Contents
What is thrombophlebitis
Thrombophlebitis is a general term for “inflammation of the veins.” The vein becomes inflamed because there is blood clotting inside it or the vein walls are damaged. Blood clots (i.e. thrombosis) can form and block one or more veins, usually in your legs. The affected vein might be near the surface of your skin (superficial thrombophlebitis) or deep within a muscle (deep vein thrombosis, or DVT). Thrombophlebitis causes include trauma, surgery or prolonged inactivity.
Thrombophlebitis may affect deeper, larger veins or veins near the skin surface. Most of the time, thrombophlebitis occurs in the pelvis and legs.
DVT (deep vein thrombosis) increases your risk of serious health problems. It’s usually treated with blood-thinning medications. Superficial thrombophlebitis is sometimes treated with blood-thinning medications, too.
See your doctor right away if you have a red, swollen or tender vein — especially if you have one or more risk factors for thrombophlebitis.
Seek immediate medical attention if you have pain, swelling and tenderness in your leg, and you develop breathlessness and chest pain, go to an emergency room. These might indicate that you have a dislodged blood clot traveling through your veins to your lungs (pulmonary embolism).
Superficial thrombophlebitis
Superficial thrombophlebitis, inflammation of superficial veins associated with thrombosis (blood clot), is a painful condition and ~3 to 11% of the population will develop superficial thrombophlebitis during their lifetime 1. Although generally considered a benign, self-limited disease, superficial thrombophlebitis can cause considerable discomfort, impact mobility and lead to further complications. Recent and accumulating evidence suggests that superficial thrombophlebitis is often associated with more serious forms of venous thromboembolism (VTE), including deep vein thrombosis (DVT) and pulmonary embolism (PE) and superficial thrombophlebitis is a strong risk factor for subsequent DVT or PE 2.
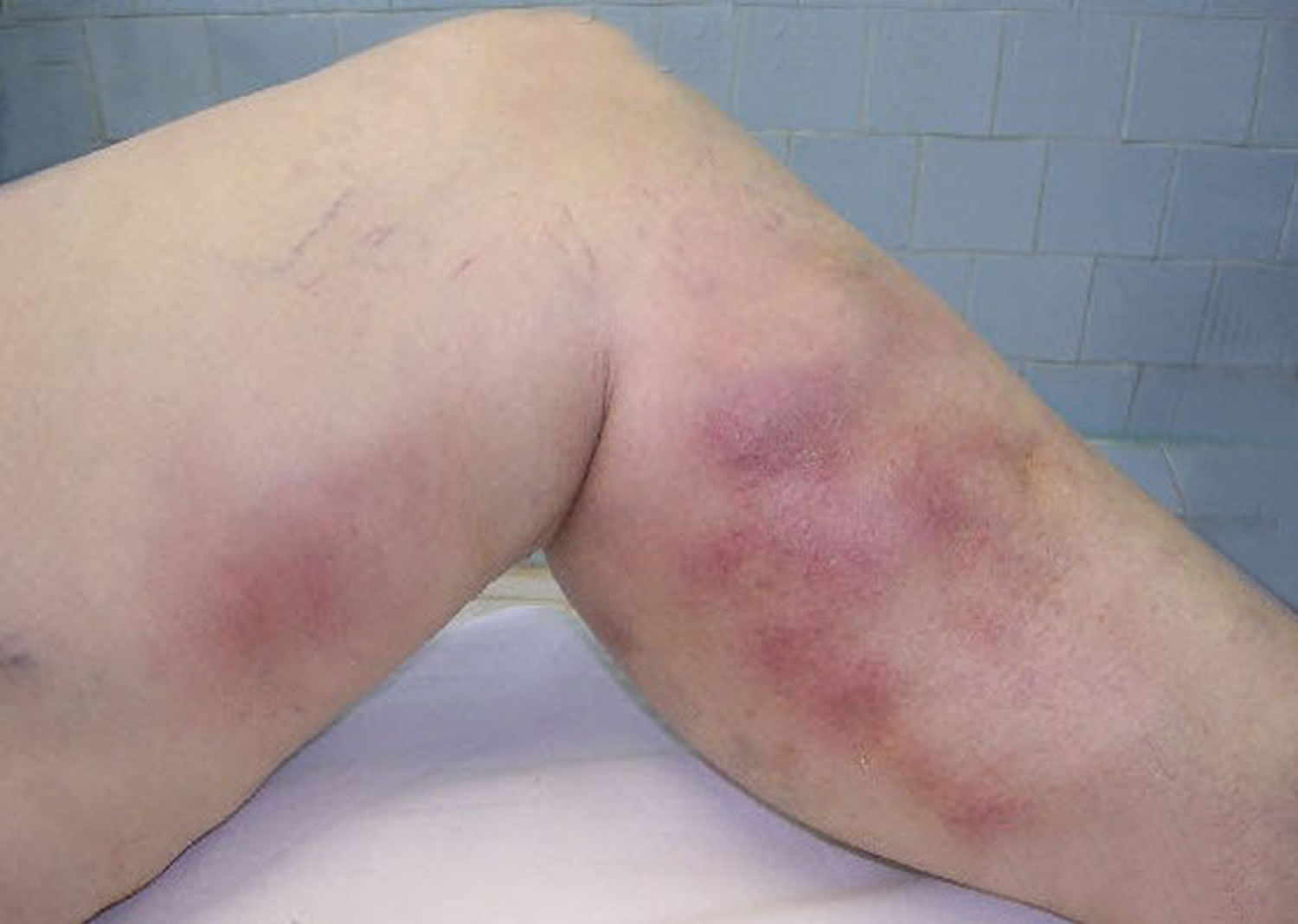
Figure 1. Superficial thrombophlebitis
Superficial thrombophlebitis may occur after injury to the vein (which can result from trauma, infection, or inflammation) or stagnant or turbulent bloodflow (often found in varicose veins). Or it may occur after having medicines given into your veins. If you have a high risk for blood clots, you may develop superficial thrombophlebitis for no apparent reason.
Superficial thrombophlebitis is typically more annoying than serious. Usually, the blood clot clears and the inflammation dies down within a few weeks.
Most people with superficial thrombophlebitis are otherwise well. There shouldn’t be any foul discharge or abscess, and it’s normally just lumps under the skin rather than swelling of the whole calf.
This may be painful, but it shouldn’t prevent you walking reasonably well.
When the inflammation settles, you may be left with darkened skin and the lump may take three or four months to go. But most people make a full recovery.
If the thrombophlebitis occurred in a varicose vein, it’s likely that the varicose veins will keep coming back, possibly with further episodes of thrombophlebitis.
This is because there’s a basic problem with the vein, and you may need this removing.
You’re more at risk of superficial thrombophlebitis if you:
- have varicose veins
- smoke
- are very overweight
- infection
- use of birth control pills or HRT (although these only slightly increase your risk of blood clots)
- are pregnant
- have had a previous blood clot or other problem with the vein
- deep vein thrombosis (DVT)
- have recently had injections or a drip put into the vein
- have a condition that causes the blood to clot more easily, such as thrombophilia, polyarteritis (inflammation of the smaller arteries) or polycythaemia (a
- high concentration of red blood cells in your blood)
- have cancer
- liver disease
- sitting or staying still for a prolonged period
Symptoms may include any of the following:
- Skin redness, inflammation, tenderness, or pain along a vein just below the skin
- Warmth of the area
- Limb pain
- Hardening of the vein
Superficial thrombophlebitis possible complications
Complications are rare. Possible problems may include the following:
- Infections (cellulitis). Conversion into a infected form of phlebitis known as septic thrombophlebitis.
- Deep vein thrombosis (DVT)
There’s a small chance of the blood clot traveling along the vein to where it meets a deeper vein, and a DVT developing. This is more likely if the surface clot extends into the upper thigh or groin, or behind the knee (in places where superficial veins meet deeper veins).
It’s also more likely to occur if the affected vein is a normal vein rather than a varicose vein, if you’ve had a DVT before, or if you’re immobile.
A DVT can cause pain, swelling and a heavy ache in your leg and and possible pulmonary embolism – see your doctor immediately if you experience these symptoms.
Superficial thrombophlebitis prevention
In the hospital, swollen or inflamed veins can be prevented by:
- The nurse regularly changing the location of your IV line and removing it if swelling, redness, or pain develop
- Walking and staying active as soon as possible after surgery or during a long-term illness
When possible, avoid keeping your legs and arms still for long periods. Move your legs often or take a stroll during long plane trips or car trips. Try to avoid sitting or lying down for long periods without getting up and moving about.
Superficial thrombophlebitis diagnosis
Your health care provider will diagnose this condition based mainly on the appearance of the affected area. Frequent checks of the pulse, blood pressure, temperature, skin condition, and blood flow may be needed.
Ultrasound of the blood vessels helps confirm the condition.
If there are signs of an infection, skin or blood cultures may be done.
Superficial thrombophlebitis treatment
There is no clear consensus on the optimal treatment of superficial thrombophlebitis. Although antithrombotic medications such as fondaparinux (2.5 mg/d for 45 days) may be more effective than placebo in reducing the risk of subsequent DVT 3, the evidence is generally of low grade and the costs and inconveniences of anticoagulant therapy are not inconsequential 4. Surveys suggest that physician opinions on the appropriate management of superficial thrombophlebitis vary significantly and management includes non-steroidal anti-inflammatory drugs (NSAIDs), topical therapies, or watchful waiting 5.
To reduce discomfort and swelling, your provider may recommend that you:
- Wear support stockings, if your leg is affected.
- Keep the affected leg or arm raised above heart level.
- Apply a warm compress to the area.
- Keep active to keep the blood circulating
- Rub an anti-inflammatory cream or gel on the area if the affected area is only small
If you have a catheter or IV line, it will likely be removed if it is the cause of the thrombophlebitis.
Medicines called NSAIDs, such as ibuprofen, may be prescribed to reduce pain and swelling.
If clots in the deeper veins are also present, your provider may prescribe medicines to thin your blood. These medicines are called anticoagulants. Antibiotics are prescribed if you have an infection.
Surgical removal (phlebectomy), stripping, or sclerotherapy of the affected vein may be needed. These treat large varicose veins or to prevent thrombophlebitis in high-risk people.
Superficial thrombophlebitis treatment guidelines
American College of Chest Physicians Recommendations 6
- In patients with superficial thrombophlebitis of the lower limb of at least 5 cm in length, the American College of Chest Physicians suggest the use of a prophylactic dose of fondaparinux or low-molecular-weight heparin (LMWH) for 45 days over no anticoagulation (Grade 2B).
Remarks: Patients who place a high value on avoiding the inconvenience or cost of anticoagulation and a low value on avoiding infrequent symptomatic venous thromboembolism (VTE) are likely to decline anticoagulation.
- In patients with superficial thrombophlebitis who are treated with anticoagulation, the American College of Chest Physicians suggest fondaparinux 2.5 mg daily over a prophylactic dose of low-molecular-weight heparin (LMWH) (Grade 2C).
Notes: Strong (Grade 1) and weak (Grade 2) recommendations based on high-quality (Grade A), moderate-quality (Grade B), and low-quality (Grade C) evidence.
Migratory thrombophlebitis
Superfcial migratory thrombophlebitis is a commonly missed sign of malignancy (cancer) and rates of misdiagnosing it as cellulitis are estimated to be as high as 28 percent in hospital settings 7. There is a broad differential for erythematous skin, including cellulitis, but also many clinical mimickers that can be broadly described as pseudocellulitis. Outpatient diagnoses, such as lymphedematous rubor, dependent rubor, psoriasis, stasis dermatitis, stasis panniculitis, and pigmented purpuric eruptions, and superfcial migratory thrombophlebitis, are characteristic forms of pseudocellulitis 8. These cases are treated differently than cases of cellulitis. Treating pseudocellulitis with antibiotics, as is typical in the case of a cellulitis, could lead to antimicrobial resistance, hospital overuse, and a delay in proper treatment. Dermatologist expertise is often required for identification and proper treatment 9, as misdiagnosis by nondermatologist physicians is all too common 7.
Serpiginous cord morphology and cord-like palpability are distinguishing features of superficial migratory thrombophlebitis 10. Additionally, superficial migratory thrombophlebitis preferentially afflicts the small and great saphenous veins of the lower extremities but can have a diffuse migrational distribution as well 11. The linear or serpiginous pattern of the purpura and palpable cord-like nodules, and the combination of both, almost certainly indicates superficial thrombophlebitis. The distinct linear serpiginous cords and palpability are caused by a hypercoagulable state (conferred by tissue), cancer procoagulants activating coagulation factor VII, and leukocytotic sludging 11. Cancers that are commonly seen in clinic in association with superficial migratory thrombophlebitis are pancreatic cancer, other gastrointestinal cancers, and various leukemias 11.
Up to 30 percent of cases are detected only after a follow-up venous duplex scans 12. Therefore, knowledge of the diagnostic test and its limitations is critical. Patients were usually admitted with a primary diagnosis of cellulitis, not because superficial migratory thrombophlebitis was not considered, but rather because the diagnostic test did not support it. Venous duplex scans results are technician-dependent. Superficial migratory thrombophlebitis might be missed due to the following errors: failure to maximize venous pressure via patient positioning, lack of appropriate transducer frequency (7–12MHz), venous constriction secondary to cold room temperatures, and/or incorrect transducer positioning 13. Additionally, miscommunication could also contribute to diagnostic errors. Ultrasound technicians are often unaware that a patient has suspected superficial migratory thrombophlebitis and, due to this miscommunication, the technicians fail to perform venous duplex scans within the affected inflammed area. Furthermore, technicians might be hesitant to apply transducer pressure over the superficial migratory thrombophlebitis due to patient pain. Technicians also do not generally evaluate the small saphenous vein without a specific request.
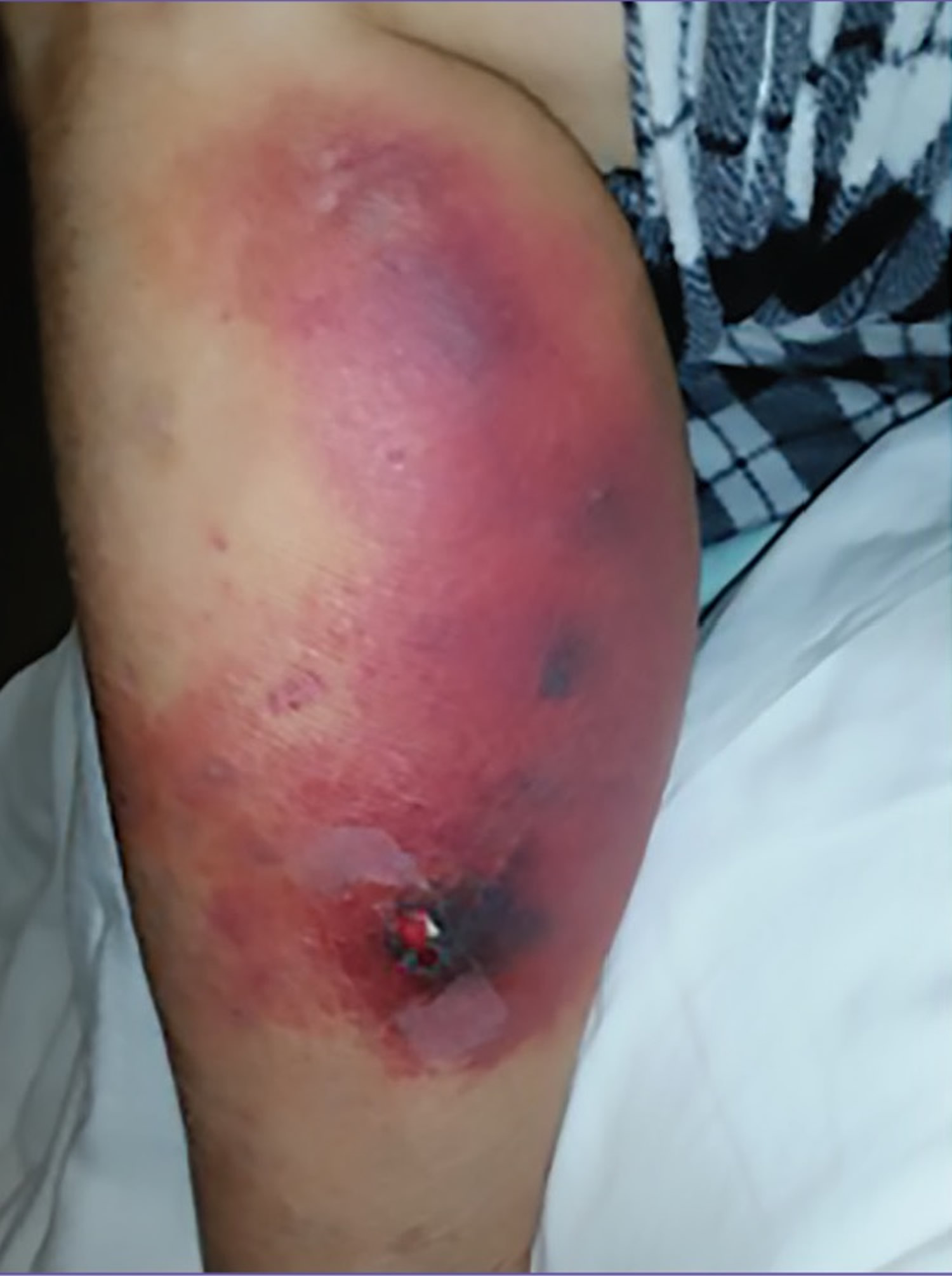
Figure 2. Superfcial migratory thrombophlebitis
Thrombophlebitis vs DVT
Deep vein thrombosis (DVT) is a blood clot that develops within a deep vein in the body, usually in the leg.
Blood clots that develop in a vein are also known as venous thrombosis.
DVT usually occurs in a deep leg vein, a larger vein that runs through the muscles of the calf and the thigh.
It can cause pain and swelling in the leg and may lead to complications such as pulmonary embolism. This is a serious condition that occurs when a piece of blood clot breaks off into the bloodstream and blocks one of the blood vessels in the lungs (see below).
DVT and pulmonary embolism together are known as venous thromboembolism (VTE).
Symptoms of DVT
In some cases, there may be no symptoms of DVT. If symptoms do occur they can include:
- pain, swelling and tenderness in one of your legs (usually your calf)
- a heavy ache in the affected area
- warm skin in the area of the clot
- red skin, particularly at the back of your leg below the knee
DVT usually (although not always) affects one leg. The pain may be worse when you bend your foot upward towards your knee.
Pulmonary embolism
If left untreated, about 1 in 10 people with a DVT will develop a pulmonary embolism. A pulmonary embolism is a very serious condition that causes:
- breathlessness – which may come on gradually or suddenly
- chest pain – which may become worse when you breathe in
- sudden collapse
Both DVT and pulmonary embolism require urgent investigation and treatment.
Anyone can develop DVT, but it becomes more common over the age of 40. As well as age, there are also a number of other risk factors, including:
- having a history of DVT or pulmonary embolism
- having a family history of blood clots
- being inactive for long periods – such as after an operation or during a long journey
- blood vessel damage – a damaged blood vessel wall can result in the formation of a blood clot
- having certain conditions or treatments that cause your blood to clot more easily than normal – such as cancer (including chemotherapy and radiotherapy
- treatment), heart and lung disease, thrombophilia and Hughes syndrome
- being pregnant – your blood also clots more easily during pregnancy
- being overweight or obese
The combined contraceptive pill and hormone replacement therapy (HRT) both contain the female hormone oestrogen, which causes the blood to clot more easily. If you’re taking either of these, your risk of developing DVT is slightly increased.
Preventing DVT
If you need to go into hospital for surgery, a member of your care team will assess your risk of developing a blood clot while you’re there.
If you’re at risk of developing DVT, there are a number of things you can do to prevent a blood clot occurring, both before you go into hospital, such as temporarily stopping taking the combined contraceptive pill, and while you’re in hospital, such as wearing compression stockings.
When you leave hospital, your care team may also make a number of recommendations to help prevent DVT returning or complications developing. These may include:
- not smoking
- eating a healthy, balanced diet
- taking regular exercise
- maintaining a healthy weight or losing weight if you’re obese
There’s no evidence to suggest that taking aspirin reduces your risk of developing DVT.
See your doctor before embarking on long-distance travel if you’re at risk of getting DVT, or if you’ve had DVT in the past.
When taking a long-distance journey (six hours or more) by plane, train or car, you should take steps to avoid getting DVT, such as drinking plenty of water, performing simple leg exercises and taking regular, short walking breaks.
Diagnosing DVT
- D-dimer test
It can be difficult to diagnose DVT from symptoms alone, so your doctor may advise that you have a specialised blood test called a D-dimer test.
This test detects pieces of blood clot that have been broken down and are loose in your bloodstream. The larger the number of fragments found, the more likely it is that you have a blood clot in your vein.
However, the D-dimer test isn’t always reliable because blood clot fragments can increase after an operation, injury or during pregnancy. Additional tests, such as an ultrasound scan, will need to be carried out to confirm DVT.
- Ultrasound scan
An ultrasound scan can be used to detect clots in your veins. A special type of ultrasound called a Doppler ultrasound can also be used to find out how fast the blood is flowing through a blood vessel. This helps doctors identify when blood flow is slowed or blocked, which could be caused by a blood clot.
- Venogram
A venogram may be used if the results of a D-dimer test and ultrasound scan can’t confirm a diagnosis of DVT.
During a venogram, a liquid called a contrast dye is injected into a vein in your foot. The dye travels up the leg and can be detected by X-ray, which will highlight a gap in the blood vessel where a clot is stopping the flow of blood.
DVT treatment
Treatment for DVT usually involves taking anticoagulant medicines, which reduce the blood’s ability to clot and stop existing clots getting bigger.
Heparin and warfarin are two types of anticoagulant often used to treat DVT. Heparin is usually prescribed first because it works immediately to prevent further clotting. After initial treatment, you may also need to take warfarin to prevent another blood clot forming.
A number of anticoagulants, known as directly acting oral anticoagulants (DOACs), may also be used to treat conditions such as DVT. These medications include rivaroxaban and apixaban, and they’ve been shown to be as effective as heparin and warfarin with less serious side effects.
Thrombophlebitis complications
Complications from superficial thrombophlebitis are rare. However, if you develop DVT, the risk of serious complications increases. Complications might include:
- Pulmonary embolism. If part of a deep vein clot becomes dislodged, it can travel to your lungs, where it can block an artery (embolism) and become potentially life-threatening.
- Post-phlebetic syndrome. This condition, also known as post-thrombotic syndrome, can develop months or even years after you’ve had DVT. Post-phlebetic syndrome can cause lasting and possibly disabling pain, swelling and a feeling of heaviness in the affected leg.
Thrombophlebitis causes
The cause of thrombophlebitis is a blood clot, which can form in your blood as a result of:
- An injury to a vein
- An inherited blood-clotting disorder
- Being immobile for long periods, such as during an injury or a hospital stay
Blood clots may form when something slows or changes the flow of blood in the veins.
Risk factors include:
- A pacemaker catheter that has been passed through the vein in the groin
- Bed rest or sitting in one position for too long such as plane travel
- Family history of blood clots
- Fractures in the pelvis or legs
- Giving birth within the last 6 months
- Pregnancy
- Obesity
- Recent surgery (most commonly hip, knee, or female pelvic surgery)
- Too many blood cells being made by the bone marrow, causing the blood to be thicker than normal (polycythemia vera)
- Having an indwelling (long-term) catheter in a blood vessel
Blood is more likely to clot in someone who has certain problems or disorders, such as:
- Cancer
- Certain autoimmune disorders, such as lupus
- Cigarette smoking
- Conditions that make it more likely to develop blood clots
- Taking estrogens or birth control pills (this risk is even higher with smoking)
Risk factors for thrombophlebitis
Your risk of thrombophlebitis increases if you:
- Are inactive for a prolonged period, either because you’re confined to bed or are traveling in a car or plane for a long period
- Have varicose veins, which are a common cause of superficial thrombophlebitis
- Have a pacemaker or have a thin, flexible tube (catheter) in a central vein, for treatment of a medical condition, which may irritate the blood vessel wall and decrease blood flow
- Are pregnant or have just given birth
- Use birth control pills or hormone replacement therapy, which can make your blood more likely to clot
- Have a family history of a blood-clotting disorder or a tendency to form blood clots
- Have had previous episodes of thrombophlebitis
- Have had a stroke
- Are older than 60
- Are overweight or obese
- Have cancer
- Smoke
If you have one or more risk factors, discuss prevention strategies with your doctor before taking long flights or road trips or if you’re planning to have elective surgery, recovery from which will require you not to move much.
Thrombophlebitis prevention
Sitting during a long flight or car ride can cause your ankles and calves to swell and increases your risk of thrombophlebitis. To help prevent a blood clot:
- Take a walk. If you’re flying or riding a train or bus, walk up and down the aisle once an hour or so. If you’re driving, stop every hour or so and move around.
- Move your legs regularly. Flex your ankles, or carefully press your feet against the floor or footrest in front of you at least 10 times each hour.
- Wear loose clothing.
- Drink plenty of nonalcoholic fluids to avoid dehydration.
Thrombophlebitis symptoms
Superficial thrombophlebitis signs and symptoms include:
- Warmth, tenderness and pain in the affected vein
- Redness and swelling in the part of the body affected
Deep vein thrombosis (DVT) signs and symptoms include:
- Pain in the part of the body affected
- Swelling in the part of the body affected
When a vein close to the surface of your skin is affected, you might see a red, hard cord just under the surface of your skin that’s tender to the touch. When a deep vein in the leg is affected, your leg may become swollen, tender and painful.
Thrombophlebitis diagnosis
To diagnose thrombophlebitis, your doctor will ask you about your discomfort and look for affected veins near your skin’s surface. To determine whether you have superficial thrombophlebitis or deep vein thrombosis, your doctor might choose one of these tests:
- Ultrasound. A wandlike device (transducer) moved over the affected area of your leg sends sound waves into your leg. As the sound waves travel through your leg tissue and reflect back, a computer transforms the waves into a moving image on a video screen. This test can confirm the diagnosis and distinguish between superficial and deep vein thrombosis.
- Blood test. Almost everyone with a blood clot has an elevated blood level of a naturally occurring, clot-dissolving substance called D dimer. But D dimer levels can be elevated in other conditions. So a test for D dimer isn’t conclusive, but can indicate the need for further testing. It’s also useful for ruling out DVT and for identifying people at risk of developing thrombophlebitis.
- Venography. For venography, a liquid called a contrast dye is injected into a vein in your foot. The dye travels up the leg and can be detected by X-ray image, which will highlight a gap in the blood vessel where a clot is stopping the flow of blood. The x ray will also show whether blood flow is slow in the vein, which may suggest a blood clot.
Thrombophlebitis treatment
For superficial thrombophlebitis, your doctor might recommend applying heat to the painful area, elevating the affected leg, using an over-the-counter nonsteroidal anti-inflammatory drug (NSAID) and possibly wearing compression stockings. The condition usually improves on its own.
Your doctor might also recommend these treatments for both types of thrombophlebitis:
Your provider may prescribe medicines such as:
- Painkillers
- Blood-thinning medications. If you have deep vein thrombosis, injection of a blood-thinning (anticoagulant) medication, such as low molecular weight heparin or fondaparinux (Arixtra), will prevent clots from enlarging. After the initial treatment, taking the oral anticoagulant warfarin (Coumadin, Jantoven, others) or the newer rivaroxaban (Xarelto) for several months continues to prevent clots from enlarging. If your doctor prescribes a blood thinner, follow directions carefully. Their most serious side effect can be excessive bleeding.
- Medicines such as ibuprofen to reduce pain and swelling
- Clot-dissolving medications. Treatment with medications such as alteplase (Activase) dissolves blood clots. Also known as thrombolysis, this treatment is used for extensive DVT, including some cases that involve a blood clot in the lungs (pulmonary embolus).
- Compression stockings. Prescription-strength compression stockings help prevent swelling and reduce the chances of complications of DVT.
- Filter. In some instances, especially if you can’t take blood thinners, a filter can be inserted into the main vein in your abdomen (vena cava) to prevent clots that break loose in leg veins from lodging in your lungs. Usually, the filter is removed when it’s no longer needed. If you have a filter placed, ask your doctor if and when it should be removed.
- Varicose vein stripping. Your doctor can surgically remove varicose veins that cause pain or recurrent thrombophlebitis in this procedure. It involves removing a long vein through small incisions. Removing the vein won’t affect circulation in your leg because veins deeper in the leg take care of the increased volumes of blood.
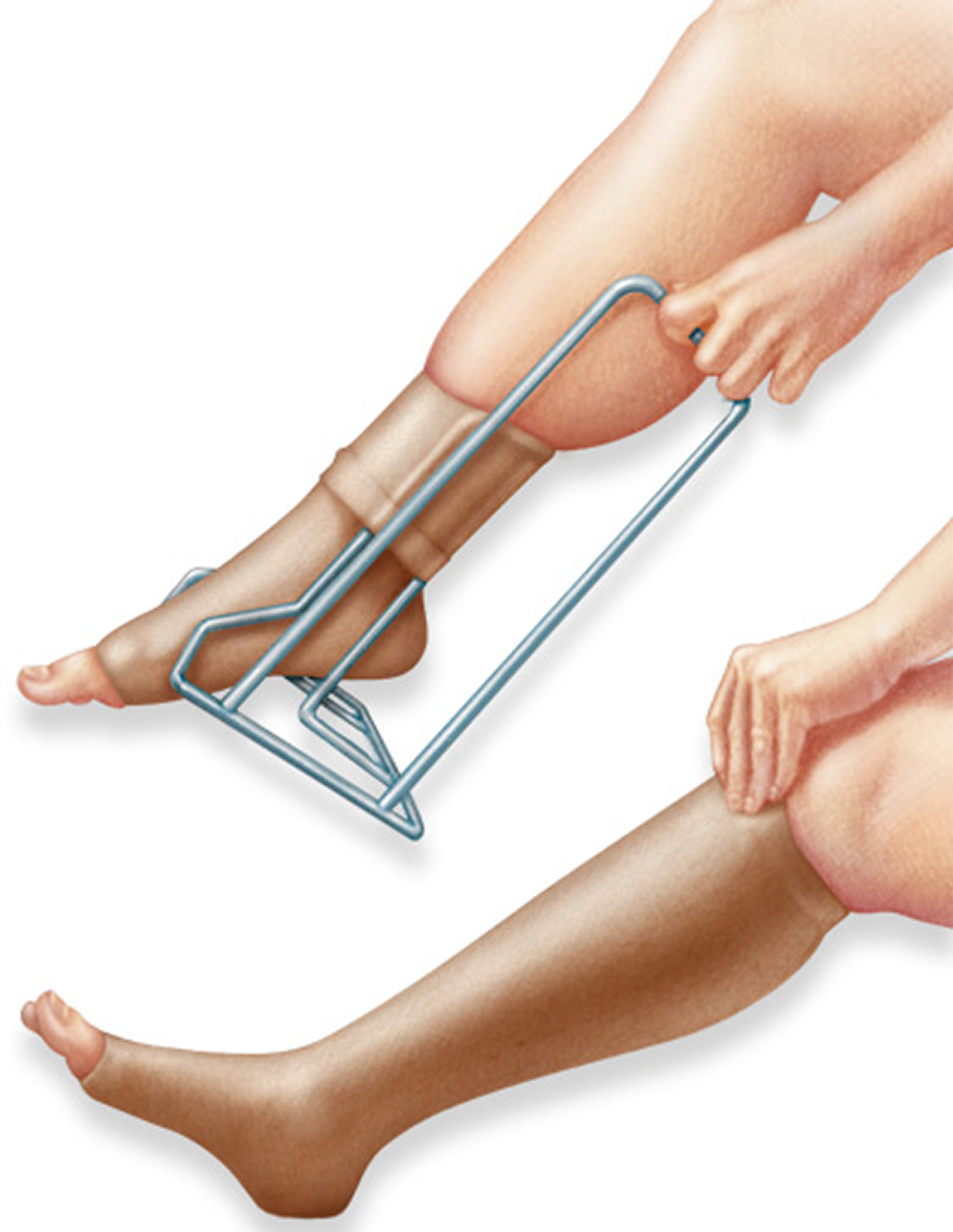
Figure 3. Support stockings or compression stockings, compress your legs, promoting circulation and wraps can help to reduce discomfort. A stocking butler may help you put on the stockings.
You may be told to do the following:
- Keep pressure off the area to reduce pain and decrease the risk of further damage.
- Raise the affected area to reduce swelling.
Rare treatment options are:
- Surgical removal of a vein near the surface
- Vein stripping
- Bypass of the vein
Home remedies
In addition to medical treatments, here are self-care measures to help improve thrombophlebitis.
If you have superficial thrombophlebitis:
- Use a warm washcloth to apply heat to the involved area several times daily
- Elevate your leg
- Use a nonsteroidal anti-inflammatory drug, such as ibuprofen (Advil, Motrin IB, others) or naproxen sodium (Aleve, others), if recommended by your doctor
If you have deep vein thrombosis:
- Take prescription anticoagulant medications as directed to prevent complications
- Elevate your leg if it’s swollen
- Wear your prescription compression stockings as directed
Let your doctor know if you’re taking another blood thinner, such as aspirin.
- Samuelson B, Go AS, Sung SH, Fan D, Fang MC. Initial Management and Outcomes after Superficial Thrombophlebitis: The CVRN VTE Study. Journal of hospital medicine. 2016;11(6):432-434. doi:10.1002/jhm.2553. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5138025/[↩]
- Cannegieter SC, Horvath-Puho E, Schmidt M, et al. Risk of venous and arterial thrombotic events in patients diagnosed with superficial vein thrombosis: a nationwide cohort study. Blood. 2015;125:229–35. http://www.bloodjournal.org/content/125/2/229.long[↩]
- Decousus H, Prandoni P, Mismetti P, et al. Fondaparinux for the treatment of superficial-vein thrombosis in the legs. N Engl J Med. 2010;363:1222–32. http://www.nejm.org/doi/full/10.1056/NEJMoa0912072[↩]
- Kearon C, Akl EA, Comerota AJ, et al. Chest. 9th ed. Vol. 141. American College of Chest Physicians Evidence-Based Clinical Practice Guidelines; 2012. Antithrombotic therapy for VTE disease: Antithrombotic Therapy and Prevention of Thrombosis; pp. e419S–94S. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3278049/[↩]
- Lane TR, Sritharan K, Herbert JR, Franklin IJ, Davies AH. The disparate management of superficial venous thrombosis in primary and secondary care. Phlebology / Venous Forum of the Royal Society of Medicine. 2015;30:172–9. https://www.ncbi.nlm.nih.gov/pubmed/24500944[↩]
- Kearon C, Akl EA, Comerota AJ, et al. Antithrombotic Therapy for VTE Disease: Antithrombotic Therapy and Prevention of Thrombosis, 9th ed: American College of Chest Physicians Evidence-Based Clinical Practice Guidelines. Chest. 2012;141(2 Suppl):e419S-e494S. doi:10.1378/chest.11-2301. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3278049/[↩]
- David CV, Chira S, Eells SJ et al. Diagnostic accuracy in patients admitted to hospitals with cellulitis. Dermatol Online J. 2011;17(3). https://www.ncbi.nlm.nih.gov/pubmed/21426867[↩][↩]
- Falagas ME, Vergidis PI. Narrative review: diseases that masquerade as infectious cellulitis. Ann Intern Med. 2005;142(1):47–55. https://www.ncbi.nlm.nih.gov/pubmed/15630108[↩]
- Levell NJ, Wingfield CG, Garioch JJ. Severe lower limb cellulitis is best diagnosed by dermatologists and managed with shared care between primary and secondary care. Br J Dermatol. 2011;164(6):1326–1328. https://www.ncbi.nlm.nih.gov/pubmed/21564054[↩]
- Tormoen GW, Haley KM, Levine RL, McCarty OJT. Do circulating tumor cells play a role in coagulation and thrombosis? Front Oncol. 2012;2:115. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3437466/[↩]
- Blumenberg RM, Barton E, Gelfand ML et al. Occult deep venous thrombosis complicating superficial thrombophlebitis. J Vasc Surg. 1998;27(2):338–343. https://www.ncbi.nlm.nih.gov/pubmed/9510288[↩][↩][↩]
- Barleben A, Bandyk DF. Interpretation of peripheral venous duplex testing. Semin Vasc Surg. 2013;26(2–3):111–119. https://www.ncbi.nlm.nih.gov/pubmed/24636608[↩]
- Meissner MH, Moneta G, Burnand K et al. The hemodynamics and diagnosis of venous disease. J Vasc Surg. 2007;46(Suppl S):4S–24S. https://www.ncbi.nlm.nih.gov/pubmed/18068561[↩]