Contents
What is preterm labor
Preterm labor is labor that happens before the 37th week of pregnancy. About 8 out of 100 babies will be born prematurely. Labor is when regular contractions lead to opening up of the cervix (neck of the womb). This normally occurs at between 37 and 42 weeks of pregnancy. If it occurs before 37 weeks, it is known as premature labor. Very premature birth is much less common, with fewer than one in 100 babies being born at between 22 and 28 weeks of pregnancy.
Preterm and premature mean the same thing — early. Preterm labor is labor that begins early, before 37 weeks of pregnancy. Labor is the process your body goes through to give birth to your baby. Preterm labor can lead to premature birth. Premature birth is when your baby is born early, before 37 weeks of pregnancy. Your baby needs about 40 weeks in the womb to grow and develop before birth.
Babies born before 37 weeks of pregnancy are called premature. Premature babies can have serious health problems at birth and later in life. About 1 in 10 babies is born prematurely each year in the United States.
- If you believe you are having preterm labor, get medical help right away. If in doubt, get checked early.
- Don’t worry about mistaking false labor for the real thing. Everyone will be pleased if it’s a false alarm.
If your preterm contractions result in preterm labor, your baby will be born early. The earlier premature birth happens, the greater the health risks for your baby. Many premature babies (preemies) need special care in the neonatal intensive care unit. Preemies can also have long-term mental and physical disabilities.
While the specific cause of preterm labor often isn’t clear, certain risk factors may up the odds of early labor. But, preterm labor can also occur in pregnant women with no known risk factors. Still, it’s a good idea to know if you’re at risk of preterm labor and how you might help prevent it.
Signs of preterm labor
The signs of preterm labor can be similar to the signs of labor that starts at full term, and may include:
- Regular or frequent contractions that make your belly tighten like a fist. The contractions may or may not be painful.
- Period-type pains
- A “show” (when the plug of mucus that has sealed the cervix during pregnancy comes away and out of the vagina)
- Change in your vaginal discharge (watery, mucus or bloody) or more vaginal discharge than usual
- Breaking of the waters (rupture of membranes) – this can be a gush or a trickle
- Constant low, dull backache
- Pressure in your pelvis or lower belly, like your baby is pushing down
- Belly cramps with or without diarrhea
If you think your labor (you are having regular, painful tightenings or you think your waters have broken) might be starting and you’re less than 37 weeks pregnant, it is important that you call your doctor or hospital maternity unit straight away. You are likely to be asked to come in. They’ll need to check you and your baby to find out whether you’re in labor, and discuss your care choices with you.
Your doctor or midwife will ask whether you have had a premature birth in a previous pregnancy. You will also be asked about your general health, whether you have had any abdominal pain, tightenings or bleeding, and whether you think your waters have broken.
They’ll offer checks, tests and monitoring to find out whether:
- your waters have broken
- you’re in labor
- you have an infection
You will have a check-up that may include:
- a general examination and a check of your temperature, pulse and blood pressure
- a vaginal examination, blood test, urine test and cardiotocography to record contractions and your baby’s heartbeat
- an examination of your abdomen
- blood sample to check for signs of infection
- urine sample to test for signs of infection
You may also be offered an ultrasound scan to check your baby’s wellbeing and which way round he or she is lying.
The start of labor is usually diagnosed by vaginal examination:
- Your doctor or midwife will use a speculum (an instrument used to separate the walls of the vagina) to see whether the cervix is changing in preparation for labor or has already opened up.
- Your doctor or midwife will also be able to see whether there is fluid leaking, which may indicate that your waters have broken. Sometimes the waters break before 37 weeks but labor doesn’t start.
- A vaginal swab may be taken to check for infection.
- Another type of swab called fetal fibronectin may be taken from the top of the vagina, if you are at between 24 and 34 weeks of pregnancy. This test helps to see whether you are likely to go into labor soon or not:
- Most women who are suspected of being in premature labor have a negative swab. This is very reassuring because fewer than one in 100 women with a negative test will go into labor within the next 2 weeks.
- A positive swab means that there is an increased chance you may go into labor. One in five women who have a positive swab go into labor within 10 days.
The swab will be less accurate if you have any bleeding, if your waters have broken or if you have had sexual intercourse in the previous 24 hours.
If labor is not confirmed or if you have a negative fetal fibronectin swab, you should be able to go home if you are well and there are no concerns for you or your baby.
If labor is suspected, you will be advised to stay in hospital. You may be offered:
- A course of two to four corticosteroids injections usually over a 24–48 hour period to help with your baby’s development and reduce the chance of problems caused by being born early (unless you have already received steroids in this pregnancy).
- A course of antibiotics if it is confirmed that your waters have broken, to reduce the risk of an infection getting into the womb.
- An opportunity to talk to one of the neonatal team about the care that your baby is likely to receive, if born early. You and your partner may also wish to visit the neonatal unit.
- Medication (tablets or through a drip) to try to stop labor, if your waters have not broken and there are no concerns about you or your baby. This is only advised in the following circumstances:
- while you are having your course of corticosteroids
- if you need to be transferred to a hospital where there is a neonatal intensive care unit, which could be some distance away; this is particularly the case if you are less than 32 weeks pregnant.
- These medications are not routinely recommended for women having twins or triplets because it is not clear that they are beneficial in that situation.
- Treatment with magnesium sulfate, through a drip in your arm. This would be considered if you are less than 30 weeks pregnant and likely to give birth within the next 24 hours. This treatment reduces the chance of complications for your baby, in particular cerebral palsy. You may experience minor side effects such as flushing and nausea. If you are advised to have this treatment, your doctor will discuss it fully with you.
Planned premature labor
In some cases, preterm labor is planned and induced because it’s safer for the baby to be born sooner rather than later.
This could be because of a health condition in the mother, such as pre-eclampsia, or in the baby. Your midwife and doctor will discuss with you the benefits and risks of continuing with the pregnancy versus your baby being born premature.
You can still make a birth plan, and discuss your wishes with your birth partner, midwife and doctor.
What are the risks of preterm birth?
Babies born before full term (before 37 weeks) are vulnerable to problems associated with premature birth. The earlier in the pregnancy a baby is born, the more vulnerable they are. Premature babies have an increased risk of health problems, particularly with breathing, feeding and infection. The earlier your baby is born, the more likely he or she is to have these problems and your baby may need to be looked after in a neonatal unit. However, more than eight out of ten premature babies born after 28 weeks survive and only a small number will have serious long-term disability. Many survivors (as children) who have long-term health problems still rate their quality of life as being good.
Your goal is to get as close to term (40 weeks) as you can before giving birth. The closer you get to term, the greater your chances of having a healthy baby. Work with your doctor or obstetrician. Together you can take steps to keep you from giving birth too early.
Babies are considered ‘viable’ at 24 weeks of pregnancy – this means it’s possible for them to survive being born at this stage. If you give birth before 24 weeks of pregnancy, it is sadly much less likely that your baby will survive. Babies who do survive after such a premature birth often have serious health problems. The possible treatment and outcomes for your baby in your individual situation will be discussed with you.
Premature baby is at risk of a variety of problems, such as:
- not breastfeeding well;
- having immature lungs, and not being able to breathe on their own;
- bleeding in the brain;
- life-threatening infections;
- jaundice;
- inflammation of the bowel;
- long-term health problems, such as cerebral palsy; or
- dying.
Babies born this early need special care in a hospital with specialist facilities for premature babies. This is called a neonatal unit. They may have health and development problems because they haven’t fully developed in the womb.
If your baby is likely to be delivered early, you should be admitted to a hospital with a neonatal unit.
Not all hospitals have facilities for the care of very premature babies, so it may be necessary to transfer you and your baby to another unit, ideally before delivery (if time permits) or immediately afterwards.
Twins and multiples
Twins and triplets are often born prematurely. The average delivery date for twins is 37 weeks, and 33 weeks for triplets.
If you have any reason to think that your labor may be starting early, contact your hospital straight away.
What causes preterm labor
For most women, the cause of preterm labor is not found. It is thought that a number of factors, sometimes involving infection, can bring about a change in the cervix that causes labor to start.
However, there are certain factors that increase the risk.
These include if:
- your waters have broken early
- you have had a premature birth or your waters broke before 37 weeks, in a previous pregnancy
- you have had a previous late miscarriage (after 14 weeks of pregnancy)
- you have had vaginal bleeding after 14 weeks in this pregnancy
- you have an abnormality in the shape of your womb
- you are carrying twins or triplets
- you have excess fluid around your baby
- you have a short cervix
- you are a smoker
- you have had fertility treatment.
Having your baby early means that you are at an increased risk of having a premature birth in a future pregnancy. However, you are still likely to have a baby born at more than 37 weeks next time.
You will be advised to be under the care of a consultant obstetrician who will discuss with you a plan for your pregnancy. This will depend on your individual situation and on whether a cause for your early delivery, such as infection, was found.
Can preterm labor be prevented?
In some circumstances, particularly if you have had a baby born prematurely or a late miscarriage in the past, you may be offered vaginal scans in pregnancy to measure the length of your cervix or you may be advised to have a suture (stitch) put around it to prevent it opening early.
A cervical suture is an operation where a suture (stitch) is placed around the cervix (neck of the womb). It is also sometimes known as cervical cerclage. It is usually done at between 12 and 24 weeks of pregnancy.
A cervical suture is sometimes recommended for women who are thought to have a high chance of a late miscarriage or of going into preterm labor. The purpose of the suture is to reduce the risk of your baby being born early. Premature babies have an increased risk of short- and long-term health problems.
The exact cause of preterm labor or late miscarriages is not clear, but they may be caused by changes in the cervix such as shortening and opening. A cervical suture helps to keep the cervix long and closed, thereby reducing the risk of premature birth or late miscarriage.
Insertion of the suture takes place in an operating theater. You may have a spinal anesthetic where you will stay awake but will be numb from the waist down or you may be given a general anesthetic where you will be asleep. Your team will advise which would be the best option for you.
You will be advised not to eat or drink for 4–6 hours before the operation. In the operating theater, your legs will be put in supports and sterile covers will be used to keep the operating area clean. The doctor will then insert a speculum (a plastic or metal instrument used to separate the walls of the vagina to show or reach the cervix) into the vagina and put the suture around the cervix. The operation should take less than 30 minute.
Afterwards, you may be given antibiotics to help prevent infection and you will be offered medication to ease any discomfort. You may also have a tube (catheter) inserted into your bladder that will be removed once the anesthetic has worn off.
You are likely to be able to go home the same day although you may be advised to stay in hospital longer.
After the operation, you will usually have some bleeding from the vagina, which should change to brown in color after a day or two. You may have a rise in temperature that should settle without treatment.
Once you recover from the operation, you can carry on as normal for the rest of your pregnancy. Resting in bed is not normally recommended. Sexual intercourse may be continued when you feel comfortable to do so. Your doctor can advise you about the activities you can do and those best avoided during the first few days after the procedure.
Are cervical sutures sometimes inserted through the abdomen?
Yes, if a vaginal cervical suture has not worked in the past or it is not possible to insert a vaginal suture. This would involve an operation through your abdomen and is called a ‘transabdominal cerclage’. It is done either before you become pregnant again or in early pregnancy. Such a suture is not removed and your baby would be born by caesarean section.
When might a cervical suture be advised?
You may be in one of the following situations:
- If you have had one or two late miscarriages or premature births (before 34 weeks), you may be offered ultrasound scans between 14 and 24 weeks of pregnancy to measure the length of your cervix. If the scans show that it has shortened to less than 25 mm, you may be advised to have a cervical suture.
- If you have suffered three or more late miscarriages or three or more premature births you may be advised to have a cervical suture inserted at about 12–14 weeks of pregnancy.
During pregnancy it is sometimes noticed during a vaginal examination or a routine scan that the cervix has started to open up. Depending on your circumstances, you may be offered a suture called a rescue suture. If you are in this situation, a senior obstetrician will discuss with you the risks and benefits of having a rescue suture.
Are there situations when a cervical suture would not be advised?
Sometimes a cervical suture is not advised. It would not normally improve the outcome for your baby/babies and may carry risks to you in the following circumstances:
- you are more than 24 weeks pregnant
- you are carrying twins or triplets
- your womb is an abnormal shape
- an ultrasound scan done for another reason happens to show that you have a short cervix
- you have had treatment to the cervix for an abnormal smear.
If a suture is not the right option for you, you will still be closely monitored. This may include regular vaginal ultrasound scans to measure the length of your cervix until 24 weeks of pregnancy. If the cervix is shortened, you may be offered corticosteroid injections after 23 weeks to increase the chance of your baby surviving if born early.
Are there situations when a cervical suture would not be put in?
Yes. A cervical suture would not be put in if:
- you are already in labor or your waters have broken
- you have signs of infection in your womb
- you have vaginal bleeding
- there are concerns about your baby’s wellbeing.
Are there any risks in having a cervical suture?
There is a small risk that your bladder or cervix may be damaged at the time of the operation. Rarely, your membranes may be ruptured. The risk of complications is higher if you have a rescue suture and this will be discussed with you before the operation.
A planned cervical suture does not increase your risk of infection, miscarriage, or premature labor. It does not increase your risk of having to be started off in labor (be induced) or needing a caesarean section.
Is there anything I should look out for?
If you experience any of the following symptoms, you should contact your maternity unit:
- contractions or cramping
- vaginal bleeding
- your waters breaking
- smelly vaginal discharge.
How and when will the suture be taken out?
Your suture will be taken out at the hospital. This will normally happen at around 36–37 weeks of pregnancy, unless you go into labor before then.
You will not normally need an anesthetic. A speculum is inserted into your vagina and the suture is cut and removed. It usually takes just a few minutes.
You may have a small amount of bleeding afterwards. Any red bleeding should settle within 24 hours but you may have a brown discharge for longer. If you have any concerns, tell your midwife or doctor.
If you go into labor with the cervical suture in place, it is very important to have it removed promptly to prevent damage to your cervix. If you think you are in labor, contact your maternity unit straight away.
If your waters break early but you are not in labor, the stitch will usually be removed because of the increased risk of infection. The timing of this will be decided by the team looking after you.
Preterm labor complications
Many women diagnosed with preterm labor deliver at or near term. However, there are no medications or surgical procedures to stop preterm labor, once it has started. In some cases, preterm labor associated with problems such as an infection or smoking can be managed by treating the infection or quitting smoking.
Preterm labor could lead to premature birth. This can pose a number of health concerns, such as low birth weight, breathing difficulties, underdeveloped organs and vision problems. Children who are born prematurely also have a higher risk of learning disabilities and behavioral problems.
Causes of premature birth
There are many causes of premature birth. Most occur spontaneously, however on occasions a mother or baby may necessitate an early induction of labor or caesarean birth. This can occur for medical or non-medical reasons.
Common reasons for preterm birth can be associated with different factors including medical and pregnancy; social, personal and economic; and behavioral.
Medical and Pregnancy
Cervical incompetence: This occurs when a weak cervix cannot support the weight of the uterus and begins to dilate (widen) and efface (thin) before pregnancy has reached term. Occasionally women diagnosed with an incompetent cervix may undergo a procedure in early stages of pregnancy called a cerclage. This involves placing a stitch in the cervix to prevent it opening up too soon and removing the stitch when nearing term.
Multiple births: Occurs when more than one fetus is carried in a single pregnancy. Twins and other multiple births are often induced early if labor is not spontaneous. Around 50% of twin pregnancies will be born before 37 weeks and a very high percentage of higher order multiples will be born prematurely.
Placental Accreta: Placenta accreta is a general term to describe a serious complication of pregnancy when part of the placenta, or entire placenta invades and is inseparable from the uterine wall causing severe blood loss after delivery. After giving birth the placenta should separate completely from the uterus. If part or all of the placenta remains attached it is called placenta accreta. It’s also possible for the placenta to invade the muscles of the uterus (placenta increta) or grow through the uterine wall, sometimes extending to nearby organs (placenta percreta).
Placenta Previa: A complication of pregnancy where the placenta has attached to the uterine wall close to or over the opening of the cervix. The most common complication of placenta Previa is bleeding leading to an increased risk of slow foetal growth and premature birth. Almost all babies are delivered via caesarean birth as the increased risk of severe bleeding associated with a vaginal birth can be life threatening. A woman is also at increased risk of having further premature births if this has occurred in previous pregnancies.
Placental abruption: A complication of pregnancy, where the placenta separates from the wall of the uterus. It is the most common cause of late pregnancy bleeding and if the separation is severe can contribute to fetal and maternal death. Direct trauma to the uterus is a known cause, and risk factors may be multiple pregnancies, smoking and high blood pressure including preeclampsia.
Placental insufficiency: This condition can prevent the baby from gaining essential nourishment. Symptoms may include below average weight gain, below average fetal development, or slow growth of the uterus. It can also lead to foetal distress decreasing their heart rate and in serious cases an inability to tolerate a vaginal birth, thus requiring a caesarean delivery. An ultrasound examination will determine if growth of the foetus is adequate and doctors may advise preterm delivery if necessary. Placental insufficiency can be caused by conditions such as diabetes, high blood pressure or preeclampsia, maternal blood clotting disorders, smoking or taking drugs such as cocaine.
Preeclampsia: A complication of pregnancy where hypertension, high blood pressure, occurs in conjunction with high levels of protein in the urine and oedema. The increases in blood pressure can prevent adequate oxygen reaching the foetus and possibly lead to health problems for the baby. It is most common after the 20th week of pregnancy. Risk is increased if the mother already has high blood pressure, diabetes or kidney disease. Preeclampsia is the most common of the dangerous pregnancy complications and can affect both mother and baby. A variation of preeclampsia is HELLP syndrome, a life threatening liver disorder, also related to hypertension in pregnancy. It is usually diagnosed as a direct result of being evaluated for preeclampsia. HELLP is an abbreviation of Hemolytic anemia, Elevated Liver enzymes and Low Platelet count. Approximately 10% to 20% of women who have severe preeclampsia develop HELLP and the only way to reverse this syndrome is the birth of the baby to prevent the potential death of both mother and fetus.
Preterm premature rupture of membranes (PPROM): A condition which occurs in pregnancy when the amniotic sac spontaneously ruptures before the onset of labor. This can lead to spontaneous delivery of the baby within hours or can take weeks until birth. The mother is usually confined to hospital to monitor the pregnancy and prevent complications. There may be no known cause or it could be related to risk factors such as an infection, lower socioeconomic conditions where it is more common adequate antenatal care has not been received, vaginal bleeding from conditions such as placental abruption and smoking.
Previous premature birth: Women who have had a premature delivery previously have an increased chance of having another pre-term delivery.
Having a family history of premature birth. This means someone in your family (like your mother, grandmother or sister) has had a premature baby. If you were born prematurely, you’re more likely than others to give birth early.
Serious or an existing medical condition and other reasons: Conditions such as rhesus negative blood group, gestational diabetes, diabetes, kidney disease and high blood pressure can all affect a developing baby. In some cases, the decision to deliver a baby prematurely is because either they or the mother are medically unwell due to a health problem, congenital abnormality or surgical need.
Twin to twin transfusion syndrome (TTTS): A complication where two or more fetuses share a common placenta and associated with high morbidity and mortality.
Urine infection: Sometimes during the middle to later months of a pregnancy a serious uterine infection can trigger preterm labor. It is important that any possible urine infection be brought to the attention of your health care professional.
Uterine abnormalities: Women with an abnormally shaped uterus such as a bicornuate uterus could be at risk of preterm labor. The baby may have less room to grow and when there isn’t enough room for the baby, the stretching of the uterus can cause labor to begin.
Connective tissue disorders, like Ehlers-Danlos syndromes (also called EDS) and vascular Ehlers-Danlos syndrome (also called vEDS). Connective tissue is tissue that surrounds and supports other tissues and organs. Ehlers-Danlos syndromes can cause joints to be loose and easy to dislocate; skin to be thin and easily stretched and bruised; and blood vessels to be fragile and small. It also can affect your uterus and intestines. Vascular Ehlers-Danlos syndrome is the most serious kind of Ehlers-Danlos syndromes because it can cause arteries and organs (like the uterus) to rupture (burst). Ehlers-Danlos syndromes and vascular Ehlers-Danlos syndrome are genetic conditions that can be passed from parent to child through genes.
Being pregnant with a baby who has certain birth defects, like heart defects or spina bifida. Birth defects are health conditions that are present at birth. They change the shape or function of one or more parts of the body. Birth defects can cause problems in overall health, how the body develops or how the body works. Spina bifida is a birth defect of the spine.
Thrombophilias. These are conditions that increase your risk of making abnormal blood clots.
Getting pregnant again too soon after having a baby. For most women it’s best to wait at least 18 months before getting pregnant again. Talk to your provider about the right amount of time for you.
Social, personal and economic
Mother’s Age: Younger than 17 years or over 35 years
Lower socioeconomic situations: even after assessing other variables such as maternal age, race, behavioral issues and medical situations, low income and social disadvantages lead to higher rates of premature birth. Studies continue to determine optimal means to address this issue.
Race: there is a greater risk of women of African descent to have premature births. This risk is seen to be as much as five times more than Caucasian women despite similar health care provision.
Behavioral
Substance use and abuse: This includes smoking, drinking alcohol or using illicit drugs. The use of some substances can lead to decreased oxygenation to the fetus and small for gestational age babies, birth defects and sadly fetal death if a baby is not delivered in time to prevent irreversible complications.
Late antenatal care: Situations that can potentially lead to premature birth can be better treated if early antenatal care is sought.
Stress: Certain hormones and proteins in the blood that help control the contraction of the uterus and the production of infection fighting cells are increased in times of stress. These can lead to increased risk of infections, uterine irritability and thereby increasing the risk of premature birth.
Risk factors for preterm labor
Preterm labor can affect any pregnancy and many women who have preterm labor have no known risk factors. Many factors have been associated with an increased risk of preterm labor, however, including:
- Previous preterm labor or premature birth, particularly in the most recent pregnancy or in more than one previous pregnancy
- Pregnancy with twins, triplets or other multiples
- Certain problems with the uterus, cervix or placenta
- A lack of prenatal medical care
- Smoking cigarettes or using illicit drugs during pregnancy
- Certain infections, particularly of the genital tract, such as urinary tract infections or vaginal infections (e.g. bacterial vaginosis)
- Some chronic conditions, such as high blood pressure, diabetes or clotting disorders
- Being underweight or overweight before pregnancy, or gaining too little or too much weight during pregnancy
- Stressful life events, such as the death of a loved one
- Red blood cell deficiency (anemia), particularly during early pregnancy
- Too much amniotic fluid (polyhydramnios)
- Pregnancy complications, such as preeclampsia
- Vaginal bleeding during pregnancy
- Presence of a fetal birth defect
- Little or no prenatal care
- An interval of less than six months since the last pregnancy
- Stress
- Being under 17 or over 35 years old
Also, having a short cervical length or the presence of fetal fibronectin — a substance that acts like a glue between the fetal sac and the lining of the uterus — in your vaginal discharge has been linked to an increased risk of preterm labor.
While some past research suggested that gum disease might be linked with premature birth, treatment of periodontal disease during pregnancy hasn’t been proved to reduce the risk of premature birth.
Preterm labor prevention
You might not be able to prevent preterm labor — but there’s much you can do to promote a healthy, full-term pregnancy. For example:
- Seek regular prenatal care. Prenatal visits can help your health care provider monitor your health and your baby’s health. Mention any signs or symptoms that concern you, even if you think they’re silly or unimportant. If you have a history of preterm labor or develop signs or symptoms of preterm labor, you might need to see your health care provider more often during pregnancy for exams and tests.
- Eat a healthy diet. During pregnancy, you’ll need more folic acid, calcium, iron and other essential nutrients. A daily prenatal vitamin — ideally starting a few months before conception — can help fill any gaps.
- Avoid risky substances. If you smoke, quit. Smoking might trigger preterm labor. Illicit drugs are off-limits, too. In addition, medications of any type — even those available over-the-counter — deserve caution. Get your health care provider’s OK before taking any medications or supplements.
- Protect yourself from infections. Talk to your provider about vaccinations that can help protect you from certain infections. Wash your hands with soap and water after using the bathroom or blowing your nose. Don’t eat raw meat, fish or eggs. Have safe sex. Don’t touch cat poop.
- Be cautious when using assisted reproductive technology (ART). If you’re planning to use ART to get pregnant, consider how many embryos will be implanted. Multiple pregnancies carry a higher risk of preterm labor.
- Wait at least 18 months between giving birth and getting pregnant again. Use birth control until you’re ready to get pregnant again. If you’re older than 35 or you’ve had a miscarriage or stillbirth, talk to your provider about how long to wait between pregnancies. Miscarriage is the death of a baby in the womb before 20 weeks of pregnancy. Stillbirth is the death of a baby in the womb after 20 weeks of pregnancy.
If your health care provider determines that you’re at increased risk of preterm labor, he or she might recommend taking additional steps to reduce your risk, such as:
- Taking preventive medications. If you have a history of premature birth, your health care provider might suggest weekly shots of a form of the hormone progesterone called hydroxyprogesterone caproate (Makena) during your second trimester. In additional, your doctor might offer progesterone, which is inserted in the vagina, as a preventive measure against preterm birth.
- Limiting certain physical activities. If you’re at risk of preterm labor or develop signs or symptoms of preterm labor, your health care provider might suggest avoiding heavy lifting or spending too much time on your feet.
- Managing chronic conditions. Certain conditions, such as diabetes and high blood pressure, increase the risk of preterm labor. Work with your health care provider to keep any chronic conditions under control.
If you have a history of preterm labor or premature birth, you’re at risk of a subsequent preterm labor. Work with your health care provider to manage any risk factors and respond to early warning signs and symptoms.
Preterm labor signs and symptoms
For some women, the signs and symptoms of preterm labor are unmistakable. For others, they’re more subtle.
If you have any of the following symptoms, contact your doctor or midwife straight away, as you could be in labor:
- either a slow trickle or a gush of clear or pinkish fluid from your vagina or any increase in vaginal discharge
- constant low, dull backache
- cramps like strong period pains
- regular or frequent painful contractions — a tightening sensation in the abdomen
- mild abdominal cramps
- a frequent need to urinate
- a feeling of pressure in your pelvis or lower abdomen (feeling that the baby is pushing down)
- vaginal spotting or bleeding
- a change in vaginal discharge – watery, mucous, or bloody vaginal discharge
- nausea, vomiting or diarrhea
- 4 or more contractions per hour
- bleeding or blood spotting after 3 months into your pregnancy
Don’t delay if you have strong pain, a smelly discharge or bleeding from your vagina, or if you are feeling feverish, sick or have a temperature, call immediately as you may need urgent medical attention.
- Don’t worry about mistaking false labor for the real thing. Everyone will be pleased if it’s a false alarm.
You may have some of the symptoms but not others. For example, your waters may have broken but with no contractions, or vice versa. Contractions don’t always indicate that you’re in labor, so your healthcare team will carry out checks to find out.
Many women experience Braxton Hicks, sometimes known as practice contractions. These can become quite strong and painful during the third trimester, and it’s easy to mistake them for the real thing.
The healthcare team will check
- whether you are actually in labor
- if labor hasn’t started, whether your symptoms are due to some other cause that needs treating
- if you are definitely in labor, whether this has been caused by something (such as an infection) that needs treating, and how far the labor is progressing, so they can line up the facilities you need, either to delay the birth or to deliver the baby.
Preterm labor diagnosis
To help diagnose preterm labor, your health care provider will document your signs and symptoms. If you’re experiencing regular, painful contractions and your cervix has begun to soften, thin and open before 37 weeks of pregnancy, you’ll likely be diagnosed with preterm labor.
Tests and procedures to diagnose preterm labor include:
- Pelvic exam. Your health care provider might evaluate the firmness and tenderness of your uterus and the baby’s size and position. He or she might also do a pelvic exam to determine if your cervix has begun to open — if your water hasn’t broken and the placenta isn’t covering your cervix (placenta previa).
- Ultrasound. An ultrasound might be used to measure the length of your cervix and determine your baby’s size, age, weight and position in your uterus. You might need to be monitored for a period of time and then have another ultrasound to measure any changes in your cervix, including cervical length.
- Uterine monitoring. Your health care provider might use a uterine monitor to measure the duration and spacing of your contractions.
- Lab tests. Your health care provider might take a swab of your vaginal secretions to check for the presence of certain infections and fetal fibronectin — a substance that acts like a glue between the fetal sac and the lining of the uterus and is discharged during labor. However, this test isn’t reliable enough to be used on its own to assess the risk of preterm labor.
- Maturity amniocentesis. Your health care provider might recommend a procedure in which amniotic fluid is removed from the uterus (amniocentesis) to determine your baby’s lung maturity. The technique can also be used to detect an infection in the amniotic fluid.
If you’re in preterm labor, your health care provider will explain the risks and benefits of trying to stop your labor. Keep in mind that preterm labor sometimes stops on its own.
Preterm labor treatment
If your waters have broken
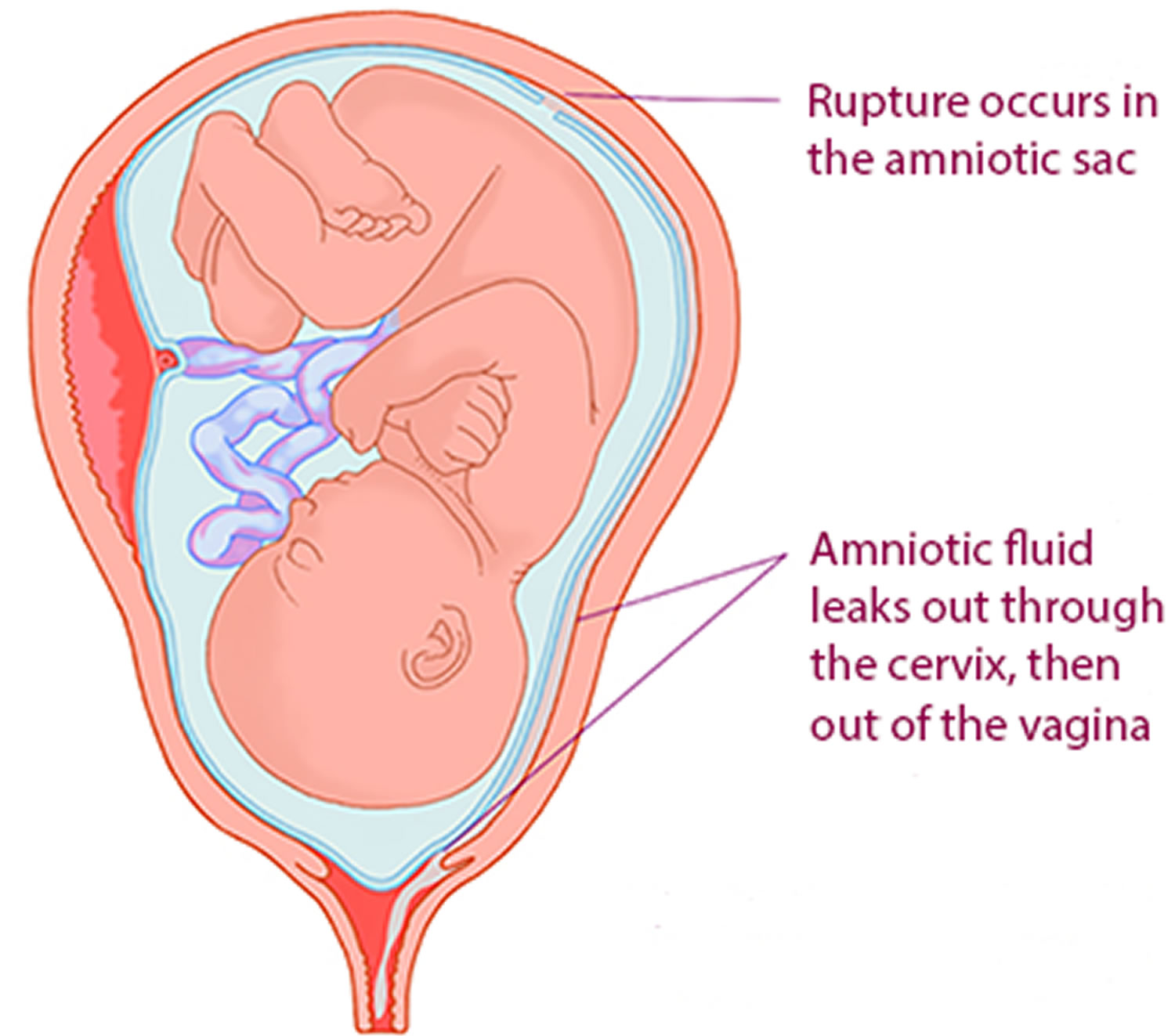
Your unborn baby lies in an amniotic sac of fluid or ‘waters’. ‘Waters breaking’ means that the sac has ruptured or broken. Your waters normally break around the time labor is due but in around 2% of pregnancies they break early for various reasons.
If your waters break before your baby has reached full term (37 weeks), the medical name for it is preterm prelabour rupture of the membranes, or PPROM. If this happens early, before the contractions start, it can (but does not always) trigger early labor.
If your waters have broken early, you will experience it as a trickle or a gush of water from your vagina. It is likely to continue leaking once it has started. If it isn’t too heavy you can use a sanitary towel to catch it. This will also allow you to see what color it is, which will be helpful information for health professionals. It may be pinkish if it contains some blood, or it may be clear. If it greenish or brown go to the maternity unit as soon as possible. If it is heavy, you may need to use a towel.
Does it hurt when my waters break?
No it shouldn’t hurt when your waters break or when they are broken for you. The amniotic sac, which is the part that ‘breaks’ doesn’t have pain receptors, which are the things that cause you to feel pain when you get a cut for example.
You are likely to have an internal examination. This will allow the doctor to look at your cervix and check:
- if the leaking fluid is amniotic fluid
- if it is changing in preparation for labor
- to check for infection by taking a swab.
You might have an ultrasound scan to estimate the amount of fluid left around your baby.
If only a very small amount of amniotic fluid leaks, it is not always easy to be sure whether your waters have broken.
- You may be advised to wear a pad and stay in hospital for a few hours to monitor the situation.
- If you go home but continue to leak fluid at home, you should return to the hospital again.
If your waters are shown to have broken, you will be advised to come into hospital for at least 48 hours. You and your unborn baby will be closely monitored for signs of infection. This will include having your temperature and pulse taken regularly, and your baby’s heart rate will also be monitored.
What are the risks if my waters break early (PPROM)?
If your waters break early the risks and treatment are dependent on the stage of pregnancy you are at.
- You are at risk of going into preterm labor – the health risks for the baby of early birth are greater the younger they are.
- If you do not go into labor, you and the baby are at risk of infection.
The doctors have to balance these two considerations. If the waters have broken because of infection, you and the baby have a high risk of getting the infection and you may need to deliver sooner to prevent this.
If the waters have broken but there is no infection currently present, you and the baby are still at risk but the immediate risk is lesser and your treatment will depend on your stage of pregnancy.
- If you are under 24 weeks of pregnancy and the baby is born, sadly, it is unlikely the baby will survive.
- If you are over 30 weeks and the baby is born, the likelihood of your baby surviving is much higher – over 95%.
If your waters have broken there’s an increased risk of infection for you and your baby. You’ll be offered:
- antibiotics to take for a maximum of 10 days, or until labor starts – whichever is sooner
- tests for infection, which may include blood and urine tests
Figure 1. Preterm labor – pre-labor rupture of membranes (P-PROM)
Preterm pre-labor rupture of membranes (P-PROM) doesn’t definitely mean you’re going into labor. You may be able to go home if there’s no infection and you don’t go into labor within 48 hours.
If you go home, you’ll be advised to tell your midwife immediately if:
- your temperature is raised (a raised temperature is usually over 99.5 °F (37.5 °C) but check with your midwife – they may need you to call before it gets to 99.5 °F (37.5 °C). You should take your temperature every four hours when you’re awake
- any fluid coming from your vagina (called vaginal loss) is colored or smelly
- you bleed from your vagina
- your baby’s movements slow down or stop.
You should avoid having sexual intercourse.
Contact your doctor or midwife and return to the hospital immediately if you have:
- a raised temperature (more than 98.6 °F or 37 °C)
- flu-like symptoms (feeling hot and shivery)
- vaginal bleeding
- if the leaking fluid becomes greenish or smelly
- contractions
- abdominal pain
- if you are worried that the baby is not moving as normal.
Inducing labor or preterm labor with PPROM
If you are past 34 weeks the doctor will weigh up the benefits of inducing labor before the due date to avoid the risk of infection with the disadvantages of being born premature, and may make a recommendation for early delivery.
You may need to stay in a hospital that has a neonatal unit and be monitored carefully for any sign of infection. You may also be treated with antibiotics, corticosteroids and magnesium sulfate (if you are less than 30 weeks) to help prepare your baby in case the are born prematurely.
Over 80% of women who have pre-labor rupture of membranes (PPROM) deliver their baby within seven days of their waters breaking.
Causes of waters breaking early (PPROM)
Intrauterine infection is present in around a third of women with pre-labor rupture of membranes (PPROM). In many cases however it happens without any infection being present. The reason for these cases is unclear, however it has been linked to heavy smoking (more than 10 cigarettes a day) in pregnancy.
What if there are no waters left in my womb?
Your baby’s amniotic sac has to have the right amount of amniotic fluid for the pregnancy to continue normally. If there is a break in the waters your baby will continue to produce amniotic fluid.
Before 23 weeks, the baby needs ‘waters’ to be present for their lungs to develop normally. Loss of water before this can lead to severe problems with lung development that can be critical after birth. After 23 weeks your baby does not need the amniotic fluid so much, so low levels of fluid may not be a problem in itself, but if the low levels are due to your waters breaking then there is a risk of infection.
If your waters haven’t broken
Your midwife or doctor should discuss with you the symptoms of preterm labor and offer checks to see if you’re in labor. These checks can include asking you about your medical and pregnancy history, and about possible labor signs, such as:
- contractions – how long, how strong and how far apart they are
- any pain
- vaginal loss, such as waters or a show
You may be offered a vaginal examination, and your pulse, blood pressure and temperature may also be checked.
Your midwife or doctor will also check your baby. They’ll probably feel your bump to find out the baby’s position and how far into your pelvis the baby’s head is.
They should also ask about your baby’s movements in the last 24 hours. If they don’t ask, tell them about the baby’s movements.
If you’re in preterm labor
The midwife or doctor may offer:
- medicine to try to slow down or stop your labor (tocolytic). Examples of this are magnesium sulphate, terbutaline and nifedipine.
- corticosteroid injections, which can help your baby’s lungs
Tocolytics
Your health care provider might give you a medication called a tocolytic to temporarily stop your contractions. These medications won’t halt preterm labor for longer than two days because they don’t address the underlying cause of preterm labor. However, they might delay preterm labor long enough for corticosteroids to provide the maximum benefit or, if necessary, for you to be transported to a facility that can provide specialized care for your premature baby.
Your health care provider can help you weigh the risks and benefits of using a tocolytic. In addition, your health care provider won’t recommend a tocolytic if you have certain conditions, such as pregnancy-induced high blood pressure.
What side effects can tocolytics cause?
Several kinds of tocolytics may be used during preterm labor, each with different side effects.
Beta-adrenergic receptor agonists, like terbutaline. Possible side effects for your baby may include having a fast heartbeat. Possible side effects for you may include:
- Chest pain; fast or irregular heartbeat
- Breathing trouble; fluid in the lungs
- Diarrhea, nausea (feeling sick to your stomach), throwing up
- Feeling dizzy; shaking or feeling nervous; seizures
- Fever, headache
- High blood sugar
- Low blood pressure; low blood potassium
Calcium channel blockers, like nifedipine. There are no side effects for your baby. Possible side effects for you may include:
- Constipation, diarrhea, nausea
- Feeling dizzy or faint
- Headache
- Low blood pressure
- Redness of the skin
Magnesium sulfate. Side effects for your baby may include:
- Being tired and drowsy
- Slowed breathing
- Weak muscles
- Low levels of calcium and bone problems, if the drug is used for more than 5 to 7 days.
Side effects for you may include:
- Breathing problems, fluid in the lungs
- Dry mouth
- Fatigue (being very tired), weak muscle
- Headache, double vision, slurred speech
- Heart attack
- Nausea or throwing up
- Redness of the skin, heavy sweating
Nonsteroidal anti-inflammatory drugs (also called NSAIDs), like indomethacin. Side effects for your baby may include:
- Bleeding in the brain or heart
- Patent ductus arteriosis, also called PDA. This is a heart problem that’s common in premature babies.
- Jaundice. This is a common condition caused by the build-up of a substance called bilirubin in the blood that makes a baby’s skin and the white parts of his eyes look yellow.
- Kidney problems, like making too little urine
- Necrotizing enterocolitis (also called NEC). This is a problem in a baby’s intestines.
- Rising blood pressure in the lungs
Side effects for you include:
- Feeling dizzy
- Heartburn
- Nausea or throwing up
- Oligohydramnios. This is when you have too little amniotic fluid. Amniotic fluid is the fluid that surrounds your baby in the womb.
- Swollen stomach lining
- Vaginal bleeding
Slowing down labor or stopping it isn’t appropriate in all circumstances – your midwife or doctor can discuss your situation with you. They will consider:
- how many weeks pregnant you are
- whether it might be safer for the baby to be born – for example, if you have an infection or you’re bleeding
- local neonatal (newborn) care facilities and whether you might need to be moved to another hospital
- your wishes
Corticosteroid injections can help your baby’s lungs get ready for breathing if they’re born prematurely. There are two injections, given 12 hours apart – your midwife or doctor will discuss the benefits and risks with you. A single course of corticosteroids has been shown to help with a baby’s development and therefore will increase the chance of your baby surviving, once born. Corticosteroid injection also lessens the chance of your baby having serious complications after birth such as breathing problems owing to the lungs not being fully developed, bleeding into the brain, serious infection or bowel inflammation.
Corticosteroids probably won’t be offered after 36 weeks as your baby’s lungs are likely to be ready for breathing on their own.
If you’re in premature labor and you’re between 24 and 29 weeks pregnant you should be offered magnesium sulfate. This can help protect your baby’s brain development. You may also be offered it if you’re in labor between 30 and 34 weeks. This is to protect your baby against problems linked to being born too soon, such as cerebral palsy.
Can corticosteroids harm me or my baby?
A single course of two to four injections is considered to be safe for you and your baby. More evidence is needed to say whether two or more courses of corticosteroids during pregnancy are safe for your baby.
At what stage of pregnancy should corticosteroids be given?
Corticosteroids help most if they are given to you between 24 weeks and 34 weeks plus 6 days of pregnancy. If you are having a planned caesarean section between 35 and 38 weeks plus 6 days, corticosteroids are usually recommended. Corticosteroids may be given earlier than 24 weeks, but the evidence that they will be helpful for your baby in that situation is less clear; your obstetrician doctor will discuss this with you.
How long are corticosteroids effective for?
Corticosteroids are of most help if the last dose is given to you between 24 hours and 1 week before you have your baby. There may still be benefit even if your baby is born within 24 hours of the first dose.
Who should be given corticosteroids in pregnancy?
You may be advised to have corticosteroids if there is an increased chance that your baby will be born before 35 weeks of pregnancy.
This includes:
- if you are in preterm labor
- if you are suspected to be in preterm labor but this has not been confirmed yet
- if your waters break even if you are not having contractions
- if it may benefit your baby to be delivered early, for example if your baby is not growing
- if it may benefit you to have your baby early, for example if you are seriously unwell, are bleeding heavily or have severe pre-eclampsia.
If you are having a planned caesarean section before 39 weeks of pregnancy, corticosteroids are recommended to lessen the chance of breathing problems for your baby. If you have diabetes or gestational diabetes, you may need to be in hospital since corticosteroids increase the blood sugar level.
When are corticosteroids not necessary?
Giving treatment just in case an event occurs is known as prophylactic treatment. If you have previously had a baby born early, have a multiple pregnancy or have had treatment to your cervix (entrance to the womb), prophylactic treatment with corticosteroids early in pregnancy is not recommended because there is no evidence that it will help your baby.
Are there any circumstances where you wouldn’t be able to have corticosteroids?
Corticosteroids can suppress the mother’s immune system, but there is no evidence that a single course of corticosteroids will cause harm even if you have a severe infection. If you or your baby are unwell, corticosteroids will usually be started but delivery of your baby will not be delayed to allow you to complete the course.