Contents
What is pityriasis rosea
Pityriasis rosea is a self-limited viral skin rash that goes away on its own within about 6–12 weeks even without treatment. However, pityriasis rosea often leaves behind patches of lighter (hypopigmented) or darker (hyperpigmented) skin, which are more obvious in darker-skinned people and may take months to return to normal color. Second attacks of pityriasis rosea are uncommon (1–3%), but another viral infection may trigger recurrence years later.
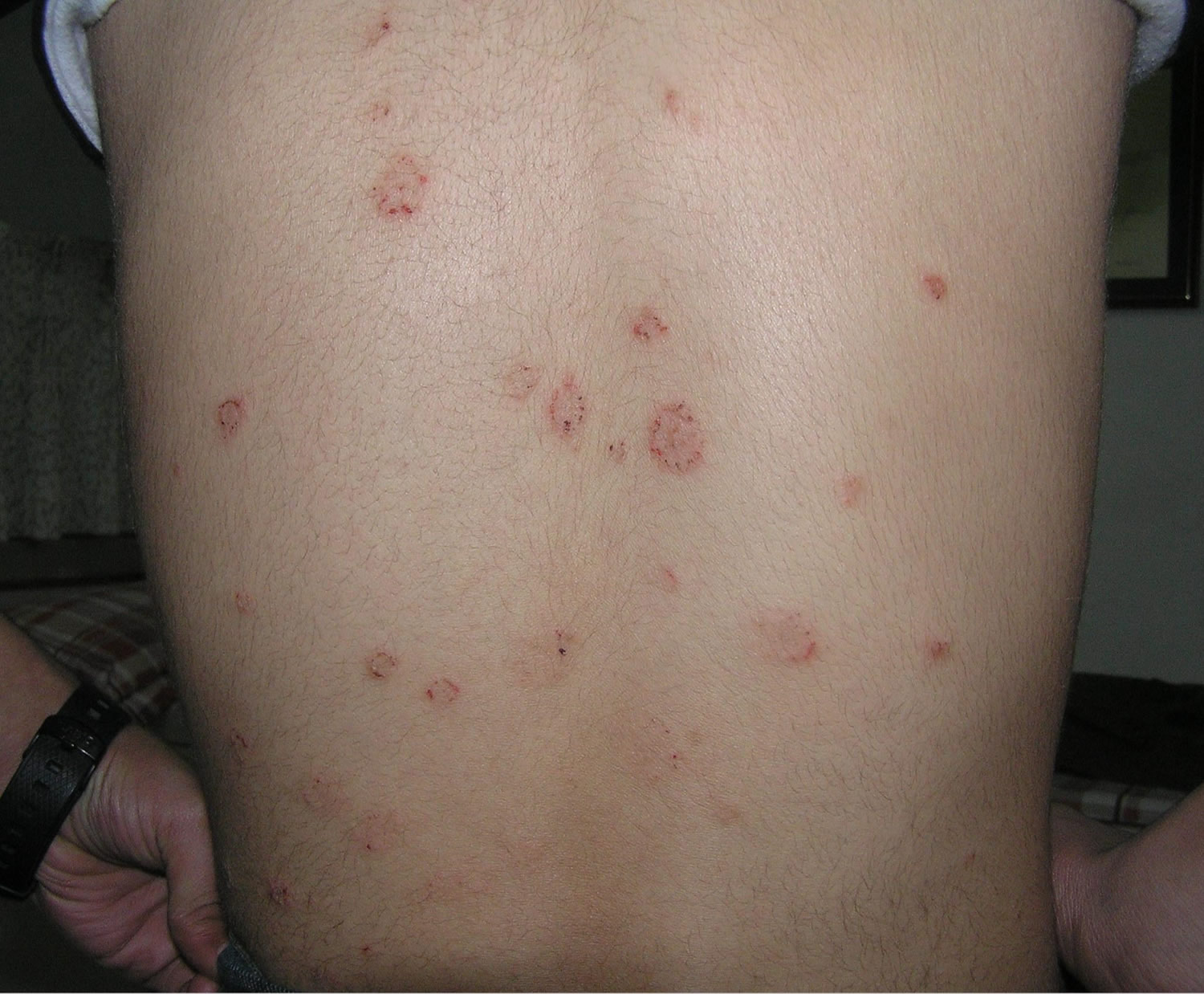
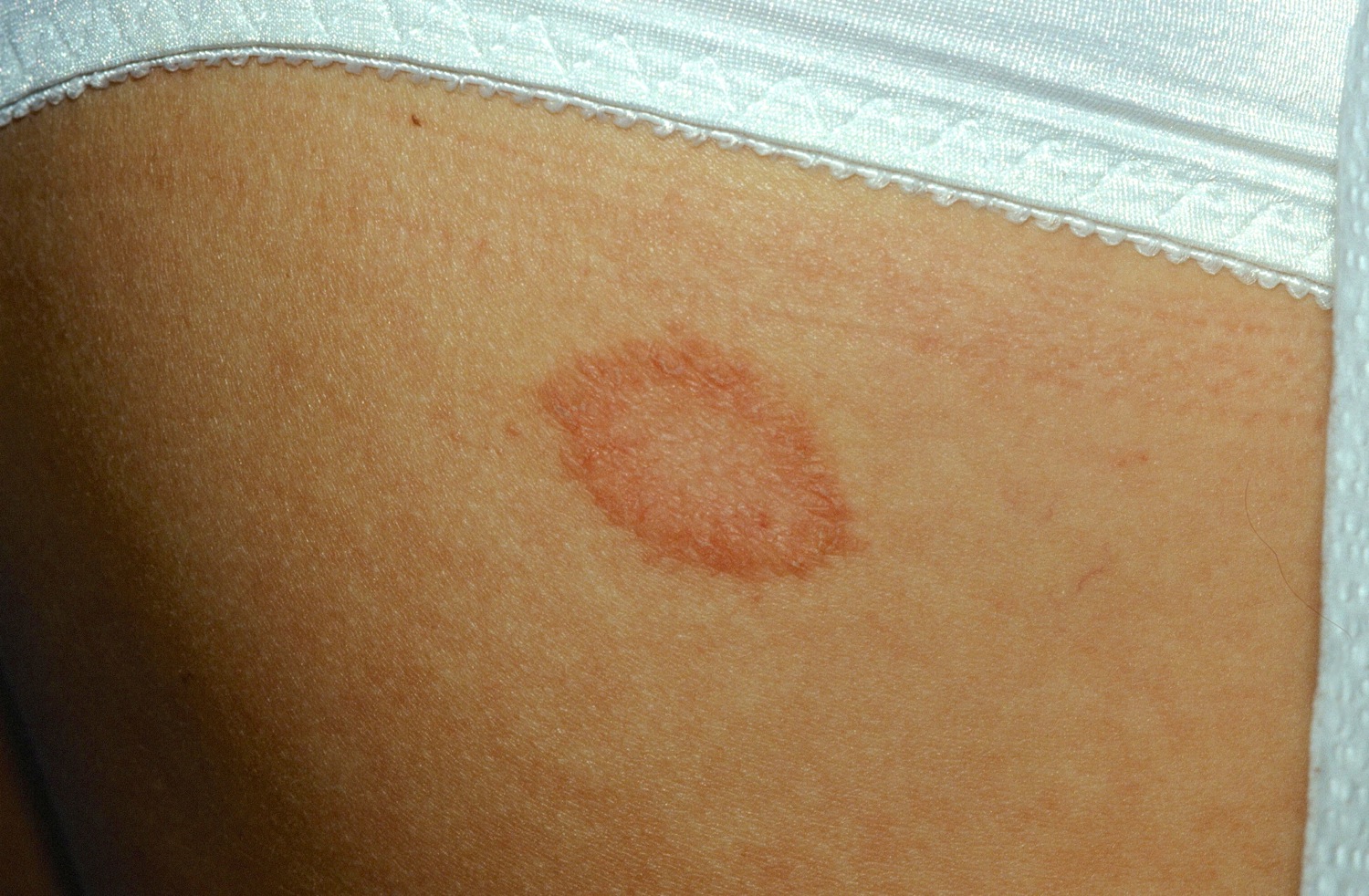
Pityriasis rosea is characterized by a herald patch followed by similar, smaller oval red patches that are located mainly on the chest and back. The herald patch is a larger papulosquamous plaque that precedes the eruption of pityriasis rosea in about half of the cases (Figure 1). After a time, lesions may clear in the center.
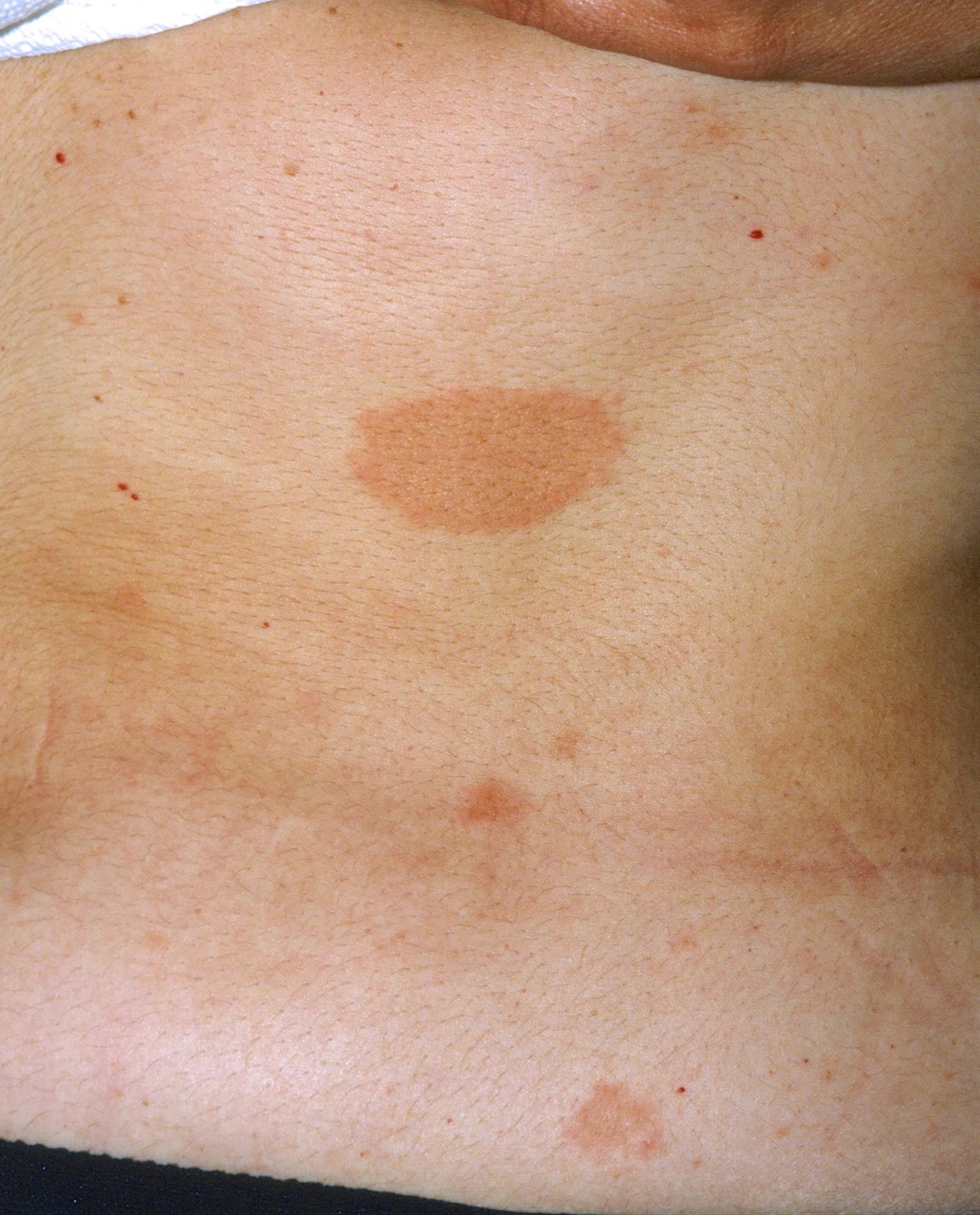
The pityriasis rosea herald patch is a single plaque that appears 1–20 days before the generalized rash of pityriasis rosea. Pityriasis rosea herald patch is an oval pink or red plaque 2–10 cm in diameter, with a scale trailing just inside the edge of the lesion like a collaret. Usually, the long axis of the plaques runs parallel to the ribs giving a Christmas tree pattern.
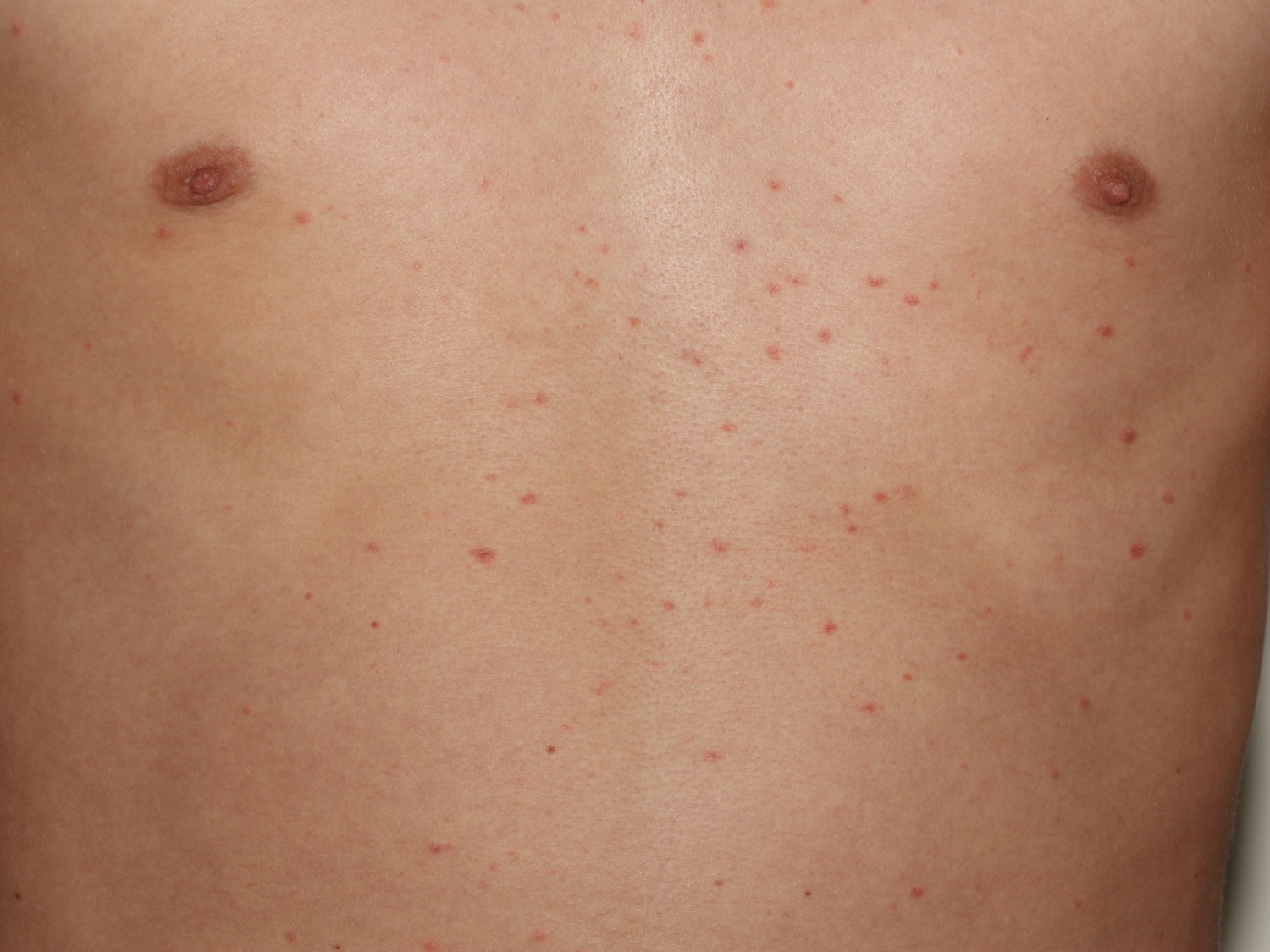
A few days to 2 weeks later, a more widespread pityriasis rosea rash develops, which may continue to spread over the following 2 to 6 weeks. It consists of smaller raised scaly patches that usually range in size from 0.5cm to 1.5cm. Most people get many pityriasis rosea rash patches across their chest, back, tummy, neck, upper arms and upper thighs. Pityriasis rosea does not like the sun. Pityriasis rosea likes the “hidden” areas (e.g., axilla, groin) and this is a helpful diagnostic sign. The palms and soles are usually spared (as compared to secondary syphilis where they are usually involved). The face is usually unaffected.
In light-skinned people, the patches are usually a pinkish-reddish color. In dark-skinned people, the patches can sometimes be grey, dark brown or black.
Pityriasis rosea can occur in people of any age, any race, and either sex, but it is most common in teenagers and young adults (10–40 years old), seventy-five percent of patients are from 10 to 35 years of age. Pityriasis rosea is uncommon in children younger than 5 years old.
Many people with pityriasis rosea have no other symptoms, but the rash sometimes follows a few days after a upper respiratory viral infection (cough, cold, sore throat or similar). Prodromal symptoms of headache and/or malaise may be elicited in some patients, but whether this occurs any more commonly than in controls is not proven.
There is no internal involvement, but oral lesions (exanthema) may occur 1. Typical are erythematous macules and papules, vesicles and petechiae especially of the palate. Pityriasis rosea is somewhat more common in the winter. Most cases occur in isolation, but occasionally there will be two family members affected. Various drugs have been reported to have caused a pityriasis rosea-like eruption, but it is highly unlikely that a drug can cause the classic presentation of a herald patch followed by secondary lesions.
Is pityriasis rosea contagious?
Pityriasis rosea isn’t contagious and can’t be spread to other people through physical contact.
Atypical pityriasis rosea
Pityriasis rosea is said to be atypical when diagnosis has been difficult. Atypical pityriasis rosea may be diagnosed when the rash has features such as:
- Atypical morphology, eg papules (small bumps), vesicles (blisters), urticated plaques (weal-like), purpura (bruising), target lesions (erythema multiforme-like)
- Large size or confluent plaques
- Unusual distribution of skin lesions, e.g., inverse pattern, with prominent involvement of the skin folds (armpits and groin), or greater involvement of limbs than the trunk
- Involvement of mucosal sites, e.g., mouth ulceration
- Solitary herald patch without generalized rash
- Multiple herald patches
- Absence of herald patch
- Large number of plaques
- Severe itch
- Prolonged course of disease
- Multiple recurrences
See your doctor if you have an unexplained rash. They’ll usually be able to confirm whether it’s pityriasis rosea, or another skin condition such as eczema, psoriasis or ringworm.
If your doctor is uncertain, they may refer you to a skin specialist (dermatologist).
What does pityriasis rosea look like
Figure 1. Pityriasis rosea herald patch
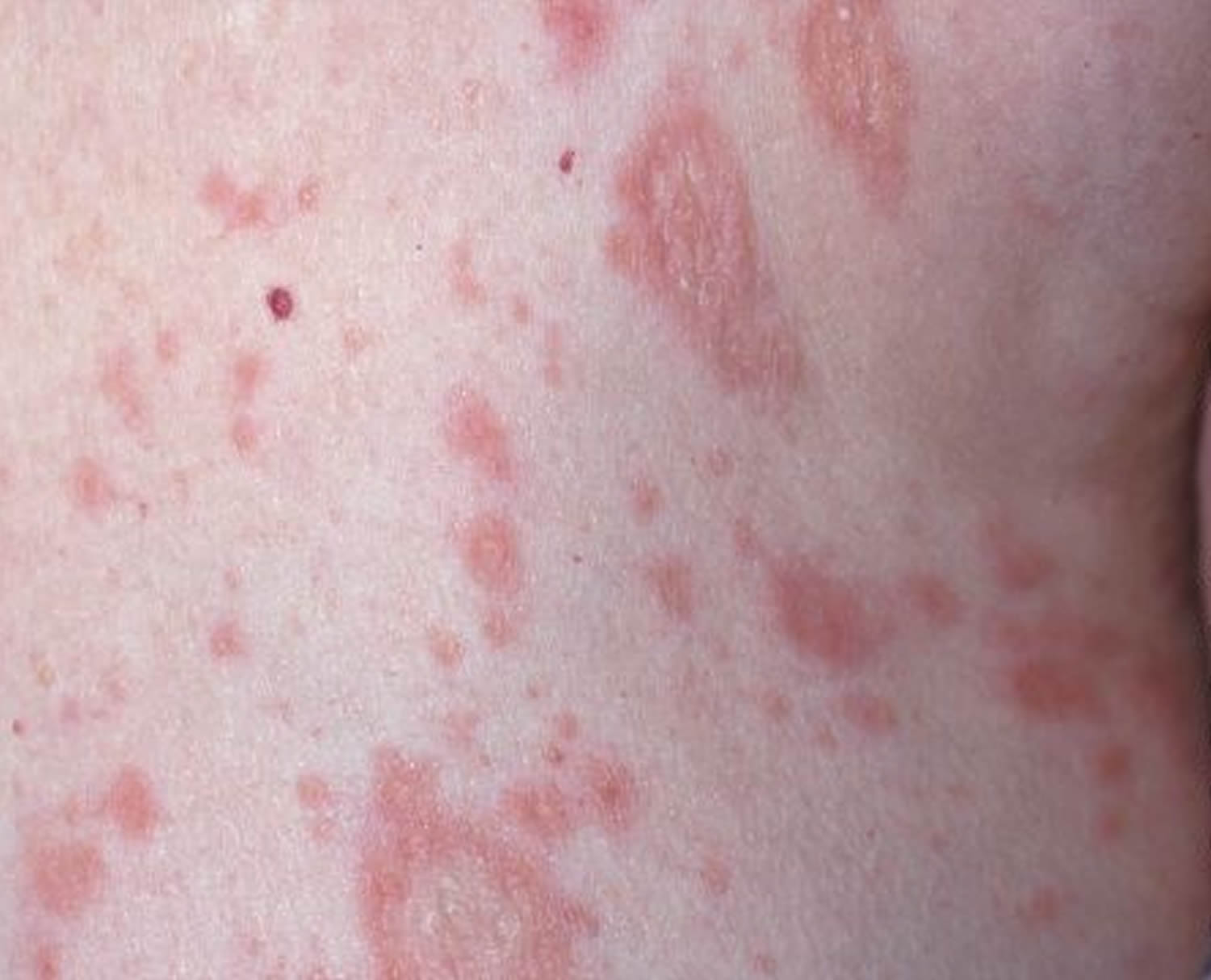
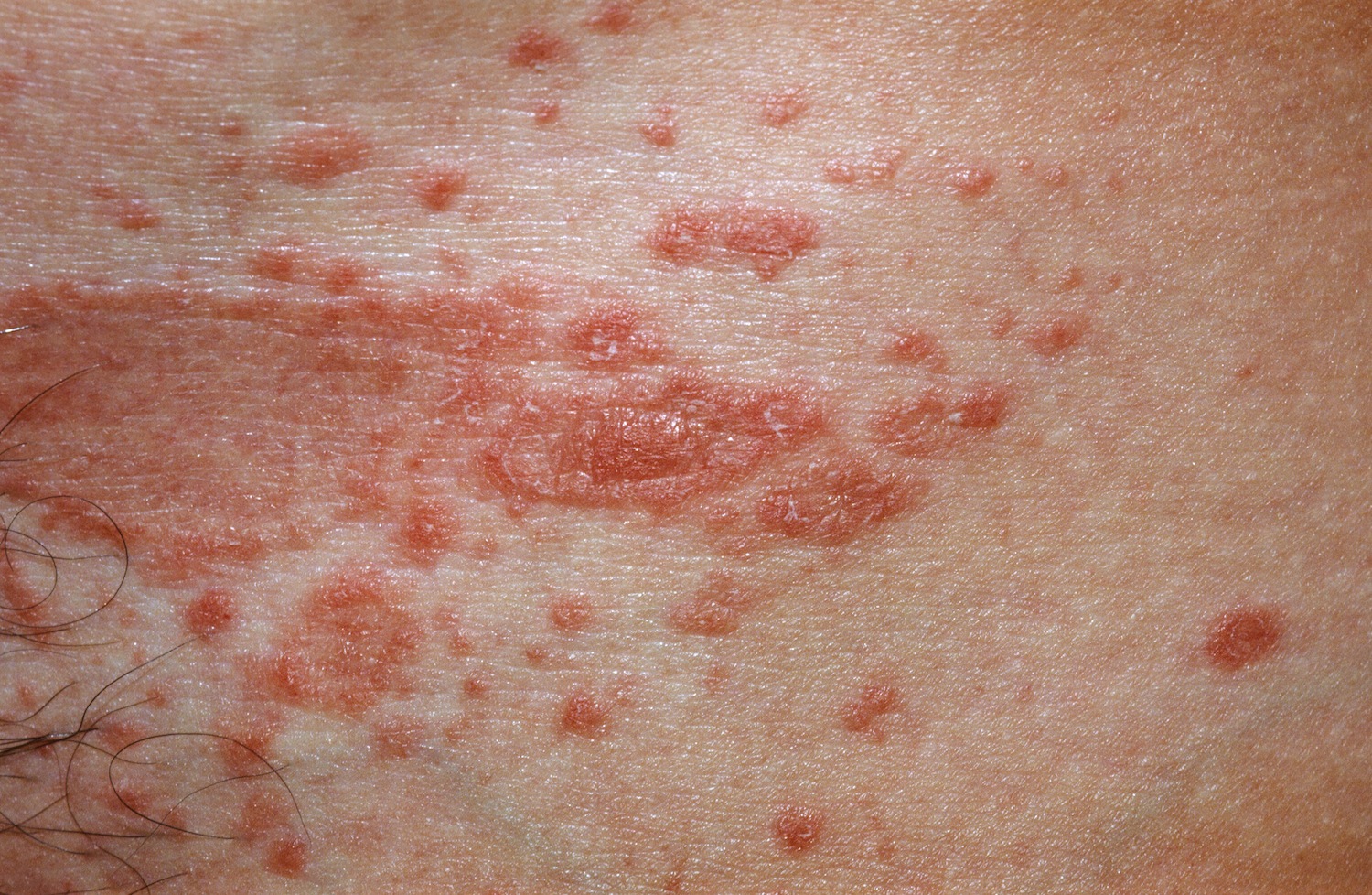
Figure 2. Pityriasis rosea rash (secondary rash)
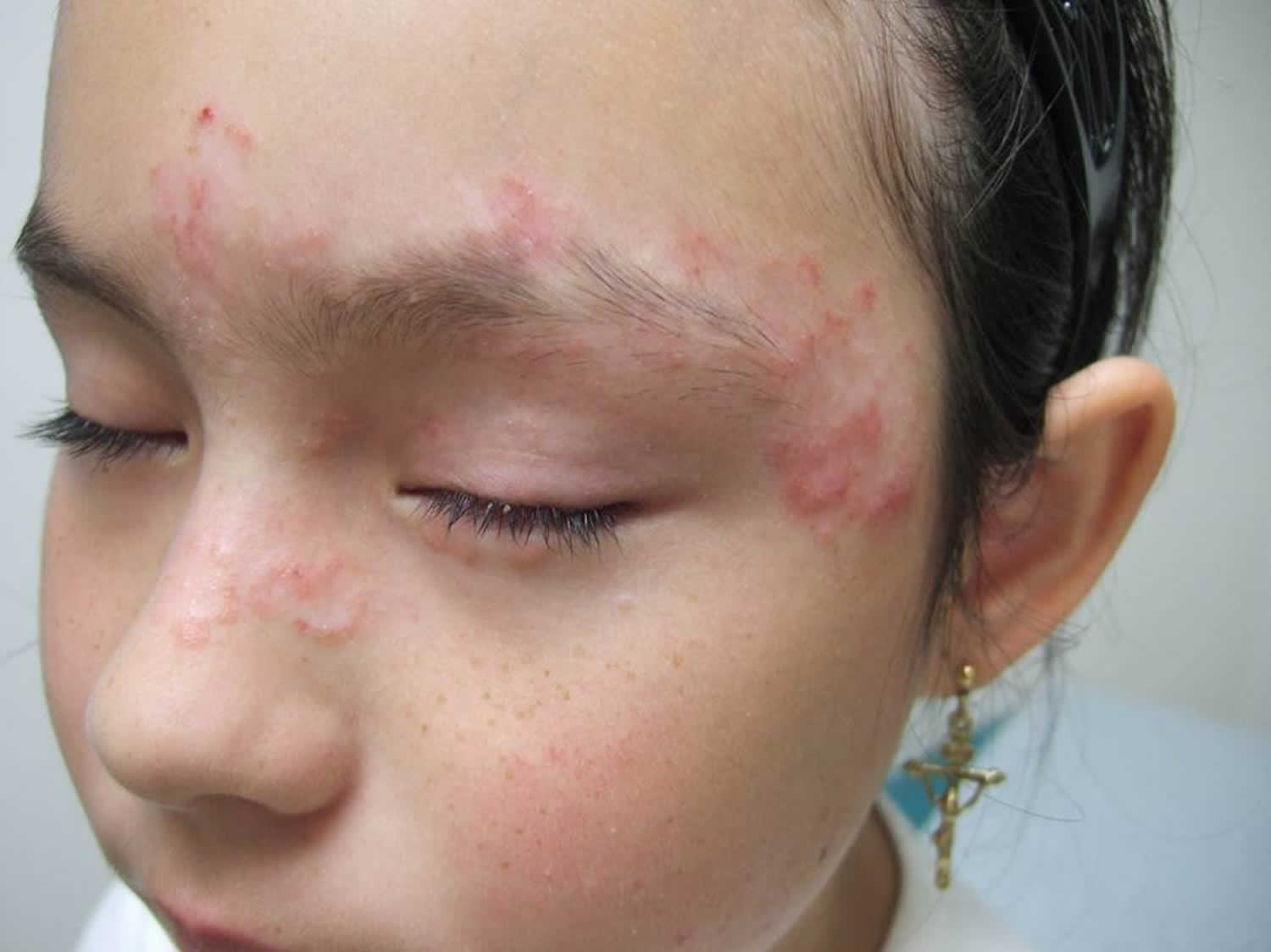
Figure 3. Pityriasis rosea on face
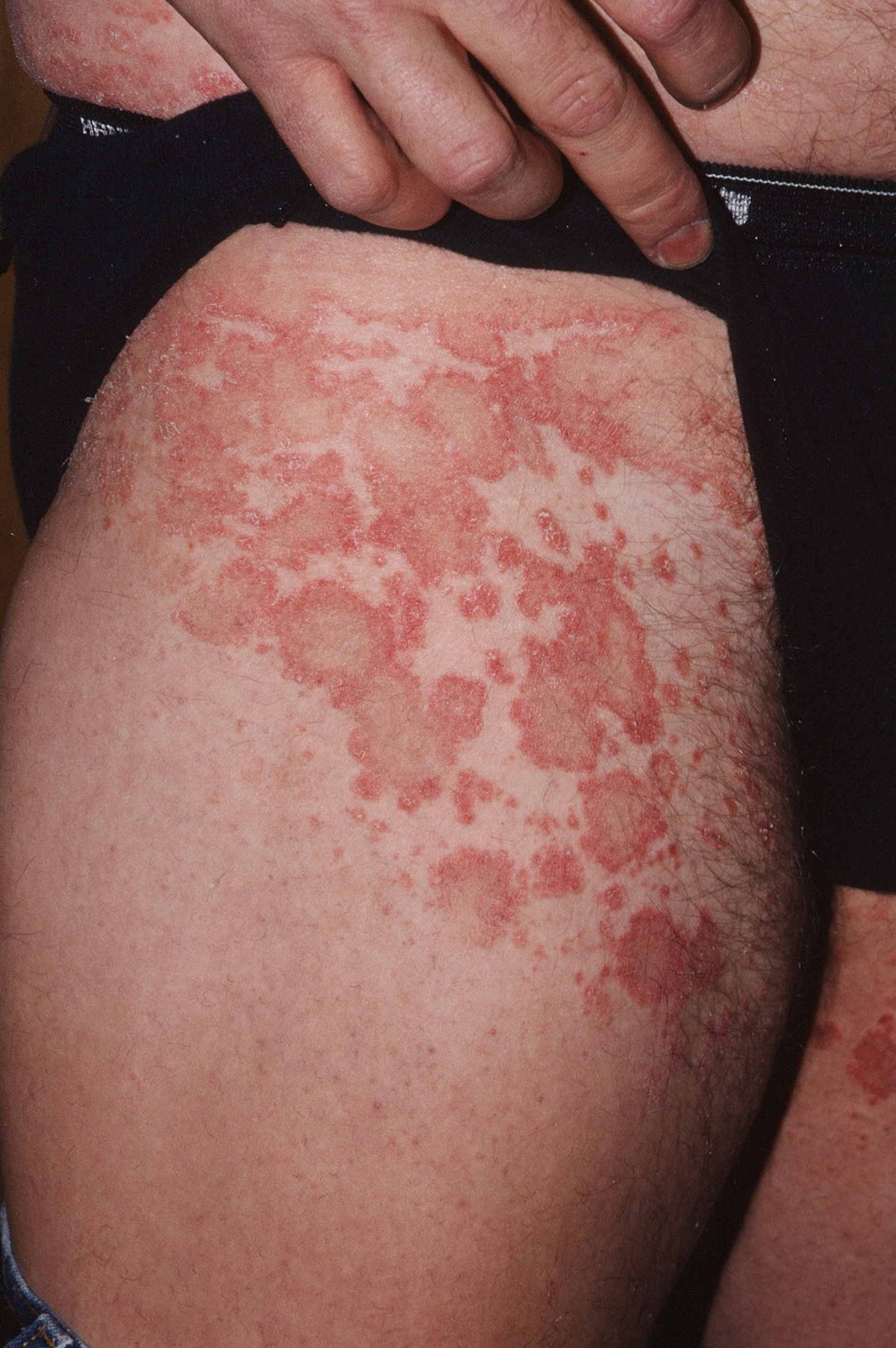
Figure 4. Pityriasis rosea rash groin/inner thigh
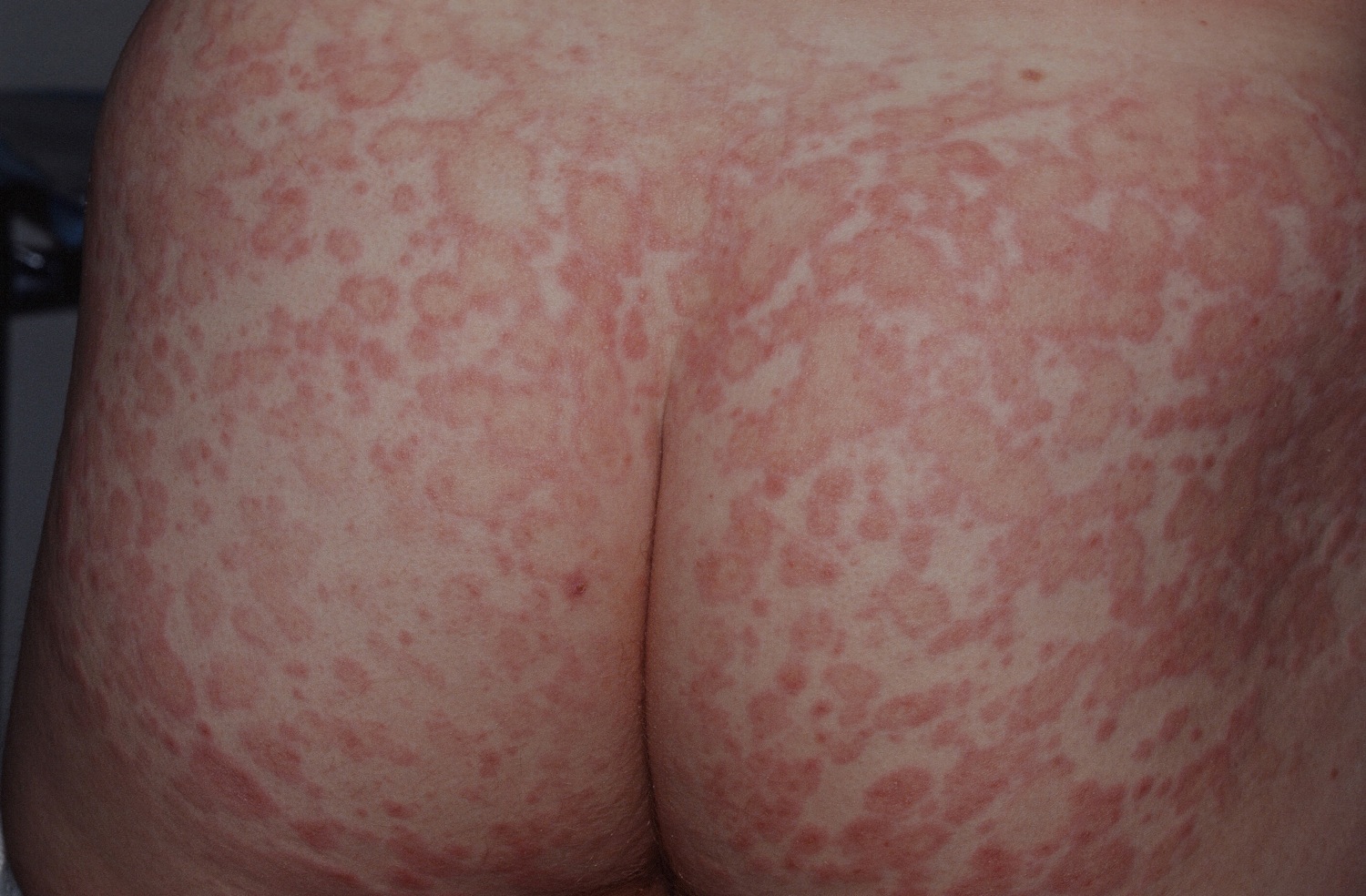
Figure 5. Pityriasis rosea rash buttock
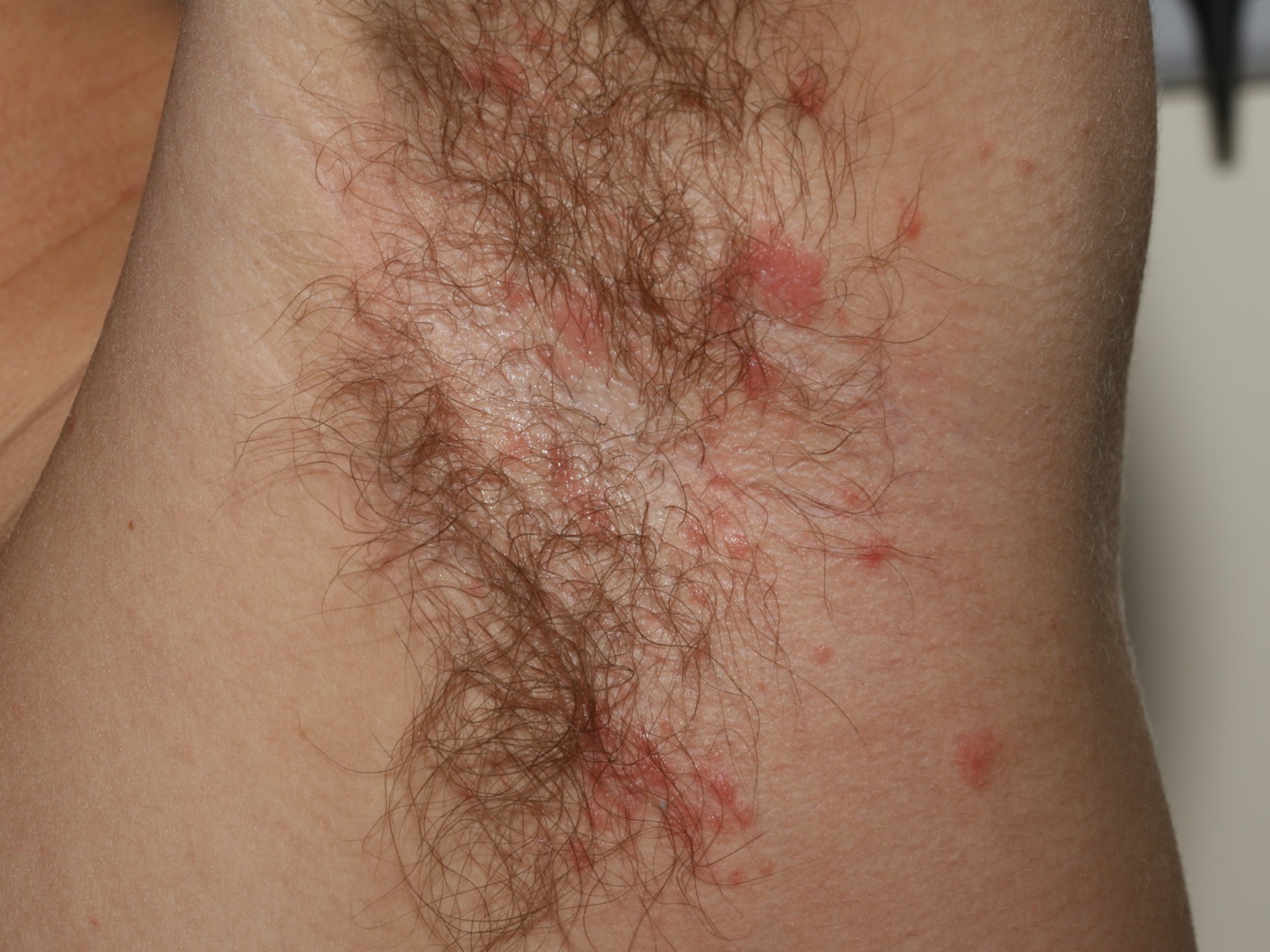
Figure 6. Pityriasis rosea rash armpit
Pityriasis rosea stages
Pityriasis rosea usually begins with a single patch of pink-to-red, scaly skin, from 2–5 cm in size. This “herald patch” is usually located on the trunk, neck, or upper arms. The herald patch is followed 1–3 weeks later by the development of a widespread rash, with smaller (0.5–2 cm) oval patches of pink-to-red, scaly skin on the trunk and upper arms. The second rash may form a “Christmas tree” pattern on the back (Figure 2).
Children sometimes have an unusual form of pityriasis rosea with lesions on the face, wrists, and legs rather than on the trunk.
Some children report feeling mildly ill (headache, stuffy nose, muscle aches) for 1–2 weeks before the herald patch forms. Additionally, some children have itching with pityriasis rosea. Becoming overheated by exercising or taking a hot shower may increase itching or make the rash more apparent.
The most common locations for pityriasis rosea rash include:
- Chest
- Upper back
- Neck
- Abdomen
- Upper arms
- Thighs
In an uncommon type of pityriasis rosea, the rash may be concentrated in the armpits and groin or on the face, forearms, and shins.
Pityriasis rosea secondary rash
A few days after the appearance of the herald patch, more scaly patches (flat lesions) or plaques (thickened lesions) appear on the chest and back. A few plaques may also appear on the thighs, upper arms and neck but are uncommon on the face or scalp. These secondary lesions of pityriasis rosea tend to be smaller than the herald patch. They are also oval in shape with a dry surface. Like the herald patch, they may have an inner collaret of scaling. Some plaques may be annular (ring-shaped).
Pityriasis rosea plaques usually follow the relaxed skin tension or cleavage lines (Langers lines) on both sides of the upper trunk. The rash has been described as looking like a fir tree. It does not involve the face, scalp, palms or soles.
Pityriasis rosea may be very itchy, but in most cases it doesn’t itch at all.
Recurrent pityriasis rosea
Recurrent pityriasis rosea and its association with oral ulcers and herald patches for each episode in different locations has been reported 2. However, another study 3, found that the herald patch was always absent, the size and number of the lesions were reduced, and duration was shorter than that of the primary episodes. Constitutional symptoms were present, though less severe than in the primary eruption. Most recurrences occurred within 1 year (16/21, 76.2%). Reactivation of human herpesvirus 6/7, as with other human herpesviruses (varicella zoster virus and Epstein-Barr virus), is proposed.
Persistant pityriasis rosea
In one study of pityriasis rosea that lasted longer than 12 weeks, a persistent reactivation of human herpesvirus-6 and/or human herpesvirus-7 with higher viral loads than in typical pityriasis rosea was found 4. Cases of persistent pityriasis rosea tended to have more frequent and more severe systemic symptoms as well as oral lesions 4.
Pityriasis rosea complications
Pityriasis rosea during early pregnancy has been reported to cause miscarriage in 8 of 61 women studied. Premature delivery and other perinatal problems also occurred in some women. When pityriasis rosea developed on or before the 15th gestational week, there has been reported an abortion rate on the order of 60% 5.
Atypical pityriasis rosea due to reactivation of herpes 6/7 in association with a drug can also lead to the severe cutaneous adverse reaction, drug hypersensitivity syndrome.
Pityriasis rosea causes
What causes pityriasis rosea
The exact cause of pityriasis rosea is unclear. Some evidence indicates the rash may be triggered by a viral infection, particularly by certain strains of the herpes virus. But it’s not related to the herpes virus that causes cold sores.
Pityriasis rosea is associated with reactivation of herpes viruses 6 and 7 6 , which cause the primary rash roseola in infants has being most strongly implicated. Influenza viruses and vaccines have triggered pityriasis rosea in some cases.
Pityriasis rosea and pityriasis rosea-like eruptions have occurred after vaccination. Some eruptions are similar to classic pityriasis rosea with a herald patch and prodromal symptoms. Others are pityriasis rosea-like and do not have prodromal symptoms nor a herald patch. These pityriasis rosea-like eruptions may also occur after drugs including captropril, barbiturates, and isotretinoin.
Pityriasis rosea or atypical pityriasis rosea-like rashes can rarely arise as an adverse reaction to a medicine. Reactivation of herpes 6/7 is reported in some but not all cases of drug-induced pityriasis rosea. Pityriasis-rosea like drug eruptions have been caused by angiotensin-converting enzyme inhibitors, nonsteroidal anti-inflammatory drugs, hydrochlorothiazide, imatinib, clozapine, metronidazole, terbinafine, gold and atypical antipsychotics.
Pityriasis rosea symptoms
Pityriasis rosea typically begins with a large, slightly raised, scaly patch — called the herald patch — on your back, chest or abdomen. Before the herald patch appears, some people experience headache, fatigue, fever, joint pain or sore throat.
Pityriasis rosea diagnosis
The diagnosis of pityriasis rosea is usually made clinically, but may be supported by the finding of a subacute dermatitis on histopathology of a skin biopsy. Eosinophils are typical of drug-induced pityriasis rosea. Blood testing for HHV6 (IgG or PCR) is not indicated because nearly 100% of individuals have been infected with the virus in childhood and existing commercial tests do not measure HHV6 activity.
Fungal scrapings are sometimes sent for mycology to exclude fungal infection (tinea corporis).
Although most people have the classic form of pityriasis rosea, some individuals develop a form of pityriasis rosea with unusual (atypical) features. These atypical types of pityriasis rosea may be more difficult to diagnose and may require a skin biopsy.
The procedure involves:
- Numbing the skin with an injectable anesthetic.
- Sampling a small piece of skin by using a flexible razor blade, a scalpel, or a tiny cookie cutter (called a “punch biopsy”). If a punch biopsy is taken, a stitch (suture) or two may be placed and will need to be removed 6–14 days later.
- Having the skin sample examined under the microscope by a specially trained physician (dermatopathologist).
In addition, the doctor may want to do blood tests for other medical conditions.
Proposed diagnostic criteria for pityriasis rosea 7
Essential clinical features
- Discrete circular or oval lesions
- Scaling on most lesions
- Peripheral collarette scaling with central clearance on >2 lesions
Optional clinical features
At least one of the following features should be present:
- Truncal and proximal limb distribution (<10% of lesions distal to mid-upper-arm and mid-thigh)
- Most lesions along skin cleavage lines
- Herald patch ≥2 days before other lesions
Pityriasis rosea treatment
Untreated, pityriasis rosea usually resolves spontaneously within 2-3 months although some cases may last 6 months. In asymptomatic patients, no active treatment is necessary. If itching is a problem, a topical steroid may be helpful.
If the condition persists beyond 4-6 months, return to your doctor for further evaluation. Such cases of chronic pityriasis rosea should be biopsied to exclude psoriasis, pityriasis lichenoides or other conditions.
Pityriasis rosea home remedies
The herald patch of pityriasis rosea may be mistaken for ringworm (tinea corporis), but over-the-counter antifungal creams do not improve it. Similarly, the herald patch may look like eczema, but over-the-counter hydrocortisone creams do not affect it. The second, widespread rash of pityriasis rosea will always develop even if the herald patch is treated.
Itching with pityriasis rosea can sometimes be reduced by:
- Expose skin to sunlight cautiously (without burning). Sunlight chases pityriasis rosea lesions away. The patient may expose his/her skin to the sun several times a week (don’t burn) or if necessary, receive light therapy (UVB) in the dermatologist’s office.
- Oatmeal baths. You can find oatmeal bath products at your pharmacy.
- Lukewarm (rather than hot) baths and showers
- Bathe or shower with plain lukewarm water and bath oil, aqueous cream, or other soap substitute.
- Take over-the-counter allergy medicine (antihistamines). These include diphenhydramine (Benadryl, others).
- Apply moisturizing creams to dry skin. Creams that moisturize and soothe the skin; some emollients can be used as soap and are often recommended because normal soap can irritate the rash; you can buy these over the counter from most pharmacists
- Topical menthol-phenol lotions
- Medium potency topical steroid (e.g. triamcinolone 0.1% cream) for the itch. Topical steroids only show modest benefit.
Other than relieving the itch, there are no self-care measures for pityriasis rosea. Although the rash should go away on its own within 6–12 weeks, see your child’s doctor for evaluation of any widespread rash.
Prescription treatments
Because pityriasis rosea is benign and self-limited, no treatment is required. However, some people with pityriasis rosea have mild-to-severe itching, and your physician may suggest the following medicines (used off-license) that have been reported to speed up clearance of pityriasis rosea:
- A 7-day course of high-dose aciclovir
- A 2-week course of oral erythromycin has also been reported to help, probably because of a nonspecific anti-inflammatory effect. Other studies have found that erythromycin and azithromycin are not effective in pityriasis rosea 8.
- Oral antihistamine pills
Topical steroid corticosteroid (cortisone) creams, lotions or ointment may reduce the itch while waiting for the rash to resolve.
Acyclovir
Drago et al in 2006 9 conducted a study of oral acyclovir (800 mg 5/day x 7 days) vs placebo in 87 patients, aged. He found on 2 week follow up, 79% of patients had fully regressed compared with 4% of the placebo group. Unfortunately, his study was neither randomized nor double blinded. Rassai et al in 2001 10 conducted a study of low dose acyclovir (400 mg 5day x 7 days) vs no treatment in a randomized, investigator-blinded study of 64 patients. They found resolution of lesions in 78% of acyclovir-treated vs 27% of placebo-treated patients at 2 weeks. Ganguly et al 11 in 2014 conducted a randomized, double-blinded, placebo controlled study of 73 patients with acyclovir 800 mg 5/day for 7 days vs placebo and found resolution of lesions on the 14th day in 87% of treated patients vs 33% of placebo-treated patients. Recently in 2016, Singh et al 12 published a smaller study of 27 patients in an randomized, blinded, placebo-controlled trial using acyclovir 800 mg 5/day x 7 days and complete clearing as the endpoint. They found no benefit to the use of acylovir. The number of days to cure was 27 in the placebo group and 33 days in the acyclovir group.
Of all the published studies, that by Ganguly et al 11 is the most robust, being randomized and double blinded. It does support the use of acyclovir in pityriasis rosea. Although the study by Singh et al gives contrary results, it is much smaller in size. It seems reasonable for more severe cases of pityriasis rosea to give acyclovir 800 mg 5/day x 7 days.
Phototherapy
Extensive or persistent cases can be treated by phototherapy (ultraviolet light, UVB).
- JAAD 2017;77;833[↩]
- Singapore Med J. 2014 Jan;55[↩]
- Dermatology. 2014;229(4):316-8[↩]
- Persistent pityriasis rosea: an unusual form of pityriasis rosea with persistent active HHV-6 and HHV-7 infection. Dermatology. 2015;230(1):23-6. doi: 10.1159/000368352. Epub 2015 Jan 16. https://www.karger.com/Article/Abstract/368352[↩][↩]
- J Am Acad Dermatology 71;198–199, July 2014[↩]
- J Invest Dermatol 124:1234 –1240, 2005[↩]
- Zawar V, Chuh A. Applicability of proposed diagnostic criteria of pityriasis rosea: results of a prospective case-control study in India. Indian J Dermatol. 2013 Nov;58(6):439-42. doi: 10.4103/0019-5154.119950. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3827514/[↩]
- Drago F, Ciccarese G, Rebora A, Parodi A. The efficacy of macrolides and acyclovir in pityriasis rosea. Indian J Dermatol Venereol Leprol 2015;81:56[↩]
- JAAD 2006;54:82[↩]
- J Eur Acad Dermatol Venereol. 2011;25:24[↩]
- Ganguly S. A Randomized, Double-blind, Placebo-Controlled Study of Efficacy of Oral Acyclovir in the Treatment of Pityriasis Rosea. Journal of Clinical and Diagnostic Research : JCDR. 2014;8(5):YC01-YC04. doi:10.7860/JCDR/2014/8140.4360. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4080052/[↩][↩]
- Indian J Dermatol Venereol Leprol 2016;82:505[↩]