Contents
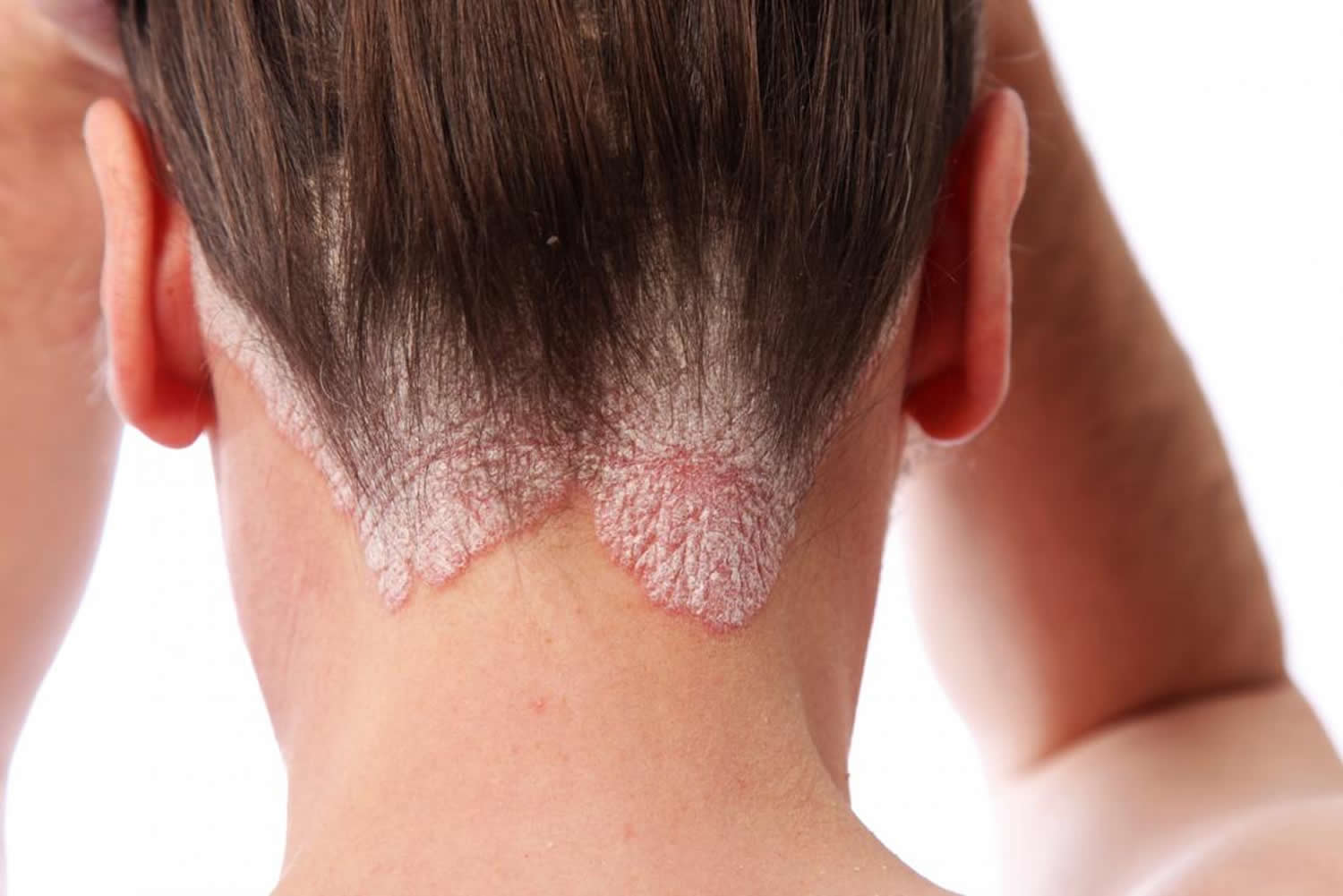
Scalp psoriasis
Psoriasis is common on the scalp. Researchers estimate that at least half (50 percent) of the people who have plaque psoriasis will have at least one flare-up on the scalp. Psoriasis is a chronic (long-lasting) immune-mediated skin disease that causes itchy or sore patches of thick, raised, red skin with silvery scales to appear on the skin 1. Scalp psoriasis can be very mild, with slight, fine scaling. It can also be very severe with thick, crusted plaques covering the entire scalp. Psoriasis can extend beyond the hairline onto the forehead, the back of the neck and appears behind the ears.
Other skin disorders, such as seborrheic dermatitis, may look similar to psoriasis. However, scalp psoriasis appears powdery with a silvery sheen, while seborrheic dermatitis appears yellowish and greasy.
Scalp psoriasis vs. seborrheic dermatitis: What’s the difference ?
Your doctor can usually tell whether you have scalp psoriasis, seborrheic dermatitis or both based on an examination of your skin, scalp and nails.
Scalp psoriasis and seborrheic dermatitis are common conditions that affect the scalp. In addition, they share some similar signs and symptoms, such as red, scaly skin.
Most often, the scales of psoriasis are thicker and somewhat drier in appearance than are the scales of seborrheic dermatitis. In addition, psoriasis usually affects more than one area of the body. If you have scalp psoriasis, you may also have mild psoriasis on your elbows, knees, hands or feet or may notice subtle nail changes, such as pitting.
Compare signs and symptoms
Scalp psoriasis
- Red skin covered with flakes and silvery scales
- Skin flakes (dandruff) that may attach to the hair shaft
- Patchy silvery scales or thick crust on the scalp that may bleed when removed
- Patches that may extend beyond hairline or appear on other parts of the body
- Itching or soreness
Seborrheic dermatitis of the scalp
- Red skin covered with greasy-looking white or yellowish scales
- Skin flakes (dandruff) that may attach to the hair shaft
- Patchy scales or crust on the scalp that may be easily removed
- Possibly itching
Scalp psoriasis and seborrheic dermatitis of the scalp share some similar treatments, including medicated shampoos and topical corticosteroid or antifungal solutions. Scalp psoriasis is often persistent and more difficult to treat than is seborrheic dermatitis of the scalp.
What is Plaque psoriasis (also called psoriasis vulgaris)
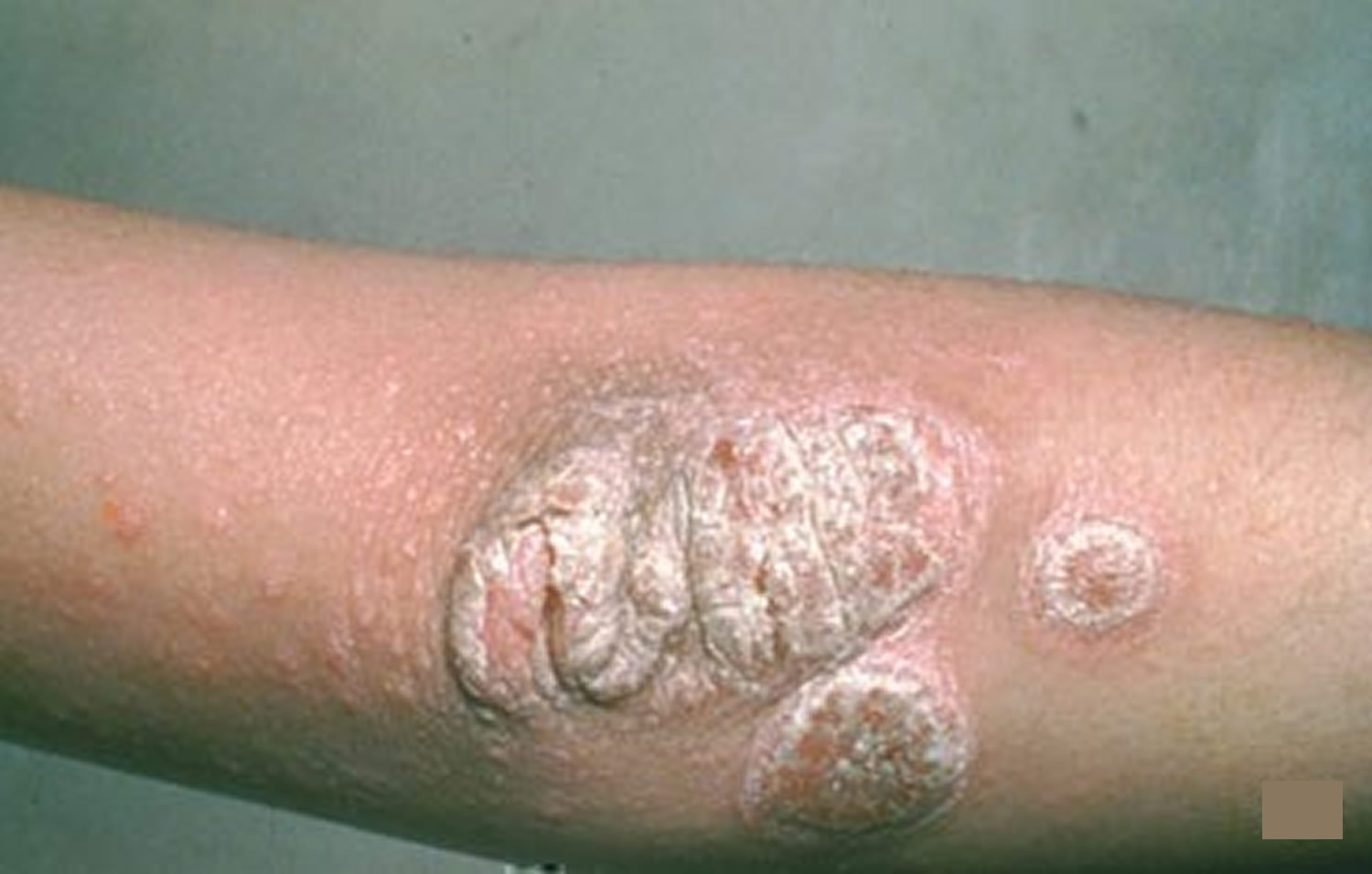
The most common form, plaque psoriasis causes dry, raised, red skin lesions (plaques) covered with silvery-white scales. The plaques might be itchy or painful and there may be few or many. They can occur anywhere on your body, including your genitals and the soft tissue inside your mouth.
Signs and symptoms (see Figure 2):
- Raised, reddish patches on the skin called plaque.
- Patches may be covered with a silvery-white coating, which dermatologists call scale.
- Patches can appear anywhere on the skin.
- Most patches appear on the knees, elbows, lower back, and scalp.
- Patches can itch.
- Scratching the itchy patches often causes the patches to thicken.
- Patches vary in size and can appear as separate patches or join together to cover a large area.
- Nail problems — pits in the nails, crumbling nail, nail falls off.
Figure 1. Scalp psoriasis
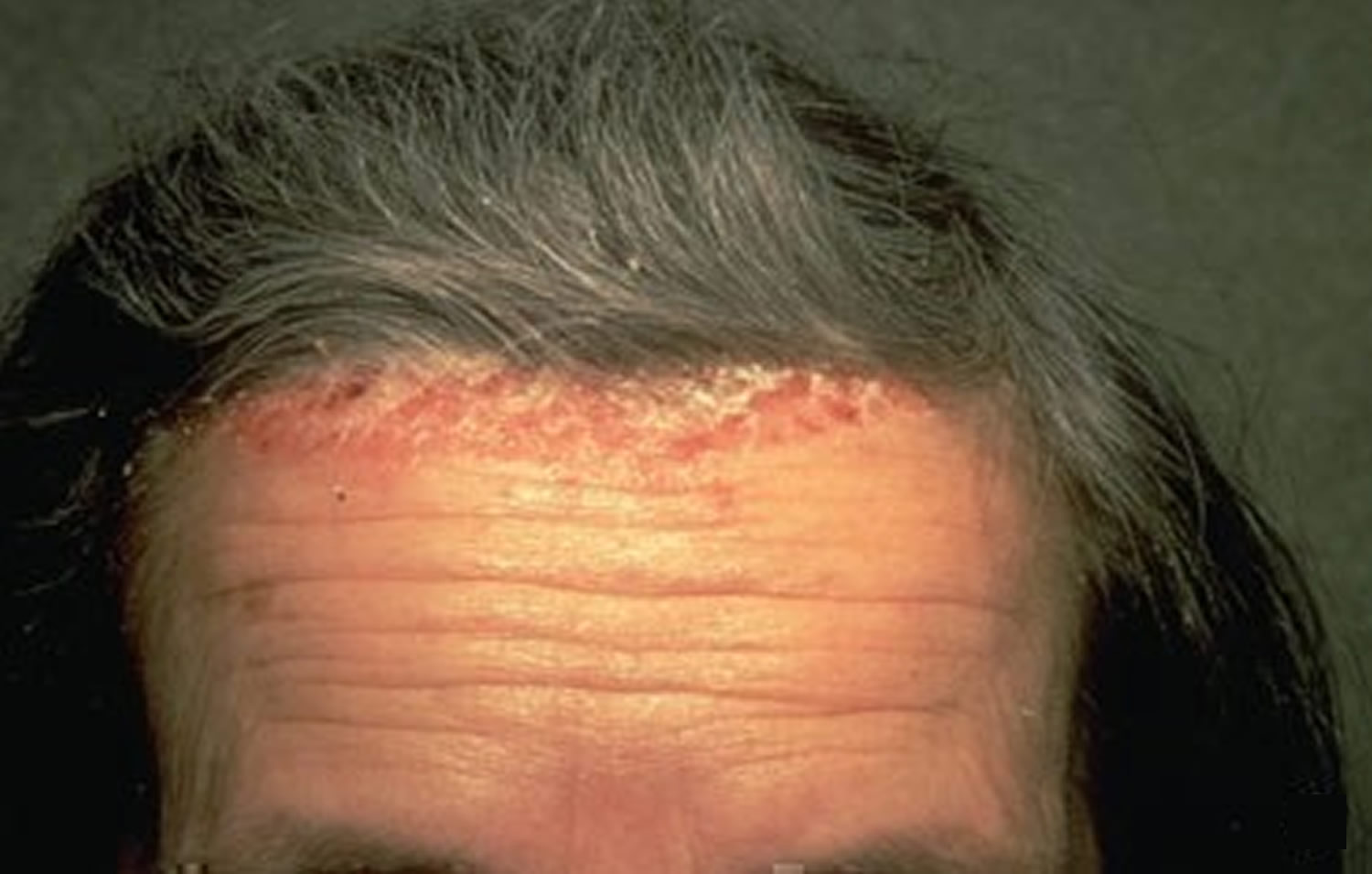
Figure 2. Plaque psoriasis
What causes psoriasis of the scalp
Regardless of where psoriasis forms, the cause is the same.
Psoriasis develops when your immune system sends faulty signals that tell skin cells to grow too quickly. In a process called cell turnover, skin cells that grow deep in your skin rise to the surface. Normally, new skin cells take weeks to rise to the surface. In psoriasis, it happens in just days because your cells rise too fast.
The body does not shed these excess skin cells. The skin cells pile up on the surface of the skin, causing patches of psoriasis to appear.
Psoriasis may look contagious, but it’s not. You cannot get psoriasis from touching someone who has it. To get psoriasis, a person must inherit the genes that cause it.
Psoriasis typically affects the outside of the elbows, knees or scalp, though it can appear on any location. Some people report that psoriasis is itchy, burns and stings. Psoriasis is associated with other serious health conditions, such as diabetes, heart disease and depression.
If you develop a rash that doesn’t go away with an over-the-counter medication, you should consider contacting your doctor.
Psoriasis can be hard to diagnose because it can look like other skin diseases. Your doctor might need to look at a small skin sample under a microscope.
While scientists do not know what exactly causes psoriasis, they do know that the immune system (problem with T cells and other white blood cells, called neutrophils, in your body) and genetics play major roles in its development.
T cells (T lymphocytes) normally travel through the body to defend against foreign substances, such as viruses or bacteria. But if you have psoriasis, the T cells (T lymphocytes) attack healthy skin cells by mistake, as if to heal a wound or to fight an infection.
Overactive T cells also trigger increased production of healthy skin cells, more T cells and other white blood cells, especially neutrophils. These travel into the skin causing redness and sometimes pus in pustular lesions. Dilated blood vessels in psoriasis-affected areas create warmth and redness in the skin lesions.
The process becomes an ongoing cycle in which new skin cells move to the outermost layer of skin too quickly — in days rather than weeks. Skin cells build up in thick, scaly patches on the skin’s surface, continuing until treatment stops the cycle.
Just what causes T cells to malfunction in people with psoriasis isn’t entirely clear. Researchers believe both genetics and environmental factors play a role.
Moreover, scientists are still trying to learn everything that happens inside the body to cause psoriasis.
Usually, something triggers psoriasis to flare. The skin cells in people with psoriasis grow at an abnormally fast rate, which causes the buildup of psoriasis lesions.
Scientists have learned that a person’s immune system and genes play important roles. It seems that many genes must interact to cause psoriasis.
Scientists also know that not everyone who inherits the genes for psoriasis will get psoriasis. It seems that a person must inherit the “right” mix of genes. Then the person must be exposed to a trigger.
Which genes make a person more likely to develop psoriasis ?
Scientists have now identified about 25 genetic variants that make a person more likely to develop psoriatic disease. At the University of Michigan, Dr. J.T. Elder and his team of researchers have identified several areas on the human genome where more than one gene may be involved in psoriasis and psoriatic arthritis.
At the University of California-San Francisco, Dr. Wilson Liao is using new genetic sequencing technology to find rare “trigger genes” that may be the leading causes of psoriasis in certain individuals.
Working with DNA samples from a large family that includes many people with psoriasis, Anne Bowcock, Ph.D., a professor of genetics at Washington University School of Medicine in St. Louis, has identified a gene mutation known as CARD14 that when triggered leads to plaque psoriasis.
At the University of Utah, Drs. Gerald Krueger and Kristina Callis Duffin have carefully catalogued the psoriasis of more than 1,200 patients. By comparing the genes of each individual to the way psoriasis shows up on his or her body, the team hopes to understand which genes are involved in specific types of disease.
Using a NPF Discovery grant, British researcher Francesca Capon found that a mutation to the gene called IL36RN might be involved in the three forms of pustular psoriasis.
What triggers psoriasis ?
Many people say that their psoriasis began after they experienced one of these common psoriasis triggers:
- A stressful event.
- Smoking.
- Heavy alcohol consumption
- Infections, such as strep throat or skin infections.
- Certain medications — including lithium, which is prescribed for bipolar disorder, high blood pressure medications such as beta blockers, antimalarial drugs, and iodides.
- Cold, dry weather.
- Injury to the skin, such as a cut or scrape, a bug bite, or a severe sunburn.
- Vitamin D deficiency.
Certain medications are associated with triggering psoriasis, including:
- Lithium: Used to treat manic depression and other psychiatric disorders. Lithium aggravates psoriasis in about half of those with psoriasis who take it.
- Antimalarials: Plaquenil, Quinacrine, chloroquine and hydroxychloroquine may cause a flare of psoriasis, usually two to three weeks after the drug is taken.
- Hydroxychloroquine is the least likely to cause side effects.
- Inderal: This high blood pressure medication worsens psoriasis in about 25 percent to 30 percent of patients with psoriasis who take it. It is not known if all high blood pressure (beta blocker) medications worsen psoriasis, but they may have that potential.
- Quinidine: This heart medication has been reported to worsen some cases of psoriasis.
- Indomethacin: This is a nonsteroidal anti-inflammatory drug used to treat arthritis. It has worsened some cases of psoriasis. Other anti-inflammatories usually can be substituted. Indomethacin’s negative effects are usually minimal when it is taken properly. Its side effects are usually outweighed by its benefits in psoriatic arthritis.
Risk factors for psoriasis
Anyone can develop psoriasis, but these factors can increase your risk of developing the disease:
- Family history. This is one of the most significant risk factors. Having one parent with psoriasis increases your risk of getting the disease, and having two parents with psoriasis increases your risk even more.
- Viral and bacterial infections. People with HIV are more likely to develop psoriasis than people with healthy immune systems are. Children and young adults with recurring infections, particularly strep throat, also may be at increased risk.
- Stress. Because stress can impact your immune system, high stress levels may increase your risk of psoriasis.
- Obesity. Excess weight increases the risk of psoriasis. Lesions (plaques) associated with all types of psoriasis often develop in skin creases and folds.
- Smoking. Smoking tobacco not only increases your risk of psoriasis but also may increase the severity of the disease. Smoking may also play a role in the initial development of the disease.
Scalp Psoriasis symptoms and signs
Psoriasis can appear anywhere on the scalp. Sometimes a small patch develops, which can be easy to hide with hair. Scalp psoriasis also can cover the entire scalp. When psoriasis appears on the scalp, you may notice:
- Reddish patches on the scalp. Some patches are barely noticeable. Patches also can be very noticeable, thick, and inflamed.
- Dandruff-like flaking and silvery-white scale. Scalp psoriasis can look a lot like dandruff. Many people who have scalp psoriasis see flaking. But there are differences between scalp psoriasis and dandruff. Unlike dandruff, scalp psoriasis causes a silvery sheen and dry scale on the scalp.
- Dry scalp. The scalp may be so dry that the skin cracks and bleeds.
- Itching. This is one of the most common symptoms. For some the itch is mild; others have intense itching that can interfere with everyday life and cause sleepless nights.
- Bleeding. Because scalp psoriasis can be very itchy, almost everyone scratches. Scratching can make the scalp bleed. Scratching also tends to worsen the psoriasis. Scratching can make the patches larger and thicker. This is why dermatologists tell their patients, “Try not to scratch your scalp.”
- Burning sensation or soreness. The scalp can burn. It can feel extremely sore.
- Temporary hair loss. Scratching the scalp or using force to remove the scale can cause hair loss. Once the scalp psoriasis clears, hair usually regrows.
These signs and symptoms can come and go. Some people have only one mild flare on their scalps. Others have many flare-ups, which can range from mild to serious. Many things can trigger a flare-up, including stress, cold, and dry air.
How to treat scalp psoriasis
Scalp psoriasis causes many people discomfort. Some people feel embarrassed. Treatment can ease these problems. There are many safe and effective treatments. Some people get relief from a medicated shampoo or solution. A few of these can be purchased without a prescription.
But scalp psoriasis can be stubborn. Many people see a dermatologist for treatment. A dermatologist can tell you what can help. The following types of treatment can help scalp psoriasis:
- Medicine applied to the scalp.
- Medicated shampoos.
- Scale softeners.
- Injections.
- Light treatments.
- Biologics and other medicines that work throughout the body.
Scalp psoriasis treatment guideline 2
Topical treatment of psoriasis affecting the scalp
- Topical corticosteroids. These drugs are the most frequently prescribed medications for treating mild to moderate psoriasis. They reduce inflammation and relieve itching and may be used with other treatments. Your doctor may prescribe stronger corticosteroid ointment applied once daily for up to 4 weeks as initial treatment for people with scalp psoriasis. Steroids can be absorbed through the skin and affect internal organs. This occurs when a steroid is excessively misused, such as when applied to widespread areas of skin, used over long periods of time or used with excessive occlusion. Women who are pregnant or nursing should discuss the use of steroids with their health care provider. Topical steroids can be absorbed through the skin and get into breast milk.
- Do not offer coal tar-based shampoos alone for the treatment of severe scalp psoriasis.
Coal Tar
Tar derived from both coal and wood (e.g., juniper, pine) are both used for medicinal purposes. However, coal tar is the type used most commonly to treat psoriasis. Tar can help slow the rapid growth of skin cells and restore the skin’s appearance. In addition, it can help reduce the inflammation, itching and scaling of psoriasis. Tar products can vary dramatically from brand to brand. Generally, the higher the concentration of tar, the more potent the product.
Tar can irritate, redden and dry the skin. Test a tar product on a small area of the skin first. If reddening occurs, try applying the tar on top of a moisturizer. Tar can stain clothing, bed linen, and light-colored hair. Tar makes skin more sensitive to sunlight, so be sure to wash it off thoroughly, use sunscreen and monitor your sun exposure. Tar remains active on the skin for at least 24 hours, and you are at increased risk of sunburn during this period.
Studies show some of the chemicals in coal tar may cause cancer, but only in very high concentrations, such as in what is used in industrial paving. Anyone using tar regularly should follow a regular skin cancer checkup schedule. California requires over-the-counter (OTC) coal tar shampoos, lotions and creams that contain more than 0.5 percent coal tar to be labeled with cancer warnings. However, the FDA maintains that over-the-counter (OTC) products with coal tar concentrations between 0.5 percent and 5 percent are safe and effective for psoriasis, and there is no scientific evidence that the tar in over-the-counter (OTC) products is carcinogenic.
If treatment with a potent corticosteroid does not result in clearance, near clearance or satisfactory control of scalp psoriasis after 4 weeks consider:
- A different formulation of the potent corticosteroid (for example, a shampoo or mousse) and/or
- Topical agents to remove adherent scale (for example, agents containing salicylic acid, emollients and oils) before application of the potent corticosteroid. A suspension of 10% salicylic acid in mineral oil may be rubbed into the scalp at bedtime manually or with a toothbrush, covered with a shower cap (to enhance penetration and avoid messiness), and washed out the next morning with a tar (or other) shampoo.
Salicylic Acid
Salicylic acid is classified as a keratolytic, or peeling agent, and works by causing the outer layer of skin to shed. It is a common and effective treatment for a wide variety of skin problems. As a psoriasis treatment, it acts as a scale lifter, helping to soften and remove psoriasis scales.
Strong salicylic acid preparations can cause irritation if left in contact with the skin for too long. The body may absorb too much salicylic acid if used over large areas of the skin. Salicylic acid may also weaken hair shafts and make them more likely to break, leading to temporary hair loss.
If the response to treatment with a potent corticosteroid for scalp psoriasis remains unsatisfactory after a further 4 weeks of treatment offer:
- A combined product containing calcipotriol monohydrate and betamethasone dipropionate applied once daily for up to 4 weeks or
- Vitamin D or a vitamin D analogue applied once daily (only in those who cannot use steroids and with mild to moderate scalp psoriasis).
If continuous treatment with either a combined product containing calcipotriol monohydrate and betamethasone dipropionatew applied once daily or vitamin D or a vitamin D analogue applied once daily for up to 8 weeksy does not result in clearance, near clearance or satisfactory control of scalp psoriasis offer:
- A very potent corticosteroid applied up to twice daily for 2 weeks for adults only or
- Coal tar applied once or twice daily or
- Referral to a specialist for additional support with topical applications and/or advice on other treatment options.
Consider topical vitamin D or a vitamin D analoguex, alone for the treatment of scalp psoriasis only in people who:
- Are intolerant of or cannot use topical corticosteroids at this site or
- Have mild to moderate scalp psoriasis.
To get maximum benefit from treatment for scalp psoriasis, follow these tips 3:
- Try not to scratch your scalp. Dermatologists realize that scalp psoriasis can be extremely itchy. Scratching, however, can make the psoriasis worse. Scratching can cause the scalp to bleed. It also can cause hair loss, which can become noticeable.
- Relieve the itch by treating the psoriasis. When the psoriasis clears, the itch will stop. If that’s too long to wait, tell your dermatologist that the itch is unbearable.
- Shampoo gently. Rubbing a shampoo into the scalp may seem best, but it’s not. Rubbing, scrubbing, and scratching your scalp tend to make scalp psoriasis worse.
- Remove scale with care. To treat scalp psoriasis, you need to loosen and remove the scale on your scalp. You must do this gently. Picking can cause psoriasis to flare. Picking also can cause hair loss.
- Dermatologists recommend using a scale softener. A scale softener that contains salicylic acid can soften the thick, stubborn patches of psoriasis. Softening these patches also allows medicine that you apply to the psoriasis to work better. When applying medicine to your scalp, be sure to lift your hair out of the way. This helps ensure that you apply the medicine to your scalp and not your hair.
- Try not to stress out. A psoriasis flare-up can be stressful. Feeling stressed, however, can make matters worse. Stress can worsen psoriasis. Stress can cause the hair on your head to fall out. Finding ways to unwind can do wonders.
Scalp psoriasis treatment options
Treatments are often combined and rotated because a person’s psoriasis may become less responsive to medications after repeated use. Systemic treatments are not commonly used just for scalp psoriasis but may be used if psoriasis is present elsewhere on the body and/or the psoriasis is moderate to severe.
Mild scalp psoriasis
Tar products and salicylic acid generally work for very mild scalp psoriasis.
There are many coal tar and non-coal tar medicated shampoos for treating scalp lesions on the market. Remember, medicated shampoos are designed for the scalp, not the hair.
Sometimes doctors inject scalp lesions with steroid medications. This is done only when the scalp psoriasis is mild and involves a few areas. Steroid injections are given sparingly because the medication can be absorbed into the system.
Moderate to severe scalp psoriasis
If you have a more severe case of scalp psoriasis, you may need to try different treatment plans before you find the one that works for you. If crusting of the scalp along with scaling occurs and/or the lymph nodes in your neck are enlarged, indicating a yeast infection, your doctor may prescribe antimicrobial treatment.
Common topical treatments for scalp psoriasis include:
- Anthralin: Anthralin comes in a cream and a scalp formulation that can be applied directly to the skin and scalp. While Anthralin used to be a common topical treatment for psoriasis, the availability of newer, easy-to-use topicals has caused a decline in its usage. Anthralin can be messy to use. It will cause brown stains if it comes into contact with unaffected skin. A stain in the center of a plaque may indicate that the psoriasis is clearing. Several weeks of use may be required to see results. It may cause skin irritation and can stain light-colored hair as well as unaffected skin, clothing and bedding. Stains on skin and hair will eventually fade and disappear. Anthralin may be combined with ultraviolet light B (UVB), PUVA (the light-sensitizing drug psoralen plus ultraviolet light A), Tazorac or topical steroids to improve the response. Ask your health care provider before initiating any such regimen.
- Dovonex: Dovonex (generic name calcipotriene) is a form of synthetic vitamin D3. It is not the same as the vitamin D found in dietary supplements taken by mouth, which should not be used to treat psoriasis. Dovonex is formulated to slow skin cell growth, flatten lesions and remove scale. It can also be used to treat psoriasis of the scalp and nails. Dovonex comes in a 0.005% cream or scalp solution. Health care providers usually recommend applying it twice per day. Dovonex can be used with many other treatments. Combining it with topical steroids can be more effective and less irritating than Dovonex alone; however, the specifics of the combination matter since some steroids, for example, may cause faster breakdown of Dovonex. If Dovonex is prescribed with other topicals, apply the medications at different times of day and never mix them unless they are known to be compatible. Dovonex has no known serious side effects when used according to guidelines. Changes in levels of calcium may occur with the use of topical Dovonex. If elevation of calcium levels is beyond a normal range, the treatment should be discontinued until the calcium levels are back to normal. The most common minor side effect is skin irritation, such as stinging or burning. Less common side effects include dry skin, peeling, rash, dermatitis and worsening of psoriasis.
- Taclonex: Taclonex is a combination of calcipotriene, a form of synthetic vitamin D3, and betamethasone dipropionate, a steroid. It slows skin cell growth, flattens lesions, removes scale and reduces itch and inflammation. It comes in an ointment and is applied once a day for no more than four weeks. Thereafter, follow your provider’s directions. Taclonex should be used on no more than 30 percent of the body’s surface at any time. The most common side effects are itching, rash, skin thinning and skin burning. Less common side effects include redness of the skin, folliculitis, skin irritation, worsening of psoriasis, change of skin color and swollen fine blood vessels at the application site.
- Tazorac: Tazorac (generic name tazarotene) is a vitamin A derivative and is also known as a topical retinoid. It is thought to slow skin cell growth. Tazorac comes in a gel and a cream that are available in either 0.05% or 0.1% strength. The gel is odorless and non-staining. The cream is in a moisturizing base which may make it more tolerable for people with sensitive or drier skin or for people who live in harsher climates. Tazorac can be applied to most parts of the body, including the face, hairline, scalp and nails. Tazorac may be combined with a mid- to high-potency topical steroid to more quickly clear plaques as well as reduce irritation, redness and itching. Combining Tazorac with phototherapy treatment has proven to be more effective for clearing psoriasis than either treatment alone. The most common side effects are skin irritation and dry skin. Tazorac may make your skin more susceptible to sunburn. Use sunscreen and wear protective clothing if skin treated with Tazorac will be exposed to the sun. It is normal for psoriasis plaques to become very red before clearing when using Tazorac. The redness is often intense in color, but it is generally not painful. If you experience discomfort, burning, itching or stinging, check with your health care provider.
- Tazorac is not recommended for use by pregnant women, women who may become pregnant or women who are breastfeeding. Women in their childbearing years should use reliable birth control during treatment. Tazorac has no effect on sperm, so it is safe for a woman to become pregnant while her partner is using the medication.
- Resistant skin or scalp patches may respond to local superficial intralesional injection of triamcinolone acetonide suspension diluted with saline to 2.5 or 5 mg/mL, depending on the size and severity of the lesion 4. Injections may cause local atrophy, which is usually reversible.
Common systemic medication treatments for psoriasis include:
- Methotrexate
- Oral retinoids
- Cyclosporine
- Biologics
- Ultraviolet light
Hair blocks ultraviolet (UV) light treatments from reaching the scalp. You can achieve better results with conventional UV units if you part your hair in many rows, if you have very thin hair or if you shave your head. Hand-held devices called UV combs are available to deliver a higher intensity of UV light. Natural sunlight may also help if the hair is very thin or your head is shaved.
Scalp itch
Itching is often a problem for those with scalp psoriasis. Over-the-counter tar shampoos and shampoos containing menthol can help reduce itching. Topical steroids and oral antihistamines are also effective for reducing scalp itch.
Managing itch of scalp psoriasis
The itch of psoriasis may have a bigger impact on quality of life than the visible effect of the disease.
Itch is present in between 70 and 90 percent of psoriasis patients, yet it is only in the last decade that it has been recognized as a common symptom of the scalp psoriasis disease.
Psoriatic itch is different than that of other skin disorders. Some people have described it as a burning, biting sensation. Others compare it to the feeling of being bitten by fire ants. Doctors were once taught that psoriatic patients couldn’t have both itch and pain, but scientists now know that itch and pain signals travel along different pathways in the spinal cord.
Treating psoriasis also can profoundly improve these symptoms and your ability to cope with psoriasis on a day-to-day basis.
Stress and itch
Stress is a common trigger for a psoriasis flare. Stress also can make itch worse. This makes managing stress a particularly important life skill for people with psoriasis. Consider the following ways some people with psoriasis and psoriatic arthritis are effectively reducing stress in their lives.
Get outside help. Consider taking a course in stress management or finding a therapist in your area who specializes in stress management. Connecting with others who know what you are going through can help, too. Connect with people living with psoriasis and psoriatic arthritis.
Meditation. Meditation has been described as a good way to clear the mind, slow down racing thoughts and relieve anxiety. You can give it try yourself: For 15 minutes, sit comfortably on the floor, with eyes closed or barely open and focus on your breathing. Read more about William Hayden, who credits meditation with relieving stress, improving his sleep and in time, improving his psoriasis.
Exercise. Exercise increases production of endorphins, chemicals that improve mood and energy. Exercise also has been shown to improve sleep and decrease anxiety. A large U.S. study showed that women who regularly participate in vigorous exercise are less likely to get psoriasis than less-active women. If you haven’t been active for awhile, get tips on starting, or resuming, an exercise program. In another study 5 involving 303 overweight or obese patients with moderate-to-severe chronic plaque psoriasis who did not achieve remission after 4 weeks of continuous systemic treatment were randomized to receive either a 20-week quantitative and qualitative dietary plan associated with physical exercise for weight loss. After a 20-week dietary intervention associated with increased physical exercise reduced psoriasis severity in systemically treated overweight or obese patients with active psoriasis 5.
Prescription treatments
Simply treating your psoriasis can help reduce itch. If your psoriasis is moderate or severe, or your itch is particularly bothersome, consider asking your doctor to put you on a more aggressive treatment.
Aspirin and noradrenergic and specific serotonergic (NaSSA) antidepressants also can relieve itch. Gabapentin, a drug more commonly used to treat neurological pain, can help, too.
There also are prescription treatments that specifically help with itch, such as:
- Antihistamines
- Phototherapy
- Steroids
- Topical treatments that contain capsaicin
- Topical anesthetics like Pramoxine
Home remedies for scalp psoriasis itch
The following are ways people with psoriasis help relieve itch:
- Keep skin moisturized. This is the first step in controlling itch because it reduces redness and itching and helps the skin heal. Dermatologists recommend heavy creams and ointments to lock water into the skin. Cooking oils and even shortening can be inexpensive substitutes for commercial moisturizers.
- Remove scale and flaking. Apply a scale softening (keratolytic) product to reduce excess skin and prevent psoriasis plaques from cracking and flaking. Over-the-counter lotions that contain ingredients like salicylic acid, lactic acid, urea or phenol can help remove scale. Removing scale can reduce itch and make itch-relieving lotions and ointments more effective.
- Cold showers and cold packs also can offer relief. Avoid hot baths and try to limit showers to 10 minutes or less. Hot water can make skin irritation and dryness worse. Apply lotion after washing to lock in moisture. Store lotions in the refrigerator. The feeling of a cool lotion on itchy skin can help.
- Over-the-counter treatments can help. There are several ingredients that have been approved by the U.S. Food and Drug Administration (FDA) for treating itch. Some of these include calamine, hydrocortisone (a weak steroid), camphor, diphenhydramine hydrochloride (HCl), benzocaine and menthol. Beware that these ingredients may increase irritation and dryness.
Scalp Psoriasis Home Remedies
There are other products which don’t contain salicylic acid or coal tar that are beneficial for treating psoriasis. Ingredients such as aloe vera, jojoba, zinc pyrithione, capsaicin and others, are frequently used to moisturize, soothe, remove scale or relieve itching.
The effectiveness of some of these products is not known. Be aware that “natural” ingredients can also cause side effects or allergic reactions. If irritation occurs, discontinue use.
- Scale lifters (keratolytics). Scale lifters help loosen and remove scale allowing medications to reach the psoriasis lesions. There are scale-lifting products designed for the scalp, body or both. Note that scalp products are usually stronger and may be too harsh for other skin sites. Over-the-counter (OTC) products that contain an active ingredient of salicylic acid, lactic acid, urea or phenol can be used as scale lifters.
- Expose your skin to small amounts of sunlight. A controlled amount of sunlight can improve psoriasis, but too much sun can trigger or worsen outbreaks and increase the risk of skin cancer. First ask your doctor about the best way to use natural sunlight to treat your skin. Log your time in the sun, and protect skin that isn’t affected by psoriasis with sunscreen.
- Avoid psoriasis triggers, if possible. Find out what triggers, if any, worsen your psoriasis and take steps to prevent or avoid them. Infections, injuries to your skin, stress, smoking and intense sun exposure can all worsen psoriasis.
- Avoid drinking alcohol. Alcohol consumption may decrease the effectiveness of some psoriasis treatments. If you have psoriasis, avoid alcohol. If you do drink, keep it moderate.
- About Psoriasis. National Psoriasis Foundation. https://www.psoriasis.org/about-psoriasis[↩]
- National Clinical Guideline Centre (UK). Psoriasis: Assessment and Management of Psoriasis. London: Royal College of Physicians (UK); 2012 Oct. (NICE Clinical Guidelines, No. 153.) 5, Guideline summary. Available from: https://www.ncbi.nlm.nih.gov/books/NBK327715/[↩]
- Scalp psoriasis. American Academy of Dermatology. https://www.aad.org/public/diseases/hair-and-scalp-problems/scalp-psoriasis#tips[↩]
- Psoriasis. Merck Manual. https://www.merckmanuals.com/professional/dermatologic-disorders/psoriasis-and-scaling-diseases/psoriasis[↩]
- Diet and physical exercise in psoriasis: a randomized controlled trial. Br J Dermatol. 2014 Mar;170(3):634-42. https://www.ncbi.nlm.nih.gov/pubmed/24641585/[↩][↩]