Contents
What is Raynaud’s disease
Raynaud’s disease is a rare disorder of the blood vessels – the arteries, usually in the fingers and toes. Raynaud’s disease causes the blood vessels to narrow (vasospasm) when you are cold or feeling stressed. When this happens, blood can’t get to the surface of the skin and the affected areas turn white and blue. When the blood flow returns, the skin turns red and throbs or tingles. Attacks generally last for minutes to hours and can vary. Most people who have Raynaud’s disease have no long-term tissue damage or disability. However, people who have severe Raynaud’s disease can develop skin sores or gangrene from prolonged or repeated Raynaud’s attacks. In severe cases, loss of blood flow can cause sores or tissue death. “Gangrene” refers to the death or decay of body tissues.
Raynaud’s disease sometimes is called Raynaud’s syndrome or Raynaud’s phenomenon depending on the cause.
People in colder climates are more likely to develop Raynaud’s disease.
Raynaud’s disease is a common disease affecting 5% of the US population and it is also more common in young women and in people with a family history, and those over age 30.
Vasospasm of the arteries reduces blood flow to the fingers and toes. In people who have Raynaud’s disease, the disorder usually affects the fingers. In about 40 percent of people who have Raynaud’s disease, it affects the toes. Rarely, Raynaud’s disease affects the nose, ears, nipples, and lips.
There are two main types of Raynaud’s—primary and secondary.
- In Primary Raynaud’s (also called Raynaud’s disease), the cause is not known. Primary Raynaud’s is more common and tends to be less severe than secondary Raynaud’s. It can be so mild that many people with primary Raynaud’s don’t seek treatment. And it can resolve on its own.
- Secondary Raynaud’s is caused by an underlying disease, injuries, condition, certain medicines or other factor. This type of Raynaud’s is often called Raynaud’s phenomenon. Although secondary Raynaud’s is less common than the primary form, it tends to be more serious.
Over 90% of patients with Raynaud’s phenomenon are female and, at the time of presentation, are often aged under 25. Up to 5% of patients initially presenting with only symptoms of Raynaud’s eventually develop an autoimmune rheumatic disease.
If you have primary or secondary Raynaud’s, cold temperatures or stress can trigger “Raynaud’s attacks.” During an attack, little or no blood flows to affected body parts.
As a result, the skin may turn white and then blue for a short time. As blood flow returns, the affected areas may turn red and throb, tingle, burn, or feel numb.
In both types of Raynaud’s, even mild or brief changes in temperature can cause Raynaud’s attacks. For example, taking something out of the freezer or being exposed to temperatures below 60 degrees Fahrenheit (15.6 °C) can cause your fingers to turn blue.
For most people who have primary Raynaud’s disease, the disorder is more of a bother than a serious illness. They usually can manage the condition with minor lifestyle changes.
Secondary Raynaud’s phenomenon may be harder to manage. However, several treatments are available to help prevent or relieve symptoms. With secondary Raynaud’s disease, it’s important to treat the underlying disease or condition that’s causing it.
Causes of secondary Raynaud’s (Raynaud’s phenomenon) include:
- Connective tissue diseases. Most people who have a rare disease that leads to hardening and scarring of the skin (scleroderma) have Raynaud’s. Other diseases that increase the risk of Raynaud’s include lupus, rheumatoid arthritis and Sjogren’s syndrome.
- Diseases of the arteries. These include a buildup of plaques in blood vessels that feed the heart (atherosclerosis), a disorder in which the blood vessels of the hands and feet become inflamed (Buerger’s disease), and a type of high blood pressure that affects the arteries of the lungs (primary pulmonary hypertension).
- Carpal tunnel syndrome. This condition involves pressure on a major nerve to your hand, producing numbness and pain in the hand that can make the hand more susceptible to cold temperatures.
- Repetitive action or vibration. Typing, playing piano or doing similar movements for long periods and operating vibrating tools, such as jackhammers, can lead to overuse injuries.
- Smoking. Smoking constricts blood vessels.
- Injuries to the hands or feet. These include wrist fracture, surgery or frostbite.
- Certain medications. These include beta blockers, used to treat high blood pressure; migraine medications that contain ergotamine or sumatriptan; attention-deficit/hyperactivity disorder medications; certain chemotherapy agents; and drugs that cause blood vessels to narrow, such as some over-the-counter cold medications.
Researchers continue to look for better ways to diagnose and treat Raynaud’s disease.
Treatment for Raynaud’s disease may include drugs to keep the blood vessels open. There are also simple things you can do yourself, such as:
- Soaking hands in warm water at the first sign of an attack
- Keeping your hands and feet warm in cold weather
- Avoiding triggers, such as certain medicines and stress.
Can you die from Raynaud’s disease
No. If you have primary or secondary Raynaud’s, cold temperatures or stress can trigger “Raynaud’s attacks.” For most people who have primary Raynaud’s disease, the disorder is more of a bother than a serious illness. You usually can manage the condition with minor lifestyle changes e.g. quit smoking, avoid cold temperatures. Dressing for the cold in layers and wearing mittens or heavy socks usually are effective in dealing with mild symptoms of Raynaud’s. And if you have secondary Raynaud’s (Raynaud’s phenomenon), it’s important to treat the underlying disease or condition that’s causing it.
A variety of steps can decrease Raynaud’s attacks and help you feel better.
- Avoid smoke. Smoking or inhaling secondhand smoke causes skin temperature to drop by constricting blood vessels, which can lead to an attack.
- Exercise. Exercise can increase circulation, among other health benefits. If you have secondary Raynaud’s, talk to your doctor before exercising outdoors in the cold.
- Control stress. Learning to recognize and avoid stressful situations might help control the number of attacks.
- Avoid rapidly changing temperatures. Try not to move from a hot environment to an air-conditioned room. If possible, avoid frozen-food sections of grocery stores.
To help prevent Raynaud’s attacks:
- Bundle up outdoors. When it’s cold, don a hat, scarf, socks and boots, and two layers of mittens or gloves before you go outside. Wear a coat with snug cuffs to go around your mittens or gloves, to prevent cold air from reaching your hands.
- Use chemical hand warmers. Wear earmuffs and a face mask if the tip of your nose and your earlobes are sensitive to cold.
- Warm your car. Run your car heater for a few minutes before driving in cold weather.
- Take precautions indoors. Wear socks. When taking food out of the refrigerator or freezer, wear gloves, mittens or oven mitts. Some people find it helpful to wear mittens and socks to bed during winter. Because air conditioning can trigger attacks, set your air conditioner to a warmer temperature. Use insulated drinking glasses.
What to do during an Raynaud’s attack
Warm your hands, feet or other affected areas. To gently warm your fingers and toes:
- Get indoors or to a warmer area
- Wiggle your fingers and toes
- Place hands under armpits
- Make wide circles (windmills) with your arms
- Run warm — not hot — water over your fingers and toes
- Massage your hands and feet
If stress triggers an attack, get out of the stressful situation and relax. Practice a stress-reduction technique that works for you, and warm your hands or feet in water to help lessen the attack.
Lifestyle changes and supplements that encourage better circulation might help you manage Raynaud’s. However, the evidence of effectiveness is unclear and more study is needed. If you’re interested, talk to your doctor about:
- Fish oil. Taking fish oil supplements could help improve your tolerance to cold.
- Ginkgo. Ginkgo supplements could help decrease the number of Raynaud’s attacks.
- Acupuncture. This practice appears to improve blood flow, so it may be helpful in relieving Raynaud’s attacks.
- Biofeedback. Using your mind to control body temperature might help decrease the severity and frequency of attacks. Biofeedback includes guided imagery to increase the temperature of hands and feet, deep breathing, and other relaxation exercises.
Your doctor may be able to suggest a therapist who can help you learn biofeedback techniques. There are books and DVDs on the subject.
Talk to your doctor before taking supplements. Your doctor can warn you if there are potential drug interactions or side effects of alternative treatments.
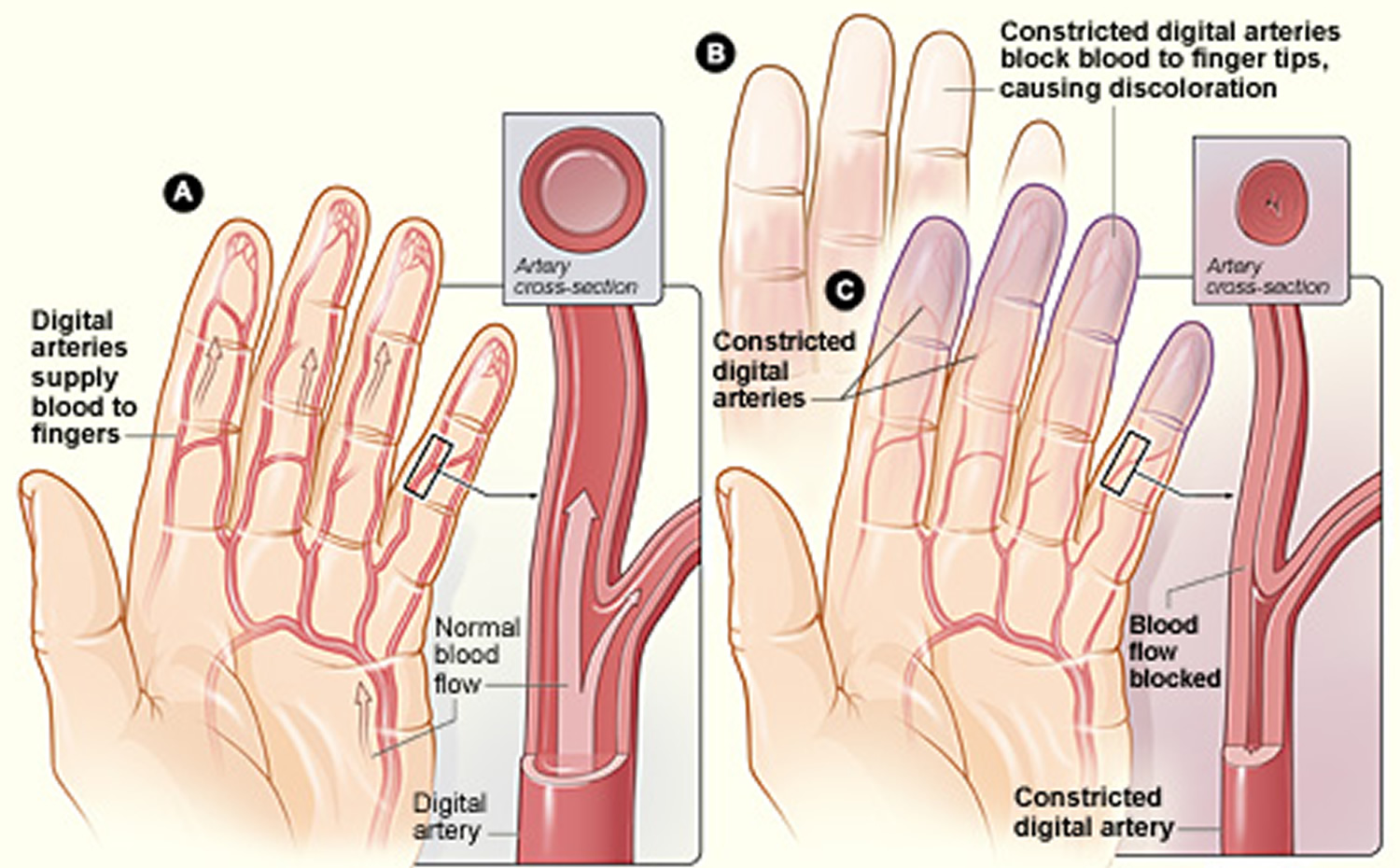
Figure 1. Raynaud’s disease
Note: Figure A shows arteries in the fingers (digital arteries) with normal blood flow. The inset image shows a cross-section of a digital artery. Figure B shows fingertips that have turned white due to blocked blood flow. Figure C shows narrowed digital arteries, causing blocked blood flow and blue fingertips. The inset image shows a cross-section of a narrowed digital artery.
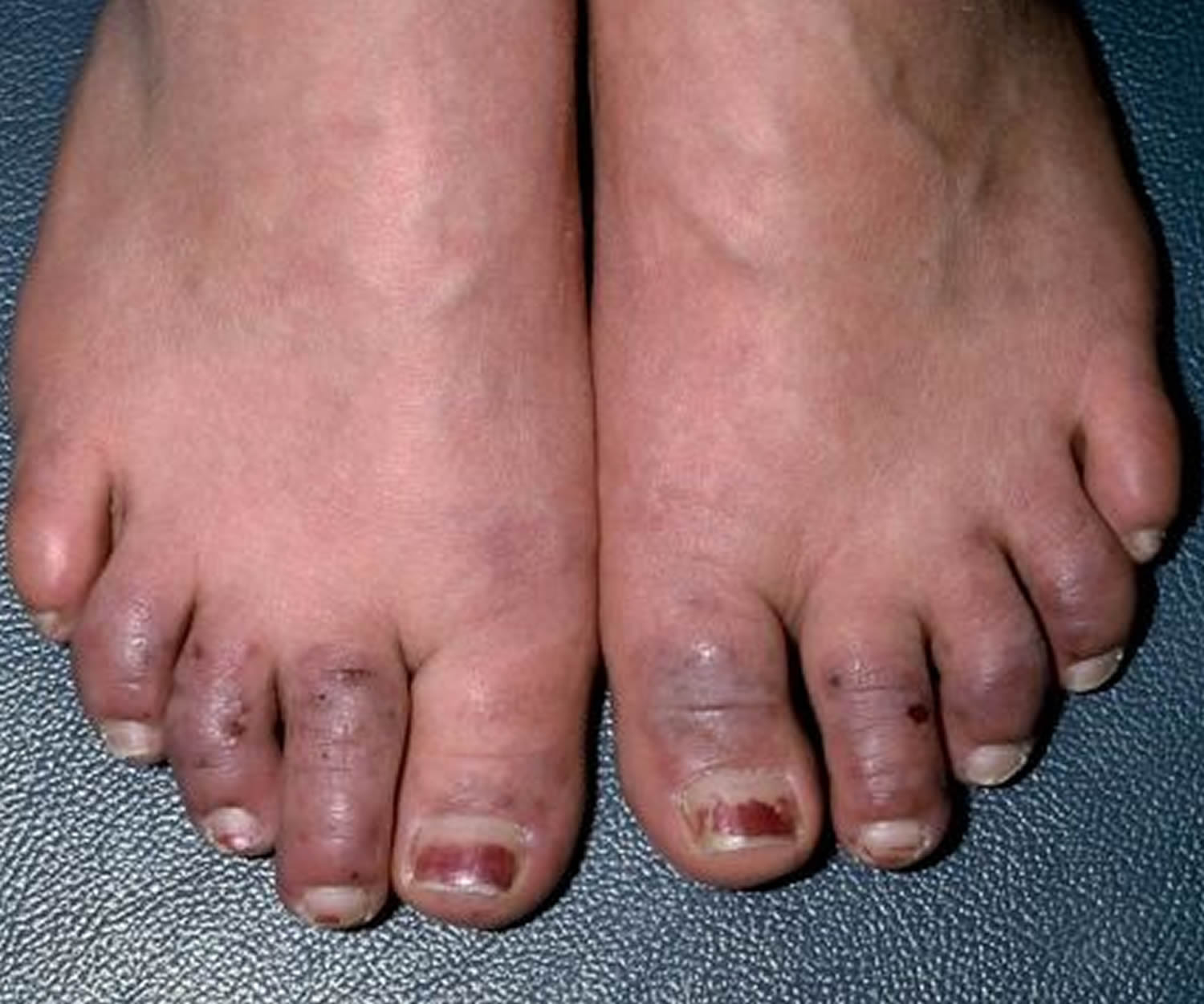
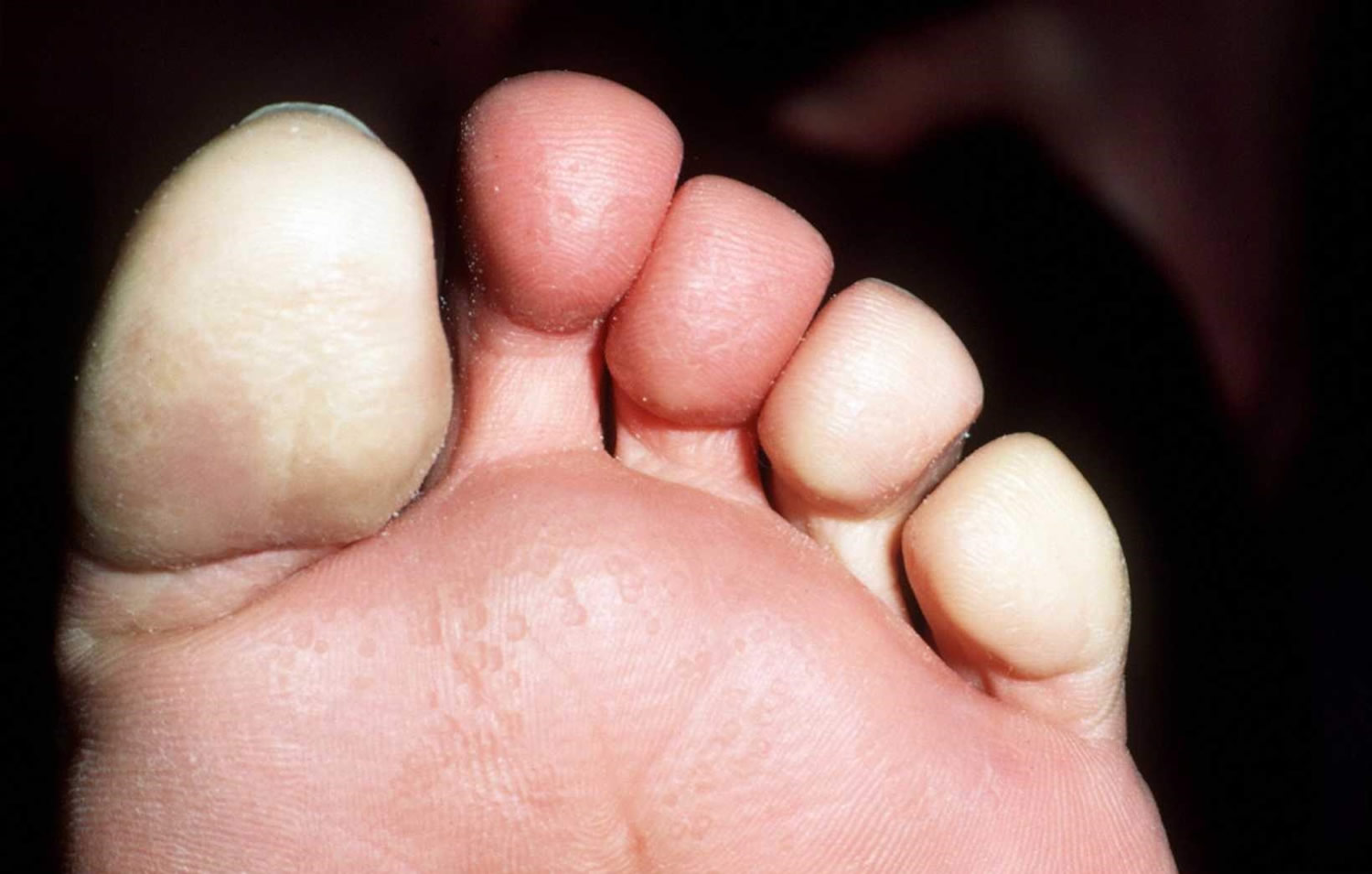
Figure 2. Raynaud’s disease feet
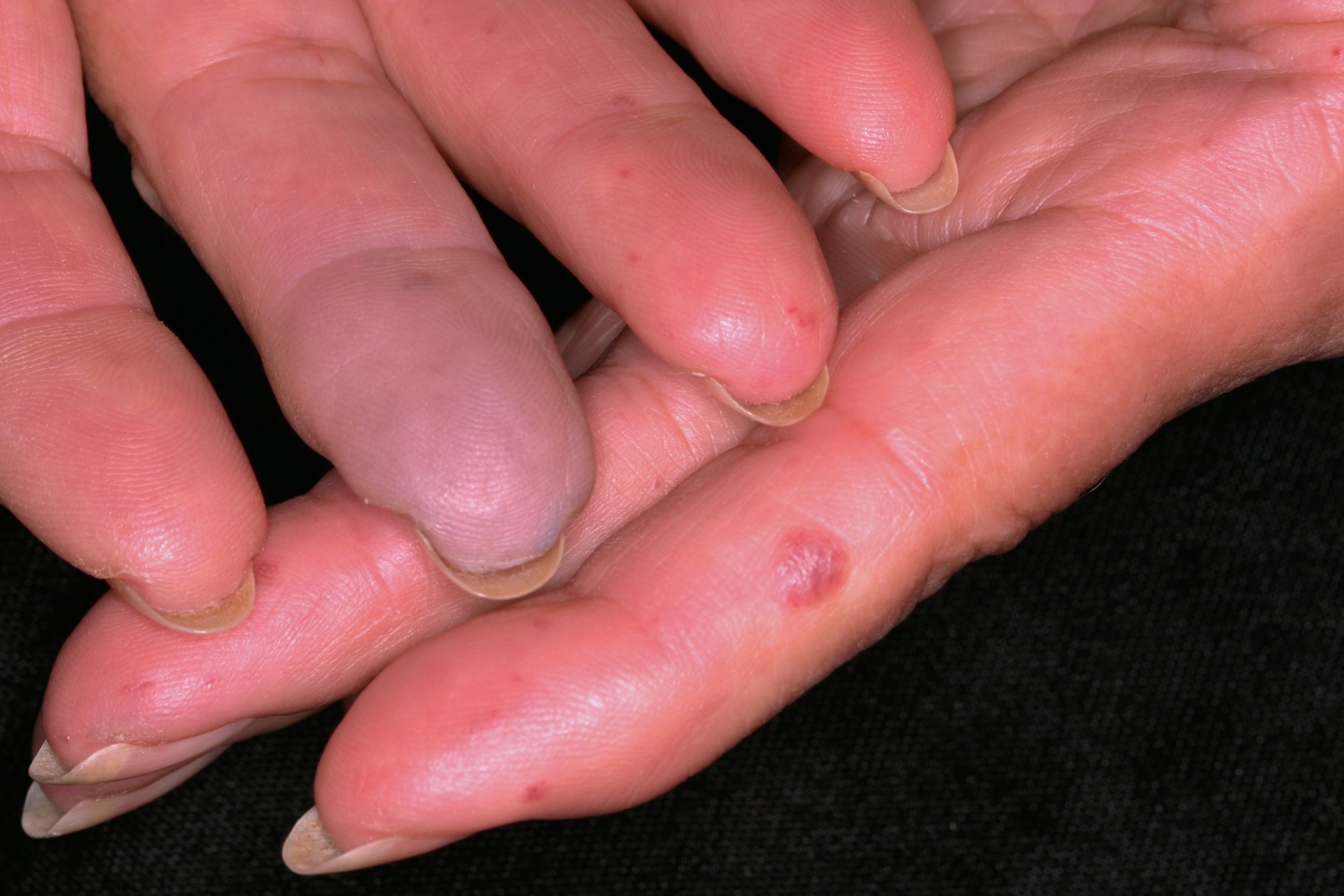
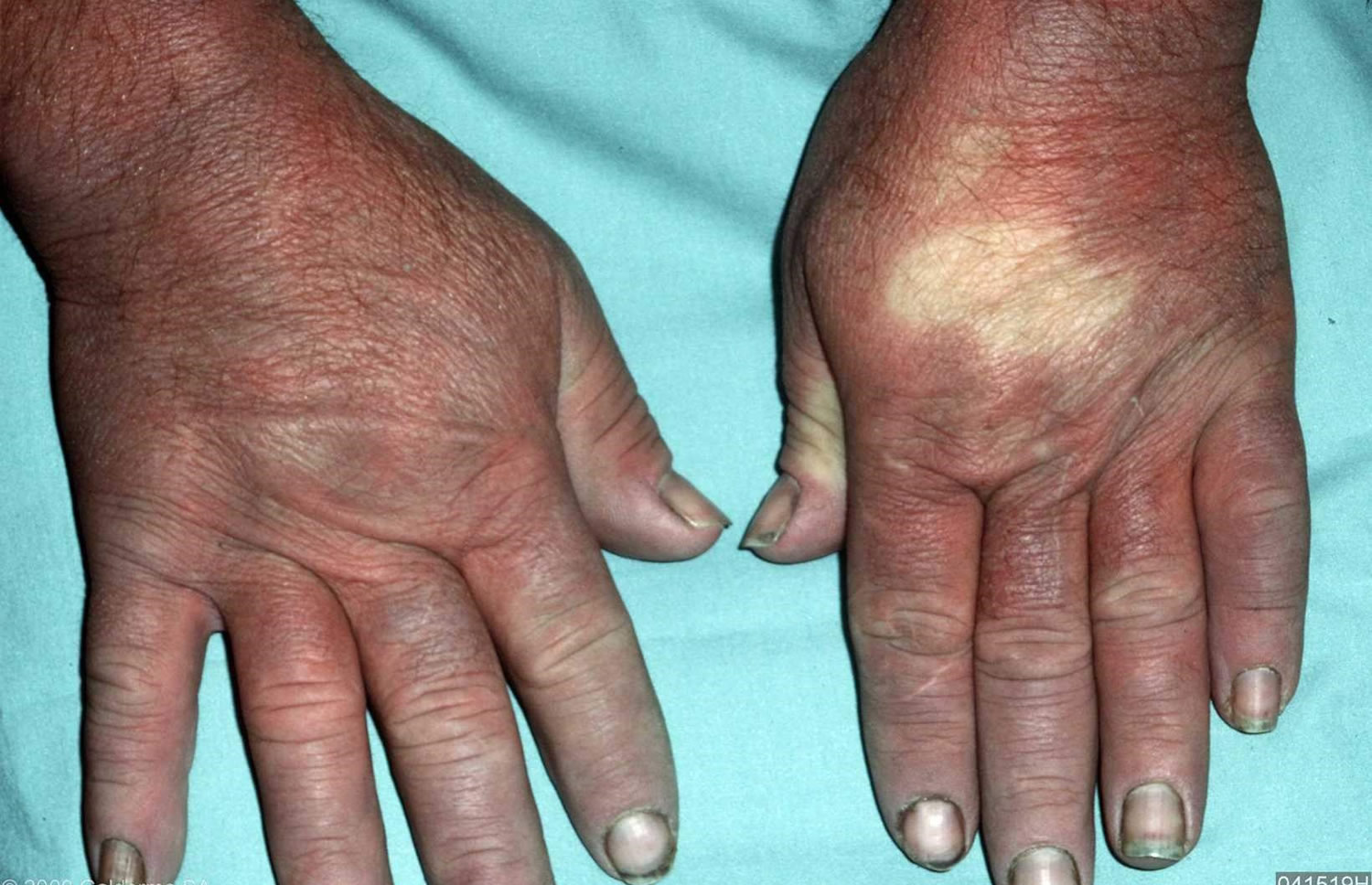
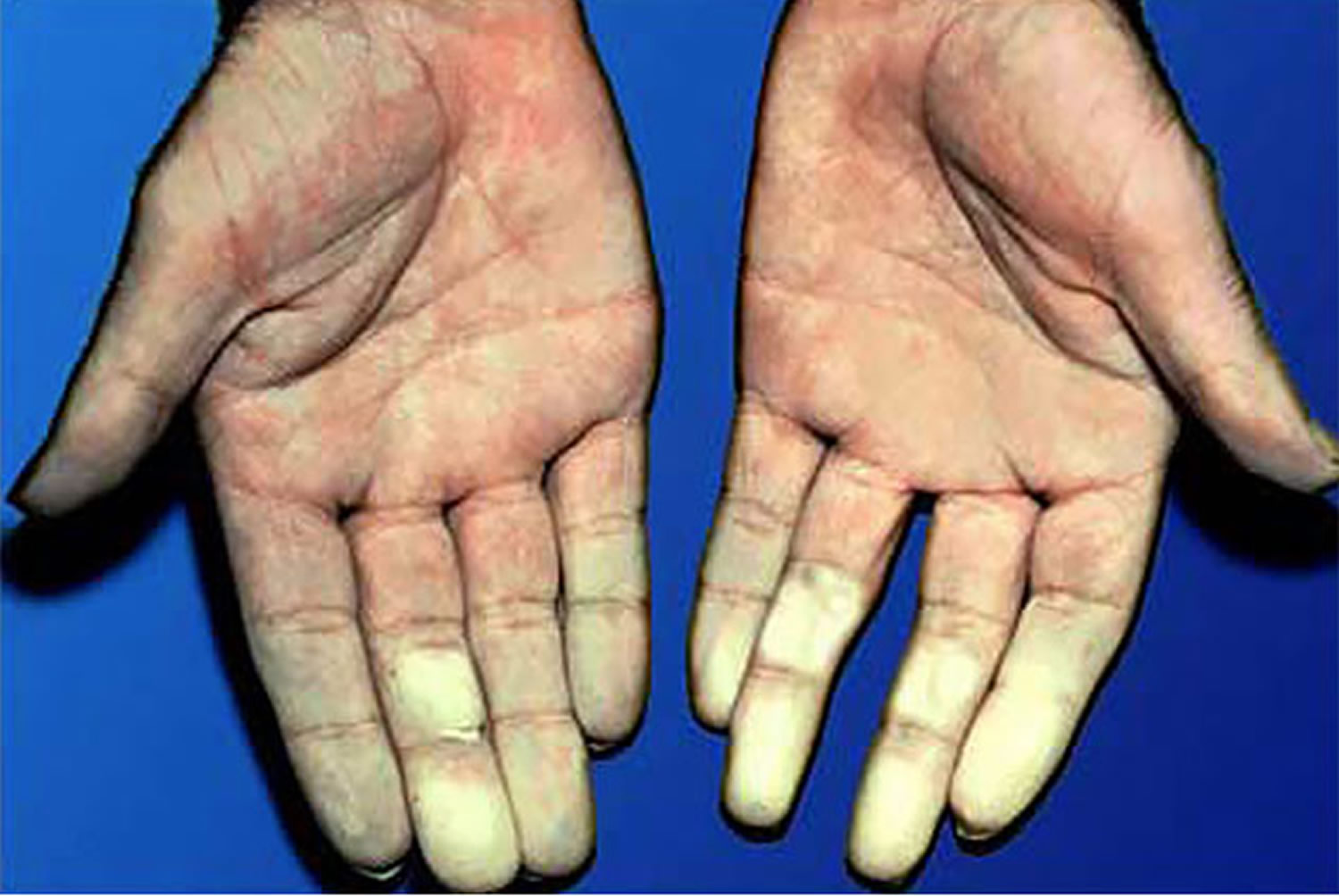
Figure 3. Raynaud’s disease fingers
Raynaud’s phenomenon complications
If secondary Raynaud’s is severe — which is rare — diminished blood circulation to your fingers or toes could cause tissue damage.
A completely blocked artery can lead to sores (skin ulcers) or dead tissue (gangrene), both of which can be difficult to treat. Rarely, extreme untreated cases might require removing the affected part of your body (amputation).
Raynaud’s disease causes
There are two main types of Raynaud’s—primary and secondary.
In primary Raynaud’s (also called Raynaud’s disease), the cause isn’t known, but blood vessels in the hands and feet appear to overreact to cold temperatures or stress. Primary Raynaud’s is more common and tends to be less severe than secondary Raynaud’s.
Secondary Raynaud’s is caused by an underlying disease, condition, or other factor. This type of Raynaud’s is often called Raynaud’s phenomenon.
With Raynaud’s, arteries to your fingers and toes go into vasospasm when exposed to cold or stress, narrowing your vessels and temporarily limiting blood supply. Over time, these small arteries can thicken slightly, further limiting blood flow.
Cold temperatures are most likely to trigger an attack. Exposure to cold, such as putting your hands in cold water, taking something from a freezer or being in cold air, is the most likely trigger. For some people, emotional stress can trigger an episode.
Causes of Secondary Raynaud’s
Many things can cause secondary Raynaud’s. Examples include:
- Diseases and conditions that directly damage the arteries or damage the nerves that control the arteries in the hands and feet
- Repetitive actions that damage the nerves that control the arteries in the hands and feet
- Injuries to the hands and feet
- Exposure to certain chemicals
- Medicines that narrow the arteries or affect blood pressure
Diseases and Conditions
Secondary Raynaud’s is linked to diseases and conditions that directly damage the arteries. The disorder also is linked to diseases and conditions that damage the nerves that control the arteries in the hands and feet.
For example, Raynaud’s occurs in most people who have scleroderma. It also is a common problem for people with lupus.
Other examples of diseases and conditions that can cause Raynaud’s phenomenon include:
- Rheumatoid arthritis
- Atherosclerosis
- Blood disorders such as cryoglobulinemia and polycythemia vera
- Sjögren’s syndrome, dermatomyositis, and polymyositis
- Buerger’s disease
Thyroid problems and pulmonary hypertension also may cause Raynaud’s.
Repetitive Actions
Repetitive actions that damage the arteries or the nerves that control the arteries in the hands and feet may lead to Raynaud’s.
Typing, playing the piano, or doing other similar movements repeatedly over long periods may lead to secondary Raynaud’s. Using vibrating tools, such as jackhammers and drills, also may raise your risk of developing Raynaud’s.
Hand or Foot Injuries
Injuries to the hands or feet from accidents, frostbite, surgery, or other causes can lead to Raynaud’s.
Chemicals
Exposure to certain workplace chemicals can cause a scleroderma-like illness that’s linked to Raynaud’s. An example of this type of chemical is vinyl chloride, which is used in the plastics industry.
The nicotine in cigarettes also can raise your risk of developing Raynaud’s.
Medicines
Certain medicines can cause secondary Raynaud’s, including:
- Migraine headache medicines that contain ergotamine. This substance causes the arteries to narrow.
- Certain cancer medicines, such as cisplatin and vinblastine.
- Some over-the-counter cold and allergy medicines and diet aids. Some of these medicines can narrow your arteries.
- Beta blockers. These medicines slow your heart rate and lower your blood pressure.
- Birth control pills. These medicines can affect blood flow.
Risk Factors for Raynaud’s disease
The risk factors for primary Raynaud’s (Raynaud’s disease) and secondary Raynaud’s (Raynaud’s phenomenon) are different.
The risk factors for primary Raynaud’s include:
- Gender. Women are more likely to have primary Raynaud’s than men.
- Age. Primary Raynaud’s usually develops before the age of 30.
- Family history. Primary Raynaud’s may occur in members of the same family. A first-degree relative — a parent, sibling or child — having the disease appears to increase your risk of primary Raynaud’s.
- Living in a cold climate. Cold temperatures can trigger Raynaud’s attacks.
The risk factors for secondary Raynaud’s include:
- Age. Secondary Raynaud’s usually develops after the age of 30.
- Certain diseases and conditions. For example, diseases that directly damage the arteries or damage the nerves that control the arteries in the hands and feet may cause secondary Raynaud’s.
- Injuries to the hands or feet.
- Exposure to certain workplace chemicals, such as vinyl chloride (used in the plastics industry).
- Repetitive actions with the hands, such as typing or using vibrating tools.
- Certain medicines, such as migraine, cancer, cold/allergy, or blood pressure medicines.
- Smoking.
- Living in a cold climate.
Raynaud’s disease symptoms
People who have primary Raynaud’s (Raynaud’s disease) or secondary Raynaud’s (Raynaud’s phenomenon) can have attacks in response to cold temperatures or emotional stress.
Raynaud’s attacks usually affect the fingers and toes. Rarely, the attacks affect the nose, ears, nipples, or lips.
During a Raynaud’s attack, the arteries become very narrow for a brief period. As a result, little or no blood flows to affected body parts. This may cause these areas to:
- Turn pale or white and then blue
- Feel numb, cold, or painful
- Turn red, throb, tingle, burn, or feel numb as blood flow returns to the affected areas
Raynaud’s attacks can last less than a minute or as long as several hours. Attacks can occur daily or weekly.
Attacks often begin in one finger or toe and move to other fingers or toes. Sometimes only one or two fingers or toes are affected. Different areas may be affected at different times.
Severe secondary Raynaud’s can cause skin sores or gangrene. “Gangrene” refers to the death or decay of body tissues. Fortunately, severe Raynaud’s is rare.
Raynaud’s disease diagnosis
Your doctor will diagnose primary Raynaud’s (Raynaud’s disease) or secondary Raynaud’s (Raynaud’s phenomenon) based on your medical history, a physical exam, and test results.
Specialists Involved
Primary care doctors and internists often diagnose and treat Raynaud’s disease.
If you have the disorder, you also may see a rheumatologist. This is a doctor who specializes in treating disorders of the joints, bones, and muscles.
Rheumatologists diagnose and treat many of the diseases that are linked to secondary Raynaud’s, such as scleroderma and lupus.
Medical History
Your doctor may ask about your risk factors for Raynaud’s. He or she also may ask about your signs and symptoms when you’re exposed to cold temperatures or stress.
For example, your doctor may ask whether your fingers or toes:
- Feel numb or painful when they’re exposed to cold temperatures
- Turn white or blue, or both, when they’re exposed to cold temperatures
Physical Exam
Your doctor will look at your fingers and toes to check the health of your skin and nails and to check blood flow to these areas.
Your doctor also may do a more complete physical exam to check for signs of diseases and conditions that are linked to secondary Raynaud’s.
Sorting out primary vs. secondary Raynaud’s
To distinguish between primary and secondary Raynaud’s, your doctor might perform a test called nail fold capillaroscopy. During the test, the doctor examines the skin at the base of your fingernail under a microscope or magnifier for deformities or enlargement of the tiny blood vessels (capillaries).
If your doctor suspects that another condition, such as an autoimmune or connective tissue disease, underlies Raynaud’s, he or she will likely order blood tests, such as:
- Antinuclear antibodies test. A positive test for the presence of these antibodies — produced by your immune system — might indicate a stimulated immune system, common in people who have connective tissue diseases or other autoimmune disorders.
- Erythrocyte sedimentation rate. This test determines the rate at which red blood cells settle to the bottom of a tube. A faster than normal rate might signal an underlying inflammatory or autoimmune disease.
No one blood test can diagnose Raynaud’s. Your doctor might order other tests, such as those that rule out diseases of the arteries, to help pinpoint a condition that can be associated with Raynaud’s.
Diagnostic Tests and Procedures
Your doctor may recommend the following tests to check for Raynaud’s and related conditions.
Cold Stimulation Test
A cold stimulation test can be used to trigger Raynaud’s symptoms. For this test, a small device that measures temperature is taped to your fingers. Your hands are then exposed to cold—they’re usually briefly put into ice water.
Your hands are then removed from the cold, and the device measures how quickly your fingers return to their normal temperature. If you have Raynaud’s, it may take more than 20 minutes for your fingers to return to their normal temperature.
Because results of this type of test are not always consistent, your doctor may do other tests to check for Raynaud’s.
Nailfold Capillaroscopy
You may have a test called nailfold capillaroscopy. For this test, your doctor puts a drop of oil at the base of your fingernail. He or she then looks at your fingernail under a microscope.
If your doctor sees abnormal arteries, it may mean you have a disease linked to Raynaud’s, such as scleroderma.
Other Tests
Your doctor may order blood tests to look for conditions that are linked to secondary Raynaud’s. Examples include antinuclear antibody (ANA), erythrocyte sedimentation rate (ESR or “sed rate”), and C-reactive protein (CRP) blood tests.
Raynaud’s disease treatment
Primary Raynaud’s (Raynaud’s disease) and secondary Raynaud’s (Raynaud’s phenomenon) have no cure. However, treatments can reduce the number and severity of Raynaud’s attacks. Treatments include lifestyle changes, medicines, and, rarely, surgery.
Most people who have primary Raynaud’s can manage the condition with lifestyle changes. People who have secondary Raynaud’s may need medicines in addition to lifestyle changes. Rarely, they may need surgery or shots.
If you have Raynaud’s and develop sores on your fingers, toes, or other parts of your body, see your doctor right away. Timely treatment can help prevent permanent damage to these areas.
Lifestyle Changes
Lifestyle changes can help you avoid things that may trigger a Raynaud’s attack. Examples of such triggers include cold temperatures, emotional stress, workplace or recreational factors, and contact with certain chemicals or medicines.
Protect Yourself From Cold Temperatures
To protect yourself from cold temperatures:
- Wear a hat, mittens (rather than gloves), scarf, coat with snug cuffs, and warm socks and shoes during cold weather. Layer your clothing for extra warmth.
- Put hand and foot warmers in your mittens, boots, socks, or pockets. Some warmers are small heat packs, and others are battery-operated. These warmers often are available at sporting goods stores.
- Turn down air conditioning or dress warmly while in an air-conditioned space.
- Warm up your car before driving in cold weather.
- Wear gloves or mittens when taking food out of the refrigerator or freezer (if cold temperatures severely affect you).
Avoid Other Triggers
Try to avoid things that make you upset or stressed. Learn ways to handle stress that you can’t avoid. Physical activity helps some people cope with stress. Other people listen to music or focus on something calm or peaceful to reduce stress. Some people learn yoga, tai chi, or meditation.
Try to avoid workplace and recreational triggers. For example, limit the use of vibrating tools, such as drills. Wear proper protective gear if you work with industrial chemicals. Also, try to limit repetitive hand actions, such as typing or playing the piano.
Some medicines can trigger Raynaud’s attacks. Examples include:
- Migraine headache medicines that contain ergotamine. This substance causes your arteries to narrow.
- Certain cancer medicines, such as cisplatin and vinblastine.
- Over-the-counter cold or allergy medicines or diet aids. Some of these medicines can narrow your arteries.
- Beta blockers. These medicines slow your heart rate and lower your blood pressure.
- Birth control pills. These medicines can affect blood flow.
Talk with your doctor about whether your medicines are safe for you.
Other Lifestyle Changes
Other lifestyle changes also can help you avoid Raynaud’s attacks. For example, include physical activity as part of your healthy lifestyle. Physical activity can increase your blood flow and help keep you warm.
Limit your use of caffeine and alcohol. These substances can trigger Raynaud’s attacks. If you smoke, quit. Smoking makes Raynaud’s worse. Ask your doctor about programs and products that can help you quit. Also, try to avoid secondhand smoke.
You also can take steps to help stop Raynaud’s attacks when they occur. For example:
- Move to a warmer spot, such as indoors, during cold weather.
- Warm your hands or feet. Place your hands under your armpits. Soak your feet or hands in warm water.
- Wiggle or massage your fingers and toes.
- Move your arms in circles or shake your arms or feet.
- Get out of stressful situations and try relaxation techniques.
If you have Raynaud’s, be sure to take care of your hands and feet. Protect them from cuts, bruises, and other injuries. For example, wear properly fitted shoes and don’t walk barefoot. Use lotion to prevent your skin from drying and cracking. Also, avoid tight wristbands and rings.
Medicines
If lifestyle changes don’t control Raynaud’s, you may need medicines or surgery. Medicines are used to improve blood flow to the fingers and toes.
Examples of medicines used to treat Raynaud’s include calcium channel blockers, alpha blockers, prescription skin creams, and ACE inhibitors (used less often).
- Calcium channel blockers. These drugs relax and open small blood vessels in your hands and feet, decreasing the frequency and severity of attacks in most people with Raynaud’s. These drugs can also help heal skin ulcers on your fingers or toes. Examples include nifedipine (Afeditab CR, Procardia, others), amlodipine (Norvasc), felodipine and isradipine.
- Vasodilators. These drugs, which relax blood vessels, include nitroglycerin cream applied to the base of your fingers to help heal skin ulcers. Other vasodilators include the high blood pressure drug losartan (Cozaar), the erectile dysfunction medication sildenafil (Viagra, Revatio), the antidepressant fluoxetine (Prozac, Sarafem, others) and a class of medications called prostaglandins.
Surgery
Rarely, people who have severe Raynaud’s may develop skin sores or gangrene. “Gangrene” refers to the death or decay of body tissues. If this happens, antibiotics or surgery to cut out the damaged tissue may be needed. In very serious cases, the affected toe or finger may need to be removed.
Another treatment for severe Raynaud’s is to block the nerves in the hands or feet that control the arteries. This can help prevent Raynaud’s attacks.
The surgery often relieves symptoms, but sometimes for only a few years. Shots may need to be repeated if symptoms persist or come back.
Surgical options include:
- Nerve surgery. Sympathetic nerves in your hands and feet control the opening and narrowing of blood vessels in your skin. Cutting these nerves interrupts their exaggerated responses. Through small incisions in the affected hands or feet, a doctor strips these tiny nerves around the blood vessels. This surgery (sympathectomy), if successful, might reduce the frequency and duration of attacks.
- Chemical injection. Doctors can inject chemicals such as local anesthetics or onabotulinumtoxin type A (Botox) to block sympathetic nerves in affected hands or feet. You might need to have the procedure repeated if symptoms return or persist.
What can I do for raynaud’s disease
Primary Raynaud’s (Raynaud’s disease) and secondary Raynaud’s (Raynaud’s phenomenon) can be lifelong conditions. However, you can take steps to help control Raynaud’s. Lifestyle changes and ongoing care can help you manage the disorder.
Most people who have primary Raynaud’s can manage the disorder with lifestyle changes. People who have secondary Raynaud’s may need medicines in addition to lifestyle changes. Rarely, they may need surgery or shots.
Lifestyle Changes
You can take steps to avoid things that trigger Raynaud’s attacks. If you have Raynaud’s:
- Protect yourself from cold temperatures.
- Try to avoid emotional stress and learn ways to cope with stress that you can’t avoid.
- Avoid certain medicines, substances, and activities that can trigger Raynaud’s attacks.
- Include physical activity as part of your healthy lifestyle and limit your use of caffeine and alcohol. If you smoke, quit. Also, try to avoid secondhand smoke.
You also can take steps to stop a Raynaud’s attack once it starts. Warm up your hands, feet, or other affected areas right away. For example, place your hands under your armpits, run warm water over your fingers and toes, or massage your hands and feet.
If you have Raynaud’s, be sure to take care of your hands and feet. Protect them from cuts, bruises, and other injuries. For example, wear properly fitted shoes and don’t walk barefoot. Use lotion to prevent your skin from drying and cracking. Also, avoid tight wristbands and rings.
Ongoing Care
If you have Raynaud’s, it’s important to get ongoing care. Talk with your doctor about how often to schedule followup visits. Take all medicines as your doctor prescribes.
See your doctor right away if your Raynaud’s symptoms get worse or if you develop sores on your fingers, toes, or other parts of your body. Timely treatment can help prevent permanent damage to these areas.