Contents
- What is Metabolic Syndrome
- Other Names for Metabolic Syndrome
- Metabolic Syndrome is composed of the following Five Symptoms:
- Metabolic Syndrome Criteria
- Metabolic Syndrome Prevention
- Metabolic Syndrome Symptoms and Signs
- Metabolic Syndrome Causes 7, 8
- Metabolic Syndrome Risk Factors
- Metabolic Syndrome Overview
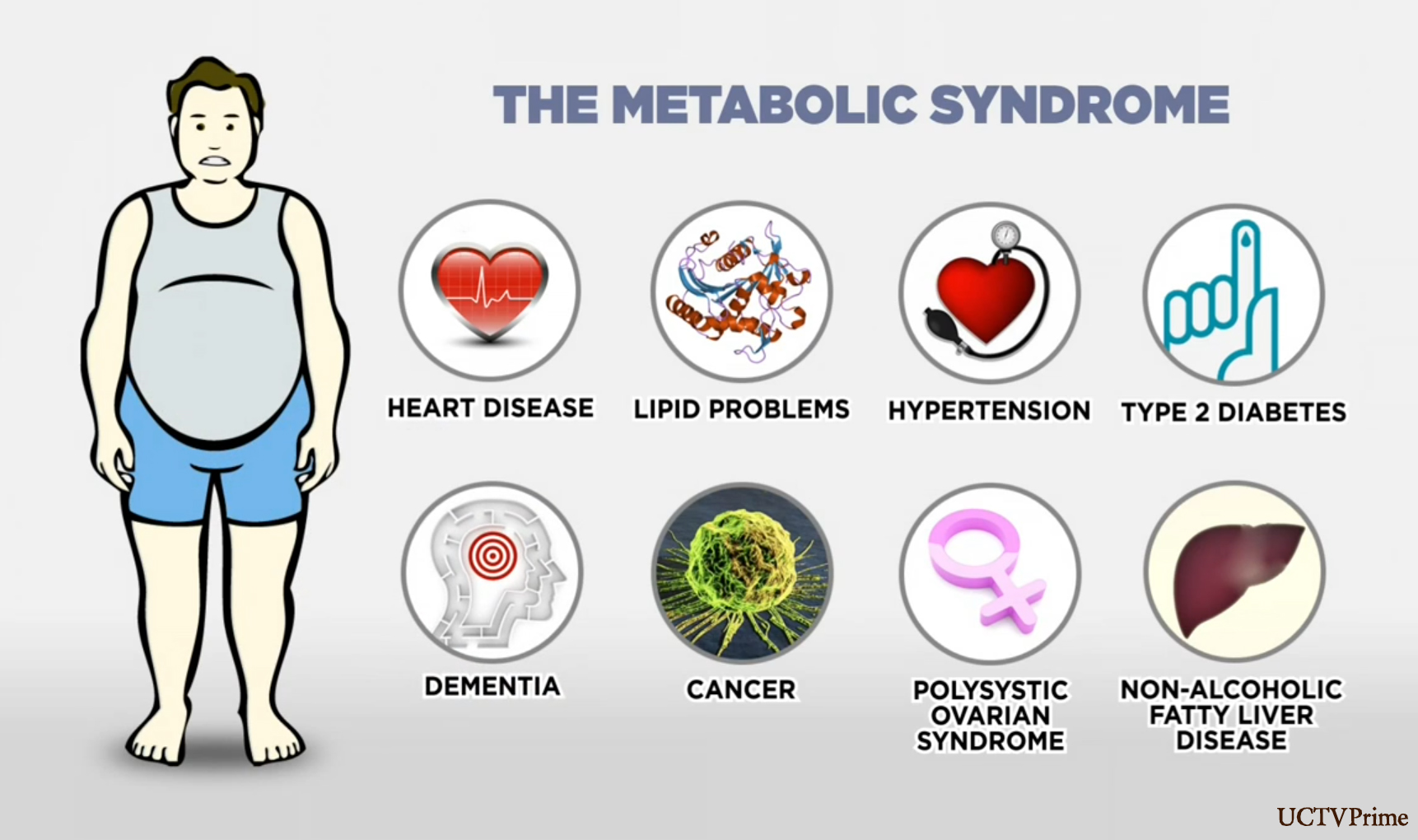
- Metabolic Syndrome is linked to heart disease and diabetes
- Metabolic Syndrome Treatment
- Metabolic Syndrome Diet
What is Metabolic Syndrome
Metabolic syndrome also called insulin resistance syndrome, is a group of traits and medical conditions linked to overweight and obesity that puts people at risk for both cardiovascular disease (coronary artery disease a condition in which a waxy substance called plaque builds up inside the coronary heart arteries) and type 2 diabetes. The high prevalence of the metabolic syndrome has considerable clinical implications, because the syndrome is an important risk factor for cardiovascular disease 1. Data from several studies have demonstrated that the metabolic syndrome is associated with a 3—4-fold increased risk of cardiovascular disease, cardiovascular mortality, and stroke 2, 3. Metabolic Syndrome involves a cluster of symptoms that, when present together, increase the chances of acquiring a chronic disease, such as diabetes, heart disease and liver disease 4. About 34% of U.S. adults and 20 to 30 percent of the adult population in most countries have metabolic syndrome 5. Although these risks are significant, there is good news. Metabolic syndrome can be treated and you can reduce your risks for cardiovascular events by maintaining a healthy weight, eating a heart-healthy diet, getting adequate physical activity, and following your healthcare providers’ instructions.
Other Names for Metabolic Syndrome
- Syndrome X
- Dysmetabolic syndrome
- Hypertriglyceridemic waist
- Insulin resistance syndrome
- Obesity syndrome
People who have metabolic syndrome often have two other conditions: excessive blood clotting and constant, low-grade inflammation throughout the body. Researchers don’t know whether these conditions cause metabolic syndrome or worsen it.
Metabolic syndrome is becoming more common due to a rise in obesity rates among adults. In the future, metabolic syndrome may overtake smoking as the leading risk factor for heart disease.
Metabolic syndrome has become increasingly common in the United States. Several factors increase the likelihood of acquiring metabolic syndrome:
- Obesity/overweight
- Obesity is an important potential cause of metabolic syndrome. Excessive fat in and around the abdomen is most strongly associated with metabolic syndrome. However, the reasons abdominal obesity and metabolic syndrome seem to be linked are complex and not fully understood.
- Insulin resistance: Metabolic syndrome is closely associated with a generalized metabolic disorder called insulin resistance, in which the body can’t use insulin efficiently. Some people are genetically predisposed to insulin resistance.
- Race and gender: When people have the same body mass index (BMI), Mexican Americans have the highest rate of metabolic syndrome, followed by Caucasians and African Americans. Men are more likely than women to develop metabolic syndrome.
Metabolic Syndrome is composed of the following Five Symptoms:
You must have at least three of the five metabolic risk factors to be diagnosed with metabolic syndrome.
– Large Waist Size: 35 inch (>88 cm) or more for women and 40 inch (>102 cm) for men
– High triglycerides: 150 mg/dL or higher (or use of cholesterol medication)
– High total cholesterol or HDL levels under 50 mg/dL for women, 40 mg for men
– High blood pressure: 135/85 mm or higher
– High blood sugar: fasting blood glucose level of 100 mg/dL or above, or taking medication for elevated blood glucose
According to the American Heart Association, 56 million Americans have metabolic syndrome, or roughly one in five people (22.9%) over age 20, placing them at higher risk for chronic disease 6. The syndrome runs in families and varies across racial-ethnic groups.
In addition to type 2 diabetes, metabolic syndrome has been linked to the following health disorders:
- Obesity
- Cardiovascular Disease (CVD)
- Polycystic Ovarian Syndrome (PCOS)
- Nonalcoholic fatty liver disease
- Chronic kidney disease
However, not everyone with these disorders has insulin resistance and some people may have insulin resistance without getting these disorders.
People who are obese or who have metabolic syndrome, insulin resistance, type 2 diabetes or prediabetes often also have low-level inflammation throughout the body and blood clotting defects that increase the risk of developing blood clots in the arteries. These conditions contribute to increased risk for cardiovascular disease.
Metabolic Syndrome Criteria
- How Is Metabolic Syndrome Diagnosed ?
Because metabolic syndrome is a cluster of conditions, many of which must be determined with lab work, this condition is not one that an individual can assess without the help of a healthcare provider. However, if you have a large waist circumference and have been told by your healthcare provider that you have another condition like elevated triglycerides, high blood sugar or high blood pressure, you will need to discuss your combined risks with your healthcare provider.
Your doctor will diagnose metabolic syndrome based on the results of a physical exam and blood tests. You must have at least three of the five metabolic risk factors to be diagnosed with metabolic syndrome.
- Metabolic Risk Factors
1) A Large Waistline
Having a large waistline means that you carry excess weight around your waist (abdominal obesity). This is also called having an “apple-shaped” figure. Your doctor will measure your waist to find out whether you have a large waistline.
A waist measurement of 35 inches or more for women (>88 cm) or 40 inches or more for men (>102 cm) is a metabolic risk factor. A large waistline means you’re at increased risk for heart disease and other health problems.
2) A High Triglyceride Level
Triglycerides are a type of fat found in the blood. A triglyceride level of 150 mg/dL or higher (or being on medicine to treat high triglycerides) is a metabolic risk factor. (The mg/dL is milligrams per deciliter—the units used to measure triglycerides, cholesterol, and blood sugar.)
3) A Low HDL Cholesterol Level
HDL cholesterol sometimes is called “good” cholesterol. This is because it helps remove cholesterol from your arteries.
An HDL cholesterol level of less than 50 mg/dL for women and less than 40 mg/dL for men (or being on medicine to treat low HDL cholesterol) is a metabolic risk factor.
4) High Blood Pressure
A blood pressure of 130/85 mmHg or higher (or being on medicine to treat high blood pressure) is a metabolic risk factor. (The mmHg is millimeters of mercury—the units used to measure blood pressure.)
If only one of your two blood pressure numbers is high, you’re still at risk for metabolic syndrome.
5) High Fasting Blood Sugar
A normal fasting blood sugar level is less than 100 mg/dL. A fasting blood sugar level between 100–125 mg/dL is considered prediabetes. A fasting blood sugar level of 126 mg/dL or higher is considered diabetes.
A fasting blood sugar level of 100 mg/dL or higher (or being on medicine to treat high blood sugar) is a metabolic risk factor.
About 85 percent of people who have type 2 diabetes—the most common type of diabetes—also have metabolic syndrome. These people have a much higher risk for heart disease than the 15 percent of people who have type 2 diabetes without metabolic syndrome.
Metabolic Syndrome Prevention
The best way to prevent metabolic syndrom is to adopt heart-healthy lifestyle changes. Make sure to schedule routine doctor visits to keep track of your cholesterol, blood pressure, and blood sugar levels. Speak with your doctor about a blood test called a lipoprotein panel, which shows your levels of total cholesterol, LDL cholesterol, HDL cholesterol, and triglycerides.
Metabolic Syndrome Symptoms and Signs
Metabolic syndrome is a group of risk factors that raises your risk for heart disease and other health problems, such as diabetes and stroke. These risk factors can increase your risk for health problems even if they’re only moderately raised (borderline-high risk factors).
- Most of the metabolic risk factors have no signs or symptoms, although a large waistline is a visible sign.
- Some people may have symptoms of high blood sugar if diabetes—especially type 2 diabetes—is present.
- Symptoms of high blood sugar often include increased thirst; increased urination, especially at night; fatigue (tiredness); and blurred vision.
- High blood pressure usually has no signs or symptoms. However, some people in the early stages of high blood pressure may have dull headaches, dizzy spells, or more nosebleeds than usual.
Metabolic Syndrome Causes 7, 8
Some people are genetically prone to develop insulin resistance or metabolic syndrome. Other people develop metabolic syndrome by:
- Putting on excess body fat
- Failing to get enough physical activity
Metabolic syndrome has several causes that act together. You can control some of the causes, such as overweight and obesity, an inactive lifestyle, and insulin resistance.
You can’t control other factors that may play a role in causing metabolic syndrome, such as growing older. Your risk for metabolic syndrome increases with age.
You also can’t control genetics (ethnicity and family history), which may play a role in causing the condition. For example, genetics can increase your risk for insulin resistance, which can lead to metabolic syndrome.
Researchers continue to study conditions that may play a role in metabolic syndrome, such as:
- A fatty liver (excess triglycerides and other fats in the liver)
- Polycystic ovarian syndrome (a tendency to develop cysts on the ovaries)
- Gallstones
- Breathing problems during sleep (such as sleep apnea)
Fortunately, many of the factors that contribute to metabolic syndrome can be addressed through lifestyle changes, such as diet, exercise, and weight loss. By making these changes, you can significantly reduce your risks.
Metabolic Syndrome Risk Factors
The five conditions described below are metabolic risk factors. You can have any one of these risk factors by itself, but they tend to occur together. You must have at least three metabolic risk factors to be diagnosed with metabolic syndrome 9.
- A large waistline. This also is called abdominal obesity or “having an apple shape.” Excess fat in the stomach area is a greater risk factor for heart disease than excess fat in other parts of the body, such as on the hips.
- A high triglyceride level (or you’re on medicine to treat high triglycerides). Triglycerides are a type of fat found in the blood.
- A low HDL cholesterol level (or you’re on medicine to treat low HDL cholesterol). HDL sometimes is called “good” cholesterol. This is because it helps remove cholesterol from your arteries. A low HDL cholesterol level raises your risk for heart disease.
- High blood pressure (or you’re on medicine to treat high blood pressure). Blood pressure is the force of blood pushing against the walls of your arteries as your heart pumps blood. If this pressure rises and stays high over time, it can damage your heart and lead to plaque buildup.
- High fasting blood sugar (or you’re on medicine to treat high blood sugar). Mildly high blood sugar may be an early sign of diabetes.
People at greatest risk for metabolic syndrome have these underlying causes:
- Abdominal obesity (a large waistline)
- An inactive lifestyle
- Insulin resistance
Some people are at risk for metabolic syndrome because they take medicines that cause weight gain or changes in blood pressure, blood cholesterol, and blood sugar levels. These medicines most often are used to treat inflammation, allergies, HIV, and depression and other types of mental illness.
Populations Affected
Some racial and ethnic groups in the United States are at higher risk for metabolic syndrome than others. Mexican Americans have the highest rate of metabolic syndrome, followed by whites and blacks.
Other groups at increased risk for metabolic syndrome include:
- People who have a personal history of diabetes
- People who have a sibling or parent who has diabetes
- Women when compared with men
- Women who have a personal history of polycystic ovarian syndrome (a tendency to develop cysts on the ovaries)
Heart Disease Risk
Metabolic syndrome increases your risk for coronary heart disease. Other risk factors, besides metabolic syndrome, also increase your risk for heart disease. For example, a high LDL (“bad”) cholesterol level and smoking are major risk factors for heart disease. For details about all of the risk factors for heart disease, go to the Coronary Heart Disease Risk Factors Health Topic.
Even if you don’t have metabolic syndrome, you should find out your short-term risk for heart disease. The National Cholesterol Education Program divides short-term heart disease risk into four categories. Your risk category depends on which risk factors you have and how many you have.
Your risk factors are used to calculate your 10-year risk of developing heart disease. The National Cholesterol Education Program has an online calculator 10 that you can use to estimate your 10-year risk of having a heart attack.
- High risk: You’re in this category if you already have heart disease or diabetes, or if your 10-year risk score is more than 20 percent.
- Moderately high risk: You’re in this category if you have two or more risk factors and your 10-year risk score is 10 percent to 20 percent.
- Moderate risk: You’re in this category if you have two or more risk factors and your 10-year risk score is less than 10 percent.
- Lower risk: You’re in this category if you have zero or one risk factor.
Even if your 10-year risk score isn’t high, metabolic syndrome will increase your risk for coronary heart disease over time.
Metabolic Syndrome Overview
Your risk for heart disease, diabetes, and stroke increases with the number of metabolic risk factors you have. The risk of having metabolic syndrome is closely linked to overweight and obesity and a lack of physical activity.
Insulin resistance also may increase your risk for metabolic syndrome. Insulin resistance is a condition in which the body can’t use its insulin properly. Insulin is a hormone that helps move blood sugar into cells where it’s used for energy. Insulin resistance can lead to high blood sugar levels, and it’s closely linked to overweight and obesity. Genetics (ethnicity and family history) and older age are other factors that may play a role in causing metabolic syndrome.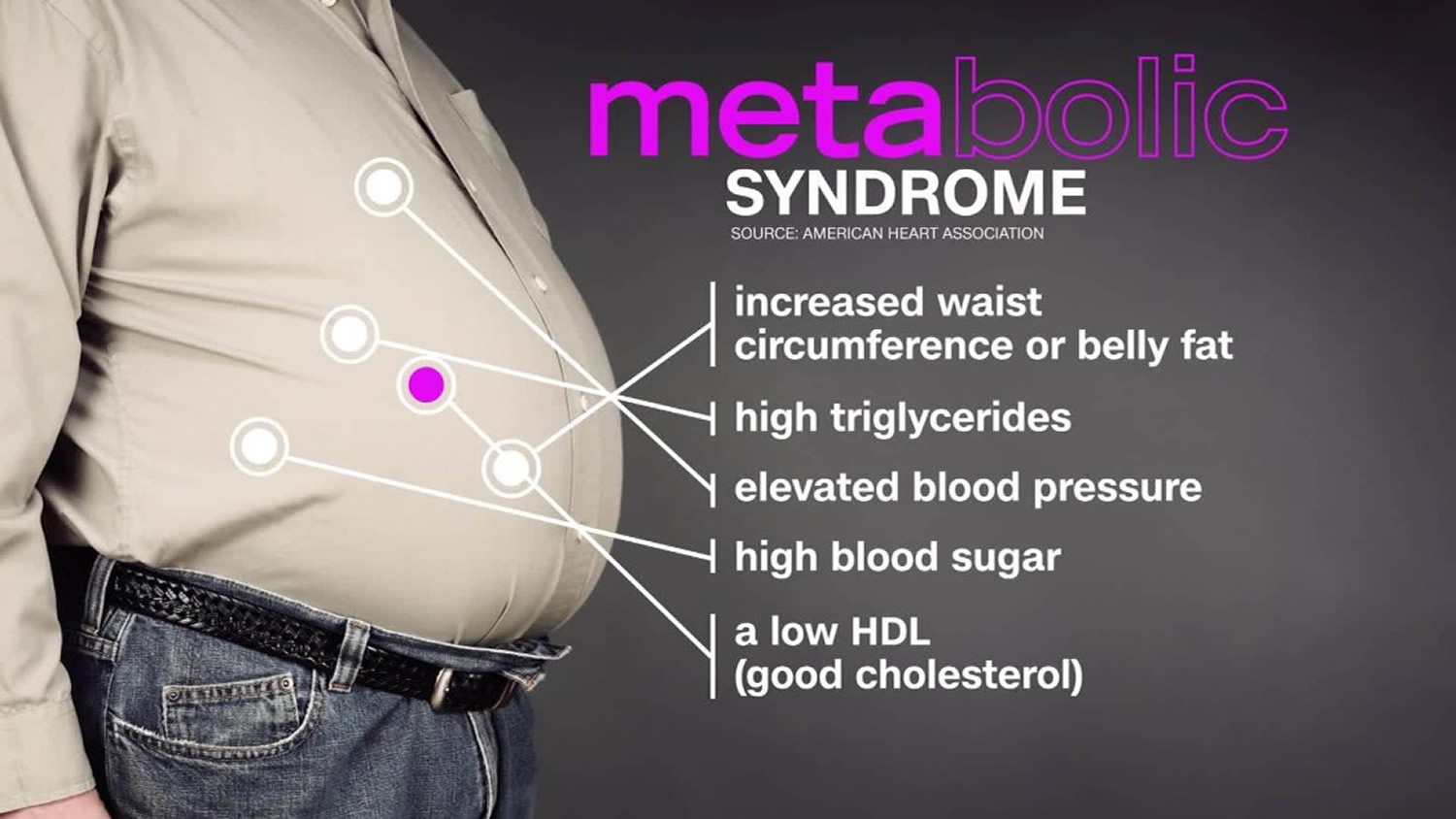
Metabolic Syndrome is linked to heart disease and diabetes
Sixteen million Americans have heart disease, which is the #1 killer in the United States. Growing scientific evidence is helping identify the various ways that sugar is implicated. We know that metabolic syndrome is a strong predictor of heart disease. Consuming too many added sugars also can lead to excess weight gain, which strains the heart.
Diabetes, which affects 25.8 million Americans, is of equal concern to public health. Diabetes can cause kidney failure, lower-limb amputations, and blindness, and doubles the risk of colon and pancreatic cancers. Diabetes is strongly associated with coronary artery disease and Alzheimer’s disease. It’s also a discriminatory disease: compared to white adults, the risk of being diagnosed with diabetes is 18% higher among Asian Americans, 66% higher among Hispanics and 77% higher among African-Americans.
Metabolic Syndrome Treatment
It is possible to prevent or delay metabolic syndrome, mainly with lifestyle changes. Treating metabolic syndrome requires addressing several conditions together. A healthy lifestyle is a lifelong commitment. Improving your overall cardiovascular health will greatly improve the individual conditions that make up metabolic syndrome. Successfully controlling metabolic syndrome requires long-term effort and teamwork with your health care providers.
Heart-healthy lifestyle changes are the first line of treatment for metabolic syndrome. If heart-healthy lifestyle changes aren’t enough, your doctor may prescribe medicines. Medicines are used to treat and control risk factors, such as high blood pressure, high triglycerides, low HDL (“good”) cholesterol, and high blood sugar.
Goals of Treatment
- The major goal of treating metabolic syndrome is to reduce the risk of coronary heart disease. Treatment is directed first at lowering LDL cholesterol and high blood pressure and managing diabetes (if these conditions are present).
- The second goal of treatment is to prevent the onset of type 2 diabetes, if it hasn’t already developed. Long-term complications of diabetes often include heart and kidney disease, vision loss, and foot or leg amputation. If diabetes is present, the goal of treatment is to reduce your risk for heart disease by controlling all of your risk factors.
Heart-Healthy Lifestyle Changes
Heart-healthy lifestyle changes include heart-healthy eating, aiming for a healthy weight, managing stress, physical activity, and quitting smoking.
Here’s what you can do starting today 11 :
- Eat better. Heart-healthy eating includes a diet rich in whole grains, fruits, vegetables, lean meats and fish, and low-fat or fat-free dairy products and avoid processed food, which often contains partially hydrogenated vegetable oils, and is high in salt and added sugar.
- Get active. Incorporate at least 150 minutes of moderately vigorous physical activity into your weekly routine. Walking is the easiest place to start, but you may want to experiment to find something else you like to do that gets your heart rate up. If needed, break your exercise up into several short, 10-minute sessions throughout the day to reach your goal.
- Lose weight. Aiming for a healthy weight. Reduce your risk for heart disease by successfully losing weight and keeping it off. Learn your recommended calorie intake, the amount of food calories you’re consuming, and the energy calories you’re burning off with different levels of physical activity. Balance healthy eating with a healthy level of exercise to reach your goals.
- Managing stress.
- Quitting smoking. The chemicals in tobacco smoke harm your blood cells. They also can damage the function of your heart and the structure and function of your blood vessels. Smoking is a major risk factor for heart disease. When combined with other risk factors—such as unhealthy blood cholesterol levels, high blood pressure, and overweight or obesity—smoking further raises the risk of heart disease.
Lifestyle changes can help you control your risk factors and reduce your risk for coronary heart disease and diabetes.
If you already have heart disease or diabetes, lifestyle changes can help you prevent or delay related problems. Examples of these problems include heart attack, stroke, and diabetes-related complications (for example, damage to your eyes, nerves, kidneys, feet, and legs).
If lifestyle changes aren’t enough, your doctor may recommend medicines. Take all of your medicines as prescribed by your doctor. Make realistic short- and long-term goals for yourself when you begin to make healthy lifestyle changes. Work closely with your doctor, and seek regular medical care.
When changes in lifestyle alone do not control the conditions related to metabolic syndrome, your health practitioner may prescribe medications to control blood pressure, cholesterol, and other symptoms. Carefully following your practitioner’s instructions can help prevent many of the long term effects of metabolic syndrome. Every step counts and your hard work and attention to these areas will make a difference in your health!
Medicines
Sometimes lifestyle changes aren’t enough to control your risk factors for metabolic syndrome. For example, you may need statin medications to control or lower your cholesterol. By lowering your blood cholesterol level, you can decrease your chance of having a heart attack or stroke. Doctors usually prescribe statins for people who have:
- Diabetes
- Heart disease or had a prior stroke
- High LDL cholesterol levels
Doctors may discuss beginning statin treatment with those who have an elevated risk for developing heart disease or having a stroke.
Your doctor also may prescribe other medications to:
- Decrease your chance of having a heart attack or dying suddenly.
- Lower your blood pressure.
- Prevent blood clots, which can lead to heart attack or stroke.
- Reduce your heart’s workload and relieve symptoms of coronary heart disease.
Take all medicines regularly, as your doctor prescribes. Don’t change the amount of your medicine or skip a dose unless your doctor tells you to. You should still follow a heart-healthy lifestyle, even if you take medicines to treat your risk factors for metabolic syndrome.
Metabolic Syndrome Diet
The Dietary Approaches to Stop Hypertension (DASH) diet and the Mediterranean diet, like many healthy-eating plans, limit unhealthy fats and emphasize fruits, vegetables, fish and whole grains. Both dietary approaches have been found to offer important health benefits — in addition to weight loss — for people who have components of metabolic syndrome 12.
- The Dietary Approaches to Stop Hypertension (DASH) Diet 13
The DASH diet is a lifelong approach to healthy eating that’s designed to help treat or prevent high blood pressure (hypertension). The DASH diet encourages you to reduce the sodium in your diet and eat a variety of foods rich in nutrients that help lower blood pressure, such as potassium, calcium and magnesium.
By following the DASH diet, you may be able to reduce your blood pressure by a few points in just two weeks. Over time, your systolic blood pressure could drop by eight to 14 points, which can make a significant difference in your health risks.
Because the DASH diet is a healthy way of eating, it offers health benefits besides just lowering blood pressure. The DASH diet is also in line with dietary recommendations to prevent osteoporosis, cancer, heart disease, stroke and diabetes.
DASH diet: Sodium levels
The DASH diet emphasizes vegetables, fruits and low-fat dairy foods — and moderate amounts of whole grains, fish, poultry and nuts.
In addition to the standard DASH diet, there is also a lower sodium version of the diet. You can choose the version of the diet that meets your health needs:
- Standard DASH diet. You can consume up to 2,300 milligrams (mg) of sodium a day.
- Lower sodium DASH diet. You can consume up to 1,500 mg of sodium a day.
The American Heart Association recommends 1,500 mg a day of sodium as an upper limit for all adults. If you aren’t sure what sodium level is right for you, talk to your doctor.
Both versions of the DASH diet aim to reduce the amount of sodium in your diet compared with what you might get in a typical American diet, which can amount to a whopping 3,400 mg of sodium a day or more.
The standard DASH diet meets the recommendation from the Dietary Guidelines for Americans to keep daily sodium intake to less than 2,300 mg a day.
DASH diet: What to eat
Both versions of the DASH diet include lots of whole grains, fruits, vegetables and low-fat dairy products. The DASH diet also includes some fish, poultry and legumes, and encourages a small amount of nuts and seeds a few times a week.
You can eat red meat, sweets and fats in small amounts. The DASH diet is low in saturated fat, cholesterol and total fat.
Here’s a look at the recommended servings from each food group for the 2,000-calorie-a-day DASH diet.
- Grains: 6 to 8 servings a day
Grains include bread, cereal, rice and pasta. Examples of one serving of grains include 1 slice whole-wheat bread, 1 ounce dry cereal, or 1/2 cup cooked cereal, rice or pasta.
Focus on whole grains because they have more fiber and nutrients than do refined grains. For instance, use brown rice instead of white rice, whole-wheat pasta instead of regular pasta and whole-grain bread instead of white bread. Look for products labeled “100 percent whole grain” or “100 percent whole wheat.”
Grains are naturally low in fat. Keep them this way by avoiding butter, cream and cheese sauces.
- Vegetables: 4 to 5 servings a day
Tomatoes, carrots, broccoli, sweet potatoes, greens and other vegetables are full of fiber, vitamins, and such minerals as potassium and magnesium. Examples of one serving include 1 cup raw leafy green vegetables or 1/2 cup cut-up raw or cooked vegetables.
Don’t think of vegetables only as side dishes — a hearty blend of vegetables served over brown rice or whole-wheat noodles can serve as the main dish for a meal.
Fresh and frozen vegetables are both good choices. When buying frozen and canned vegetables, choose those labeled as low sodium or without added salt.
To increase the number of servings you fit in daily, be creative. In a stir-fry, for instance, cut the amount of meat in half and double up on the vegetables.
- Fruits: 4 to 5 servings a day
Many fruits need little preparation to become a healthy part of a meal or snack. Like vegetables, they’re packed with fiber, potassium and magnesium and are typically low in fat — coconuts are an exception. Examples of one serving include one medium fruit, 1/2 cup fresh, frozen or canned fruit, or 4 ounces of juice.
Have a piece of fruit with meals and one as a snack, then round out your day with a dessert of fresh fruits topped with a dollop of low-fat yogurt. Leave on edible peels whenever possible. The peels of apples, pears and most fruits with pits add interesting texture to recipes and contain healthy nutrients and fiber. Remember that citrus fruits and juices, such as grapefruit, can interact with certain medications, so check with your doctor or pharmacist to see if they’re okay for you.
If you choose canned fruit or juice, make sure no sugar is added.
- Dairy: 2 to 3 servings a day
Milk, yogurt, cheese and other dairy products are major sources of calcium, vitamin D and protein. But the key is to make sure that you choose dairy products that are low fat or fat-free because otherwise they can be a major source of fat — and most of it is saturated. Examples of one serving include 1 cup skim or 1 percent milk, 1 cup low fat yogurt, or 1 1/2 ounces part-skim cheese.
Low-fat or fat-free frozen yogurt can help you boost the amount of dairy products you eat while offering a sweet treat. Add fruit for a healthy twist.
If you have trouble digesting dairy products, choose lactose-free products or consider taking an over-the-counter product that contains the enzyme lactase, which can reduce or prevent the symptoms of lactose intolerance.
Go easy on regular and even fat-free cheeses because they are typically high in sodium.
- Lean meat, poultry and fish: 6 servings or fewer a day
Meat can be a rich source of protein, B vitamins, iron and zinc. Choose lean varieties and aim for no more than 6 ounces a day. Cutting back on your meat portion will allow room for more vegetables.
Trim away skin and fat from poultry and meat and then bake, broil, grill or roast instead of frying in fat.
Eat heart-healthy fish, such as salmon, herring and tuna. These types of fish are high in omega-3 fatty acids, which can help lower your total cholesterol.
- Nuts, seeds and legumes: 4 to 5 servings a week
Almonds, sunflower seeds, kidney beans, peas, lentils and other foods in this family are good sources of magnesium, potassium and protein. They’re also full of fiber and phytochemicals, which are plant compounds that may protect against some cancers and cardiovascular disease.
Serving sizes are small and are intended to be consumed only a few times a week because these foods are high in calories. Examples of one serving include 1/3 cup nuts, 2 tablespoons seeds, or 1/2 cup cooked beans or peas.
Nuts sometimes get a bad rap because of their fat content, but they contain healthy types of fat — monounsaturated fat and omega-3 fatty acids. They’re high in calories, however, so eat them in moderation. Try adding them to stir-fries, salads or cereals.
Soybean-based products, such as tofu and tempeh, can be a good alternative to meat because they contain all of the amino acids your body needs to make a complete protein, just like meat.
- Fats and oils: 2 to 3 servings a day
Fat helps your body absorb essential vitamins and helps your body’s immune system. But too much fat increases your risk of heart disease, diabetes and obesity. The DASH diet strives for a healthy balance by limiting total fat to less than 30 percent of daily calories from fat, with a focus on the healthier monounsaturated fats.
Examples of one serving include 1 teaspoon soft margarine, 1 tablespoon mayonnaise or 2 tablespoons salad dressing.
Saturated fat and trans fat are the main dietary culprits in increasing your risk of coronary artery disease. DASH helps keep your daily saturated fat to less than 6 percent of your total calories by limiting use of meat, butter, cheese, whole milk, cream and eggs in your diet, along with foods made from lard, solid shortenings, and palm and coconut oils.
Avoid trans fat, commonly found in such processed foods as crackers, baked goods and fried items.
Read food labels on margarine and salad dressing so that you can choose those that are lowest in saturated fat and free of trans fat.
- Sweets: 5 servings or fewer a week
You don’t have to banish sweets entirely while following the DASH diet — just go easy on them. Examples of one serving include 1 tablespoon sugar, jelly or jam, 1/2 cup sorbet, or 1 cup lemonade.
When you eat sweets, choose those that are fat-free or low-fat, such as sorbets, fruit ices, jelly beans, hard candy, graham crackers or low-fat cookies.
Artificial sweeteners such as aspartame (NutraSweet, Equal) and sucralose (Splenda) may help satisfy your sweet tooth while sparing the sugar. But remember that you still must use them sensibly. It’s OK to swap a diet cola for a regular cola, but not in place of a more nutritious beverage such as low-fat milk or even plain water.
- Cut back on added sugar, which has no nutritional value but can pack on calories.
DASH diet: Alcohol and caffeine
Drinking too much alcohol can increase blood pressure. The Dietary Guidelines for Americans recommends that men limit alcohol to no more than two drinks a day and women to one or less.
The DASH diet doesn’t address caffeine consumption. The influence of caffeine on blood pressure remains unclear. But caffeine can cause your blood pressure to rise at least temporarily. If you already have high blood pressure or if you think caffeine is affecting your blood pressure, talk to your doctor about your caffeine consumption.
- Ford ES, Giles WH, Dietz WH. Prevalence of the metabolic syndrome among US adults: findings from the third National Health and Nutrition Examination Survey. JAMA. 2002;287:356–359. [↩]
- Circulation. 2003 Jul 29;108(4):414-9. Epub 2003 Jul 14. Metabolic syndrome with and without C-reactive protein as a predictor of coronary heart disease and diabetes in the West of Scotland Coronary Prevention Study. https://www.ncbi.nlm.nih.gov/pubmed/12860911[↩]
- Diabetes Care. 2001 Apr;24(4):683-9. Cardiovascular morbidity and mortality associated with the metabolic syndrome. https://www.ncbi.nlm.nih.gov/pubmed/11315831[↩]
- National Institutes of Health. National Heart, Lung and Blood Institute. What Is Metabolic Syndrome ? – https://www.nhlbi.nih.gov/health/health-topics/topics/ms/[↩]
- Mayo Foundation for Medical Education and Research. Metabolic Syndrome (MetS) Study and Prevention. – http://www.mayo.edu/research/labs/renovascular-disease/research-activities/metabolic-syndrome-study-and-prevention[↩]
- JAMA. 2002 Jan 16;287(3):356-9. Prevalence of the metabolic syndrome among US adults: findings from the third National Health and Nutrition Examination Survey. https://www.ncbi.nlm.nih.gov/pubmed/11790215[↩]
- National Institutes of Health. National Heart, Lung and Blood Institute. What Causes Metabolic Syndrome ? – https://www.nhlbi.nih.gov/health/health-topics/topics/ms/causes[↩]
- American Heart Association. Your Risk for Metabolic Syndrome, Updated:Sep 15,2016. http://www.heart.org/HEARTORG/Conditions/More/MetabolicSyndrome/Your-Risk-for-Metabolic-Syndrome_UCM_301924_Article.jsp[↩]
- National Institutes of Health. National Heart, Lung and Blood Institute. What Is Metabolic Syndrome ?. https://www.nhlbi.nih.gov/health/health-topics/topics/ms/[↩]
- https://www.nhlbi.nih.gov/health-pro/guidelines/in-develop/cardiovascular-risk-reduction/risk-assessment/[↩]
- American Heart Association. Prevention and Treatment of Metabolic Syndrome, Updated:Sep 15,2016. http://www.heart.org/HEARTORG/Conditions/More/MetabolicSyndrome/Prevention-and-Treatment-of-Metabolic-Syndrome_UCM_301927_Article.jsp[↩]
- Mayo Foundation for Medical Education and Research. Metabolic syndrome – Lifestyle and home remedies. – http://www.mayoclinic.org/diseases-conditions/metabolic-syndrome/manage/ptc-20197547[↩]
- Mayo Foundation for Medical Education and Research. Healthy Lifestyle: Nutrition and healthy eating. – http://www.mayoclinic.org/healthy-lifestyle/nutrition-and-healthy-eating/in-depth/dash-diet/art-20048456?pg=2[↩]