Contents
What is prehypertension
Prehypertension is a relatively new category of blood pressure identified by the Seventh Report of the Joint National Committee on Prevention, Detection, Evaluation, and Treatment of High Blood Pressure.
Prehypertension is defined as a systolic blood pressure of 120 to 139 mm Hg or a diastolic BP of 80 to 89 mm Hg.
| BLOOD PRESSURE CATEGORY | SYSTOLIC mm Hg (upper number) | DIASTOLIC mm Hg (lower number) | |
|---|---|---|---|
| Normal | LESS THAN 120 | and | LESS THAN 80 |
| PREHYPERTENSION | 120 – 139 | and | 80 – 89 |
| High Blood Pressure (Hypertension) Stage 1 | 140 – 159 | or | 90 – 99 |
| High Blood Pressure (Hypertension) Stage 2 | 160 OR HIGHER | or | 100 OR HIGHER |
| HYPERTENSIVE CRISIS (consult your doctor immediately) | HIGHER THAN 180 | and/or | HIGHER THAN 120 |
The only way to know (diagnose) if you have prehypertension is to have your blood pressure tested.
Your blood pressure reading is recorded as two numbers:
- Systolic blood pressure (the top number) — indicates how much pressure your blood is exerting against your artery walls during heartbeats (shown as the top number in a blood pressure reading).
- Diastolic blood pressure (the bottom number) — indicates how much pressure your blood is exerting against your artery walls while the heart is resting between beats (shown as the bottom number in a blood pressure reading).
If your blood pressure reading is higher than normal (120/80 mmHg):
Your doctor may take several readings over time and/or have you monitor your blood pressure at home before diagnosing you with prehypertension.
A single high reading does not mean that you have prehypertension. But, if your readings continue to stay high, your doctor will most likely want you to begin a treatment program.
Prehypertension may progress to hypertension and lead to heart diseases.
A recent study demonstrated that prehypertension is associated with a higher risk of developing myocardial infarction (heart attack) and coronary artery disease (when the arteries that supply blood to the heart muscle, called coronary arteries, become hardened and narrowed), but it was not shown in the study that there is an increased risk of developing stroke.
Prehypertension is a common condition. In the United States population aged 20 or greater, an estimated 41.9 million men and 27.8 million women have prehypertension. It is more common in men, and among certain ethnic groups (non-Hispanic White, African American, and Hispanic persons).
Just like hypertension, a majority of prehypertension has no known cause. In some patients, a cause may be identified, e.g. kidney diseases, hormonal diseases, hypertension in pregnancy, excessive alcohol intake.
Weight loss, exercise and other healthy lifestyle changes can often control and reverse prehypertension, and set the stage for a lifetime of better health.
Prehypertension outlook (prognosis)
The prognosis depends on whether the patient develops myocardial infarction (heart attack), coronary artery disease and stroke. Generally, a person with prehypertension blood pressure is 3.5 times more likely to have myocardial infarction and 1.7 times more likely to have coronary artery disease compared with someone with a normal blood pressure.
The risk of coronary artery disease with prehypertension is higher among people over 45 years. Men have twice the risk compared with women. In the presence of diabetes mellitus, smoking, obesity and high cholesterol level, the risk of heart diseases increases.
Prehypertension complications
Prehypertension itself doesn’t often have complications. If you have prehypertension, it’s likely to worsen and develop into high blood pressure (hypertension). The term “prehypertension” is often used by doctors to signal that it’s time to begin making lifestyle changes or, if you have certain conditions such as diabetes, to consider taking medications to stop your blood pressure from rising to definite high blood pressure.
High blood pressure can damage your organs and increase the risk of several conditions including heart attack, heart failure, stroke, aneurysms and kidney failure.
Prehypertension causes
Any factor that increases pressure against the artery walls can lead to prehypertension. Atherosclerosis, which is the buildup of fatty deposits in your arteries, can lead to high blood pressure. Sometimes an underlying condition causes blood pressure to rise. Possible conditions that can lead to prehypertension or high blood pressure include:
- Atherosclerosis
- Obstructive sleep apnea
- Kidney disease
- Adrenal disease
- Thyroid disease
Certain medications — including birth control pills, cold remedies, decongestants, over-the-counter pain relievers and some prescription drugs — also may cause blood pressure to temporarily rise. Illegal drugs, such as cocaine and amphetamines, can have the same effect.
Often, however, high blood pressure develops gradually over many years without a specific identifiable cause.
Risk factors for prehypertension
Risk factors for prehypertension include:
- Being overweight or obese. A primary risk factor is being overweight. The greater your body mass, the more blood you need to supply oxygen and nutrients to your tissues. As the volume of blood circulated through your blood vessels increases, so does the force on your artery walls.
- Age. Younger adults are more likely to have prehypertension than are older adults. Many older adults have progressed to high blood pressure, and the risk of high blood pressure increases as you age.
- Sex. Prehypertension is more common in men than in women. Through early middle age, or about age 45, high blood pressure is more common in men. Women are more likely to develop high blood pressure after age 65.
- Race. High blood pressure is particularly common among blacks, often developing at an earlier age than it does in whites.
- Family history of high blood pressure. High blood pressure tends to run in families. If a first-degree relative, such as a parent or sibling, has high blood pressure, you’re more likely to develop the condition.
- Not being physically active. Not exercising can increase your risk of high blood pressure and increase your risk of being overweight.
- Diet high in salt (sodium) or low in potassium. Sodium and potassium are two key nutrients in the way your body regulates your blood pressure. If you have too much sodium or too little potassium in your diet, you’re more likely to have high blood pressure.
- Tobacco use. Smoking cigarettes, chewing tobacco or even being around other people who are smoking (secondhand smoke) can increase your blood pressure.
- Drinking too much alcohol. Drinking more than two drinks a day if you’re a man age 65 or younger or more than one drink a day if you’re a woman of any age or a man older than age 65 can increase your blood pressure. One drink equals 12 ounces of beer, 5 ounces of wine or 1.5 ounces of 80-proof liquor.
- Certain chronic conditions. Certain chronic conditions — including kidney disease, diabetes and sleep apnea — may increase the risk of prehypertension.
Although prehypertension and high blood pressure are most common in adults, children may be at risk, too. For some children, high blood pressure is caused by problems with the kidneys or heart. But for a growing number of kids, poor lifestyle habits, such as an unhealthy diet, obesity and lack of exercise, contribute to prehypertension and high blood pressure.
Prehypertension Prevention
The same healthy lifestyle changes recommended to treat prehypertension also help prevent high blood pressure. You’ve heard it before — eat healthy foods, use less salt, exercise regularly, maintain a healthy weight, drink less alcohol and quit smoking. But take the advice to heart. Start adopting healthier habits today.
Prehypertension symptoms
Prehypertension doesn’t cause symptoms. In fact, severe high blood pressure may not cause symptoms.
The only way to detect prehypertension is to keep track of your blood pressure readings. Have your blood pressure checked at each doctor’s visit — or check it yourself at home with a home blood pressure monitoring device.
Prehypertension diagnosis
To diagnose prehypertension, you’ll have a blood pressure test. Your doctor or a specialist will usually place an inflatable arm cuff around your arm and measure your blood pressure using a pressure-measuring gauge.
A blood pressure reading, given in millimeters of mercury (mm Hg), has two numbers. The first, or upper, number measures the pressure in your arteries when your heart beats (systolic pressure). The second, or lower, number measures the pressure in your arteries between beats (diastolic pressure).
Your blood pressure is considered normal if it’s below 120/80 mm Hg. Other blood pressure measurements are categorized as:
- Prehypertension. Prehypertension is a systolic pressure ranging from 120 to 139 mm Hg or a diastolic pressure ranging from 80 to 89 mm Hg.
- Stage 1 hypertension. Stage 1 hypertension is a systolic pressure ranging from 140 to 159 mm Hg or a diastolic pressure ranging from 90 to 99 mm Hg.
- Stage 2 hypertension. More severe hypertension, stage 2 hypertension is a systolic pressure of 160 mm Hg or higher or a diastolic pressure of 100 mm Hg or higher.
Because blood pressure tends to fluctuate, a diagnosis of prehypertension is based on the average of two or more blood pressure readings taken on separate occasions in a consistent manner. Your blood pressure generally should be measured in both arms to determine if there is a difference. Your doctor may ask you to record your blood pressure at home and at work to provide additional information.
Your doctor may suggest a 24-hour blood pressure monitoring test called ambulatory blood pressure monitoring. The device used for this test measures your blood pressure at regular intervals over a 24-hour period and provides a more accurate picture of blood pressure changes over an average day and night. However, these devices aren’t available in all medical centers, and they’re rarely reimbursed.
Prehypertension treatment
In people with prehypertension, the recommended treatment is mainly lifestyle and dietary changes. These include moderate restriction on salt in the diet, weight reduction in those who are overweight, regular exercise, avoidance of excessive alcohol intake.
Your doctor will likely suggest that you control prehypertension with lifestyle changes, such as:
- Maintaining a healthy weight or losing weight if you’re overweight or obese
- Eating a healthy, low-salt diet
- Exercising regularly
- Limiting the amount of alcohol you drink
- Quitting smoking
While patients with prehypertension are mainly treated with lifestyle modifications, recent findings that prehypertension does increase the risk of complications e.g. heart diseases, raising the question of whether prehypertensive patients should be treated more aggressively with antihypertensive medications. This requires further research in time to come to determine.
If you have prehypertension accompanied by diabetes, kidney disease or cardiovascular disease, your doctor may recommend blood pressure medication in addition to lifestyle changes.
Lifestyle and home remedies
As your blood pressure increases, so does your risk of cardiovascular disease. That’s why it’s so important to control prehypertension. The key is a commitment to healthy lifestyle changes.
- Eat healthy foods. Eat a healthy diet. Try the Dietary Approaches to Stop Hypertension (DASH) diet. Choose fruits, vegetables, whole grains, poultry, fish and low-fat dairy foods. Get plenty of potassium, which can help lower blood pressure. Eat less saturated fat and trans fat.
- Maintain a healthy weight. Keeping a healthy weight, or losing weight if you’re overweight or obese, can help you control your blood pressure and lower your risk of related health problems. If you’re overweight, losing even 5 pounds (2.3 kilograms) can lower your blood pressure.
- Use less salt. The Dietary Guidelines for Americans recommend limiting sodium to less than 2,300 mg a day. A lower sodium level — 1,500 milligrams (mg) a day — is appropriate for people 51 years of age or older, and individuals of any age who are black or who have hypertension, diabetes or chronic kidney disease. While you can reduce the amount of salt you eat by putting down the saltshaker, you usually should also pay attention to the amount of salt that’s in the processed foods you eat, such as canned soups or frozen dinners.
- Increase physical activity. Regular physical activity can help lower your blood pressure, manage stress, reduce your risk of other health problems and keep your weight under control. For most healthy adults, the Department of Health and Human Services recommends that you get at least 150 minutes a week of moderate aerobic activity or 75 minutes a week of vigorous aerobic activity, or a combination or moderate and vigorous activity. Aim to do muscle-strengthening exercises at least two days a week.
- Limit alcohol. If you choose to drink alcohol, do so in moderation. For healthy adults, that means up to one drink a day for women of all ages and men older than age 65, and up to two drinks a day for men age 65 and younger. One drink equals 12 ounces of beer, 5 ounces of wine or 1.5 ounces of 80-proof liquor.
- Don’t smoke. Tobacco injures blood vessel walls and speeds up the process of hardening of the arteries. If you smoke, ask your doctor to help you quit.
- Manage stress. Reduce stress as much as possible. Practice healthy coping techniques, such as muscle relaxation, deep breathing or meditation. Getting regular physical activity and plenty of sleep can help, too.
Prehypertension diet
Managing Blood Pressure with a Heart-Healthy Diet.
Eating a heart-healthy diet is important for managing your blood pressure and reducing your risk of heart attack, stroke and other health threats.
Get quality nutrition from healthy food sources.
Aim to eat a diet that’s rich in:
- Fruits
- Vegetables
- Whole-grains
- Low-fat dairy products
- Skinless poultry and fish
- Nuts and legumes
- Non-tropical vegetable oils
Limit:
- Saturated and trans fats
- Sodium
- Red meat (if you do eat red meat, compare labels and select the leanest cuts available)
- Sweets and sugar-sweetened beverages
The American Heart Association recommends no more than 2,300 milligrams (mgs) a day and an ideal limit of no more than 1,500 mg per day for most adults, especially for those with high blood pressure and prehypertension. Even cutting back by 1,000 mg a day can improve blood pressure and heart health.
Salt vs. Sodium Equivalents
Sodium chloride or table salt is approximately 40 percent sodium. It’s important to understand just how much sodium is in salt so you can take measures to control your intake. These amounts are approximate.
- 1/4 teaspoon salt = 575 mg sodium
- 1/2 teaspoon salt = 1,150 mg sodium
- 3/4 teaspoon salt = 1,725 mg sodium
- 1 teaspoon salt = 2,300 mg sodium
Sea salt has boomed in popularity, but it usually isn’t any less salty. Just like table salt, it typically contains 40 percent sodium.
The American Heart Association recommends CONSUMING LESS THAN 1,500 mg daily. Even for people who don’t have high blood pressure, less sodium will significantly blunt the rise in blood pressure that occurs as we age and will also reduce the risk developing other conditions, such as kidney disease, associated with eating too much sodium.
Seasoning Alternatives — Spice It Up.
There is a rich world of creative and flavorful alternatives to salt. Get started with this guide to spices, herbs and flavorings and the food items with which they are a particularly good flavor match. Then get creative and experiment! Here are some seasonings to add variety:
- Allspice: Lean meats, stews, tomatoes, peaches, applesauce, cranberry sauce, gravies, lean meat
- Almond extract: Puddings, fruits
- Basil: Fish, lamb, lean ground meats, stews, salads, soups, sauces, fish cocktails
- Bay leaves: Lean meats, stews, poultry, soups, tomatoes
- Caraway seeds: Lean meats, stews, soups, salads, breads, cabbage, asparagus, noodles
- Chives: Salads, sauces, soups, lean meat dishes, vegetables
- Cider vinegar: Salads, vegetables, sauces
- Cinnamon: Fruits (especially apples), breads
- Curry powder: Lean meats (especially lamb), veal, chicken, fish, tomatoes, tomato soup
- Dill: Fish sauces, soups, tomatoes, cabbages, carrots, cauliflower, green beans, cucumbers, potatoes, salads, macaroni, lean beef, lamb, chicken, fish
- Garlic (not garlic salt): Lean meats, fish, soups, salads, vegetables, tomatoes, potatoes
- Ginger: Chicken, fruits
- Lemon juice: Lean meats, fish, poultry, salads, vegetables
- Mace: Hot breads, apples, fruit salads, carrots, cauliflower, squash, potatoes, veal, lamb
- Mustard (dry): Lean meats, chicken, fish, salads, asparagus, broccoli, Brussels sprouts, cabbage, sauces
- Nutmeg: Fruits, potatoes, chicken, fish, lean meat loaf, toast, veal, pudding
- Onion powder (not onion salt): Lean meats, stews, vegetables, salads, soups
- Paprika: Lean meats, fish, soups, salads, sauces, vegetables
- Parsley: Lean meats, fish, soups, salads, sauces, vegetables
- Peppermint extract: Puddings, fruits
- Pimiento: Salads, vegetables, casserole dishes
- Rosemary: Chicken, veal, lean meat loaf, lean beef, lean pork, sauces, stuffings, potatoes, peas, lima beans
- Sage: Lean meats, stews, biscuits, tomatoes, green beans, fish, lima beans, onions, lean pork
- Savory: Salads, lean pork, lean ground meats, soups, green beans, squash, tomatoes, lima beans, peas
- Thyme: Lean meats (especially veal and lean pork), sauces, soups, onions, peas, tomatoes, salads
- Turmeric: Lean meats, fish, sauces, rice
Sodium Sources
Sodium can be sneaky. Taking control of your sodium means checking labels and reducing preservatives.
These six popular foods can add high levels of sodium to your diet.
- Breads and Rolls: – Some foods that you eat several times a day, such as bread, add up to a lot of sodium even though each serving may not seem high in sodium. Check labels to find lower-sodium varieties.
- Cold Cuts and Cured Meats: – One 2 oz. serving, or 6 thin slices, of deli meat can contain as much as half of your daily recommended dietary sodium. Look for lower-sodium varieties of your favorite lunch meats.
- Sandwiches: A sandwich or burger from a fast food restaurant can contain more than 100 percent of you daily suggested dietary sodium, Try half a sandwich with a side salad instead.
- Pizza: – A slice of pizza with several toppings can contain more than half of your daily recommended dietary sodium. Limit the cheese and add more veggies to your next slice.
- Soup: – Sodium in one cup of canned soup can range from 100 to as much as 940 milligrams – more than half your daily recommended intake. Check the labels to find lower sodium varieties.
- Chicken: – Sodium levels in poultry can vary based on preparation methods. You will find a wide range of sodium in poultry products, so it is important to choose wisely.
Americans consume up to 75 percent of their sodium from processed foods like soups, tomato sauce, condiments and canned goods. That’s why it’s so important to compare NUTRITION FACTS labels and serving sizes. Watch for the words “soda” and “sodium” and the symbol “Na” on labels, which warn you that these products contain sodium compounds. Many canned and frozen food labels help the consumer by printing “low salt” or “low sodium” boldly on the packaging.
Table 1. Tips for Lowering Salt (Sodium) When Shopping, Cooking, and Eating Out
Shopping | Cooking | Eating Out |
|---|---|---|
|
|
|
*Examples of convenience foods are frozen dinners, prepackaged foods, and soups; examples of condiments are mustard, ketchup, soy sauce, barbecue sauce, and salad dressings.
Other foods to be aware of include:
- Processed foods
- Natural foods with a higher-than-average sodium content, including cheese, seafood, olives and some legumes
- Table salt, sea salt and kosher salt (sodium chloride)
- Some over-the-counter drugs
- Some prescription medications
When cooking at home, try heart-healthy recipes. When dining out, look for healthy options.
Shop smart, cook smart
- Choose lower-sodium foods or low-sodium versions of your favorites.
- Although it may take some time for your taste buds to adjust to a lower sodium diet, there are delicious options for very flavorful low-sodium meals. Once the adjustment to healthier dining is made, many people report they would not choose to go back to the highly processed, sodium-rich foods.
- When buying prepared and prepackaged foods, read the labels.
- Eat more fruits and vegetables.
- When buying canned or frozen varieties, be sure to choose the no-salt added versions, and look for the choices without added sauces.
- Use fruit and raw vegetables as snacks.
- Select unsalted nuts or seeds, dried beans, peas and lentils.
- Select unsalted or low-sodium fat-free broths, bouillons or soups.
- Avoid adding salt and canned vegetables with added salt to homemade dishes.
- Don’t use salt during cooking and remove the salt shaker from your table.
- Certain salt substitutes contain a large amount of potassium and very little sodium. They are not expensive and may be used freely by most people, except those with kidney disease. Talk with your healthcare professional about whether a salt substitute is right for you.
- Learn to use spices and herbs to enhance the natural flavor of food.
- Ditch salt for healthier, delicious salt-free seasoning alternatives.
- Don’t salt food before you taste it; enjoy the natural taste of food.
- Follow the DASH eating plan.
The DASH Diet
As its name implies, the DASH (Dietary Approaches to Stop Hypertension) eating plan is designed to help you manage blood pressure.
The DASH diet eating plan requires no special foods and has no hard-to-follow recipes. It simply calls for a certain number of daily servings from various food groups to provide your daily and weekly nutritional goals.
DASH eating plan recommends:
- Limiting foods that are high in saturated fat, such as fatty meats, full-fat dairy products, and tropical oils such as coconut, palm kernel and palm oils
- Limiting sugar-sweetened beverages and sweets.
- Limiting added sugars
- The American Heart Association recommends 1,500 mg a day of sodium as an upper limit for all adults.
- Eating more vegetables, fruits, and fat-free or low-fat dairy products.
- Includes whole grains, fish, poultry, beans, seeds, nuts, and vegetable oils.
Along with the DASH diet, other lifestyle changes can help lower your blood pressure. They include staying at a healthy weight, exercising, and not smoking.
When following the DASH diet eating plan, it is important to choose foods that are:
- Low in saturated and trans fats
- Rich in potassium, calcium, magnesium, fiber, and protein
- Lower in sodium
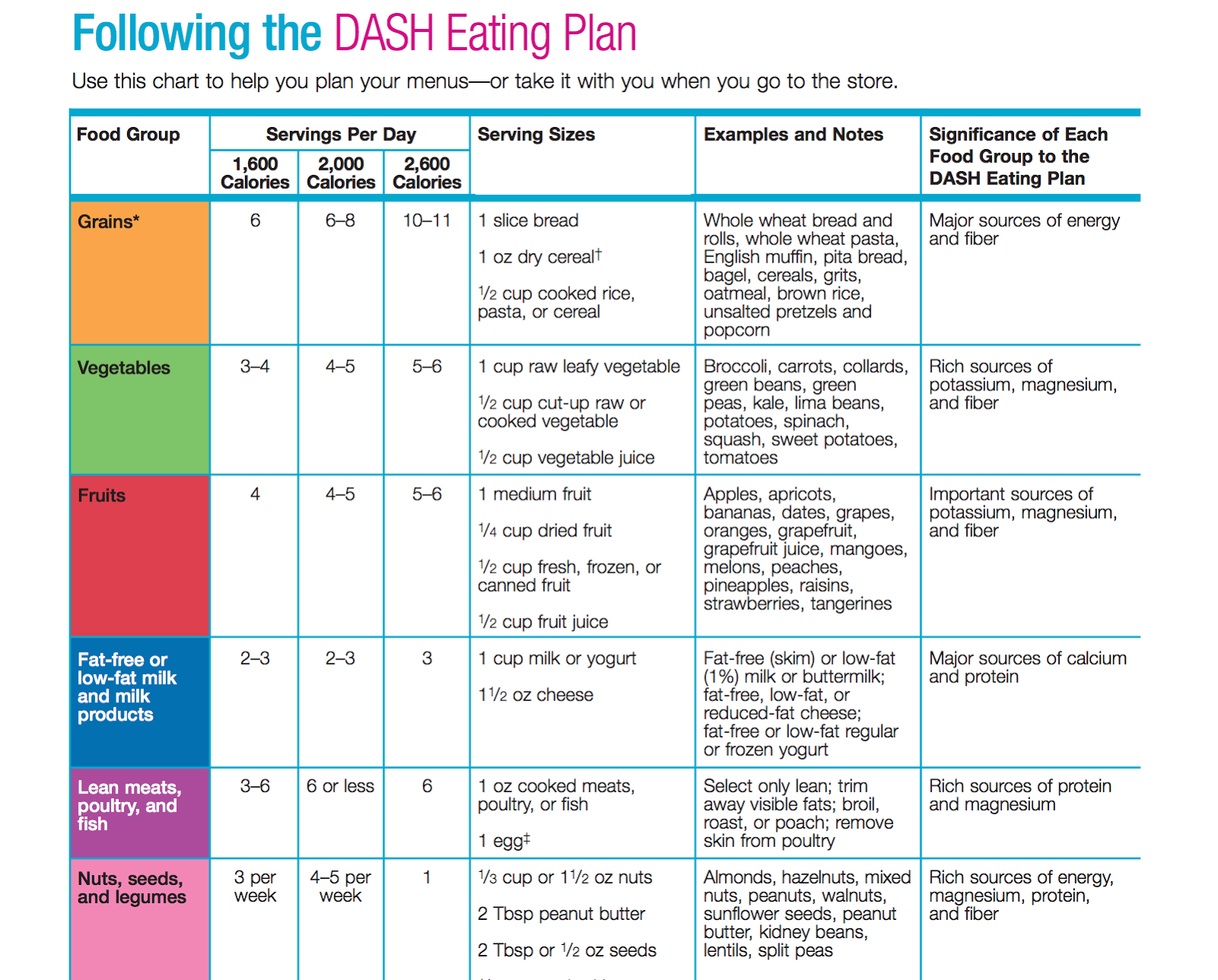
Table 2. Daily and Weekly DASH Diet Eating Plan Goals for a 2,000-Calorie-a-Day Diet
| Food Group | Daily Servings | Serving Sizes | Examples and Notes | Significance of Each Food Group to the DASH Eating Pattern |
|---|---|---|---|---|
| Grains* | 6-8 | 1 slice bread 1 oz dry cereal** 1/2 cup cooked rice, pasta, or cereal | Whole wheat bread and rolls, whole wheat pasta, English muffin, pita bread, bagel, cereals, grits, oatmeal, brown rice, unsalted pretzels and popcorn | Major sources of energy and fiber |
| Vegetables | 4-5 | 1 cup raw leafy vegetable 1/2 cup cut-up raw or cooked vegetable 1/2 cup vegetable juice | Broccoli, carrots, collards, green beans, green peas, kale, lima beans, potatoes, spinach, squash, sweet potatoes, tomatoes | Rich sources of potassium, magnesium, and fiber |
| Fruits | 4-5 | 1 medium fruit 1/4 cup dried fruit 1/2 cup fresh, frozen, or canned fruit 1/2 cup fruit juice | Apples, apricots, bananas, dates, grapes, oranges, grapefruit, grapefruit juice, mangoes, melons, peaches, pineapples, raisins, strawberries, tangerines | Important sources of potassium, magnesium, and fiber |
| Fat-free or low-fat milk and milk products | 2-3 | 1 cup milk or yogurt 1 1/2 oz cheese | Fat-free (skim) or low-fat (1%) milk or buttermilk, fat-free, low-fat, or reduced-fat cheese, fat-free or low-fat regular or frozen yogurt | Major sources of calcium and protein |
| Lean meats, poultry, and fish | 6 or less | 1 oz cooked meats, poultry, or fish 1 egg*** | Select only lean; trim away visible fats; broil, roast, or poach; remove skin from poultry | Rich sources of protein and magnesium |
| Nuts, seeds, and legumes | 4-5 per week | 1/3 cup or 1 1/2 oz nuts 2 Tbsp peanut butter 2 Tbsp or 1/2 oz seeds 1/2 cup cooked legumes (dry beans and peas) | Almonds, hazelnuts, mixed nuts, peanuts, walnuts, sunflower seeds, peanut butter, kidney beans, lentils, split peas | Rich sources of energy, magnesium, protein, and fiber |
| Fats and oils**** | 2-3 | 1 tsp soft margarine 1 tsp vegetable oil 1 Tbsp mayonnaise 2 Tbsp salad dressing | Soft margarine, vegetable oil (such as canola, corn, olive, or safflower), low-fat mayonnaise, light salad dressing | The DASH study had 27 percent of calories as fat, including fat in or added to foods |
| Sweets and added sugars | 5 or less per week | 1 Tbsp sugar 1 Tbsp jelly or jam 1/2 cup sorbet, gelatin 1 cup lemonade | Fruit-flavored gelatin, fruit punch, hard candy, jelly, maple syrup, sorbet and ices, sugar | Sweets should be low in fat |
* Whole grains are recommended for most grain servings as a good source of fiber and nutrients.
** Serving sizes vary between 1/2 cup and 11/4 cups, depending on cereal type. Check the product’s Nutrition Facts label.
*** Since eggs are high in cholesterol, limit egg yolk intake to no more than four per week; two egg whites have the same protein content as 1 oz of meat.
**** Fat content changes serving amount for fats and oils. For example, 1 Tbsp of regular salad dressing equals one serving; 1 Tbsp of a low-fat dressing equals one-half serving; 1 Tbsp of a fat-free dressing equals zero servings.
(Source 1).
Dash Diet Eating Plan
To benefit from the DASH diet eating plan, it is important to consume the appropriate amount of calories to maintain a healthy weight.
The DASH diet eating plan can be used to help you lose weight. To lose weight, follow the DASH eating plan and try to reduce your total daily calories gradually. Find out your daily calorie needs or goals with the Body Weight Planner and calorie chart. Talk with your doctor before beginning any diet or eating plan.
General tips for reducing daily calories include:
- Eat smaller portions more frequently throughout the day.
- Reduce the amount of meat that you eat while increasing the amount of fruits, vegetables, whole grains, or dry beans.
- Substitute low-calorie foods, such as when snacking (choose fruits or vegetables instead of sweets and desserts) or drinking (choose water instead of soda or juice), when possible.
Tips for Following DASH Diet
It’s easy to follow the DASH diet. But it might mean making some changes to how you currently eat. To get started:
- DO NOT try to make changes all at once. It’s fine to change your eating habits gradually.
- To add vegetables to your diet, try having a salad at lunch. Or, add cucumber, lettuce, shredded carrots, or tomatoes to your sandwiches.
- There should always been something green on your plate. It’s fine to use frozen vegetables instead of fresh. Just make sure the package does not contain added salt or fat.
- Add sliced fruit to your cereal or oatmeal for breakfast.
- For dessert, choose fresh fruit or low-fat frozen yogurt instead of high-calorie sweets, such as cakes or pies.
- Choose healthy snacks, such as unsalted rice cakes or popcorn, raw vegetables, or yogurt. Dried fruits, seeds, and nuts also make great snack choices. Just keep these portions small.
- Choose whole grain foods for most grain servings to get added nutrients, such as minerals and fiber. For example, choose whole wheat bread or whole grain cereals.
- Think of meat as part of your meal, instead of the main course. Limit your servings of lean meat to 6 ounces (170 grams) a day. You can have two 3-ounce (85 grams) servings during the day. If you now eat large portions of meats, cut them back gradually by a half or a third at each meal.
- Try these snacks ideas: unsalted rice cakes; nuts mixed with raisins; graham crackers; fat-free and low-fat yogurt and frozen yogurt; popcorn with no salt or butter added; raw vegetables.
- Try cooking without meat at least twice each week. Instead, eat beans, nuts, tofu, or eggs for your protein.
- If you are allergic to nuts, use seeds or legumes (cooked dried beans or peas).
- National Institutes of Health. National Heart, Lung and Blood Institute. Your Guide to Lowering Your Blood Pressure With DASH. https://www.nhlbi.nih.gov/health/resources/heart/hbp-dash-how-to[↩]