Contents
- What is soft tissue sarcoma
What is soft tissue sarcoma
Soft tissue sarcomas are a group of cancers that develop from cells of connective tissue. These include cells that make up our muscles, tendons, nerves, fibrous tissues, fat, deep skin tissues, lining of joints and blood vessels. Soft tissue sarcomas can therefore develop almost anywhere in the body. Most of them develop in the arms or legs. Soft tissue sarcomas can also be found in the trunk, head and neck area, internal organs, and the area in back of the abdominal cavity (known as the retroperitoneum). Sarcomas are not common tumors, and most cancers are the type of tumors called carcinomas.
There are many kinds, based on the type of tissue they started in. Soft tissue sarcomas may cause a lump or swelling in the soft tissue. Sometimes soft tissue sarcomas spread and can press on nerves and organs, causing problems such as pain or trouble breathing.
The American Cancer Society’s estimates for soft tissue sarcomas in the United States for 2018 are (these statistics include both adults and children):
- About 13,040 new soft tissue sarcomas will be diagnosed (7,370 cases in males and 5,670 cases in females).
- 5,150 Americans (2,770 males and 2,380 females) are expected to die of soft tissue sarcomas.
The most common types of sarcoma in adults are undifferentiated pleomorphic sarcoma (previously called malignant fibrous histiocytoma), liposarcoma, and leiomyosarcoma. Certain types occur more often in certain areas of the body than others. For example, leiomyosarcomas are the most common abdominal sarcoma, while liposarcomas and undifferentiated pleomorphic sarcoma are most common in legs. But pathologists (doctors who specialize in diagnosing cancers by how they look under the microscope), may not always agree on the exact type of sarcoma. Sarcomas of uncertain type are very common.
The most common type of soft tissue sarcoma in children is called a rhabdomyosarcoma, which forms from early cell types (called rhabdomyoblasts) that make up skeletal muscles. Rhabdomyosarcomas are more common in younger children (under 10 years of age), although they can also develop in teenagers and adults.
There are many types of soft tissue tumors, and not all of them are cancerous. When the term sarcoma is part of the name of a disease, it means the tumor is malignant (cancer).
There more than 50 different types of soft tissue sarcomas (not all are listed here), such as:
- Adult fibrosarcoma
- Alveolar soft-part sarcoma
- Angiosarcoma (includes hemangiosarcoma and lymphangiosarcoma)
- Clear cell sarcoma
- Desmoplastic small round cell tumor
- Epithelioid sarcoma
- Fibromyxoid sarcoma, low-grade
- Gastrointestinal stromal tumor (GIST): This is a type of sarcoma that develops in the digestive tract. It is covered in Gastrointestinal Stromal Tumor (GIST).
- Kaposi sarcoma: This is a type of sarcoma that develops from the cells lining lymph or blood vessels. It is covered in Kaposi Sarcoma.
- Liposarcoma, which forms in fat (includes dedifferentiated, myxoid, and pleomorphic liposarcomas)
- Leiomyosarcoma, which forms in smooth muscle
- Malignant mesenchymoma
- Malignant peripheral nerve sheath tumors (includes neurofibrosarcomas, neurogenic sarcomas, and malignant schwannomas)
- Myxofibrosarcoma, low-grade
- Rhabdomyosarcoma: This is the most common type of soft tissue sarcoma seen in children and is discussed in Rhabdomyosarcoma.
- Synovial sarcoma, which can form near a joint such as the elbow or knee, or in other places in the body
- Undifferentiated pleomorphic sarcoma (previously known as malignant fibrous histiocytoma).
There are many other types of tumors called soft tissue sarcomas, but these are all quite rare.
Some soft tissue tumors behave in ways between a cancer and a non-cancer. These are called intermediate soft tissue tumors.
Intermediate soft tissue tumors include:
- Dermatofibrosarcoma protuberans
- Fibromatosis (also known as desmoid tumor, musculoaponeurotic fibromatosis, and aggressive fibromatosis
- Hemangioendothelioma
- Infantile fibrosarcoma
- Solitary fibrous tumor
No one knows exactly what causes these cancers. Soft tissue sarcomas are not common, but you have a higher risk if you have been exposed to certain chemicals, have had radiation therapy, or have certain genetic diseases.
Doctors diagnose soft tissue sarcomas with a biopsy. Treatments include surgery to remove the tumor, radiation therapy, chemotherapy, or a combination.
Types of soft tissue sarcomas
- Adult fibrosarcoma usually affects fibrous tissue in the legs, arms, or trunk. It is most common in people between the ages of 20 and 60, but can occur in people of any age, even in infants.
- Alveolar soft-part sarcoma is a rare cancer that mostly affects young adults. These tumors most commonly occur in legs.
- Angiosarcoma can develop either from blood vessels (hemangiosarcomas) or from lymph vessels (lymphangiosarcomas). These tumors sometimes start in a part of the body that has been treated with radiation. Angiosarcomas are sometimes seen in the breast after radiation therapy and in limbs with lymphedema.
- Clear cell sarcoma is a rare cancer that often develops in tendons of the arms or legs. Under the microscope, it has some features of malignant melanoma, a type of cancer that develops from pigment-producing skin cells. How cancers with these features start in parts of the body other than the skin is not known.
- Desmoplastic small round cell tumor is a rare sarcoma of adolescents and young adults, found most often in the abdomen.
- Epithelioid sarcoma most often develops in tissues under the skin of the hands, forearms, feet, or lower legs. Adolescents and young adults are often affected.
- Fibromyxoid sarcoma, low-grade is a slow growing cancer that most often develops as a painless growth in the trunk or arms and legs (particularly the thigh). It is more common in young to middle aged adults. It is also sometimes called an Evans’ tumor.
- Liposarcomas are malignant tumors of fat tissue. They can develop anywhere in the body, but they most often develop in the thigh, behind the knee, and inside the back of the abdomen. They occur mostly in adults between 50 and 65 years old.
- Malignant mesenchymoma is a rare type of sarcoma that shows features of fibrosarcoma and features of at least 2 other types of sarcoma.
- Malignant peripheral nerve sheath tumors include neurofibrosarcomas, malignant schwannomas, and neurogenic sarcomas. These are sarcomas that develop from the cells that surround a nerve.
- Myxofibrosarcomas, low-grade are most often found in the arms and legs of elderly patients. They are most common in or just under the skin and there might be more than one tumor nodule.
- Synovial sarcoma is a malignant tumor of the tissue around joints. The most common locations are the hip, knee, ankle, and shoulder. This tumor is more common in children and young adults, but it can occur in older people.
- Undifferentiated pleomorphic sarcoma, previously known as malignant fibrous histiocytoma, is most often found in the arms or legs. Less often, it can start inside at the back of the abdomen (the retroperitoneum). This sarcoma is most common in older adults. Although it mostly tends to grow locally, it can spread to distant sites.
Intermediate soft tissue tumors
- Dermatofibrosarcoma protuberans is a slow-growing cancer of the fibrous tissue beneath the skin, usually in the trunk or limbs. It grows into nearby tissues but rarely spreads to distant sites.
- Fibromatosis is the name given to fibrous tissue tumor with features in between fibrosarcoma and benign tumors such as fibromas and superficial fibromatosis. They tend to grow slowly but, often, steadily. They are also called desmoid tumors, as well as the more scientific name musculoaponeurotic fibromatosis or just aggressive fibromatosis. They rarely, if ever, spread to distant sites, but they do cause problems by growing into nearby tissues. They can sometimes be fatal. Some doctors consider them a type of low-grade fibrosarcoma; but others believe they are a unique type of fibrous tissue tumors. Certain hormones, particularly estrogen, make some desmoid tumors grow. Anti-estrogen drugs are sometimes useful in treating desmoids that cannot be completely removed by surgery.
- Hemangioendothelioma is a blood vessel tumor that is considered a low-grade cancer (meaning it grows slowly and is slow to spread). It does grow into nearby tissues and sometimes can spread to distant parts of the body (metastasize). It may start in soft tissues or in internal organs, such as the liver or lungs.
- Infantile fibrosarcoma is the most common soft tissue sarcoma in children under one year of age. It tends to be slow-growing and is less likely to spread to other organs than adult fibrosarcomas.
- Solitary fibrous tumors are most often not cancerous (benign) but can be malignant. Some start in the thigh, underarm, and pelvis. They can also start in the tissue surrounding the lung (called the pleura). Many tumors that were once called hemangiopericytomas are now considered solitary fibrous tumors.
Spindle cell tumors
Spindle cell tumor and spindle cell sarcoma are descriptive names based on the long, narrow appearance of the cells under the microscope. Spindle cell tumor is not a specific diagnosis or a specific type of cancer. The tumor may be a sarcoma, or it can be sarcomatoid — meaning another type of tumor (like a carcinoma) that looks like a sarcoma under the microscope.
Tumor-like conditions of soft tissue
Some conditions of soft tissues are caused by inflammation or injury and can form a mass that looks like a soft tissue tumor. Unlike a true tumor, they do not come from a single abnormal cell, they have limited capacity to grow or spread to nearby tissues, and never spread through the bloodstream or lymph system. Nodular fasciitis and myositis ossificans are 2 examples which affect tissues under the skin and muscle tissues, respectively.
Soft tissue sarcoma prognosis
Many children with cancer are cured of the disease. Children’s bodies have great capacity for healing. Also, huge improvements have been made in the treatment of childhood cancer in the past few decades. In the 1980s, around 65% of children diagnosed with cancer were alive more than 5 years after their diagnosis. Today, around 83% of children are successfully treated and become long-term survivors.
Long-term survival (also called the outlook or prognosis) and treatment options depend on a range of factors, including:
- age of your child at diagnosis
- extent or stage of the cancer
- appearance of the cancer cells under the microscope (the shape, function and structure of the cells)
- how the cancer responds to treatment
- cancer or tumour biology, which includes
- the patterns of the cancer cells
- how different the cancer cells are from normal cells
- how fast the cancer cells are growing.
Talk to your child’s doctor about your child’s individual disease, treatment options and outlook.
Soft tissue sarcoma causes
Scientists still don’t know exactly what causes most cases of soft tissue sarcoma, but they have found several risk factors that can make a person more likely to develop these cancers. And research has shown that some of these risk factors affect the DNA of cells in the soft tissues.
Researchers have made great progress in understanding how certain changes in DNA can cause normal cells to become cancerous. Your DNA carries the instructions for nearly everything your cells do. You usually look like your parents because they are the source of your DNA. However, DNA affects more than the way you look.
The DNA is divided into units called genes. Genes carry the recipes for making proteins, the molecules that determine all cell functions. Some genes contain instructions for proteins that control when our cells grow and divide.
Certain genes that promote cell division are called oncogenes. Others that slow down cell division or cause cells to die at the right time are called tumor suppressor genes. Cancers can be caused by DNA mutations (defects) that turn on oncogenes or turn off tumor suppressor genes.
Several family cancer syndromes have been found in which inherited DNA mutations cause a very high risk of developing breast, colon, kidney, eye, or other cancers. In some of these, there is also an increased risk of developing soft tissue sarcomas.
They are caused by defects (mutations) in genes that can be inherited from a parent. These gene defects can be found through testing.
DNA mutations in soft tissue sarcoma are common. They are usually acquired during life rather than having been inherited before birth. Acquired mutations may result from exposure to radiation or cancer-causing chemicals. In most sarcomas, they occur for no apparent reason.
Researchers still do not know why most soft tissue sarcomas develop in people who have no apparent risk factors.
Risk factors for soft tissue sarcoma
A risk factor is anything that changes your chance of getting a disease like cancer. Different cancers have different risk factors. For example, unprotected exposure to strong sunlight is a risk factor for skin cancer. Smoking is a risk factor for cancers of the lung, and many other cancers. But risk factors don’t tell us everything. Having a risk factor, or even several, doesn’t mean that you will get the cancer. Also, many people get cancer without having a risk factor.
Scientists have found a few risk factors that make a person more likely to develop soft tissue sarcomas. These include:
- Radiation
- Certain family cancer syndromes
- A damaged lymph system
- Exposure to certain chemicals
Injury and lifestyle factors such as smoking, diet, and exercise are NOT linked to the risk of soft tissue sarcoma.
Radiation given to treat other cancers
Patients might develop sarcomas from radiation given to treat other cancers, like breast cancer or lymphoma. The sarcoma often starts in the area of the body that had been treated with radiation. The average time between the radiation treatments and the diagnosis of a sarcoma is about 10 years. Radiation exposure accounts for less than 5% of sarcomas.
Radiation therapy techniques have improved steadily over several decades. Treatments now target cancers more precisely, and more is known about selecting radiation doses. These advances are expected to reduce the number of cancers caused by radiation therapy. But because these cancers take so long to develop, the results of these changes may not be seen for a long time. Still, radiation therapy is used only when its benefits (improved survival rate and relief of symptoms) outweigh the risk of cancer and other complications.
Family cancer syndromes
Family cancer syndromes are disorders caused by gene defects (mutations) that people are born with (often inherited from a parent) that are linked to a high risk of getting certain cancers. Some family cancer syndromes increase a person’s risk of developing soft tissue sarcomas.
Neurofibromatosis
Neurofibromatosis usually runs in families and is characterized by many benign tumors that form in nerves under the skin and in other parts of the body (neurofibromas). It is also known as von Recklinghausen disease. It is caused by a defect (mutation) in a gene called NF1. About 5% of people with neurofibromatosis will develop a malignant peripheral nerve sheath tumor in a neurofibroma.
Gardner syndrome
Gardner syndrome is a disease caused by defects in the APC gene. This syndrome is a type of familial adenomatous polyposis, and people with it get many polyps in the colon (and intestines) and have a high risk of getting colon cancer. It also causes problems outside the colon including desmoid tumors.
Li-Fraumeni syndrome
Li-Fraumeni syndrome is caused by inherited defects in the TP53 gene. People affected by this syndrome have a high risk of cancer, such as breast cancer, brain tumors, and sarcomas. People with this syndrome are sensitive to the cancer-causing effects of radiation. If their cancer is treated with radiation, they have a very high chance of developing a new cancer in the part of the body that received the radiation.
Retinoblastoma
Retinoblastoma is an eye cancer in children that can be caused by defects in the RB1 gene. Children with one of these gene defects also have a higher risk of developing bone or soft tissue sarcomas, especially if treated for cancer with radiation.
Werner syndrome
Werner syndrome is caused by defects in the RECQL2 gene. Children with this syndrome have problems like those seen in the elderly. These include cataracts, skin changes, and clogged heart arteries (arteriosclerosis) which can lead to heart attacks. They also have an increased risk of cancer, including soft tissue sarcomas.
Gorlin syndrome
Gorlin syndrome, also called nevoid basal cell carcinoma syndrome, is caused by defects in the PTCH1 gene. People with this syndrome have a high risk of developing many basal cell skin cancers. They also have an increased risk of getting fibrosarcoma and rhabdomyosarcoma.
Tuberous sclerosis
Tuberous sclerosis can be caused by a defect in the TSC1 gene. It can also be caused by a defect in another gene: TSC2. People with this syndrome often have seizures and learning problems. They get benign tumors in many different organs. They also get kidney problems, often along with a kidney tumor called angiomyolipoma. People with tuberous sclerosis have an increased risk of getting rhabdomyosarcoma.
Damaged lymph system
Lymph is a clear fluid containing immune system cells that is carried throughout the body by a series of lymph vessels. These vessels connect lymph nodes (small bean-shaped collections of immune system cells). When lymph nodes have been removed by surgery or damaged by radiation therapy, lymph fluid can build up and cause swelling. This is called lymphedema.
Lymphangiosarcoma (a malignant tumor that develops in lymph vessels) is a very rare complication of chronic lymphedema.
Chemicals
Exposure to vinyl chloride (a chemical used in making plastics) is a risk factor for developing sarcomas of the liver, but it has not been proven to cause soft tissue sarcomas. Arsenic has also been linked to a type of liver sarcoma but not soft tissue sarcoma. Exposure to dioxin and to herbicides that contain phenoxyacetic acid at high doses (such as might occur in people who work on farms) may also be risk factors, but this is not known for certain. There is no evidence that herbicides (weed killers) or insecticides, at levels encountered by the general public, cause sarcomas.
Injury
An injury is not a risk factor for developing sarcomas. But this issue has caused some confusion in the past. One reason is that an injured area might swell. That swelling could resemble a tumor but is not a true tumor. Also, when you are injured, the pain may draw your attention to the injured area. The area may be examined closely, and x-rays or other imaging studies may be obtained. This can make it more likely that any sarcoma that is present will be discovered, even though it may have been present for some time.
Soft tissue sarcoma prevention
The only way to prevent some soft tissue sarcomas is to avoid exposure to risk factors whenever possible. Most sarcomas, however, develop in people with no known risk factors, so there is no way known at this time to prevent most cases. And for people receiving radiation therapy, there is usually little choice.
Soft tissue sarcoma symptoms
A soft tissue sarcoma may not cause any signs and symptoms in its early stages.
Symptoms of soft tissue sarcomas may include a painless lump under the skin.
More than half of sarcomas begin in an arm or leg. Most people simply notice a lump that has grown over a period of time (weeks to months). Although the lump is often not painful, in some cases it will hurt.
If the tumor grows and presses on nearby organs, tissue, nerves or blood vessels, other symptoms can appear, such as pain or weakness. These symptoms vary, depending on where in the body the tumor has formed.
When sarcomas grow in the back of the abdomen (the retroperitoneum), the symptoms they cause more often come from other problems. Sometimes the tumors cause pain. They may also cause blockage or bleeding of the stomach or bowels. They can grow large enough for the tumor to be felt in the abdomen. About 20% of sarcomas begin in the abdomen (stomach) area.
Sarcomas can also begin on the outside of the chest or abdomen (about 10%) or in the head or neck area (around 10%).
If you have any of the following problems, see a doctor right away:
- A new lump or a lump that is growing (anywhere on your body)
- Abdominal pain that is getting worse
- Blood in your stool or vomit
- Black, tarry stools (when bleeding happens in the stomach or bowels, the blood can turn black as it is digested, and it may make the stool very black and sticky)
These symptoms are more often caused by things other than sarcoma, but they still need to be checked out by a doctor.
Can Soft Tissue Sarcomas Be Found Early?
People who have a strong family history of sarcomas or who have had other cancers when they were young, might wish to discuss the benefits and disadvantages of genetic testing with their doctor. The test results should always be explained by a genetic counselor or a specially trained doctor who can interpret the results and advise high-risk patients about the need for early cancer detection tests.
Families with a history of certain inherited conditions caused by defects in certain genes have an increased risk of developing soft tissue sarcomas. The mutated genes can be detected by genetic testing, so family members should discuss this option with their doctors. They should let their doctor know about any lumps or growths right away.
No screening tests and exams are recommended for people who have no family history of sarcoma or other sarcoma risk factors. For these people, the best approach to early detection is to tell their health care professional about any unexplained lumps or growths or other symptoms that may be caused by a soft tissue sarcoma.
Soft tissue sarcoma diagnosis
If you have signs or symptoms or other reasons to suggest you might have a sarcoma, your doctor will talk with you, examine you, and probably need to order some tests to find out if you have cancer.
Your doctor will order a number of tests to investigate their symptoms and confirm a diagnosis of soft tissue sarcoma, including:
- Medical imaging, which may include:
- X-ray
- ultrasound
- computed tomography (CT) scan
- magnetic resonance imaging (MRI)
- bone scan
- positron emission tomography (PET) scan
- Biopsy – where a small sample of the cancer is removed to be examined under a microscope. The sample can also be tested for genetic changes that can help determine the best type of treatment for you
- Lumbar puncture (spinal tap) – where a sample of cerebrospinal fluid is taken to be examined under a microscope
- Bone marrow aspiration and biopsy – where a sample of bone marrow is taken with a small piece of bone to be examined under a microscope.
Tests such as a computed tomography (CT) scan or a magnetic resonance imaging (MRI) scan, are often done to look for the cause of symptoms and to find a tumor (such as a sarcoma). Other tests may be done after a sarcoma is diagnosed to look for cancer spread.
Plain x-ray
A regular x-ray of the area with the lump may be the first test ordered. A chest x-ray may be done after you are diagnosed to see if the sarcoma has spread to the lungs.
Computed tomography scans
The CT scan is an x-ray procedure that produces detailed, cross-sectional images of your body. Instead of taking one picture like a conventional x-ray, a CT scanner takes many pictures as it rotates around you. A computer then combines these pictures into an image of a slice of your body. The machine will create multiple images of the part of your body being studied. A CT scan is often done if the doctor suspects a soft tissue sarcoma in the chest, abdomen, or the retroperitoneum (the of the abdomen) . This test is also used to see if the sarcoma has spread into the lungs, liver or other organs.
A CT scanner has been described as a large donut, with a narrow table in the middle opening. You will need to lie still on the table while the scan is being done. CT scans take longer than regular x-rays, and you might feel a bit confined by the ring while the pictures are being taken
Before any pictures are taken, you might be asked to drink 1 to 2 pints of a liquid called oral contrast. This helps outline the intestine more clearly. You may also receive an IV (intravenous) line through which a different kind of contrast dye (IV contrast) is injected. This helps better outline structures in your body.
The IV contrast dye can also cause some flushing (redness and warm feeling). Some people are allergic and get hives or, rarely, have more serious reactions like trouble breathing and low blood pressure. Be sure to tell the doctor if you have ever had a reaction to any contrast material used for x-rays.
CT scans might be done to precisely guide a biopsy needle into a tumor inside the body — the chest or abdomen, for example. For this procedure, called a CT-guided needle biopsy, the patient remains on the CT scanning table while a radiologist advances a biopsy needle toward the location of the mass. CT scans are repeated until the doctors are sure the needle is within the mass.
Magnetic resonance imaging scans
Magnetic resonance imaging (MRI) scans use radio waves and strong magnets instead of x-rays to take pictures of the body. The energy from the radio waves is absorbed and then released in a pattern formed by the type of tissue and by certain diseases. A computer translates the pattern of radio waves given off by the tissues into a very detailed image of parts of the body. A contrast material might be injected, just as with CT scans, but is used less often.
MRI scans are often part of the work-up of any tumor that could be a sarcoma. They are often better than CT scans in evaluating sarcomas in the arms or legs. They provide a good picture of the extent of the tumor. They can show your health care team many things about the tumor, including location, size, and sometimes even the type of tissue it comes from (like fat or muscle). This makes MRI scans useful in planning a biopsy.
MRIs are also very helpful in examining the brain and spinal cord.
MRI scans are a little more uncomfortable than CT scans. First, they take longer — often up to an hour. Also, you have to lie inside a long tube, which is confining and can be upsetting. Special “open” MRI machines sometimes are an option for people who have claustrophobia (fear of enclosed spaces), but the drawback is that the pictures are often not as clear. MRI machines also make a thumping noise that you may find disturbing. Some places will provide headphones with music to block this noise out.
Ultrasound
Ultrasound uses sound waves and their echoes to produce pictures of parts of the body. A small instrument called a transducer emits sound waves and picks up the echoes as they bounce off the organs. A computer converts the sound wave echoes into an image that is displayed on a computer screen.
This is a very easy procedure to have. It uses no radiation, which is why it is often used to look at developing fetuses. For most ultrasounds, you simply lie on a table while a technician moves the transducer over the part of your body being examined. Usually, the skin is first lubricated with gel. Ultrasound may be done before a biopsy to see if a lump is a cyst, meaning if it has fluid and is likely benign, or if it is solid and more likely a tumor. This test is often not needed if a CT or MRI was done.
Positron emission tomography scan
In this test, radioactive glucose (sugar) is injected into the patient’s vein to look for cancer cells. Because cancers use glucose (sugar) at a higher rate than normal tissues, the radioactivity will tend to concentrate in the cancer. A scanner can spot the radioactive deposits. A positron emission tomography (PET) scan is useful when your doctor thinks the cancer has spread but doesn’t know where. A PET scan can be used instead of several different x-rays because it scans your whole body. Often the PET scan is used with a CT scan. This helps decide if abnormalities seen on the CT scan are cancer or something else. PET is not often used for sarcoma, but it can be helpful in certain cases.
Biopsy
A biopsy is a procedure that removes a sample of tissue from a tumor to see if it is cancer. The piece of tissue is looked at under a microscope and, some other tests may be done on the sample as well. A physical exam or imaging test may suggest that a tumor is a sarcoma, but a biopsy is the only way to be certain that it is a sarcoma and not another type of cancer or a benign disease.
Several types of biopsies are used to diagnose sarcomas. Doctors experienced with these tumors will choose one, based on the size and location of the tumor. Most prefer to use a fine needle aspiration or a core needle biopsy as the first step.
Fine needle aspiration (FNA) biopsy
In FNA, the doctor uses a very thin needle and a syringe to withdraw small pieces of tissue from the tumor mass. The doctor can often aim the needle while feeling the mass near the surface of the body. If the tumor is too deep to feel, the doctor can guide the needle while viewing it on a computed tomography (CT) scan or ultrasound. The main advantage of FNA is that it can be used to biopsy tumors deep in the body without surgery. The disadvantage is that the thin needle may not remove enough tissue to make a precise diagnosis.
FNA is often useful in showing that a mass first thought to be a sarcoma (found on physical exam or imaging tests) is really another type of cancer, a benign tumor, an infection, or some other disease. But if FNA results suggest a sarcoma, another type of biopsy will usually be done to remove enough tissue to confirm that diagnosis. After a sarcoma is diagnosed, FNA is most useful in determining whether additional tumors in other organs are metastases.
Core needle biopsy
Core needle biopsies use a needle that is larger than the FNA needle. Sometimes this needle is called a Tru-Cut needle. It removes a cylindrical piece of tissue about 1/16 inch across and 1/2 inch long. It usually removes enough tissue to see if a sarcoma is present. Like FNA, CT scan and ultrasound can be used to guide the needle into tumors of internal organs.
Surgical biopsy
In a surgical biopsy, the entire tumor or a piece of the tumor is removed during an operation. There are 2 types of surgical biopsies, excisional and incisional. In an excisional biopsy, the surgeon removes the entire tumor. In an incisional biopsy, only a piece of a large tumor is removed. An incisional biopsy almost always removes enough tissue to diagnose the exact type and grade of sarcoma. If the tumor is near the skin surface, this is a simple operation that can be done with local or regional anesthesia (numbing medication given near the mass or into a nerve). But if the tumor is deep inside the body, general anesthesia is used (the patient is asleep).
If a tumor is rather small, near the surface of the body, and not located near critical tissues (such as important nerves or large blood vessels), the doctor may choose to remove the entire mass and a margin of normal tissue in an excisional biopsy. This surgery combines the biopsy and the treatment into one operation, so it should only be done by a surgeon with experience in treating sarcomas.
If the tumor is large, then an incisional biopsy is needed. Only a surgeon experienced in sarcoma treatment should perform this procedure.
You might want to ask about your surgeon’s experience with this procedure. Proper biopsy technique is a very important part of successfully treating soft tissue sarcomas. An improper biopsy can lead to tumor spread and problems removing the tumor later on. An incisional biopsy in the wrong place or an excision without wide enough margins can make it harder to completely remove a sarcoma later on. To prevent these problems, these 2 types of biopsies should only be done by a surgeon experienced in treating sarcomas. It is best that an incisional biopsy be done by the same surgeon who will later remove the entire tumor (if a sarcoma is found).
Testing biopsy samples
The tissue removed will be looked at under the microscope to see if cancer is present. If it is, the doctor will try to determine what kind it is (sarcoma or carcinoma).
- Grading: If a sarcoma is present, the biopsy will be used to determine what type it is and its grade. The grade of a sarcoma is based on how the cancer cells look under the microscope. In grading a cancer, the pathologist (a doctor who specializes in diagnosing diseases by looking at the tissue under a microscope) considers how closely the tumor resembles normal tissue (differentiation), how many of the cells appear to be dividing, and how much of the tumor is made up of dying tissue. Each factor is given a score, and the scores are added to determine the grade of the tumor. Sarcomas that have cells that look more normal and have fewer cells dividing are generally placed in a low-grade category. Low-grade tumors tend to be slow growing, slower to spread, and often have a better outlook (prognosis) than higher-grade tumors. Certain types of sarcoma are automatically given higher differentiation scores. This affects the overall score so much that they are never considered low grade. Examples of these include synovial sarcomas and embryonal sarcomas. The grade is partly used to determine the stage of a sarcoma. The official staging system (see How Are Soft Tissue Sarcomas Staged?) divides sarcomas into 3 grades (1 to 3). The grade of a sarcoma helps predict how rapidly it will grow and spread. It is useful in predicting a patient’s outlook and helps determine treatment options.
- Immunohistochemistry: Sometimes these special tests are needed to accurately determine whether a sarcoma is present and, if so, what type. Part of the biopsy sample is treated with special man-made antibodies that recognize cell proteins typical of certain kinds of sarcomas. The cells are treated with chemicals that make the cells containing these specific proteins change color. The color change is then seen under a microscope.
- Cytogenetics: For this test, cells’ chromosomes are examined with a microscope to look for changes. For example, in certain types of sarcomas part of one chromosome may be abnormally attached to part of a different chromosome (called a translocation). To see the chromosomes clearly, the cancer cells must be grown in laboratory dishes until they start dividing. This can take a week or more.
- Fluorescent in situ hybridization (FISH) can sometimes be used to detect translocations and other chromosome changes without first growing the cells in the lab. Tests of chromosome changes are not required to diagnose a sarcoma, but they are sometimes very useful in confirming that a certain type of sarcoma is present. And as new changes are discovered, these tests may become more important and more common.
- Reverse transcription polymerase chain reaction (RT-PCR): This test is another way to find translocations in some sarcomas (such as the Ewing family of tumors, alveolar rhabdomyosarcoma, and synovial sarcoma) to confirm the type of tumor. Instead of using a microscope to look for the chromosome changes as in cytogenetic testing or FISH, RT-PCR uses chemical analysis of the RNA (a substance that is made from DNA) from genes affected by the translocation. RT-PCR testing is often able to find translocations that aren’t detected by cytogenetics.
Soft tissue sarcoma stages
After someone is diagnosed with a soft tissue sarcoma, doctors will try to figure out if it has spread, and if so, how far. This process is called staging. The stage of a cancer describes how much cancer is in the body. It helps determine how serious the cancer is and how best to treat it. Doctors also use a cancer’s stage when talking about survival statistics.
The stages of soft tissue sarcomas range from stages I (1) through IV (4). As a rule, the lower the number, the less the cancer has spread. A higher number, such as stage IV, means cancer has spread more. And within a stage, an earlier letter means a lower stage. Although each person’s cancer experience is unique, cancers with similar stages tend to have a similar outlook and are often treated in much the same way.
How is the stage determined?
The staging system most often used for soft tissue sarcomas is the American Joint Committee on Cancer (AJCC) TNM system, which is based on 4 key pieces of information:
- The extent of the tumor (T): How large is the cancer?
- The spread to nearby lymph nodes (N): Has the cancer spread to nearby lymph nodes?
- The spread (metastasis) to distant sites (M): Has the cancer spread to distant organs such as the lungs?
- The grade (G) of the cancer: How much do the sarcoma cells look like normal cells?
The grade of a sarcoma is determined using a system known as the French or FNCLCC system, and is based on 3 factors:
- Differentiation: Cancer cells are given a score of 1 to 3, with 1 being assigned when they look similar to normal cells and 3 being used when the cancer cells look very abnormal. Certain types of sarcoma are given a higher score automatically.
- Mitotic count: How many cancer cells are seen dividing under the microscope; given a score from 1 to 3 (a lower score means fewer cells were seen dividing)
- Tumor necrosis: How much of the tumor is made up of dying tissue; given a score from 0 to 2 (a lower score means there was less dying tissue present).
The scores for each factor are added to determine the grade for the cancer. Higher-grade cancers tend to grow and spread faster than lower-grade cancers.
GX: The grade cannot be assessed (because of incomplete information).
Grade 1 (G1): Total score of 2 or 3
Grade 2 (G2): Total score of 4 or 5
Grade 3 (G3): Total score of 6, 7 or 8.
There are different staging systems for soft tissue sarcomas depending on where the cancer is in the body.
- Head and neck
- Trunk and extremities (arms and legs)
- Abdomen and thoracic (chest) visceral organs
- Retroperitoneum
Numbers or letters after T, N, and M provide more details about each of these factors. Higher numbers mean the cancer is more advanced. Once a person’s T, N, and M categories have been determined, this information is combined in a process called stage grouping to assign an overall stage. Of the 4 main locations, only 2 (Trunk and Extremities and Retroperitoneum) have stage groupings.
The staging system in the table below uses the pathologic stage (also called the surgical stage). It is determined by examining tissue removed during an operation. Sometimes, if surgery is not possible right away or at all, the cancer will be given a clinical stage instead. This is based on the results of a physical exam, biopsy, and imaging tests. The clinical stage will be used to help plan treatment. Sometimes, though, the cancer has spread further than the clinical stage estimates, and may not predict the patient’s outlook as accurately as a pathologic stage.
The system described below is the most recent AJCC system, effective January 2018. Cancer staging can be complex, so ask your doctor to explain it to you in a way you understand.
Table 1. Trunk and Extremities Sarcoma Stages
| AJCC stage | Stage grouping | Trunk and Extremities Sarcoma Stage description* |
| IA | T1 N0 M0 G1 or GX | The cancer is 5 cm (2 inches) or smaller (T1). It has not spread to nearby lymph nodes (N0) or to distant sites (M0). The cancer is grade 1 (G1) or the grade cannot be assessed (GX). |
| IB | T2, T3, T4 N0 M0 G1 or GX | The cancer is:
It has not spread to nearby lymph nodes (N0) or to distant sites (M0). The cancer is grade 1 (G1) or the grade cannot be assessed (GX). |
| II | T1 N0 M0 G2 or G3 | The cancer is 5 cm (2 inches) or smaller (T1). It has not spread to nearby lymph nodes (N0) or to distant sites (M0). The cancer is grade 2 (G2) or grade 3 (G3). |
| IIIA
| T2 N0 M0 G2 or G3 | The cancer is larger than 5 cm (2 inches) but not more than 10 cm (T2). It has not spread to nearby lymph nodes (N0) or to distant sites (M0). The cancer is grade 2 (G2) or grade 3 (G3). |
| IIIB | T3 or T4 N0 M0 G2 or G3 | The cancer is:
It has not spread to nearby lymph nodes (N0) or to distant sites (M0). The cancer is grade 2 (G2) or grade 3 (G3). |
| IV | Any T N1 M0 Any G | The cancer is any size (Any T) AND it has spread to nearby lymph nodes (N1). It has not spread to distant sites (M0). It can be any grade. |
| OR | ||
| Any T Any N M1 Any G | The cancer is any size (Any T) AND it has spread to nearby lymph nodes (N1). It has spread to distant sites such as the lungs (M1). It can be any grade. | |
*The following additional categories are not listed in the table above:
- TX: Main tumor cannot be assessed due to lack of information.
- T0: No evidence of a primary tumor.
- NX: Regional lymph nodes cannot be assessed due to lack of information.
Table 2. Retroperitoneum Sarcoma Stages
| AJCC stage | Stage grouping | Retroperitoneum Sarcoma Stage description* |
| IA | T1 N0 M0 G1 or GX | The cancer is 5 cm (2 inches) or smaller (T1). It has not spread to nearby lymph nodes (N0) or to distant sites (M0). The cancer is grade 1 (G1) or the grade cannot be assessed (GX). |
| IB | T2, T3, T4 N0 M0 G1 or GX | The cancer is:
It has not spread to nearby lymph nodes (N0) or to distant sites (M0). The cancer is grade 1 (G1) or the grade cannot be assessed (GX). |
| II | T1 N0 M0 G2 or G3 | The cancer is 5 cm (2 inches) or smaller (T1). It has not spread to nearby lymph nodes (N0) or to distant sites (M0). The cancer is grade 2 (G2) or grade 3 (G3). |
| IIIA
| T2 N0 M0 G2 or G3 | The cancer is larger than 5 cm (2 inches) but not more than 10 cm (T2). It has not spread to nearby lymph nodes (N0) or to distant sites (M0). The cancer is grade 2 (G2) or grade 3 (G3). |
| IIIB | T3 or T4 N0 M0 G2 or G3 | The cancer is:
It has not spread to nearby lymph nodes (N0) or to distant sites (M0). The cancer is grade 2 (G2) or grade 3 (G3). |
| OR | ||
| Any T N1 M0 Any G | The cancer is any size (Any T) AND it has spread to nearby lymph nodes (N1). It has not spread to distant sites (M0). It can be any grade. | |
| IV | Any T Any N M1 Any G | The cancer is any size (Any T) AND it has spread to nearby lymph nodes (N1). It has spread to distant sites such as the lungs (M1). It can be any grade. |
*The following additional categories are not listed in the table above:
- TX: Main tumor cannot be assessed due to lack of information.
- T0: No evidence of a primary tumor.
- NX: Regional lymph nodes cannot be assessed due to lack of information.
Soft tissue sarcoma survival rate
Survival rates are often used by doctors as a standard way of discussing a person’s prognosis (outlook).
The 5-year survival rate (or observed survival rate) refers to the percentage of patients who live at least 5 years after their cancer is diagnosed. Of course, many people live much longer than 5 years (and many are cured).
Five-year relative survival rates assume that some people will die of other causes and compare the observed survival with that expected for people without the cancer. This is a better way to see the effect of the cancer on survival.
To get 5-year survival rates, doctors have to look at people who were treated at least 5 years ago. If treatment has improved since then, people now being diagnosed with soft tissue sarcoma may have a more favorable outlook.
Survival rates are often based on previous outcomes of large numbers of people who had the disease, but they cannot predict what will happen in any individual’s case. Many other factors might affect a person’s outlook, like the type of sarcoma, the location of the tumor, the treatment received, and the age of the patient. For example, sarcomas of the arms or legs have a better outcome than those found in other places. Also, older patients tend to have worse outcomes than younger people. Your doctor can tell you how the numbers below may apply to you, as he or she is familiar with your particular situation.
The rates below are based on the stage of the cancer at the time of diagnosis. When looking at survival rates, it’s important to understand that the stage of a cancer does not change over time, even if the cancer progresses. A cancer that comes back or spreads is still referred to by the stage it was given when it was first found and diagnosed, but more information is added to explain the current extent of the cancer. (And the treatment plan is adjusted based on the change in cancer status.)
The overall relative 5-year survival rate of people with soft tissue sarcomas is around 50% according to statistics from the National Cancer Institute (NCI). These statistics include people with Kaposi sarcoma, which has a poorer outlook than many sarcomas. The NCI doesn’t use the AJCC staging system. Instead, they group sarcomas only by whether they are still confined to the primary site (called localized) have spread to nearby lymph nodes or tissues (called regional); or have spread (metastasized) to sites away from the main tumor (called distant). The 5-year survival rates for soft tissue sarcomas have not changed much for many years. The corresponding 5-year relative survival rates were:
- 83% for localized sarcomas (56% of soft tissue sarcomas were localized when they were diagnosed)
- 54% for regional stage sarcomas; (19% were in this stage)
- 16% for sarcomas with distant spread (16% were in this stage)
The 10-year relative survival rate is only slightly worse for these stages, meaning that most people who survive 5 years are probably cured.
For sarcomas of the arms and legs, Memorial Sloan-Kettering Cancer Center has survival rates broken down by AJCC stage (these are for observed, not relative survival):
| Stage | 5-year observed survival rate |
| I | 90% |
| II | 81% |
| III | 56% |
| IV | Not available |
Survival is worse when the sarcoma has developed somewhere other than the arms or legs. For example, the 5-year survival for retroperitoneal sarcomas is around 40% to 60%.
Soft tissue sarcoma treatment
Your treatment options for soft tissue sarcoma will depend on the size, type and location of your tumor.
Experts recommend that patients with sarcoma have a health care team made up of doctors from different specialties, such as:
- An orthopedic surgeon: a surgeon who specializes in diseases of the bones, muscles, and joints (for sarcomas of the arms and legs)
- A surgical oncologist: a doctor who treats cancer with surgery (for sarcomas of the abdomen and retroperitoneum [the back of the abdomen])
- A thoracic surgeon: a doctor who treats diseases of the lungs and chest with surgery (for sarcomas in the chest)
- A medical oncologist: a doctor who treats cancer with medicines such as chemotherapy
- A radiation oncologist: a doctor who treats cancer with radiation therapy
- A physiatrist (or rehabilitation doctor): a doctor who treat injuries or illnesses that affect how you move
Many other specialists may be involved in your care as well, including physician assistants, nurse practitioners, nurses, respiratory therapists, social workers, physical therapists, and other health professionals.
After a sarcoma is found and staged, your team will recommend one or several treatment options. This decision is important, so take time and think about all of the choices. In choosing a treatment plan, factors to consider include the type, location, and stage of the cancer, as well as your overall physical health.
The main types of treatment for soft tissue sarcoma are:
- Surgery
- Radiation
- Chemotherapy
- Targeted therapy
It is important to discuss all of your treatment options, including their goals and possible side effects, with your doctors to help make the decision that best fits your needs. It’s also very important to ask questions if there is anything you’re not sure about.
Surgery
Surgery is a common treatment for soft tissue sarcoma. Most patients can be treated with surgery to remove the tumor without amputation (called limb-sparing surgery). This is usually followed by radiation therapy. These patients have the same survival rates as those who have amputations.
Sometimes, an amputation can’t be avoided. It might be the only way to remove all of the cancer. Other times, critical nerves, muscles, bone, and blood vessels would have to be removed along with the cancer. If removing this tissue would mean leaving a limb that can’t function well or would result in chronic pain, amputation may be the best option.
If the sarcoma has spread to distant sites (such as the lungs or other organs), all of the cancer will be removed if possible. That includes the original tumor plus the areas of spread. If it isn’t possible to remove all of the sarcoma, then surgery may not be done at all.
When soft tissue sarcoma affects the arms and legs, radiation and chemotherapy may be considered to shrink the tumor to avoid amputation. This, called neoadjuvant treatment, can shrink the tumor and allow it to be removed completely. Chemo or radiation can also be given before surgery to treat high-grade sarcomas when there is a great risk of the cancer spreading.
Most of the time, surgery cannot cure a sarcoma once it has spread. But if it has only spread to a few spots in the lung, the metastatic tumor can sometimes be removed. This can cure many patients, or at least lead to long-term survival.
Radiation therapy
Radiation therapy involves treating cancer with high-powered beams of energy. Options include:
- Before surgery. Radiation before surgery can help shrink the tumor so that it’s easier to remove.
- During surgery. Intraoperative radiation allows a higher dose of radiation to be delivered directly to the target area, while sparing surrounding tissues.
- After surgery. Postoperative radiation can help kill any remaining cancer cells.
Types of radiation therapy
- External beam radiation therapy: For this treatment, radiation delivered from outside the body is focused on the cancer. This is the type of radiation therapy most often used to treat sarcomas. Treatments are often given daily, 5 days a week, usually for several weeks. Often a technique called intensity modulated radiation therapy (IMRT) is used. This better focuses the radiation on the cancer and lessens the impact on healthy tissue. In some centers, proton beam radiation is an option. This uses streams of protons instead of x-ray beams to treat the cancer. Although this has some advantages over IMRT in theory, it hasn’t been proven to be a better treatment for soft tissue sarcoma. Proton beam therapy is not widely available.
- Intraoperative radiation therapy (IORT): This is a type of external beam radiation that is available in only a few centers. For this treatment, one large dose of radiation is given in the operating room after the tumor is removed but before the wound is closed. Giving radiation this way means that it doesn’t have to travel through healthy tissue to get to the area that needs to be treated. It also allows nearby healthy areas to be shielded more easily from the radiation. Often, IORT is only one part of radiation therapy, and the patient receives some other type of radiation after surgery.
- Brachytherapy: Brachytherapy (sometimes called internal radiation therapy) is a treatment that places small pellets (or seeds) of radioactive material in or near the cancer. For soft tissue sarcoma, these pellets are put into catheters (very thin tubes) that have been placed during surgery. In high-dose rate (HDR) brachytherapy, the pellets give off a lot of radiation in a short time, and so stay in place for only minutes at a time. In low-dose rate brachytherapy, the pellets may stay in place for days at a time, and are then removed. Brachytherapy may be the only form of radiation therapy used or it can be combined with external beam radiation.
Side effects of radiation treatment
Side effects of radiation therapy depend on which area is treated and the dose given. Common side effects include:
- Skin changes in the area the radiation went through the skin, which can range from redness to blistering and peeling
- Fatigue.
- Nausea and vomiting (more common with radiation to the abdomen)
- Diarrhea (most common with radiation to the pelvis and abdomen)
- Pain with swallowing (from radiation to the head, neck, or chest)
- Lung damage leading to problems breathing (from radiation to the chest)
- Bone weakness, which can lead to fracture years later
Radiation of large areas of an arm or leg can cause swelling, pain, and weakness in that limb.
Side effects of radiation therapy to the brain for metastatic sarcoma include hair loss, headaches, and problems thinking.
If given before surgery, radiation may cause problems with wound healing.
Many side effects improve or even go away some time after radiation is finished. Some though, like bone weakness and lung damage, can be permanent.
Chemotherapy
Chemotherapy is a drug treatment that uses chemicals to kill cancer cells. Chemotherapy can be administered by pill or through a vein (intravenously). Some forms of soft tissue sarcoma respond better to chemotherapy than do others. For instance, chemotherapy is often used to treat rhabdomyosarcoma.
Chemotherapy for soft tissue sarcoma generally uses a combination of several anti-cancer drugs.
The most commonly used drugs are ifosfamide (Ifex®) and doxorubicin (Adriamycin®). When ifosfamide is used, the drug mesna is also given. Mesna is not a chemo drug. It protects the bladder from the toxic effects of ifosfamide.
Other chemo drugs may be used as well, including cisplatin, dacarbazine (DTIC), docetaxel (Taxotere®), gemcitabine (Gemzar®), methotrexate, oxaliplatin, paclitaxel (Taxol®), vincristine, vinorelbine (Navelbine®), trabectedin (Yondelis®), and eribulin (Halaven®).
When several drugs are used together, the combination is given a shortened name such as: MAID (mesna, Adriamycin [doxorubicin], ifosfamide, and dacarbazine).
Chemotherapy drugs kill cancer cells but also damage some normal cells. Side effects depend on the type of drugs, the amount taken, and the length of treatment.
Common chemo side effects include:
- Nausea and vomiting
- Loss of appetite
- Loss of hair
- Mouth sores
- Fatigue
- Low blood counts
Because chemotherapy can damage the blood-producing cells of the bone marrow, patients may have low blood cell counts. This can result in:
- Increased chance of infection (from too few white blood cells)
- Problems with bleeding or bruising (from too few blood platelets)
- Fatigue and weakness (from too few red blood cells)
Most side effects disappear once treatment is stopped. Hair will grow back after treatment ends, but it might look different. There are remedies for many of the temporary side effects of chemotherapy. For example, drugs can be given that prevent or reduce nausea and vomiting.
Some chemo side effects can last a long time or even be permanent. For example, doxorubicin can weaken the heart if too much is given. If you are to be treated with this drug, your doctor might check your heart function with special studies before starting this drug. The doctor will also watch the dose of doxorubicin closely during therapy.
Some chemo drugs cause nerve damage (called neuropathy), leading to numbness, tingling, or even pain in the hands and feet.
Chemotherapy may also permanently damage ovaries or testicles, which can lead to infertility (not being able to have children).
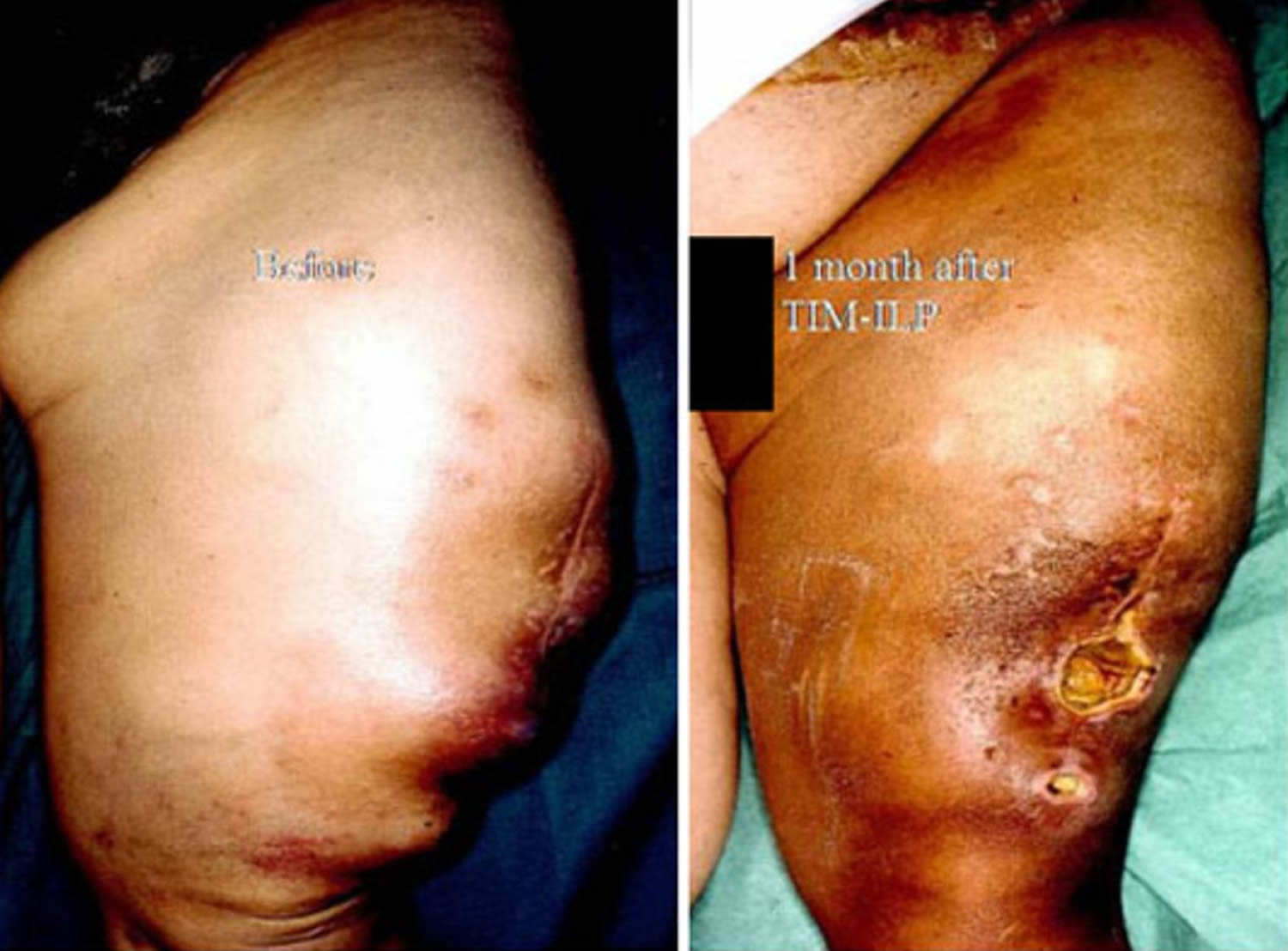
Isolated limb perfusion
This procedure is a different way to give chemo. The circulation of the limb (arm or leg) with the tumor in it is separated from that of the rest of the body. Chemo is given just to that limb. Sometimes the blood is warmed up a bit to help the chemo work better (this is called hyperthermia). This can help shrink tumors, but it isn’t clear that it helps patients live longer than standard chemo. It should only be done at centers with a lot of experience in giving chemo this way.
Targeted drug treatment
Targeted therapy is a newer type of cancer treatment that uses drugs or other substances to identify and attack cancer cells while doing little damage to normal cells. These therapies attack parts of cancer cells that make them different from normal, healthy cells. Each type of targeted therapy works differently, but all alter the way a cancer cell grows, divides, repairs itself, or interacts with other cells.
Some types of soft tissue sarcoma have specific characteristics in their cells that can be attacked via targeted drug treatments. These medicines work better than chemotherapy and aren’t nearly as toxic. Targeted treatments have been particularly helpful in gastrointestinal stromal tumors (GISTs).
- Olaratumab (Lartruvo)
This drug is a type of monoclonal antibody, which is a manmade version of an immune system protein. It targets PDGFR-alpha, a protein on tumor cells that can help them grow. By blocking this protein, olaratumab can cause some tumors to shrink or stop growing. This may help people live longer.
This drug can be used along with the chemotherapy drug doxorubicin to treat soft tissue sarcomas that cannot be cured with radiation therapy or surgery.
Olaratumab is given by infusion into a vein (IV). Some people have allergic-like reactions while getting this drug, which can cause symptoms such as low blood pressure, fever, chills, and rash. Less often, reactions can be more serious or even life-threatening. Other possible side effects of this drug include nausea and vomiting, feeling tired, muscle or joint pain, swelling in the mouth or throat, hair loss, headache, loss of appetite, diarrhea, and nerve damage (neuropathy), which can cause numbness, tingling, or pain in the hands or feet.
- Pazopanib (Votrient)
Pazopanib blocks several cellular enzymes called tyrosine kinases that are important for cell growth and survival. In a study of patients with advanced soft tissue sarcomas that had been treated with chemotherapy, pazopanib stopped the cancers from growing for an average of about 3 months longer than the patients given a sugar pill. So far, though, this drug hasn’t been shown to help patients live longer. This drug is taken in pill form, once a day.
Common side effects include high blood pressure, nausea, diarrhea, headaches, low blood cell counts, and liver problems. In some patients this drug causes abnormal results on liver function tests, but it also rarely leads to severe liver damage that can be life threatening. Bleeding, clotting, and wound healing problems can occur, as well. This drug also rarely causes a problem with the heart rhythm or even a heart attack. If you are taking pazopanib, your doctor will monitor your heart with EKGs as well as check your blood tests to check for liver or other problems.
- Imatinib (Gleevec)
Imatinib is a tyrosine kinase inhibitor drug approved to treat gastrointestinal stromal tumors and some kinds of leukemia. It also can be helpful in treating desmoid tumors that can’t be removed with surgery. Although it rarely causes tumors to shrink, it often causes them to stop growing for a time, which can be very helpful.
Side effects can include mild stomach upset, diarrhea, muscle pain, and skin rashes. The stomach upset is lessened if the drug is taken with food. Imatinib can also make people retain fluid. Often this causes some swelling in the face (around the eyes) or in the ankles. Rarely the drug causes more severe problems, such as fluid build up in the lungs or abdomen or causing problems with heart function.
Coping and support
A diagnosis of cancer can be overwhelming. With time you’ll find ways to cope with the distress and uncertainty of cancer. Until then, you may find it helps to:
- Learn enough about sarcoma to make decisions about your care. Ask your doctor about your soft tissue sarcoma, including your treatment options and, if you like, your prognosis. As you learn more about soft tissue sarcoma, you may become more confident in making treatment decisions.
- Keep friends and family close. Keeping your close relationships strong will help you deal with your soft tissue sarcoma. Friends and family can provide the practical support you’ll need, such as helping take care of your house if you’re in the hospital. And they can serve as emotional support when you feel overwhelmed by cancer.
- Find someone to talk with. Find a good listener who is willing to listen to you talk about your hopes and fears. This may be a friend or family member. The concern and understanding of a counselor, medical social worker, clergy member or cancer support group also may be helpful.