Contents
What is smallpox
Smallpox is a disease caused by the variola major virus (smallpox virus). Some experts say that over the centuries smallpox has killed more people than all other infectious diseases combined. Smallpox has existed for at least 3,000 years and was one of the world’s most feared diseases until it was eradicated by a collaborative global vaccination programme led by the World Health Organization. Thanks to the success of vaccination, the last natural outbreak of smallpox in the United States occurred in 1949. The last known natural case was in Somalia in 1977. Since then, the only known cases were caused by a laboratory accident in 1978 in Birmingham, England, which killed one person and caused a limited outbreak. In 1980 the World Health Assembly officially declared smallpox eradicated (eliminated), and no cases of naturally occurring smallpox have happened since.
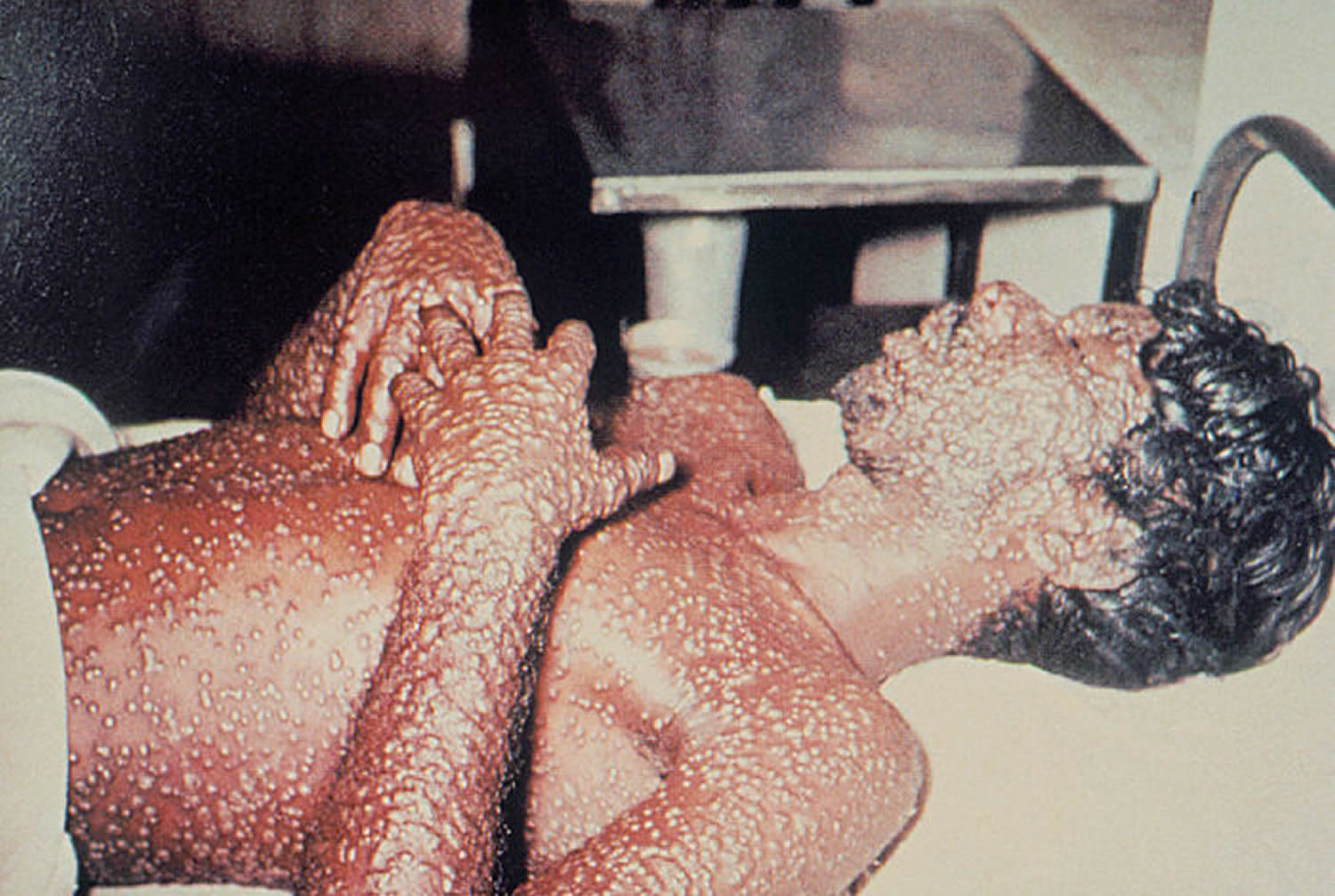
Early symptoms of smallpox include high fever and fatigue. The smallpox virus then produces a characteristic rash, particularly on the face, arms and legs. The resulting spots become filled with clear fluid and later, pus, and then form a crust, which eventually dries up and falls off. Smallpox was fatal in up to 30% of cases.
Smallpox spreads very easily from person to person. Symptoms are flu-like. They include:
- High fever
- Fatigue
- Headache
- Backache
- A rash with flat red sores
There is no treatment. Fluids and medicines for pain or fever can help control symptoms. Most people with smallpox recovered, but about 3 out of every 10 people with smallpox died. Many smallpox survivors have permanent scars over large areas of their body, especially their faces. Some are left blind.
The U.S. stopped routine smallpox vaccinations in 1972. Military and other high-risk groups continue to get the vaccine. The U.S. has increased its supply of the vaccine in recent years. The vaccine makes some people sick, so doctors save it for those at highest risk of disease.
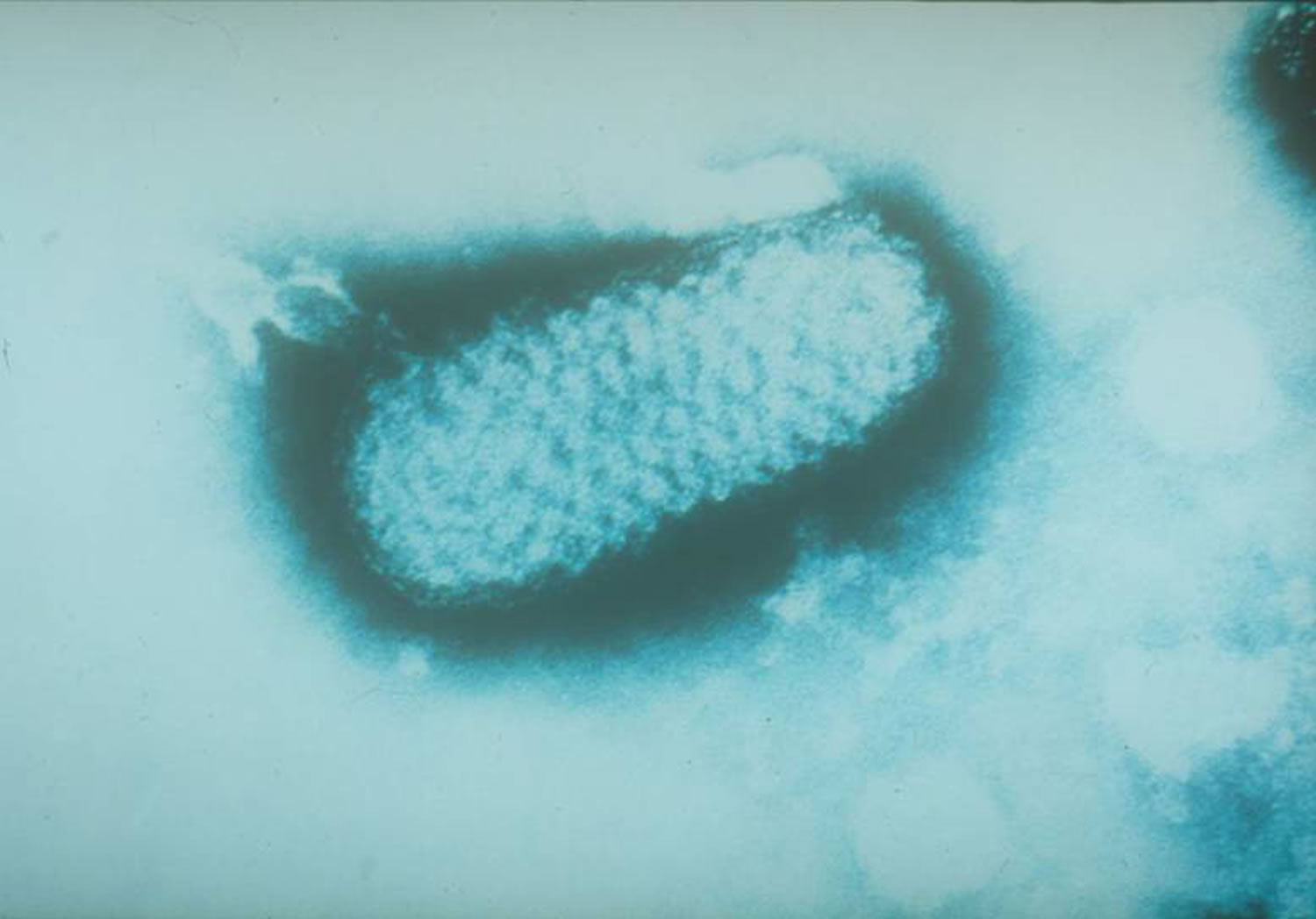
Figure 1. Smallpox virus
Figure 2. Smallpox rash
Smallpox history
The origin of smallpox is unknown. Smallpox is thought to date back to the Egyptian Empire around the 3rd century BC, based on a smallpox-like rash found on three mummies. The earliest written description of a disease that clearly resembles smallpox appeared in China in the 4th century AD. Early written descriptions also appeared in India in the 7th century and in Asia Minor in the 10th century.
Spread of Smallpox
The global spread of smallpox can be traced to the growth and spread of civilizations, exploration, and expanding trade routes over the centuries.
Historical Highlights:
- 6th Century – Increased trade with China and Korea introduces smallpox into Japan.
- 7th Century – Arab expansion spreads smallpox into northern Africa, Spain, and Portugal.
- 11th Century – Crusades further spread smallpox in Europe.
- 15th Century – Portuguese occupation introduces smallpox into part of western Africa.
- 16th Century – European colonization and the African slave trade import smallpox into the Caribbean and Central and South America.
- 17th Century – European colonization imports smallpox into North America.
- 18th Century – Exploration by Great Britain introduces smallpox into Australia.
Early Control Efforts
Smallpox was a devastating disease. On average, 3 out of every 10 people who got it died. Those who survived were usually left with scars, which were sometimes severe.
One of the first methods for controlling the spread of smallpox was the use of variolation. Named after the virus that causes smallpox (variola virus), variolation is the process by which material from smallpox sores (pustules) was given to people who had never had smallpox. This was done either by scratching the material into the arm or inhaling it through the nose. With both types of variolation, people usually went on to develop the symptoms associated with smallpox, such as fever and a rash. However, fewer people died from variolation than if they had acquired smallpox naturally.
The basis for vaccination began in 1796 when an English doctor named Edward Jenner observed that milkmaids who had gotten cowpox did not show any symptoms of smallpox after variolation. The first experiment to test this theory involved milkmaid Sarah Nelmes and James Phipps, the 9 year-old son of Jenner’s gardener. Dr. Jenner took material from a cowpox sore on Nelmes’ hand and inoculated it into Phipps’ arm. Months later, Jenner exposed Phipps a number of times to variola virus, but Phipps never developed smallpox. More experiments followed, and, in 1801, Jenner published his treatise “On the Origin of the Vaccine Inoculation,” in which he summarized his discoveries and expressed hope that “the annihilation of the smallpox, the most dreadful scourge of the human species, must be the final result of this practice.”
Vaccination became widely accepted and gradually replaced the practice of variolation. At some point in the 1800s (the precise time remains unclear), the virus used to make the smallpox vaccine changed from cowpox to vaccinia virus.
Smallpox eradication
In 1959, the World Health Organization (WHO) initiated a plan to rid the world of smallpox. Unfortunately, this global eradication campaign suffered from lack of funds, personnel, and commitment from countries, as well as a shortage of vaccine donations. Despite their best efforts, smallpox was still widespread in 1966, causing regular outbreaks in multiple countries across South America, Africa, and Asia.
The Intensified Eradication Program began in 1967 with a promise of renewed efforts. This time, laboratories in many countries where smallpox occurred regularly (endemic countries) were able to produce more, higher quality freeze-dried vaccine. A number of other factors also played an important role in the success of the intensified efforts, including the development of the bifurcated needle, establishment of a surveillance system to detect and investigate cases, and mass vaccination campaigns, to name a few.
By the time the Intensified Eradication Program began in 1967, smallpox had already been eliminated in North America (1952) and Europe (1953), leaving South America, Asia, and Africa (smallpox was never widespread in Australia). The Program made steady progress toward ridding the world of this disease, and by 1971 smallpox was eradicated from South America, followed by Asia (1975), and finally Africa (1977).
World Free of Smallpox
Almost two centuries after Jenner published his hope that vaccination could annihilate smallpox, on May 8, 1980, the 33rd World Health Assembly officially declared the world free of this disease. Eradication of smallpox is considered the biggest achievement in international public health.
Smallpox vs chickenpox
Chickenpox is caused by the varicella zoster virus. It can be spread either through close person-to-person contact, or through sneezing and coughing just like a cold or flu. Later in the illness, the virus is spread by direct contact with the fluid in the blisters. Chickenpox infection triggers an immune response and people rarely get chickenpox twice.
Chickenpox is infectious from 2 days before the spots appear to until they’ve crusted over, usually 5 days after they first appeared. It takes 1 to 3 weeks from the time you were exposed to chickenpox for the spots to start appearing.
Chickenpox is usually a mild and common childhood illness that can also occur at any stage of life. The illness can be associated with severe complications and even death so must be treated seriously in all cases.
Immunisation can help prevent the spread of chickenpox.
Chickenpox causes a rash of red, itchy spots that turn into fluid-filled blisters. They then crust over to form scabs, which eventually drop off.
Your child is likely to have a fever at least for the first few days of the illness and the spots can be incredibly itchy, so expect them to feel pretty miserable and irritable while they have chickenpox.
Some children have only a few spots, but in others they can cover the entire body.
The spots are most likely to appear on the face, ears and scalp, under the arms, on the chest and belly and on the arms and legs.
The incubation period for chickenpox is between one and three weeks. The most infectious time is between one and two days before the rash appears, but it continues to be infectious until all the blisters have crusted over.
Chickenpox can be severe at any age and have serious complications. Complications include:
- bacterial skin infections
- pneumonia
- swelling of the membranes covering the brain (aseptic meningitis)
- decrease in blood platelet cell (thrombocytopenia)
- may have a short term effect on movement (acute cerebellar ataxia)
- fetal abnormalities in pregnant women
- encephalitis (inflammation of the brain).
Pregnant women should be especially careful to avoid chickenpox as it can affect the unborn baby by causing foetal malformations, skin scarring and other serious problems (congenital varicella syndrome).
There is no specific treatment for chickenpox, but there are medicines and pharmacy products which can help alleviate symptoms, such as:
- acetaminophen to relieve fever
- calamine lotion and cooling gels to ease itching.
In most children, the blisters crust up and fall off naturally within one to two weeks.
Adults who have had chickenpox as a child may also get shingles later in life, as they are both caused by the virus varicella zoster.
What causes smallpox
Smallpox is caused by infection with the variola virus. Variola virus is a member of the orthopoxvirus genus, which also includes viruses that cause cowpox, monkeypox, orf, and molluscum contagiosum. Poxviruses are the largest animal viruses, visible with a light microscope. They are larger than some bacteria and contain double-stranded DNA.
Poxviruses are the only viruses that do not need a cell’s nucleus to replicate inside the cell. The variola virus is the only known cause of smallpox. The disease affects only humans. No animal reservoirs or insect vectors (insects that spread a disease) exist, and no carrier state (period when the virus is in the body, but the person is not actively sick) occurs. Before smallpox was wiped out, the disease survived through continual person-to-person transmission. Pregnant women and children had a heightened risk for the illness. Smallpox also affected them more severely than normal. The virus is only transmitted from human to human; there are no known animal infections.
The virus is acquired from inhalation (breathing into the lungs). Virus particles can remain on such items as clothing, bedding, and surfaces for up to one week.
The virus starts in the lungs. From there, the virus invades the bloodstream and spreads to the skin, intestines, lungs, kidneys, and brain. The virus activity in the skin cells creates a rash that starts as macules (flat, red lesions). After this, vesicles (raised blisters) form. Then, pustules (pus-filled pimples) appear about 12-17 days after a person becomes infected. Survivors of smallpox often have severely deformed skin from the pustules.
- Types: Variola major, or smallpox, has a death rate of 30%. Variola minor, or alastrim, is a milder form of the virus with a death rate of 1%. Four types of variola exist: classic, hemorrhagic, malignant, and modified.
- Classic smallpox is believed to be the most communicable disease; about a third of unvaccinated people who come in contact with it become infected.
- The hemorrhagic variety of variola has a much higher death rate than classic smallpox and leads to death more quickly. Infected people often die before the pustules form. This variety is recognizable by certain types of bleeding sores in mucous tissues. Pregnant women are more likely to contract this version.
- Prior to eradication, the malignant or flat form of smallpox affected 6% of the population and evolved more slowly than the classic type. Lesions were flat, often described as feeling velvety. The death rate for this form approaches 100%.
- The modified variety of smallpox essentially affects people who have been vaccinated and still have some immune response to the vaccine. In a vaccinated population, this version could affect about 15%.
The virus can be transmitted:
- Directly from person to person. Smallpox is highly contagious and mainly spreads from person to person by inhalation. Direct transmission of the virus requires fairly prolonged face-to-face contact. The virus can be transmitted through the air by droplets that escape when an infected person coughs, sneezes or talks. However, infectious smallpox virus particles can remain viable on surfaces, clothing, and bedding for up to one week.
- Indirectly from an infected person. In rare instances, airborne virus can spread farther, possibly through the ventilation system in a building, infecting people in other rooms or on other floors.
- Via contaminated items. Smallpox can also spread through contact with contaminated clothing and bedding, although the risk of infection from these sources is less common.
- As a terrorist weapon, potentially. A deliberate release of smallpox is a remote threat. However, because any release of the virus could spread the disease quickly, government officials have taken numerous precautions to protect against this possibility, such as stockpiling smallpox vaccine.
Before smallpox was eradicated, it was mainly spread by direct and fairly prolonged face-to-face contact between people. Smallpox patients became contagious once the first sores appeared in their mouth and throat (early rash stage). They spread the virus when they coughed or sneezed and droplets from their nose or mouth spread to other people. They remained contagious until their last smallpox scab fell off.
These scabs and the fluid found in the patient’s sores also contained the variola virus. The virus can spread through these materials or through the objects contaminated by them, such as bedding or clothing. People who cared for smallpox patients and washed their bedding or clothing had to wear gloves and take care to not get infected.
Rarely, smallpox has spread through the air in enclosed settings, such as a building (airborne route).
Smallpox can be spread by humans only. Scientists have no evidence that smallpox can be spread by insects or animals.
Smallpox vaccine
The smallpox vaccine protects people from smallpox by helping their bodies develop immunity to smallpox. The vaccine is made from a virus called vaccinia, which is a poxvirus similar to smallpox, but less harmful. The smallpox vaccine contains live vaccinia virus, not a killed or weakened virus like many other vaccines. For that reason, people who are vaccinated must take precautions when caring for the place on their arm where they were vaccinated, so they can prevent the vaccinia virus from spreading.
- The vaccine does not contain the smallpox virus and cannot give you smallpox.
For most people with healthy immune systems, live virus vaccines are effective and safe. Sometimes a person getting a live virus vaccine experiences mild symptoms such as rash, fever, and head and body aches. In certain groups of people, complications from the vaccinia virus can be severe.
Smallpox vaccination can protect you from smallpox for about 3 to 5 years. After that time, its ability to protect you decreases. If you need long-term protection, you may need to get a booster vaccination.
Historically, the vaccine has been effective in preventing smallpox infection in 95% of those vaccinated. In addition, the vaccine was proven to prevent or substantially lessen infection when given within a few days after a person was exposed to the variola virus.
If you get the smallpox vaccine:
- Before contact with the virus, the vaccine can protect you from getting sick.
- Within 3 days of being exposed to the virus, the vaccine might protect you from getting the disease. If you still get the disease, you might get much less sick than an unvaccinated person would.
- Within 4 to 7 days of being exposed to the virus, the vaccine likely gives you some protection from the disease. If you still get the disease, you might not get as sick as an unvaccinated person would.
Once you have developed the smallpox rash, the vaccine will not protect you.
Currently, the smallpox vaccine is not available to the general public because smallpox has been eradicated, and the virus no longer exists in nature. However, there is enough smallpox vaccine to vaccinate every person in the United States if a smallpox outbreak were to occur.
Smallpox vaccination side effects
For most people, the smallpox vaccination is safe and effective. Most people experience normal, typically mild reactions to the vaccine, which indicates that the vaccine is beginning to work. Some people may experience reactions requiring medical attention.
Normal, Typically Mild Reactions
You may experience these reactions, which usually go away without treatment:
- Your arm where you received the vaccination may be sore and red.
- The glands (lymph nodes) in your armpits may become large and sore.
- You may run a slight fever.
- You might feel bad enough to miss work, school, or recreational activity or have trouble sleeping. This happens to about 1 out of every 3 people who get the vaccine.
Serious Reactions
In the past, for every 1,000 people vaccinated, 1 person experienced a serious but not life-threatening reactions. These reactions may require medical attention:
- Spreading the vaccinia virus by touching the vaccination site and then touching another part of the body or another person. It usually occurs on the genitals or face, including the eyes, where it can damage sight. You can prevent this by washing your hands with soap and water after touching the vaccine site and by following the instructions for caring for the vaccine site.
- A toxic or allergic rash that can take various forms.
Life-Threatening Reactions
Rarely, people have had very bad reactions to the vaccine. In the past, between 14 and 52 people out of every 1 million people vaccinated for the first time experienced potentially life-threatening reactions. These reactions require immediate medical attention:
- Serious rash caused by widespread infection of the skin (known as eczema vaccinatum). This happened in people with pre-existing skin conditions such as eczema or atopic dermatitis. Many people who got this complication were not vaccinated, but got infected with the virus from the vaccine site of their family member or friend who received vaccination. To help reduce the risk for your loved ones, be sure to follow the instructions for caring for the vaccine site.
- Buildup of inflamed tissue around the vaccination site that may at first look like a bullseye and will grow into a large, non-healing sore (known as progressive vaccinia). This usually happened to people with a deficient immune system.
- Inflammation of the brain (known as postvaccinal encephalitis).
People with certain medical conditions—including people with weakened immune systems or certain skin conditions—are more likely to have these reactions and should not get the smallpox vaccine unless they have been exposed to smallpox.
Other serious side effects
A few people who have gotten the smallpox vaccine have developed heart inflammation (myocarditis), inflammation of the lining of the heart (pericarditis), or a combination of both (myopericarditis).
Other people have experienced heart pain (angina) and heart attack after getting the smallpox vaccination. However, it is not known if the smallpox vaccination caused these problems or if they occurred by chance alone.
If you have chest pain, shortness of breath, or other symptoms of heart disease after getting the smallpox vaccination, you should seek medical attention.
Smallpox vaccine safety
The smallpox vaccine is the best protection you can get if you are exposed to the smallpox virus. Anyone directly exposed to smallpox, regardless of how healthy they are, would be offered the smallpox vaccine because the risks associated with smallpox disease are far greater than those posed by the vaccine.
There are side effects and risks related to the smallpox vaccine. Most people have normal, usually mild reactions such as a sore arm, fever, and body aches. However, some people may have reactions ranging from serious to life-threatening.
You are more likely to have serious side effects if:
- You currently have or have ever had certain chronic skin conditions, even if it was only once (especially eczema or atopic dermatitis.)
- You have active breaks in the skin at the time of vaccination, like poison ivy or acne.
- You have a weakened immune system. You may have a weakened immune system if you:
- Have had a transplant.
- Are HIV-positive.
- Have cancer or are being treated for cancer.
- Are taking medications that suppress your immune system, like steroids.
Who should get smallpox vaccination
After smallpox was eliminated from the world, routine vaccination against smallpox among the general public was stopped because it was no longer needed. However, because of concern that variola virus might be used as an agent of bioterrorism, the U.S. government has stockpiled enough smallpox vaccine to vaccinate everyone who would need it if a smallpox outbreak were to occur.
When there is NO smallpox outbreak, you should get the smallpox vaccine if you:
- Are a lab worker who works with virus that causes smallpox or other viruses that are similar to it.
If you need long-term protection, you may need to get booster vaccinations regularly. To stay protected from smallpox, you should get booster vaccinations every 3 years.
When there IS a smallpox outbreak, you should get the smallpox vaccine if you:
- Are directly exposed to smallpox virus. For example, if you had a prolonged face-to-face contact with someone who has smallpox.
If there is a smallpox outbreak, public health officials will say who else should get the vaccine. CDC works with federal, state, and local officials to prepare for a smallpox outbreak.
Getting the Smallpox Vaccine
The smallpox vaccine is given by a special technique. It is not administered as a “shot” in the way that most other vaccines are. It is given using a two-pronged (bifurcated) needle that is dipped into the vaccine solution. When removed, the needle holds a droplet of the vaccine. The needle is used to prick the skin a number of times in a few seconds. The pricking is not deep, but it will cause a sore spot and one or two drops of blood to form. The vaccine usually is given in the upper arm.
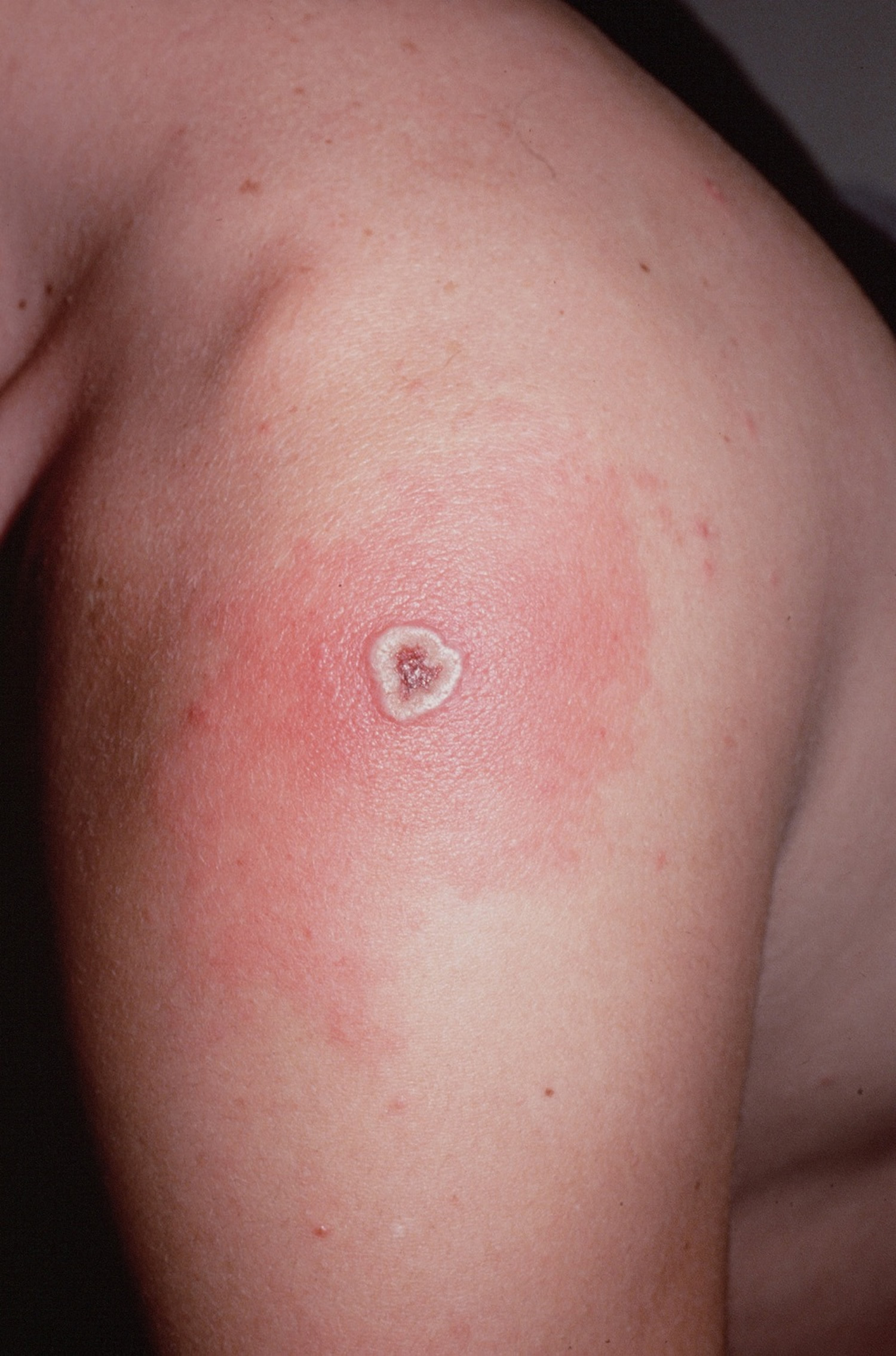
If the vaccination is successful, a red and itchy lesion develops at the vaccine site in 3 to 4 days. In the first week, the lesion becomes a large blister, fills with pus, and begins to drain. During the second week, the lesion begins to dry and a scab forms. The scab falls off in the third week, leaving a small scar.
People who are being vaccinated for the first time have a stronger reaction than those who are being revaccinated. The following pictures show the progression of the site where the vaccine is given in someone who has not gotten the vaccine before.
Figure 3. Smallpox vaccine scar
Caring for the smallpox vaccine site
Because the vaccinia virus is live, it is important to follow care instructions for the vaccination site. You can spread the vaccinia virus by touching the vaccination site before it has healed or by touching bandages or clothing that have been in contact with the live virus from the vaccination site.
After you are vaccinated, you must:
- Cover the vaccination site loosely with a piece of gauze held in place with first aid tape or a semi-permeable bandage (one that allows air to flow through, but not fluids).
- Wear a shirt with sleeves that cover the bandage.
- Keep the vaccination site dry.
- If the gauze bandage gets wet, change it right away.
- While bathing, cover your vaccination site with a waterproof bandage, and don’t share towels.
- Change your bandage at least every 3 days. Change it sooner if it gets dirty or wet.
- Wash your hands carefully every time after you touch the vaccination site or anything that might be contaminated with the virus from the vaccination site.
- Try not to touch your vaccination site. Do not let others touch the site or items that have touched it such as bandages, clothes, sheets, or towels.
- Do your own laundry. Use a separate laundry hamper for clothes, towels, sheets, and other items that may come into contact with your vaccination site or
- pus from the site. Machine wash items that have touched the vaccination site in hot water with detergent and/or bleach.
- Put used bandages in plastic zip bags, then throw them away in the regular trash.
- After the scab falls off, put it in a plastic zip bag and throw it away.
If you do not follow these instructions, you can spread the virus to other parts of your body or to other people.
Smallpox prevention
In the event of an outbreak, people who had smallpox would be kept in isolation in an effort to control the spread of the virus. Anyone who had contact with someone who developed an infection would need the smallpox vaccine, which can prevent or lessen the severity of the disease if given within four days of exposure to the smallpox virus.
The vaccine uses a live virus that’s related to smallpox, and it can occasionally cause serious complications, such as infections affecting the heart or brain. That’s why a general vaccination program for everyone isn’t recommended at this time. The potential risks of the vaccine outweigh the benefits, in the absence of an actual smallpox outbreak.
Lab tests suggest certain antiviral drugs may be effective against the virus that causes smallpox. These drugs have not been tested in people who are sick with smallpox, however, so it’s not known if these drugs are effective treatment options.
If you were vaccinated as a child
Immunity or partial immunity after a smallpox vaccine may last up to 10 years, and 20 years with revaccination. If an outbreak ever occurred, people who were vaccinated as children would still likely receive a new vaccination after direct exposure to someone with the virus.
Smallpox symptoms
A person with smallpox goes through several stages as the disease progresses. Each stage has its own signs and symptoms.
Incubation Period
This stage can last anywhere from 7 to 19 days (although the average length is 10 to 14 days).
Contagious? No
The incubation period is the length of time the virus is in a person’s body before they look or feel sick. During this period, a person usually has no symptoms and may feel fine.
Initial Symptoms
The first stage of disease in smallpox is a severe febrile prodrome, which is a critical feature of the disease. This stage lasts anywhere from 2 to 4 days.
Contagious? Sometimes. Smallpox may be contagious during this phase, but is most contagious during the next 2 stages (early rash and pustular rash and scabs).
The first symptoms include:
- High fever 102.2 -107.6 °F to (39ºC to 41ºC)
- Head and body aches
- Sometimes vomiting
At this time, people are usually too sick to carry on their normal activities.
Early Rash
This stage lasts about 4 days.
Contagious? Yes. At this time, the person is most contagious.
A rash starts as small red spots on the tongue and in the mouth. These spots change into sores that break open and spread large amounts of the virus into the mouth and throat. The person continues to have a fever.
Once the sores in the mouth start breaking down, a rash appears on the skin, starting on the face and spreading to the arms and legs, and then to the hands and feet. Usually, it spreads to all parts of the body within 24 hours. As this rash appears, the fever begins to decline, and the person may start to feel better.
By the fourth day, the skin sores fill with a thick, opaque fluid and often have a dent in the center.
Once the skin sores fill with fluid, the fever may rise again and remain high until scabs form over the bumps.
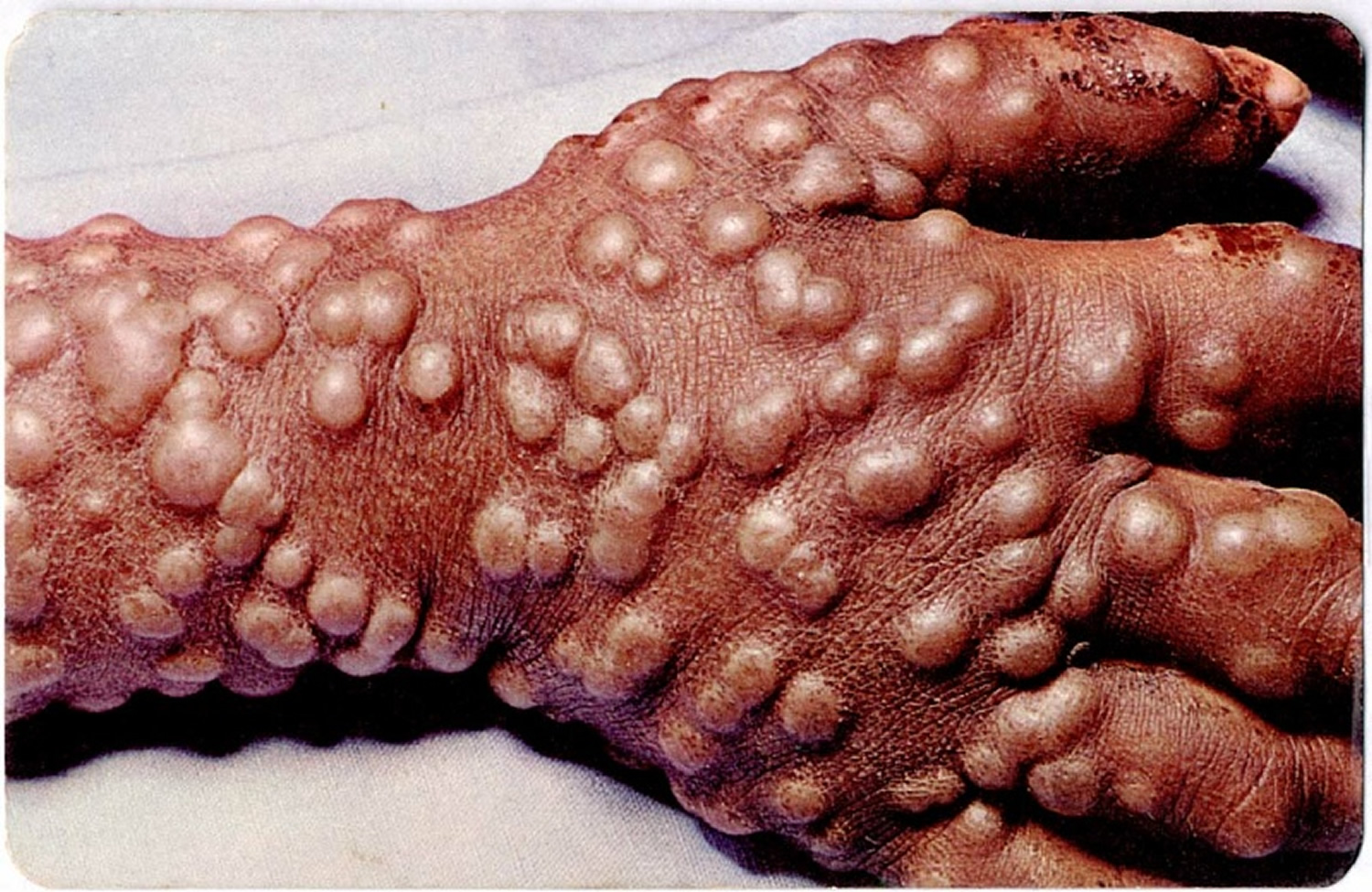
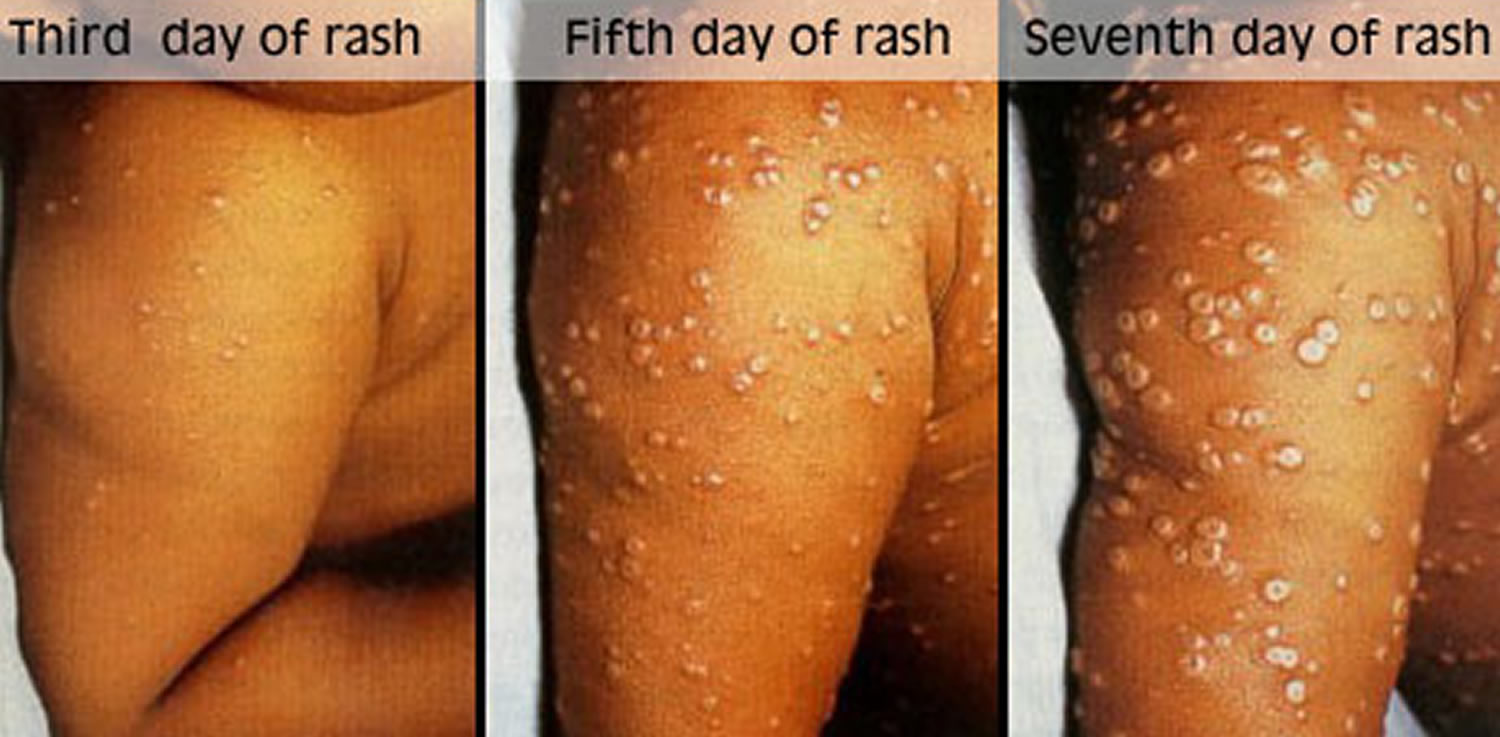
Figure 4. Smallpox rash
Figure 5. Smallpox rash
Pustular Rash and Scabs
By day 6 of the rash, the sores become pustules.
This stage lasts about 10 days.
Contagious? Yes
The sores become pustules (sharply raised, usually round and firm to the touch, like peas under the skin).
After about 5 days, the pustules begin to form a crust and then scab.
By the end of the second week after the rash appears, most of the sores have scabbed over.
Scabs Fall Off
This stage lasts about 6 days.
Contagious? Yes
The scabs begin to fall off, leaving marks on the skin.
Three weeks after the rash appears, most scabs will have fallen off.
No Scabs
Contagious? No.
Four weeks after the rash appears, all scabs should have fallen off. Once all scabs have fallen off, the person is no longer contagious.
Smallpox diagnosis
If an outbreak of smallpox were to occur today, it’s likely that most doctors wouldn’t realize what it was in its early stages, which would allow the disease to spread.
Even one confirmed case of smallpox would be considered an international health emergency.
Major Diagnostic Criteria for Smallpox
- Febrile prodrome occurring 1 to 4 days before rash onset:
- Fever ≥101°F (38.3°C) AND at least one of the following:
- prostration
- headache
- backache
- chills
- vomiting
- severe abdominal pain
- Fever ≥101°F (38.3°C) AND at least one of the following:
- Classic smallpox lesions: deep-seated, firm/hard, round, well-circumscribed vesicles or pustules. As they evolve, lesions may become umbilicated or confluent.
- Lesions in the same stage of development (e.g., all are vesicles or all are pustules) on any ONE part of the body (e.g., the face, arms).
Minor Diagnostic Criteria for Smallpox
- Centrifugal distribution of rash: greatest concentration of lesions on face and distal extremities
- First lesions on the oral mucosa/palate, face, or forearms
- Severity: Patient appears toxic or moribund
- Slow rash evolution: lesions evolved from macules to papules to pustules over days (each stage lasts 1 to 2 days)
- Lesions on the palms and/or soles
Laboratory Confirmation
For patients with a high risk of having smallpox, the state health department will contact CDC to conduct laboratory testing to confirm or rule out smallpox. In the absence of known smallpox disease, the predictive value of a positive smallpox test diagnosis is low, so only cases that meet the clinical definition of the disease should be tested.
Laboratory Case Definition
Laboratory diagnostic testing for variola virus will occur in a CDC Laboratory Response Network (LRN) laboratory using LRN-approved PCR tests and protocols for variola virus. Initial positive results require confirmatory testing at CDC.
The laboratory criteria for diagnosis are:
- Polymerase chain reaction (PCR) identification of variola DNA in a clinical specimen, OR
- Isolation of smallpox (variola) virus from a clinical specimen (WHO Smallpox Reference Laboratory or laboratory with appropriate reference capabilities) with variola PCR confirmation.
Note: Generic orthopoxvirus PCR and negative stain electron microscopy identification of a poxvirus in a clinical specimen are suggestive of an orthopoxvirus infection but not diagnostic for smallpox.
Smallpox treatment
There is no proven treatment for smallpox disease, but some antiviral drugs may help treat it or prevent it from getting worse.
- In laboratory tests, Tecovirimat has been shown to be effective against the virus that causes smallpox. In laboratory settings this drug was effective in treating animals which had diseases similar to smallpox. Tecovirimat has not been tested in people who are sick with smallpox, but it has been given to healthy people. Test results showed that it is safe and causes only minor side effects.
- In laboratory tests, Cidofovir and Brincidofovir have been shown to be effective against the virus that causes smallpox. In laboratory settings this drug was effective in treating animals which had diseases similar to smallpox. Cidofovir and Brincidofovir have not been tested in people who are sick with smallpox, but they have been tested in healthy people and in those with other viral illnesses. Test results indicate that Brincidofovir may cause fewer side effects than Cidofovir, which can be toxic to kidneys.
- Because these drugs were not tested in people sick with smallpox, it is not known if a person with smallpox would benefit from treatment with them. However, their use may be considered if there ever is an outbreak of smallpox.
- Tecovirimat and Cidofovir are currently stockpiled by CDC’s Strategic National Stockpile, which has medicine and medical supplies to protect the American public if there is a public health emergency, including one involving smallpox.