Contents
Human heart
Your heart is a strong muscle about the size of the palm of your hand. Your body depends on the heart’s pumping action to deliver oxygen- and nutrient-rich blood to the body’s cells. When the cells are nourished properly, the body can function normally. Just like an engine makes a car go, the heart keeps your body running. The heart has two pumps. The stronger pump uses arteries to send blood with oxygen away from the heart, throughout the body. The other pump uses veins to bring blood back to the heart and sends it to the lungs to get more oxygen. An electrical system in the heart controls the heart’s pumps (the heart beat or pulse).
How the Heart Works
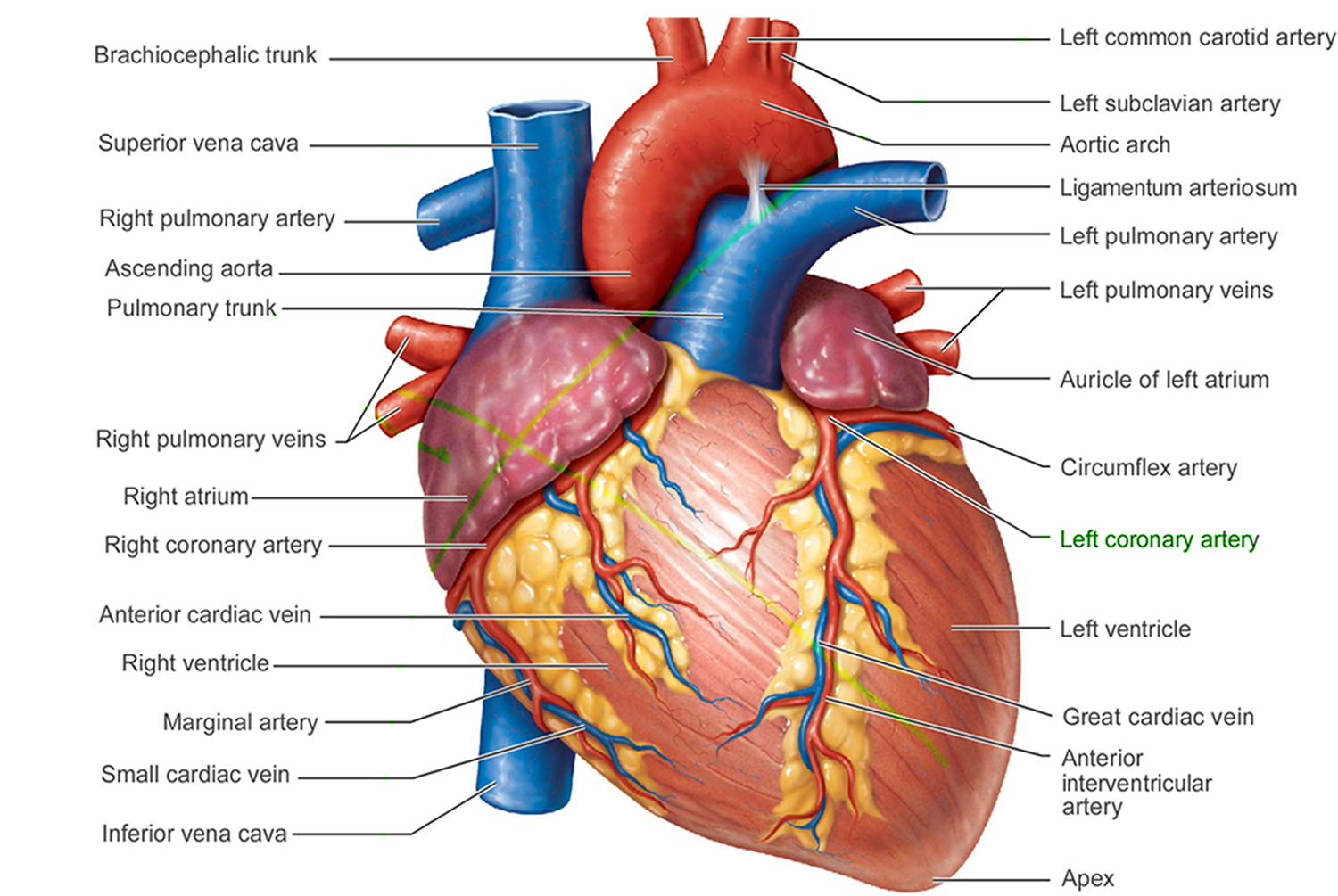
Figure 1. The anatomy of the heart
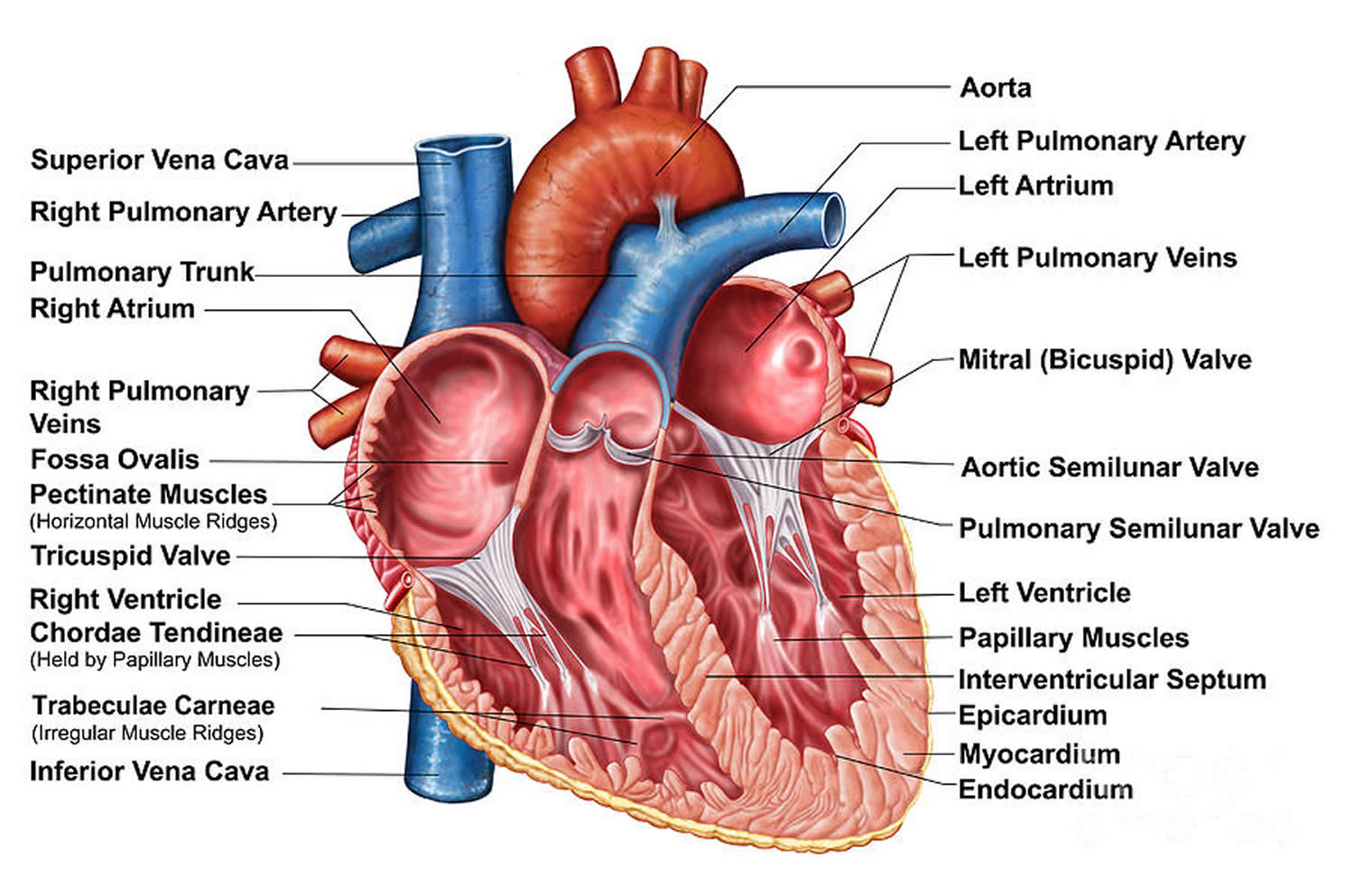
Figure 2. The anatomy of the heart chambers
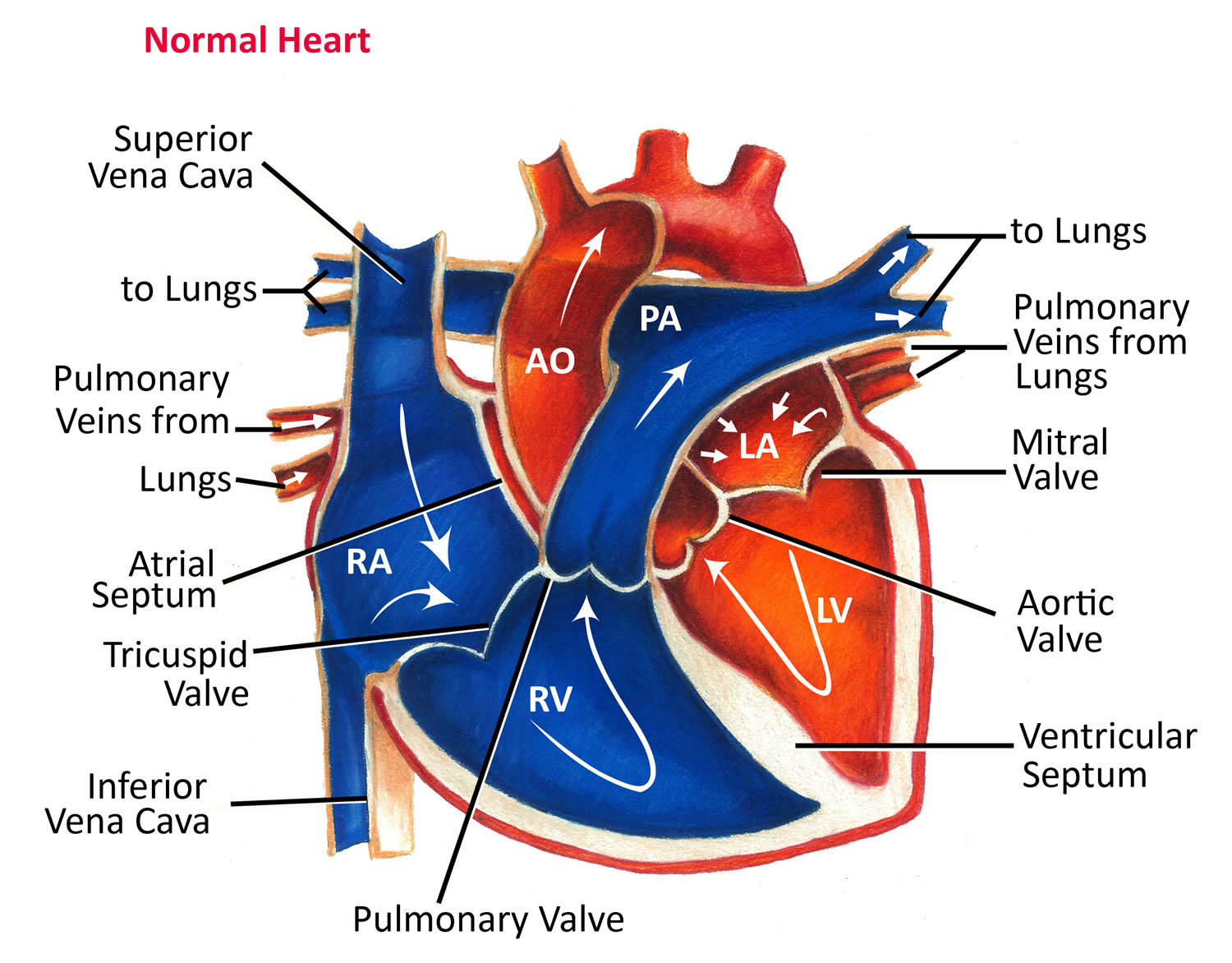
Figure 3. Normal heart blood flow
The heart has two sides, separated by an inner wall called the septum. The right side of the heart pumps blood to the lungs to pick up oxygen. The left side of the heart receives the oxygen-rich blood from the lungs and pumps it to the body.
The heart has four chambers 1, two on the right and two on the left:
- Two upper chambers are called atrium (two is called an atria). The atria collect blood as it flows into the heart.
- Two lower chambers are called ventricles. The ventricles pump blood out of the heart to the lungs or other parts of the body.
The heart also has four valves that open and close to let blood flow from the atria to the ventricles and from the ventricles into the two large arteries connected to the heart in only one direction when the heart contracts (beats). The four heart valves are:
- Tricuspid valve, located between the right atrium and right ventricle
- Pulmonary or pulmonic valve, between the right ventricle and the pulmonary artery. This artery carries blood from the heart to the lungs.
- Mitral valve, between the left atrium and left ventricle
- Aortic valve, between the left ventricle and the aorta. This aorta carries blood from the heart to the body.
Each valve has a set of flaps (also called leaflets or cusps). The mitral valve has two flaps; the others have three. Valves are like doors that open and close. They open to allow blood to flow through to the next chamber or to one of the arteries. Then they shut to keep blood from flowing backward. Blood flow occurs only when there’s a difference in pressure across the valves, which causes them to open. Under normal conditions, the valves permit blood to flow in only one direction.
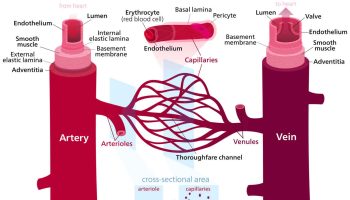
The heart four chambers and four valves and is connected to various blood vessels. Veins are blood vessels that carry blood from the body to the heart. Arteries are blood vessels that carry blood away from the heart to the body.
The heart pumps blood to the lungs and to all the body’s tissues by a sequence of highly organized contractions of the four chambers. For the heart to function properly, the four chambers must beat in an organized way.
When the heart’s valves open and close, they make a “lub-DUB” sound that a doctor can hear using a stethoscope 2.
- The first sound—the “lub”—is made by the mitral and tricuspid valves closing at the beginning of systole. Systole is when the ventricles contract, or squeeze, and pump blood out of the heart.
- The second sound—the “DUB”—is made by the aortic and pulmonary valves closing at the beginning of diastole. Diastole is when the ventricles relax and fill with blood pumped into them by the atria.
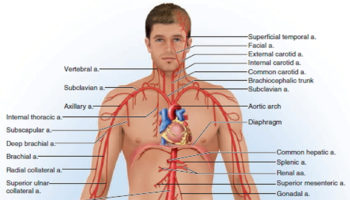
Arteries
The arteries are major blood vessels connected to your heart.
- The pulmonary artery carries blood from the right side of the heart to the lungs to pick up a fresh supply of oxygen.
- The aorta is the main artery that carries oxygen-rich blood from the left side of the heart to the body.
- The coronary arteries are the other important arteries attached to the heart. They carry oxygen-rich blood from the aorta to the heart muscle, which must have its own blood supply to function.
Veins
The veins also are major blood vessels connected to your heart.
- The pulmonary veins carry oxygen-rich blood from the lungs to the left side of the heart so it can be pumped to the body.
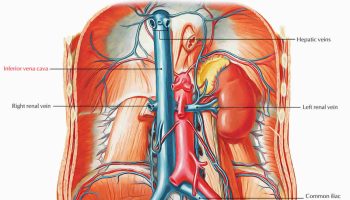
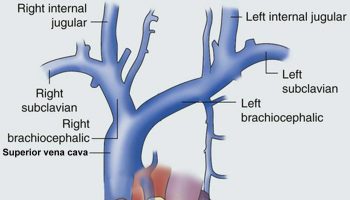
- The superior and inferior vena cavae are large veins that carry oxygen-poor blood from the body back to the heart.
Blood Flow
- The Right Side of Your Heart
In figure 3 above, the superior and inferior vena cavae are shown in blue to the left of the heart muscle as you look at the picture. These veins are the largest veins in your body.
After your body’s organs and tissues have used the oxygen in your blood, the vena cavae carry the oxygen-poor blood back to the right atrium of your heart.
The superior vena cava carries oxygen-poor blood from the upper parts of your body, including your head, chest, arms, and neck. The inferior vena cava carries oxygen-poor blood from the lower parts of your body.
The oxygen-poor blood from the vena cavae flows into your heart’s right atrium. From the right atrium, blood is pumped into the right ventricle. And then from the right ventricle, blood is pumped to your lungs through the pulmonary arteries (shown in blue in the center of figure 3).
Once in the lungs, the blood travels through many small, thin blood vessels called capillaries. There, the blood picks up more oxygen and transfers carbon dioxide to the lungs—a process called gas exchange.
The oxygen-rich blood passes from your lungs back to your heart through the pulmonary veins (shown in red to the left of the right atrium in figure 3).
- The Left Side of Your Heart
Oxygen-rich blood from your lungs passes through the pulmonary veins (shown in red to the right of the left atrium in figure 3 above). The blood enters the left atrium and is pumped into the left ventricle.
From the left ventricle, the oxygen-rich blood is pumped to the rest of your body through the aorta. The aorta is the main artery that carries oxygen-rich blood to your body.
Like all of your organs, your heart needs oxygen-rich blood. As blood is pumped out of your heart’s left ventricle, some of it flows into the coronary arteries (shown in red in figure 3).
Your coronary arteries are located on your heart’s surface at the beginning of the aorta. They carry oxygen-rich blood to all parts of your heart.
For the heart to work well, your blood must flow in only one direction. Your heart’s valves make this possible. Both of your heart’s ventricles have an “in” (inlet) valve from the atria and an “out” (outlet) valve leading to your arteries.
Healthy valves open and close in exact coordination with the pumping action of your heart’s atria and ventricles. Each valve has a set of flaps called leaflets or cusps that seal or open the valve. This allows blood to pass through the chambers and into your arteries without backing up or flowing backward.
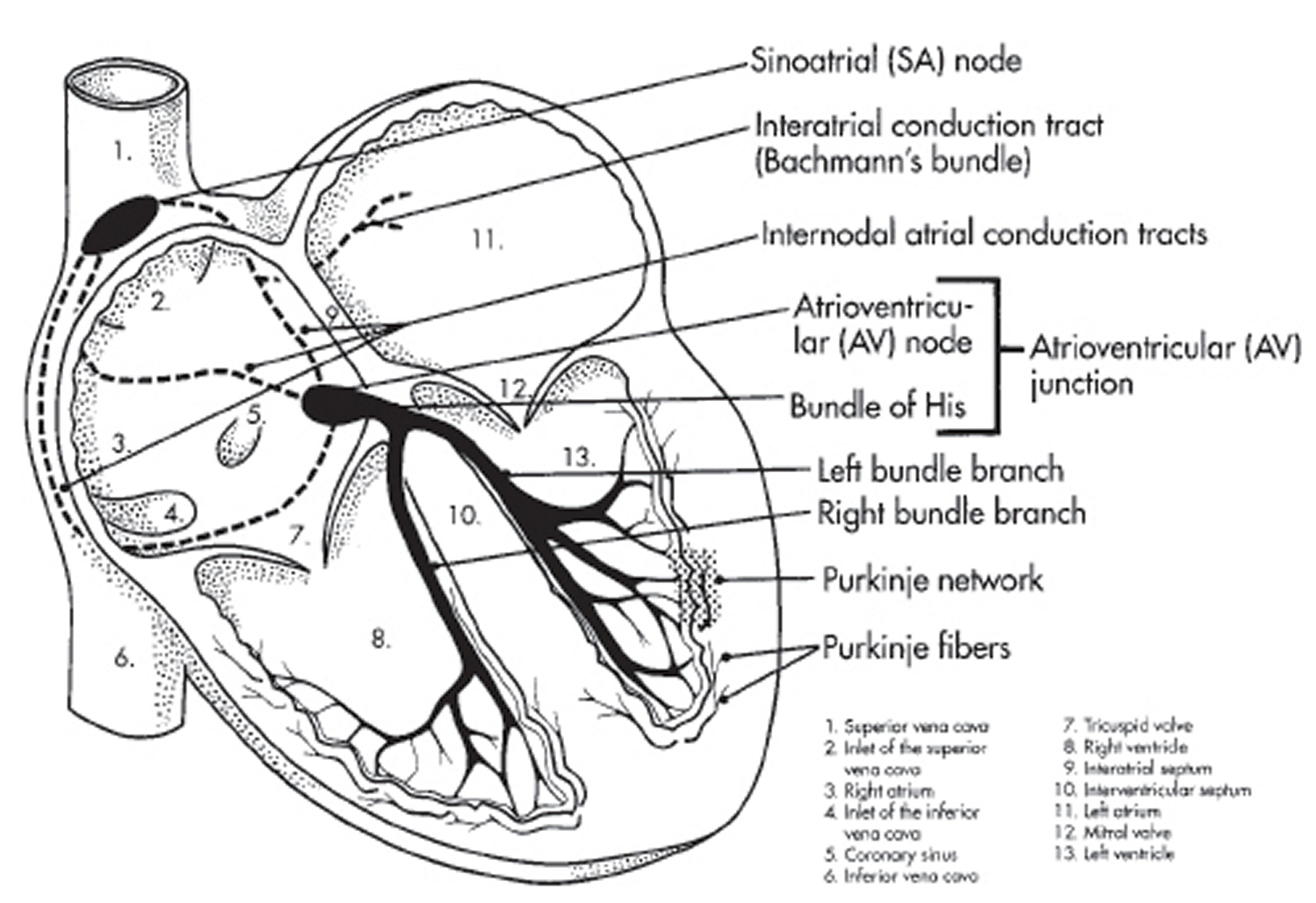
Understanding the Heart’s Electrical System
The heart’s electrical system controls the rate and rhythm of the heartbeat.
With each heartbeat, an electrical signal spreads from the top of the heart to the bottom. As the signal travels, it causes the heart to contract and pump blood.
Your heart’s electrical system controls all the events that occur when your heart pumps blood 3. The electrical system also is called the cardiac conduction system. If you’ve ever seen the heart test called an EKG (electrocardiogram), you’ve seen a graphical picture of the heart’s electrical activity.
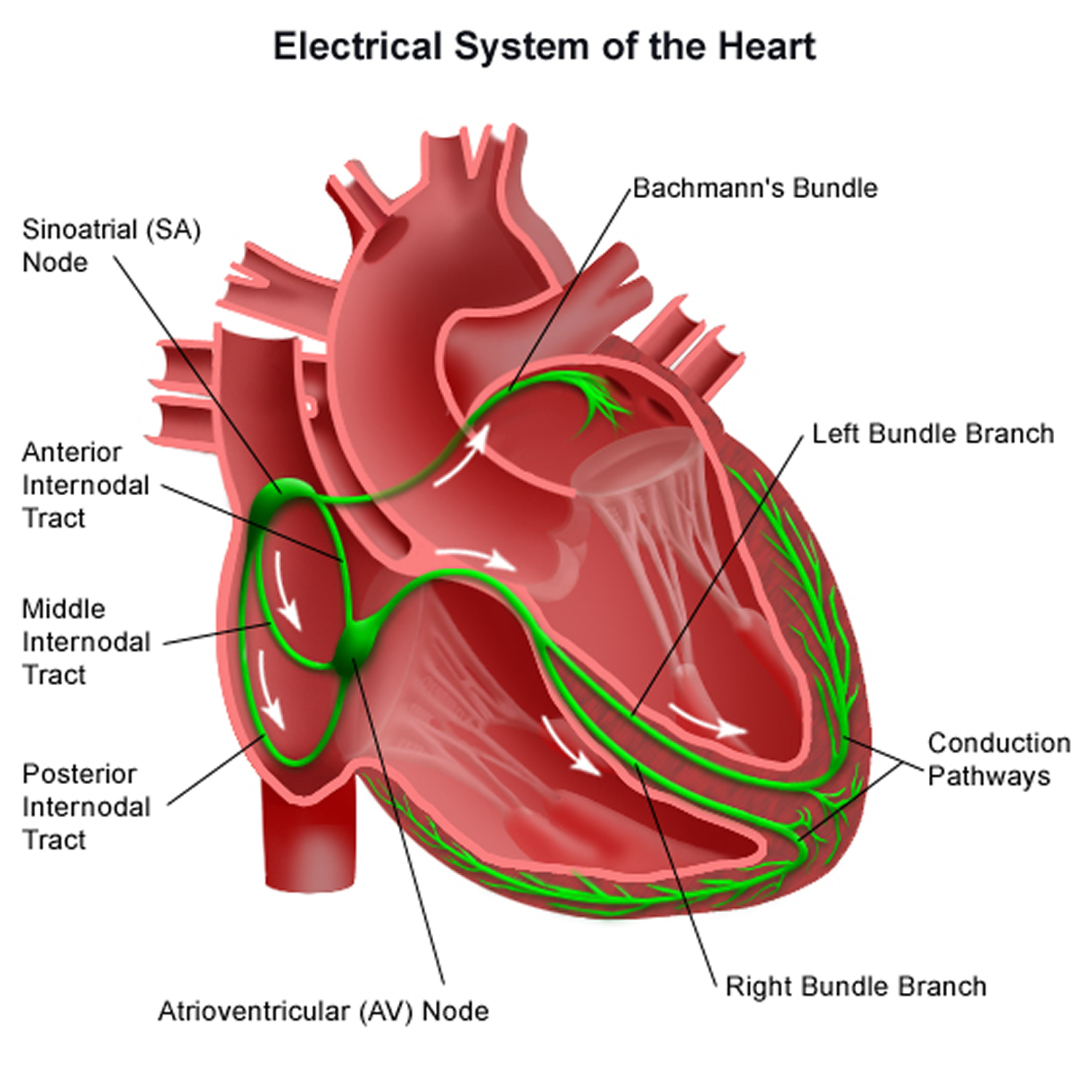
Your heart’s electrical system is made up of three main parts:
- The Sinoatrial (SA) node, located in the right atrium of your heart
- The Atrioventricular (AV) node, located on the interatrial septum close to the tricuspid valve
- The His-Purkinje system, located along the walls of your heart’s ventricles
A heartbeat is a complex series of events. These events take place inside and around your heart. A heartbeat is a single cycle in which your heart’s chambers relax and contract to pump blood. This cycle includes the opening and closing of the inlet and outlet valves of the right and left ventricles of your heart.
Each heartbeat has two basic parts: diastole and systole. During diastole, the atria and ventricles of your heart relax and begin to fill with blood.
At the end of diastole, your heart’s atria contract (atrial systole) and pump blood into the ventricles. The atria then begin to relax. Your heart’s ventricles then contract (ventricular systole), pumping blood out of your heart.
Each electrical signal begins in a group of cells called the sinus node or sinoatrial (SA) node. The SA node is located in the heart’s upper right chamber, the right atrium. In a healthy adult heart at rest, the SA node fires off an electrical signal to begin a new heartbeat 60 to 100 times a minute. In a normal, healthy heart, each beat begins with a signal from the SA node. This is why the SA node sometimes is called your heart’s natural pacemaker. Your pulse, or heart rate, is the number of signals the SA node produces per minute.
The signal is generated as the vena cavae fill your heart’s right atrium with blood from other parts of your body. The signal spreads across the cells of your heart’s right and left atria.
From the SA node, the electrical signal travels through special pathways in the right and left atria. This causes the atria to contract and pump blood through the open valves from the atria into heart’s two lower chambers, the ventricles.
The electrical signal then moves down to a group of cells called the atrioventricular (AV) node, located between the atria and the ventricles. Here, the signal slows down just a little, allowing your heart’s right and left ventricles time to finish filling with blood.
The electrical signal then leaves the AV node and travels along a pathway called the bundle of His. This pathway divides into a right bundle branch and a left bundle branch. The signal goes down these branches to the ventricles, causing them to contract and pump blood to the lungs and the rest of the body.
From the bundle of His, the signal fibers divide into left and right bundle branches through the Purkinje fibers. These fibers connect directly to the cells in the walls of your heart’s left and right ventricles.
The signal spreads across the cells of your ventricle walls, and both ventricles contract. However, this doesn’t happen at exactly the same moment.
The left ventricle contracts an instant before the right ventricle. This pushes blood through the pulmonary valve (for the right ventricle) to your lungs, and through the aortic valve (for the left ventricle) to the rest of your body.
As the signal passes, the walls of the ventricles relax and await the next signal.
This process continues over and over as the atria refill with blood and more electrical signals come from the SA node.
A problem with any part of this process can cause an arrhythmia. For example, in atrial fibrillation, a common type of arrhythmia, electrical signals travel through the atria in a fast and disorganized way. This causes the atria to quiver instead of contract.
Figure 4. The heart’s electrical system
How to keep your heart healthy
You can help prevent heart disease by doing four key things and making them into habits:
- Don’t smoke (or quit if you do). Smoking adds to the damage to artery walls. It’s never too late to get some benefit from quitting smoking. Quitting, even in later life, can over time, lower your risk of heart disease and cancer.
- Maintain a healthy weight. Your healthcare provider will probably check your weight and height to learn your BMI (body mass index). A BMI of 25 or higher means you are at greater risk for heart disease as well as diabetes (high blood sugar) and other health conditions. Extra fat around the middle of your body may increase your risk of heart disease. A man’s risk of heart disease is increased if his waist measures more than 40 inches. A woman’s risk is increased at 35 inches. Following a healthy eating plan and being physically active might help you.
- Exercise; be active. If possible, aim to get at least 30 minutes of moderate-intensity activity on most or all days of the week. Every day is best. It doesn’t have to be done all at once—10-minute periods will do. Start by doing activities you enjoy—brisk walking, dancing, bowling, bicycling, or gardening, for example.
- Follow a healthy diet. Choose low-fat foods and those that are low in salt. Eat plenty of fruits, vegetables, and foods high in fiber like those made from whole grains. And if you drink alcohol, men should not have more than two drinks a day and women only one.
A heart-healthy lifestyle can help you prevent a heart attack and it includes heart-healthy eating, being physically active, quitting smoking, managing stress, and managing your weight.
In the United States, coronary heart disease is a leading cause of death for both men and women. Each year, about 370,000 Americans die from coronary heart disease 4.
Certain traits, conditions, or habits may raise your risk for coronary heart disease. The more risk factors you have, the more likely you are to develop the disease.
You can control many risk factors, which may help prevent or delay coronary heart disease.
Major Risk Factors
- Unhealthy blood cholesterol levels. This includes high LDL cholesterol (sometimes called “bad” cholesterol) and low HDL cholesterol (sometimes called “good” cholesterol). Your doctor can check the cholesterol in your blood with a blood test. This will tell you your overall or total cholesterol level as well as the LDLs (“bad” cholestrol), HDLs (“healthy” cholesterol), and triglycerides (another type of fat in the blood that puts you at risk for heart problems). High blood cholesterol levels could add to the plaque in your arteries.
- High blood pressure. Blood pressure is considered high if it stays at or above 140/90 mmHg over time. If you have diabetes or chronic kidney disease, high blood pressure is defined as 130/80 mmHg or higher. (The mmHg is millimeters of mercury—the units used to measure blood pressure.)
- Smoking. Smoking can damage and tighten blood vessels, lead to unhealthy cholesterol levels, and raise blood pressure. Smoking also can limit how much oxygen reaches the body’s tissues.
- Insulin resistance. This condition occurs if the body can’t use its own insulin properly. Insulin is a hormone that helps move blood sugar into cells where it’s used for energy. Insulin resistance may lead to diabetes.
- Diabetes. With this disease, the body’s blood sugar level is too high because the body doesn’t make enough insulin or doesn’t use its insulin properly.
Overweight or obesity. The terms “overweight” and “obesity” refer to body weight that’s greater than what is considered healthy for a certain height. - Metabolic syndrome. Metabolic syndrome is the name for a group of risk factors that raises your risk for coronary heart disease and other health problems, such as diabetes and stroke.
- Lack of physical activity. Being physically inactive can worsen other risk factors for coronary heart disease, such as unhealthy blood cholesterol levels, high blood pressure, diabetes, and overweight or obesity.
- Unhealthy diet. An unhealthy diet can raise your risk for coronary heart disease. Foods that are high in saturated and trans fats, cholesterol, sodium, and sugar can worsen other risk factors for coronary heart disease.
- Older age. Genetic or lifestyle factors cause plaque to build up in your arteries as you age. In men, the risk for coronary heart disease increases starting at age 45. In women, the risk for coronary heart disease increases starting at age 55.
- A family history of early coronary heart disease is a risk factor for developing coronary heart disease, specifically if a father or brother is diagnosed before age 55, or a mother or sister is diagnosed before age 65.
Although older age and a family history of early heart disease are risk factors, it doesn’t mean that you’ll develop coronary heart disease if you have one or both. Controlling other risk factors often can lessen genetic influences and help prevent coronary heart disease, even in older adults.
Other conditions and factors also may contribute to coronary heart disease, including:
- Sleep apnea. Sleep apnea is a common disorder in which you have one or more pauses in breathing or shallow breaths while you sleep. Untreated sleep apnea can increase your risk for high blood pressure, diabetes, and even a heart attack or stroke.
- Stress. Research shows that the most commonly reported “trigger” for a heart attack is an emotionally upsetting event, especially one involving anger.
- Alcohol. Heavy drinking can damage the heart muscle and worsen other coronary heart disease risk factors. Men should have no more than two drinks containing alcohol a day. Women should have no more than one drink containing alcohol a day.
- Preeclampsia. This condition can occur during pregnancy. The two main signs of preeclampsia are a rise in blood pressure and excess protein in the urine. Preeclampsia is linked to an increased lifetime risk of heart disease, including coronary heart disease, heart attack, heart failure, and high blood pressure.
Table 1. Lifestyle factors for healthy heart
| Goal/Metric | Ideal Heart Health Condition |
|---|---|
| *The committee selected 5 aspects of diet to define a healthy dietary score. The score is not intended to be comprehensive. Rather, it is a practical approach that provides individuals with a set of potential concrete actions. A comprehensive rationale is set forth in the text of this document, and a comprehensive set of nutrition recommendations is provided in the 2006 Nutrition Guidelines 5, 6, 7. | |
| †Untreated values. | |
| Current smoking | |
| Adults >20 y of age | Never or quit >12 mo ago |
| Children 12–19 y of age | Never tried; never smoked whole cigarette |
| Body mass index | |
| Adults >20 y of age | <25 kg/m2 |
| Children 2–19 y of age | <85th Percentile |
| Physical activity | |
| Adults >20 y of age | ≥150 min/wk moderate intensity or ≥75 min/wk vigorous intensity or combination |
| Children 12–19 y of age | ≥60 min of moderate- or vigorous-intensity activity every day |
| Healthy diet score* | |
| Adults >20 y of age | 4–5 Components* |
| Children 5–19 y of age | 4–5 Components* |
| Total cholesterol | |
| Adults >20 y of age | <200 mg/dL† |
| Children 6–19 y of age | <170 mg/dL† |
| Blood pressure | |
| Adults >20 y of age | <120/<80 mm Hg† |
| Children 8–19 y of age | <90th Percentile† |
| Fasting plasma glucose | |
| Adults >20 y of age | <100 mg/dL† |
| Children 12–19 y of age | <100 mg/dL† |
Following a healthy lifestyle can help you and your children prevent or control many coronary heart disease risk factors.
Because many lifestyle habits begin during childhood, parents and families should encourage their children to make heart healthy choices. For example, you and your children can lower your risk of coronary heart disease if you maintain a healthy weight, follow a healthy diet, do physical activity regularly, and don’t smoke.
Strong studies make it possible to link reductions in risk to these habits. Following a healthy lifestyle may prevent over 80% of cases of coronary artery disease 9, 10, 50% of ischemic strokes 11, 80% of sudden cardiac deaths 12 and 72% of premature deaths related to heart disease 13. In other words, a healthy lifestyle is a good investment in a longer, healthier life.
Changes to Your Heart With Age
Aging can cause changes in the heart and blood vessels. For example, as you get older, your heart can’t beat as fast during physical activity or stress as when you were younger. However, the number of heart beats per minute (heart rate) at rest does not change as you age 14.
Many of the problems older people have with their heart and blood vessels are really caused by disease, not by aging. For example, an older heart can normally pump blood as strong as a younger heart; less ability to pump blood is caused by disease. But, changes that happen with age may increase a person’s risk of heart disease. The good news is there are things you can do to delay, lower, or possibly avoid or reverse your risk.
A common problem related to aging is “hardening of the arteries,” called arteriosclerosis. This problem is why blood pressure goes up with age.
Age can cause other changes to the heart 14. For example:
- Blood vessels can become stiffer, and some parts of the heart wall will thicken to help with blood flow.
- Your heart valves may become thicker and stiffer, causing leaks or problems with pumping blood out of the heart.
- The size of the sections of your heart may increase.
Other factors, such as thyroid disease or chemotherapy, may weaken the heart muscle. Things you can’t control, like your family history, might also increase your risk of heart disease. But even so, leading a heart-healthy lifestyle might help you avoid or delay serious illness 14.
Check Your Blood Pressure
As you get older, it is important for you to have your blood pressure checked regularly, even if you are healthy. You may feel fine, but if not treated, high blood pressure can lead to stroke and problems with your heart, eyes, and kidneys. Exercise and reducing salt in your diet can help, but often medication is needed to manage high blood pressure and the related problems.
Heart Disease
There are many different kinds of heart disease. The most common is atherosclerosis, the buildup of fatty deposits or plaques in the walls of arteries. As plaque builds up, there is less space for blood to flow normally and deliver oxygen throughout the body, including to the heart. Depending on where the buildup is, it can cause a heart attack, leg pain, or a stroke. Atherosclerosis is not part of normal aging and can be serious. There are choices you can make to prevent or delay heart disease, including:
- Don’t smoke
- Stay at a healthy weight
- Avoid spending hours every day sitting
- Exercise
- Keep your diabetes, high blood pressure, and/or high cholesterol under control
- Manage your stress
- Don’t drink a lot of alcohol
Heart rate
Your heart rate, or pulse, is the number of times your heart beats per minute. Normal heart rate varies from person to person. Knowing yours can be an important heart-health gauge.
According to the National Institute of Health, the average resting heart rate:
- for children 10 years and older, and adults (including seniors) is 60 – 100 beats per minute
- for well-trained athletes is 40 – 60 beats per minute.
As you age, changes in the rate and regularity of your pulse can change and may signify a heart condition or other condition that needs to be addressed.
The best places to find your pulse are the:
- wrists
- inside of your elbow
- side of your neck
- top of the foot
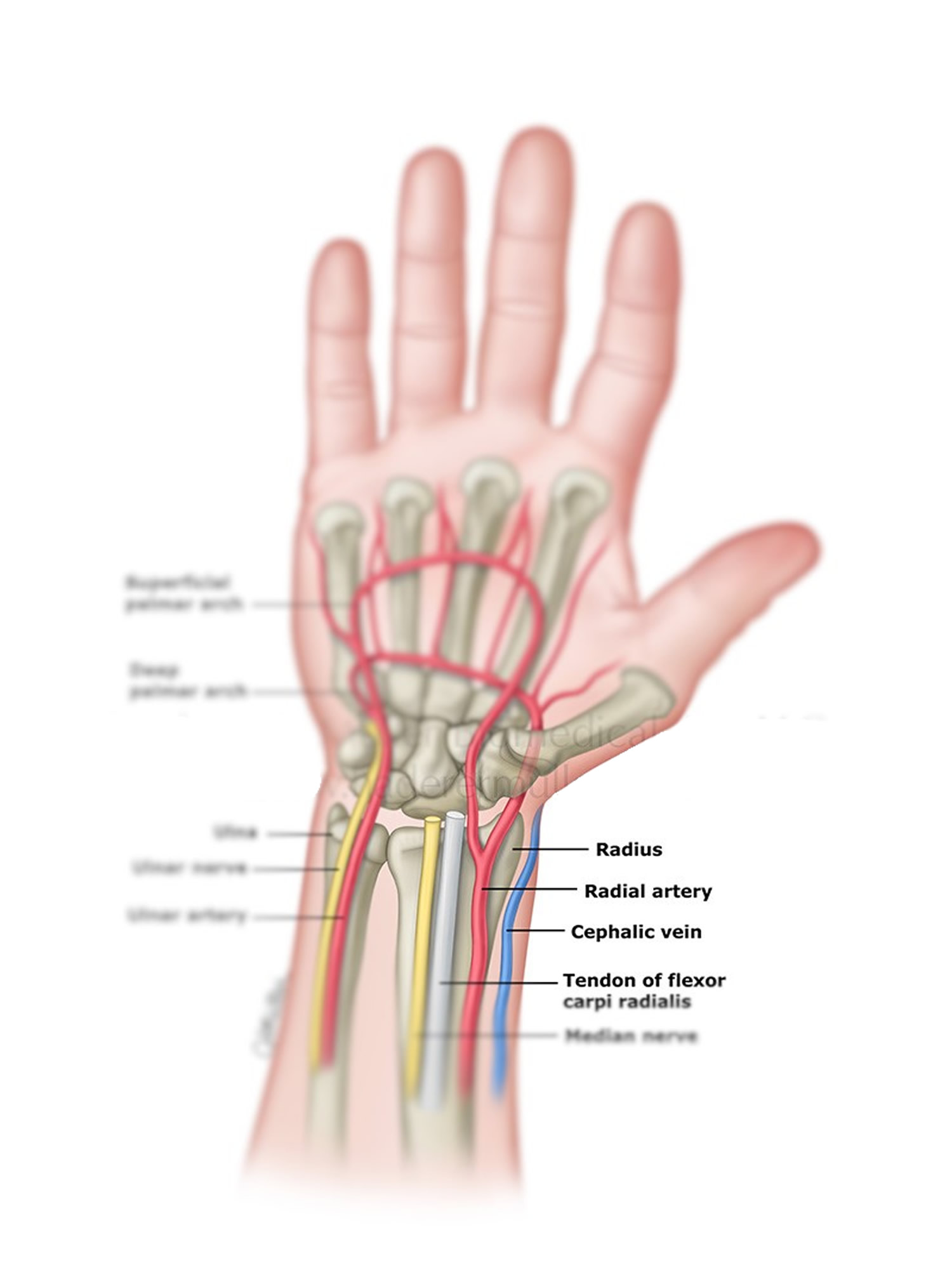
Figure 5. Radial artery at the wrist and taking a radial pulse
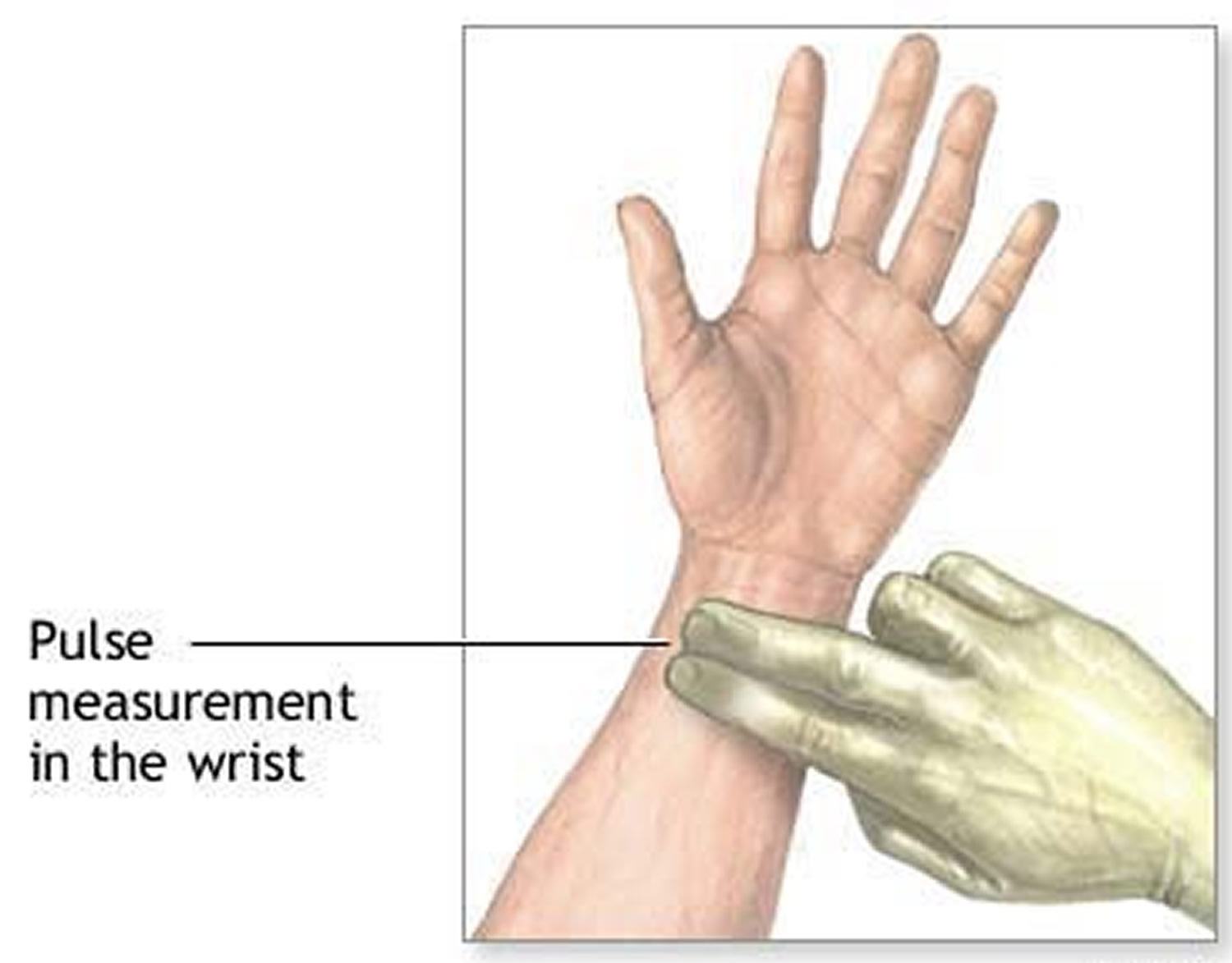
To get the most accurate reading, put your finger over your pulse and count the number of beats in 60 seconds.
How to take your pulse at the wrist:
- Take your pulse on the inside of your wrist, on the thumb side.
- Use the tips of your first two fingers (not your thumb) to press lightly over the blood vessels on your wrist.
- Count your pulse for 10 seconds and multiply by 6 to find your beats per minute.
Your resting heart rate is the heart pumping the lowest amount of blood you need because you’re not exercising. If you’re sitting or lying and you’re calm, relaxed and aren’t ill, your heart rate is normally between 60 (beats per minute) and 100 (beats per minute).
But a heart rate lower than 60 doesn’t necessarily signal a medical problem. It could be the result of taking a drug such as a beta blocker. A lower heart rate is also common for people who get a lot of physical activity or are very athletic. Active people often have lower heart rates because their heart muscle is in better condition and doesn’t need to work as hard to maintain a steady beat.
Moderate physical activity doesn’t usually change the resting pulse much. If you’re very fit, it could change to 40 beats per minute. A less active person might have a heart rate between 60 and 100 beats per minute. That’s because the heart muscle has to work harder to maintain bodily functions, making it higher.
How Other Factors Affect Heart Rate
- Air temperature: When temperatures (and the humidity) soar, the heart pumps a little more blood, so your pulse rate may increase, but usually no more than five to 10 beats a minute.
- Body position: Resting, sitting or standing, your pulse is usually the same. Sometimes as you stand for the first 15 to 20 seconds, your pulse may go up a little bit, but after a couple of minutes it should settle down.
- Emotions: If you’re stressed, anxious or “extraordinarily happy or sad” your emotions can raise your pulse.
- Body size: Body size usually doesn’t change pulse. If you’re very obese, you might see a higher resting pulse than normal, but usually not more than 100.
- Medication use: Medications that block your adrenaline (beta blockers) tend to slow your pulse, while too much thyroid medication or too high of a dosage will raise it.
- Energy drinks.
- Caffeine in beverages and foods.
How do you get your heart rate on target during exercise ?
When you work out, are you doing too much or not enough ?
There’s a simple way to know: Your target heart rate helps you hit the bull’s eye.
This table shows estimated target heart rates for different ages.
- Your maximum heart rate is about 220 minus your age.
In the age category closest to yours, read across to find your target heart rate. Heart rate during moderately intense activities is about 50-69% of your maximum heart rate, whereas heart rate during hard physical activity is about 70% to less than 90% of the maximum heart rate.
The figures are averages, so use them as general guidelines.
Table 1. Target heart rate during exercise
| Age | Target HR Zone 50-85% | Average Maximum Heart Rate, 100% |
|---|---|---|
| 20 years | 100-170 beats per minute | 200 beats per minute |
| 30 years | 95-162 beats per minute | 190 beats per minute |
| 35 years | 93-157 beats per minute | 185 beats per minute |
| 40 years | 90-153 beats per minute | 180 beats per minute |
| 45 years | 88-149 beats per minute | 175 beats per minute |
| 50 years | 85-145 beats per minute | 170 beats per minute |
| 55 years | 83-140 beats per minute | 165 beats per minute |
| 60 years | 80-136 beats per minute | 160 beats per minute |
| 65 years | 78-132 beats per minute | 155 beats per minute |
| 70 years | 75-128 beats per minute | 150 beats per minute |
Important Note: A few high blood pressure medications lower the maximum heart rate and thus the target zone rate. If you’re taking such medicine, call your physician to find out if you need to use a lower target heart rate.
If your heart rate is too high, you’re straining. So slow down. If it’s too low, and the intensity feels “light” or “moderate/brisk,” you may want to push yourself to exercise a little harder.
During the first few weeks of working out, aim for the lower ranger of your target zone (50 percent) and gradually build up to the higher range (85 percent). After six months or more, you may be able to exercise comfortably at up to 85 percent of your maximum heart rate.
Normal Blood Pressure
Blood pressure is the force of blood pushing against the walls of the arteries as the heart pumps blood 16. High blood pressure, sometimes called hypertension, happens when this force is too high. Health care workers check blood pressure readings the same way for children, teens, and adults. They use a gauge, stethoscope or electronic sensor, and a blood pressure cuff. With this equipment, they measure:
- Systolic Pressure: blood pressure when the heart beats while pumping blood.
- Diastolic Pressure: blood pressure when the heart is at rest between beats.
Normal blood pressure for adults is defined as a systolic pressure below 120 mmHg and a diastolic pressure below 80 mmHg. It is normal for blood pressures to change when you sleep, wake up, or are excited or nervous. When you are active, it is normal for your blood pressure to increase. However, once the activity stops, your blood pressure returns to your normal baseline range.
Blood pressure normally rises with age and body size. Newborn babies often have very low blood pressure numbers that are considered normal for babies, while older teens have numbers similar to adults.
Abnormal Blood Pressure
Abnormal increases in blood pressure are defined as having blood pressures higher than 120/80 mmHg. The following table outlines and defines high blood pressure severity levels.
Table 2. Stages of High Blood Pressure in Adults
| Stages | Systolic (top number) | Diastolic (bottom number) | |
|---|---|---|---|
| Prehypertension | 120–139 | OR | 80–89 |
| High blood pressure Stage 1 | 140–159 | OR | 90–99 |
| High blood pressure Stage 2 | 160 or higher | OR | 100 or higher |
The ranges in the table are blood pressure guides for adults who do not have any short-term serious illnesses. People with diabetes or chronic kidney disease should keep their blood pressure below 130/80 mmHg.
Although blood pressure increases seen in prehypertension are less than those used to diagnose high blood pressure, prehypertension can progress to high blood pressure and should be taken seriously. Over time, consistently high blood pressure weakens and damages your blood vessels, which can lead to complications.
- American Heart Association. About Arrhythmia. http://www.heart.org/HEARTORG/Conditions/Arrhythmia/AboutArrhythmia/About-Arrhythmia_UCM_002010_Article.jsp[↩]
- Centers for Disease Control and Prevention. Division of Birth Defects and Developmental Disabilities. Congenital Heart Defects (CHDs). https://www.cdc.gov/ncbddd/heartdefects/index.html[↩]
- National Institutes of Health. National Heart, Lung and Blood Institute. Your Heart’s Electrical System. https://www.nhlbi.nih.gov/health/health-topics/topics/hhw/electrical[↩]
- National Institutes of Health. National Heart, Lung and Blood Institute. Who Is at Risk for Coronary Heart Disease ? https://www.nhlbi.nih.gov/health/health-topics/topics/cad/atrisk[↩]
- Stamler R. Implications of the INTERSALT study. Hypertension. 1991; 17 (suppl): I16–I20. https://www.ncbi.nlm.nih.gov/pubmed/1986996?access_num=1986996[↩]
- US Department of Health and Human Services and US Department of Agriculture. Dietary Guidelines for Americans, 2005. 6th ed. Washington, DC: US Government Printing Office; 2005.[↩]
- Johnson RK, Appel LJ, Brands M, Howard BV, Lefevre M, Lustig RH, Sacks F, Steffen LM, Wylie-Rosett J; on behalf of the American Heart Association Nutrition Committee of the Council on Nutrition, Physical Activity, and Metabolism and the Council on Epidemiology and Prevention. Dietary sugars intake and cardiovascular health: a scientific statement from the American Heart Association. Circulation. 2009; 120: 1011–1020. http://circ.ahajournals.org/content/120/11/1011[↩]
- Lloyd-Jones DM, Hong Y, Labarthe D, et al. Defining and setting national goals for cardiovascular health promotion and disease reduction: the American Heart Association’s strategic Impact Goal through 2020 and beyond. Circulation. 2010;121:586-613. http://circ.ahajournals.org/content/121/4/586.long[↩]
- Dowse GK, Gareebo H, Alberti KG, Zimmet P, Tuomilehto J, Purran A, Fareed D, Chitson P, Collins VR. Changes in population cholesterol concentrations and other cardiovascular risk factor levels after five years of the Non-communicable Disease Intervention Programme in Mauritius. BMJ. 1995; 311: 1255–1259. http://www.bmj.com/content/311/7015/1255[↩]
- http://www.bmj.com/content/313/7064/1044[↩]
- Chiuve SE, Rexrode KM, D. S, Logroscino G, Manson JE, Rimm EB. Primary prevention of stroke by healthy lifestyle. Circulation. 2008;118:947-54. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2730914/[↩]
- Chiuve SE, Fung TT, Rexrode KM, et al. Adherence to a low-risk, healthy lifestyle and risk of sudden cardiac death among women. JAMA. 2011;306:62-9. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3210472/[↩]
- van Dam RM, Li T, Spiegelman D, Franco OH, Hu FB. Combined impact of lifestyle factors on mortality: prospective cohort study in US women. BMJ. 2008;337:a1440. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2658866/[↩]
- National Institutes of Health. National Institute of Aging. Heart Health. https://www.nia.nih.gov/health/heart-health [↩][↩][↩]
- American Heart Association. Target Heart Rates. http://www.heart.org/HEARTORG/HealthyLiving/PhysicalActivity/FitnessBasics/Target-Heart-Rates_UCM_434341_Article.jsp[↩]
- National Institutes of Health. High Blood Pressure. https://www.nhlbi.nih.gov/health/health-topics/topics/hbp/[↩][↩]