Contents
What is rosacea
Rosacea is a common but poorly understood long-term skin inflammation that causes redness, flushing, and sometimes pimples and pustules that mainly affects your face and there is no permanent cure. Rosacea isn’t contagious but there is some evidence that it may be hereditary. While there’s no cure for rosacea, there are several treatments your doctor or skin specialist (dermatologist) may recommend to help control the symptoms. Rosacea typically appears after age 30, first as red blotches on the cheeks, nose, chin, or forehead. Over time, the affected areas become more severe and more persistent, and blood vessels may appear. Untreated, acne rosacea can develop into bumps and pimples. Many sufferers also experience irritated eyes that appear watery or bloodshot.
Approximately 14 million people in the US and millions more worldwide have rosacea. Adults between 30 and 60 are most often affected by rosacea. Rosacea is more common in women and in fair-skinned individuals, although dark-skinned people may also be affected as well as individuals with Mediterranean skin types. Women tend to develop rosacea at a younger age than men. The rhinophyma type of rosacea (swollen oil glands in the nose) is an exception, in that men are more likely to develop this particular form of rosacea than women. In most people, rosacea comes and goes periodically. In others it gets worse with time.
Recent surveys by the National Rosacea Society reveal that more than 76% of rosacea patients have lowered self-confidence and self-esteem. Of those with severe symptoms, 70% of patients with severe symptoms said the disorder had seriously affected their professional interactions, and almost 30% missed work as a direct result of their condition.
Rosacea is NOT the same as acne. Quite often when an adult has acne, they are quick to label it as a form of rosacea that is commonly referred to as adult acne. It’s true that pimples can be a symptom of rosacea, but they can also exist as true acne or acne vulgaris on someone with no rosacea. How can you tell the difference between a pimple caused by rosacea versus one caused by acne vulgaris?
In reality, a rosacea pimple and an acne vulgaris pimple look similar to the naked eye. Differences between the two are revealed only when they’re examined under a microscope. Your dermatologist will look for additional clues that can help him/her determine which type of pimple you have. A pimple caused by rosacea will be accompanied with redness caused by extra blood vessels. Redness is a common symptom of rosacea. True acne or acne vulgaris will often have black- or whiteheads in addition to the pimple.
To prescribe the most effective treatment, it’s important to determine if you have rosacea or true acne (acne vulgaris). The medications may be similar or quite different depending on your type of acne. In both cases, it’s important to see an experienced dermatologist who can diagnose and prescribe the most appropriate course of action for you.
Many people with rosacea find that certain factors can trigger their symptoms, such as sun exposure, stress, hot weather, alcohol, hot, spicy foods, exercise, hot baths, or certain medications or skin care products. You may try keeping a diary to help identify what triggers your symptoms. Then you’ll know what to try to avoid.
Rosacea symptoms often begin with episodes of flushing, where the skin turns red for a short period, but other symptoms can develop as the condition progresses.
You may have rosacea if you have:
- frequent blushing, flushing or redness on your cheek, nose, chin or forehead
- permanent redness that looks similar to a sunburn that does not go away
- small visible blood vessels on your face
- bumps or pimples on your face that might sting or burn
- red or irritated eyes or swollen eyelids
- burning and stinging sensations
- spots (papules and pustules)
- small blood vessels in the skin becoming visible
Rosacea is a relapsing condition, which means there are periods when symptoms are particularly bad, but less severe as others.
Over time, the redness may become more persistent.
You may also notice that your skin becomes thicker, especially around your nose, and your nose may become swollen.
In some people rosacea can affect the eyes. This can cause red, sore or gritty eyes or eye margins, which can lead to conjunctivitis and swollen eyelids. See an eye specialist if your eyes are being affected, so treatment can be given to prevent damage.
Four different types of rosacea have been described:
- “Red face” rosacea, with a tendency to face flushing (or blushing), which can progress to a persistent redness of the nose or central face
- “Acne”-like bumps and/or pus-filled lesions (papulopustular rosacea), with or without a red face or flushing
- Rhinophyma – slow enlargement of oil glands and skin thickening of the nose and sometimes other face areas, usually in men
- Eye problems (ocular rosacea), which may occur before skin changes – a burning or gritty feeling may be present as well as reddening of the eyes and lids
In severe and rare rosacea cases, the oil glands (sebaceous glands) in your nose and sometimes your cheeks become enlarged, resulting in a buildup of tissue on and around your nose — a condition called rhinophyma. This complication is much more common in men and develops slowly over a period of years.
Rosacea can be controlled to some degree with long-term treatment, but sometimes the changes in physical appearance can have a significant psychological impact.
Common treatments include creams or gels containing antibiotics or azelaic acid to put on your skin, and antibiotic pills. Laser treatment may be suggested to treat redness or visible blood vessels.
If you have eye symptoms, you may need to see an eye specialist (ophthalmologist).
Surgery or laser therapy may be recommended if you’ve developed a swollen nose.
Your doctor will probably suggest that you use non-irritating skin-care products, wash your face gently and use sunscreen with an SPF of 15 or more to minimise skin irritation.
What Can I Do if I Have Rosacea?
While no one knows for certain what causes rosacea, there are certain triggers that seem to activate it, specifically, things that increase blood flow to the face – sunlight, hot drinks, spicy foods, alcohol, exercise, hot baths or saunas, temperature extremes, and emotional stress. With this knowledge, the best way to treat rosacea is to manage your lifestyle and reduce stress, alcohol consumption, and exposure to heat as much as possible. Any actions you can take to reduce exposure to these triggers will help. Cool compresses after heat exposure, sun screen, and protection from the elements are a few examples.
Your dermatologist can also provide many therapy options. Treatment really depends on the types of rosacea symptoms that you have. Someone with rhinophyma (bulbous nose) requires a different type of treatment than someone with pimples or visible facial blood vessels.
What Does Rosacea Look Like?
There are different forms of rosacea, and its appearance can range from mild to severe. All forms of rosacea have at least one of the three primary symptoms:
- Redness,
- Pimples, or
- An enlarged ruddy nose.
A person with rosacea may have just one symptom, a combination of two symptoms, or all three.
Rosacea is usually limited to the central facial area and/or eyes. This central facial area includes the nose, cheeks, brow, and chin. However, in some cases it may extend through the neck and chest area.
There are four main types of rosacea:
- “Red face” rosacea. A person with this type of rosacea is described as being prone to facial flushing or blushing. This can progress to chronic redness of the nose or central face.
- Papulopustular rosacea (acne rosacea). This is the type of rosacea often referred to as “adult acne,” and to the naked eye, both conditions can appear the same. A dermatologist can distinguish rosacea acne from “true acne” to determine the best treatment options.
- Rhinophyma (abnormal appearing nose). This type of rosacea is identified by the slow enlargement of oil glands and skin thickening of the nose. People with rhinophyma are usually described as having a large, bulbous, ruddy (reddish colored) nose. This type of rosacea affects men more than women. And while heavy alcohol consumption can aggravate rhinophyma, it is not the cause of the condition.
- Ocular rosacea (eye problems). This type of rosacea may occur before skin changes are seen. A burning or gritty feeling of the eyes may be present with reddening of the eyes and lids.
Rosacea can range from mild (occasional blushing and pimples) to extremely severe (all the symptoms listed above).
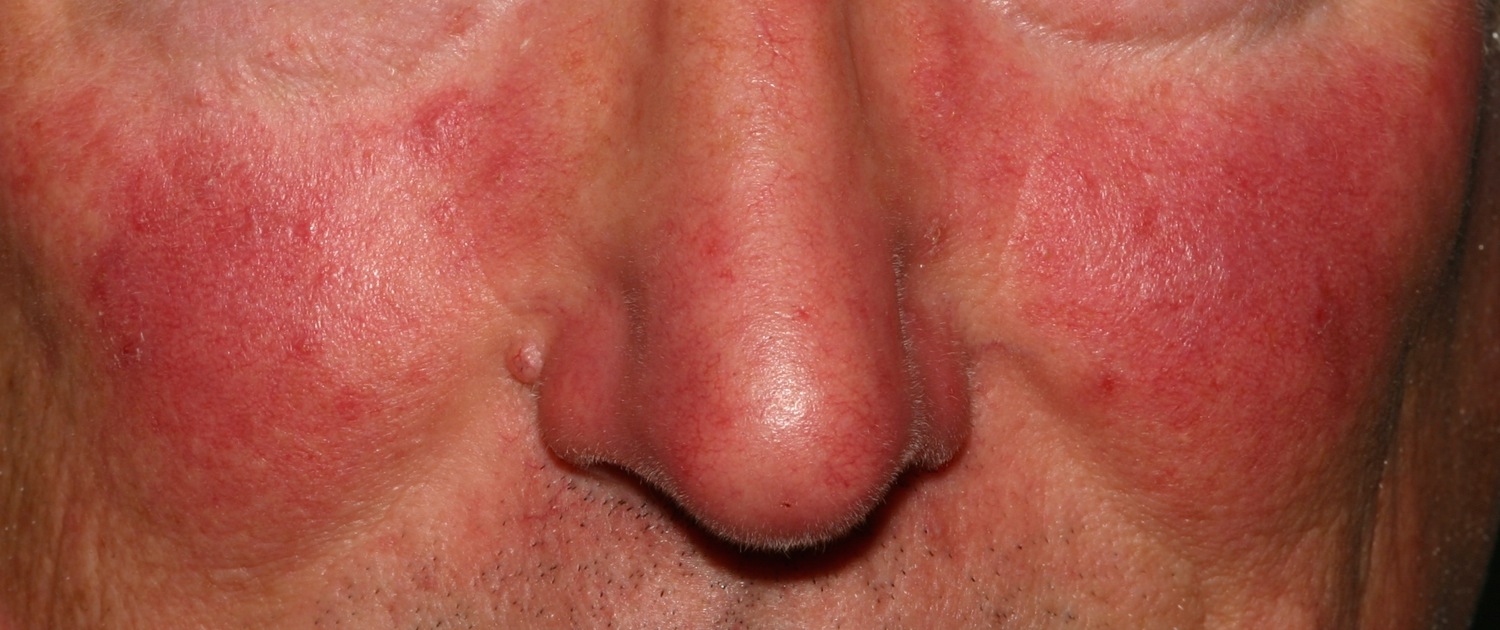
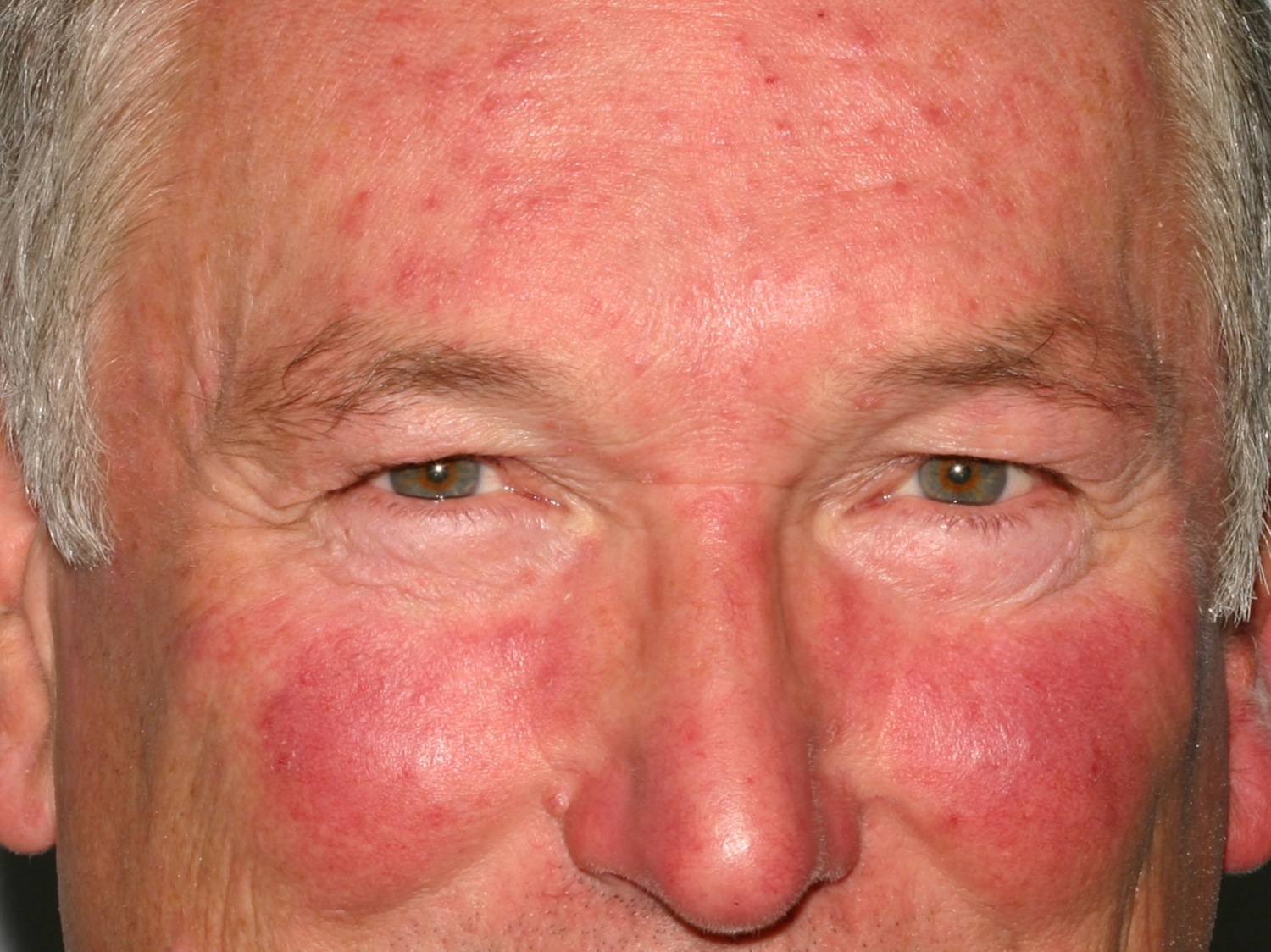
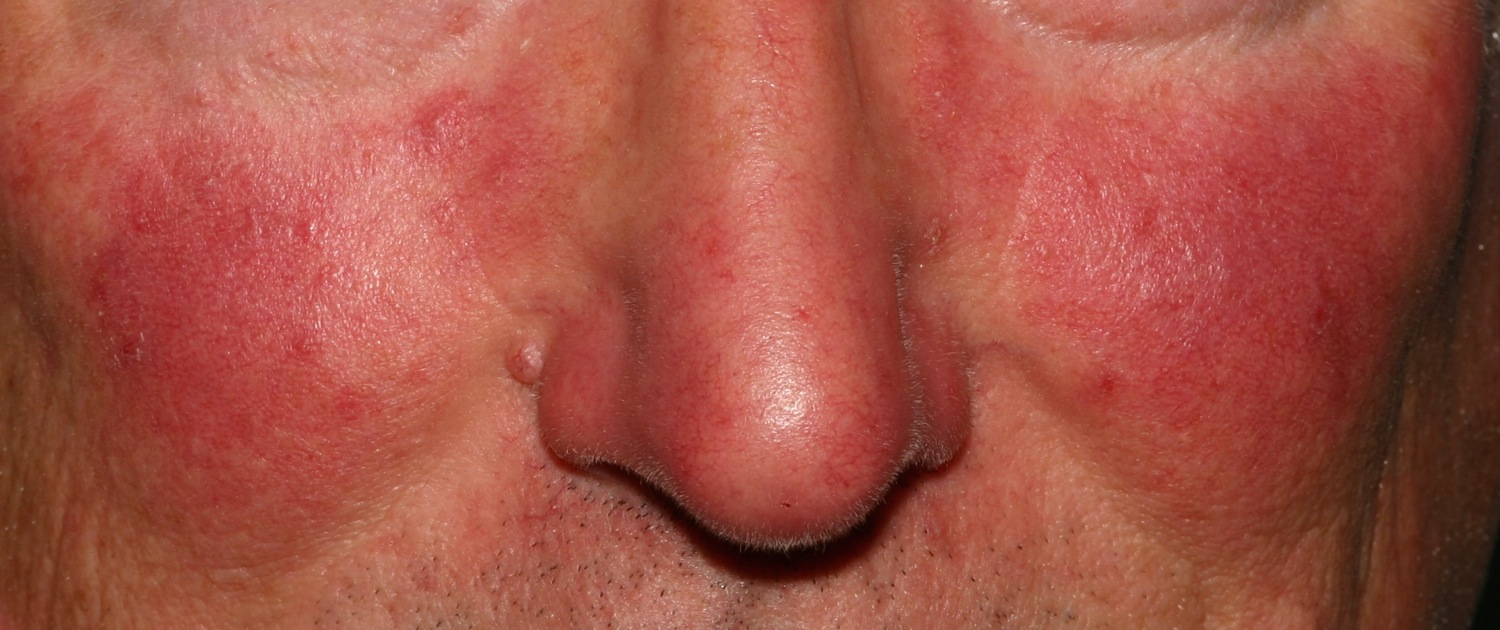
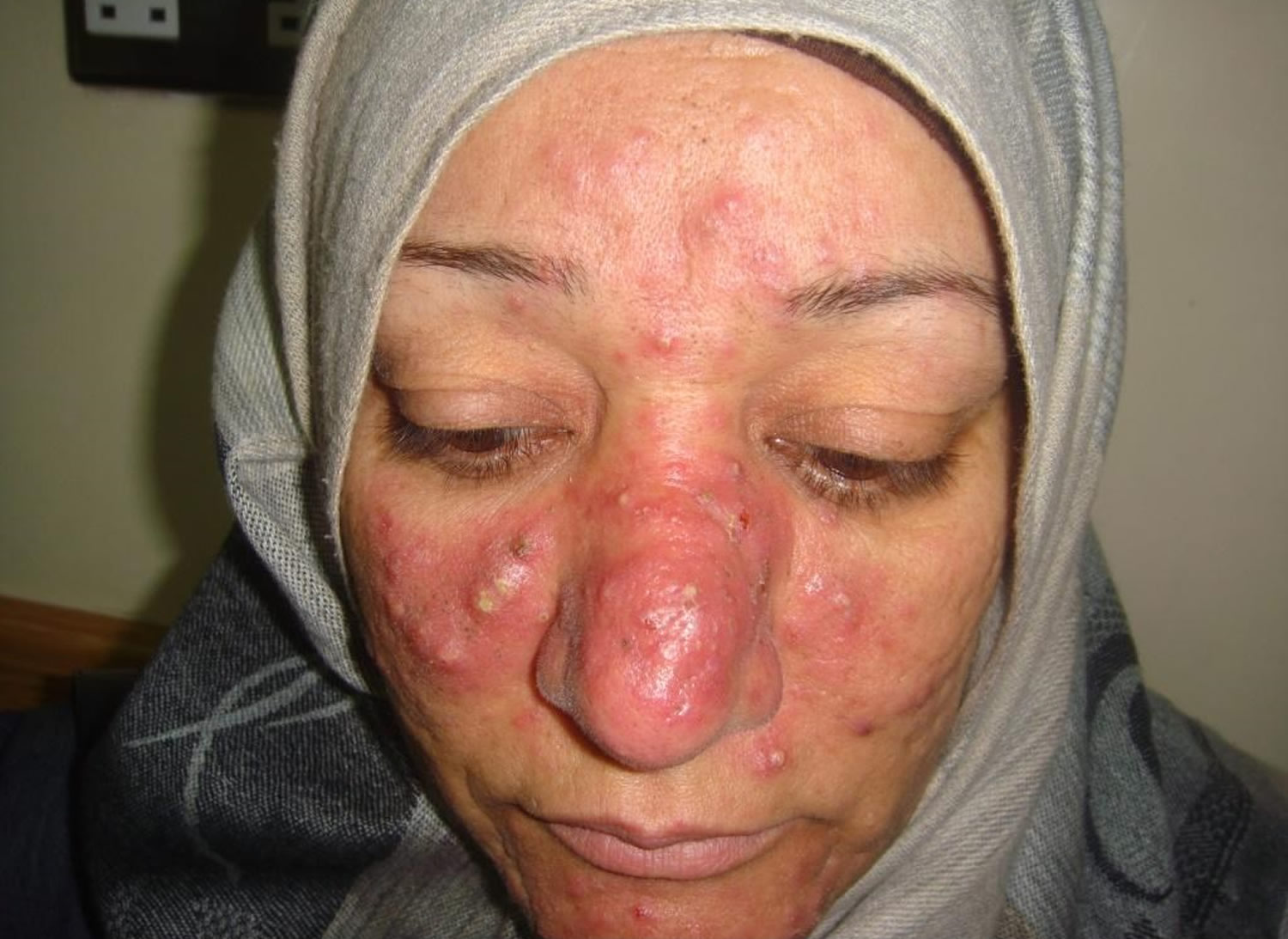
Figure 1. Rosacea face (red face rosacea)
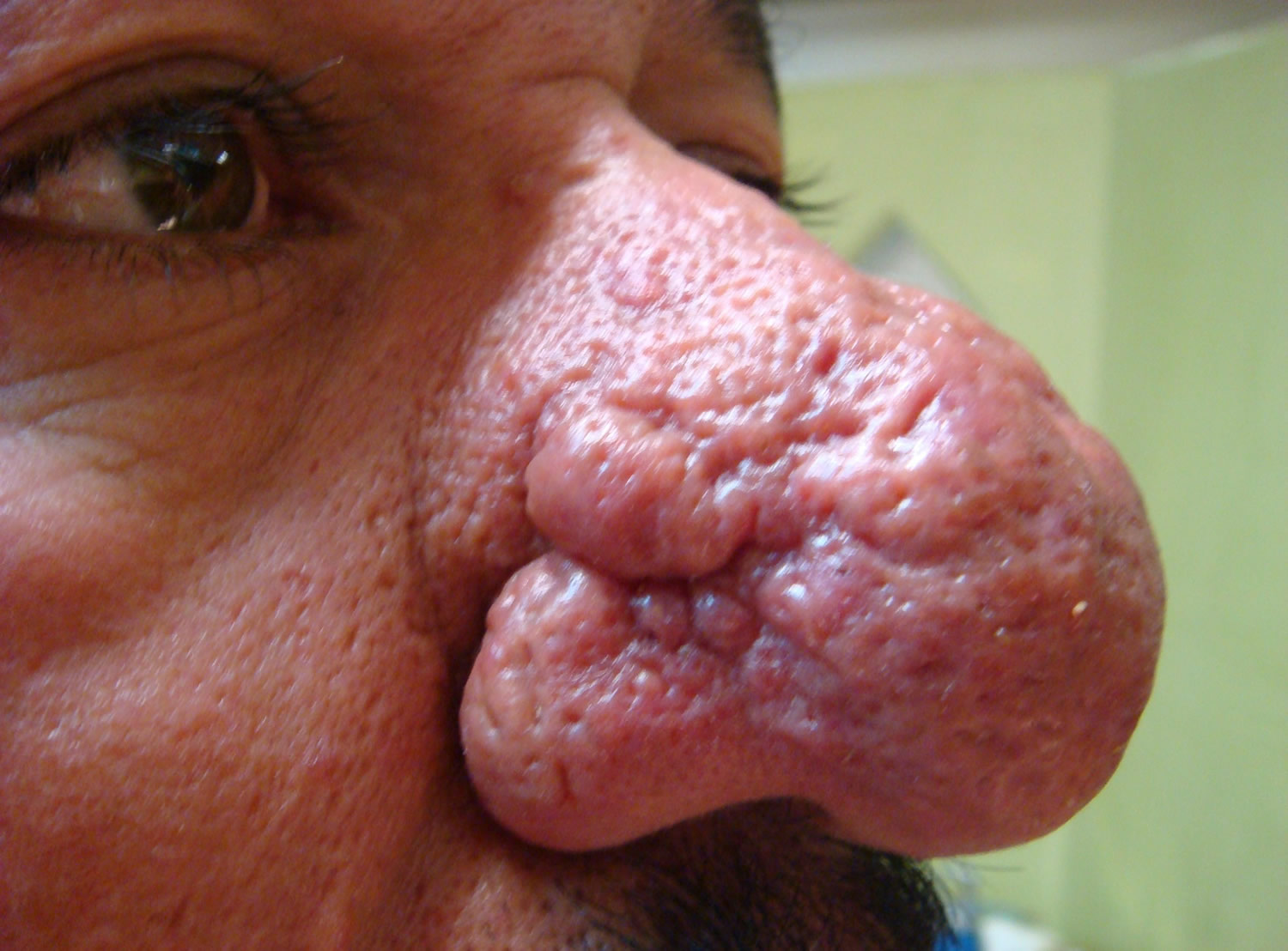
Figure 2. Rhinophyma
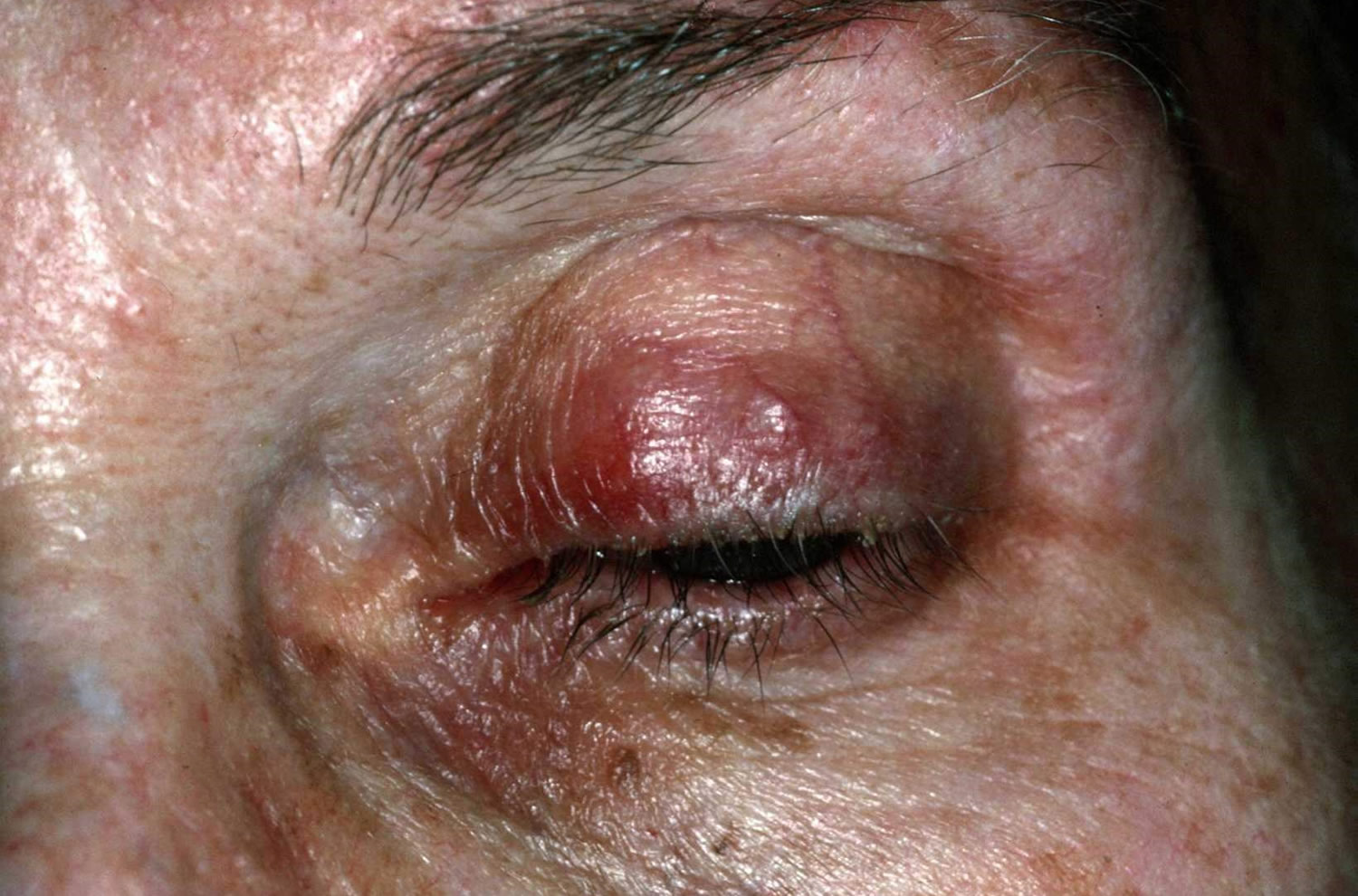
Figure 4. Ocular rosacea
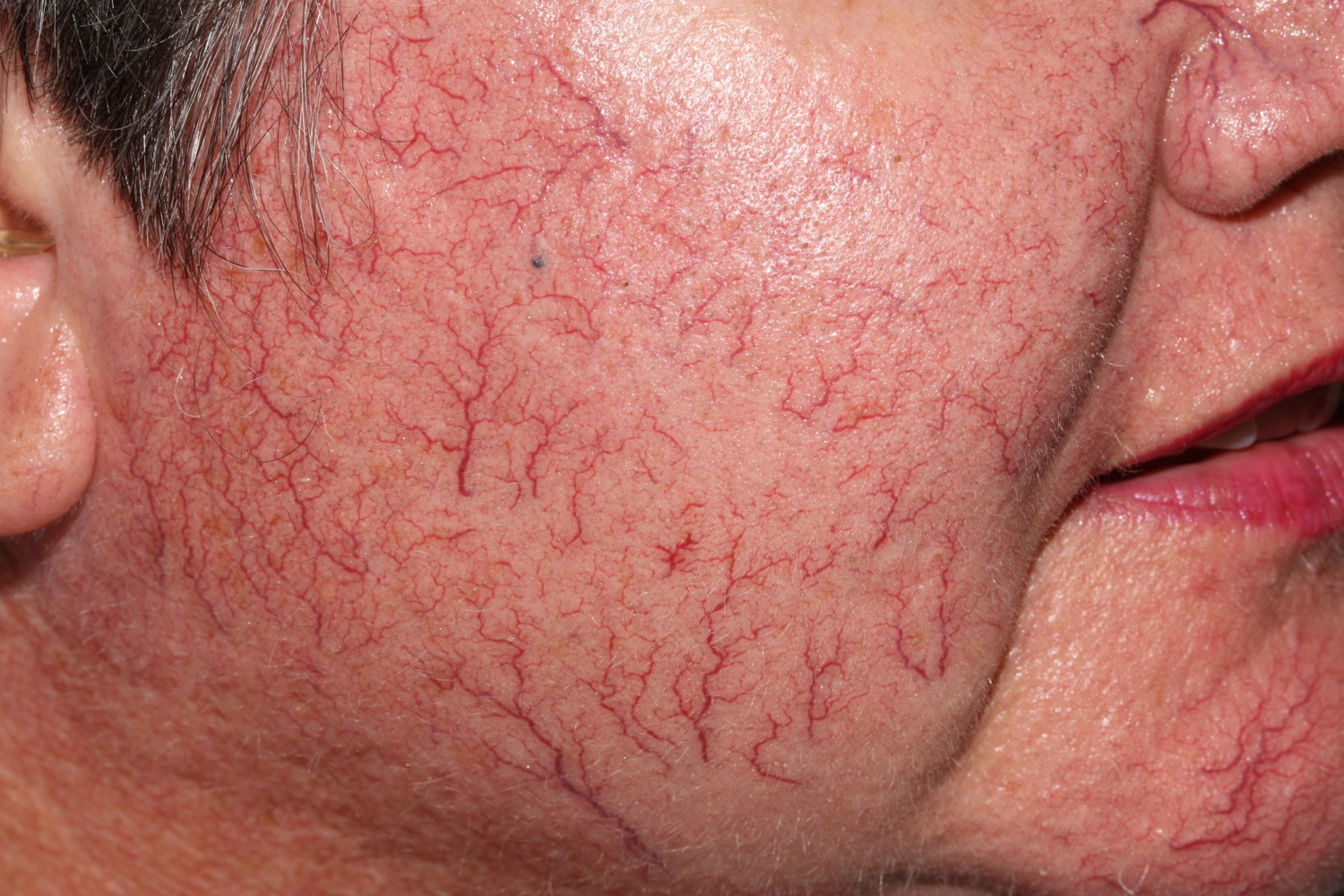
Figure 5. Rosacea telangiectasia face
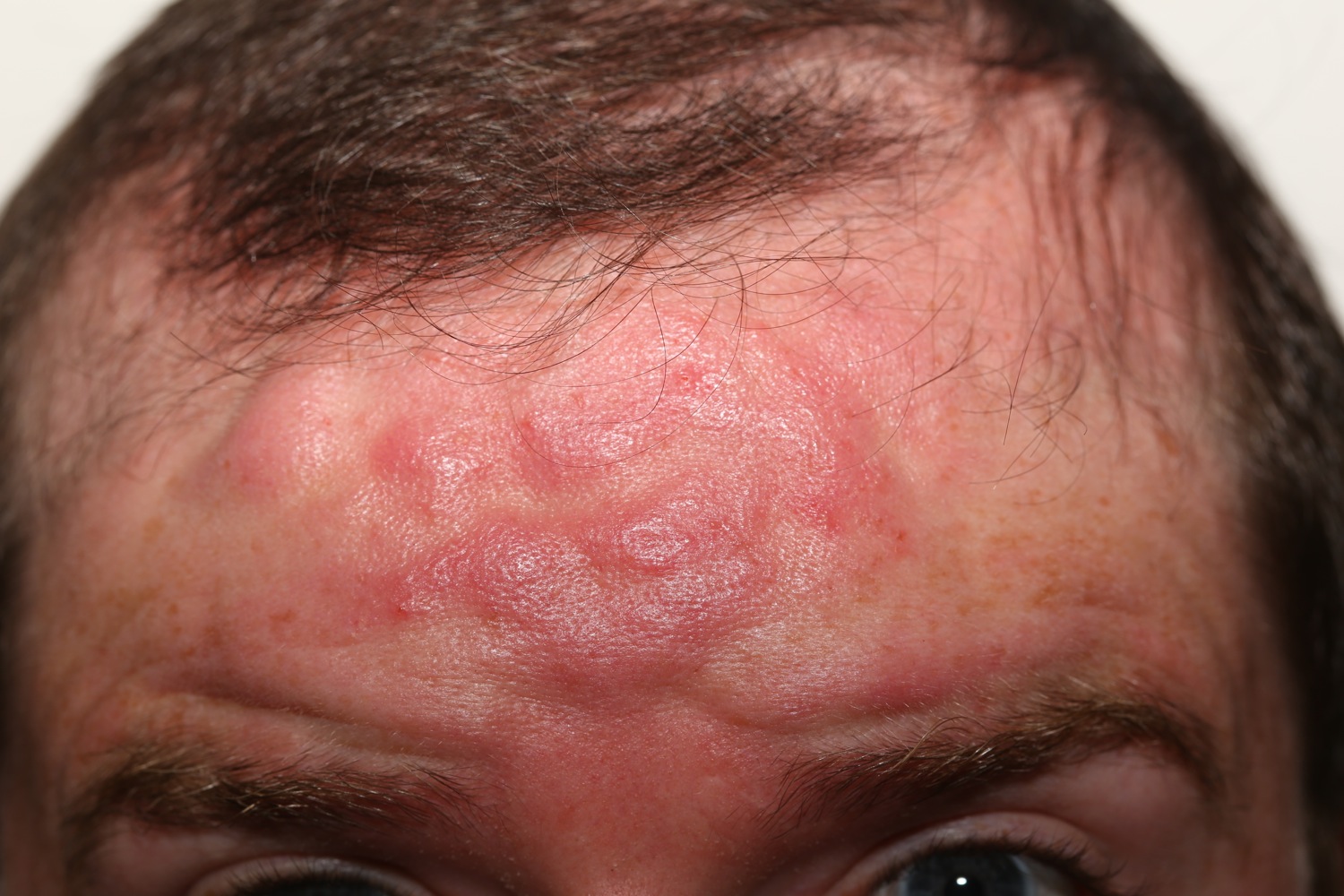
Figure 6. Rosacea face – chronic edema
Rosacea causes
The exact cause of rosacea is unknown. There are several theories regarding the cause of rosacea, including genetic, environmental, vascular and inflammatory factors. Skin damage due to chronic exposure to ultraviolet radiation plays a part.
The skin’s innate immune response appears to be important, as high concentrations of antimicrobial peptides such as cathelicidins have been observed in rosacea.
- Cathelicidins are part of the skin’s normal defence against microbes.
- Cathelicidins promote infiltration of neutrophils in the dermis and dilation of blood vessels.
- Neutrophils release nitric acid also promoting vasodilation.
- Fluid leaks out of these dilated blood vessels causing swelling (oedema); and proinflammatory cytokines leak into the dermis, increasing the inflammation.
Matrix metalloproteinases such as collagenase and elastase also appear important in rosacea.
- These enzymes remodel normal tissue and help in wound healing and production of blood vessels (angiogenesis).
- In rosacea, they are in high concentration and may contribute to cutaneous inflammation and thickened, hardened skin.
- Matrix metalloproteinasesmay also activate cathelicidins contributing to inflammation.
Hair follicle mites (Demodex folliculorum) are sometimes observed within rosacea papules but their role is unclear.
An increased incidence of rosacea has been reported in those who carry the stomach bacterium Helicobacter pylori, but most dermatologists do not believe it to be the cause of rosacea.
Frequent triggers (things that increase face blood flow) of rosacea include sunlight, hot drinks, spicy foods, alcohol, exercise, hot baths or saunas, temperature extremes, and emotional stress. Prolonged use of cortisone creams on the face can also lead to rosacea. Some drugs may worsen flushing (nasal steroids, amiodarone, high doses of some B vitamins, tamoxifen, and rifampin) and drugs that dilate blood vessels, including some blood pressure medications.
It’s possible a combination of these factors may be responsible for the condition, although there isn’t enough evidence to say this for certain.
Some of the main factors that have been suggested are outlined below.
Blood vessel abnormalities
Some experts believe abnormalities in the blood vessels of the face may be a major contributing factor for rosacea. This may explain symptoms of flushing, persistent redness and visible blood vessels.
It’s not known what causes these abnormalities. But sun damage may be responsible for degeneration of the elastic tissue of the skin and the dilation of blood vessels.
Skin peptides
Recent research has shown external triggers such as ultraviolet (UV) light, spicy food, alcohol (particularly red wine), exercise, stress, heat and cold can lead to the activation of certain molecules within the skin called peptides.
Increased levels of these peptides may in turn affect the immune system or nerves and blood vessels (neurovascular system) of the skin. Activation of these systems can cause dilation of blood vessels, redness and inflammation.
Microscopic mites
Microscopic mites called demodex folliculorum usually live harmlessly on human skin, but people with rosacea have particularly large numbers, which may play a role in the condition.
It is currently uncertain whether the mite is a cause or an effect of rosacea, although some researchers have suggested the symptoms may be caused by the skin reacting to bacteria in the mites’ feces.
Helicobacter pylori bacteria
Helicobacter pylori bacteria are bacteria found in the digestive system. It’s been suggested these bacteria may be a possible cause of rosacea, although a link hasn’t been proven.
One theory is the bacteria may stimulate the production of a protein called bradykinin, which is known to cause blood vessels to expand.
Genetics
Rosacea seems to be more common in families, although it’s not clear which genes – if any – are involved or how they’re passed on.
Triggers of rosacea
Although they’re not thought to be direct causes of the condition, many people with rosacea find certain triggers make their symptoms worse.
Different people can have different triggers, but triggers that have been commonly reported include:
- exposure to sunlight
- stress
- hot or cold weather
- strong winds
- strenuous exercise
- alcohol
- hot baths
- spicy foods
- hot drinks
- humidity
- caffeine – found in tea, coffee and cola
- the menopause
- dairy products
- other medical conditions
- certain medicines – such as amiodarone, corticosteroids and high doses of vitamins B6 and B12.
Risk factors for rosacea
Anyone can develop rosacea. But you may be more likely to develop it if you:
- Are a woman
- Have fair skin, particularly if it has been damaged by the sun
- Are over age 30
- Smoke
- Have a family history of rosacea
Rosacea symptoms
Rosacea causes a range of symptoms, although not everyone will experience them all.
Most people with rosacea have periods when their symptoms are particularly troublesome, followed by periods when their symptoms are less so.
- Mild rosacea – occasional blushing and/or only rare pimples
- Moderate rosacea – frequent blushing, persistent face redness and/or a few pimples almost all the time
- Severe rosacea – lots of pimples or bumps all the time and/or red, uncomfortable eyes all the time and/or large bulbous nose and/or lots of blood vessels on the face, all of which can be bothersome in appearance
The main symptoms of rosacea include:
- flushing
- persistent or recurrent redness of the central face (“high color,” “ruddy”), sometimes with swelling
- visible blood vessels
- papules, pimples and pustules (but no blackheads or whiteheads)
- thickened skin
Other symptoms associated with rosacea include:
- sensitive skin – burning, itching, stinging and pain
- dry, rough skin
- raised red patches (plaques) on your skin
- facial swelling (lymphoedema)
- red, bulb-shaped nose
- burning or gritty feeling in eyes with or without red eyelids
Permanent damage to the face (scarring) almost never occurs in rosacea.
Flushing
Flushing is when your skin turns red for a short period – usually a few minutes. It tends to mainly affect the face, although it can spread to your neck and chest.
In some cases the redness may be accompanied by an unpleasant feeling of heat.
In rosacea flushing is often caused by a certain trigger, such as sun exposure, hot drinks or exercise.
Persistent facial redness
Persistent facial redness (erythema) is like a blush or a patch of sunburn that doesn’t go away, or the sort of blotchy skin often associated with drinking too much alcohol.
This can be upsetting for those with rosacea as people can mistakenly assume they are heavy drinkers.
The redness usually affects the cheeks, nose and chin, but may spread to other areas, such as the forehead, neck and chest.
Visible blood vessels
Over time the blood vessels in the skin may become permanently widened (dilated) and visible. The medical name for visible blood vessels is telangiectasia.
Papules and pustules
If you have rosacea, you may develop round red bumps that rise from your skin (papules) and pus-filled swellings (pustules).
These spots appear on your face and are similar to acne. Rosacea used to be called acne rosacea, but the two conditions are quite different.
In rosacea there are no blackheads and the skin is not greasy, but dry and peeling. Rosacea spots also don’t cause scarring.
Thickened skin
In the most serious cases of rosacea the skin can thicken and form excess tissue, usually around the nose. This causes the nose to take on a large, bulbous appearance (rhinophyma).
Rhinophyma is an uncommon, severe symptom of rosacea and takes several years to develop. It almost exclusively affects men.
Rosacea diagnosis
There’s no specific test for rosacea. Instead, doctors rely on the history of your symptoms and a physical examination of your skin. In some cases, your doctor may have you undergo tests that may include skin biopsy which shows chronic inflammation and vascular changes, to rule out other conditions, such as other forms of acne, psoriasis, eczema or lupus. These conditions can sometimes cause signs and symptoms similar to those of rosacea.
If your eyes are involved, your doctor may refer you to an eye specialist (ophthalmologist).
The Global Rosacea Consensus Panel recommends classification using diagnostic, major and minor phenotypes. One diagnostic or two major phenotypes are required for diagnosis.
Diagnostic phenotypes
- Fixed centrofacial erythema in a characteristic pattern that may periodically intensify
- Phymatous changes
Major phenotypes
- Papules and pustules
- Flushing
- Telangiectasia
- Ocular rosacea (lid margin telangiectases, interpalpebral conjunctival injection, spade-shaped infiltrates in cornea, scleritis, sclerokeratitis)
Minor phenotypes
- Burning or stinging
- Edema
- Dry appearance
Rosacea treatment
Although rosacea can’t be cured, treatment can help keep the symptoms under control.
Long-term treatment is usually necessary, although there may be periods where your symptoms improve and you can stop treatment temporarily.
Treatment choices depend on which type of symptom is most troublesome, but usually involves a combination of self-help measures and medication.
Papules and pustules treatment
If you have round red bumps that rise from your skin (papules) and pus-filled swellings (pustules) caused by rosacea, there are a number of different medications that can be effective.
These can be divided into topical treatments that are applied to the skin, or oral treatments, which are taken by mouth.
Rosacea cream
Topical medications are usually prescribed first. These include:
- metronidazole cream or gel
- azelaic acid cream or gel
- ivermectin cream (Soolantra)
Ivermectin is a relatively new medicine. There’s some evidence to suggest it may be more effective and perhaps less irritating to the skin than metronidazole and may only be recommended if the other treatments don’t work. Topical ivermectin 1% cream (Soolantra) once daily is approved in the US for the treatment of rosacea. In two pivotal studies, the number of patients who were clear or almost clear at 12 weeks was 38%-40% for ivermectin vs. 12%-19% placebo. Side effects were actually less in the ivermectin group than the placebo group. A systematic literature review of 57 studies 1 found ivermectin 1 % cream once daily more effective than topical metronidazole and azelaic acid topical in the treatment of inflammatory rosacea.
You’ll usually need to apply these topical treatments once or twice a day, taking care not to get them in your eyes or mouth. It may be several weeks before you notice any significant improvement in your symptoms.
Side effects of these treatments can include a burning or stinging sensation, itchiness and dry skin.
Topical Sodium Sulfacetamide/Sulfur
Topical Sodium Sulfacetamide/Sulfur is a topical antibiotic agent applied 1-3/day that that may be helpful for rosacea, seborrheic dermatitis and acne. It may be particularly advantageous in overlap situations and in those who wish to avoid oral antibiotics.
Topical Praziquantel
Topical praziquantel 3% ointment twice daily in a placebo-controlled trial showed benefit as a topical agent for rosacea 2. 41.9% of patients in the praziquantel group and 18.2% of those in the placebo group achieved an equivalent score of “clear”. Also, topical praziquantel 3% ointment was significantly better than placebo in the treatment of perioral dermatitis 3. Praziquantel is an anti parasitic agent used to treat schistosomiasis, flat worms, and other parasites.
Other Topical Agents
Topical metronidazole, azelaic acid or sodium sulfacetamide and sulfur may be given topically as monotherapy for mild disease in conjunction with a tetracycline initially or to maintain a remission. Any of these topical agents should be applied once or twice daily in the areas that the rosacea occurs. It is important to try to prevent the rosacea, not just spot-treat those pimples that have already developed. This is a common mistake made by patients using topical therapy. Topical 5% permethrin twice daily decreases demodex density and improves the clinical appearance 4.
It is always important to determine if ocular rosacea is present. If so, the oral tetracyclines should be the preferred therapy both to remit the condition and for maintenance.
Oral antibiotics
If your symptoms are more severe, an oral antibiotic medication may be recommended as these can help reduce inflammation of the skin.
Antibiotics often used to treat rosacea include tetracycline, oxytetracycline, doxycycline and erythromycin.
First-line treatment for rosacea is the oral antibiotic, e.g., tetracycline 500 mg or doxycycline 20-100 mg twice daily initially and then tapered to once every day or every other day. Many advocate “sub-microbial therapy”, and indeed, low-dose doxycycline, (e.g., 20 mg twice daily) capsule is available if oral antibiotics need to be taken long term, does seem to be effective. Minocycline 50-100 once a day to twice daily is very effective as well, but since therapy is longterm, the risk of blue teeth and other signs of minocycline pigmentation make it second choice.
These medications are usually taken for four to six weeks, but longer courses may be necessary if the spots are persistent. Although rosacea usually responds within weeks, you may have to stay on the oral antibiotic for years to decades. Control, not cure, is the rule. Treating with an oral tetracycline may reduce the incidence of vascular events 5.
Common side effects of these medications include:
- feeling and being sick
- diarrhea
- bloating and indigestion
- tummy (abdominal) pain
- loss of appetite
Some of the medications used can also make your skin sensitive to sunlight and artificial sources of light, such as sun lamps and sunbeds.
As with the topical treatments mentioned above, these medications usually need to be taken once or twice a day and you may not notice a significant improvement in your symptoms for several weeks.
Oral isotretinoin
Isotretinoin is a medicine often used to treat severe acne, but at lower doses it’s also occasionally used to treat rosacea.
For resistant rosacea (which is uncommon), oral isotretinoin may be given. It is usually given at a slightly lower dose than for acne patients as the drying symptoms may be harder for the rosacea patient to handle. One study found that very low-dose isotretinoin (e.g., 10-20 mg once to five times a week, equivalent to 5 mg/day) is an effective treatment for mild to moderate papulopustular rosacea and is well tolerated 6. Higher doses may aggravate any ocular rosacea.
As isotretinoin is a strong medication that can cause a range of side effects, it can only be prescribed by a specialist in treating skin conditions (dermatologist) and not your doctor.
Common side effects of isotretinoin include:
- dryness and cracking of the skin, lips and nostrils
- inflammation of your eyelids (blepharitis) or eyes (conjunctivitis)
- headaches
- muscle or joint pain
- back pain
- blood in your urine (hematuria)
- mood changes
Isotretinion can also cause birth defects if taken during pregnancy.
Rifaximin
Two studies link rosacea and small intestinal bacterial overgrowth (SIBO) and show a benefit of rifaximin (e.g., 400 mg three times daily for 10 days) in clearing rosacea 7, 8. Rifaximin (Rifagut) is a semisynthetic antibiotic based on rifamycin. It has poor oral bioavailability, meaning that very little of the drug is absorbed into the blood stream when it is taken orally. In the second study, among 28 patients who took rifaximin for their SIBO, the rosacea cleared in 46%, moderately improved in 25%, mildly improved in 11% and failed to improve in 18%.
Spironolactone
One study has shown that rosacea develops at a substantially decreased rate during spironolactone exposure 9. As no other class of diuretics affected the risk estimate, a diuretic drug effect is an unlikely cause for the observed effect.
Flushing and Redness Treatment
Treating facial redness and flushing caused by rosacea is generally more difficult than treating papules and pustules caused by rosacea.
But as well as the self-help measures/home remedies mentioned below, there are some medications that can help.
Brimonidine tartrate
Brimonidine tartrate is a relatively new medication for facial redness caused by rosacea. It comes in the form of a gel that’s applied to the face once a day.
Brimonidine 0.33% topical gel (Mirvaso) is FDA-approved for the facial erythema associated with rosacea in patients 18 and over. It is applied twice daily and is generally well tolerated. Potential side effects include worsening erythema and/or flushing, pruritus, skin irritation, allergic contact dermatitis, and worsening of rosacea. Rebound erythema has been reported greater than baseline 10 and counseling about the potential for worsening erythema, initial use in a test area, and limiting use to special occasions may be warranted. Erythema in skin adjacent to the area of long-term use has been reported 11.
Common side effects of brimonidine tartrate include itchiness and a burning sensation where the gel is applied.
Less common side effects can include:
- a dry mouth
- headaches
- pins and needles
- dry skin
A rebound effect, where flushing becomes worse, has also been reported with this medication.
Oxymetazoline HCL 1% cream (Rhofade) is also FDA-approved for facial redness in rosacea. If one dose not work, the other may be tried. In one national speaker’s opinion, oxymetazoline might be just slightly less efficacious, but with fewer side effects.
The medication works by restricting the widening (dilation) of the blood vessels in your face. Research has shown it can start to have an effect about 30 minutes after it’s first used, and this can last for around 12 hours.
Other Strategies
Avoidance of excessively hot foods or liquids, sun, wind and other triggers.
Sucking on ice chips once the flushing begins may be tried.
Flushing may be treated with propranolol 40 mg twice daily or clonidine 50 mg twice daily. The telangiectasias (prominent blood vessels)–whether rosacea is present or not–may be removed with the pulsed dye laser.
Botox
Intradermal injection of botulism toxin is an effective and safe method of treating facial erythema of rosacea according to one study of 25 patients 12.
Oral treatments
Alternatively, there are a number of oral medications that may help improve redness caused by rosacea.
These include:
- clonidine – a medication that relaxes the blood vessels
- beta-blockers – medications that decrease the activity of the heart
- anxiety medications – medications sometimes used to help calm the person and reduce blushing
It’s not clear how effective these medications are at treating redness caused by rosacea, but they may sometimes be prescribed under the supervision of a dermatologist.
Laser and intense pulsed light (IPL) treatment
Redness and visible blood vessels (telangiectasia) can also sometimes be successfully improved with vascular laser or intense pulsed light (IPL) treatment. These treatments may also improve flushing.
A referral to a dermatologist is usually required before having these treatments, so you may need to pay for them privately. Around two to four treatments may be needed, so the overall cost may be significant.
Laser and intense pulsed light machines produce narrow beams of light that are aimed at the visible blood vessels in the skin. The heat from the lasers damages the dilated veins and causes them to shrink so they’re no longer visible, with minimal scarring or damage to the surrounding area.
Laser treatment can cause pain, but most people don’t need an anesthetic. Side effects of laser treatment are usually mild and can include:
- bruising
- crusting of the skin
- swelling and redness of the skin
- blisters (in rare cases)
- infection (in very rare cases)
These side effects usually only last a few days and are rarely permanent.
Rhinophyma treatment
In some people with rosacea the skin of the nose can become thickened. This is known as rhinophyma. Rhinophyma is the result of enlarged oil glands in the nose.
For mild cases, isotretinoin can gradually shrink the oil glands.
If you have severe rhinophyma, your doctor may refer you to a dermatologist or plastic surgeon to discuss ways the appearance of your skin can be improved. Treatments for more advanced rhinophyma are more dramatic – you must remove the excessive skin with an erbium or CO2 laser. In some instances, plastic surgeon even use a scalpel, specially designed abrasive instruments using a technique called dermabrasion or heated wire loop. All these treatments leave the skin totally raw, and you must wait for it to heal, which can take about 2 weeks. Fortunately, depending on the severity of each individual case, the results can last anywhere from 10 to 20 years.
Home remedies
There are a number of things you can do yourself to help keep the symptoms of rosacea under control, including:
- Avoiding things that trigger your symptoms – for example, by using sun cream and covering yourself up if direct sunlight makes your symptoms worse
- Taking good care of your skin – for example, by using products suitable for sensitive skin
- Using make-up – patches of persistent red skin can be disguised using specially designed camouflage make-up
- Keeping your eyelids clean – if rosacea is causing your eyelids to become inflamed (blepharitis)
- Sunlight – use a broad-spectrum sunscreen with a sun protection factor (SPF) of 30 or more on your face.
- Avoid drinking hot liquids and alcohol, eating spicy foods, and excessive heat exposure.
- Protect the face in winter with a scarf or mask.
- Avoid facial products with alcohol or other skin irritants (astringents, toners, sorbic acid, menthol, camphor), and use mild cleansers for the face.
- Fair-skinned people may find a green- or yellow-tinted makeup helps to hide redness.
- Cool compresses, gel masks, and central face massage may be of some benefit.
- Benzoyl peroxide may help some people but can also be easily irritating to the skin.
- Nicomide T is a combination of a vitamin (nicotinamide) and zinc available in cream and gel form, which may be helpful.
Avoid triggers
Many people with rosacea notice certain triggers make their symptoms worse. Although it’s not always practical or possible, taking steps to avoid these triggers can help reduce the severity and frequency of your symptoms.
If you’re not sure whether your symptoms have a specific trigger, it may be useful to keep a diary to identify whether your symptoms get worse depending on things like the activities you do and foods or drinks you have.
Advice about how to avoid some common triggers can be found below.
Sunlight
As sunlight is the most commonly reported trigger of rosacea, you should use sun cream whenever possible, even when it’s overcast.
A sunscreen cream with broad-spectrum and a sun protection factor (SPF) of at least 30 is recommended. A broad-spectrum sun cream that protects against UVA and UVB light should be used.
Using sun creams specifically designed for children may help reduce skin irritation. Covering exposed skin with clothes or a sun hat may also help.
Try to minimise your exposure to the sun during the summer months, particularly in the middle of the day when the sun is at its hottest.
But remember, sun can also be strong in the morning and evening, so take adequate precautions at these times as well.
Stress
Stress is also a commonly reported trigger of rosacea. Successfully managing your stress levels can help control your symptoms.
Ways you can reduce stress include:
- learning relaxation techniques, such as deep breathing exercises, meditation and yoga
- taking regular exercise
As strenuous exercise can sometimes make rosacea symptoms worse, a low-intensity exercise programme, such as walking or swimming, may be better than high-intensity activities, such as running or aerobics.
Food and drink
Some of the most commonly reported food- and drink-related triggers are alcohol and spicy foods. You may want to try completely removing these from your diet to see if your rosacea improves.
But there are many other dietary triggers that can also affect some people with rosacea.
It’s a good idea to include information about how your diet affects your rosacea symptoms in your rosacea diary.
Cold weather
Covering your face and nose with a scarf can help protect your skin from cold temperatures and wind.
If you need to spend considerable time outside during cold weather, protect your face with a balaclava.
Skincare techniques
The advice below about skincare techniques may also help control your rosacea symptoms.
- Gently clean your skin every morning and evening using a gentle, non-abrasive cleanser – use soap-free cleansers with non-alkaline or neutral pH. Avoid scented soaps and alcohol-based skin cleansers.
- Rinse your face with lukewarm water and allow skin to dry thoroughly before you apply medication or make-up.
- Look for products suitable for sensitive skin – these are usually described as mild, hypoallergenic, fragrance-free and non-comedogenic (will not block pores).
- Use a moisturizer to soothe skin if it feels sore.
- Avoid oil-based or waterproof cosmetics requiring solvents for removal – use water-based make-up and skin products instead.
- Avoid astringents, toners and other facial or hair products that contain ingredients that might irritate your skin – such as fragrances, alcohol, menthol, witch hazel, eucalyptus oil, camphor, clove oil, peppermint, sodium lauryl sulphate and lanolin.
- You may want to avoid using anything on your skin that you aren’t sure of – you can then gradually reintroduce products once your symptoms have been treated and cleared to see if you can use them again without any problems.
- Men may find that using an electric razor, rather than a blade, helps reduce skin irritation.
- Some people find regular gentle facial massage reduces swelling (lymphoedema).
- Don’t use steroid cream unless you’re specifically instructed to by your doctor – it may make your symptoms worse.
Make-up
It may be possible to disguise patches of persistent red skin using specially designed camouflage make-up.
Eyelid hygiene
If your eyelids are inflamed as a result of rosacea (blepharitis), cleaning your eyelids every day with warm water and a small amount of cleaning solution can help ease your symptoms.
Avoiding eye make-up can also help reduce your symptoms, but if you do choose to wear eye make-up, make sure it is a type that washes off easily so you can still clean your eyelids.
It’s important to clean your eyelids every day if you have blepharitis, even if you’re using medication or don’t currently have any symptoms.
Good eyelid hygiene can help ease your symptoms and prevent it happening again.
Follow the steps below to keep your eyelids clean.
Warm compresses
- boil water and leave it to cool to a warm temperature
- soak a clean flannel or eye pad in the water and gently place this over the eyes for around 10 minutes
- make sure the flannel doesn’t get cold by reheating it in the warm water
You can also buy a special microwaveable compress for your eyes to use instead of a flannel.
Eye lid massage
- gently massage your closed eyes by rolling your little finger in a circular motion
- take a cotton wool bud and, with your eyes shut, gently roll it downwards on the upper eyelid towards the lashes and edges of the eyelids – this helps to push the melted oil out of the glands, but you won’t be able to see the tiny droplets
- repeat this process along the whole width of the upper and lower eyelids
This process may slightly irritate your eyes at first, a bit like getting soap in your eyes. However, this is normal and should get better with time.
Lid margin hygiene
Various eyelid-cleaning solutions and eyelid wipes are available commercially, or you can try making one at home.
- For a home-made solution, fill a bowl with one pint of boiled water and allow it to cool to a warm temperature. Add a teaspoon of bicarbonate of soda.
Once you’ve made a cleaning solution:
- soak some clean cotton wool in the solution and remove crustiness from around the eyelids, paying special attention to the eyelashes
- repeat this process if necessary using a clean piece of cotton wool
- dip a clean cotton bud into the solution and gently clean the edges of the eyelids by wiping the cotton bud along the bases and lengths of the lashes
Your doctor, pharmacist or optometrist can advise you about suitable cleaning solutions, although you may need to try more than one product to find one that suits you.
It’s important to continue lid margin hygiene two or three times a week, even if you don’t have symptoms. This helps to prevent permanent scarring of the eyelid margins.
Antibiotic drops and ointments
If you have blepharitis that doesn’t respond to regular cleaning, you may be prescribed a course of antibiotic ointments, creams or eye drops (topical antibiotics). You’ll usually need to use these for around four to six weeks.
Ointments and creams should be rubbed gently on to the edge of your eyelids, usually several times a day at first, using either clean fingers or a cotton bud.
Once your condition begins to improve, you may only need to do this once a day, usually at night after cleaning your eyelids using the method outlined above.
Cautions
You should avoid wearing contact lenses when using antibiotic eye drops, as the drops may build up behind the lenses and irritate your eye.
If you’re using more than one type of eye drop at the same time of day, leave at least five minutes before applying the second type of drops.
Let your doctor or optometrist know if you have continual irritation as they may recommend lubricant treatments.
You may experience some mild stinging or burning when applying antibiotic ointment or drops, but this should pass quickly. Don’t drive if the ointment blurs your vision.
Oral antibiotics
Low doses of antibiotics can be used as anti-inflammatory agents for a minimum of three to four months, or sometimes much longer.
You may be prescribed antibiotics to take by mouth once or twice a day if your blepharitis doesn’t respond to other treatments.
Oral antibiotics may also be recommended at the start of your treatment if it’s thought rosacea is aggravating your symptoms.
Most people respond well within the first few weeks of treatment, although you may need to take them for up to three months. It’s important for you to finish the course of antibiotics, even if your symptoms get better.
Cautions
Some oral antibiotics used to treat blepharitis have been known to make people more sensitive to the effects of the sun. While you’re taking them, you should avoid prolonged exposure to sunlight and using sun lamps or sunbeds.
Oral antibiotics can also sometimes affect unborn and developing babies, so they’re not normally used to treat women who are pregnant or breastfeeding. Certain types of antibiotics are avoided in children under 12.
Side effects of oral antibiotics are rare because the dose is very low. However, you should be aware of stomach upsets, vomiting or diarrhoea.
Oily tear eye drops
Oily tear drops are particularly useful if your blepharitis is causing quick evaporation of tears.
Eye drops that replace the oily part of the tear film and reduce evaporation from the surface of the eye are increasingly being used. These preparations include synthetic guar gums or liposomal sprays.
Liposomal sprays are over-the-counter medications that aren’t available on prescription. They’re sprayed on to the edges of your eyelids when your eyes are closed. When you open your eyes, the solution spreads across the surface of the eye, creating a new oily film.
Rosacea diet
There’s some evidence to suggest a diet high in omega-3 fats can help improve blepharitis.
The best sources of omega-3s are oily fish, such as:
- mackerel
- salmon
- sardines
- herring
- fresh or frozen tuna – not canned, as the canning process sometimes removes the beneficial oils
Aim to eat at least two portions of fish a week, one of which should be oily fish.
You can also get omega-3s from various nuts and seeds, vegetable oils, soya and soya products, and green leafy vegetables.
Omega 7 or sea buckthorn oil has also been found to be helpful.
Treating other conditions
If you have an underlying medical condition that’s causing blepharitis, your doctor will prescribe treatment for it or refer you to an appropriate specialist to ensure the condition is treated effectively.
Depending on the suspected cause of your condition and any other symptoms you have, you may also need additional treatment.
For example, if you have seborrheic dermatitis or dandruff, you may need to use an anti-dandruff shampoo on your scalp and eyebrows.
If you have dry eye syndrome, which frequently occurs alongside blepharitis, you may need separate treatment for this, such as “artificial tear” eye drops.
Dry eye syndrome
Dry eye syndrome is a common complication of blepharitis. It occurs when your eyes don’t make enough tears or your tears evaporate too quickly. This can lead to your eyes drying out and becoming inflamed, which can cause them to feel dry, gritty and sore.
Dry eye syndrome can be caused by the same skin conditions that can cause blepharitis, as these can also affect the quality of your tears. These include:
- seborrheic dermatitis – a condition that causes your skin to become oily or flaky
- rosacea – a condition that mainly affects the face
Treatment for dry eye syndrome helps to control the symptoms, but there’s no cure. Some people may have recurring episodes for the rest of their lives.
The exact treatment for dry eye syndrome depends on whether symptoms are caused by:
- decreased production of tears
- tears that evaporate too quickly
- an underlying condition
The first thing to consider is whether there are any obvious factors, such as a medication, causing the symptoms.
If your dry eye syndrome is caused by an underlying condition, your doctor can prescribe treatment or refer you to an appropriate specialist.
You may also be able to help prevent dry eye syndrome or ease your symptoms by adjusting your environment, keeping your eyes clean, and improving your diet.
There are a number of things you can do to help prevent dry eye syndrome or ease your symptoms.
Environmental factors
Certain environments can irritate your eyes. Keep your eyes protected from:
- wind
- hot air
- smoke
- dust
Wrap-around glasses may provide good protection. Avoid smoky environments, and you should try to stop smoking if you smoke.
Avoid using eye make-up. Eyeliner and mascara can block the glands in the eyelids and cause the area around your eyes to become inflamed.
Specialized eyewear
Some cases of dry eye disease can be treated using specialized eyewear. These include specially made glasses called moisture chamber spectacles. These wrap around your eyes like goggles, helping to retain moisture and protecting your eyes from irritants.
If your previous contact lenses were causing dry eye disease, special contact lenses are also available. You should discuss various options with your optometrist.
Adjust your computer
If you regularly use a computer, make sure your computer workstation is set up correctly to minimize eye strain. Your monitor should stand at eye level or just below it.
If you use a computer at work, most employers have a health and safety officer or an occupational health representative who can advise you.
You should also make sure to take regular breaks away from your computer screen every hour.
Use a humidifier or air filter
A humidifier, such as a cool mist device, at work and home will moisten the surrounding air and can help reduce your symptoms.
Opening windows for a few minutes on cold days and longer in spring and summer will also help keep air moist and prevent a build-up of mould.
If you work or live in a particularly dusty environment, you may also find it useful to use an air filter.
Lubricant treatments
Mild to moderate cases of dry eye syndrome can usually be treated using lubricant eye treatments that consist of a range of drops, gels and ointments.
These lubricants are often called artificial tears because they replace the missing water in the tear film. However, they don’t contain the antibodies, vitamins and nutrients found in normal tears that are essential for eye health.
Most lubricants are available without a prescription over the counter from a chemist.
There are many different types of eye drops and gels, and it’s often worth trying a number of different ones to find one that suits you.
Sometimes you may have to use two or three different compounds to have the best effect. However, it’s important you discuss any changes you wish to make to your treatment with your optometrist or doctor.
Preservative-free drops
Some eye drops contain preservatives to prevent harmful bacteria growing inside the medicine bottle. If your symptoms mean you need to use these eye drops more than six times a day, it’s better to use preservative-free eye drops.
This is particularly important if your ophthalmologist has told you that you have severe dry eye disease. Preservatives used in large quantities or over a prolonged period of time – months or years – may damage the delicate cells on the surface of the eye or cause inflammation.
If you wear soft contact lenses, you may also need to use a preservative-free lubricant, as preservatives attach to the contact lens and damage the eye. These types of eye drops may be more expensive.
If you have any difficulty putting in your drops, please discuss this with your doctor or optometrist. There are mechanical devices to help squeeze bottles, multi-dose bottles with valves, and single dose containers that may be easier for you.
‘Oily’ tear eye drops
Eye drops that replenish the oily part of the tear film and reduce evaporation from the surface of the eye are also increasingly being used. These preparations include synthetic guar gums or liposomal sprays.
Liposomal sprays are over-the-counter medications that aren’t available on a prescription. They are sprayed on to the edges of your eyelids when your eyes are closed.
When you open your eyes, the solution spreads across the surface of the eye, creating a new oily film.
Oily tear drops are particularly useful if you have blepharitis or dry eye syndrome caused by your tears evaporating too quickly.
Eye ointments
Eye ointments can also be used to help lubricate your eyes and keep them moist overnight, as your tears can evaporate while you sleep if your eyes aren’t fully closed.
These ointments tend to be used overnight because they can cause blurred vision.
If you wear contact lenses, don’t use eye ointments while wearing them. Ask your pharmacist or doctor for advice about alternative treatments that may be suitable for you.
Anti-inflammatory treatments
The underlying problem with long-term dry eye syndrome is inflammation in and around the eye. One of the anti-inflammatory treatments mentioned below may also be recommended, but these can only be obtained after you’ve seen an ophthalmologist.
Corticosteroid eye drops and ointments
Corticosteroids are powerful anti-inflammatory medications that can be given as eye drops or ointments in severe cases of dry eye syndrome.
They have side effects in around one in every three people, which may include:
- cataracts
- raising the pressure within the eye
This group of treatments should only be used if you’re being reviewed by an ophthalmologist at an eye clinic. You shouldn’t use these treatments if you have no follow-up at an eye clinic.
Oral tetracyclines
Low doses of medications called tetracyclines can be used as anti-inflammatory agents for a minimum of three to four months, and sometimes for much longer.
The most common tetracycline used is doxycycline, but others, such as oxytetracycline and lymecycline, are sometimes also prescribed.
Ciclosporin eye drops
Ciclosporin is a medication that suppresses the activity of your immune system. It is sometimes used in the treatment of severe dry eye syndrome that doesn’t respond to lubricants.
This treatment is only available through a specialist in dry eye syndrome at a hospital eye department.
Serum eye drops
Serum eye drops may be required in very rare cases where all other medications haven’t worked. These are special eye drops made using components of your own blood or blood from a donor.
To make serum eye drops, one unit of blood is taken under sterile conditions, as for regular blood donation. The blood cells are then removed and the remaining serum is diluted and put into eye drop bottles.
Because of quality standards, this process can take several months before the treatment is finally available to use.
Treating underlying medical conditions
If you have an underlying medical condition that’s causing dry eye syndrome, your doctor will prescribe treatment for it or refer you to an appropriate specialist.
Surgery
If your dry eyes are severe and fail to respond to other forms of treatment, surgery may be an option. Two types of surgery sometimes used to treat dry eye syndrome are described below.
Punctal occlusion
Punctal occlusion involves using small plugs called punctal plugs to seal your tear ducts. This means your tears won’t drain into the tear ducts and your eyes should remain moist.
Temporary plugs made of silicone are normally used first to determine whether the procedure has a positive effect. If it does, more permanent plugs can replace the silicone ones.
In more severe cases, the tear ducts are sealed using heat (cauterised). This permanently seals the drainage hole to increase the amount of tears on the surface.
Salivary gland autotransplantation
Salivary gland autotransplantation is an uncommon procedure that’s usually only recommended after all other treatment options have been tried.
This procedure involves removing some of the glands that produce saliva from your lower lip and placing them under the skin around your eyes. The saliva produced by the glands acts as a substitute for tears.
Conjunctivitis
Conjunctivitis is inflammation of the conjunctiva. This is the transparent membrane that covers the white part of the eyeball and the inner surfaces of the eyelids.
Conjunctivitis can occur when bacteria in the eyelid infect the eyes. The condition isn’t usually serious and shouldn’t affect your vision.
Most cases of conjunctivitis are mild and pass in one to two weeks without the need for treatment. However, you should contact your doctor or an optometrist if you think you have conjunctivitis.
If you wear contact lenses, you should remove these and not wear them again until the conjunctivitis is better.
Antibiotic eye drops may be prescribed if your symptoms continue or you have repeated infections.
Rosacea natural treatment
Gentle daily facial massage may help reduce swelling and inflammation. Use a circular motion with your fingers starting on the central part of the face and work toward the ears.
Many other alternative therapies — including colloidal silver, emu oil, laurelwood and oregano oil — have been touted as possible ways to treat rosacea. But no conclusive evidence supports the idea that any of these substances are effective.
Talk with your doctor if you’re considering dietary supplements or other alternative therapies to treat rosacea. He or she can help you weigh the pros and cons of specific alternative therapies.
- Siddiqui K, Gold LS, Gill J. The efficacy, safety, and tolerability of ivermectin compared with current topical treatments for the inflammatory lesions of rosacea: a network meta-analysis. SpringerPlus. 2016;5(1):1151. doi:10.1186/s40064-016-2819-8. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4956638/[↩]
- Int J Dermatol. 2015 Apr;54(4):481-7.[↩]
- Clin Exp Dermatol 2014;39;448-453[↩]
- JEADV 2016;30;2105[↩]
- JID 2014;134;2267[↩]
- Australas J Dermatol. 2016 Jul 20[↩]
- Small intestinal bacterial overgrowth in rosacea: clinical effectiveness of its eradication. Clin Gastroenterol Hepatol. 2008 Jul;6(7):759-64. doi: 10.1016/j.cgh.2008.02.054. Epub 2008 May 5. https://www.ncbi.nlm.nih.gov/pubmed/18456568[↩]
- Rosacea and small intestinal bacterial overgrowth: Prevalence and response to rifaximin. J Am Acad Dermatol. 2013 May;68(5):875-6. doi: 10.1016/j.jaad.2012.11.038. http://www.jaad.org/article/S0190-9622(12)02330-4/fulltext[↩]
- Journal of Investigative Dermatology 2013;133;2480–2483[↩]
- JAAD Feb and May 2014[↩]
- JAMADerm 2015;151;136[↩]
- Dermatol Surg 2015 Jan.:S9-S16[↩]