Contents
- Renal artery
- Urine production
- Renal artery stenosis
- Renal artery aneurysm
Renal artery
Twenty to twenty-five percent of the total cardiac output, or about 1200 mL of blood, flows through the kidneys each minute. Each kidney receives blood from a renal artery. Every day, the two kidneys filter about 120 to 150 quarts (115 to 142 liters) of blood to produce about 1 to 2 quarts (950 mL to 1.9 liter) of urine, composed of wastes and extra fluid.
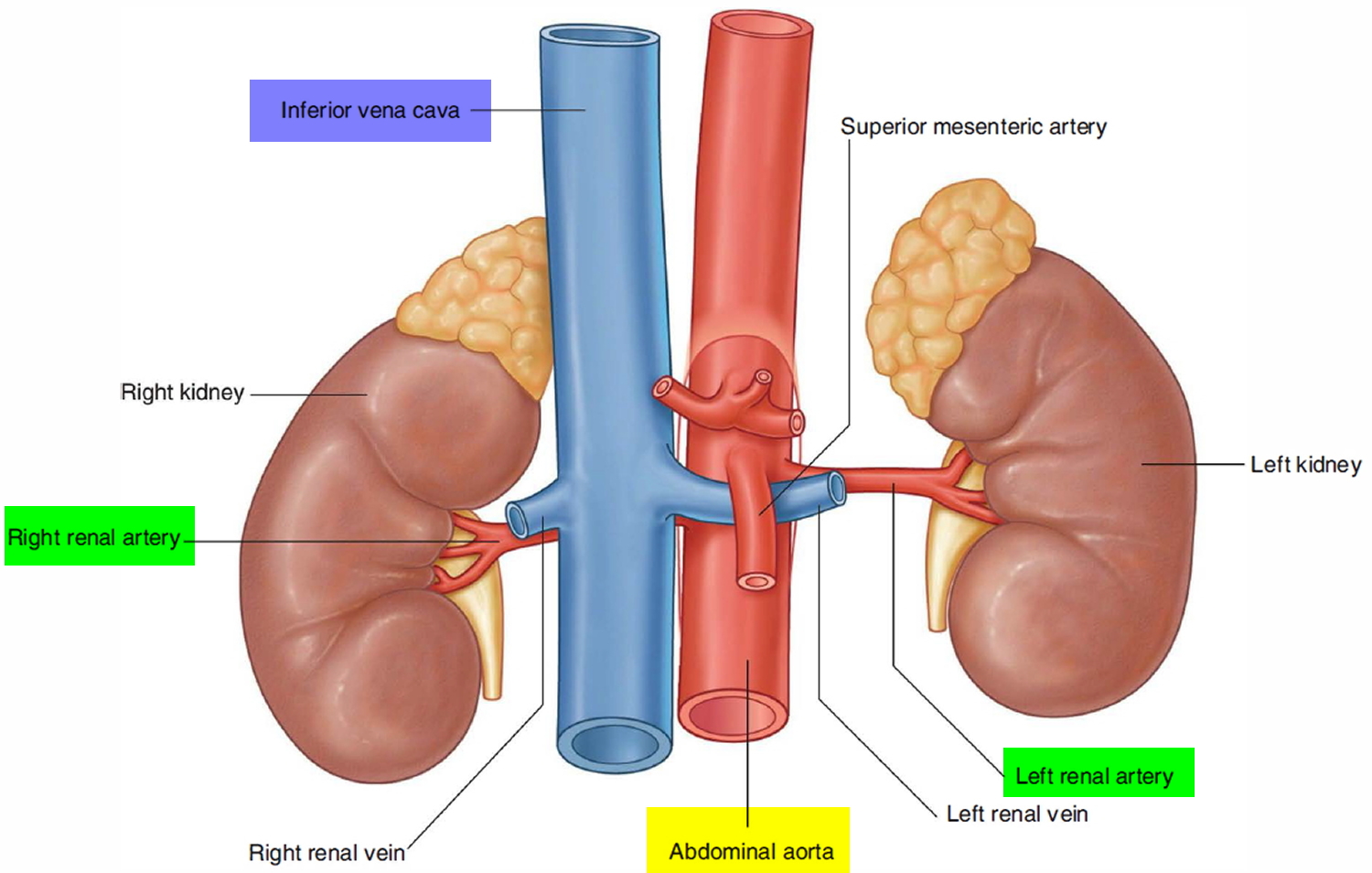
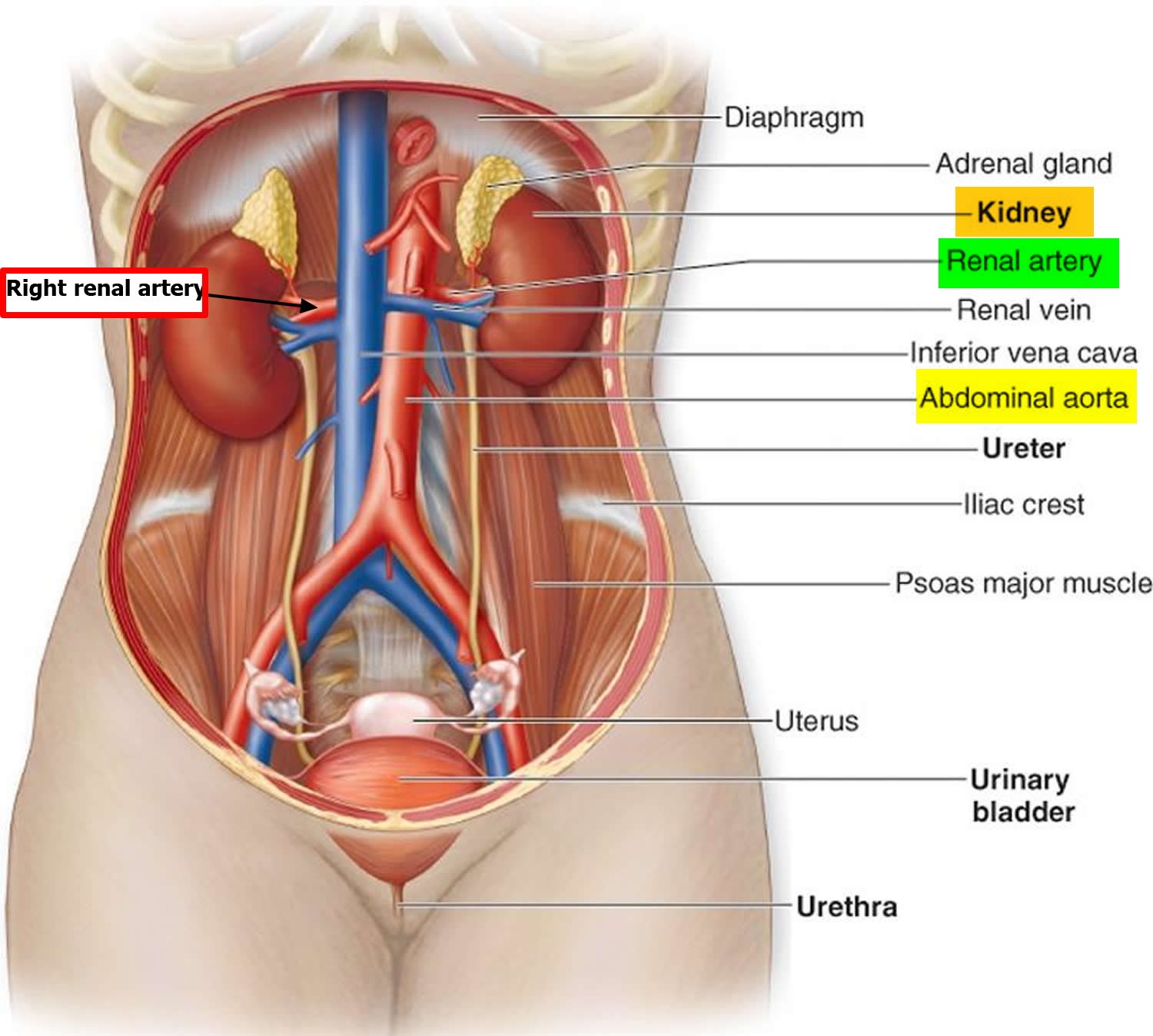
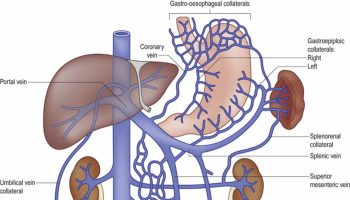
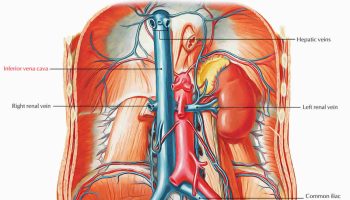
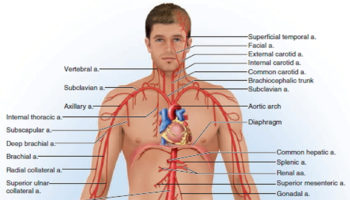
Right and left renal arteries usually arise from lateral aspects of abdominal aorta at superior border of second lumbar (L2) vertebra, about 1 cm inferior to superior mesenteric artery (see Figure 1 and 2). Right renal artery, which is longer than left, arises slightly lower than left and passes posterior to right renal vein and inferior vena cava. Left renal artery is posterior to left renal vein and is crossed by inferior mesenteric vein.
As each renal artery approaches the renal hilum, it divides into segmental arteries, which supply the renal parenchyma. However, there are often accessory renal arteries called extrahilar arteries. The extrahilar arteries are common. They originate from the lateral aspect of the abdominal aorta, either above or below the primary renal arteries, enter the hilum with the primary arteries or pass directly into the kidney at some other level. Regardless of its origin, each renal artery divides as it approaches the kidney and all the branches usually traverse the hilum. A polar artery may occasionally be found entering the medial border of the kidney above or below the hilum. Stenosis of a renal artery can lead to systemic arterial hypertension.
Branches of the renal artery (a small inferior suprarenal artery) also supply blood to each adrenal gland.
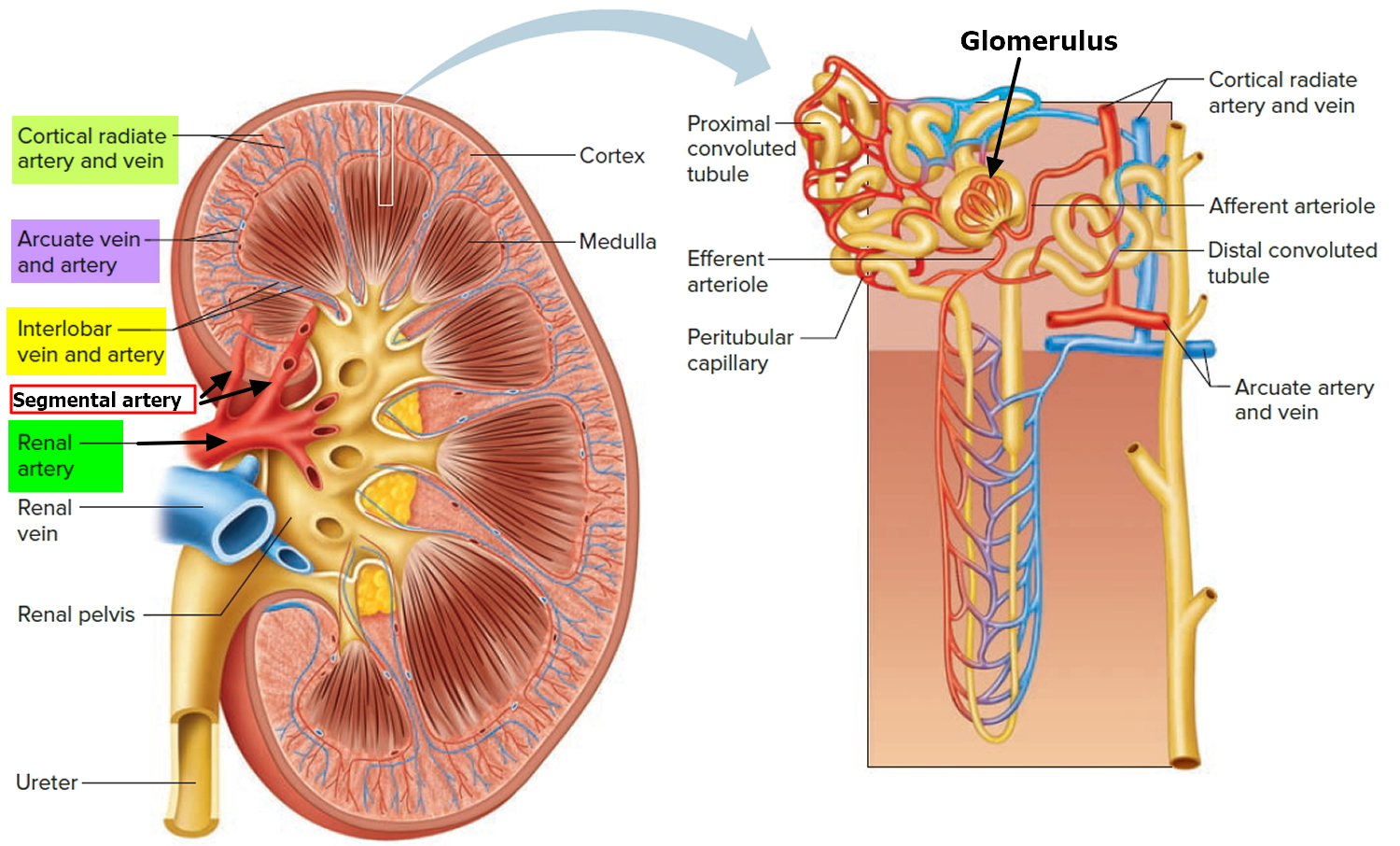
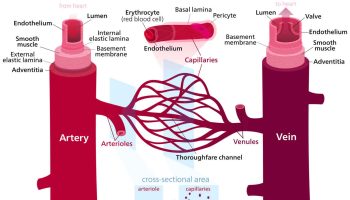
Each kidney is supplied by a renal artery arising from the aorta. Just before or after entering the hilum, the renal artery divides into a few segmental arteries, and each of these gives rise to a few interlobar arteries (see Figure 3). An interlobar artery penetrates each renal column and travels between the pyramids toward the corticomedullary junction, the boundary between the cortex and medulla (see Figure 3). Along the way, it branches again to form arcuate arteries, which make a sharp 90° bend and travel along the base of the pyramid. Each arcuate artery gives rise to several cortical radiate arteries, which pass upward into the cortex. As a cortical radiate artery ascends through the cortex, a series of afferent arterioles arise from it at nearly right angles like the limbs of a pine tree. Each afferent arteriole supplies one nephron. It leads to a spheroidal mass of capillaries called a glomerulus, enclosed in a nephron structure called the glomerular capsule. The glomerulus is drained by an efferent arteriole. The efferent arteriole usually leads to a plexus of peritubular capillaries, named for the fact that they form a network around the tubules of the nephron. These capillaries pick up the water and solutes reabsorbed by the tubules.
Figure 1. Renal artery location
Figure 2. Renal artery
Urine production
Kidneys regulate blood volume and composition; help regulate blood pressure, pH, and glucose levels; produce two hormones (calcitriol and erythropoietin); and excrete wastes in urine. As the kidneys selectively excrete waste products and excess materials in the urine, they maintain the composition of the internal environment, thereby contributing to homeostasis.
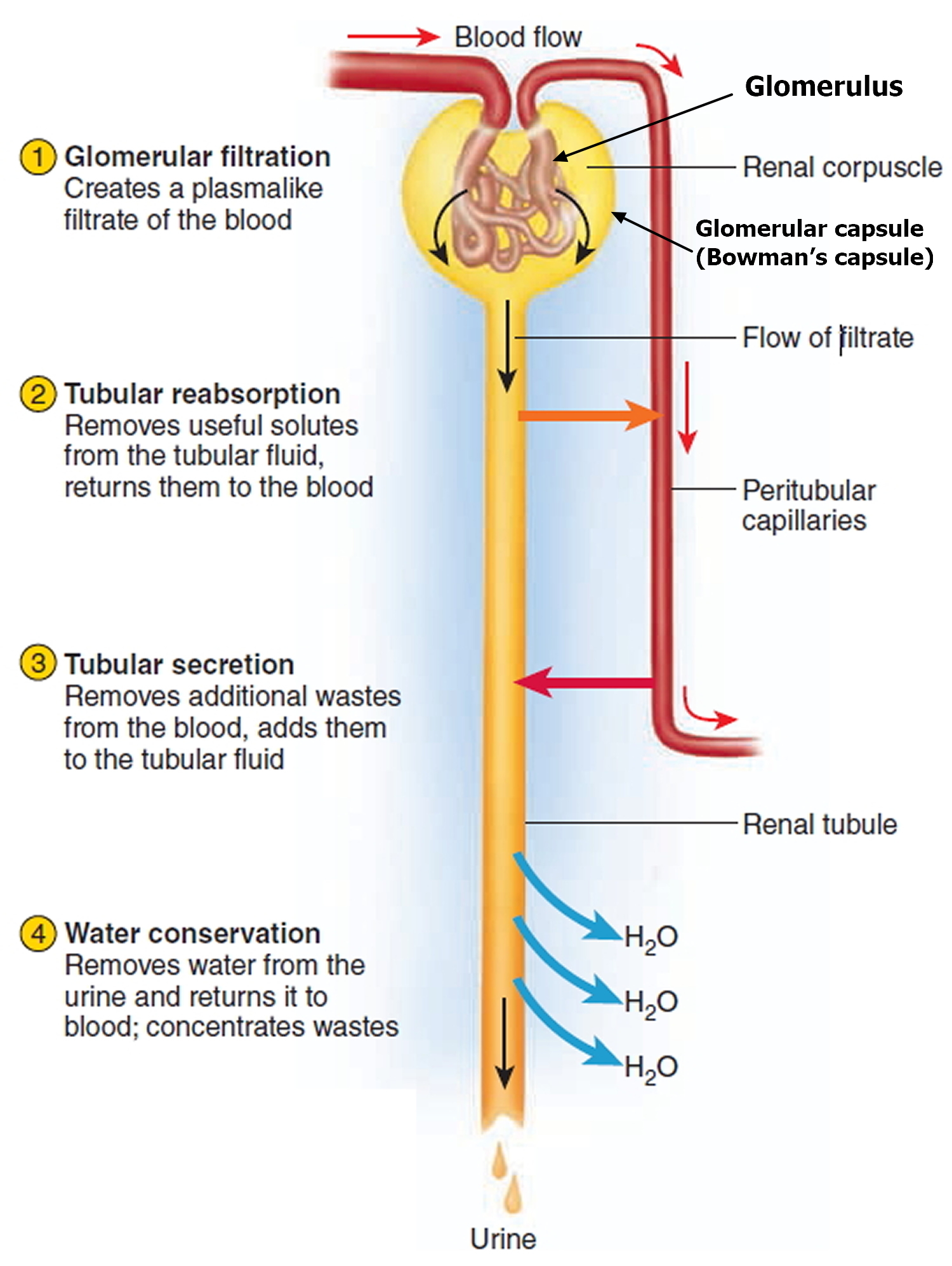
The kidney converts blood plasma to urine in four stages (Figure 4):
- Glomerular filtration is the passage of fluid from the bloodstream into the nephron, carrying not only wastes but also chemicals useful to the body. The fluid filtered from the blood is called glomerular filtrate. In contrast to the blood, it is free of cells and very low in protein. After it passes into the renal tubule, its composition is quickly modified by the following processes, and we call it tubular fluid.
- Tubular reabsorption, in which useful substances such as glucose are reabsorbed from the tubular fluid and returned to the blood.
- Tubular secretion, in which tubule cells extract blood borne substances such as hydrogen ions and some drugs from the peritubular capillaries and add them to the tubular fluid, to be eliminated in the urine.
- Water conservation, achieved by reabsorbing variable amounts of water from the fluid so the body can eliminate metabolic wastes without losing excess water. If water reabsorption did not occur, a typical adult hypothetically would produce 180 liters of urine per day—although in reality, this would be an impossible feat considering that we have only about 5 liters of blood and about 40 liters of total body water. Usually, the kidneys excrete urine that is hypertonic to the blood plasma—that is, it has a higher ratio of waste solutes to water than the plasma does. Water reabsorption occurs in all parts of the renal tubule, but is the final change occurring in the urine as it passes through the collecting duct. The fluid is regarded as urine once it has entered this duct.
Figure 3. Renal artery and its interlobar arteries in the kidney
Figure 4. Urine production in the kidney
Renal artery stenosis
Renal artery stenosis is the narrowing of one or both renal arteries 1. “Renal” means “kidney” and “stenosis” means “narrowing.” The renal arteries are blood vessels that carry blood to the kidneys from the aorta—the main blood vessel that carries blood from the heart to arteries throughout the body.
Renovascular hypertension is high blood pressure caused by renal artery stenosis 1. Blood pressure is written with two numbers separated by a slash, 120/80, and is said as “120 over 80.” The top number is called the systolic pressure and represents the pressure as the heart beats and pushes blood through the blood vessels. The bottom number is called the diastolic pressure and represents the pressure as blood vessels relax between heartbeats. A person’s blood pressure is considered normal if it stays at or below 120/80. High blood pressure is a systolic pressure of 140 or above or a diastolic pressure of 90 or above 2.
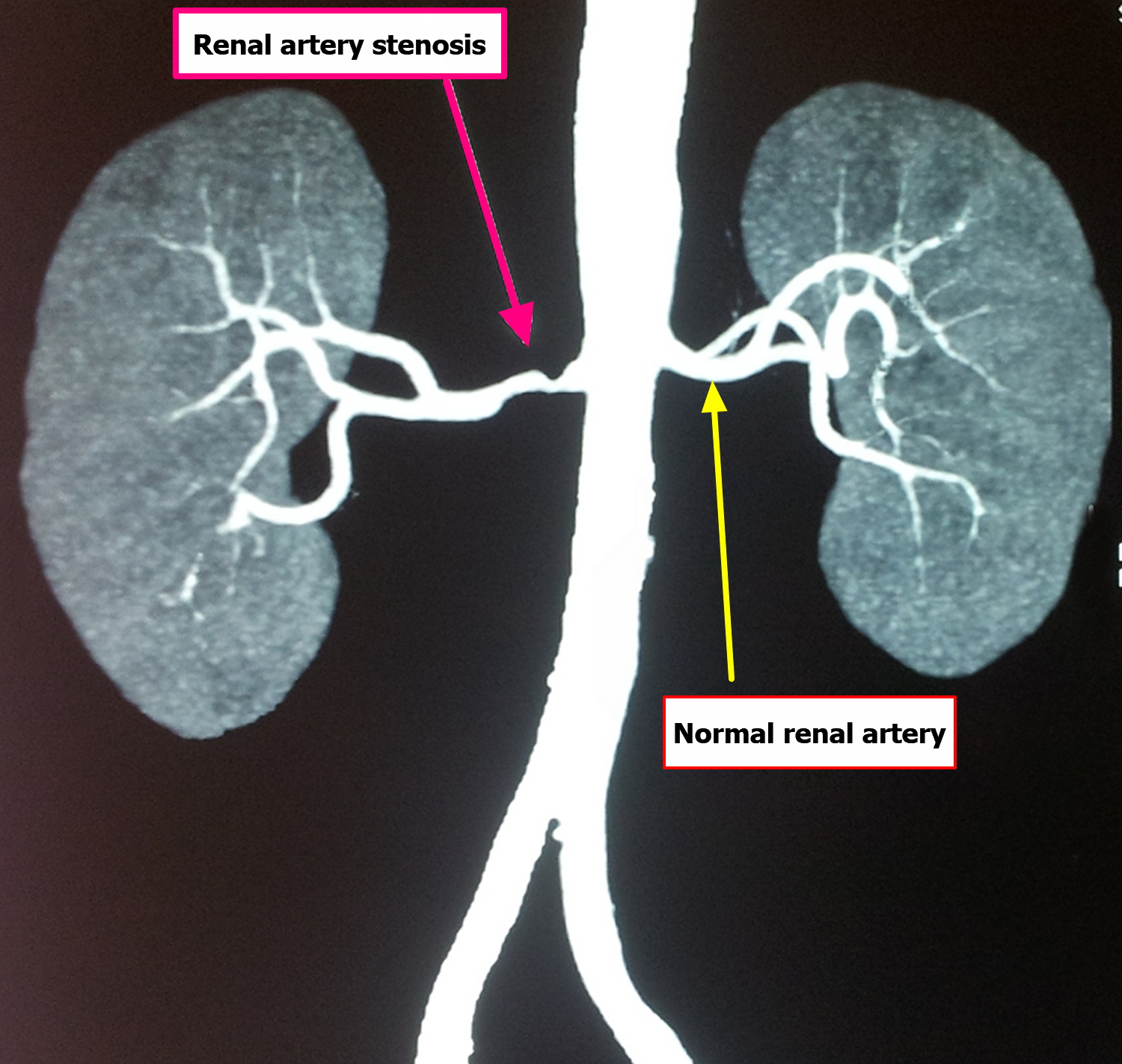
Figure 5. Renal artery stenosis (CT angiogram)
What causes renal artery stenosis ?
About 90 percent of renal artery stenosis is caused by atherosclerosis—clogging, narrowing, and hardening of the renal arteries 3. In these cases, renal artery stenosis develops when plaque—a sticky substance made up of fat, cholesterol, calcium, and other material found in the blood—builds up on the inner wall of one or both renal arteries. Plaque buildup is what makes the artery wall hard and narrow.
Most other cases of renal artery stenosis are caused by fibromuscular dysplasia—the abnormal development or growth of cells on the renal artery walls—which can cause blood vessels to narrow 1. Rarely, renal artery stenosis is caused by other conditions.
Who is at risk for renal artery stenosis ?
People at risk for artherosclerosis are also at risk for renal artery stenosis. Risk factors for renal artery stenosis caused by artherosclerosis include:
- high blood cholesterol levels
- high blood pressure
- smoking
- insulin resistance
- diabetes
- being overweight or obese
- lack of physical activity
- a diet high in fat, cholesterol, sodium, and sugar
- being a man older than 45 or a woman older than 55
- a family history of early heart disease
The risk factors for renal artery stenosis caused by fibromuscular dysplasia are unknown, but fibromuscular dysplasia is most common in women and people 25 to 50 years of age 4. Fibromuscular dysplasia can affect more than one person in a family, indicating that it may be caused by an inherited gene.
What are the symptoms of renal artery stenosis ?
- In many cases, renal artery stenosis has no symptoms until it becomes severe.
The signs of renal artery stenosis are usually either high blood pressure or decreased kidney function, or both, but renal artery stenosis is often overlooked as a cause of high blood pressure.
Renal artery stenosis should be considered as a cause of high blood pressure in people who:
- are older than age 50 when they develop high blood pressure or have a marked increase in blood pressure
- have no family history of high blood pressure
- cannot be successfully treated with at least three or more different types of blood pressure medications.
Symptoms of a significant decrease in kidney function include:
- increase or decrease in urination
- edema—swelling, usually in the legs, feet, or ankles and less often in the hands or face
- drowsiness or tiredness
- generalized itching or numbness
- dry skin
- headaches
- weight loss
- appetite loss
- nausea
- vomiting
- sleep problems
- trouble concentrating
- darkened skin
- muscle cramps
What are the possible complications of renal artery stenosis ?
People with renal artery stenosis are at increased risk for complications resulting from loss of kidney function or atherosclerosis occurring in other blood vessels, such as:
- chronic kidney disease (CKD)—reduced kidney function over a period of time
- coronary artery disease—narrowing and hardening of arteries that supply blood to the heart
- stroke—brain damage caused by lack of blood flow to the brain
- peripheral vascular disease—blockage of blood vessels that restricts flow of blood from the heart to other parts of the body, particularly the legs
Renal artery stenosis can lead to kidney failure, described as end-stage renal disease when treated with blood-filtering treatments called dialysis or a kidney transplant, though this is uncommon in people who receive ongoing treatment for renal artery stenosis.
How is renal artery stenosis diagnosed ?
A health care provider can diagnose renal artery stenosis by listening to the abdomen with a stethoscope and performing imaging tests. When blood flows through a narrow artery, it sometimes makes a whooshing sound, called a bruit. The health care provider may place a stethoscope on the front or the side of the abdomen to listen for this sound. The absence of this sound, however, does not exclude the possibility of renal artery stenosis.
In some cases, renal artery stenosis is found when a person has a test for another reason. For example, a health care provider may find renal artery stenosis during a coronary angiogram for diagnosis of heart problems. A coronary angiogram is a procedure that uses a special dye, called contrast medium, and x-rays to see how blood flows through the heart.
The following imaging tests are used to diagnose renal artery stenosis:
Duplex ultrasound
Duplex ultrasound combines traditional ultrasound with Doppler ultrasonography. Traditional ultrasound uses a device, called a transducer, that bounces safe, painless sound waves off organs to create an image of their structure. Doppler ultrasonography records sound waves reflected off of moving objects, such as blood, to measure their speed and other aspects of how they flow. The procedure is performed in a health care provider’s office, outpatient center, or hospital by a specially trained technician, and the images are interpreted by a radiologist—a doctor who specializes in medical imaging. Anesthesia is not needed. The images can show blockage in the renal artery or blood moving through nearby arteries at a lower-than-normal speed. Ultrasound is noninvasive and low cost.
Catheter angiogram
A catheter angiogram, also called a traditional angiogram, is a special kind of x-ray in which a thin, flexible tube called a catheter is threaded through the large arteries, often from the groin, to the artery of interest—in this case, the renal artery. The procedure is performed in a hospital or outpatient center by a radiologist. Anesthesia is not needed though a sedative may be given to lessen anxiety during the procedure. Contrast medium is injected through the catheter so the renal artery shows up more clearly on the x-ray. Catheter angiogram is the “gold standard” for diagnosing renal artery stenosis due to the high quality of the image produced. In addition, severe renal artery stenosis can be treated during the same visit. However, a catheter angiogram is an invasive procedure, and a person may have side effects from the sedative or contrast medium or may have bleeding or injury to the artery from the catheter. The procedure is also more expensive than other imaging tests.
Computerized tomographic angiography (CTA) scan
Computerized tomographic angiography scans use a combination of x-rays and computer technology to create images. The procedure is performed in an outpatient center or hospital by an x-ray technician, and the images are interpreted by a radiologist. Anesthesia is not needed. Contrast medium is injected into a vein in the person’s arm to better see the structure of the arteries. Computerized tomographic angiography scans require the person to lie on a table that slides into a tunnel-shaped device where the x-rays are taken. Computerized tomographic angiography scans are less invasive than catheter angiograms and take less time. However, the risks from the x-ray radiation still exist, and the test often requires more contrast medium than a catheter angiogram, so it may not be recommended for a person with poor kidney function.
Magnetic resonance angiogram (MRA)
Magnetic resonance angiogram uses radio waves and magnets to produce detailed pictures of the body’s internal organs and soft tissues without using x-rays. The procedure is performed in an outpatient center or hospital by an x-ray technician, and the images are interpreted by a radiologist. Anesthesia is not needed though light sedation may be used for people with a fear of confined spaces. Contrast medium may be injected into a vein in the person’s arm to better see the structure of the arteries. With most magnetic resonance angiogram scans, the person lies on a table that slides into a tunnel-shaped device that may be open ended or closed at one end; some newer machines are designed to allow the person to lie in a more open space. In addition to providing high-quality images noninvasively, magnetic resonance angiogram can provide a functional assessment of blood flow and organ function. However, the use of contrast medium for an magnetic resonance angiogram is not advised for people with poor kidney function because of the risk of complications to the skin and other organs if the kidneys do not remove the contrast medium well enough.
How is renal artery stenosis treated ?
Treatment for renal artery stenosis includes lifestyle changes, medications, and surgery and aims to:
- prevent renal artery stenosis from getting worse
- treat renovascular hypertension
- relieve the blockage of the renal arteries
Renal artery stenosis that has not led to renovascular hypertension or caused a significant blockage of the artery may not need treatment. Renal artery stenosis that needs to be treated, also called critical renal artery stenosis, is defined by the American Heart Association as a reduction by more than 60 percent in the diameter of the renal artery 2. However, health care providers are not exactly sure what degree of blockage will cause significant problems.
Lifestyle Changes
The first step in treating renal artery stenosis is making lifestyle changes that promote healthy blood vessels throughout the body, including the renal arteries. The best ways to keep plaque from building up in the arteries are to exercise, maintain a healthy body weight, and choose healthy foods. People who smoke should quit to help protect their kidneys and other internal organs.
Medications
People with renovascular hypertension may need to take medications that—when taken as prescribed by their health care provider—lower blood pressure and can also significantly slow the progression of kidney disease. Two types of blood pressure-lowering medications, angiotensin-converting enzyme (ACE) inhibitors and angiotensin receptor blockers (ARBs), have proven effective in slowing the progression of kidney disease. Many people require two or more medications to control their blood pressure. In addition to an angiotensin-converting enzyme (ACE) inhibitor or an angiotensin receptor blocker (ARB), a diuretic—a medication that helps the kidneys remove fluid from the blood—may be prescribed. Beta blockers, calcium channel blockers, and other blood pressure medications may also be needed. Some people with renal artery stenosis cannot take an ACE inhibitor or ARB due to the effects on the kidneys. People with renovascular hypertension who are prescribed an ACE inhibitor or ARB should have their kidney function checked within a few weeks of starting the medication.
A cholesterol-lowering medication to prevent plaque from building up in the arteries and a blood-thinner, such as aspirin, to help the blood flow more easily through the arteries may also be prescribed.
Surgery
Although surgery has been used in the past for treatment of renal artery stenosis due to atherosclerosis, recent studies have not shown improved outcomes with surgery compared with medication. However, surgery may be recommended for people with renal artery stenosis caused by fibromuscular dysplasia or renal artery stenosis that does not improve with medication. Different types of surgery for renal artery stenosis include the following. The procedures are performed in a hospital by a vascular surgeon—a doctor who specializes in repairing blood vessels. Anesthesia is needed.
Angioplasty and stenting. Angioplasty is a procedure in which a catheter is put into the renal artery, usually through the groin, just as in a catheter angiogram. In addition, for angioplasty, a tiny balloon at the end of the catheter can be inflated to flatten the plaque against the artery wall. A small mesh tube, called a stent, may then be positioned inside the artery to keep plaque flattened and the artery open. People with renal artery stenosis caused by fibromuscular dysplasia may be successfully treated with angioplasty alone, while angioplasty with stenting has a better outcome for people with renal artery stenosis caused by atherosclerosis.
Endarterectomy or bypass surgery. In an endarterectomy, the plaque is cleaned out of the artery, leaving the inside lining smooth and clear. To create a bypass, a vein or synthetic tube is used to connect the kidney to the aorta. This new path serves as an alternate route for blood to flow around the blocked artery into the kidney. These procedures are not performed as often as in the past due to a high risk of complications during and after the procedure.
Eating, Diet, and Nutrition
Limiting intake of fats, cholesterol, sodium, and sugar can help prevent atherosclerosis, which can lead to renal artery stenosis. Most sodium in the diet comes from salt. A healthy diet that prevents people from becoming overweight or obese can also help prevent atherosclerosis. People with renal artery stenosis that has caused decreased kidney function should limit their intake of protein, cholesterol, sodium, and potassium to slow the progression of kidney failure.
Renal artery aneurysm
Renal artery aneurysms are uncommon 5. They are often identified incidentally during abdominal computed tomography (CT) screening for other diseases 6. Renal artery aneurysm may be associated with hypertension and are usually asymptomatic at presentation but may result in rupture, hematuria, or renal infarction 5. The natural history of renal artery aneurysms is poorly understood.
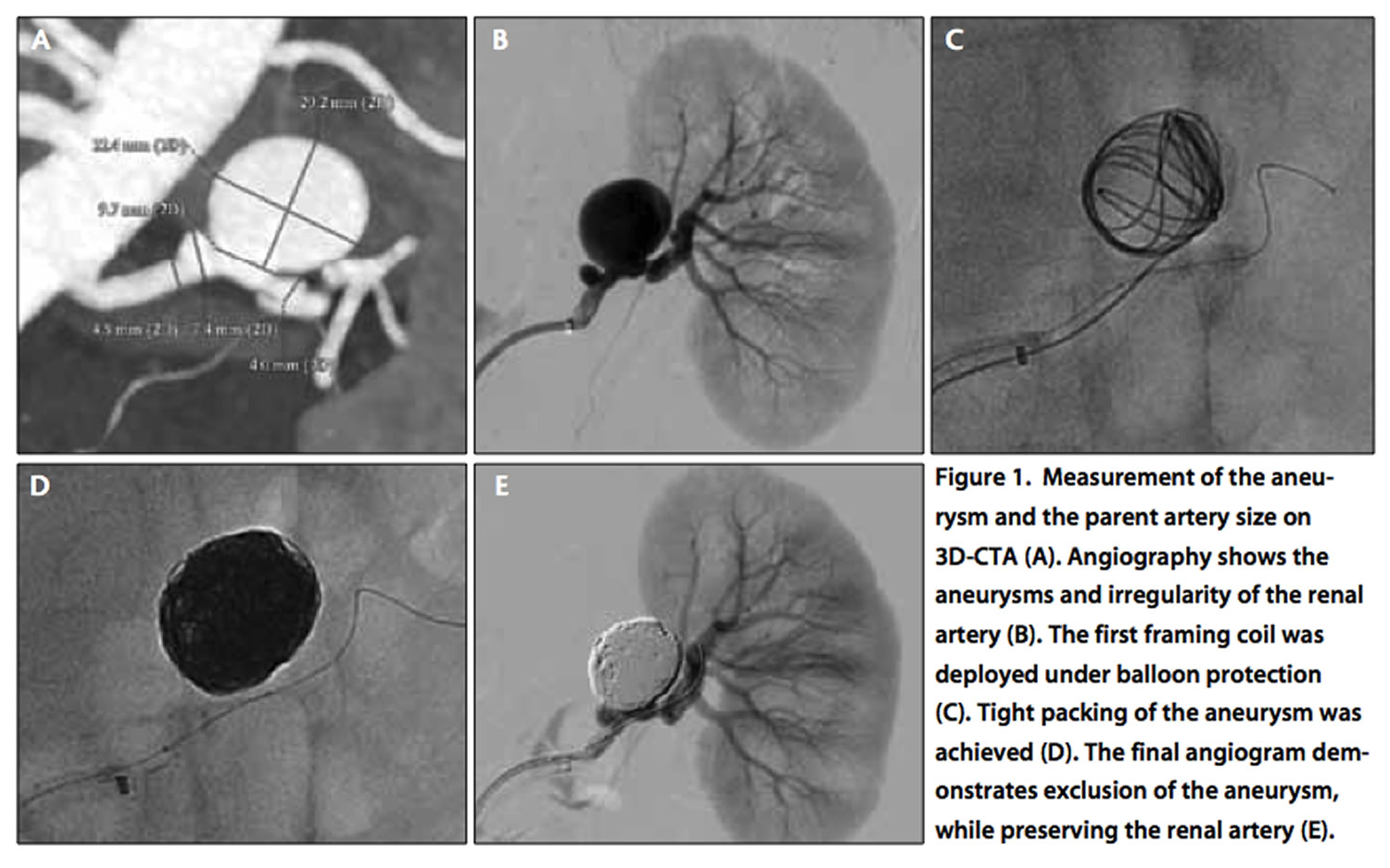
Figure 6. Renal artery aneurysm (3D Computerized tomographic angiogram)
Treatment options for renal artery aneurysms include observation, aneurysmectomy with surgical repair, endovascular procedures, nephrectomy or partial nephrectomy. Observation is indicated for asymptomatic intraparenchymal renal artery aneurysms measuring less than 2 cm in diameter. Although there is general consensus that renal artery aneurysm that are symptomatic (renovascular hypertension, dissection, urologic symptoms, embolization, local expansion) or identified in women at risk for pregnancy should be repaired, diameter criteria for repair of asymptomatic renal artery aneurysm are controversial and emerging evidence suggests that rupture incidence is low for those <2.5 cm in diameter.
Options for repair of renal artery aneurysm have expanded over the preceding decades with expansion of both open surgical and endovascular treatments. In recent years, coil embolization or stent-graft with the coil embolization was successful for treating renal artery aneurysms, but complex aneurysms may require aneurysmectomy and renal artery reconstruction by in-situ repair or ex-vivo technique.
In recent years, transcatheter arterial embolization has emerged as a simple, useful and effective technique in managing renal artery aneurysms. The procedure is performed by transfemoral catheterization as well as by superselective catheterization and embolization of interlobar arteries with 3F microcatheters. Endovascular occlusion is obtained by using gelatin sponge, steel coils, detachable baloons, and conventional non-detachable microcoils delivered through a microcatheter. Nephrectomy or partial nephrectomy are reserved for conditions precluding renal revascularization which include overt renal artery aneurysm rupture, covert renal artery aneurysm rupture, artery-to-vein fistula, renal cell carcinoma, end stage nephropaty, renal infarction, severe ischemic renal atrophy or complex intrarenal aneurysms. Recently, partial nephrectomy by the laparoscopic approach has been proposed for managing renal artery aneurysms and the procedure is considered feasible and safe.
- Renal Artery Stenosis. National Institute of Diabetes and Digestive and Kidney Diseases. https://www.niddk.nih.gov/health-information/kidney-disease/renal-artery-stenosis[↩][↩][↩]
- James PA, Oparil S, Carter BL, et al. 2014 evidence-based guideline for the management of high blood pressure in adults—report from the panel members appointed to the Eighth Joint National Committee (JNC 8). The Journal of the American Medical Association. Published online December 18, 2013.[↩][↩]
- Plouin PF, Bax L. Diagnosis and treatment of renal artery stenosis. Nature Reviews Nephrology. 2010;6:151–159.[↩]
- Fibromuscular Dysplasia. National Institute of Neurological Disorders and Stroke. https://www.ninds.nih.gov/Disorders/All-Disorders/Fibromuscular-Dysplasia-Information-Page[↩]
- Peterson LA, Corriere MA. Treatment of renal artery aneurysms. J Cardiovasc Surg 2015 August;56(4):559-65.[↩][↩]
- Jibiki M, Inoue Y, Kudo T, Toyofuku T. Surgical Procedures for Renal Artery Aneurysms. Annals of Vascular Diseases. 2012;5(2):157-160. doi:10.3400/avd.oa.11.00055. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3595876/[↩]