Contents
Broken rib
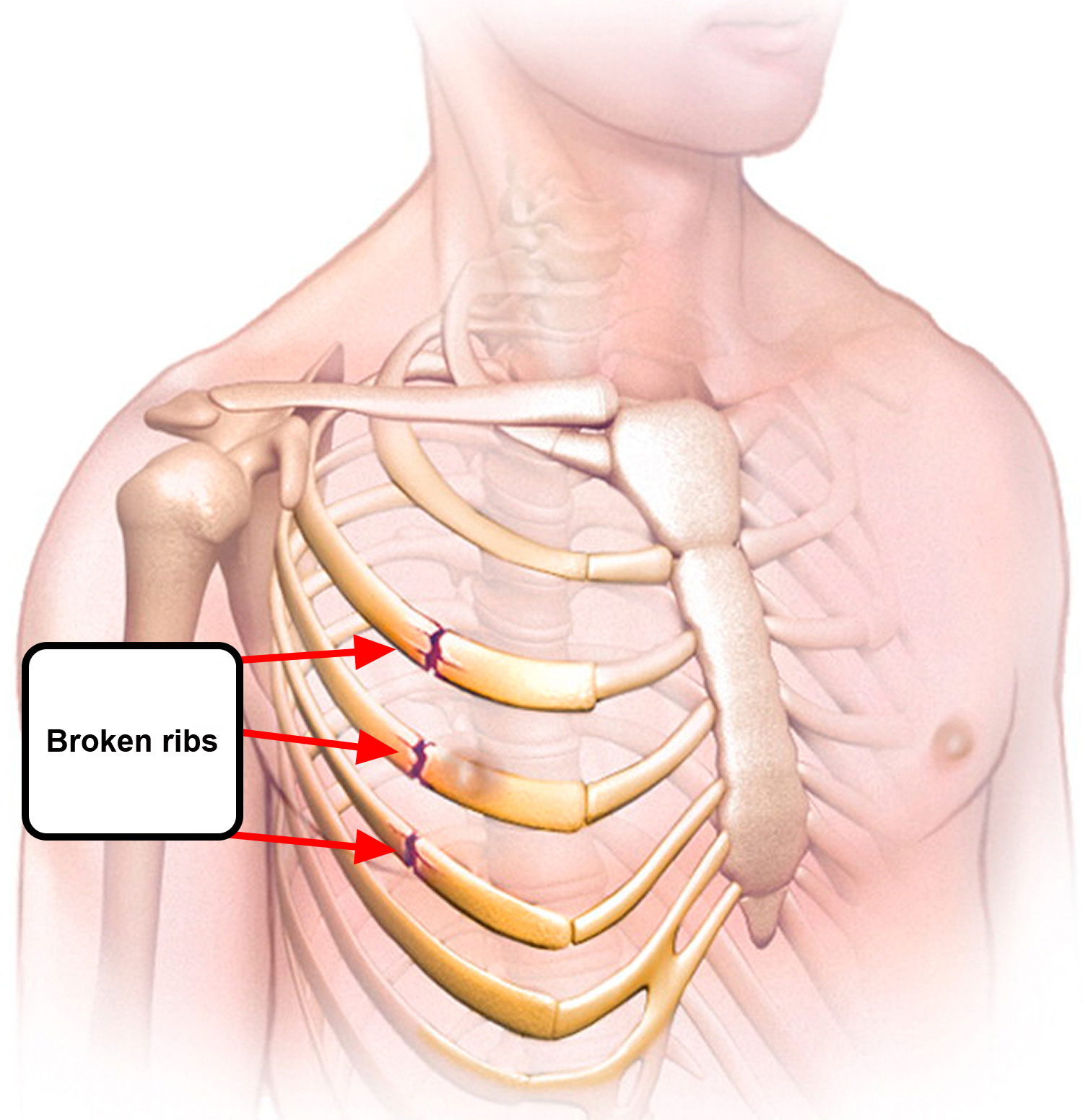
A broken rib also called a rib fracture is a common injury that occurs when one of the bones in your rib cage breaks or cracks (see Figure 4). The most common cause is strong blunt force trauma to the chest, such as from a fall, motor vehicle accident, a hit with a baseball bat or impact during contact sports. However, sometimes in older people who have osteoporosis, only a slight force (as occurs in a minor fall) is required.
Many broken ribs are merely cracked. While still painful, cracked ribs aren’t as potentially dangerous as ribs that have been broken into separate pieces. A jagged edge of broken bone can damage major blood vessels or internal organs, such as the lung.
The fracture itself is rarely serious, although the force that caused the fracture occasionally causes other problems, such as a bruised lung (pulmonary contusion) or a collapsed lung (pneumothorax). An injury that fractures the lower ribs sometimes also damages the liver or spleen. The more ribs that are broken, the more likely lungs or other organs are to be damaged.
Flail chest can result if several adjacent ribs are broken in more than one place. In flail chest, a segment of the chest wall separates from the rest and moves in the opposite direction from the rest of the chest wall when a person breathes. Breathing becomes more difficult and tiring. Usually, a blow strong enough to cause flail chest also bruises the lung beneath the injured area.
In most cases, broken ribs usually heal on their own in one or two months (most broken ribs heal on their own within six weeks). Adequate pain control is important so that you can continue to breathe deeply and avoid lung complications, such as pneumonia.
See your doctor if you have a very tender spot in your rib area that occurs after trauma or if you have difficulty breathing or pain with deep breathing.
Seek medical attention immediately if you feel pressure, fullness or a squeezing pain in the center of your chest that lasts for more than a few minutes or pain that extends beyond your chest to your shoulder or arm. These symptoms can indicate a heart attack.
Broken rib complications
A broken rib can injure blood vessels and internal organs. The risk increases with the number of broken ribs. Complications vary depending on which ribs break.
The ribs enclose vital organs such as the heart and lungs, so chest trauma can cause life-threatening injuries.
Possible complications include:
- Cardiac and torn or punctured aorta – for example, a sharp end of a break in one of the first three ribs at the top of your rib cage could rupture your aorta or another major blood vessel servicing the heart (coronary artery)
- Pneumothorax – collapsed lung due to changes in pressure within the chest. This could be caused by a broken rib tearing the lung or a puncture in the chest wall. Symptoms can include breathing difficulties, chest pain and coughing up blood.
- acerated spleen, liver or kidneys. The bottom two ribs rarely fracture because they have more flexibility than do the upper and middle ribs, which are anchored to the breastbone. But if you break a lower rib, the broken ends can cause serious damage to your spleen, liver or a kidney. Splenic rupture – the spleen is located on the left side of the abdomen. Its roles include filtering the blood to remove abnormal cells and the manufacture of some immune system cells including antibodies and lymphocytes. Splenic rupture means the outer capsule has split and the spleen bleeds into the abdominal cavity.
Flail chest is a serious injury
Flail chest is the most common serious injury to the ribs. It occurs when three or more ribs are broken in at least two places, front and back. This will only happen if there has been a great deal of blunt force. The key sign of flail chest is ‘paradoxical movement’, which means the natural movement of the ribcage during breathing is in reverse. For example, the injured area of ribcage sinks in when the person inhales, instead of lifting outwards.
This reversal is caused by changes to air pressure in the ribcage as a result of injury. However, it is the accompanying injury to the lungs that usually causes complications, not the broken ribcage. Intubating the person (putting oxygen into the lungs via a tube placed down the trachea, or windpipe) will create a ‘normal’ pressure in the lungs.
If you have:
- An injury caused by a serious accident – such as a car accident
- Shortness of breath that is getting worse
- Chest pain that is getting worse
- Pain in your tummy or shoulder
- Coughing up blood
- Coughing up yellow or green mucus
- Avery high temperature or you feel hot and shivery
It could mean you have a chest infection or that a broken rib has damaged something else like your lung, liver or spleen.
Structure of the ribs
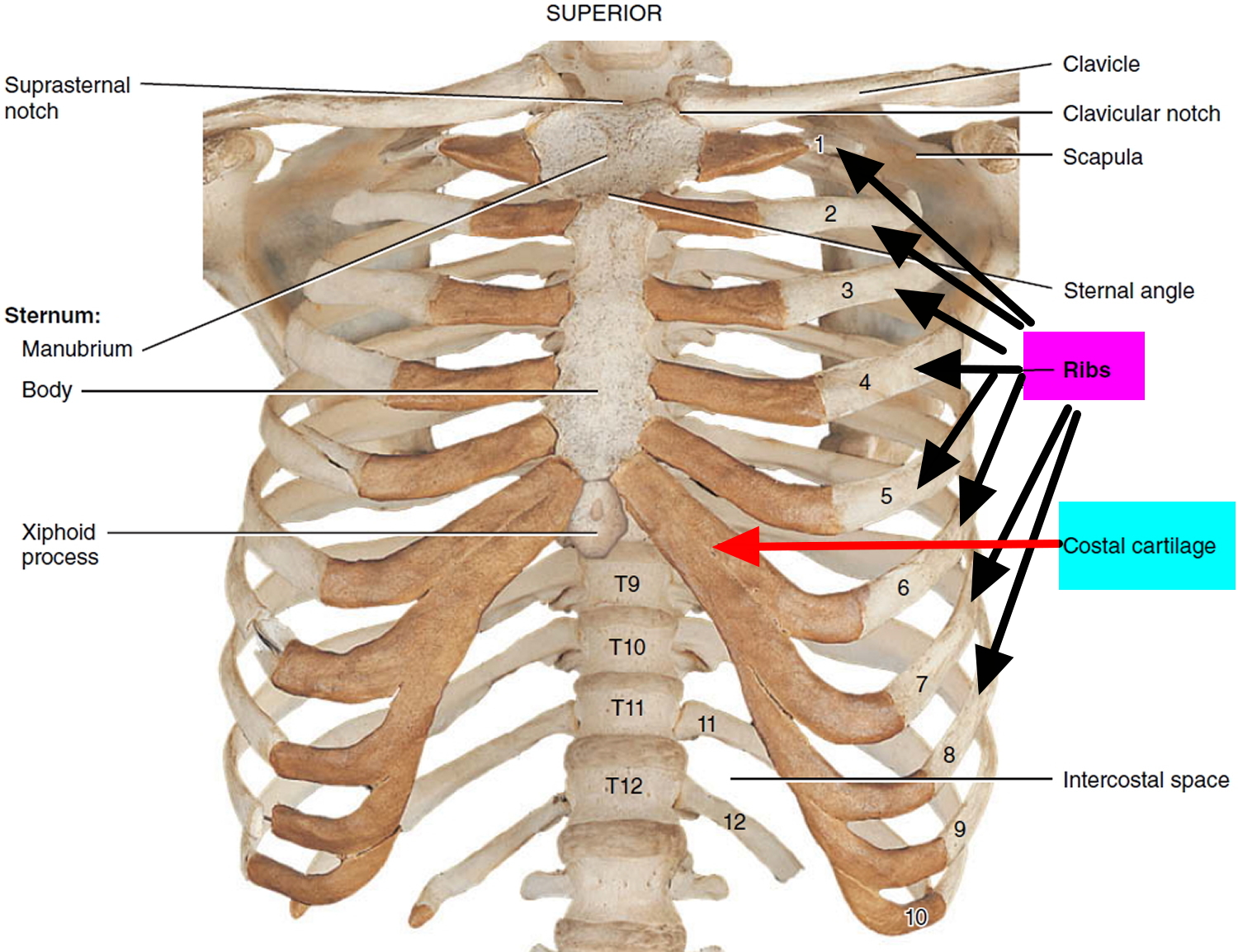
You have twelve pairs of ribs, numbered 1–12 from superior (top) to inferior (bottom). Your ribs give structural support to the sides of the thoracic cavity (Figure 1). The ribs increase in length from the first through seventh (ribs #1 to ribs #7) and then decrease in length to rib 12. Each rib articulates posteriorly with its
corresponding thoracic vertebra.
The first through seventh pairs of ribs (ribs #1 to ribs #7) have a direct anterior attachment to the sternum by a strip of hyaline cartilage called costal cartilage. The costal cartilages contribute to the elasticity of the thoracic cage and prevent various blows to the chest from fracturing the sternum and/or ribs. The ribs that have costal cartilages and attach directly to the sternum are called true (vertebrosternal) ribs. The articulations formed between the true ribs and the sternum are called sternocostal joints. The remaining five pairs of ribs (ribs #8 to ribs #12) are termed false ribs because their costal cartilages either attach indirectly to the sternum or do not attach to the sternum at all (see ribs #11 to ribs #12). The cartilages of the eighth, ninth, and tenth pairs of ribs attach to one another and then to the cartilages of the seventh pair of ribs. These false ribs are called vertebrochondral ribs. The eleventh and twelfth pairs of ribs are false ribs designated as floating (vertebral) ribs because the costal cartilages at their anterior ends do not attach to the sternum at all. These ribs attach only posteriorly to the thoracic vertebrae. Inflammation of one or more costal cartilages, called costochondritis, is characterized by local tenderness and pain in the anterior chest wall that may radiate. The symptoms mimic the chest pain (angina pectoris) associated with a heart attack.
The ribcage is supported by ligaments and muscles, including the muscles between the ribs (intercostal muscles). These muscles allow the ribcage to expand when you breathe in and to drop when you breathe out.
The curved design of the ribs makes them resistant to fractures. Their ability to flex helps the bone to absorb the force of a blow. However, any bone will break if the force exerted against it is stronger than it can structurally withstand. A rib is most likely to fracture at its outer curve, which is its weakest point.
Older people are more prone to rib fractures because bones thin with age. Children are less likely to break ribs because their bones are relatively flexible.
Figure 1. Ribs
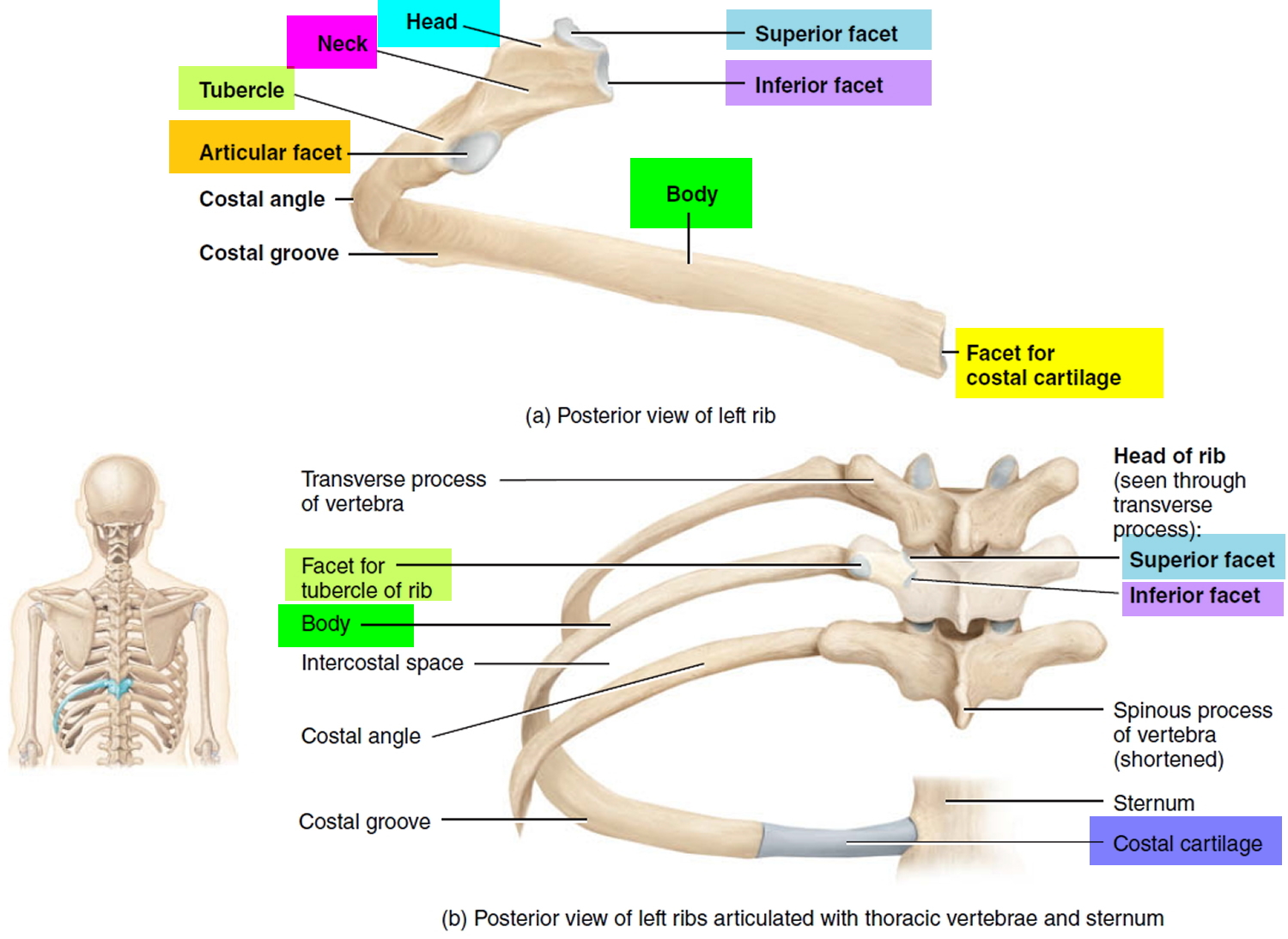
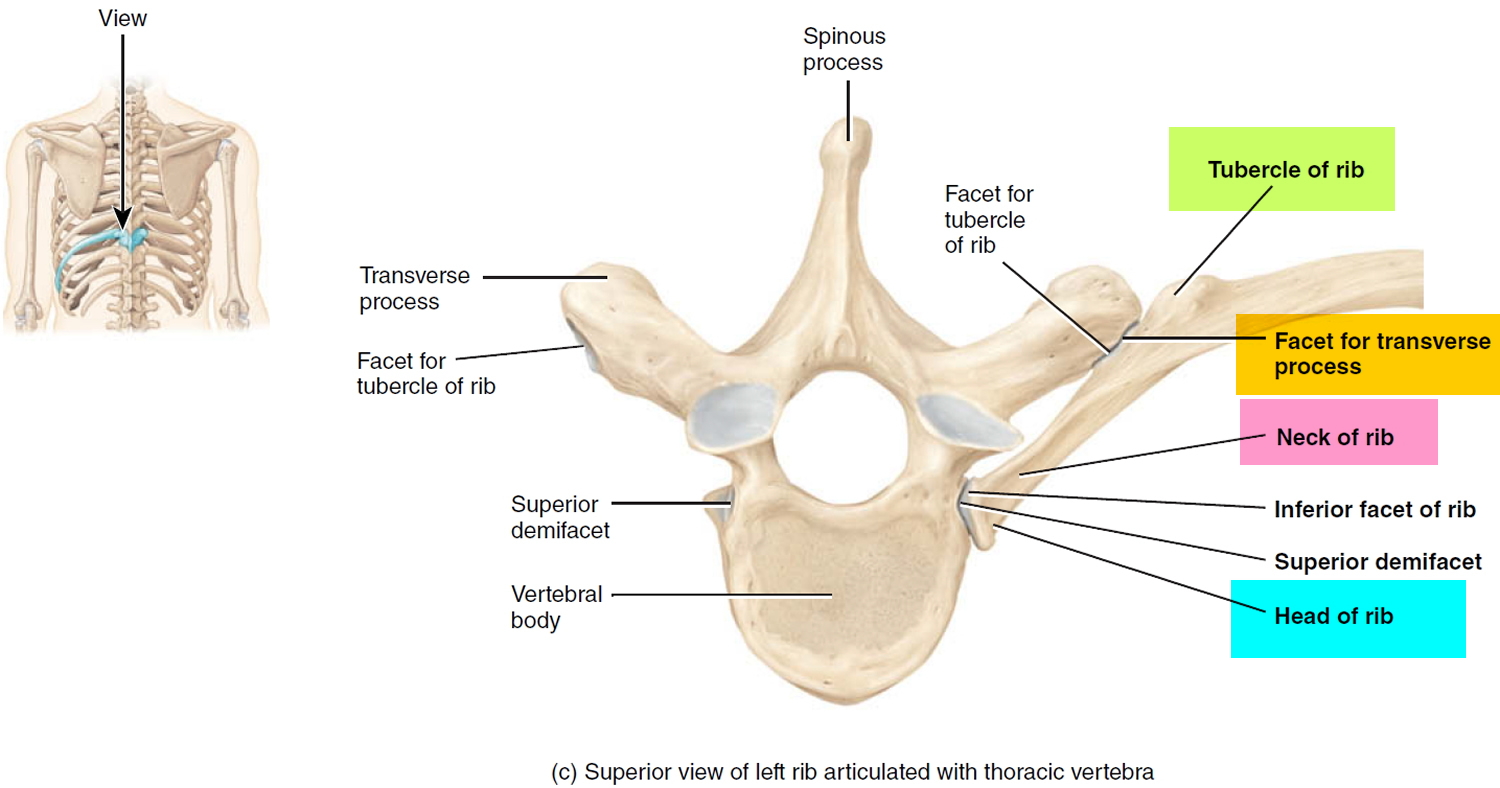
Figure 3. Rib articulation with the thoracic vertebra
Broken rib causes
Broken ribs are most commonly caused by direct impacts — such as those from motor vehicle accidents, falls, child abuse or contact sports. Ribs also can be fractured by repetitive trauma from sports like golf and rowing or from severe and prolonged coughing.
Blunt force is the common cause of injury
Rib injuries typically occur when the chest is directly hit. Situations that could cause blunt injuries to the ribcage include:
- Motor vehicle accidents – for example, slamming the chest against the steering wheel
- Crush injuries – for example, a heavy object landing directly on the chest
- Sports-related injuries – for example, a heavy tackle
- Falling from a reasonable height – for example, off a roof or ladder
- Assault – for example, getting hit by a baseball bat.
Risk factors for broken ribs
The following factors can increase your risk of breaking a rib:
- Osteoporosis. Having this disease in which your bones lose their density makes you more susceptible to a bone fracture.
- Sports participation. Playing contact sports, such as hockey or football, increases your risk of trauma to your chest.
- Cancerous lesion in a rib. A cancerous lesion can weaken the bone, making it more susceptible to breaks.
Broken rib prevention
The following measures may help you prevent a broken rib:
- Protect yourself from athletic injuries. Wear protective equipment when playing contact sports.
- Reduce your risk of household falls. Remove clutter from your floors and clean spills promptly, use a rubber mat in the shower, keep your home well-lit, and put skidproof backing on carpets and area rugs.
- Strengthen your bones. Getting enough calcium and vitamin D in your diet is important for maintaining strong bones. Aim for about 1,200 milligrams of calcium and 600 International Units of vitamin D daily from food and supplements.
Broken rib signs and symptoms
Broken rib can cause severe pain, particularly when people breathe deeply. The pain lasts for weeks.
Because of the pain, people may breathe less deeply, increasing the risk of complications, such as collapse of parts of the lung (atelectasis) and pneumonia.
Complications are more likely to occur in:
- Older people
- People with several rib fractures
Because older people are more likely to develop these complications, they also have a higher risk of death due to a rib fracture than do younger people.
Broken rib symptoms include:
- Strong pain in your chest area, particularly when you breathe in
- Pain when the ribcage flexes – with movement, with a deep breath or when you cough, sneeze or laugh
- Swelling or tenderness around the affected ribs
- Muscle spasms of the ribcage
- Crunching or grinding sounds (crepitus) when the injury site is touched or moved
- Muscle spasms of the ribcage
- Sometimes bruising on the skin
- Feeling or hearing a crack if it’s a broken rib
- Muscle spasms of the ribcage
Ribs can’t be easily splinted or supported like other bones, so they’re usually left to heal naturally. There’s often no need for an X-ray.
Soft tissue injuries
Soft tissue of the ribcage includes the intercostal muscles and the costal cartilage. Common injuries include:
- Bruising – the blood vessels rupture and leak blood into the surrounding tissues. Bruising of the chest wall is a common rib trauma.
- Intercostal strains – intercostal muscles allow the ribcage to move up and down. These muscles can be strained by any activity that involves extreme or forceful twisting of the body or swinging of the arms. Sports that commonly cause this type of injury include golf and tennis.
- Costochondral separation – the rib is torn loose from the costal cartilage and is detached from the sternum.
Broken rib diagnosis
During the physical exam, your doctor will press gently on your ribs. He or she might also listen to your lungs and watch your rib cage move as you breathe.
Your doctor likely will order one or more of the following imaging tests:
- X-ray. Using low levels of radiation, X-rays make bones visible. But X-rays often have problems revealing fresh rib fractures, especially if the bone is merely cracked. X-rays are also useful in diagnosing a collapsed lung.
- CT scan. This often can uncover rib fractures that X-rays might miss. Injuries to soft tissues and blood vessels are also easier to see on CT scans. This technology takes X-rays from a variety of angles and combines them to depict cross-sectional slices of your body’s internal structures.
- MRI. This can be used to look at the soft tissues and organs around the ribs to determine if there’s damage. It can also help in the detection of more subtle rib fractures. An MRI uses a powerful magnet and radio waves to produce cross-sectional images.
- Bone scan. This technique is good for viewing stress fractures, where a bone is cracked after repetitive trauma — such as long bouts of coughing. During a bone scan, a small amount of radioactive material is injected into your bloodstream. It collects in the bones, particularly in places where a bone is healing, and is detected by a scanner.
Broken rib treatment
Unlike bones of the arms and legs, broken ribs can’t be set in a cast. Most broken ribs heal on their own within six weeks. Treatment aims to relieve pain while the injury heals, which can take up to six weeks (in the case of fracture), and 12 weeks or more if the rib has been torn from the cartilage. Treatment for bruised ribs is the same as for fractured ribs, but with a shorter recovery time.
Restricting activities and icing the area regularly can help with healing and pain relief.
How to treat broken ribs yourself
Options include:
- Rest
- Prescription strength pain-killing drugs
- Non-steroidal anti-inflammatory drugs (NSAIDs)
- Avoiding activities that aggravate the injury, such as sport
- Icepacks – may help to reduce inflammation in the early stages
- Mechanical ventilation (help with breathing) – may be needed in cases of severe flail chest.
Medications
It’s important to obtain adequate pain relief — if it hurts to breathe deeply, you may develop pneumonia. If oral medications don’t help enough, your doctor might suggest injections of long-lasting anesthesia around the nerves that supply the ribs.
How to heal broken ribs faster
DO
- take painkillers such as paracetamol or ibuprofen – avoid taking ibuprofen for 48 hours after your injury as it may slow down healing
- hold an ice pack (or bag of frozen peas in a tea towel) to the affected ribs regularly in the first few days to bring down swelling
- rest and take time off work if you need to
- breathe normally and cough when you need to – this helps clear mucus from your lungs to prevent chest infections
- if you need to cough, hold a pillow against your chest
- walk around and sometimes move your shoulders to help you breathe and clear mucus from your lungs
- take 10 slow, deep breaths every hour to help clear your lungs
- try to sleep more upright for the first few nights
DON’T
- wrap a bandage tightly around your chest to stop your lungs expanding properly
- lie down or stay still for a long time
- strain yourself or lift heavy objects
- play any sports or do any exercise that makes your pain worse
- smoke – stopping smoking may also help your recovery
Therapy
Once your pain is under control, your doctor might prescribe breathing exercises to help you breathe more deeply because shallow breathing can put you at risk of developing pneumonia.
- In the past, doctors would use compression wraps — elastic bandages that you can wrap around your chest — to help splint and immobilize the area. Compression wraps aren’t recommended for broken ribs anymore because they can keep you from breathing deeply, which can increase the risk of pneumonia.