Contents
What is behcet’s disease
Behcet’s disease or Behçet’s syndrome also known as Adamantiades–Behçet’s disease or “silk road disease“, is a rare and poorly understood condition that results in inflammation of the blood vessels (vasculitis) and tissues. The disease is named after the doctor who first described it, Dr. Hulusi Behçet. Behcet’s disease is a rare, chronic, lifelong disorder that involves inflammation of blood vessels throughout the body 1. Behçet’s disease is a multi-system disease; it may involve any organ in the body including the central nervous system (brain and spinal cord), resulting in memory loss and impaired speech, balance, and movement.
In severe Behcet’s disease cases, there’s also a risk of serious and potentially life-threatening problems, such as permanent vision loss, strokes, swelling of the spinal cord, and intestinal complications.
Most people with the condition experience episodes where their symptoms are severe (flare-ups or relapses), followed by periods where the symptoms disappear (remission).
Over time, some of the symptoms can settle down and become less troublesome, although they may never resolve completely.
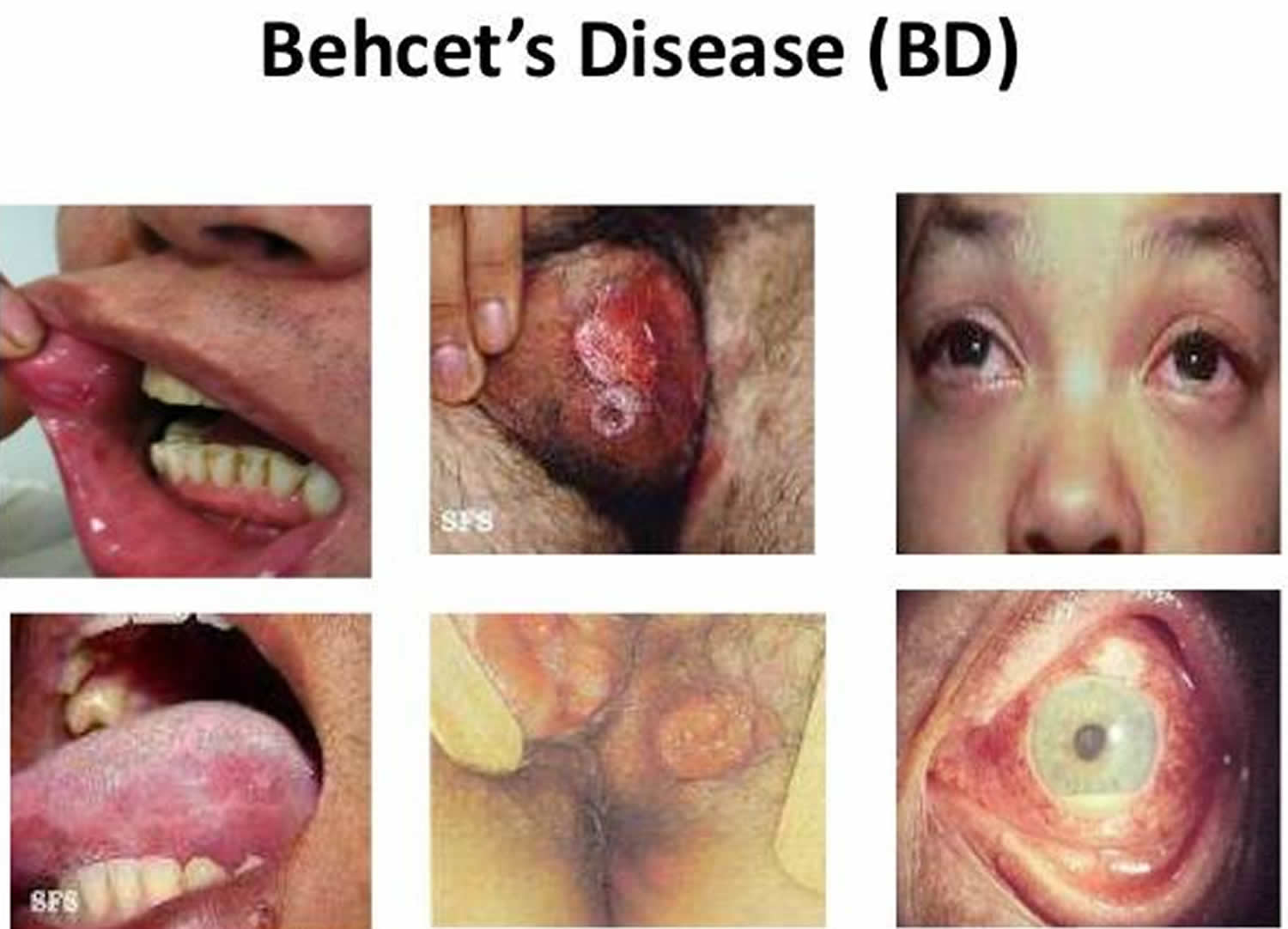
The main symptoms of Behçet’s disease include 2:
- Genital and (painful) mouth ulcers;
- Ocular symptoms such as red, painful eyes, blurred vision, periorbital pain, photophobia, eye redness and excessive tear production;
- Acne-like spots;
- Headaches;
- Inflammatory arthritis with painful, stiff, warm and red swollen joints.
Other possible symptoms of Behçet’s disease include:
- Memory loss, personality changes and speech impairment;
- Instability;
- Incontinence;
- Back pain;
- Meningitis (inflammation of the membranes of the brain and spinal cord);
- Cranial nerve palsies;
- Blood clots;
- Inflammation of the digestive system;
- Blindness;
- Diarrhea, flatulence and vomiting.
Behçet’s disease is one of the few forms of vasculitis (inflammation of blood vessels) in which there is a known genetic predisposition. The presence of a specific gene is a risk factor for this disease. However, it must be emphasized that presence of the gene in itself is not enough to cause Behçet’s disease; many people possess the gene, but relatively few develop Behçet’s disease. Despite the predisposition to Behçet’s disease conferred by this particular gene, familial cases make up only 5% of cases. It is believed that other factors (perhaps more than one) play a role. Possibilities include infections and other environmental exposures.
Behçet’s disease is common in the Middle East, Asia, and Japan, but rare in the United States. Behçet’s disease is most common along the “Old Silk Route”, which spans the region from Japan and China in the Far East to the Mediterranean Sea, including countries such as Turkey and Iran. In Japan, the current prevalence is 10-15 per 100,000; in Turkey, it is 80-300 per 100,000.
Behçet’s disease is most common among patients aged 15-45 years, although it can happen at any age. On average, the first symptoms appear between the ages of 10 and 30.
Behcet’s disease tends to occur more often in men five to 10 times more frequently than women. However, in the United States and Australia, Behçet’s disease is more common in women than men, and the symptoms tend to be less severe.
Behçet’s disease initially is an inflammatory disease, but in severe cases, or if left untreated, the effects of the disease may include blindness, stroke, swelling of the spinal cord, and intestinal complications.
Confirming a diagnosis of Behçet’s disease can be difficult and can take a long time, because the symptoms are so wide-ranging, symptoms may come and go, and general (they can be shared with a number of other conditions). Diagnosing Behcet’s may take months or even years to have all of the symptoms.
There is no cure for Behçet’s disease. Treatment for Behçet’s disease is is symptomatic and supportive – focusing on reducing pain and preventing serious problems. Medication may be prescribed to reduce inflammation and/or regulate the immune system. Immunosuppressive therapy may be considered. Most people can control symptoms with treatment.
Behcet’s disease life expectancy
There is no cure for Behcet’s disease. Behçet’s disease is a lifelong disorder that comes and goes. Permanent remission of symptoms has not been reported. Death from Behçet’s disease is rare.
Behcet’s disease causes
The exact cause of Behçet’s disease is not known. Studies suggest that some people may have a genetic predisposition to the condition. A genetic predisposition means that a person may carry a gene for a disease but it may not be expressed unless something in the environment triggers the disease. Researchers have demonstrated that certain individuals with Behçet’s disease, especially those of Middle Eastern and Asian descent, have an increased frequency of certain “human leukocyte antigens” (HLAs) in the blood. Individuals with Behçet’s disease are more likely to have HLA-B51 than the general population. The possible role of HLA-B51 in predisposing individuals to Behçet’s disease and its overall association with the disorder is unknown. Other genetic markers and their role in the development of Behçet’s disease are being studied. Viral or bacterial infections have also been suggested as a possible cause for the disorder. Still another theory is that the disease is an auto-inflammatory disorder in which the body loses the ability to appropriately regulate and control inflammation.
Autoimmune disorders are caused when the body’s natural defenses against “foreign” or invading organisms (e.g., antibodies) begin to attack healthy tissue for unknown reasons. While investigation is ongoing, no autoantibodies to date have been identified to suggest that Behçet’s disease is an autoimmune disease.
Affected Populations
Behçet’s disease is a rare disorder in the United States and Western Europe. It occurs most frequently in the Middle East and Asia, along ancient trading routes between the Mediterranean basin and eastern Asia, known as the Silk Road. Turkey has the highest prevalence rate (80-370 cases per 100,000); Japan, Korea, China, Iran, and Saudi Arabia also have high prevalence rates. The disorder is the leading cause of blindness in Japan. The age of onset is typically between 30 and 40 years.
In the United States and Australia, this disease is more common in women than men, and the symptoms tend to be less severe. Men may be more commonly affected in Middle Eastern countries and usually have more severe disease. Central nervous system involvement is more common among native populations of northern Europe and the United States.
Related Disorders
Symptoms of the following disorders can be similar to those of Behçet’s disease. Comparisons may be useful for a differential diagnosis:
- Reactive arthritis, previously known as Reiter’s disease, is a rare infectious disorder characterized by arthritis, inflammation of the urinary tract (non-gonococcal urethritis), and inflammation of the membranes that line the eyes (conjunctivitis). Lesions may also appear on the skin and mucous membranes. The symptoms may not all appear at once. There may by spontaneous remissions and recurrences. Symptoms may include pus in the urine, swollen painful joints, and ulcers in the mouth. Occasionally the iris of the eyes may become inflamed (iritis). This disorder can be transmitted through sexual contact.
- Stevens-Johnson disease is a rare skin disorder characterized by large bullous lesions on the skin and mucous membranes of the mouth, throat, nose, eyes, and genitals. The lesions are typically painful. Inflammation of the membranes that line the eyes (conjunctivitis) may also occur and be accompanied by a discharge. This can lead to scarring of the cornea and loss of vision. Some people may experience fever and fatigue.
- Sweet disease is a rare skin disorder characterized by painful red eruptions usually on the arms, face, neck, and legs. Major symptoms of Sweet disease are tender or painful skin eruptions and general feeling of discomfort (malaise). Skin lesions usually occur on the arms, but also on the face, neck, legs, and occasionally the thighs and trunk. The lesions may be up to an inch in diameter. They are usually bluish-red, irregular, flat or raised, sharply outlined, circular, and/or hardened, with a rounded edge. Scarring is usually absent. Remission may occur after a few weeks, but recurrences are possible. On rare occasions, the female genital tract (vagina and uterus) may be involved. The exact cause of this disorder is not known.
Risk factors for Behcet’s disease
Factors that may increase your risk of Behcet’s disease include:
- Age. Behcet’s disease commonly affects men and women in their 20s and 30s, though children and older adults also can develop the condition.
- Where you live. People from countries in the Middle East and Far East, including Turkey, Iran, Japan and China, are more likely to develop Behcet’s disease.
- Sex. While Behcet’s disease occurs in both men and women, the disease is usually more severe in men.
- Genes. Having certain genes is associated with a higher risk of developing Behcet’s disease.
Behcet’s disease symptoms
Behçet’s disease can cause a wide range of symptoms, but it’s rare for someone with the condition to have all of them at once.
Most people experience times when the symptoms improve (remission) and times when they get worse (flare-ups or relapses).
The main symptoms of Behçet’s disease are outlined below.
Mouth ulcers
Almost everyone with Behçet’s disease develops mouth ulcers. The ulcers look the same as normal mouth ulcers (canker sores or aphthous stomatitis), but can be more numerous and painful. They most often develop on the tongue, lips, gums and the insides of the cheeks.
The sores are usually round or oval with reddish (erythematous) borders that may occur anywhere within the mouth. They may be shallow or deep and may appear as a single lesion or a cluster of multiple lesions. The sores typically heal within a few days, up to a week or more, without scarring, but frequently recur. They may precede other symptoms of Behçet’s syndrome by a number of years. Sometimes similar sores may appear on the genitals, specifically the scrotum and shaft of the penis in males and the vulva in females. The sores are also round and painful, but may be larger and deeper than those affecting the mouth.
These sores also recur and usually heal within a couple of weeks but unlike oral sores may tend to scar.
Genital ulcers
Like mouth ulcers, recurrent genital ulcers are also a common symptom of Behçet’s disease.
In men, the ulcers usually appear on the scrotum. In women, they usually appear on the cervix (neck of the womb), vulva or vagina. However, genital ulcers can appear anywhere in the groin area, including on the penis.
The genital ulcers are usually painful and leave scarring in around half of all cases. Men may also experience inflammation (swelling) of the testicles and women may find the ulcers make having sex painful.
Genital ulcers caused by Behçet’s disease are not contagious and can’t be spread through sexual intercourse.
Skin lesions
Many people with Behçet’s disease also develop skin lesions. A lesion is any type of unusual growth or abnormality that develops on your skin, such as a bump or a discolored area of skin.
Individuals with Behçet’s syndrome may also exhibit the formation of small, pus-filled growths on the skin (pustules). Some affected individuals, especially females, may develop lesions that resemble those of erythema nodosum, a skin disorder characterized by the formation of tender, reddish, inflammatory nodules on the front of the legs. These nodules disappear on their own (spontaneously) sometimes leaving faint scars or discoloration (pigmentation). Some individuals with Behçet’s disease may develop more widespread acne-like skin eruptions (acneiform eruptions) and/or inflammation that mistakenly appear to affect the hair follicles on the skin (pseudofolliculitis).
Skin lesions often heal within 14 days, although they may come back frequently. Erythema nodosum lesions may leave permanently discolored areas of skin.
Inflammation of the joints
Behçet’s disease affects the joints in up to two in every three people with the condition, causing arthritis-like symptoms such as pain, stiffness, swelling, warmth and tenderness.
Affected individuals experience painful joints (arthralgia) and swelling in various joints of the body (polyarthritis). This may occur before, during, or after the onset of the other symptoms associated with Behçet’s syndrome. Pain, which can range from mild to severe, typically affects the joints of the knees, wrists, elbows and ankles, and may become chronic. The joints most often affected include the knees, ankles, wrists and small joints in the hands. Lasting damage to affected joints is extremely rare.
Unlike some conditions affecting the joints, permanent joint damage is rare in Behçet’s disease and symptoms can usually be controlled successfully.
Behcet’s disease eye
Inflammation of the eyes is another common symptom of Behçet’s disease, occurring in around half of all cases. It often develops very suddenly.
Behcet’s disease eye symptoms may include inflammation of the back of the eye (posterior uveitis) and inflammation of the anterior chamber (anterior uveitis or iridocyclitis). Sometimes both eyes may be affected at the same time. Inflammation of the iris accompanied by pain, tearing (lacrimation), and the accumulation of pus (hypopyon iritis) may also occur. The retina may become inflamed resulting in blurred vision, abnormal sensitivity to light (photophobia), and/or, inflammation of the thin membranous layer of blood vessels behind the retina (chorioretinitis). Although the lesions that cause inflammation in various parts of the eyes may resolve, repeated recurrences may result in the partial loss of vision (decreased visual acuity) or complete blindness if the disease is uncontrolled. In some cases, eye abnormalities may be the first symptom of Behçet’s syndrome. In other cases, they may not develop until several years later.
Inflammation of the uveal tract (uveitis) can cause symptoms that include:
- painful red eyes
- floaters (dots that move across the field of vision)
- blurred vision
In the most severe cases of Behçet’s disease, inflammation of the eyes can lead to permanent loss of vision. However, this is far less likely with early and appropriate treatment.
Sensitive skin
In some people with Behçet’s disease, the skin is particularly sensitive to injury or irritation. This is known as pathergy.
For example, if a needle is used to prick the skin of someone who has pathergy, a large red bump would develop within a day or two that appears out of proportion to the original needle prick.
Gastrointestinal symptoms
Individuals with Behçet’s disease may also have recurring ulcers in the digestive tract. Symptoms vary from mild abdominal discomfort to severe inflammation of the large intestine and rectum accompanied by diarrhea or bleeding. Having blood in your stools is a possible symptom of inflammation of the internal lining of the bowel.
Behçet’s disease can cause inflammation of the stomach and bowel, which can lead to symptoms such as:
- feeling sick and vomiting
- abdominal (tummy) pain
- indigestion
- loss of appetite
- diarrhea with bleeding.
Blood clots
The inflammation of the lining of the blood vessels associated with Behçet’s disease can sometimes cause blood clots to form.
One of the most common types of blood clot to affect people with Behçet’s disease is deep vein thrombosis (DVT), where a blood clot develops in one of the deep veins of the body, usually in the legs.
Symptoms of deep vein thrombosis (DVT) include:
- pain, swelling and tenderness in one of your legs (usually in the calf)
- a heavy ache in the affected area
- warm skin in the area of the clot
- redness of your skin, particularly at the back of your leg below the knee
DVT often requires immediate medical treatment. If you suspect deep vein thrombosis (DVT), go to your nearest accident and emergency department immediately.
In people with Behçet’s disease, careful assessment is needed to determine if it’s safe to use blood thinning treatment for this complication. Treatment to control inflammation is usually more effective.
Cerebral venous thrombosis
A less common type of blood clot associated with Behçet’s disease is cerebral venous thrombosis (cerebral venous thrombosis). This occurs when a blood clot develops inside the blood vessels that run through channels located between the outer and inner layer of your brain.
The blood clot can increase the pressure inside your skull and also lead to an interruption of the blood supply to the brain (stroke).
Symptoms of a cerebral venous thrombosis include:
- a severe headache – this has been described as a throbbing, piercing, band of pain, or as a very severe pain that suddenly appears out of nowhere
- slurred speech
- seizures (fits)
- hearing loss
- double vision
- stroke-like symptoms, such as muscle weakness or paralysis – but, unlike most strokes, both sides of the body can be affected
Cerebral venous thrombosis should be regarded as a medical emergency. If you suspect a stroke, dial your local emergency number immediately to request an ambulance.
Aneurysms
Inflammation of the blood vessels can cause the walls of your blood vessels to weaken. This causes the walls to bulge outwards as a result of blood pressure. The bulge is known as an aneurysm.
Aneurysms don’t usually cause any noticeable symptoms unless the wall of the blood vessel becomes so weak that it enlarges or ruptures. This can place pressure on nearby areas and can sometimes lead to internal bleeding or organ dysfunction.
The symptoms of a ruptured aneurysm can vary depending on where in the body the aneurysm developed. Possible symptoms include:
- pain in a limb
- a sudden agonizing headache
- dizziness
- breathlessness
- coughing up blood
- confusion
- loss of consciousness
Inflammation of the nervous system
Approximately 10%-20% of individuals with Behçet’s disease also have involvement of the central nervous system. Inflammation of the central nervous system (CNS) causes the most serious symptoms associated with Behçet’s disease. These symptoms usually appear months or years after the initial symptoms of Behçet’s disease. Recurring attacks of inflammation involving the brain (parenchymal Neuro-Behçet) or the membranes that surround the brain or spinal cord (meningitis or meningoencephalitis) can result in neurological damage.
The symptoms of central nervous system (CNS) inflammation usually develop quickly over the space of a few days, and can include:
- headache
- inability to coordinate voluntary movement (cerebellar ataxia)
- double vision
- loss of balance
- seizures (fits) (rarely)
- partial paralysis on one side of the body
- impaired muscle movements of the face and throat (pseudobulbar palsies)
- behavioral or personality changes
- stroke
General symptoms
It’s also common for people with Behçet’s disease to experience more general symptoms as a result of the condition, including periods of extreme physical or mental tiredness (fatigue). This can affect a person’s ability to perform any sort of activity.
How is Behcet’s Disease Diagnosed?
There is no specific test for Behçet’s disease. Consequently, the diagnosis is based on the clinical signs and symptoms that are compatible with the disease – such as the presence of oral/genital ulcers, uveitis and skin lesions, etc.
An international group of physicians has established a set of guidelines to aid in the classification of Behçet’s patients for the purpose of conducting research in the disease. The criteria put forth by the group include recurrent oral ulceration (at least three occasions in a year). In addition, a patient must also meet two of the following four criteria for Behçet’s disease:
- recurrent genital ulcerations,
- eye lesions (uveitis or retinal vasculitis),
- skin lesions (erythema nodosum, lesions, acne), and/or
- positive “pathergy test”.
The pathergy test is a simple test in which the forearm is pricked with a small, sterile needle. Occurrence of a small red bump or pustule at the site of needle insertion constitutes a positive test. Although a positive pathergy test is helpful in the diagnosis of Behcet’s, only a minority of Behçet’s patients demonstrates the pathergy phenomenon (i.e., have positive tests). Patients from the Mediterranean region are more likely to demonstrate pathergy. In addition, other conditions can occasionally result in positive pathergy tests, so the test is not 100% specific.
Behcet’s disease treatment
There’s currently no cure for Behçet’s disease, but a number of treatments can help to relieve symptoms and reduce the risk of serious complications.
Once a diagnosis of Behçet’s disease has been confirmed, you’ll usually be referred to several different specialists who have experience of treating the condition. They’ll help draw up a specific treatment plan for you.
The specialists involved in your care may include:
- a dermatologist – a doctor who specializes in treating skin conditions
- an oral medicine specialist – a doctor or dentist who specializes in conditions affecting the mouth
- a rheumatologist – a doctor who specializes in treating joint conditions and conditions affecting the entire body
- an ophthalmologist – a doctor who specializes in treating eye conditions
- a neurologist – a doctor who specializes in treating conditions that affect the nervous system and brain
You may see more than one specialist during the same visit to hospital, to help with diagnosis and creating a treatment plan.
Your treatment plan usually involves the use of a combination of different medications. Depending on the type and severity of your symptoms, you may only need to take medication when you have a flare-up.
Alternatively, you may have to take medication on a long-term basis to stop serious complications developing, such as vision loss.
Medications
A number of different medications can be used to treat the various symptoms of Behçet’s disease, but the main types of medication used can be broadly divided into:
- corticosteroids
- immunosuppressants
- biological therapies
Corticosteroids
Corticosteroids are powerful anti-inflammatory medications that can be useful in reducing the inflammation associated with Behçet’s disease.
Depending on the specific symptoms being treated, corticosteroids are available as:
- topical corticosteroids – applied directly to the area affected as eye drops, creams or gels
- oral corticosteroids – these reduce inflammation throughout the body and come as tablets or capsules
Occasionally, corticosteroid injections may also be used.
Side effects depend on the form of corticosteroid you are taking. Side effects associated with topical corticosteroids are uncommon, but long-term use may lead to problems such as a thinning of your skin.
The long-term use of oral corticosteroids is associated with some potentially more serious side effects, including:
- increased appetite, leading to weight gain
- mood swings
- increased pressure in the eye (glaucoma)
- high blood pressure (hypertension)
- weak and brittle bones (osteoporosis)
- cataracts
- diabetes
Immunosuppressants
Immunosuppressants are a type of medication that reduces the activity of the immune system, which in turn interrupts the inflammation process that causes most of the symptoms of Behçet’s disease.
Examples of immunosuppressants used to treat Behçet’s disease include azathioprine, ciclosporine, methotrexate, mycophenolate mofetil and thalidomide.
These medications are usually available as tablets, capsules and injections. Colchicine, an anti-inflammatory medication often used for gout, may also be beneficial.
While immunosuppressants can be useful in treating a wide range of Behçet’s disease symptoms, they can also cause some potentially significant side effects.
For this reason, you’ll be given careful advice about potential side effects and monitoring through blood tests. This is often co-ordinated by a specialist nurse.
General side effects of these medications can include:
- effects on blood cells and liver function (regular monitoring of blood tests may be required)
- increased risk of infections – you should report any symptoms of a possible infection to your doctor or healthcare team as soon as possible
- feeling sick and vomiting
- abdominal (tummy) pain
- diarrhea
- hair loss, which is usually temporary
- pins and needles
- muscle cramps and weakness
Some immunosuppressants can also cause birth defects and shouldn’t be taken if you’re pregnant or planning a pregnancy.
If you’re taking any of these medications, you should ensure you talk to your specialist or doctor about the possible effects of your medication on a potential pregnancy.
Biological therapies
Biological therapies are a newer type of medication that target the biological processes involved in the process of inflammation more selectively.
For example, one group of medications called tumor necrosis factor alpha inhibitors (TNFa-inhibitors) work by targeting the antibodies thought to cause much of the inflammation associated with Behçet’s disease.
Biological therapies used to treat Behçet’s disease include infliximab and interferon alpha. These may either be given directly into a vein (intravenously) or by injection under the skin (subcutaneous injection) at varying intervals.
While they’re often effective, biological therapies are also very expensive. Your local hospital will usually use biological therapies if your symptoms are severe and other medications haven’t been effective.
Biological therapies can also cause a range of side effects, including:
- increased risk of infections
- headaches
- dizziness
- nausea
- muscle and joint pain
- sudden, noticeable heartbeats (palpitations)
- increased heart rate (tachycardia)
As with immunosuppressant treatment, you should report any symptoms of a possible infection to your doctor or healthcare team as soon as possible.
Treating specific symptoms
The specific medications used for Behçet’s disease vary depending on the symptom being treated. The treatments for some of the main symptoms associated with the condition are outlined below.
Ulcers and skin lesions
Topical corticosteroids – such as creams, lozenges, mouthwashes and sprays – are usually the first treatment recommended for mouth and genital ulcers.
Some people find that using a corticosteroid inhaler is effective. These inhalers are commonly used to treat asthma and are normally used to spray the medication into the lungs. However, rather than inhaling the steroids, you can use the inhaler to spray the steroids directly on to an ulcer.
If you have red, tender swellings on your legs (erythema nodosum), you may be prescribed colchicine tablets to reduce the inflammation of your skin.
For severe ulcers and lesions that don’t respond to other treatments, other immunosuppressant tablets or biological therapies may be recommended.
Eye inflammation
Because of the potential risk of vision loss in serious cases, any eye inflammation caused by Behçet’s disease should be carefully monitored by an ophthalmologist.
Treatment for eye problems often involves taking azathioprine and corticosteroid tablets, although corticosteroid eye drops may also be useful.
In severe cases where these treatments haven’t helped, mycophenolate mofetil, ciclosporine or biological therapies may also be recommended.
Joint pain
For people with joint pain caused by Behçet’s disease, conventional painkillers such as paracetamol and non-steroidal anti-inflammatory drugs (NSAIDs) may sometimes help relieve the pain.
Daily colchicine tablets can also help by reducing the inflammation in your joints.
In severe cases where these treatments haven’t helped, azathioprine or biological therapies may be recommended.
Gastrointestinal symptoms
A number of different medications may be used to help reduce inflammation of the stomach and bowel caused by Behçet’s disease, including corticosteroids, immunosuppressants and biological therapies.
Sometimes the inflammation in your bowel causes it to become damaged and bleed. Medical treatment is usually successful, though rarely emergency surgery may be needed to stop the bleeding and remove the affected section of bowel.
Headaches
In cases of Behçet’s disease, headaches are usually treated in the same way as migraines. This means there are two types of medication that can be used:
- medication to prevent the symptoms of a headache occurring, such as beta-blockers
- medication to help relieve the headache, such as NSAIDs and a type of medication called triptans
Blood clots
It’s not entirely clear whether blood clots associated with Behçet’s disease should be treated in the same way as blood clots caused by other conditions, or whether using medication to treat the underlying inflammation is more appropriate.
Normally, blood clots are treated with a type of medication called an anticoagulant, which helps thin the blood and reduces the risk of the blood clot blocking the flow of blood.
However, the use of anticoagulants for Behçet’s disease is controversial because the blood clots are slightly different to other clots – they tend to stick to the side of the blood vessel walls, rather than break off and travel through the bloodstream.
Using anticoagulants in Behçet’s disease could also potentially increase the risk of any aneurysms rupturing and causing serious internal bleeding.
Blood clots are often treated with a combination of corticosteroid or immunosuppressant tablets to reduce the inflammation in the blood vessels. Anticoagulants are only used if you’ve been screened to make sure there are no aneurysms.
Aneurysms
Aneurysms caused by Behçet’s disease are normally treated with a combination of corticosteroid and immunosuppressant tablets, or infusions of cyclophosphamide to reduce inflammation in the affected blood vessel and stop the aneurysm getting worse.
Surgery or procedures may also be considered. The aneurysm may be repaired or bypassed using small tubes called stents, or it can be blocked off. This is often combined with medical treatment to reduce or prevent the risk of recurrence.
For more information about how surgery is used to treat some common types of aneurysm, see treating brain aneurysms and treating abdominal aortic aneurysms.
Central nervous system inflammation
Relatively minor symptoms of central nervous system inflammation, such as double vision, may get better on their own without the need for treatment.
However, more serious symptoms, such as paralysis and behavioral changes, usually require treatment with medication. This will often be in the form of corticosteroid or immunosuppressant injections, or biological therapies.
Pregnancy and fertility
Fertility is usually unaffected in women with Behçet’s disease, but it’s important that any pregnancy is planned where possible. This is because many of the medications used to treat the condition, such as thalidomide, can cause birth defects.
It’s recommended that you use at least one reliable method of contraception until you decide that you want to have a baby. You should discuss your plans to have a baby with your care team, who will be able to adjust your treatment plan to make your pregnancy as safe as possible.
There’s little evidence that having Behçet’s disease increases your risk of pregnancy-related complications, although there’s a very small chance of your baby being born with a temporary condition called neonatal Behçet’s disease.
The fertility of men with Behçet’s disease may be affected. This can be the result of the condition itself or of a side effect of some of the immunosuppressant medications. Colchicine may temporarily lower sperm count, but this often improves when treatment is stopped.
Where fertility is affected, further investigation – and, in some cases, fertility treatment such as in vitro fertilisation (IVF) – may be needed to conceive successfully. Read more about treating infertility.
Neonatal Behçet’s disease
There’s a possibility that a baby can be born with a type of Behçet’s disease that can cause ulcers on the baby’s genitals and mouth. This type of Behçet’s disease, known as neonatal Behçet’s disease, is extremely rare, with only one or two cases being reported every few years.
Corticosteroids can be used to help relieve symptoms of neonatal Behçet’s disease. The condition usually resolves within six to eight weeks of the birth.
Investigational Therapies
There are no FDA approved therapies for the treatment of Behçet’s Syndrome. Immunosuppressive drugs such as azathioprine (Imuran), chlorambucil (Leukeran), cyclophosphamide (Cytoxan), cyclosporine (Sandimmune), interferon alpha, and anti-TNF inhibitors have being studied for use as treatments for the disorder. It has been suggested that cyclosporine may be beneficial for the treatment of oral ulcers, skin lesions, and inflammation of the eyes, but the symptoms of Behçet’s syndrome return quickly when the drug is stopped. Apremilast (Otezla) is currently being studied for use in treatment of recurrent oral and genital ulcerations as well as other manifestations.
Coping and support
The unpredictability of Behcet’s disease can make it particularly frustrating. Taking good care of yourself may help you better cope. Your approach to caring for yourself will depend on what signs and symptoms you’re feeling on a particular day. In general, try to:
- Rest during flares. When signs and symptoms appear, take time for yourself. Be flexible and adjust your schedule when possible so that you can rest when you need it. It’s also a good idea to keep stress to a minimum, because stress can aggravate your symptoms.
- Be active when you have the energy. Moderate exercise, such as walking or swimming, can make you feel better between Behcet’s disease flares. Exercise strengthens your body, helps keep your joints flexible and can improve your mood.
- Connect with others. Because Behcet’s disease is a rare disorder, it may be difficult to find others with the disease nearby. Ask your doctor about support groups in your area. If it’s not possible to connect with someone close, the American Behcet’s Disease Association 3 offers message boards and chat rooms where you can connect with other people who have Behcet’s disease.