Contents
What is toxic shock syndrome
Toxic shock syndrome is a rare complication of infection from bacteria. Toxic shock syndrome is a medical emergency. Toxic shock syndrome is often caused by the Staphylococcus aureus (Staph) and less commonly Streptococcus pyogenes bacteria which are able to produce harmful toxins. The bacteria release toxins into your bloodstream which cause symptoms of shock. The toxins can also damage organs and body tissue, which can cause death if left untreated.
Toxic shock syndrome can affect anyone, males or females at any age, but is more common during adolescence. Risk factors for toxic shock syndrome include skin wounds and surgery. Toxic shock syndrome is more common among women when they are menstruating, but there is no evidence that tampons cause toxic shock syndrome. Toxic shock syndrome is caused by bacteria releasing harmful toxins.
Toxic shock syndrome received much publicity in the 1980s when an outbreak occurred among US women who were using particular types of tampon during their periods (menstruation). However, nowadays only about half of all cases of toxic shock syndrome are linked to tampons. Manufacturers of tampons sold in the United States no longer use the materials or designs that were associated with toxic shock syndrome. Also, the Food and Drug Administration requires manufacturers to use standard measurement and labeling for absorbency and to print guidelines on the boxes.
If you use tampons, read the labels and use the lowest absorbency tampon you can. Change tampons frequently, at least every four to eight hours. Alternate using tampons and sanitary napkins, and use minipads when your flow is light.
Toxic shock syndrome can affect anyone, including postmenopausal women, men and children.
Toxic shock syndrome can develop quickly and if not treated urgently, can be life-threatening. But if it’s diagnosed and treated early on, most people will make a full recovery.
There are several ways you can help lower your chance of developing toxic shock syndrome, these include:
- washing your hands before and after inserting a tampon
- using low absorbency tampons if possible
- alternating tampons with sanitary towels every so often during your period
- changing the tampons as often as advised on the pack
- never inserting more than one tampon
- making sure you remove the last tampon at the end of your period
- inserting a fresh tampon when going to bed and removing it when waking.
Signs of toxic shock syndrome
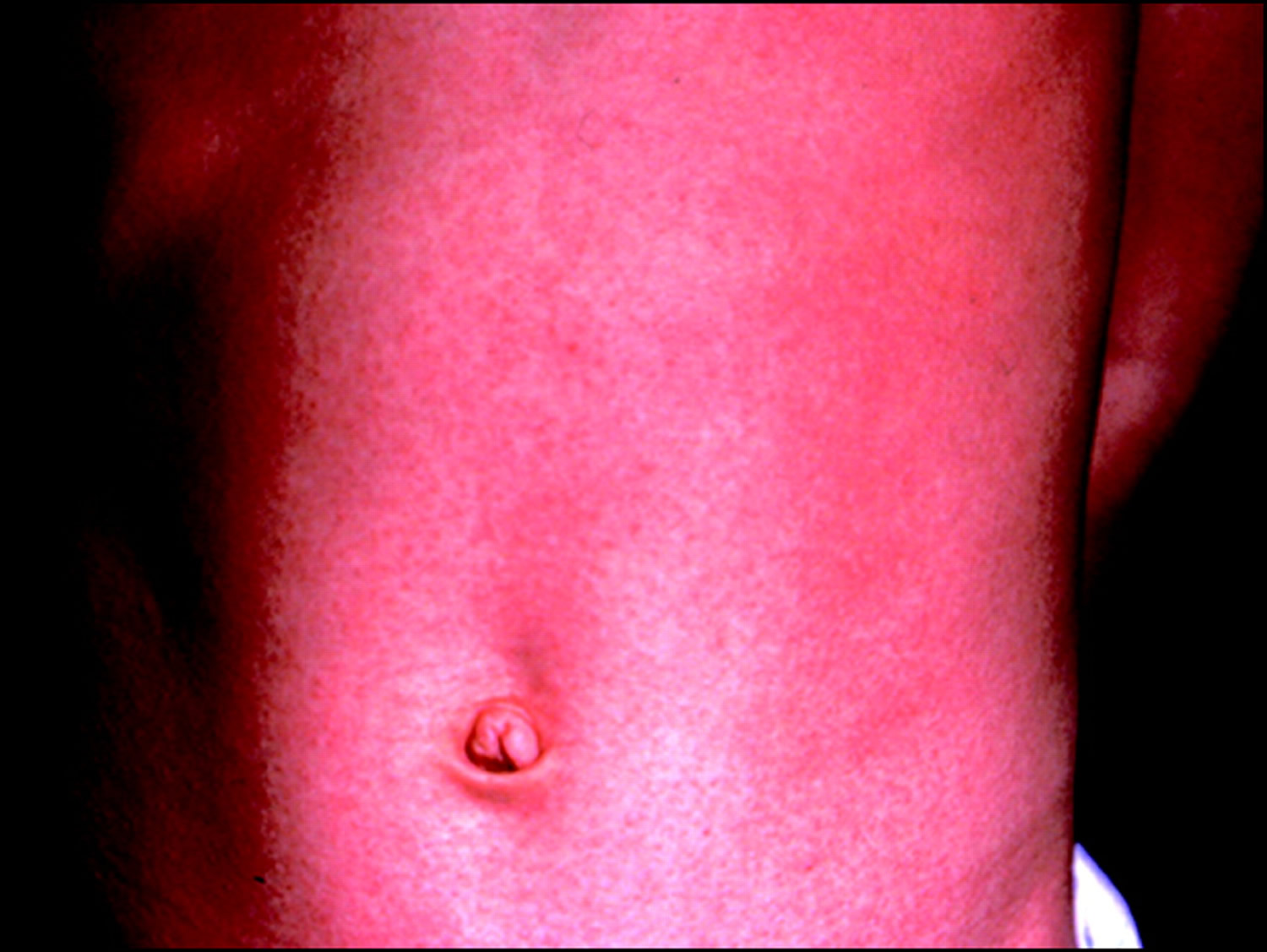
Toxic shock syndrome usually starts off as a sudden flu-like illness with a high temperature, aching muscles, vomiting and diarrhea. The affected person may feel dizzy and may faint due to a fall in blood pressure. They may have a rash that looks like sunburn.
Toxic shock syndrome can cause a number of symptoms, these include:
- diarrhea
- a sudden high temperature 104 °F (40°C) or above
- confusion
- dizziness
- tiredness
- vomiting
- aching muscles
- headaches
- low blood pressure
- red eyes, mouth and throat
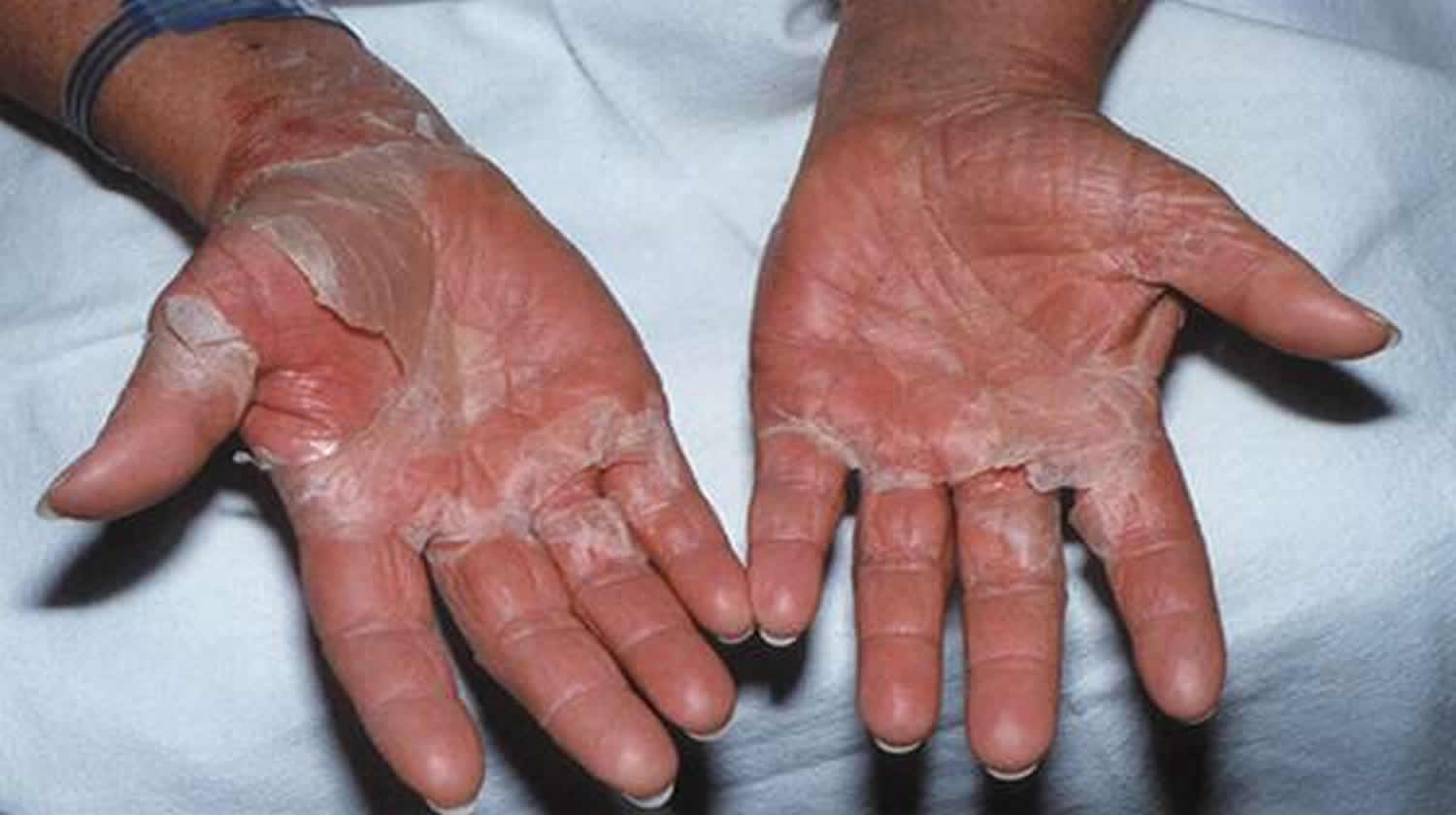
- a red rash found on the hands and feet that peels.
- seizures
Toxic shock syndrome usually needs to be treated in hospital with antibiotics, which are often given intravenously (IV). You may also need ‘supportive’ treatment, including medicines to maintain your blood pressure and fluids to treat dehydration. As toxic shock syndrome can lead to kidney failure, you may need dialysis. Treatment is normally successful if toxic shock syndrome is detected early on.
Women who have had an episode of toxic shock syndrome are at increased risk of a second episode. Therefore a doctor may advise against tampon use in women who have had toxic shock syndrome.
If you experience the symptoms of toxic shock syndrome, seek medical attention immediately. This is especially important if you are menstruating and using tampons, or have a skin infection or wound. If you are wearing a tampon, remove it immediately.
Figure 1. Toxic shock syndrome rash
Figure 2. Toxic shock syndrome rash
How do you get toxic shock syndrome
These bacteria (Staphylococcus aureus and less commonly Streptococcus pyogenes) are normally found on the skin, in the nose, armpit, groin or vagina of one in every three people, where they usually live without causing any health problems (colonization). In rare cases, the bacteria produce a toxin which can cause toxic shock syndrome in some individuals.
The majority of cases of toxic shock syndrome occur in women during menstruation, mostly associated with tampon use. There is no evidence that tampons directly cause toxic shock syndrome – the bacteria Staphylococcus aureus are the cause of the illness – not the tampon. This explains why women using pads, men and children can get toxic shock syndrome. However, women who use tampons during their period have a higher risk of toxic shock syndrome than women who do not. Cases have also followed surgery. In more than 30% of cases, no obvious bacterial infection can be found.
Incubation period (time between becoming infected and developing symptoms)
- Uncertain, probably varies from case to case.
Infectious period (time during which an infected person can infect others)
- Direct person-to-person spread does NOT occur.
Toxic shock syndrome complications
Toxic shock syndrome can progress rapidly. Complications may include:
- Shock
- Renal failure
- Death
Toxic shock syndrome causes
What causes toxic shock syndrome
Toxic shock syndrome is caused by a toxin (poison) produced by a common bacterium Staphylococcus aureus, often called ‘golden staph’ and less commonly Streptococcus pyogenes. These bacteria normally live harmlessly on your skin and in areas such as the nose and vagina of many people, where they usually cause no harm, but if they get deeper into the body they can release toxins that damage tissue and stop organs working. Only particular types (strains) of the staph bacteria produce the toxin that causes toxic shock syndrome.
When conditions are suitable these bacteria can multiply and produce the Toxic shock syndrome toxin. This can happen in skin infections, wounds (e.g. burns and after operations) and in the vagina, particularly when a tampon or contraceptive sponge is present. Research suggests that tampon absorbency is a factor in toxic shock syndrome.
The following can increase your risk of developing toxic shock syndrome:
- using tampons – particularly if you leave them in for longer than recommended or you use “super-absorbent” tampons
- using female barrier contraceptives, such as a contraceptive diaphragm or contraceptive cap
- a break in your skin, such as a cut, burn, boil, insect bite or surgical wound
- childbirth
- using nasal packing to treat a nosebleed
- having a Staphylococcal infection or Streptococcal infection, such as a throat infection, impetigo or cellulitis
Toxic shock syndrome isn’t spread from person to person. You don’t develop immunity to it once you’ve had it, so you can get it more than once.
Risk factors for toxic shock syndrome
Toxic shock syndrome can affect anyone. About half the cases of toxic shock syndrome associated with Staphylococci bacteria occur in women of menstruating age; the rest occur in older women, men and children. Streptococcal toxic shock syndrome occurs in people of all ages.
Toxic shock syndrome has been associated with:
- Having cuts or burns on your skin
- Having had recent surgery
- Using contraceptive sponges, diaphragms or superabsorbent tampons
- Having a viral infection, such as the flu or chickenpox
Toxic shock syndrome prevention
The following measures can help reduce your risk of toxic shock syndrome:
- Wash your hands before and after inserting a tampon. Unwrap a fresh, clean tampon just before insertion and do not handle it more than is necessary;
- Change tampons regularly, preferably every 3-4 hours, and never leave a tampon in place for longer than 8 hours;
- Choose a tampon with the lowest absorbency possible for your period flow;
- Change to lower absorbency tampons as the flow reduces over the course of your period;
- Consider using a sanitary pad or panty liner instead of a tampon whenever possible, especially at night;
- If high fever, vomiting or diarrhea develops during menstruation, stop using tampons and seek medical advice immediately. It may not be toxic shock syndrome but this must be verified because toxic shock syndrome can be dangerous if not treated in its early stages
- The risk of toxic shock syndrome may be reduced by using tampons intermittently during menstruation. Overnight, it is advisable to use a pad
- Take special care with personal hygiene during menstruation. Bathe or shower daily
- Discard any tampons you may have unwrapped and not used immediately. Insert the tampon gently and carefully
- Never insert more than one tampon at a time
- Remove tampons at the end of a period
- When using female barrier contraception, follow the manufacturer’s instructions about how long you can leave it in
- Treat wounds and burns quickly and get medical advice if you develop signs of an infection, such as swelling, redness and increasing pain
It’s a good idea to avoid using tampons or female barrier contraception if you’ve had toxic shock syndrome before.
Toxic shock syndrome signs and symptoms
The symptoms of toxic shock syndrome are caused by the effect of the toxin on the body, rather than the bacterial infection itself.
The symptoms of toxic shock syndrome start suddenly and get worse quickly.
Symptoms include:
- a sudden onset of high fever 104 °F (40°C) or above
- flu-like symptoms, such as a headache, chills, muscle aches, a sore throat and a cough
- feeling and being sick
- vomiting
- diarrhea
- dizziness (from low blood pressure) or fainting
- muscle aches
- confusion and collapse
- the whites of your eyes, lips and tongue turning a bright red
- breathing difficulties
- drowsiness
- a sunburn-like rash present at the time of illness, followed by peeling of the skin on the palms and soles 1 to 2 weeks later.
Sometimes you may also have a wound on your skin where the bacteria got into your body, but this isn’t always there and it may not look infected.
Toxic shock syndrome diagnosis
There’s no one test for toxic shock syndrome. You may need to provide blood and urine samples to test for the presence of a staph or strep infection. Your vagina, cervix and throat may be swabbed for samples for laboratory analysis.
Because toxic shock syndrome can affect multiple organs, your doctor may order other tests, such as a CT scan, lumbar puncture or chest X-ray, to assess the extent of your illness.
Toxic shock syndrome treatment
If you have toxic shock syndrome, you’ll need to be admitted to hospital and may need to be treated in an intensive care unit.
Treatment may involve:
- antibiotics to treat the infection
- in some cases, pooled immunoglobulin (purified antibodies taken out of donated blood from many people) may also be given to fight the infection
- oxygen to help with breathing
- fluids to help prevent dehydration and organ damage
- medication to help control blood pressure
- dialysis if the kidneys stop functioning
- in severe cases, surgery to remove any dead tissue – rarely, it may be necessary to amputate the affected area
Most people will start to feel better within a few days, but it may be several weeks before they’re well enough to leave hospital.