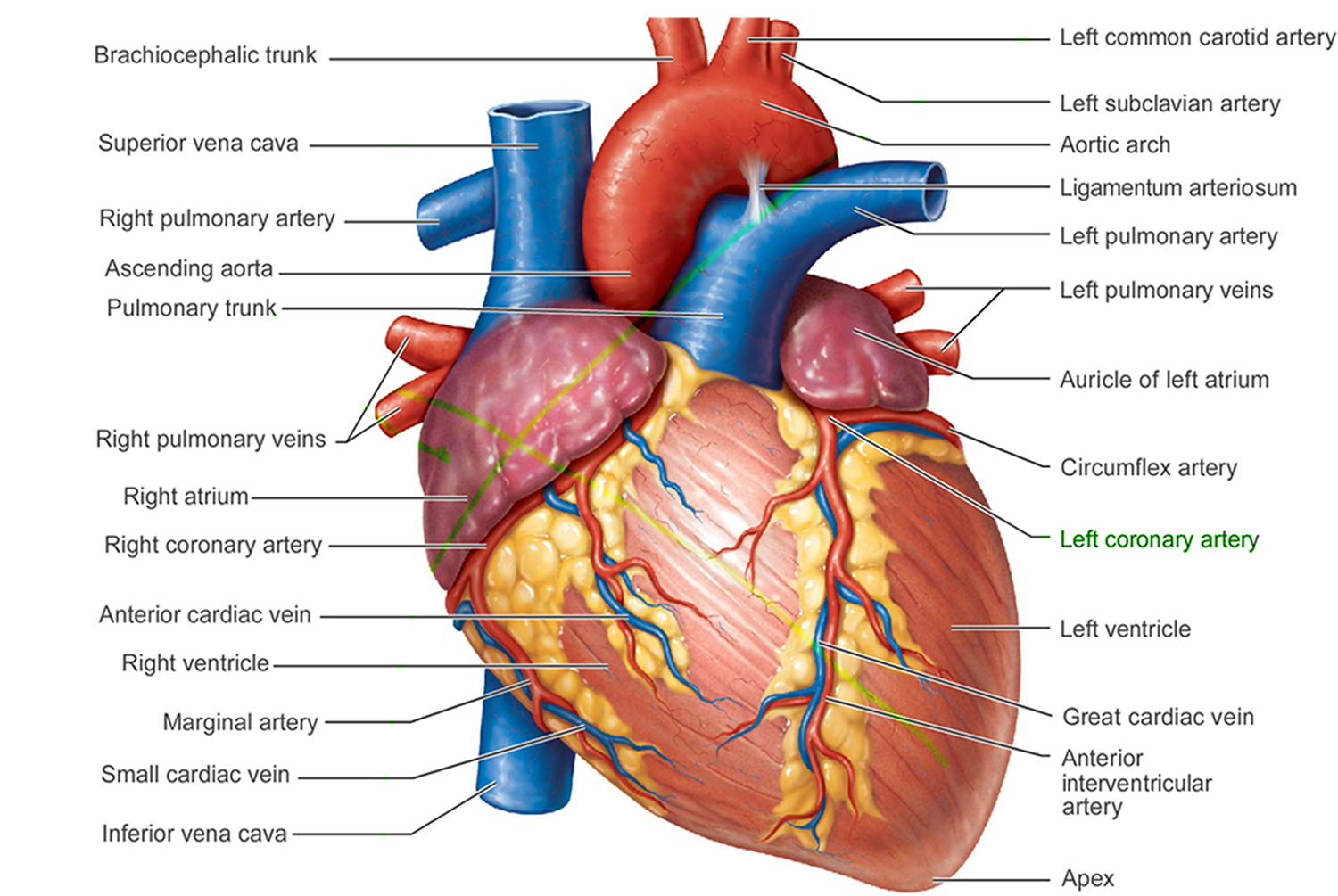
Figure 1. The anatomy of the heart
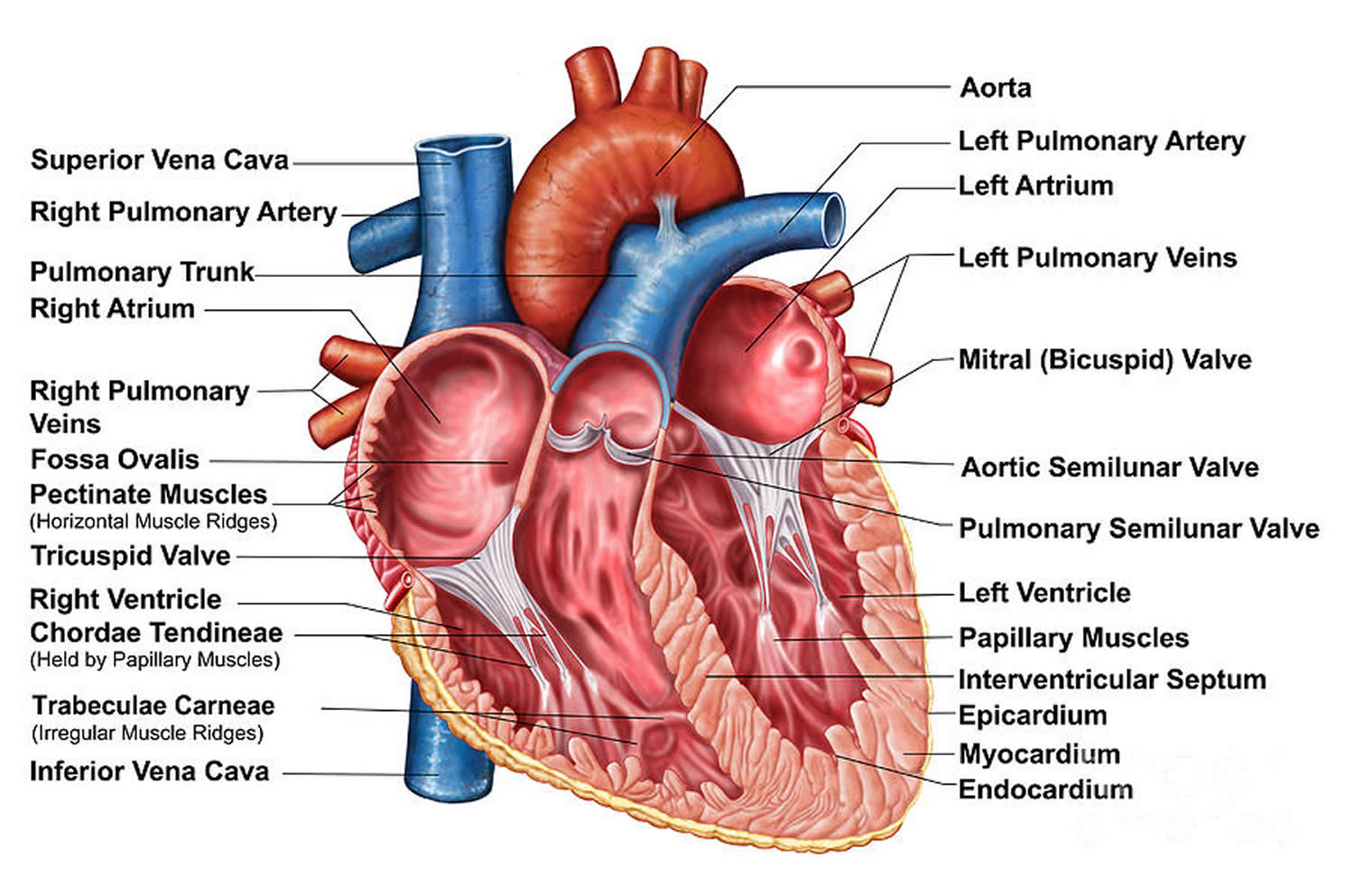
Figure 2. The anatomy of the heart chambers
Figure 3. Normal heart blood flow
Patent foramen ovale causes
A foramen ovale allows blood to go around the lungs. A baby’s lungs are not used when it grows in the womb, so the hole does not cause problems in an unborn infant.
The opening is supposed to close soon after birth, but sometimes it does not. In about 1 out of 4 people (25 percent), the opening never closes. If it does not close, it is called a patent foramen ovale.
The cause of a patent foramen ovale is unknown. There are no known risk factors, though genetics may play a role.
Patent foramen ovale complications
Generally, a patent foramen ovale doesn’t cause complications. But some studies have found the disorder is more common in people with certain conditions, such as unexplained strokes called paradoxical thromboembolic stroke and migraines with aura. In a paradoxical stroke, a blood clot that develops in a vein (often leg veins) breaks free and travels to the right side of the heart. Normally, this clot would then continue to the lungs, but in someone with a patent foramen ovale, the clot could pass through the hole to the left side of the heart. It may then be pumped out to the body, travel to the brain and become stuck there, preventing blood flow to that part of the brain (stroke).
In most cases, there are other reasons for these neurologic conditions, and it’s just a coincidence the person also has a patent foramen ovale.
The possible link between a patent foramen ovale and a stroke or migraine is controversial, and research studies are ongoing.
In rare cases a patent foramen ovale can cause a significant amount of blood to bypass the lungs, resulting in low blood oxygen levels (hypoxemia).
In decompression illness, which can occur in scuba diving, an air blood clot can travel through a patent foramen ovale.
In some cases, other heart defects may be present in addition to a patent foramen ovale.
Patent foramen ovale symptoms
Infants with a patent foramen ovale and no other heart defects do not have symptoms.
Most people with a patent foramen ovale don’t know they have it, because it’s usually a hidden condition that doesn’t create signs or symptoms.
Patent foramen ovale diagnosis
A doctor trained in heart conditions (cardiologist) may order one or more of the following tests to diagnose a patent foramen ovale:
Echocardiogram
An echocardiogram shows the anatomy, structure and function of your heart.
A common type of echocardiogram is called a transthoracic echocardiogram. In this test, sound waves directed at your heart from a wandlike device (transducer) held on your chest produce video images of your heart in motion. Doctors may use this test to diagnose a patent foramen ovale and detect other heart problems.
Variations of this procedure may be used to identify patent foramen ovale, including:
- Color flow Doppler. When sound waves bounce off blood cells moving through your heart, they change pitch. These characteristic changes (Doppler signals) and computerized colorization of these signals can help your doctor examine the speed and direction of blood flow in your heart. If you have a patent foramen ovale, a color flow Doppler echocardiogram could detect the flow of blood between the right atrium and left atrium.
- Saline contrast study (bubble study). With this approach, a sterile salt solution is shaken until tiny bubbles form and then is injected into a vein. The bubbles travel to the right side of your heart and appear on the echocardiogram. If there’s no hole between the left atrium and right atrium, the bubbles will simply be filtered out in the lungs. If you have a patent foramen ovale, some bubbles will appear on the left side of the heart. The presence of a patent foramen ovale may be difficult to confirm by a transthoracic echocardiogram.
Transesophageal echocardiogram
Doctors may conduct another type of echocardiogram called a transesophageal echocardiogram to get a closer look at the heart and blood flow through the heart. In this test, a small transducer attached to the end of a tube is inserted down the tube leading from your mouth to your stomach (esophagus).
This is generally the most accurate available test for doctors to see a patent foramen ovale by using the ultrasound in combination with color flow Doppler or a saline contrast study.
Other tests
Your doctor may recommend additional tests if you’re diagnosed with a patent foramen ovale and you have had a stroke. Your doctor may also refer you to a doctor trained in brain and nervous system conditions (neurologist).
Patent foramen ovale treatment
Most people with a patent foramen ovale don’t need treatment. In certain circumstances, however, your doctor may recommend that you or your child have a procedure to close the patent foramen ovale.
Reasons for closure
If a patent foramen ovale is found when an echocardiogram is done for other reasons, a procedure to close the opening usually isn’t performed. Procedures to close the patent foramen ovale may be done in certain circumstances, such as to treat low blood oxygen levels linked to the patent foramen ovale.
Closure of a patent foramen ovale to prevent migraines isn’t currently recommended. Closure of a patent foramen ovale to prevent a stroke remains controversial.
In some cases, doctors may recommend closure of the patent foramen ovale in individuals who have had recurrent strokes despite medical therapy, when no other cause has been found.
In a systematic review and meta-analysis with data from 20 studies and 6961 patients 1, demonstrated that in patients with a patent foramen ovale who had a cryptogenic ischemic stroke, patent foramen ovale closure was associated with a significantly lower incidence of the composite outcome of ischemic stroke, transient ischemic attack (TIA) or all-cause death as compared with medical therapy (moderate-quality evidence), mainly driven by protection against recurrent ischemic stroke. However, the same study showed patent foramen ovale closure increased the risks for atrial fibrillation or atrial flutter [most was periprocedure] (high-quality evidence) and pulmonary embolism (moderate-quality evidence) 1. The risks for transient ischemic attack (TIA), all-cause death, major bleeding and any serious adverse events were not different.
In the setting of patent foramen ovale and concurrent deep venous thrombosis (DVT) without cancer, in which patients are indicated to receive anticoagulant therapy (dabigatran, rivaroxaban, apixaban, or edoxaban over vitamin K antagonist), the most recent 2014 American Heart Association (AHA) and American Stroke Association guideline recommended that patent foramen ovale closure might be considered, depending on the risk of recurrent DVT 2. It is important to realize that the American Heart Association guideline was written when the current evidence was yet not available. Based on the updated evidence from randomized trials and meta-analysis, patent foramen ovale closure might be an alternative in young patients with patent foramen ovale and cryptogenic stroke without DVT, particular in but not limited to those concomitant with the presence of an atrial septal aneurysm or large shunt size 1. Whether benefits of closure would be achieved in other subgroup populations awaits further study. It is important to take into account the benefits in reducing risks for stroke but also the harm in increasing pulmonary embolism.
Surgical and other procedures for closure
Procedures to close a patent foramen ovale include:
- Device closure. Using cardiac catheterization, doctors can insert a device that plugs the patent foramen ovale. In this procedure, the device is on the end of a long flexible tube (catheter). The doctor inserts the device-tipped catheter into a vein in the groin and guides the device into place with the imaging assistance of an echocardiogram. Although complications are uncommon with this procedure, a tear of the heart or blood vessels, dislodgement of the device, or the development of irregular heartbeats may occur.
- Surgical repair. A surgeon can close the patent foramen ovale by opening up the heart and stitching shut the flap-like opening. This procedure can be conducted using a very small incision and may be performed using robotic techniques. If you or your child is undergoing surgery to correct another heart problem, your doctor may recommend that you have the patent foramen ovale corrected surgically at the same time. Research is ongoing to determine the benefits of closing the patent foramen ovale during heart surgery to correct another problem.
Stroke prevention
Medications can be used to try to reduce the risk of blood clots crossing a patent foramen ovale. Antiplatelet therapy such as aspirin or clopidogrel (Plavix) and other blood thinning medications (anticoagulants) — such as warfarin (Coumadin, Jantoven), dabigatran (Pradaxa), apixaban (Eliquis) and rivaroxaban (Xarelto) — may be helpful for people with a patent foramen ovale who’ve had a stroke.
It’s not clear whether medications or procedures to close the defect are most appropriate for stroke prevention in people with a patent foramen ovale. Studies are ongoing to answer this question.
Home remedies
If you know you have a patent foramen ovale, but don’t have symptoms, you probably won’t have any restrictions on your activities.
If you’ll be traveling long distances, it’s important to follow recommendations for preventing blood clots. If you’re traveling by car, stop periodically and go for a short walk. On an airplane, be sure to stay well-hydrated and walk around whenever it’s safe to do so.
- Zhang X-L, Kang L-N, Wang L, Xu B. Percutaneous closure versus medical therapy for stroke with patent foramen Ovale: a systematic review and meta-analysis. BMC Cardiovascular Disorders. 2018;18:45. doi:10.1186/s12872-018-0780-x. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5834900/[↩][↩][↩]
- Kernan WN, Ovbiagele B, Black HR, Bravata DM, Chimowitz MI, Ezekowitz MD, et al. Guidelines for the prevention of stroke in patients with stroke and transient ischemic attack: a guideline for healthcare professionals from the American Heart Association/American Stroke Association. Stroke. 2014;45:2160–2236. doi: 10.1161/STR.0000000000000024 http://stroke.ahajournals.org/content/45/7/2160.long[↩]