Contents
What is a prolapsed bladder
A prolapsed bladder, also called a cystocele, anterior prolapse or dropped bladder, is the bulging or dropping of the bladder into the vagina 1. The bladder, located in the pelvis between the pelvic bones, is a hollow, muscular, balloon-shaped organ that expands as it fills with urine. During urination, also called voiding, the bladder empties through the urethra, located at the bottom of the bladder. The urethra is the tube that carries urine outside of the body. The vagina is the tube in a woman’s body that runs beside the urethra and connects the womb, or uterus, to the outside of the body.
Straining the muscles that support your pelvic organs may lead to anterior prolapse. Such straining occurs during vaginal childbirth or with chronic constipation, violent coughing or heavy lifting. Prolapsed bladder also tends to cause problems after menopause, when estrogen levels decrease 2.
For a mild or moderate prolapsed bladder , nonsurgical treatment is often effective. In more severe cases, surgery may be necessary to keep the vagina and other pelvic organs in their proper positions.
Figure 1. Urinary bladder location
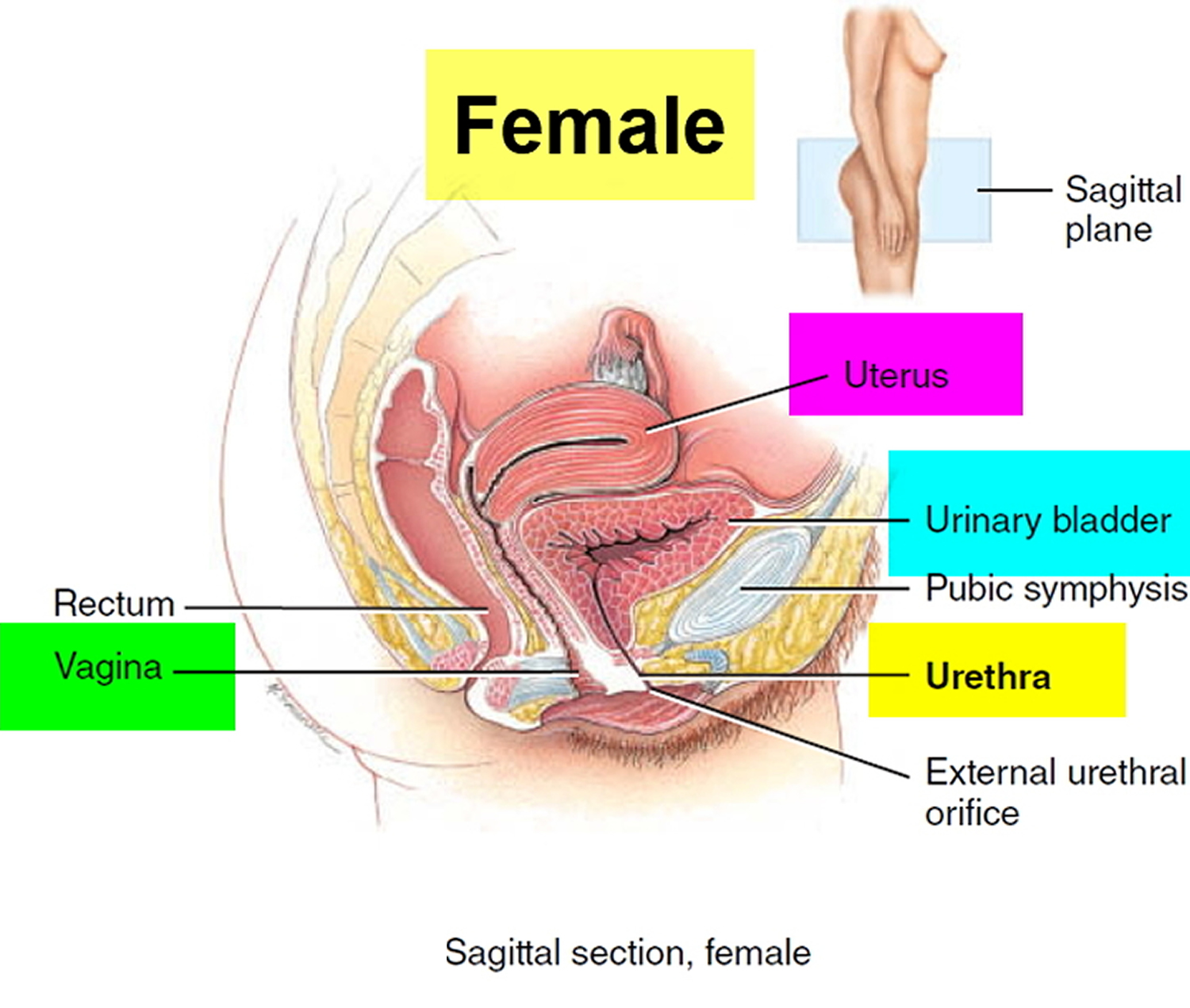
Figure 2. Urinary bladder anatomy
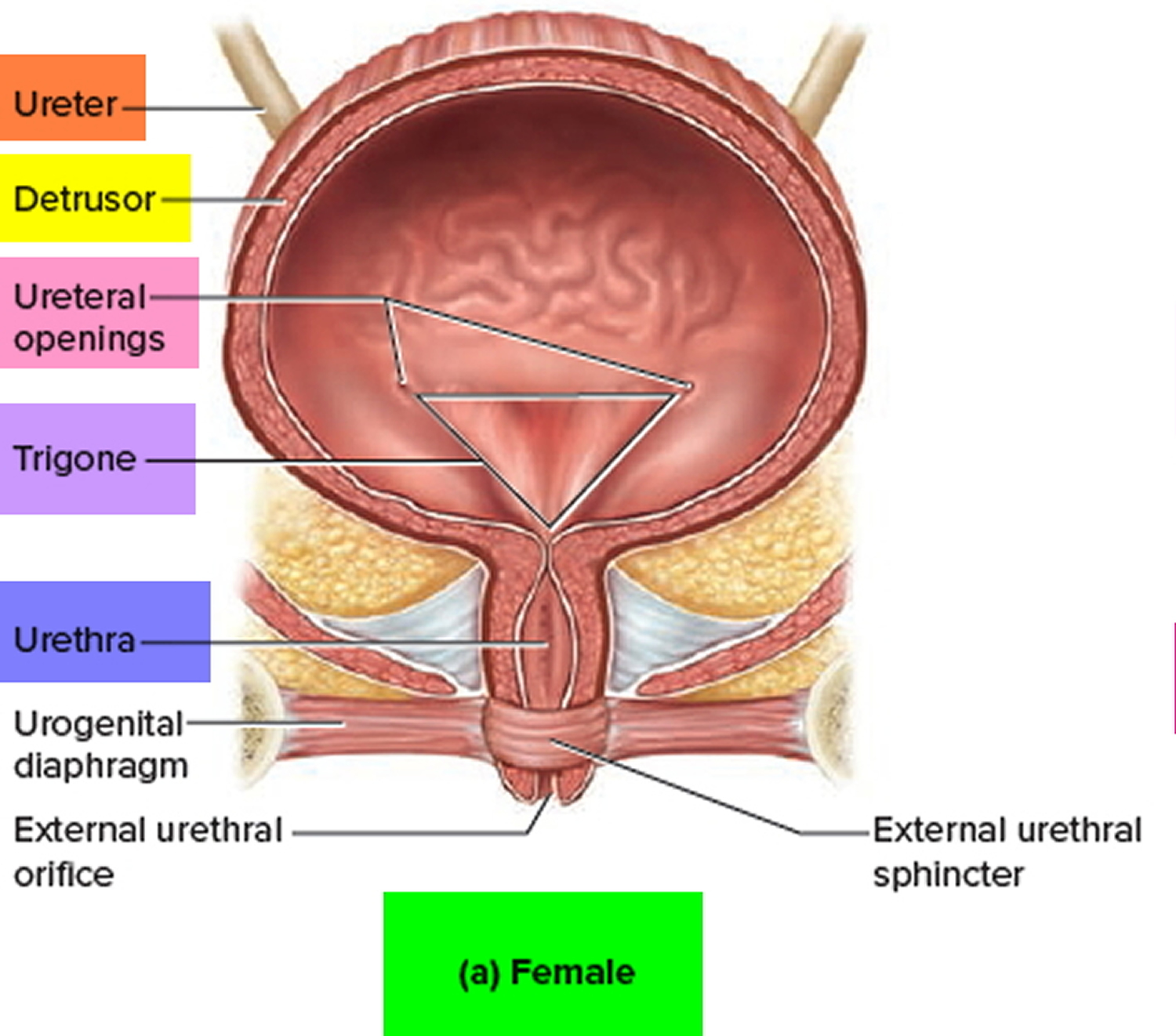
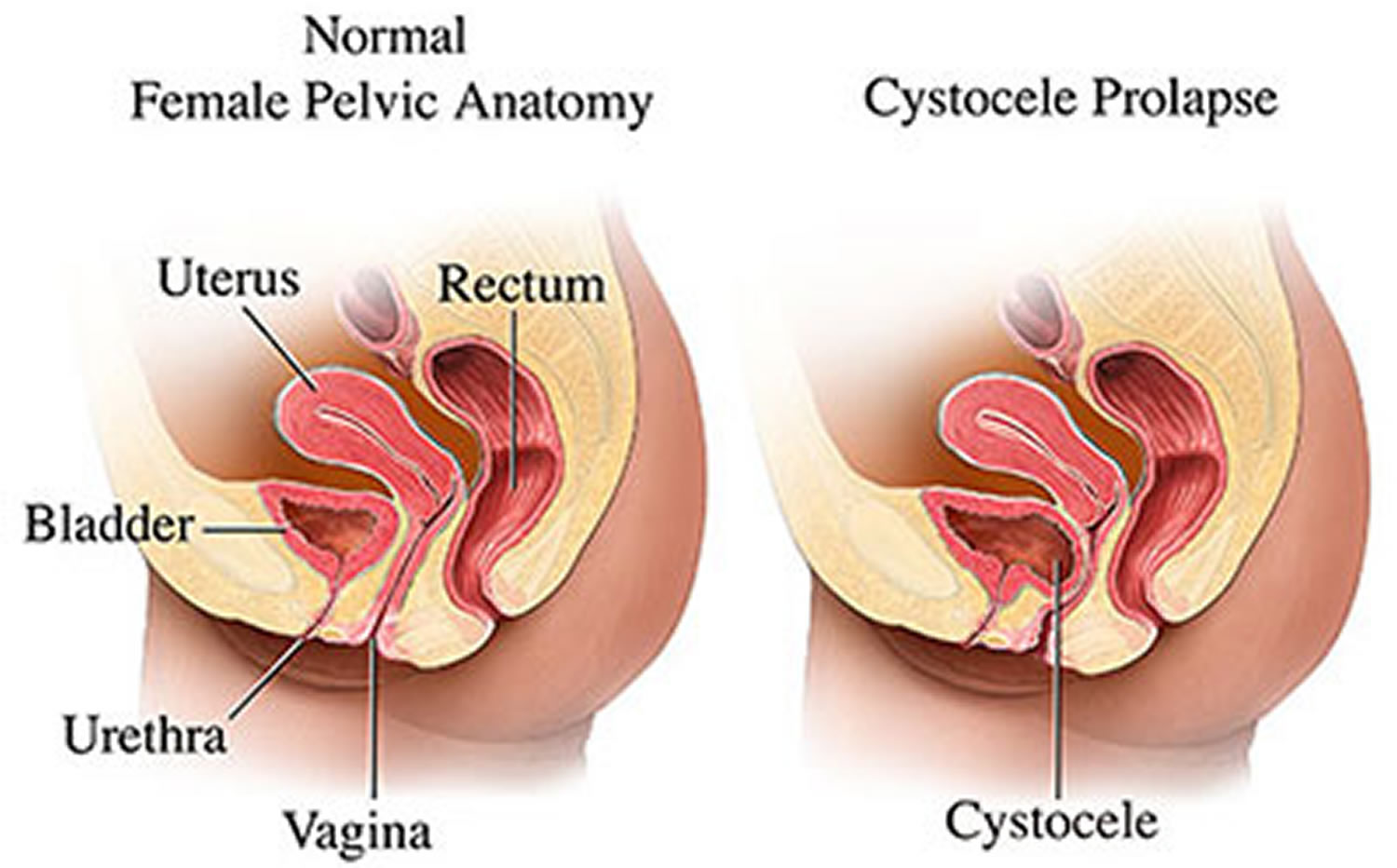
Figure 3. Prolapsed bladder
What causes prolapsed bladder ?
A prolapsed bladder occurs when the muscles, ligaments and connective tissues between a woman’s bladder and vagina weaken and stretch, letting the bladder sag from its normal position and bulge into the vagina or through the vaginal opening. In a prolapsed bladder, the bladder tissue remains covered by the vaginal skin. A prolapsed bladder may result from damage to the muscles and tissues that hold the pelvic organs up inside the pelvis. A woman’s pelvic organs include the vagina, cervix, uterus, bladder, urethra, and small intestine. Damage to or weakening of the pelvic muscles and supportive tissues may occur after vaginal childbirth and with conditions that repeatedly strain or increase pressure in the pelvic area, such as:
- pregnancy and vaginal childbirth
- repetitive straining for bowel movements
- constipation
- chronic or violent coughing
- heavy lifting
- being overweight or obese
A woman’s chances of developing a cystocele increase with age, possibly because of weakening muscles and supportive tissues from aging. Whether menopause increases a woman’s chances of developing a prolapsed bladder is unclear.
Risk factors for prolapsed bladder
These factors may increase your risk of anterior prolapse:
- Childbirth. Women who have vaginally delivered one or more children have a higher risk of anterior prolapse.
- Aging. Your risk of anterior prolapse increases as you age. This is especially true after menopause, when your body’s production of estrogen — which helps keep the pelvic floor strong — decreases.
- Hysterectomy. Having your uterus removed may contribute to weakness in your pelvic floor support.
- Genetics. Some women are born with weaker connective tissues, making them more susceptible to anterior prolapse.
- Obesity. Women who are overweight or obese are at higher risk of anterior prolapse.
What are the symptoms of a prolapsed bladder ?
Women with mild prolapsed bladders often do not have any symptoms.
The symptoms of a prolapsed bladder may include:
- a vaginal bulge
- the feeling that something is falling out of the vagina
- a feeling of fullness or pressure in your pelvis and vagina
- difficulty starting a urine stream
- a feeling that you haven’t completely emptied your bladder after urinating
- frequent or urgent urination
- increased discomfort when you strain, cough, bear down or lift
- repeated bladder infections
- pain or urinary leakage during sexual intercourse
- in severe cases, a bulge of tissue that protrudes through your vaginal opening and may feel like sitting on an egg
Signs and symptoms often are especially noticeable after standing for long periods of time and may go away when you lie down.
Women who have a prolapsed bladder may also leak some urine as a result of movements that put pressure on the bladder, called stress urinary incontinence. These movements can include coughing, sneezing, laughing, or physical activity, such as walking. Urinary retention—the inability to empty the bladder completely—may occur with more severe cystoceles if the prolapsed bladder creates a kink in the woman’s urethra and blocks urine flow.
How is a prolapsed bladder diagnosed ?
Diagnosing a prolapsed bladder requires medical tests and a physical exam of the vagina. Medical tests take place in a health care provider’s office, an outpatient center, or a hospital. The health care provider will ask about symptoms and medical history. A health care provider uses a grading system to determine the severity of a woman’s prolapsed bladder . A cystocele receives one of three grades depending on how far a woman’s bladder has dropped into her vagina:
- Grade 1—Mild, when the bladder drops only a short way into the vagina
- Grade 2—Moderate, when the bladder drops far enough to reach the opening of the vagina
- Grade 3—Most advanced, when the bladder bulges out through the opening of the vagina
If a woman has difficulty emptying her bladder, a health care provider may measure the amount of urine left in the woman’s bladder after she urinates. The remaining urine is called the postvoid residual. A health care provider can measure postvoid residual with a bladder ultrasound. A bladder ultrasound uses a device, called a transducer, that bounces safe, painless sound waves off the bladder to create an image and show the amount of remaining urine. A specially trained technician performs the procedure, and a radiologist—a doctor who specializes in medical imaging—interprets the images. A woman does not need anesthesia.
A health care provider can also use a catheter—a thin, flexible tube—to measure a woman’s postvoid residual. The health care provider inserts the catheter through the woman’s urethra into her bladder to remove and measure the amount of remaining urine after the woman has urinated. A postvoid residual of 100 mL or more is a sign that the woman is not completely emptying her bladder. A woman receives local anesthesia.
A health care provider may use a voiding cystourethrogram—an x-ray exam of the bladder—to diagnose a cystocele as well. A woman gets a voiding cystourethrogram while urinating. The x-ray images show the shape of the woman’s bladder and let the health care provider see any problems that might block normal urine flow. An x-ray technician performs a voiding cystourethrogram, and a radiologist interprets the images. A woman does not need anesthesia; however, some women may receive sedation. A health care provider may order additional tests to rule out problems in other parts of a woman’s urinary tract.
How is a prolapsed bladder treated ?
Prolapsed bladder treatment depends on the severity of the cystocele and whether a woman has symptoms. If a woman’s prolapsed bladder does not bother her, a health care provider may recommend only that she avoid heavy lifting or straining, which could worsen her prolapsed bladder. If a woman has symptoms that bother her and wants treatment, the health care provider may recommend pelvic muscle exercises, a vaginal pessary, or surgery.
Mild cases — those with few or no obvious symptoms — typically don’t require treatment. You could opt for a wait-and-see approach, with occasional visits to your doctor to see if your prolapse is worsening, along with self-care measures, such as exercises that strengthen your pelvic floor muscles.
Pelvic floor, or Kegel, exercises involve strengthening pelvic floor muscles. Strong pelvic floor muscles more effectively hold pelvic organs in place. A woman does not need special equipment for Kegel exercises.
The exercises involve tightening and relaxing the muscles that support pelvic organs. A health care provider can help a woman learn proper technique.
What are Kegel exercises ?
To do Kegel exercises, you just squeeze your pelvic floor muscles. The part of your body including your hip bones is the pelvic area. At the bottom of the pelvis, several layers of muscle stretch between your legs. The muscles attach to the front, back, and sides of the pelvic bone.
Kegel exercises are designed to make your pelvic floor muscles stronger. These are the muscles that hold up your bladder and help keep it from leaking.
Building up your pelvic muscles with Kegel exercises can help with your bladder control.
How do you exercise your pelvic muscles ?
Find the right muscles. Try one of the following ways to find the right muscles to squeeze.
- Imagine that you are trying to stop passing gas. Squeeze the muscles you would use. If you sense a “pulling” feeling, you are squeezing the right muscles for pelvic exercises.
- Imagine that you are sitting on a marble and want to pick up the marble with your vagina. Imagine “sucking” the marble into your vagina.
- If you still are not sure you are tightening the right muscles: Lie down and put your finger inside your vagina. Squeeze as if you were trying to stop urine from coming out. If you feel tightness on your finger, you are squeezing the right pelvic muscles.
Once you know what the movement feels like, do Kegel exercises three times a day:
- Make sure your bladder is empty, then sit or lie down.
- Tighten the pelvic floor muscles. Hold tight and count to 6 to 8.
- Relax the muscles and count to 10.
- Repeat 10 times, three times a day (morning, afternoon, and night).
At first, find a quiet spot to practice—your bathroom or bedroom—so you can concentrate. Lie on the floor. Pull in the pelvic muscles and hold for a count of 6 to 8. Then relax for a count of 10. Work up to 10 to 15 repeats each time you exercise.
Do your pelvic exercises at least three times a day. Every day, use three positions: lying down, sitting, and standing. You can exercise while lying on the floor, sitting at a desk, or standing in the kitchen. Using all three positions makes the muscles strongest.
Breathe deeply, and relax your body when you are doing these exercises. Make sure you are not tightening your stomach, thigh, buttock, or chest muscles.
After 4 to 6 weeks, you should feel better and have fewer symptoms. Keep doing the exercises, but do not increase how many you do. Overdoing it can lead to straining when you urinate or move your bowels.
Some notes of caution:
- Once you learn how to do them, do not practice Kegel exercises at the same time you are urinating more than twice a month. Doing the exercises while you are urinating can weaken your pelvic floor muscles over time.
- In women, doing Kegel exercises incorrectly or with too much force may cause vaginal muscles to tighten too much. This can cause pain during sexual intercourse.
- Incontinence will return if you stop doing these exercises. Once you start doing them, you may need to do them for the rest of your life.
It may take several months for your incontinence to lessen once you start doing these exercises.
Let your doctor, nurse, or therapist help you. Many people have trouble finding the right muscles. Your doctor, nurse, or therapist can check to make sure you are doing the exercises correctly. You can also exercise by using special weights or biofeedback. Ask your health care team about these exercise aids.
Don’t squeeze other muscles at the same time. Be careful not to tighten your stomach, legs, or other muscles. Squeezing the wrong muscles can put more pressure on your bladder control muscles. Just squeeze the pelvic muscle. Don’t hold your breath.
Be patient. Don’t give up. It’s just 5 minutes, three times a day. You may not feel your bladder control improve until after 3 to 6 weeks. Still, most women do notice an improvement after a few weeks.
If self-care measures aren’t effective, anterior prolapse treatment might involve:
A supportive device (pessary). A vaginal pessary is a small, silicone medical device placed in the vagina that supports the vaginal wall and holds the bladder in place. Pessaries come in a number of shapes and sizes. A health care provider has many options to choose from to find the most comfortable pessary for a woman. Your doctor or other care provider fits you for the device and shows you how to clean and reinsert it on your own. Many women use pessaries as a temporary alternative to surgery, and some use them when surgery is too risky.
Estrogen therapy. Your doctor may recommend using estrogen — usually a vaginal cream, pill or ring — especially if you’ve already experienced menopause. This is because estrogen, which helps keep pelvic muscles strong, decreases after menopause.
When surgery is necessary
If you have noticeable, uncomfortable symptoms, anterior prolapse may require surgery.
A heath care provider may recommend surgery to repair the vaginal wall support and reposition the woman’s bladder to its normal position. The most common cystocele repair is an anterior vaginal repair—or anterior colporrhaphy. The surgeon makes an incision in the wall of the woman’s vagina and repairs the defect by folding over and sewing together extra supportive tissue between the vagina and bladder. The repair tightens the layers of tissue that separate the organs, creating more support for the bladder. A surgeon who specializes in the urinary tract or female reproductive system performs an anterior vaginal repair in a hospital. The woman receives either regional or general anesthesia. The woman may stay overnight in the hospital, and full recovery may take up to 4 to 6 weeks.
How it’s done. Often, the surgery is performed vaginally and involves lifting the prolapsed bladder back into place, removing extra tissue, and tightening the muscles and ligaments of the pelvic floor. Your doctor may use a special type of tissue graft to reinforce vaginal tissues and increase support if your vaginal tissues seem very thin.
If you have a prolapsed uterus. For anterior prolapse associated with a prolapsed uterus, your doctor may recommend removing the uterus (hysterectomy) in addition to repairing the damaged pelvic floor muscles, ligaments and other tissues.
If you’re thinking about becoming pregnant, your doctor may recommend that you delay surgery until after you’re done having children. Using a pessary may help relieve your symptoms in the meantime. The benefits of surgery can last for many years, but there’s some risk of recurrence — which may mean another surgery at some point.
Dealing with incontinence
If your anterior prolapse is accompanied by stress incontinence — involuntary loss of urine during strenuous activity — your doctor may recommend one of a number of procedures to support the urethra (urethral suspension) and ease your incontinence symptoms.
Home remedies for prolapsed bladder
Kegel exercises strengthen your pelvic floor muscles, which support the uterus, bladder and bowel. A strengthened pelvic floor provides better support for your pelvic organs and relief from symptoms associated with anterior prolapse.
Ask your health care provider for feedback on whether you’re using the right muscles. Kegel exercises may be most successful when they’re taught by a physical therapist and reinforced with biofeedback. Biofeedback involves using monitoring devices that help ensure you’re tightening the proper muscles with optimal intensity and length of time.
Once you’ve learned the proper method, you can do Kegel exercises discreetly just about anytime, whether you’re sitting at your desk or relaxing on the couch.
Prevention of prolapsed bladder
To reduce your risk of developing anterior prolapse, try these self-care measures:
- Perform Kegel exercises on a regular basis. These exercises can strengthen your pelvic floor muscles, and this is especially important after you have a baby.
- Treat and prevent constipation. High-fiber foods can help.
- Avoid heavy lifting, and lift correctly. When lifting, use your legs instead of your waist or back.
- Control coughing. Get treatment for a chronic cough or bronchitis, and don’t smoke.
- Avoid weight gain. Talk to your doctor to determine your ideal weight and get advice on weight-loss strategies, if you need them.
- Cystocele (Prolapsed Bladder). National Institute of Diabetes and Digestive and Kidney Diseases. https://www.niddk.nih.gov/health-information/urologic-diseases/bladder-control-problems-women/cystocele-prolapsed-bladder[↩]
- Anterior prolapse (cystocele). Mayo Clinic. https://www.mayoclinic.org/diseases-conditions/cystocele/basics/definition/con-20026175[↩]