Contents
- What is hydrocephalus
- Hydrocephalus types and classification
- Hydrocephalus causes
- Hydrocephalus prevention
- Hydrocephalus life expectancy
- Hydrocephalus prognosis
- Hydrocephalus complications
- Hydrocephalus symptoms
- Hydrocephalus diagnosis
- Hydrocephalus treatment
What is hydrocephalus
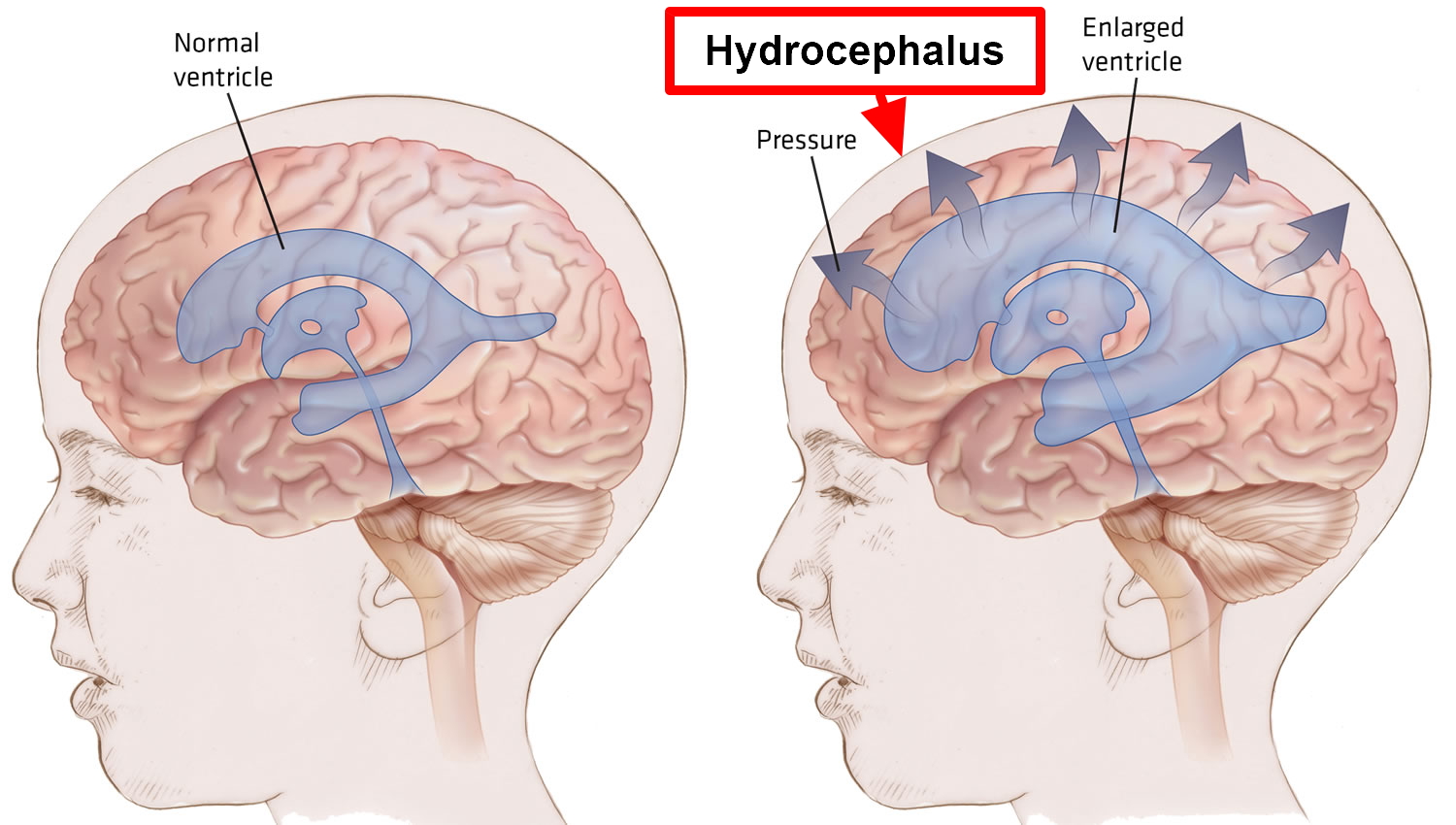
Hydrocephalus is a serious condition characterized by excessive accumulation of cerebrospinal fluid (CSF) in the brain. In babies, hydrocephalus (fluid accumulation in the brain) can cause the babies’ head to grow unusually quickly. Hydrocephalus may also result in bulging fontanelles, or a bulging area at the soft spot at the top of the infant’s head. In adults, hydrocephalus causes neurological problems such as drowsiness, seizures, unstable balance, poor coordination, difficulty walking, gait disturbances, impaired vision, memory loss and urinary urgency or incontinence.
Hydrocephalus is a condition, not a disease. It can develop for a variety of reasons, sometimes as part of another condition.
- The incidence of congenital (present at birth) hydrocephalus is approximately 3 for every 1000 live births.
- The incidence of adult hydrocephalus depends on the frequency of precipitating causes, such as brain infections and so forth. Hydrocephalus is estimated to affect 1 in every 10,000 people at some point in their lifetime.
- The incidence of hydrocephalus in males and females is roughly equal. Peak incidence occurs in infancy and adulthood.
The excessive accumulation of cerebrospinal fluid (CSF) results in an abnormal widening of spaces in the brain called ventricles (see Figures 1 – 3). This widening creates potentially harmful pressure on the tissues of the brain.
The ventricular system is made up of four ventricles connected by narrow passages (see Figure 1). Normally, cerebrospinal fluid (CSF) flows through the ventricles, exits into cisterns (closed spaces that serve as reservoirs) at the base of the brain, bathes the surfaces of the brain and spinal cord, and then reabsorbs into the bloodstream.
Cerebrospinal fluid (CSF) has three important life-sustaining functions:
- To keep the brain tissue buoyant, acting as a cushion or “shock absorber”;
- To act as the vehicle for delivering nutrients to the brain and removing waste; and
- To flow between the cranium and spine and compensate for changes in intracranial blood volume (the amount of blood within the brain).
The balance between production and absorption of CSF is critically important. Because CSF is made continuously, medical conditions that block its normal flow or absorption will result in an over-accumulation of CSF. The resulting pressure of the fluid against brain tissue is what causes hydrocephalus.
The number of people who develop hydrocephalus or who are currently living with it is difficult to establish since the condition occurs in children and adults, and can develop later in life. A 2008 data review by the University of Utah found that, in 2003, hydrocephalus accounted for 0.6 percent of all pediatric hospital admissions in the United States. Some estimates report one to two of every 1,000 babies are born with hydrocephalus. Over 1,000,000 people in the United States currently live with hydrocephalus.
If hydrocephalus remains untreated the intracranial pressure will rise eventually resulting in compression of the brain stem and subsequently death from respiratory causes.
Hydrocephalus is the most common reason for brain surgery in children.
Ventricles and Cerebrospinal Fluid
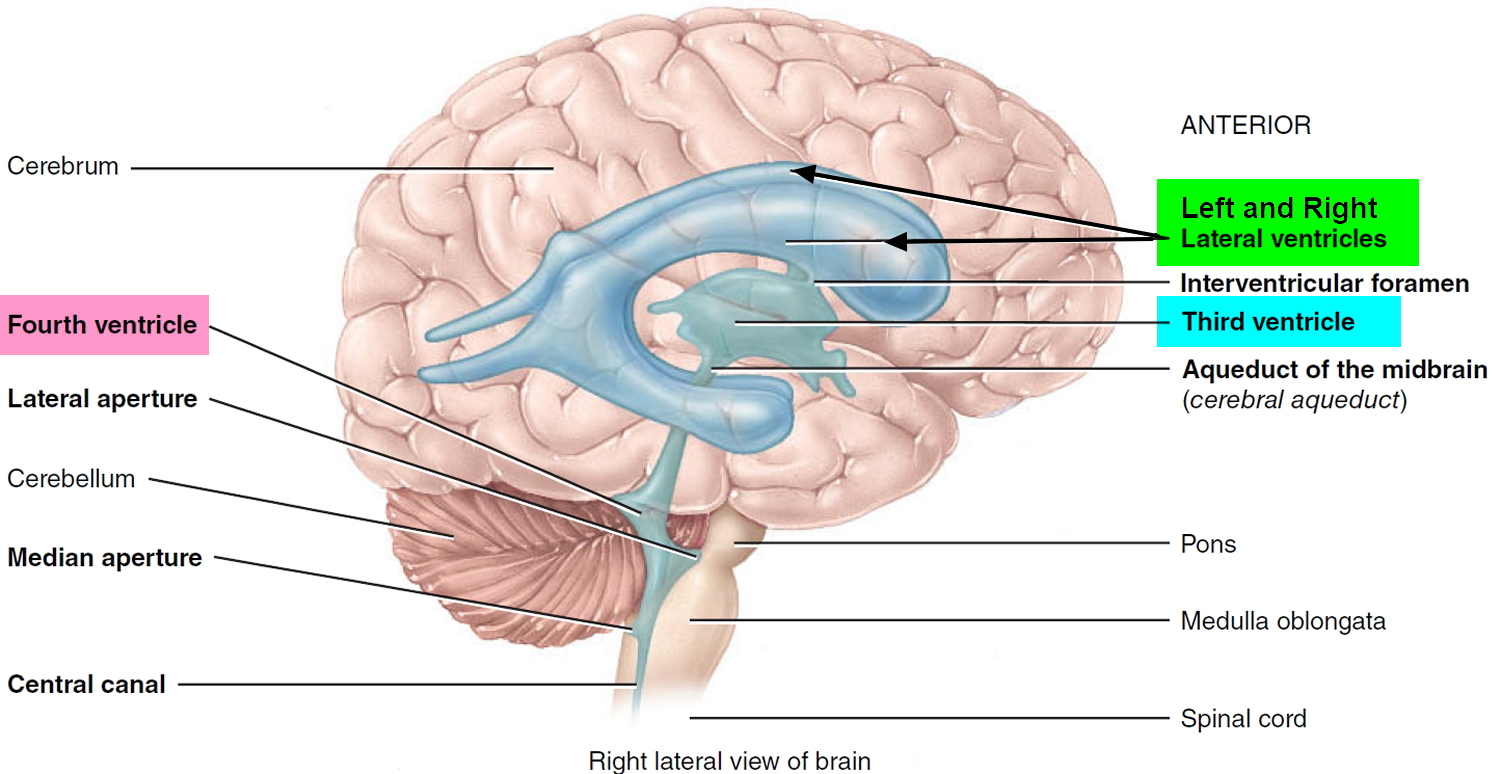
The brain has four internal chambers called ventricles. The largest and most frontal ones are the two lateral ventricles, which form an arc in each cerebral hemisphere. Through a tiny pore called the interventricular foramen, each lateral ventricle is connected to the third ventricle, a narrow median space inferior to the corpus callosum. From here, a canal called the cerebral aqueduct passes down the core of the midbrain and leads to the fourth ventricle, a small triangular chamber between the pons and cerebellum. Caudally, this space narrows and forms a central canal that extends through the medulla oblongata into the spinal cord.
Figure 1. Ventricles of the brain
On the floor or wall of each ventricle is a spongy mass of blood capillaries called a choroid plexus, named for its histological resemblance to a fetal membrane called the chorion. Ependyma, a type of neuroglia that resembles a cuboidal epithelium, lines the ventricles and canals and covers the choroid plexuses. It produces cerebrospinal fluid (CSF).
Cerebrospinal fluid is a clear, colorless liquid that fills the ventricles and canals of the CNS and bathes its external surface. The brain produces about 500 mL of cerebrospinal fluid per day, but the fluid is constantly reabsorbed at the same rate and only 100 to 160 mL is normally present at one time. About 40% of it is formed in the subarachnoid space external to the brain, 30% by the general ependymal lining of the brain ventricles, and 30% by the choroid plexuses. Cerebrospinal fluid production begins with the filtration of blood plasma through the capillaries of the brain. Ependymal cells modify the filtrate as it passes through them, so the cerebrospinal fluid has more sodium chloride than blood plasma, but less potassium, calcium, and glucose and very little protein.
Cerebrospinal fluid serves three functions for the brain:
- Buoyancy. Because the brain and cerebrospinal fluid are similar in density, the brain neither sinks nor floats in the cerebrospinal fluid. It hangs from delicate specialized fibroblasts of the arachnoid meninx. A human brain removed from the body weighs about 1.5 kg, but when suspended in cerebrospinal fluid its effective weight is only about 50 g. This buoyancy allows the brain to attain considerable size without being impaired by its own weight. If the brain rested heavily on the floor of the cranium, the pressure would kill the nervous tissue.
- Protection. Cerebrospinal fluid also protects the brain from striking the cranium when the head is jolted. If the jolt is severe, however, the brain still may strike the inside of the cranium or suffer shearing injury from contact with the angular surfaces of the cranial floor. This is one of the common findings in head injuries (concussions) from contact sports like NFL, rugby and boxing.
- Chemical stability. Cerebrospinal fluid rinses metabolic wastes from the nervous tissue and regulates its chemical environment. Slight changes in cerebrospinal fluid composition can cause malfunctions of the nervous system. For example, a high glycine concentration disrupts the control of body temperature and blood pressure, and a high pH causes dizziness and fainting.
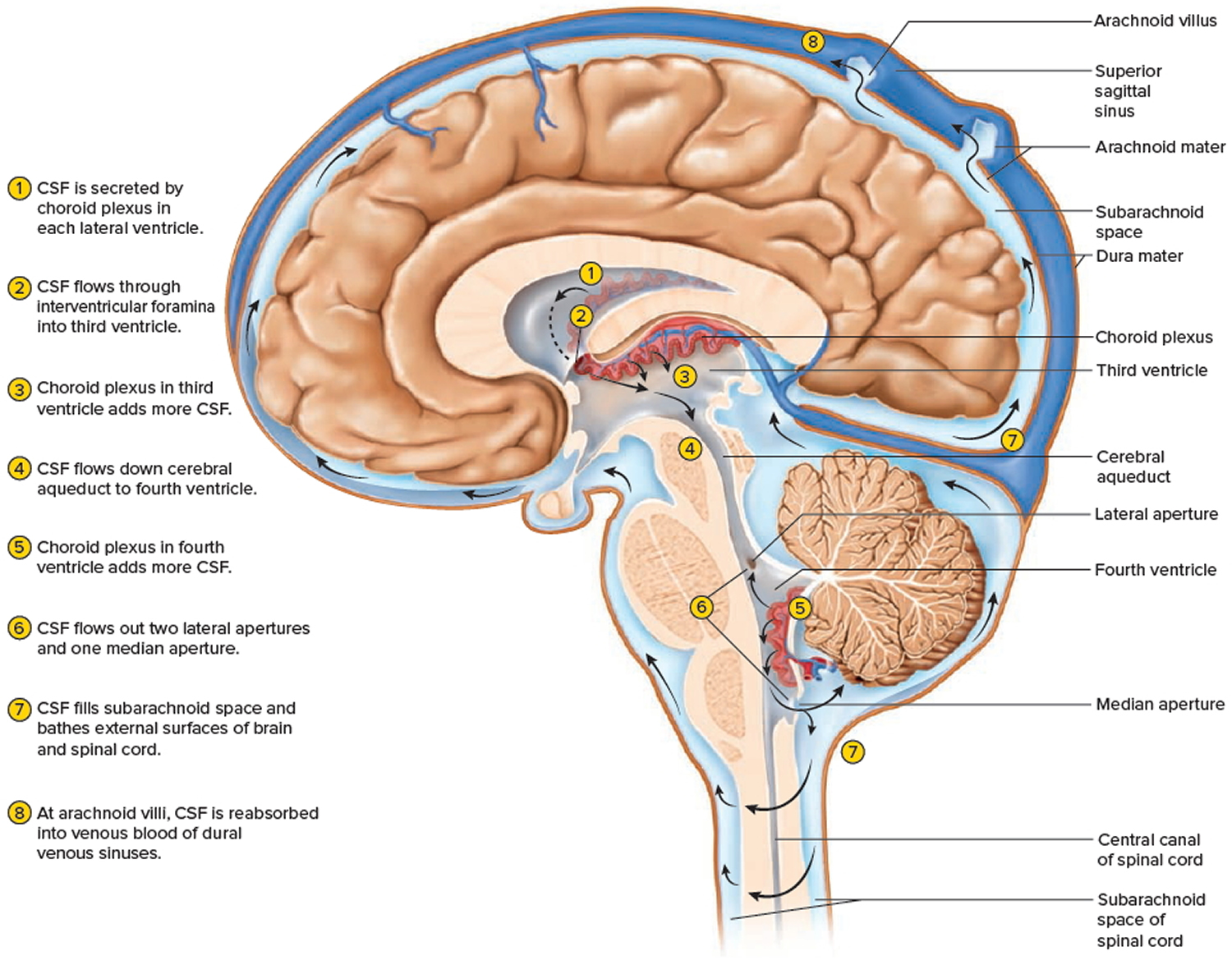
Cerebrospinal fluid continually flows through and around the brain and spinal cord, driven partly by its own pressure, partly by the beating of ependymal cilia, and partly by rhythmic pulsations of the brain produced by each heartbeat. The cerebrospinal fluid of the lateral ventricles flows through the interventricular foramina into the third ventricle, then down the cerebral aqueduct to the fourth ventricle. The third and fourth ventricles and their choroid plexuses add more cerebrospinal fluid along the way. A small amount of cerebrospinal fluid fills the central canal of the spinal cord, but ultimately, all of it escapes through three pores in the fourth ventricle—a median aperture and two lateral apertures. These lead into the subarachnoid space on the brain and spinal cord surface. From here, cerebrospinal fluid is reabsorbed by arachnoid granulations, extensions of the arachnoid meninx shaped like little sprigs of cauliflower, protruding through the dura mater into the superior sagittal sinus. Cerebrospinal fluid penetrates the walls of the granulations and mixes with blood in the sinus.
Figure 2. Cerebrospinal fluid formation, absorption and circulation around and within the brain
Hydrocephalus types and classification
Hydrocephalus may be congenital or acquired.
- Congenital hydrocephalus is present at birth and may be caused by either events or influences that occur during fetal development, or genetic abnormalities. Congenital hydrocephalus is now often diagnosed before birth through routine ultrasound. The incidence of congenital hydrocephalus is approximately 3 for every 1000 live births.
- Acquired hydrocephalus develops at the time of birth or at some point afterward. This type of hydrocephalus can affect individuals of all ages and may be caused by head trauma, brain tumor, cyst, intraventricular hemorrhage or infection of the central nervous system.
Hydrocephalus may also be communicating or non-communicating.
- Communicating hydrocephalus. If the cerebrospinal fluid (CSF) flows freely throughout the brain’s ventricular system and the subarachnoid space, it is referred to as communicating hydrocephalus. Communicating hydrocephalus is the result of defective absoprtion of cerebrospinal fluid (CSF) and/or increased production (rare).
- Non-communicating hydrocephalus — also called “obstructive” hydrocephalus — occurs when the flow of CSF is blocked along one or more of the narrow passages connecting the ventricles. One of the most common causes of hydrocephalus is “aqueductal stenosis.” In this case, hydrocephalus results from a narrowing of the aqueduct of Sylvius (cerebral aqueduct), a small passage between the third and fourth ventricles in the middle of the brain. Obstruction may be caused by a variety of things including mass lesions such as brain tumors or cysts.
Hydrocephalus in adults
There are two other forms of hydrocephalus which do not fit exactly into the categories mentioned above and primarily affect adults: hydrocephalus ex-vacuo and normal pressure hydrocephalus.
- Hydrocephalus ex-vacuo occurs when stroke or traumatic injury cause damage to the brain. In these cases, brain tissue may actually shrink.
- Normal pressure hydrocephalus occurs in older adults (most often affects people over the age of 60) when the ventricles of the brain are enlarged, but there is little or no increase in the pressure within the ventricles. Sometimes the cause of normal pressure hydrocephalus is known – that may result from a subarachnoid hemorrhage, head trauma, infection, tumor, or complications of surgery. But most often normal pressure hydrocephalus is idiopathic, which means the cause is not known. It is estimated that more than 700,000 Americans have normal pressure hydrocephalus, but less than 20% receive an appropriate diagnosis. Normal pressure hydrocephalus occurs due to reduced absorption of the CSF. However, the exact mechanism of normal pressure hydrocephalus is unknown. Normal pressure hydrocephalus develops insidiously. In fact, over the time the lateral ventricles (CSF filled cavity in the middle of the brain) in the brain gradually enlarge but with little increase in CSF pressure. Because of this, there is stretching and distortion of the brain tissue. Specifically, the part of the brain that is distorted contains nerve fibers that innervate the legs and bladder, hence explaining the gait and bladder problems in normal pressure hydrocephalus. Dementia occurs due to distortion of the brain tissue surrounding the ventricles.Mobility problems, dementia and urinary incontinence are the main symptoms of normal pressure hydrocephalus, but because they come on gradually and are similar to the symptoms of other, more common conditions, such as Alzheimer’s disease, it can be difficult to diagnose. It’s important to diagnose normal pressure hydrocephalus correctly because, unlike Alzheimer’s disease, the symptoms can be relieved with treatment.
- Prognosis of Normal pressure hydrocephalusThe major disability caused by normal pressure hydrocephalus is progressive dementia, and it is important to recognize normal pressure hydrocephalus as a cause of dementia because it is potentially treatable. While dementia caused by other diseases (such as Alzheimer’s disease and Parkinson’s disease) will take on a slowly progressive course, with treatment of normal pressure hydrocephalus the dementia can be improved or even reversed. Considering that, the prognosis of normal pressure hydrocephalus is better than other causes of dementia.
Hydrocephalus causes
Hydrocephalus is caused by an imbalance between how much cerebrospinal fluid is produced and how much is absorbed into the bloodstream.
The causes of hydrocephalus are still not well understood. Hydrocephalus may result from inherited genetic abnormalities (such as the genetic defect that causes aqueductal stenosis) or developmental disorders (such as those associated with neural tube defects including spina bifida and encephalocele). Other possible causes include complications of premature birth such as intraventricular hemorrhage, diseases such as meningitis, tumors, traumatic head injury, or subarachnoid hemorrhage, which block the exit of CSF from the ventricles to the cisterns or eliminate the passageway for CSF within the cisterns.
Excess cerebrospinal fluid in the ventricles occurs for one of the following reasons:
- Obstruction. The most common problem is a partial obstruction of the normal flow of cerebrospinal fluid, either from one ventricle to another or from the ventricles to other spaces around the brain.
- Poor absorption. Less common is a problem with the mechanisms that enable the blood vessels to absorb cerebrospinal fluid. This is often related to inflammation of brain tissues from disease or injury.
- Overproduction. Rarely, cerebrospinal fluid is created more quickly than it can be absorbed.
Common causes of Congenital Hydrocephalus
- Aqueductal stenosis – The most common cause of congenital hydrocephalus is an obstruction called aqueductal stenosis. This occurs when the long, narrow passageway between the third and fourth ventricles (the aqueduct of Sylvius = cerebral aqueduct) is narrowed or blocked, perhaps because of infection, hemorrhage, or a tumor. Fluid accumulates “upstream” from the obstruction, producing hydrocephalus.
- Neural tube defect – Another common cause of hydrocephalus is a neural tube defect. An open neural tube defect, where the spinal cord is exposed at birth and is often leaking CSF, is called a myelomeningocele, and is often referred to as spina bifida. This kind of neural tube defect usually leads to the Chiari II malformation, which causes part of the cerebellum and the fourth ventricle to push downward through the opening at the base of the skull into the spinal cord area, blocking CSF flow out of the fourth ventricle and causing hydrocephalus.
- Arachnoid cysts – Congenital hydrocephalus can also be caused by arachnoid cysts, which may occur anywhere in the brain. In children, they’re often located at the back of the brain (posterior fossa) and in the area of the third ventricle. These cysts are filled with CSF and lined with the arachnoid membrane, one of the three meningeal coverings. Some arachnoid cysts are self-contained, while others are connected with the ventricles or the subarachnoid space. The fluid trapped by the cysts may block the CSF pathways, causing hydrocephalus.
- Dandy-Walker syndrome – In Dandy-Walker syndrome, another cause of congenital hydrocephalus, the fourth ventricle becomes enlarged because its outlets are partly or completely closed and part of the cerebellum fails to develop. Dandy-Walker syndrome may also be associated with abnormal development in other parts of the brain and sometimes leads to aqueductal stenosis. In some instances, two shunts are placed in the child’s ventricles — one in the lateral ventricle and another in the fourth ventricle to manage the hydrocephalus.
- Chiari malformation – There are two types of Chiari malformation. Both types occur in the bottom of the brain stem where the brain and spinal cord join. The lowest portion of the brain is displaced and is lower than normal pushing down into the spinal column.
Congenital hydrocephalus can be caused by a condition such as spina bifida, or an infection the mother develops during pregnancy, such as mumps or rubella (German measles).
It’s estimated spina bifida affects one baby in every 700 born in United States. Most of them will have hydrocephalus.
Many babies born with hydrocephalus (congenital hydrocephalus) have permanent brain damage.
This can cause a number of long-term complications, such as:
- learning disabilities
- impaired speech
- memory problems
- short attention span
- problems with organizational skills
- vision problems, such as a squint and visual impairment
- problems with physical co-ordination
- epilepsy
If your child has learning disabilities, they’ll need extra support from their nursery or school to ensure their needs are being met.
Common causes of Acquired Hydrocephalus
- Intraventricular hemorrhage – An intraventricular hemorrhage, which most frequently affects premature newborns, may cause an acquired form of hydrocephalus. When small blood vessels alongside the ventricular lining rupture, blood may block or scar the ventricles or plug the arachnoid villi, which allow CSF to be absorbed. When the CSF can’t be absorbed, hydrocephalus results.
- Meningitis – Meningitis is an inflammation of the membranes of the brain and spinal cord. Caused by a bacterial or (less frequently) viral infection, meningitis can scar the delicate membranes called meninges that line the CSF pathway. An acquired form of hydrocephalus may develop if this scarring obstructs the flow of CSF as it passes through the narrow ventricles or over the surfaces of the brain in the subarachnoid space.
- Head injury – A head injury can damage the brain’s tissues, nerves, or blood vessels. Blood from ruptured vessels may enter the CSF pathway, causing inflammation. Sites of CSF absorption might then be blocked by scarred membranes – meninges – or by blood cells. The CSF flow is restricted, and hydrocephalus develops.
- Brain tumors – In children, brain tumors most commonly occur in the back of the brain which is referred to as the posterior fossa. As a tumor grows, it may fill or compress the fourth ventricle, blocking the flow of CSF and causing hydrocephalus. A tumor somewhere else in the brain might also block or compress the ventricular system.
Risk factors for hydrocephalus
In many cases, the exact event leading to hydrocephalus is unknown. However, a number of developmental or medical problems can contribute to or trigger hydrocephalus.
Newborns
Hydrocephalus present at birth (congenital) or shortly after birth may occur because of any of the following:
- Abnormal development of the central nervous system that can obstruct the flow of cerebrospinal fluid
- Bleeding within the ventricles, a possible complication of premature birth
- Infection in the uterus during a pregnancy, such as rubella or syphilis, that can cause inflammation in fetal brain tissues
Other contributing factors
Other factors that can contribute to hydrocephalus among any age group include:
- Lesions or tumors of the brain or spinal cord
- Central nervous system infections, such as bacterial meningitis or mumps
- Bleeding in the brain from a stroke or head injury
- Other traumatic injury to the brain.
Hydrocephalus prevention
Hydrocephalus isn’t a preventable condition. However, there are ways to potentially reduce the risk of hydrocephalus:
- If you’re pregnant, get regular prenatal care. Following your doctor’s recommended schedule for checkups during pregnancy can reduce your risk of premature labor, which places your baby at risk of hydrocephalus and other complications.
- Protect against infectious illness. Follow the recommended vaccination and screening schedules for your age and sex. Preventing and promptly treating the infections and other illnesses associated with hydrocephalus may reduce your risk.
To prevent head injury:
- Use appropriate safety equipment. For babies and children, use a properly installed, age- and size-appropriate child safety seat on all car trips. Make sure all your baby equipment — crib, stroller, swing, highchair — meets all safety standards and is properly adjusted for your baby’s size and development. Children and adults should wear helmets while riding bicycles, skateboards, motorcycles, snowmobiles or all-terrain vehicles.
- Always wear a seat belt in a motor vehicle. Small children should be secured in child safety seats or booster seats. Depending on their size, older children may be adequately restrained with seat belts.
Should you be vaccinated against meningitis?
Ask your doctor if you or your child should receive a vaccine against meningitis, once a common cause of hydrocephalus. The Centers for Disease Control and Prevention recommends meningitis vaccination for preteen children and boosters for teenagers. It’s also recommended for younger children and adults who may be at increased risk of meningitis for any of the following reasons:
- Traveling to countries where meningitis is common
- Having an immune system disorder called terminal complement deficiency
- Having a damaged spleen or having had the spleen removed
- Living in a college dormitory
- Joining the military
Hydrocephalus life expectancy
The life expectancy for individuals diagnosed with hydrocephalus is difficult to predict, although there is some correlation between the specific cause of the hydrocephalus and the outcome. Prognosis is further clouded by the presence of associated disorders, the timeliness of diagnosis, and the success of treatment. The degree to which relief of CSF pressure following shunt surgery can minimize or reverse damage to the brain is not well understood.
Affected individuals and their families should be aware that hydrocephalus poses risks to both cognitive and physical development. However, many children diagnosed with the disorder benefit from rehabilitation therapies and educational interventions and go on to lead normal lives with few limitations. Treatment by an interdisciplinary team of medical professionals, rehabilitation specialists, and educational experts is critical to a positive outcome. Left untreated, progressive hydrocephalus may be fatal.
The symptoms of normal pressure hydrocephalus usually get worse over time if the condition is not treated, although some people may experience temporary improvements. While the success of treatment with shunts varies from person to person, some people recover almost completely after treatment and have a good quality of life. Early diagnosis and treatment improves the chance of a good recovery.
Hydrocephalus prognosis
The prognosis is dependent on the underlying cause. The outlook is particularly poor for untreated hydrocephalus in infants; these often result in infection and death.
A small number will survive to childhood, but have some degree of intellectual handicap and developmental issues. The outlook is good for infants with treated non-tumor related hydrocephalus – 70% will maintain a normal IQ and attend normal school.
Damage already sustained tends to be permanent – loss of cognitive function may pesist even after treatment as may visual loss.
Hydrocephalus complications
Long-term complications of hydrocephalus can vary widely and are often difficult to predict.
If hydrocephalus has progressed by the time of birth, it may result in significant intellectual, developmental and physical disabilities. Less severe cases, when treated appropriately, may have few, if any, serious complications.
Adults who have experienced a significant decline in memory or other thinking skills generally have poorer recoveries and persistent symptoms after treatment of hydrocephalus.
The severity of complications depends on:
- Underlying medical or developmental problems
- Severity of initial symptoms
- Timeliness of diagnosis and treatment
Hydrocephalus symptoms
Symptoms of hydrocephalus vary with age, disease progression, and individual differences in tolerance to the condition. For example, an infant’s ability to compensate for increased CSF pressure and enlargement of the ventricles differs from an adult’s. The infant skull can expand to accommodate the buildup of CSF because the sutures (the fibrous joints that connect the bones of the skull) have not yet closed.
In infancy, the most obvious indication of hydrocephalus is often a rapid increase in head circumference or an unusually large head size. Other symptoms may include vomiting, sleepiness, irritability, downward deviation of the eyes (also called “sun setting”), and seizures.
Older children and adults may experience different symptoms because their skulls cannot expand to accommodate the buildup of CSF. Symptoms may include headache followed by vomiting, nausea, blurred or double vision, sun setting of the eyes, problems with balance, poor coordination, gait disturbance, urinary incontinence, slowing or loss of developmental progress, lethargy, drowsiness, irritability, or other changes in personality or cognition including memory loss.
Symptoms of normal pressure hydrocephalus include problems with walking, impaired bladder control leading to urinary frequency and/or incontinence, and progressive mental impairment and dementia. An individual with this type of hydrocephalus may have a general slowing of movements or may complain that his or her feet feel “stuck.” Because some of these symptoms may also be experienced in other disorders such as Alzheimer’s disease, Parkinson’s disease, and Creutzfeldt-Jakob disease, normal pressure hydrocephalus is often incorrectly diagnosed and never properly treated. Doctors may use a variety of tests, including brain scans such as computed tomography (CT) and magnetic resonance imaging (MRI), a spinal tap or lumbar catheter, intracranial pressure monitoring, and neuropsychological tests, to help them accurately diagnose normal pressure hydrocephalus and rule out any other conditions.
The symptoms described in this section account for the most typical ways in which progressive hydrocephalus is noticeable, but it is important to remember that symptoms vary significantly from person to person.
The symptoms of untreated hydrocephalus vary. During pregnancy, routine ultrasound can detect enlarged ventricles or spaces within a baby’s brain. In an infant, the most obvious sign of hydrocephalus is an abnormal enlargement of the baby’s head. In children symptoms tend to be related to high pressure and may include nausea, vomiting, headache and vision problems.
In young and middle aged adults symptoms most often include dizziness and vision problems. In older adults with normal pressure hydrocephalus the symptoms are more likely to be loss of function in three main areas: walking, thinking and bladder control.
Infants
Common signs and symptoms of hydrocephalus in infants include:
Changes in the head
- An unusually large head
- A rapid increase in the size of the head
- A bulging or tense soft spot (fontanel) on the top of the head
Physical signs and symptoms
- Vomiting
- Sleepiness
- Irritability
- Poor feeding
- Seizures
- Eyes fixed downward (sunsetting of the eyes)
- Deficits in muscle tone and strength
- Poor responsiveness to touch
- Poor growth
Toddlers and older children
Among toddlers and older children, signs and symptoms may include:
Physical signs and symptoms
- Headache
- Blurred or double vision
- Eyes fixed downward (sunsetting of eyes)
- Abnormal enlargement of a toddler’s head
- Sleepiness or lethargy
- Nausea or vomiting
- Unstable balance
- Poor coordination
- Poor appetite
- Seizures
- Urinary incontinence
Behavioral and cognitive changes
- Irritability
- Change in personality
- Decline in school performance
- Delays or problems with previously acquired skills, such as walking or talking
Young and Middle Aged Adults
- Chronic headaches
- Difficulty walking/gait disturbances
- Cognitive challenges or complaints
- Urinary urgency or incontinence
- Impaired vision
- Decline in memory, concentration and other thinking skills that may affect job performance
Older Adults (normal pressure hydrocephalus)
- Difficulty walking/gait disturbances, often described as a shuffling gait or the feeling of the feet being stuck
- Cognitive challenges/mild dementia/memory loss
- Urinary urgency or incontinence
- Poor coordination or balance
Hydrocephalus diagnosis
The most common initial diagnostic test to determine hydrocephalus at any age is an image of the brain using CT or MRI to identify if the ventricles or spaces within the brain are enlarged. More tests are often performed in adults in order to diagnosis the condition. The decision to order a particular test may depend on the specific clinical situation, as well as the preference and experience of the medical team. Not all of the tests described here are required in order to make a diagnosis.
- Clinical exams to evaluate symptoms consist of an interview and/or physical neurological examination.
- Brain images to detect enlarged ventricles commonly include magnetic resonance imaging (MRI) and computerized tomography (CT).
- CSF tests to predict shunt responsiveness and/or determine shunt pressure include lumbar puncture, external lumbar drainage, measurement of CSF outflow resistance, intracranial pressure (ICP) monitoring and isotopic cisternography.
Neurological exam
The type of neurological exam will depend on a person’s age. The neurologist may ask questions and conduct relatively simple tests in the office to judge muscle condition, movement, well-being and how well the senses are functioning.
Brain imaging
Brain imaging tests can show enlarged ventricles caused by excess cerebrospinal fluid. They may also be used to identify underlying causes of hydrocephalus or other conditions contributing to the symptoms. Imaging tests may include:
- Ultrasound. Ultrasound imaging, which uses high-frequency sound waves to produce images, is often used for an initial assessment for infants because it’s a relatively simple, low-risk procedure. The ultrasound device is placed over the soft spot (fontanel) on the top of a baby’s head. Ultrasound may also detect hydrocephalus prior to birth when the procedure is used during routine prenatal examinations.
- Magnetic resonance imaging (MRI) uses radio waves and a magnetic field to produce detailed 3-D or cross-sectional images of the brain. This test is painless, but it is noisy and requires lying still. Children may need mild sedation for some MRI scans. However, some hospitals use a very fast version of MRI that generally doesn’t require sedation.
- Computerized tomography (CT) scan is a specialized X-ray technology that can produce cross-sectional views of the brain. Scanning is painless and quick. But this test also requires lying still, so a child usually receives a mild sedative. Drawbacks to CT scanning include less detailed images than an MRI, and exposure to a small amount of radiation. CT scans for hydrocephalus are usually used only for emergency exams.
Normal pressure hydrocephalus
Normal pressure hydrocephalus can be difficult to diagnose because the symptoms come on gradually and are similar to those of more common conditions, such as Alzheimer’s disease.
It’s important to make a correct diagnosis because, unlike Alzheimer’s disease, the symptoms of normal pressure hydrocephalus can be relieved with treatment.
Your doctors will assess:
- how you walk (your gait)
- your mental ability
- symptoms that affect your bladder control, such as urinary incontinence
- the appearance of your brain (using scans)
Normal pressure hydrocephalus may be diagnosed if you have walking, mental and bladder problems, and cerebrospinal fluid (CSF) levels are higher than usual. However, you may not have all of the above symptoms.
Further tests may also be carried out to decide whether you would benefit from having surgery, such as a:
- lumbar puncture
- lumbar drainage test
- lumbar infusion test
Lumbar puncture
A lumbar puncture is a procedure where a sample of CSF is taken from your lower back. The pressure of the CSF sample is then checked.
Removing some CSF during a lumbar puncture may help improve your symptoms.
If this is the case, it’s a good indication that you may benefit from treatment with surgery – see treating hydrocephalus to find out more.
Lumbar drain
You may have a lumbar drain if a lumbar puncture doesn’t improve your symptoms.
A tube is inserted between your back bones to drain a large amount of CSF. This is carried out over a few days to see whether your symptoms improve. The procedure is usually carried out under local anesthetic.
Lumbar infusion test
During a lumbar infusion test, fluid is slowly injected into your lower back while measuring the pressure.
Your body should absorb the extra fluid and the pressure should stay low. If your body can’t absorb the extra fluid, the pressure will rise, which could indicate normal pressure hydrocephalus and that surgery will be beneficial.
Hydrocephalus treatment
Hydrocephalus is most often treated by surgically inserting a shunt system. This system diverts the flow of CSF from the brain and spinal cord to another area of your body where it can be absorbed as part of the normal circulatory process.
The increased pressure on the brain caused by hydrocephalus can be relieved by an operation to insert a ventricular peritoneal shunt (common type of hydrocephalus shunt). The shunt drains the fluid from the brain to another part of the body. The hydrocephalus shunt is a long, thin piece of tubing with a one way valve that takes the fluid from the ventricles in the brain, under the skin to the abdominal cavity. It is completely inside the body, but the outline of the tubing can be seen as it passes down the side of the neck, below the ear. A long coil of tubing is normally placed in the abdomen to allow the shunt to lengthen as the person grows. The shunt does not cure Hydrocephalus, but by draining the excess fluid it can allow the head and brain to grow normally.
A limited number of individuals can be treated with an alternative procedure called third ventriculostomy. In this procedure, a neuroendoscope — a small camera that uses fiber optic technology to visualize small and difficult to reach surgical areas — allows a doctor to view the ventricular surface. Once the scope is guided into position, a small tool makes a tiny hole in the floor of the third ventricle, which allows the CSF to bypass the obstruction and flow toward the site of resorption around the surface of the brain.
Having a pediatrician is vital for monitoring of developmental milestones and a good family doctor is required into adult life.
Hydrocephalus shunt
A shunt is a flexible but sturdy plastic tube. A shunt system consists of the shunt, a catheter, and a valve. One end of the catheter is placed within a ventricle inside the brain or in the CSF outside the spinal cord. The other end of the catheter is commonly placed within the abdominal cavity, but may also be placed at other sites in the body such as a chamber of the heart or areas around the lung where the CSF can drain and be absorbed. A valve located along the catheter maintains one-way flow and regulates the rate of CSF flow.
Hydrocephalus shunt lies completely inside your body, but the outline of the tubing can be seen as it passes down the side of the neck, below the ear. A long coil of tubing is normally placed in the abdomen to allow the shunt to lengthen as the person grows. The shunt does not cure hydrocephalus, but by draining the excess fluid it can allow the head and brain to grow normally.
A shunt is a delicate piece of equipment that can malfunction, usually by becoming blocked or infected.
It’s estimated up to 4 out of 10 shunts will malfunction in the first year after surgery.
Sometimes a scan after the operation shows the shunt isn’t in the best position, and further surgery is needed to reposition it.
If a baby or child has a shunt fitted, the shunt may become too small as the child grows, and it will need to be replaced. As most people need a shunt for the rest of their life, more than one replacement may be needed.
Bleeding can occasionally occur when shunt tubes are positioned. This can result in nerve problems, such as weakness down one side. There is also a small risk of fits after any type of brain surgery.
In younger children, particularly babies, cerebrospinal fluid (CSF) can run alongside the shunt rather than down it, and the fluid can leak through the skin wound. Additional stitches will be needed to stop the leak.
Figure 4. Hydrocephalus shunt
 What problems can occur with hydrocephalus shunts?
What problems can occur with hydrocephalus shunts?
Shunt systems are imperfect devices. Complications may include mechanical failure, infections, tubing can be blocked, or kinked, breaks and becomes disconnected or if the valve stops working properly, and the need to lengthen or replace the catheter. Infection can also cause shunt dysfunction. Shunt infection can occur at any stage, but is more common just after a new shunt has been inserted or after revision of the shunt. Generally, shunt systems require monitoring and regular medical follow up. When complications occur, subsequent surgery to replace the failed part or the entire shunt system may be needed.
Hydrocephalus is monitored in the outpatient clinic by the pediatrician, rehabilitation specialist and/or the neurosurgeon. A review of the signs and symptoms of shunt dysfunction is carried out at each clinic visit.
Some complications can lead to other problems such as overdraining or underdraining. Overdraining occurs when the shunt allows CSF to drain from the ventricles more quickly than it is produced. Overdraining can cause the ventricles to collapse, tearing blood vessels and causing headache, hemorrhage (subdural hematoma), or slit-like ventricles (slit ventricle syndrome). Underdraining occurs when CSF is not removed quickly enough and the symptoms of hydrocephalus recur. Overdrainage and underdrainage of CSF are addressed by adjusting the drainage pressure of the shunt valve; if the shunt has an adjustable pressure valve these changes can be made by placing a special magnet on the scalp over the valve. In addition to the common symptoms of hydrocephalus, infections from a shunt may also produce symptoms such as a low-grade fever, soreness of the neck or shoulder muscles, and redness or tenderness along the shunt tract. When there is reason to suspect that a shunt system is not functioning properly (for example, if the symptoms of hydrocephalus return), medical attention should be sought immediately.
The warning signs of shunt dysfunction or infection can include some of the following:
In infants:
- Rapid head growth (in babies).
- Full,bulging or tense soft spot (fontanel) at the top of the head (present until the skull closes at about 18 months of age).
- Swelling and/or pain along the shunt, especially at the side of the neck.
- Unusual irritability
- Nausea and vomiting
- Crossed eyes/sun setting eye
- Periods when the baby stops breathing (apnea) or drowsiness
- Difficulty drinking/swallowing/crying.
In older children:
- Headache
- Visual disturbance (blurred vision)
- Drowsiness
- Loss or decrease of consciousness
- Lethargy.
Less common signs can include:
- Difficulty in walking and changed mobility (due to weakness, balance problems, deterioration in sensation worsening of orthopedic problems)
- Memory problems or significant change in intellectual functioning
- Decline in milestones
- Seizures (new or worsening or increased frequency of existing seizures)
- Back pain or worsening scoliosis
- Changes in incontinence
- Hearing sensitivities.
Shunt infection
Shunt infection is also a relatively common complication after shunt surgery. The risk of infection is around 3-15% and is more likely to occur during the first few months after surgery.
The signs and symptoms of a shunt infection may include:
- Redness and tenderness along the line of the shunt
- A high temperature (fever) of 38 °C (100.4 °F) or above
- Headache
- Vomiting
- Neck stiffness
- Abdominal pain if the shunt drains into your tummy
- Leakage from the shunt wound area or tenderness along the tract
- Irritability or sleepiness in babies
Contact your care team immediately if you or your child has these symptoms.
Antibiotics may be needed to treat the infection and, in some cases, surgery may be required to replace the shunt.
Shunt alert cards
Shine (of United Kingdom), the hydrocephalus and spina bifida charity, has produced a series of shunt alert cards for adults and children. You carry the card with you if you’ve had a shunt fitted.
The card is useful in a medical emergency if you have symptoms of a blockage or infection.
The healthcare professionals treating you will be aware that you have a shunt fitted and will check whether this is causing your symptoms.
To apply for a shunt alert card, you can either fill out a form on the Shine website here: https://www.shinecharity.org.uk/hydrocephalus/taking-care-of-yourself/shuntalertcards
Additional treatments
Some people with hydrocephalus, particularly children, may need additional treatment, depending on the severity of long-term complications of hydrocephalus.
A care team for children may include a:
- Pediatrician or physiatrist (physical medicine and rehabilitation physician), who oversees the treatment plan and medical care
- Pediatric neurologist, who specializes in the diagnosis and treatment of neurological disorders in children
- Occupational therapist, who specializes in therapy to develop everyday skills
- Developmental therapist, who specializes in therapy to help your child develop age-appropriate behaviors, social skills and interpersonal skills
- Mental health provider, such as a psychologist or psychiatrist
- Social worker, who assists the family with accessing services and planning for transitions in care
- Special education teacher, who addresses learning disabilities, determines educational needs and identifies appropriate educational resources
Adults with more-severe complications also may require the services of occupational therapists, social workers, specialists in dementia care or other medical specialists.
Endoscopic Third Ventriculostomy
A second treatment option for hydrocephalus is a surgical procedure called endoscopic third ventriculostomy. This same endoscopic third ventriculostomy procedure with the addition of choroid plexus cauterization is available for infants. In the endoscopic third ventriculostomy procedure, an endoscope is used to puncture a membrane in the floor of the third ventricle creating a pathway for CSF flow within the cavities in the brain. This approach is an important alternative to shunting for obstructive hydrocephalus and may be useful in other cases as well.
The third treatment option involves the addition of choroid plexus cauterization with endoscopic third ventriculostomy in infants. The neurosurgeon uses a device to burn or cauterize tissue from the choroid plexus. The choroid plexus is a network of vessels in the ventricles of the brain where cerebrospinal fluid is produced.
The success rate for endoscopic third ventriculostomy or endoscopic third ventriculostomy/choroid plexus cauterization depends upon patient factors such as age, cause of hydrocephalus, and whether there is scarring in the fluid space below the floor of the third ventricle. For some patients, the chance for success of the endoscopic third ventriculostomy may be up to 90%; however, for others, endoscopic third ventriculostomy – with the addition of choroid plexus cauterization for infants – may not be recommended because the chances for success are sufficiently low. Your neurosurgeon should be able to provide you with a reliable estimate of the likelihood for success in your particular situation prior to the operation. It’s critical that parents and patients understand that endoscopic third ventriculostomy is not always a permanent cure for hydrocephalus. Candid communication with your physician regarding the definition of success is important when considering endoscopic third ventriculostomy.
Complications of endoscopic third ventriculostomy
The endoscopic third ventriculostomy/choroid plexus cauterization procedure is only available to infants.
The success rate for endoscopic third ventriculostomy or endoscopic third ventriculostomy/choroid plexus cauterization depends upon patient factors such as age, cause of hydrocephalus, and whether there is scarring in the fluid space below the floor of the third ventricle. For some patients, the chance for success of the endoscopic third ventriculostomy may be up to 90%; however, for others, endoscopic third ventriculostomy – with the addition of choroid plexus cauterization for infants – may not be recommended because the chances for success are sufficiently low. Your neurosurgeon should be able to provide you with a reliable estimate of the likelihood for success in your particular situation prior to the operation.
The most common complication with these two procedures is closure of the pathway that is surgically created with endoscopic third ventriculostomy and infection.
- Sudden Pathway Closure with endoscopic third ventriculostomy and endoscopic third ventriculostomy/choroid plexus cauterization
Sudden closure of the pathway created using endoscopic third ventriculostomy can be sudden and life-threatening. Pathway closure occurs in 20 to 50% of patients within five years of the procedure with the great majority of treatment failures occurring within the first six months of the operation. Although late failures can occur, they are rare, and the ongoing risk of treatment failure over subsequent years is much less than that for patients with shunt-dependence.
It’s critical that parents and patients understand that endoscopic third ventriculostomy is not a permanent cure for hydrocephalus. Candid communication with your physician regarding the definition of success is important when considering endoscopic third ventriculostomy.
- Infection with endoscopic third ventriculostomy and endoscopic third ventriculostomy/choroid plexus cauterization
Infection occurs in up to less than one percent of those treated surgically with endoscopic third ventriculostomy or endoscopic third ventriculostomy/choroid plexus cauterization procedures.
- Fever and Bleeding with endoscopic third ventriculostomy and endoscopic third ventriculostomy/choroid plexus cauterization
With new technologies the risks of endoscopic third ventriculostomy have been minimized, however there are still potential complications including fever and bleeding. Attempts to perforate or create an opening in the ventricular floor can lead to bleeding, as can damage to ventricular walls or perforation of the basilar artery. Large bleeds due to vessel injury under the third ventricle can be catastrophic, but they are rare.
Other complications from endoscopic third ventriculostomy include short-term memory loss, since the procedure may affect the hypothalamus and the areas of the mammillary body which are responsible for memory. This is typically a temporary complication. Endocrinologic irregularities can occur following endoscopic third ventriculostomy and endoscopic third ventriculostomy/choroid plexus cauterization as a result of the small opening in the area of the third ventricle which is responsible for some hormonal function. This complication is also often short lived.
Hydrocephalus Shunt and Endoscopic Third Ventriculostomy Complications
When things are going well, it’s easy to put the concerns about hydrocephalus and the complications that come with it out of your mind. However, it’s critical to understand the signs and symptoms of a shunt failure or the closure of an endoscopic third ventriculostomy. Seeing your physician or visiting the Emergency Department, even if symptoms are not ultimately related to hydrocephalus, the shunt, endoscopic third ventriculostomy or endoscopic third ventriculostomy/choroid plexus cauterization, is the right choice. Seeking immediate medical attention can identify a resolvable complication and enable you or your family member to avoid brain damage or even death, especially in children.
Symptoms of shunt malfunction or endoscopic third ventriculostomy closure vary considerably from person to person, but recurring failures tend to have similar symptoms for a particular person. When an abrupt malfunction occurs, symptoms can develop very rapidly potentially leading to coma and possibly death. In infants and toddlers, it’s important to be aware that medication with a side effect of drowsiness can mimic or mask signs of shunt malfunction or endoscopic third ventriculostomy closure and should be used with caution in those with hydrocephalus, especially infants and young children.
Infants
- Enlargement of baby’s head
- Fontanel full and tense when infant is upright and quiet
- Prominent scalp veins
- Swelling along shunt tract
- Vomiting
- Sleepiness
- Irritability
- Downward deviation of eyes
- Less interest in feeding
- Fever, potentially present with shunt failure or infection
- Redness along shunt tract, potentially present with shunt failure or infection
Toddlers
- Enlargement of head
- Swelling along shunt tract
- Vomiting
- Headache
- Sleepiness
- Irritability
- Loss of previous abilities (sensory or motor function)
- Fever, potentially present with shunt failure or infection
- Redness along shunt tract, potentially present with shunt failure or infection
Children and Adults
- Vomiting
- Headache
- Vision problems
- Irritability and/or tiredness
- Swelling along shunt tract
- Personality change
- Loss of coordination of balance
- Difficulty waking up or staying awake (this symptom requires urgent attention as it can potentially lead to a coma)
- Decline in academic or job performance
- Fever, potentially present with shunt failure or infection
- Redness along shunt tract, potentially present with shunt failure or infection
Older Adults with Normal Pressure Hydrocephalus
People who are diagnosed and treated in adulthood, including those with Normal Pressure Hydrocephalus, tend to revert to the symptoms they experienced before initial treatment when they are experiencing a shunt malfunction.
- Difficulty walking/Gait disturbances
- Cognitive challenges/Mild dementia
- Urinary Urgency or incontinence
- Fever (sign of shunt failure or infection)
- Redness along the shunt tract (sign of shunt failure or infection)
Normal pressure hydrocephalus
Normal pressure hydrocephalus, which usually affects older people, can sometimes be treated with a shunt, although not everyone with the condition will benefit from shunt surgery.
As there’s a risk of complications with shunt surgery, you’ll need tests to assess whether the potential benefits of surgery outweigh the risks.
Lumbar drainage or a lumbar infusion test, or both, can be used to determine whether shunt surgery will benefit you.
Coping and support
With the help of rehabilitative therapies and educational interventions, many people with hydrocephalus live with few limitations.
There are many resources available to provide emotional and medical support as you parent a child with hydrocephalus. Children with developmental problems due to hydrocephalus may be eligible for government-sponsored health care and other support services. Check with your state or county social services agency.
Hospitals and voluntary organizations serving people with disabilities are good resources for emotional and practical support, as are doctors and nurses. Ask these resources to help you connect with other families who are coping with hydrocephalus.
Adults living with hydrocephalus may find valuable information and support from organizations dedicated to hydrocephalus education and support, such as the Hydrocephalus Association https://www.hydroassoc.org/.