Contents
What is whooping cough
Whooping cough, also called pertussis, is a highly contagious bacterial infection of the lungs and airways. Whooping cough is caused by the bacterium Bordetella pertussis. These bacteria attach to the cilia (tiny, hair-like extensions) that line part of the upper respiratory system. The bacteria release toxins (poisons), which damage the cilia and cause airways to swell.
Whooping cough (pertussis) is known for uncontrollable, violent coughing bouts which often makes it hard to breathe. Whooping cough (pertussis) causes repeated coughing bouts that can last for two to three months or more, and can make babies and young children in particular very ill.
After cough fits, someone with whooping cough (pertussis) often needs to take deep breaths, which result in a “whooping” sound. Pertussis can affect people of all ages, but can be very serious, even deadly, for babies less than a year old.
Young babies with whooping cough can get pneumonia (lung infection), have trouble breathing, or even die. About half of babies younger than 1 year old who get whooping cough end up in the hospital.
People with whooping cough usually spread the disease by coughing or sneezing while in close contact with others. Parents, older siblings, or other caregivers can give whooping cough to babies without even knowing they have the disease.
Whooping cough is spread in the droplets of the coughs or sneezes of someone with the infection.
- The best way to protect against pertussis is by getting vaccinated.
How you can help protect your baby with whooping cough vaccines:
- Women pass protection to their babies when they get the whooping cough vaccine around the third trimester (27th through 36th week of each pregnancy) of each pregnancy, preferably during the earlier part of this time period. After you get the shot, your body creates protective antibodies and passes some of them to your baby before birth. These antibodies give your baby some short-term protection against whooping cough in early life. This early protection is important because babies don’t start getting their own vaccine until they are 2 months old. These antibodies also help protect your baby from serious and sometimes deadly complications that can come along with whooping cough.
- Family members and caregivers surround the baby with some protection by being up to date with their whooping cough vaccines.
- Babies build their own protection by getting vaccinated according to the Centers for Disease Control and Prevention’s (CDC’s) recommended schedule, which begins when they are 2 months old (see Table 1 below).
Everyone around Your Baby Needs to Be Up-to-Date with their Whooping Cough Vaccine
When one member of a household has a respiratory illness, other members are at risk for getting sick, too. Parents should encourage everyone around their baby to be up to date with their whooping cough vaccines. The table below gives information, by age, about the Centers for Disease Control and Prevention’s whooping cough vaccine recommendations.
If you get pertussis after getting pertussis vaccines, you are less likely to have a serious infection. Typically, your cough won’t last as many days and coughing fits, whooping, and vomiting after coughing fits won’t occur as often. When vaccinated children get pertussis, fewer have apnea (life-threatening pauses in breathing), cyanosis (blue/purplish skin coloration due to lack of oxygen), and vomiting.
Not up to date on your whooping cough vaccine?
Get vaccinated at least two weeks before coming into close contact with a baby. These two weeks give your body enough time to build up protection against whooping cough.
Getting sick with pertussis or getting pertussis vaccines doesn’t provide lifelong protection. This means you can still get pertussis and pass it onto others, including babies.
Pertussis vaccines are effective, but not perfect. They typically offer good levels of protection within the first 2 years after getting the vaccine, but then protection decreases over time. Public health experts call this ‘waning immunity.’ Similarly, natural infection may also only protect you for a few years.
In general, DTaP vaccines are 80% to 90% effective. Among kids who get all 5 doses of DTaP on schedule, effectiveness is very high within the year following the 5th dose – at least 9 out of 10 kids are fully protected. There is a modest decrease in effectiveness in each following year. About 7 out of 10 kids are fully protected 5 years after getting their last dose of DTaP and the other 3 out of 10 kids are partially protected – protecting against serious disease.
CDC’s current estimate is that in the first year after getting vaccinated with Tdap, it protects about 7 out of 10 people who receive it. There is a decrease in effectiveness in each following year. About 3 or 4 out of 10 people are fully protected 4 years after getting Tdap.
Keeping up-to-date with recommended pertussis vaccines is the best way to protect you and your loved ones.
Table 1. Centers for Disease Control and Prevention’s whooping cough vaccine recommendations
| Age | Whooping Cough Vaccine Recommendations |
|---|---|
| Birth through 6 years | CDC recommends DTaP for children at the following ages:
|
| 11 through 18 years | CDC recommends one dose of Tdap at 11 or 12 years old:
|
| 19 years and older | CDC recommends one dose of Tdap for adults who have never received Tdap:
|
Is whooping cough contagious?
Whooping cough (Pertussis) is a very contagious disease only found in humans. Pertussis spreads from person to person. A person with pertussis can infect up to 12 to 15 other people. People with pertussis usually spread the disease to another person by coughing or sneezing or when spending a lot of time near one another where you share breathing space. Many babies who get pertussis are infected by older siblings, parents, or caregivers who might not even know they have the disease.
That’s why being up to date with pertussis vaccines and practicing good cough and sneeze etiquette are so important.
Older siblings, parents, or caregivers who might not know they have the disease infect many babies who get pertussis. If pertussis is circulating in the community, there’s a chance that even a fully vaccinated person of any age can catch this very contagious disease. But if you received pertussis vaccines, your infection is usually less serious.
If you or your child develops a cold that includes a very bad cough or a cough that lasts a long time, it may be pertussis. The best way to know is to contact your doctor.
Infected people are most contagious up to about 2 weeks after the cough begins. Antibiotics may shorten the amount of time someone is contagious.
Vaccines are the most effective tool doctors have to provide protection against pertussis. It’s important that everyone get their recommended pertussis vaccines to protect themselves.
While pertussis vaccines are the most effective tool to prevent this disease, no vaccine is 100% effective. When pertussis circulates in the community, there is a chance that a fully vaccinated person, of any age, can catch this disease. If you have gotten the pertussis vaccine but still get sick, the infection is usually not as bad.
Doesn’t herd immunity protect most people?
When enough of a population is immune to an infectious disease, through vaccination or prior illness, its spread from person to person is unlikely. Public health experts call this ‘herd immunity’ (or community immunity). Even people not vaccinated (such as newborns and those with chronic illnesses) typically have protection because the disease has little opportunity to spread within their community. Public health experts cannot rely on herd immunity to protect people from pertussis since:
- Pertussis spreads so easily
- Vaccine protection decreases over time
- Acellular pertussis vaccines may not prevent colonization (carrying the bacteria in your body without getting sick) or spread of the bacteria.
Who’s at risk of whooping cough
Whooping cough can affect people of any age, including:
- babies and young children – young babies under six months of age are at a particularly increased risk of complications of whooping cough
- older children and adults – it tends to be less serious in these cases, but can still be unpleasant and frustrating
- people who’ve had whooping cough before – you’re not immune to whooping cough if you’ve had it before, although it tends to be less severe the second time around
- people vaccinated against whooping cough as a child – protection from the whooping cough vaccine tends to wear off after a few years
You can get whooping cough if you come into close contact with someone with the infection.
A person with whooping cough is infectious from about six days after they were infected – when they just have cold-like symptoms – until three weeks after the coughing bouts start.
Antibiotic treatment can reduce the length of time someone is infectious.
Stopping the whooping cough infection spreading
If you or your child are taking antibiotics for whooping cough, you need to be careful not to spread the infection to others.
- Stay away from nursery, school or work until 48 hours from the start of antibiotic treatment or three weeks after the coughing bouts started (whichever is sooner).
- Cover your or your child’s mouth and nose with a tissue when coughing and sneezing.
- Dispose of used tissues immediately.
- Wash your and your child’s hands regularly with soap and water.
Other members of your household may also be given antibiotics and a dose of the whooping cough vaccine to stop them becoming infected.
I’ve heard about parents refusing to get their children vaccinated and travelers to the United States spreading disease; are they to blame for pertussis outbreaks?
Even though children who haven’t received DTaP vaccines are at least 8 times more likely to get pertussis than children who received all 5 recommended doses of DTaP, they are not the driving force behind the large scale outbreaks or epidemics. However, their parents are putting them at greater risk of getting a serious pertussis infection and then possibly spreading it to other family or community members.
Scientists often see people blaming pertussis outbreaks on people coming to the United States from other countries. This is not the case. The United States never eliminated pertussis like measles or polio, so there’s always the chance for it to get into a community. Plus, every country vaccinates against pertussis.
Whooping cough complications
Babies and young children under six months are usually most severely affected by whooping cough.
Babies and Children Whooping Cough Complications
Pertussis (whooping cough) can cause serious and sometimes deadly complications in babies and young children, especially those who have not received all recommended pertussis vaccines.
About half of babies younger than 1 year old who get pertussis need care in the hospital. The younger the baby, the more likely they will need treatment in the hospital. Of those babies who are treated in the hospital with pertussis about:
- 1 out of 4 (23%) get pneumonia (lung infection)
- 1 out of 100 (1.1%) will have convulsions (violent, uncontrolled shaking)
- 3 out of 5 (61%) will have apnea (slowed or stopped breathing)
- 1 out of 300 (0.3%) will have encephalopathy (disease of the brain)
- 1 out of 100 (1%) will die
Other complications can include anorexia, dehydration, difficulty sleeping, epistaxis, hernias, otitis media, and urinary incontinence. More severe complications can include refractory pulmonary hypertension, pneumothorax, rectal prolapse, and subdural hematomas.
They’re also at an increased risk of:
- dehydration
- breathing difficulties
- weight loss
- pneumonia – an infection of the lungs
- fits (seizures)
- kidney problems
- brain damage caused by a lack of oxygen reaching the brain
- death – although this is very rare
Older children and adults tend to be less severely affected, although they may experience problems caused by repeated coughing, such as nosebleeds, bruised ribs or a hernia.
Teens and Adults
Teens and adults can also get complications from pertussis. They are usually less serious in this older age group, especially in those who have been vaccinated with a pertussis vaccine. The cough itself often causes complications in teens and adults. For example, you may pass out or break (fracture) a rib during violent coughing fits.
In one study, less than 1 out of 20 (5%) teens and adults with pertussis needed care in the hospital. Healthcare professionals diagnosed pneumonia (lung infection) in 1 out of 50 (2%) of those patients. The most common complications in another study were:
- Weight loss in 1 out of 3 (33%) adults
- Loss of bladder control in 1 out of 3 (28%) adults
- Passing out in 3 out of 50 (6%) adults
- Rib fractures from severe coughing in 1 out of 25 (4%) adults
Other complications can include anorexia, dehydration, epistaxis, hernias, and otitis media. More severe complications can include encephalopathy as a result of hypoxia from coughing or possibly from toxin, pneumothorax, rectal prolapse, subdural hematomas, and seizures.
Whooping cough prevention
Whooping cough vaccines can prevent pertussis, or whooping cough. Before pertussis vaccines became widely available in the 1940s, about 200,000 children got sick with it each year in the United States and about 9,000 died as a result of the infection. Now doctors see about 10,000 to 40,000 cases reported each year and unfortunately up to 20 deaths.
The best way to prevent pertussis (whooping cough) among babies, children, teens, and adults is to get vaccinated. Also, keep babies and other people at high risk for pertussis complications away from infected people.
CDC recommends pertussis vaccines for people of all ages. Babies and children should get 5 doses of DTaP for maximum protection. Healthcare professionals give a dose at 2, 4 and 6 months, at 15 through 18 months, and again at 4 through 6 years. They give a booster dose of Tdap to preteens at 11 or 12 years old.
Teens or adults who didn’t get Tdap as a preteen should get one dose. Getting Tdap is especially important for pregnant women during the third trimester of each pregnancy. It’s also important that those who care for babies are up-to-date with pertussis vaccination. You can get the Tdap booster dose no matter when you got your last regular tetanus and diphtheria booster shot (Td). Also, you need to get Tdap even if you got pertussis vaccines as a child or have been sick with pertussis in the past.
Vaccine protection for whooping cough fades with time. Today there is a booster (called Tdap) for preteens, teens, and adults that contains protection against tetanus, diphtheria and pertussis.
Whooping cough vaccine
There are two routine vaccinations that can protect babies and children from whooping cough:
- the whooping cough vaccine in pregnancy – Tdap (Reduced Diphtheria toxoid and Acellular Pertussis) – this can protect your baby during the first few weeks of life; the best time to have it is soon after the 20th week of your pregnancy
- the DTaP (Diphtheria, Tetanus, and Pertussis) – offered to babies at 2 months through 6 years of age
These vaccines don’t offer lifelong protection from whooping cough, but they can help stop children getting it when they’re young and more vulnerable to the effects of the infection.
Older children and adults aren’t routinely vaccinated, except during pregnancy or a whooping cough outbreak.
Whooping cough vaccination in pregnancy
There’s a lot of whooping cough (pertussis) around at the moment and babies who are too young to start their vaccinations are at greatest risk.
Young babies with whooping cough are often very unwell and most will be admitted to hospital because of their illness. When whooping cough is particularly severe, they can die. Whooping cough (pertussis) vaccines are the best way to prevent this disease.
- If you are pregnant, you should get a Tdap vaccine during the 3rd trimester of every pregnancy to help protect your baby from whooping cough in the first few months of life.
Pregnant women can help protect their babies by getting vaccinated – ideally from 27 weeks up to 36 weeks pregnant of each pregnancy 1. The Centers for Disease Control and Prevention (CDC) recommends that pregnant women receive the whooping cough vaccine for adolescents and adults (called Tdap vaccine) during the third trimester of each pregnancy. The recommended time to get the shot is during your 27th through 36th week of pregnancy, preferably during the earlier part of this time period. If for any reason you miss having the vaccine, you can still have it up until you go into labor.
There are 2 different whooping cough vaccines. Both vaccines combine protection against whooping cough, tetanus and diphtheria, but they are for different age groups:
- Tdap (Reduced Diphtheria toxoid and Acellular Pertussis): for everyone 11 years or older, including pregnant women
- DTaP (Diphtheria, Tetanus, and Pertussis): for children 2 months through 6 years of age
Note: For whooping cough pregnancy vaccination, doctors use the Tdap vaccine.
Whereas for whooping cough vaccination for babies and children younger than 7 years old doctor use DTaP.
Who should not get the Tdap vaccine
Some people should not get Tdap vaccine.
- A person who has ever had a life-threatening allergic reaction after a previous dose of any diphtheria, tetanus or pertussis containing vaccine, OR has a severe allergy to any part of this vaccine, should not get Tdap vaccine. Tell the person giving the vaccine about any severe allergies.
- Anyone who had coma or long repeated seizures within 7 days after a childhood dose of DTP or DTaP, or a previous dose of Tdap, should not get Tdap, unless a cause other than the vaccine was found. They can still get Td.
- Talk to your doctor if you:
- have seizures or another nervous system problem,
- had severe pain or swelling after any vaccine containing diphtheria, tetanus or pertussis,
- ever had a condition called Guillain Barré Syndrome (GBS),
- aren’t feeling well on the day the shot is scheduled.
Who should NOT get the DTaP vaccine
Some children should not get DTaP vaccine.
- Children with minor illnesses, such as a cold, may be vaccinated. But children who are moderately or severely ill should usually wait until they recover before getting DTaP vaccine.
- Any child who had a life-threatening allergic reaction after a dose of DTaP should not get another dose.
- Any child who suffered a brain or nervous system disease within 7 days after a dose of DTaP should not get another dose.
- Talk with your doctor if your child:
- had a seizure or collapsed after a dose of DTaP,
- cried non-stop for 3 hours or more after a dose of DTaP,
- had a fever over 105°F after a dose of DTaP.
Ask your doctor for more information. Some of these children should not get another dose of pertussis vaccine, but may get a vaccine without pertussis, called DT.
Why are pregnant women advised to have the vaccine?
Getting vaccinated while you’re pregnant is highly effective in protecting your baby from developing whooping cough in the first few weeks of their life.
The immunity you get from the vaccine will pass to your baby through the placenta and provide passive protection for them until they are old enough to be routinely vaccinated against whooping cough at two months old.
After receiving the whooping cough vaccine, your body will create protective antibodies (proteins produced by the body to fight off diseases) and pass some of them to your baby before birth. These antibodies provide your baby some short-term protection against whooping cough in early life. These antibodies can also protect your baby from some of the more serious complications that come along with whooping cough.
Your protective antibodies are at their highest about 2 weeks after getting the vaccine, but it takes time to pass them to your baby. So the preferred time to get the whooping cough vaccine is early in your third trimester.
The amount of whooping cough antibodies in your body decreases over time. That is why the Centers for Disease Control and Prevention (CDC) recommends you get a whooping cough vaccine during each pregnancy. Doing so allows each of your babies to get the greatest number of protective antibodies from you. This means each of your babies will get the best protection possible against this disease.
Why is the focus on protecting babies from pertussis?
Babies are at greatest risk for getting pertussis and then having serious complications from it, including death. About half of babies younger than 1 year old who get pertussis need care in the hospital, and 1 out of 100 babies who get treatment in the hospital die.
There are two strategies to protect babies until they’re old enough to receive vaccines and build their own immunity against this disease.
- First, vaccinate pregnant women with Tdap between 27 and 36 weeks of each pregnancy, preferably during the earlier part of this time period. By getting Tdap during pregnancy, mothers build antibodies that transfer to the newborn. These antibodies provide protection against pertussis in early life, before the baby can start getting DTaP vaccines at 2 months old. Tdap also helps protect mothers, making them less likely to spread pertussis to their babies.
- Second, make sure everyone around the baby is up to date with their pertussis vaccines. This includes parents, siblings, grandparents (including those 65 years and older), other family members, babysitters, etc. They should be up to date with the age-appropriate vaccine (DTaP or Tdap) at least two weeks before coming into close contact with the baby. Unless pregnant, only one dose of Tdap is recommended in a lifetime.
These two strategies should reduce infection in babies.
It’s also critical that healthcare professionals are up to date with a one-time Tdap booster dose, especially those who care for babies.
Getting the whooping cough vaccine while pregnant is better than getting the vaccine after you give birth
Whooping cough vaccination during pregnancy is ideal so your baby will have short-term protection as soon as he is born. This early protection is important because your baby will not start getting his whooping cough vaccines until he is 2 months old. These first few months of life are when your baby is at greatest risk for catching whooping cough. This is also when he’s at greatest risk for having severe, potentially life-threatening complications from the infection. To avoid that gap in protection, it is best to get a whooping cough vaccine during pregnancy. You will then pass protection to your baby before he is born. To continue protecting your baby, he should get whooping cough vaccines starting at 2 months old.
You may never have gotten the Tdap vaccine before and did not get it during this pregnancy. If so, you should make sure to get the vaccine immediately after you give birth, before leaving the hospital or birthing center. It will take about 2 weeks before your body develops protection (antibodies) in response to the vaccine. Once you have protection from the vaccine, you are less likely to give whooping cough to your newborn while caring for him. But remember, your baby will still be at risk for catching whooping cough from others.
A recent study looked to see how effective Tdap was at preventing whooping cough in babies whose mothers got the vaccine while pregnant or in the hospital after giving birth. The study found that getting Tdap between 27 through 36 weeks of pregnancy is 85% more effective at preventing whooping cough in babies younger than 2 months old.
There are no blood tests that can tell you if you have enough antibodies in your body to protect yourself or your baby against whooping cough. Even if you have been sick with whooping cough in the past or previously received the vaccine, you still should get the vaccine during each pregnancy.
When should I have the whooping cough vaccine?
The best time to get vaccinated to protect your baby is from 27 weeks up to 36 weeks of pregnancy. This maximizes the chance that your baby will be protected from birth, through the transfer of your antibodies before he or she is born.
If for any reason you miss having the vaccine, you can still have it up until you go into labor. However, this is not ideal, as your baby is less likely to get protection from you. At this stage of pregnancy, having the vaccination may not directly protect your baby, but would help protect you from whooping cough and from passing it on to your baby.
Breastfeeding may pass some protective antibodies onto your baby
By breastfeeding, you may pass some antibodies you have made in response to the vaccine to your baby. When you get a whooping cough vaccine during your pregnancy, you will have antibodies in your breast milk that you can share with your baby as soon as your milk comes in. However, your baby will not get protective antibodies immediately if you wait to get the whooping cough vaccine until after delivering your baby. This is because it takes about 2 weeks for your body to create antibodies.
Is the vaccine safe in pregnancy?
It’s understandable that you might have concerns about the safety of having a vaccine during pregnancy, but there’s no evidence to suggest that the whooping cough vaccine is unsafe for you or your unborn baby.
Whooping cough vaccine side effects
You may have some mild side effects such as swelling, redness or tenderness where the vaccine is injected in your upper arm, just as you would with any vaccine. These only last a few days. Other side effects can include fever, irritation at the injection site, swelling of the vaccinated arm, loss of appetite, irritability and headache. Serious side effects are extremely rare.
Most side effects from Tdap vaccination, including vaccination during pregnancy, are mild or moderate, and self-resolving. The most common side effects include
- Erythema, swelling, pain, and tenderness at the injection site
- Body-ache
- Fatigue
- Fever
Severe side effects are extremely rare, especially in adults.
Babies Build Their Own Protection with Vaccines
Pregnant women give their babies short-term protection by getting Tdap during each pregnancy, but children need to build their own protection. For best protection against whooping cough, children need five doses of DTaP. CDC recommends the first dose when your baby is 2 months old. She will need 2 more doses, given at 4 months and 6 months, to build up high levels of protection. Vaccine protection for whooping cough decreases over time. CDC recommends booster shots at 15 through 18 months and at 4 through 6 years to maintain protection during childhood.
Whooping cough signs and symptoms
Early Symptoms
The first symptoms of whooping cough are similar to those of a cold, such as a runny nose, red and watery eyes, a sore throat, and a slightly raised temperature.
The disease usually starts with cold-like symptoms and maybe a mild cough or fever. In babies, the cough can be minimal or not even there. Babies may have a symptom known as “apnea.” Apnea is a pause in the child’s breathing pattern. Pertussis is most dangerous for babies. About half of babies younger than 1 year who get the disease need care in the hospital.
Early symptoms can last for 1 to 2 weeks and usually include:
- Runny nose
- Low-grade fever (generally minimal throughout the course of the disease)
- Mild, occasional cough
- Apnea – a pause in breathing (in babies)
Pertussis in its early stages appears to be nothing more than the common cold. Therefore, healthcare professionals often do not suspect or diagnose it until the more severe symptoms appear.
Later-stage Symptoms
After 1 to 2 weeks and as the disease progresses, the traditional symptoms of pertussis may appear and include:-
Intense coughing bouts start about a week later.
- The coughing bouts usually last a few minutes at a time and tend to be more common at night.
- Coughing usually brings up thick mucus and may be followed by vomiting.
- Between coughs, you or your child may gasp for breath – this may cause a “whoop” sound, although not everyone has this.
- The strain of coughing can cause the face to become very red, and there may be some slight bleeding under the skin or in the eyes.
- Young children can sometimes briefly turn blue (cyanosis) if they have trouble breathing – this often looks worse than it is and their breathing should start again quickly.
- In very young babies, the cough may not be particularly noticeable, but there may be brief periods where they stop breathing.
Pertussis can cause violent and rapid coughing, over and over, until the air is gone from your lungs. When there is no more air in the lungs, you are forced to inhale with a loud “whooping” sound. This extreme coughing can cause you to throw up and be very tired. Although you are often exhausted after a coughing fit, you usually appear fairly well in-between. Coughing fits generally become more common and bad as the illness continues, and can occur more often at night. The coughing fits can go on for up to 10 weeks or more. In China, pertussis is known as the “100 day cough.”
The “whoop” is often not there if you have milder (less serious) disease. The infection is generally milder in teens and adults, especially those who have gotten the pertussis vaccine.
How long does whooping cough last
Recovery from pertussis can happen slowly. The cough becomes milder and less common. The coughing bouts will eventually start to become less severe and less frequent over time, but it may be a few months before they stop completely. Furthermore, coughing fits can return with other respiratory infections for many months after the pertussis infection started.
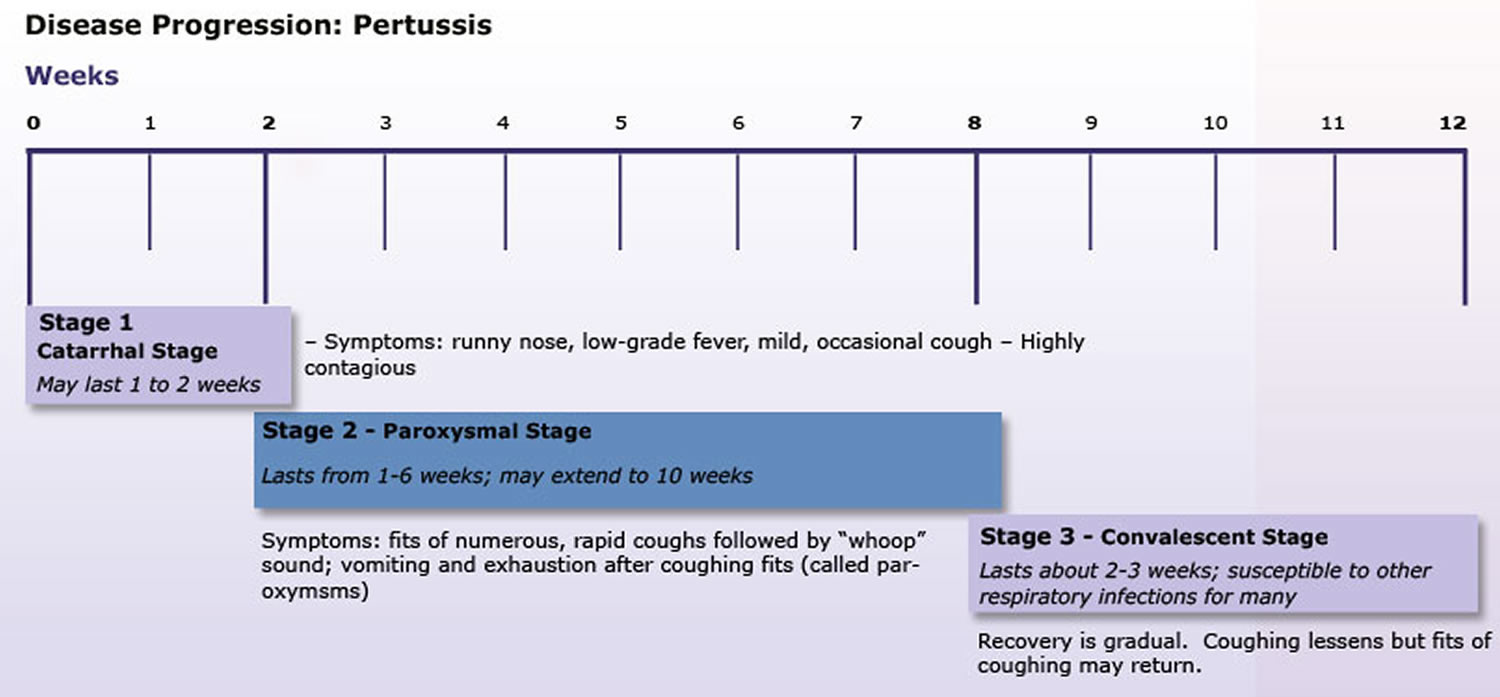
Figure 1. Whooping cough disease progression
[Source 2]Are most coughs pertussis and does everyone with pertussis “whoop”?
There are a lot of causes behind a person’s cough and not every cough is pertussis. In general, pertussis starts off with cold-like symptoms and maybe a mild cough or fever. But after 1 to 2 weeks, severe coughing can begin. Unlike the common cold, pertussis can become a series of coughing fits that continues for weeks. The best way to know if you have pertussis is to see your doctor. Your doctor can make a diagnosis and prescribe antibiotics if needed.
The name “whooping cough” comes from the sound people make gasping for air after a pertussis coughing fit. However, not everyone with pertussis will cough and many who cough will not “whoop.”
Teens and adults, especially those who did not get pertussis vaccines, may have a prolonged (lengthy) cough that keeps them up at night. Those who do get the coughing fits say it’s the worst cough of their lives. And the cough may last for weeks or months. It can also cause major disruptions to daily life and complications like broken ribs and ruptured blood vessels.
Babies may not cough at all. Instead, they may have life-threatening pauses in breathing (apnea) or struggle to breathe. Any time someone is struggling to breathe, it is important to get them to a doctor right away.
Whooping cough treatment
Treatment for whooping cough depends on your age and how long you’ve had the infection.
- Children under six months who are very ill and people with severe symptoms will usually be admitted to hospital for treatment. Your child may need help keeping breathing passages clear, which may require suctioning (drawing out) of mucus. Doctors monitor breathing and give oxygen, if needed. Children might need intravenous (IV, through the vein) fluids if they show signs of dehydration or have difficulty eating. You should take precautions, like practicing good hand hygiene and keeping surfaces clean.
- People diagnosed during the first three weeks of infection may be prescribed antibiotics to take at home – these will help stop the infection spreading to others, but may not reduce the symptoms.
- People who’ve had whooping cough for more than three weeks won’t normally need any specific treatment, as they’re no longer contagious and antibiotics are unlikely to help.
While you’re recovering at home, it can help to get plenty of rest, drink lots of fluids, clean away mucus and sick from your or your child’s mouth, and take painkillers such as paracetamol or ibuprofen for a fever.
Avoid using cough medicines, as they’re not suitable for young children and are unlikely to be of much help.
Antibiotics
If you or a member of your household has been diagnosed with pertussis, your doctor or local health department may recommend preventive antibiotics (medications that can help prevent diseases caused by bacteria) to other members of the household to help prevent the spread of disease. Additionally, they may recommend preventive antibiotics to some other people outside the household who have been exposed to a person with pertussis, including
- People at risk for serious disease
- People who have routine contact with someone that is considered at high risk of serious disease
Babies younger than 1 year old are most at risk for serious complications from pertussis. Pregnant women are not at increased risk for serious disease. However, experts consider those in their third trimester to be at increased risk since they could in turn expose their newborn to pertussis. You should discuss whether or not you need preventative antibiotics with your doctor. This is especially important if there is a baby or pregnant woman in your household. It is also important if you plan to have contact with a baby or pregnant woman.
Timing
Early treatment of pertussis is very important. The earlier a person, especially an infant, starts treatment the better. If a patient starts treatment for pertussis early in the course of illness, during the first 1 to 2 weeks before coughing paroxysms occur, symptoms may be lessened. Clinicians should strongly consider treating prior to test results if clinical history is strongly suggestive or patient is at risk for severe or complicated disease (e.g., infants). If a clinician diagnoses the patient late, antibiotics will not alter the course of the illness and, even without antibiotics, the patient should no longer be spreading pertussis.
Persons with pertussis are infectious from the beginning of the catarrhal stage (runny nose, sneezing, low-grade fever, symptoms of the common cold) through the third week after the onset of paroxysms (multiple, rapid coughs) or until 5 days after the start of effective antimicrobial treatment.
A reasonable guideline is to treat persons older than 1 year of age within 3 weeks of cough onset and infants younger than 1 year of age and pregnant women (especially near term) within 6 weeks of cough onset.
Administer a course of antibiotics to close contacts within 3 weeks of exposure, especially in high-risk settings. Use the same doses as in the treatment schedule.
Antibiotics of Choice
The recommended antimicrobial agents for treatment or chemoprophylaxis of pertussis are azithromycin*, clarithromycin, and erythromycin. Clinicians can also use Trimethoprim-sulfamethoxasole. Clinicians should choose the antimicrobial after consideration of the:
- Potential for adverse events and drug interactions
- Tolerability
- Ease of adherence to the regimen prescribed
- Cost
Infants
Macrolides erythromycin, clarithromycin, and azithromycin are preferred for the treatment of pertussis in persons 1 month of age and older. For infants younger than 1 month of age, azithromycin is preferred for post exposure prophylaxis and treatment because azithromycin has not been associated with infantile hypertrophic pyloric stenosis (IHPS), whereas erythromycin has. For infants younger than 1 month of age, the risk of developing severe pertussis and life-threatening complications outweighs the potential risk of infantile hypertrophic pyloric stenosis that has been associated with macrolide use. Clinicians should monitor infants younger than 1 month of age who receive a macrolide for the development of infantile hypertrophic pyloric stenosis and for other serious adverse events. For persons 2 months of age and older, an alternative to macrolides is trimethoprim-sulfamethoxazole.
On March 12, 2013, the Food and Drug Administration 3 issued a warning that azithromycin can cause abnormal changes in the electrical activity of the heart that may lead to a potentially fatal irregular heart rhythm in some patients. Azithromycin remains one of the recommended drugs for treatment and chemoprophylaxis of pertussis, but consider using an alternative drug in those who have known cardiovascular disease, including:
- Patients with known prolongation of the QT interval, a history of torsades de pointes, congenital long QT syndrome, bradyarrhythmias, or uncompensated heart failure
- Patients on drugs known to prolong the QT interval
- Patients with ongoing proarrhythmic conditions such as uncorrected hypokalemia or hypomagnesemia, clinically significant bradycardia, and in patients receiving Class IA (quinidine, procainamide) or Class III (dofetilide, amiodarone, sotalol) antiarrhythmic agents.
Elderly patients and patients with cardiac disease may be more susceptible to the effects of arrhythmogenic drugs on the QT interval.
If Your Child Gets Treatment for Pertussis at Home
Do not give cough medications unless instructed by your doctor. Giving cough medicine probably will not help and is often not recommended for kids younger than 4 years old.
Manage pertussis and reduce the risk of spreading it to others by:
- Following the schedule for giving antibiotics exactly as your child’s doctor prescribed.
- Keeping your home free from irritants – as much as possible – that can trigger coughing, such as smoke, dust, and chemical fumes.
- Using a clean, cool mist vaporizer to help loosen mucus and soothe the cough.
- Practicing good handwashing.
- Encouraging your child to drink plenty of fluids, including water, juices, and soups, and eating fruits to prevent dehydration (lack of fluids). Report any signs of dehydration to your doctor immediately. These include dry, sticky mouth, sleepiness or tiredness, or thirst. They also include decreased urination or fewer wet diapers, few or no tears when crying, muscle weakness, headache, dizziness or lightheadedness.
- Encouraging your child to eat small meals every few hours to help prevent vomiting (throwing up) from occurring.
Hygiene
Like many respiratory illnesses, pertussis spreads by coughing and sneezing while in close contact with others, who then breathe in the bacteria. CDC recommends practicing good hygiene to prevent the spread of respiratory illnesses. To practice good hygiene you should:
- Cover your mouth and nose with a tissue when you cough or sneeze.
- Put your used tissue in the waste basket.
- Cough or sneeze into your upper sleeve or elbow, not your hands, if you don’t have a tissue.
- Wash your hands often with soap and water for at least 20 seconds.
- Use an alcohol-based hand rub if soap and water are not available.
- Get the Whooping Cough Vaccine While You Are Pregnant. https://www.cdc.gov/pertussis/pregnant/mom/get-vaccinated.html[↩]
- Pertussis (Whooping Cough). https://www.cdc.gov/pertussis/about/signs-symptoms.html[↩]
- FDA Drug Safety Communication: Azithromycin (Zithromax or Zmax) and the risk of potentially fatal heart rhythms. https://www.fda.gov/Drugs/DrugSafety/ucm341822.htm[↩]