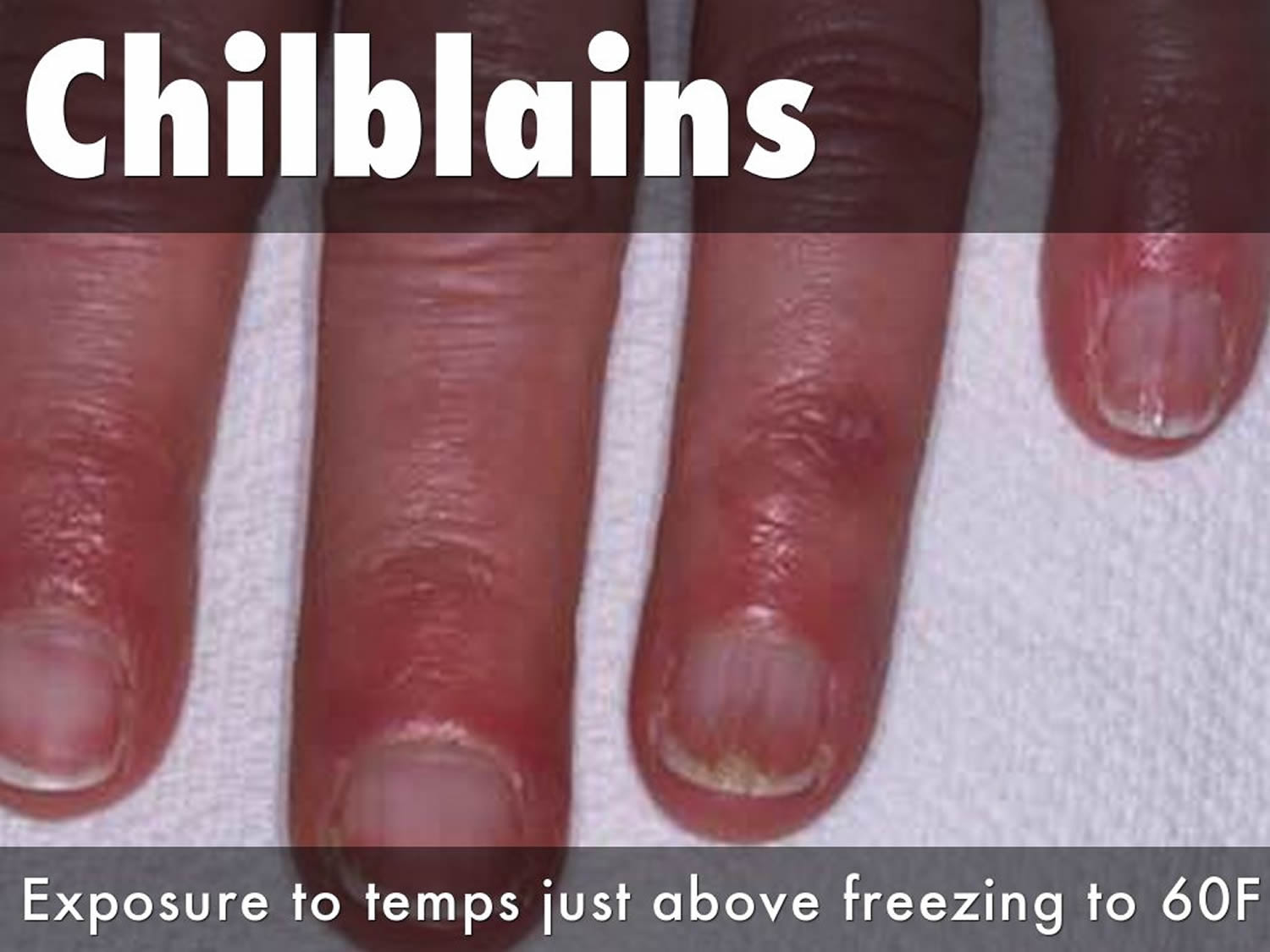
What are chilblains
Chilblains are itchy, swollen and painful inflammation of small blood vessels in your skin, forming after exposure to cold but not freezing air and damp conditions 1. Also known as pernio, chilblains can cause itching, red patches, swelling and blistering on your hands and feet. They usually affect fingers and toes but can also appear on the nose and ears 2. They’re not the same as frostbite which is more serious.
Characteristically, chilblains begin in the fall or winter and disappear in the spring or early summer. There is controversy regarding whether dry cold or dampness is more likely to cause chilblains 3, 4. In advanced cases, the seasonal variation may disappear and chronic occlusive vascular disease may develop.
Chilblains do not cause lasting damage. Chilblains usually clear up within one to three weeks, especially if the weather gets warmer. However, the affected area might stay sensitive to cold after they heal. You may have recurrences seasonally for years. Treatment involves protecting yourself from the cold and using lotions to ease the symptoms. Chilblains don’t usually result in permanent injury. But the condition can lead to infection, which may cause severe damage if left untreated.
The best approach to chilblains is to avoid developing them by limiting your exposure to cold, dressing warmly and covering exposed skin.
Symptoms of chilblains
Chilblains can appear quickly. The affected area might be itchy, reddish blue, swollen and painful due to inflammation. Blisters containing clear fluid may also form.
Signs and symptoms of chilblains may include:
- Small, itchy red areas on your skin, often on your feet or hands
- Possible blistering or skin ulcers
- Swelling of your skin
- Burning sensation on your skin
- Changes in skin color from red to dark blue, accompanied by pain
When to see a doctor
Chilblains will usually get better on their own. Seek medical care to check for complications if the pain is unusually severe, if you suspect an infection, or if your symptoms aren’t improving after one to two weeks. If the symptoms extend into the warm season, see a doctor to rule out other conditions.
- If you have diabetes or poor circulation, healing may be impaired. Be cautious and seek care.
Causes of chilblains
No one knows exactly what causes chilblains 2. They may be an abnormal reaction of your body to cold exposure followed by rewarming. Rewarming of cold skin can cause small blood vessels under the skin to expand more quickly than nearby larger blood vessels can handle. This results in a bottleneck effect and the blood leaking into nearby tissues.
Risk factors of chilblains
Factors that may increase your risk of chilblains include:
- Clothing that is tight or exposes skin to the cold. Wearing tight-fitting clothing and shoes in cold, damp weather may make you more susceptible to chilblains. And skin that’s exposed to cold, damp conditions is more likely to develop chilblains.
- Your sex and weight. Women are more likely to get chilblains than are children and males. Also, people who weigh about 20 percent less than is expected for their height have an increased risk of chilblains.
- Environment and season. Chilblains are less likely in colder and drier areas because the living conditions and clothing used in these areas are more protective against cold. Your risk of chilblains is higher if you live in an area with high humidity and cold, but not freezing, temperatures. They are more common from November to April.
- Having poor circulation. People with poor circulation tend to be more sensitive to changes in temperature, making them more susceptible to chilblains.
- Having been diagnosed with Raynaud’s disease. People with Raynaud’s disease are more susceptible to chilblains. Either condition can result in sores, but Raynaud’s causes different types of color changes on the skin.
Complications of chilblains
Chilblains may cause complications if your skin blisters. If that happens, you may develop ulcers and infections. Besides being painful, infections are potentially life-threatening if left untreated. See a doctor if you suspect infection.
Prevention of chilblains
To prevent chilblains:
- Avoid or limit your exposure to cold.
- Dress in layers of loose clothing and wear mittens and warm, water-resistant footwear.
- Cover all exposed skin as completely as possible when going outside in cold weather.
- Keep your hands, feet and face dry and warm.
- Keep your home and workplace comfortably warm.
- Don’t smoke.
If your skin is exposed to cold, it’s helpful to rewarm it gradually because sudden rewarming of cold skin may worsen chilblains.
Diagnosis of Chilblains
You generally won’t need to see your doctor for chilblains. If you do visit your doctor, he or she will be able to diagnose your skin condition by looking at it and talking with you about any recent cold exposure. The exam might also include checking your circulation.
He or she may do further tests, such as a skin biopsy, to rule out other causes for your signs and symptoms.
Treatment of Chilblains
In most cases, you will be able to treat your chilblains yourself. You can 5:
- use lanolin-based creams to ease the itching and swelling
- avoid scratching which delays healing and can cause infection
- massage the affected area if it’s not too painful or ulcerated
- keep the affected area warm but not hot.
They should disappear within 2-3 weeks. Once you have been affected, chilblains can recur after even brief exposure to cold, so it’s important to stay warm.
See your doctor if the symptoms remain or you can’t get the pain under control. Your doctor might prescribe:
For adults whose chilblains don’t clear up with home remedies, treatment may include prescription drugs:
- Topical corticosteroid. A corticosteroid such as triamcinolone 0.1 percent cream is applied to the affected area.
- Blood pressure medicine. A blood pressure lowering drug called nifedipine (Procardia). Nifedipine, which blood vessels to dilate, has been demonstrated to be effective in reducing pain, facilitating healing, and preventing new lesions of pernio.
Home remedies for Chilblains
Chilblains usually clear up in one to three weeks after cold exposure. In the meantime, you can take steps to ease your signs and symptoms, including:
- Rewarming affected skin gently, without massaging, rubbing or applying direct heat
- Avoiding cold exposure whenever possible
- Keeping your affected skin dry and warm, but away from sources of heat
- Applying lotion to alleviate itching
- Making sure the affected skin is cleaned with an antiseptic and gently bandaged to prevent infection
- Avoiding scratching.
What is Chilblain Lupus Erythematosus
Chilblain lupus erythematosus is a chronic form of lupus erythematosus seen especially in women, affecting the fingertips, rims of ears, calves, and heels 6. Chilblain lupus erythematosus lesions may be clinically indistinguishable from simple chilblains or pernio due to exposure to cold air (see above), which is seen in healthy individuals.
Lupus is a chronic systemic autoimmune disease that occurs when your body’s immune system attacks your own tissues and organs 7. The main role of your immune system is to fight foreign invaders such as bacteria, fungi and viruses. In autoimmune diseases the immune system produces antibodies that attack your body’s own healthy tissue. Lupus is an autoimmune disease, and the antibodies produced by the immune system in lupus cause inflammation, tissue damage and pain.
Inflammation caused by lupus can affect many different body systems — including your joints, skin, kidneys, blood cells, brain, heart and lungs.
Types of Lupus
There are many different types of lupus 8:
- Systemic lupus erythematosus (also known as SLE) can affect almost any organ or system. Systemic lupus erythematosus is characterised by flare ups and periods of improvement (remissions), and can can affect almost any organ or system of the body 9. In most people only the skin and joints are affected. However, in some people SLE can also affect the kidneys, lungs, heart, blood vessels and/or brain.
- Discoid lupus (also known as chronic cutaneous lupus erythematosus) is generally milder than SLE and usually appears as a red scaly rash on sun exposed areas such as the face, scalp, arms, legs or trunk. Most people with discoid lupus have symptoms only on their skin. However, a small number of people with discoid lupus will develop SLE. chronic cutaneous lupus erythematosus is generally milder, with most people having only skin symptoms.
- Subacute cutaneous lupus is similar, but milder still. Subacute cutaneous lupus main symptoms are skin rashes, sun sensitivity and joint aches.
- Drug-induced lupus – this is usually a transient form that develops as a reaction to certain medications and clears up when the medications are ceased.
Lupus is fairly rare. About 90 per cent of people with lupus are women and the majority develop the condition between 15 and 45 years.
Lupus can be difficult to diagnose because its signs and symptoms often mimic those of other ailments. The most distinctive sign of lupus — a facial rash that resembles the wings of a butterfly unfolding across both cheeks — occurs in many but not all cases of lupus (see Figure 2).
Some people are born with a tendency toward developing lupus, which may be triggered by infections, certain drugs or even sunlight. While there’s no cure for lupus, treatments can help control symptoms.
Figure 1. Chilblain lupus erythematosus
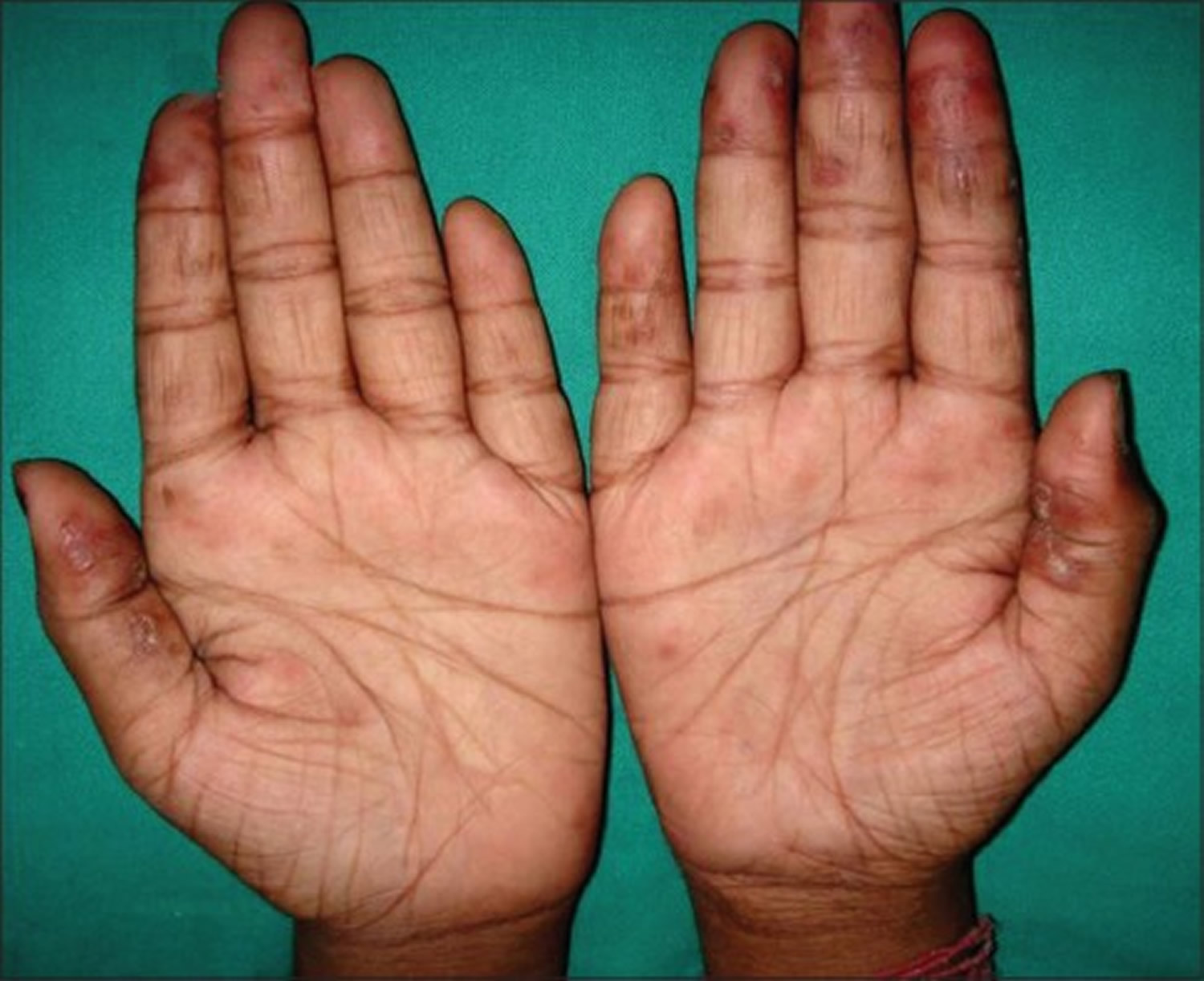
Figure 2. Lupus facial rash
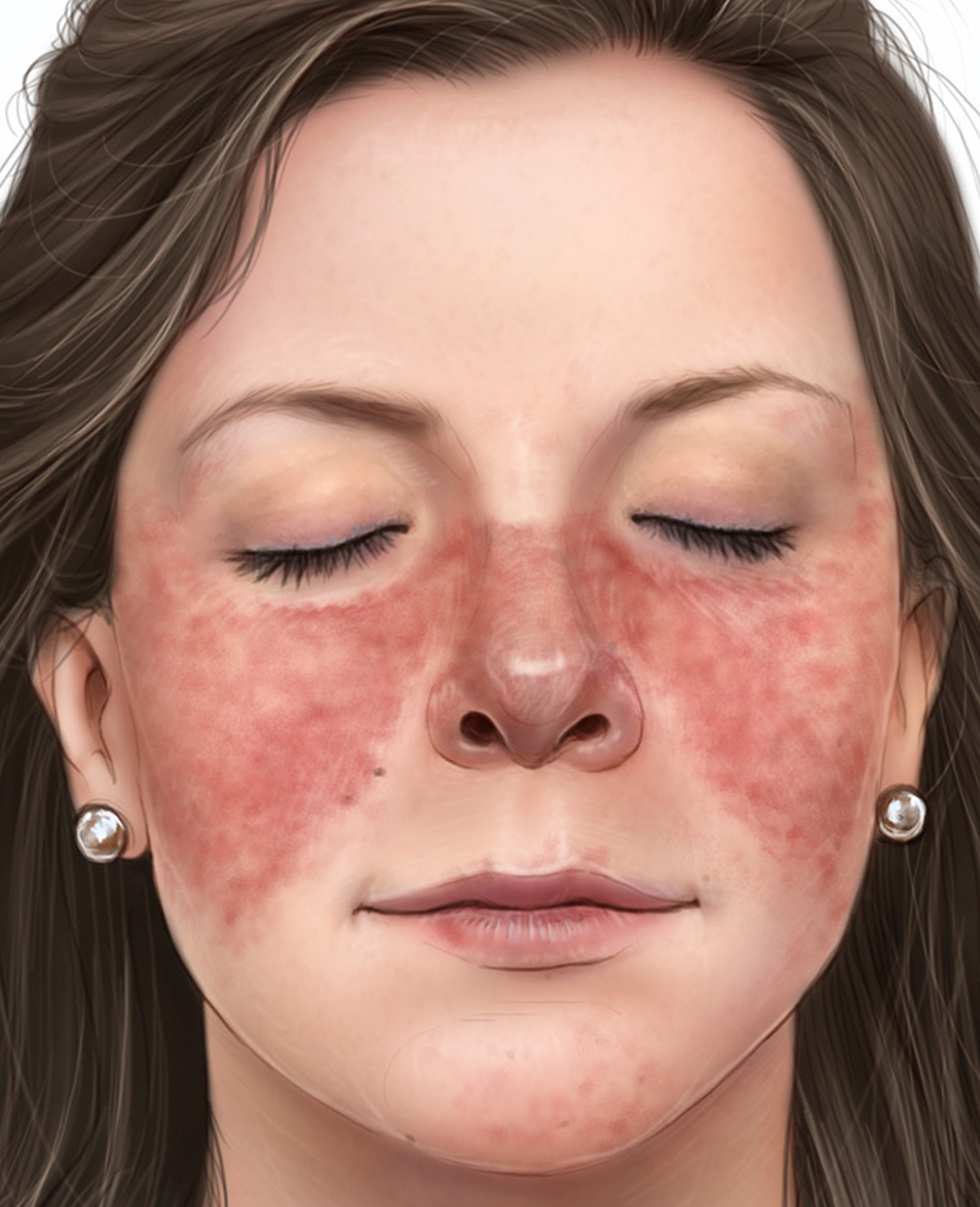
Note: A typical sign of lupus is a red, butterfly-shaped rash over your cheeks and nose, often following exposure to sunlight.
Symptoms of lupus
Symptoms can be vague and vary greatly from person to person. The most common symptoms include pain, stiffness or swelling in joints, skin rashes, fever and feeling tired. Diagnosing it is difficult and may take some time.
No two cases of lupus are exactly alike. Signs and symptoms may come on suddenly or develop slowly, may be mild or severe, and may be temporary or permanent. Most people with lupus have mild disease characterized by episodes — called flares — when signs and symptoms get worse for a while, then improve or even disappear completely for a time.
The signs and symptoms of lupus that you experience will depend on which body systems are affected by the disease. The most common signs and symptoms include:
- Fatigue
- Fever
- Joint pain, stiffness and swelling
- Butterfly-shaped rash on the face that covers the cheeks and bridge of the nose or rashes elsewhere on the body
- Skin lesions that appear or worsen with sun exposure (photosensitivity)
- Fingers and toes that turn white or blue when exposed to cold or during stressful periods (Raynaud’s phenomenon)
- Shortness of breath
- Chest pain
- Dry eyes
- Headaches, confusion and memory loss
When to see a doctor
See your doctor if you develop an unexplained rash, ongoing fever, persistent aching or fatigue.
Causes of lupus
Lupus occurs when your immune system attacks healthy tissue in your body (autoimmune disease). It’s likely that lupus results from a combination of your genetics and your environment.
It appears that people with an inherited predisposition for lupus may develop the disease when they come into contact with something in the environment that can trigger lupus. The cause of lupus in most cases, however, is unknown. Some potential triggers include:
- Sunlight. Exposure to the sun may bring on lupus skin lesions or trigger an internal response in susceptible people.
- Infections. Having an infection can initiate lupus or cause a relapse in some people.
- Medications. Lupus can be triggered by certain types of blood pressure medications, anti-seizure medications and antibiotics. People who have drug-induced lupus usually get better when they stop taking the medication. Rarely, symptoms may persist even after the drug is stopped.
Risk factors of lupus
Factors that may increase your risk of lupus include:
- Your sex. Lupus is more common in women.
- Age. Although lupus affects people of all ages, it’s most often diagnosed between the ages of 15 and 45.
- Race. Lupus is more common in African-Americans, Hispanics and Asian-Americans.
Complications of lupus
Inflammation caused by lupus can affect many areas of your body, including your:
- Kidneys. Lupus can cause serious kidney damage, and kidney failure is one of the leading causes of death among people with lupus.
- Brain and central nervous system. If your brain is affected by lupus, you may experience headaches, dizziness, behavior changes, vision problems, and even strokes or seizures. Many people with lupus experience memory problems and may have difficulty expressing their thoughts.
- Blood and blood vessels. Lupus may lead to blood problems, including anemia and increased risk of bleeding or blood clotting. It can also cause inflammation of the blood vessels (vasculitis).
- Lungs. Having lupus increases your chances of developing an inflammation of the chest cavity lining (pleurisy), which can make breathing painful. Bleeding into lungs and pneumonia also are possible.
- Heart. Lupus can cause inflammation of your heart muscle, your arteries or heart membrane (pericarditis). The risk of cardiovascular disease and heart attacks increases greatly as well.
Other types of complications
Having lupus also increases your risk of:
- Infection. People with lupus are more vulnerable to infection because both the disease and its treatments can weaken the immune system.
- Cancer. Having lupus appears to increase your risk of cancer; however the risk is small.
- Bone tissue death (avascular necrosis). This occurs when the blood supply to a bone diminishes, often leading to tiny breaks in the bone and eventually to the bone’s collapse.
- Pregnancy complications. Women with lupus have an increased risk of miscarriage. Lupus increases the risk of high blood pressure during pregnancy (preeclampsia) and preterm birth. To reduce the risk of these complications, doctors often recommend delaying pregnancy until your disease has been under control for at least six months.
Lupus and pregnancy
Women with lupus should talk to their doctor before considering pregnancy. They should be made aware of any potential risk for themselves and the baby. It is preferable for lupus to be in remission, as this reduces the risk of a disease flare occurring during pregnancy. Lupus flares occurring during pregnancy are usually mild and occur in the first three months (trimester). In the first few weeks after birth new mothers may experience lupus flares but this can be controlled with corticosteroids.
It is important to discuss therapy options with your doctor to ensure that any current medication taken will not adversely affect the pregnancy. Women should have no difficulty becoming pregnant as lupus does not usually lower fertility. However, a small proportion of women with lupus are at increased risk of blood clots and recurrent miscarriages.
Diagnosis of lupus
Diagnosing lupus is difficult because signs and symptoms vary considerably from person to person. Signs and symptoms of lupus may vary over time and overlap with those of many other disorders.
No one test can diagnose lupus. The combination of blood and urine tests, signs and symptoms, and physical examination findings leads to the diagnosis.
Laboratory tests
Blood and urine tests may include:
- Complete blood count. This test measures the number of red blood cells, white blood cells and platelets as well as the amount of hemoglobin, a protein in red blood cells. Results may indicate you have anemia, which commonly occurs in lupus. A low white blood cell or platelet count may occur in lupus as well.
- Erythrocyte sedimentation rate. This blood test determines the rate at which red blood cells settle to the bottom of a tube in an hour. A faster than normal rate may indicate a systemic disease, such as lupus. The sedimentation rate isn’t specific for any one disease. It may be elevated if you have lupus, an infection, another inflammatory condition or cancer.
- Kidney and liver assessment. Blood tests can assess how well your kidneys and liver are functioning. Lupus can affect these organs.
Urinalysis. An examination of a sample of your urine may show an increased protein level or red blood cells in the urine, which may occur if lupus has affected your kidneys. - Antinuclear antibody (ANA) test. A positive test for the presence of these antibodies — produced by your immune system — indicates a stimulated immune system. While most people with lupus have a positive ANA test, most people with a positive ANA do not have lupus. If you test positive for ANA, your doctor may advise more-specific antibody testing.
Imaging tests
If your doctor suspects that lupus is affecting your lungs or heart, he or she may suggest:
- Chest X-ray. An image of your chest may reveal abnormal shadows that suggest fluid or inflammation in your lungs.
- Echocardiogram. This test uses sound waves to produce real-time images of your beating heart. It can check for problems with your valves and other portions of your heart.
Biopsy
Lupus can harm your kidneys in many different ways, and treatments can vary, depending on the type of damage that occurs. In some cases, it’s necessary to test a small sample of kidney tissue to determine what the best treatment might be. The sample can be obtained with a needle or through a small incision.
Skin biopsy is sometimes performed to confirm a diagnosis of lupus affecting the skin.
Treatment of lupus
Treatment for lupus depends on your signs and symptoms. Determining whether your signs and symptoms should be treated and what medications to use requires a careful discussion of the benefits and risks with your doctor.
As your signs and symptoms flare and subside, you and your doctor may find that you’ll need to change medications or dosages. The medications most commonly used to control lupus include:
- Nonsteroidal anti-inflammatory drugs (NSAIDs). Over-the-counter NSAIDs, such as naproxen sodium (Aleve) and ibuprofen (Advil, Motrin IB, others), may be used to treat pain, swelling and fever associated with lupus. Stronger NSAIDs are available by prescription. Side effects of NSAIDs include stomach bleeding, kidney problems and an increased risk of heart problems.
- Antimalarial drugs. Medications commonly used to treat malaria, such as hydroxychloroquine (Plaquenil), affect the immune system and can help decrease the risk of lupus flares. Side effects can include stomach upset and, very rarely, damage to the retina of the eye. Regular eye exams are recommended when taking these medications.
- Corticosteroids. Prednisone and other types of corticosteroids can counter the inflammation of lupus. High doses of steroids such as methylprednisolone (A-Methapred, Medrol) are often used to control serious disease that involves the kidneys and brain. Side effects include weight gain, easy bruising, thinning bones (osteoporosis), high blood pressure, diabetes and increased risk of infection. The risk of side effects increases with higher doses and longer term therapy.
- Immunosuppressants. Drugs that suppress the immune system may be helpful in serious cases of lupus. Examples include azathioprine (Imuran, Azasan), mycophenolate mofetil (CellCept) and methotrexate (Trexall). Potential side effects may include an increased risk of infection, liver damage, decreased fertility and an increased risk of cancer.
- Biologics. A different type of medication, belimumab (Benlysta) administered intravenously, also reduces lupus symptoms in some people. Side effects include nausea, diarrhea and infections. Rarely, worsening of depression can occur.
- Rituximab (Rituxan) can be beneficial in cases of resistant lupus. Side effects include allergic reaction to the intravenous infusion and infections.
Home remedies for Lupus
Take steps to care for your body if you have lupus. Simple measures can help you prevent lupus flares and, should they occur, better cope with the signs and symptoms you experience. Try to:
- See your doctor regularly. Having regular checkups instead of only seeing your doctor when your symptoms worsen may help your doctor prevent flare-ups, and can be useful in addressing routine health concerns, such as stress, diet and exercise that can be helpful in preventing lupus complications.
- Be sun smart. Because ultraviolet light can trigger a flare, wear protective clothing — such as a hat, long-sleeved shirt and long pants — and use sunscreens with a sun protection factor (SPF) of at least 55 every time you go outside.
- Get regular exercise. Exercise can help keep your bones strong, reduce your risk of heart attack and promote general well-being.
- Don’t smoke. Smoking increases your risk of cardiovascular disease and can worsen the effects of lupus on your heart and blood vessels.
- Eat a healthy diet. A healthy diet emphasizes fruits, vegetables and whole grains. Sometimes you may have dietary restrictions, especially if you have high blood pressure, kidney damage or gastrointestinal problems.
- Ask your doctor if you need vitamin D and calcium supplements. There is some evidence to suggest that people with lupus may benefit from supplemental vitamin D. A 1,200- to 1,500-milligram calcium supplement taken daily may help keep your bones healthy.
Alternative medicine
Sometimes people with lupus seek alternative or complementary medicine. However, there aren’t any alternative therapies that have been shown to alter the course of lupus, although some may help ease symptoms of the disease.
Discuss these treatments with your doctor before initiating them on your own. He or she can help you weigh the benefits and risks and tell you if the treatments will interfere adversely with your current lupus medications.
Complementary and alternative treatments for lupus include:
- Dehydroepiandrosterone (DHEA). Supplements containing this hormone may help fatigue and muscle pain. It may lead to acne in women.
- Fish oil. Fish oil supplements contain omega-3 fatty acids that may be beneficial for people with lupus. Preliminary studies have found some promise, though more study is needed. Side effects of fish oil supplements can include nausea, belching and a fishy taste in the mouth.
- Acupuncture. This therapy uses tiny needles inserted just under the skin. It may help ease the muscle pain associated with lupus.
- Pernio in Pediatrics. Pediatrics September 2005, VOLUME 116 / ISSUE 3. http://pediatrics.aappublications.org/content/116/3/e472.long[↩]
- Chilblains. Mayo Clinic. https://www.mayoclinic.org/diseases-conditions/chilblains/symptoms-causes/syc-20351097[↩][↩]
- Fritz RL, Perrin DH. Cold exposure injuries: prevention and treatment. Clin Sports Med.1989;8 :111– 128[↩]
- Weston WL, Morelli JG. Childhood pernio and cryoproteins. Pediatr Dermatol.2000;17 :97– 99[↩]
- Chilblains. Health Direct. https://www.healthdirect.gov.au/chilblains[↩]
- Bansal S, Goel A. Chilblain lupus erythematosus in an adolescent girl. Indian Dermatology Online Journal. 2014;5(Suppl 1):S30-S32. doi:10.4103/2229-5178.144522. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4252947/[↩]
- Lupus. Mayo Clinic. https://www.mayoclinic.org/diseases-conditions/lupus/symptoms-causes/syc-20365789[↩]
- Lupus. Health Direct. https://www.healthdirect.gov.au/lupus[↩]
- Systemic Lupus Erythematosis (SLE). Australasian Society of Clinical Immunology and Allergy. https://www.allergy.org.au/patients/autoimmunity/systemic-lupus-erythematosus-sle[↩]