Contents
What is oral lichen planus
Oral lichen planus is lichen planus inside the mouth. Lichen planus is a chronic inflammatory skin condition. Oral lichen planus is as common as psoriasis and affects approximately 1-2% of the population 1. Oral lichen planus develops in women more than twice as often as in men and most commonly occurs in the fifth to sixth decade of life; although, oral lichen planus can sometimes affect younger adults and children 2. In patients with oral lichen planus, cutaneous lichen planus develops in approximately 50% of patients and vulvar lichen planus and/or vaginal involvement in 25%. But oral lichen planus may occur without skin lesions elsewhere. Moreover, scalp, nail, esophageal and ocular involvement are uncommon 3. A history of lichen planus in family members is sometimes present. Cutaneous lichen planus are self-limiting and pruritic 4, whereas oral lichen planus are chronic, rarely undergo spontaneous remission, potentially premalignant, and are often a source of morbidity and difficult to palliate. Oral lichen planus, particularly the erosive form, may rarely lead to oral cancer (squamous cell carcinoma). Persistent ulcers and enlarging nodules should undergo biopsy.
Oral lichen planus typically appear as lace-like white streaks on the inside of the cheeks (reticular oral lichen planus) but they can also affect the side of the tongue, gums and lips. An erosive form of oral lichen planus results in pain and ulceration which may lead to scarring. Sometimes eating is so uncomfortable that affected person is unable to maintain adequate nutrition. Some oral lichen planus may result from sensitivity to dental restorative materials or toothpaste. In rare cases, it can involve other mucosal sites such as the eyes, nasal mucosa, larynx, esophagus and anus.
Oral lichen planus may manifest in one of five patterns:
- Reticular oral lichen planus is characterized by painless white streaks in a lacy or fern-like pattern, including raised hyperkeratotic papules and plaques. Reticular lesions, the most recognized form of oral lichen planus, often occur as isolated lesions and may be the only clinical manifestation of the disease.
- Erythematosus oral lichen planus, including atrophic lesions. Erythematous oral lichen planus are accompanied by reticular oral lichen planus and erosive oral lichen planus in almost all cases. This feature helps clinically differentiate oral lichen planus from other diseases such as pemphigus and pemphigoid, which are characterized by isolated areas of erythema and/or erosions. Erythematous and erosive oral lichen planus result in varying degrees of pain as well as burning, swelling, irritation, and bleeding with brushing.
- Erosive oral lichen planus, including ulcerated and bullous lesions. Erosive oral lichen planus is characterized by painful and persistent erosions and ulcers often with a whitish border. Most often affects the gums (gingiva) and lips. May be associated with erosive lichen planus affecting genital sites.
- Plaque type oral lichen planus characterized by confluent white patches similar to oral keratoses. Usually seen in smokers
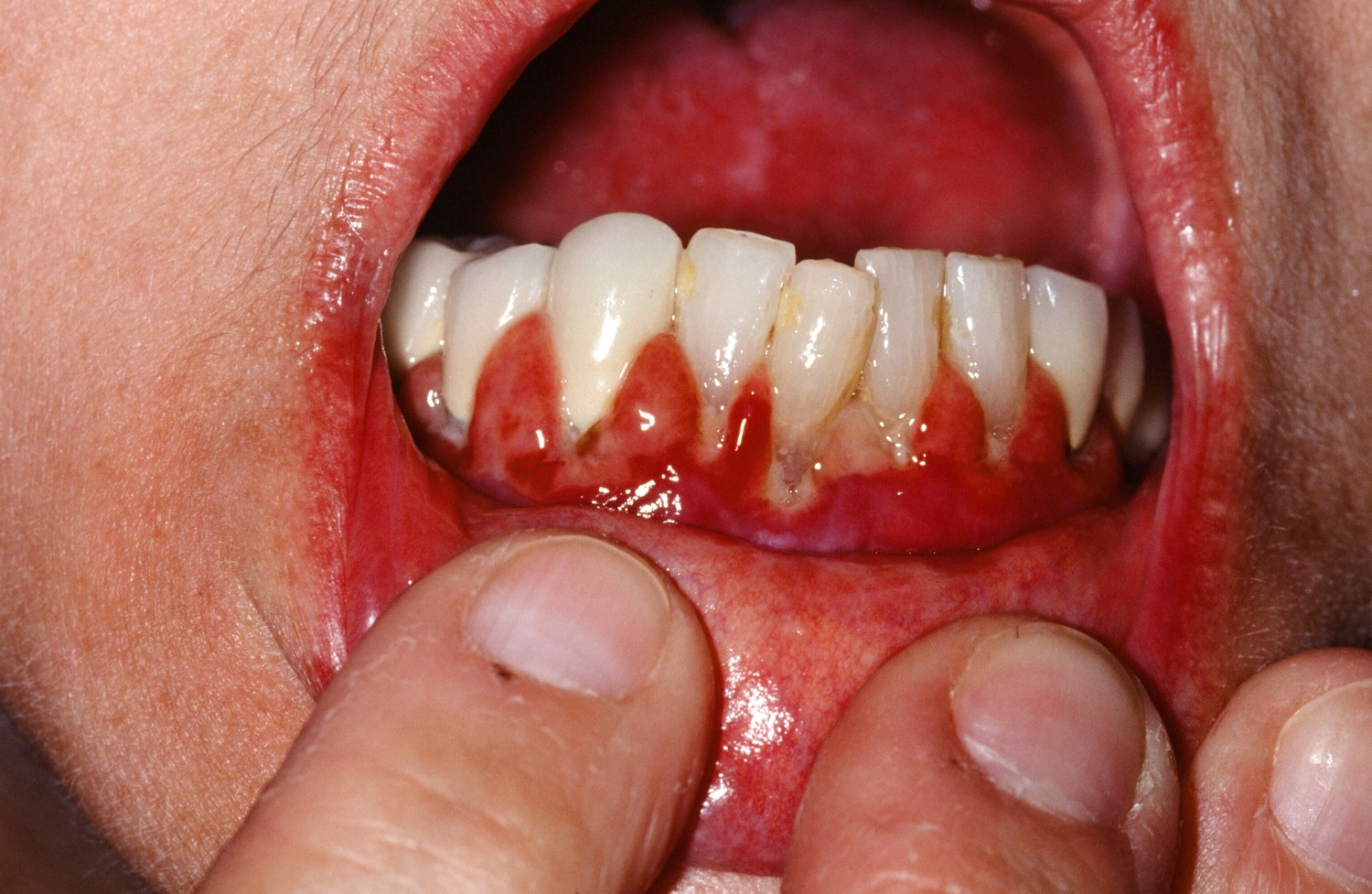
- Diffuse redness and peeling of the gums (desquamative gingivitis)
- Localized inflammation of the gums adjacent to amalgam fillings
Oral lichen planus develops most frequently on the posterior buccal mucosa followed by the tongue, gingiva, labial mucosa, and vermilion of the lower lip. Lesions on the palate, floor of the mouth, and upper lip are uncommonly observed. Approximately 10% of patients with oral lichen planus have the disease confined to the gingiva and present as raised white lacy lesions or more commonly as desquamative gingivitis, typically with atrophic and erosive lesions. Direct immunofluorescence is an effective method of excluding other causes of desquamative gingivitis that share similar clinical features with oral lichen planus, including pemphigus, pemphigoid, linear IgA disease and foreign body gingivitis 5.
Oral lichenoid reactions, eruptions in the oral cavity that have an identifiable cause and that clinically and histologically resemble oral lichen planus, are well recognized. An allergy or toxic reaction should be suspected when oral lichen planus lesions are confined to areas of the oral mucosa in close contact with amalgam restorations, especially fillings that are worn and cracked. When identified, such lesions show considerable improvement after replacement of the filling. Although uncommon, drug-induced oral lichenoid reactions are reversible upon withdrawal of the implicated drug. Therefore, a thorough medication history, with emphasis on non-steroidal anti-inflammatory drugs and angiotensin-converting enzyme inhibitors, is warranted. Many drugs implicated in cutaneous lichenoid reactions have not been associated with oral lesions.
An association between hepatitis C virus (HCV) infection and oral lichen planus has been investigated, but studies have been inconsistent. While many reports have demonstrated a significant association of the two diseases in Southern Europe and in Asia, studies from Northern Europe and North America failed to demonstrate any link 6. These conflicting results may be related to genetic factors however, with further prospective studies warranted.
The development of squamous cell carcinoma is controversial but is the most feared complication of oral lichen planus. Studies of the malignant potential of oral lichen planus have been fraught with inconsistencies in the diagnostic criteria of oral lichen planus and the criteria adopted to identify a true case of malignant transformation. The reported frequency of malignant transformation varies between 0.4% to over 5% over periods of observation from 0.5 to over 20 years, with almost all carcinomas developing in patients with atrophic and/or erosive lesions 7. Given the uncertainty of the premalignant nature of oral lichen planus and the fact that early detection of oral cancer results in improved survival, it seems prudent to monitor all patients with oral lichen planus carefully and long term.
The prognosis for oral lichen planus is uncertain. It can clear up within a few months or persist (with or without treatment) for decades. There are often periods of remission and relapse.
It is important to minimize or eliminate exacerbating factors such as heat and irritation from tobacco products, friction from sharp cusps, rough dental restorations and poorly fitting dental prostheses, and oral habits including lip and cheek chewing. Oral lichen planus lesions will then either revert to the less severe forms of the disease or resolve completely.
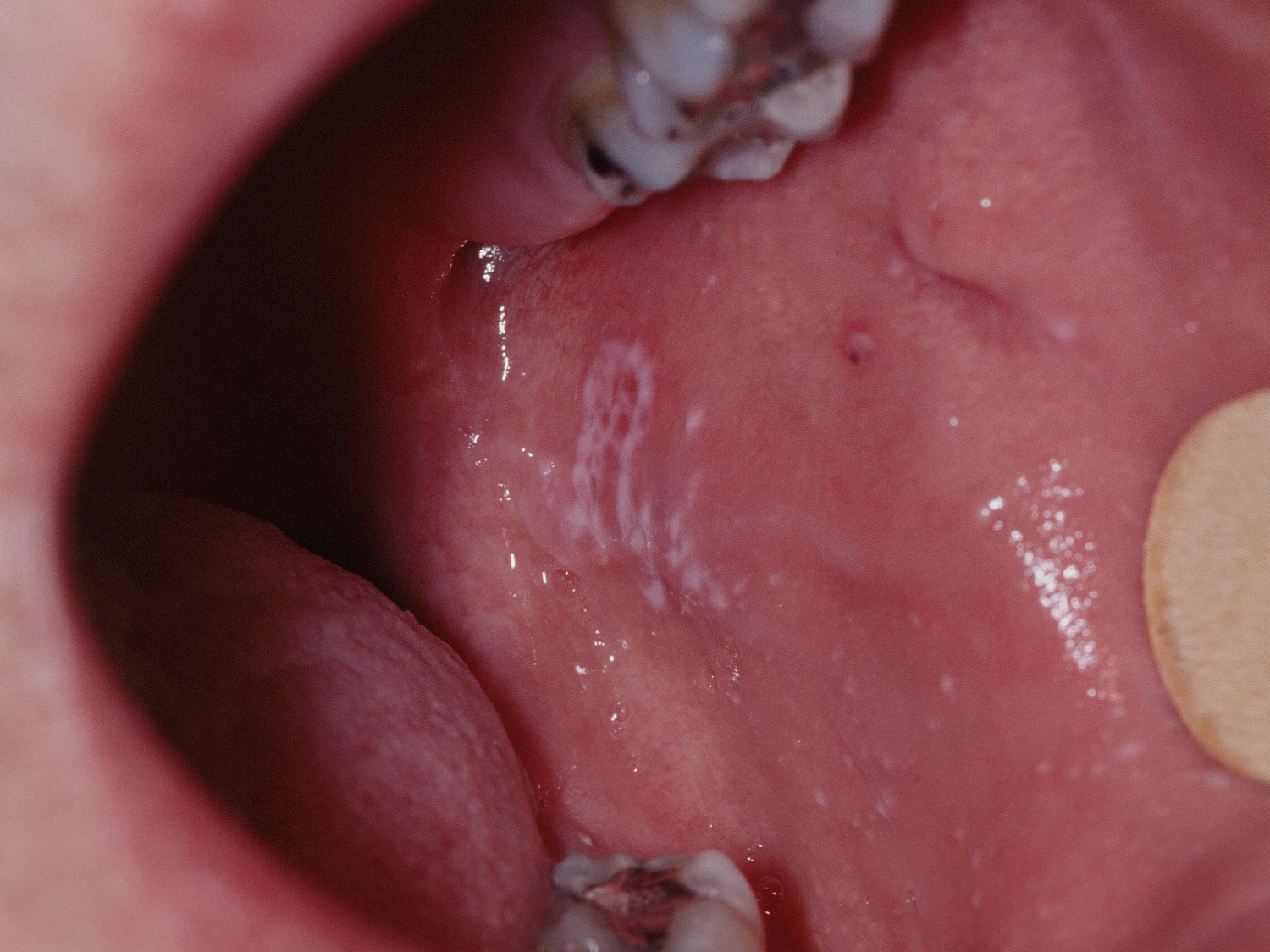
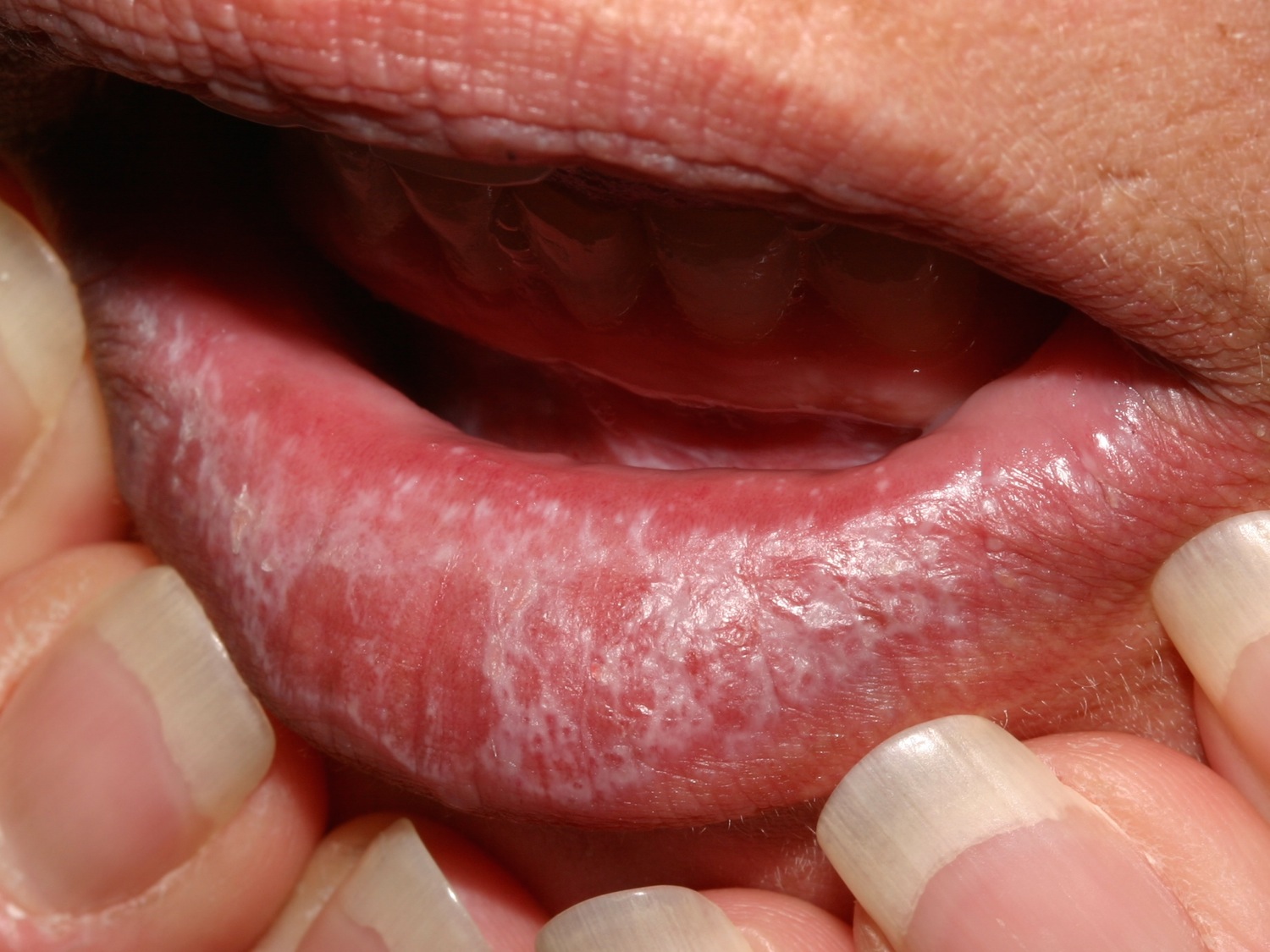
Figure 1. Oral lichen planus – note the reticular (lace-like) pattern called Wikcham’s stria
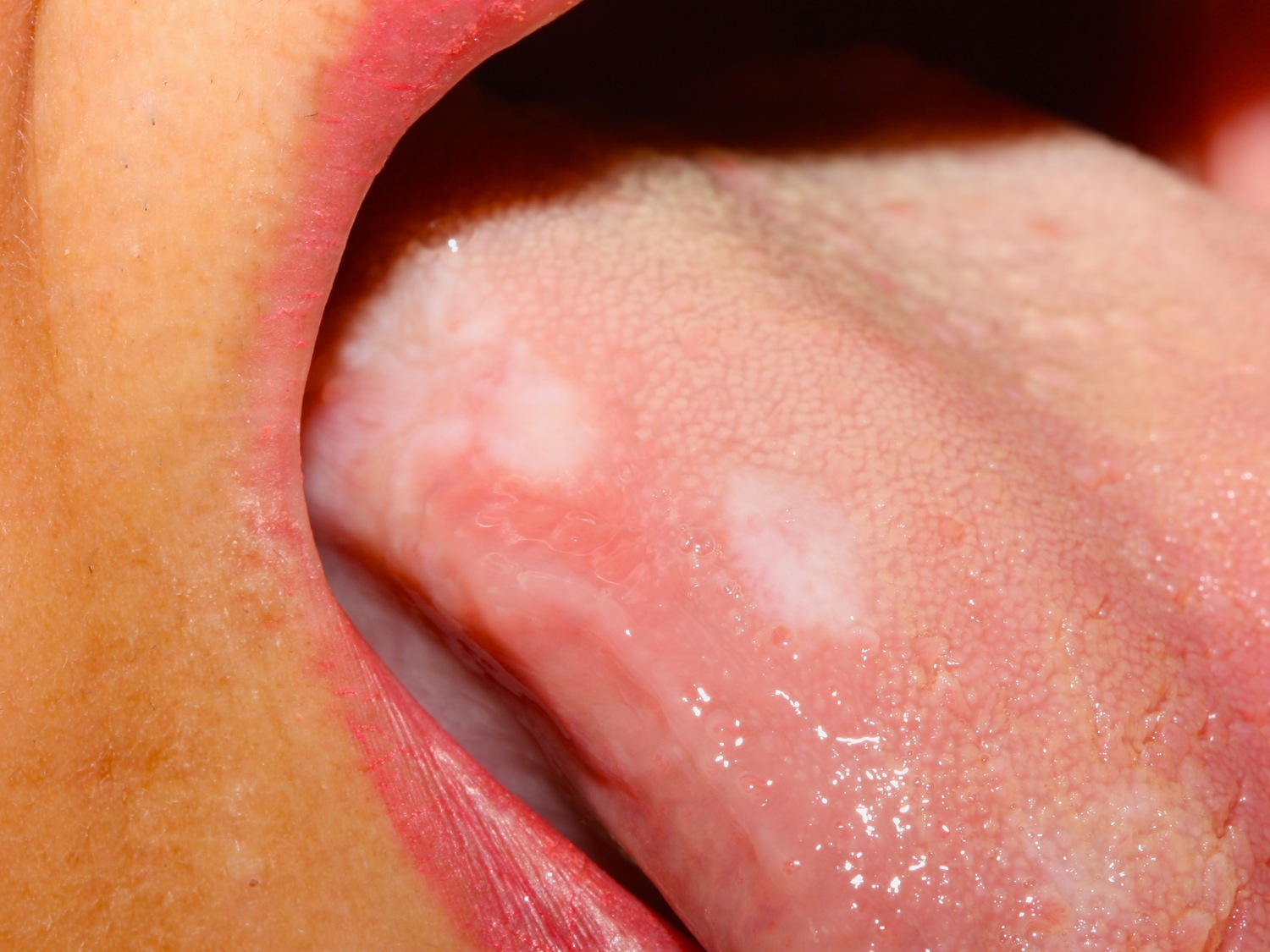
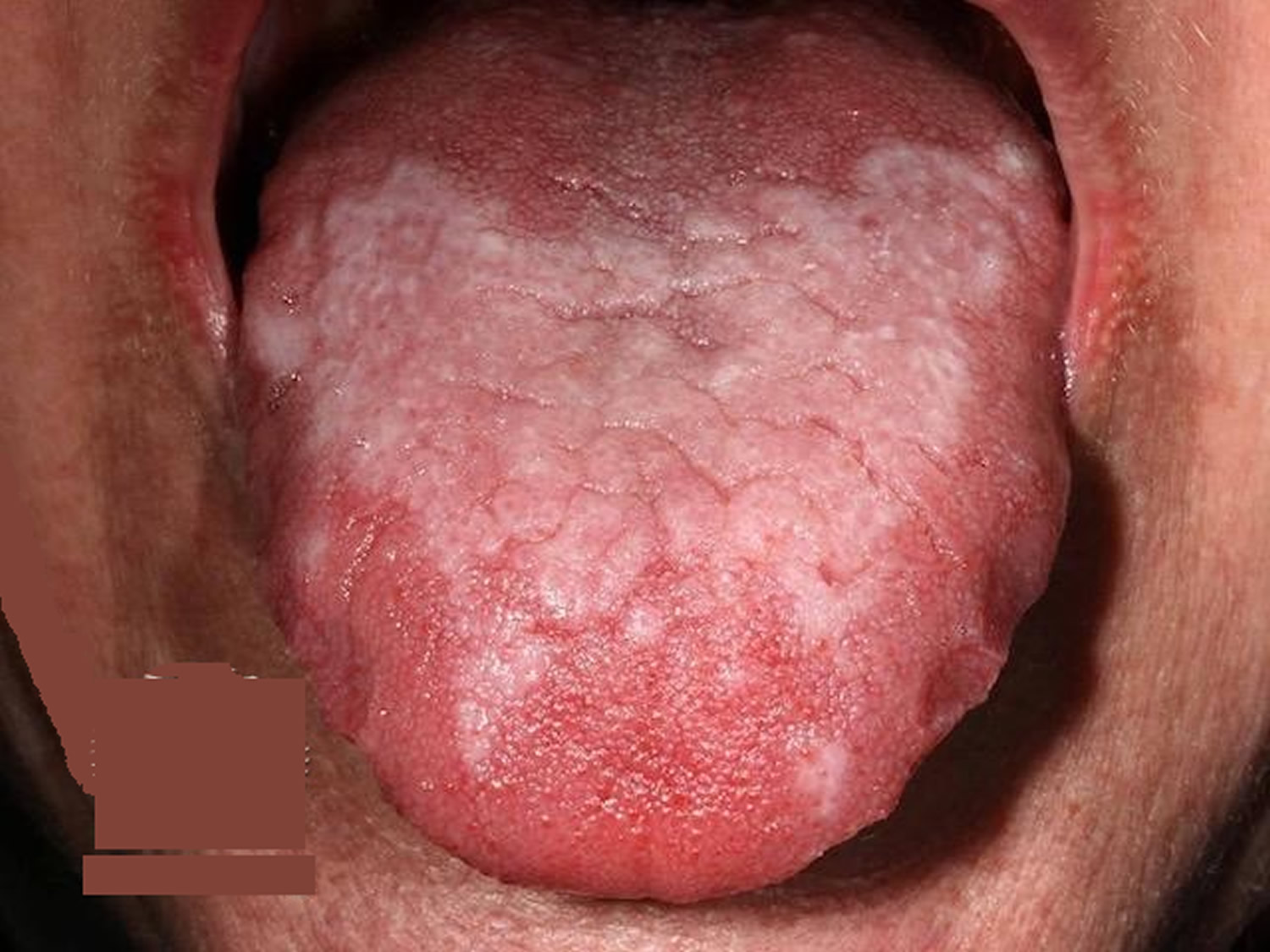
Figure 2. Oral lichen planus tongue – plaque type
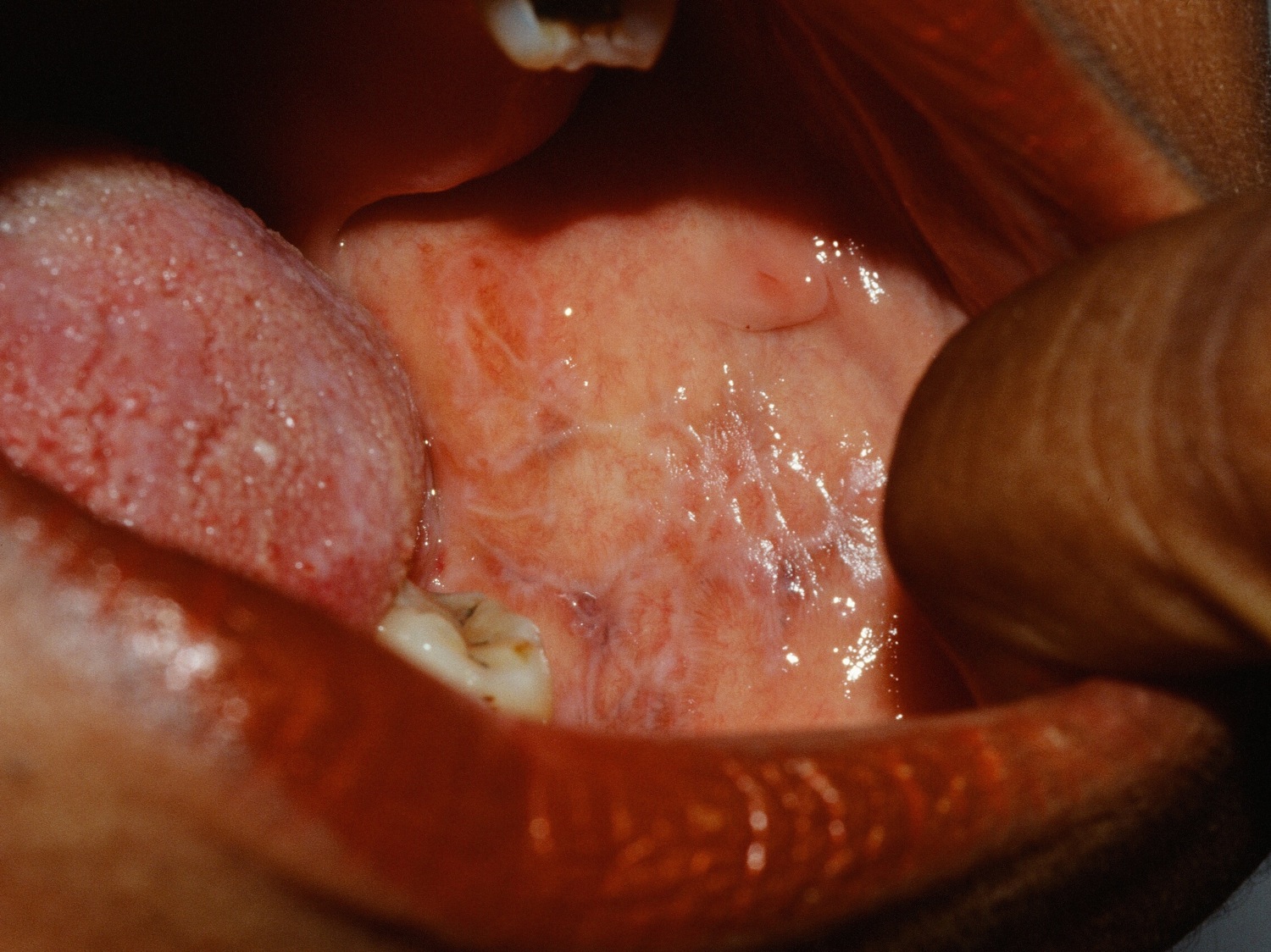
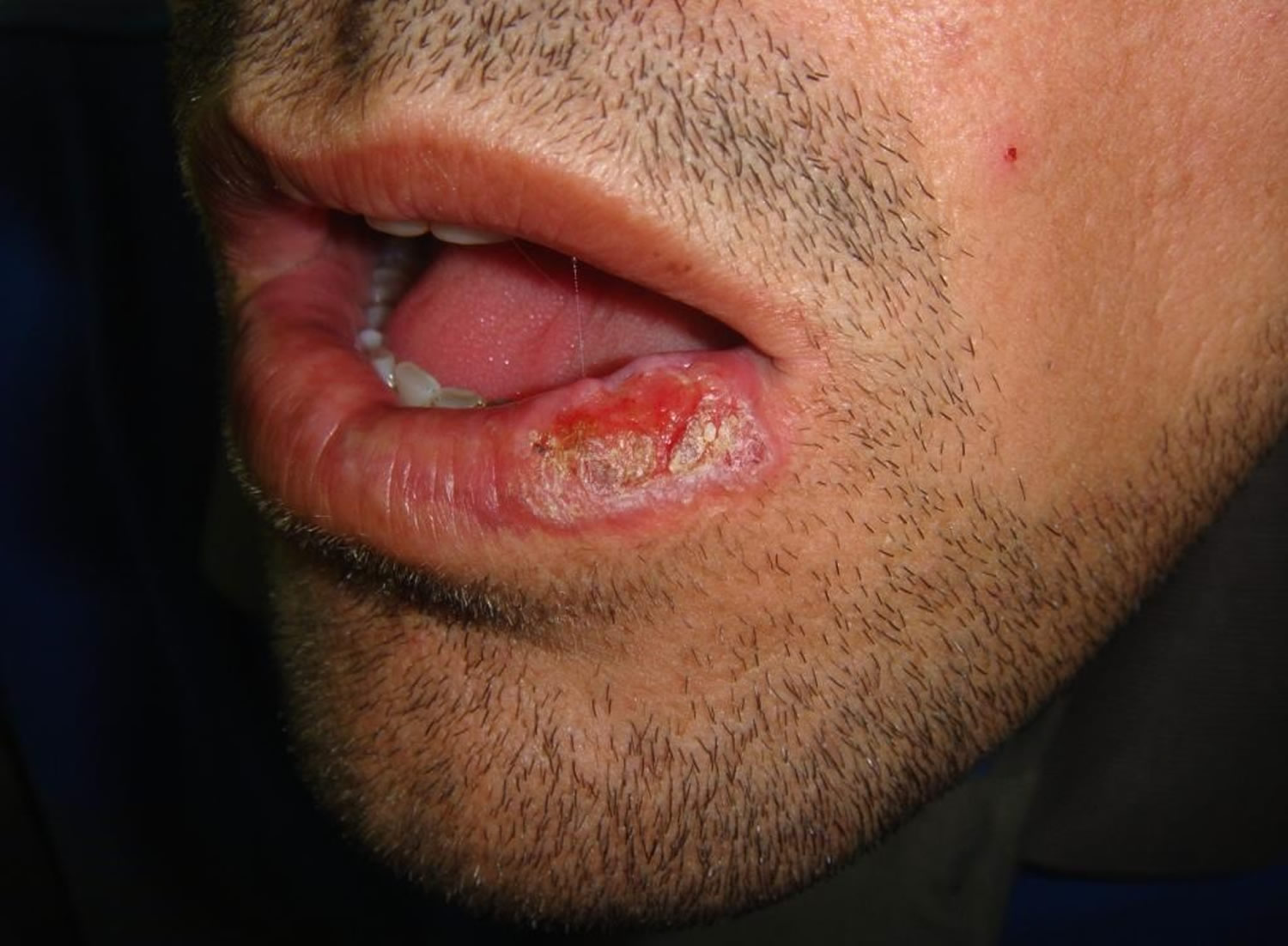
Figure 3. Erosive oral lichen planus
Oral lichen planus causes
The precise cause of oral lichen planus is not fully understood. It involves cytotoxic CD8+ T lymphocytes and pro-inflammatory cytokines, which attack the oral epithelial cells — resulting in their death. The immune response is mediated by antigen-specific cells.
In most cases oral lichen planus is idiopathic, when the reaction is thought to be against autoantigens. In other cases, it may be precipitated by exogenous antigens described below.
- Drugs — this is called oral lichenoid drug reaction. It is most often due to gold therapy. Other medications include some antibiotics, nonsteroidal anti-inflammatory drugs, antimalarials, drugs used for treating hypertension and heart disease, and antiretroviral medicines. These drugs more commonly cause a lichenoid skin eruption, with the mouth being affected less often.
- Contact allergens in dental restorative materials (mercury, nickel, gold, resins, acrylates) or toothpaste, particularly spearmint. These may be identified by careful patch testing.
- Viral infection, particularly Hepatitis C
Oral lichenoid lesions are also part of the spectrum of chronic graft-versus-host disease that occurs after bone marrow transplantation.
Oral lichen planus complications
Oral lichen planus can be very painful and ulceration may lead to scarring. Sometimes eating is so uncomfortable that affected person is unable to maintain adequate nutrition.
Lichen planus, particularly the erosive form, may rarely lead to oral cancer (squamous cell carcinoma). Persistent ulcers and enlarging nodules should undergo biopsy.
Severe cases of oral lichen planus may increase the risk of:
- Significant pain
- Weight loss or nutritional deficiency
- Stress or anxiety
- Depression
- Scarring from erosive lesions
- Secondary oral yeast or fungal infections
- Oral cancer (squamous cell carcinoma)
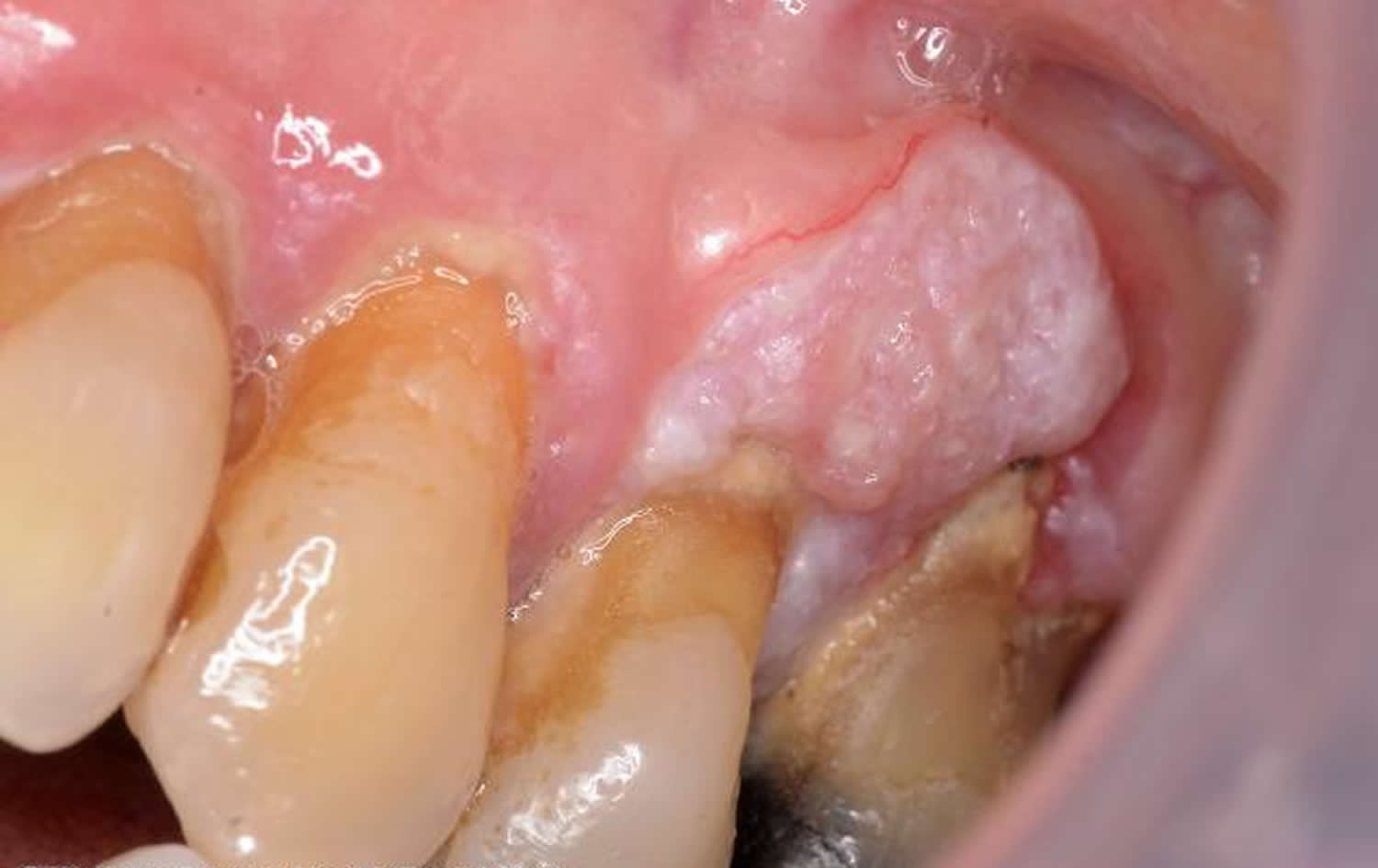
Figure 4. Oral lichen planus cancer (squamous cell carcinoma)
Oral lichen planus symptoms
A white, reticulated, lace-like lesion (Wickham striae) on the buccal mucosa, often bilaterally, is characteristic. Erosions may occur. White plaques may form on the tongue and lips. The patient may complain of stinging or burning, especially when eating. Any dental work should be noted as allergic contact dermatitis to oral metals can simulate lichen planus.
Signs and symptoms of oral lichen planus affect the mucous membranes of the mouth.
Appearance
The lesions may appear as:
- Lacy, white, raised patches of tissues
- Red, swollen, tender patches of tissues
- Open sores
Location
These lesions may appear on the:
- Inside of the cheeks, the most common location
- Gums
- Tongue
- Inner tissues of the lips
- Palate
Pain or discomfort
The white, lacy patches may not cause discomfort when they appear on the inside of the cheeks. However, symptoms accompanying red, swollen patches and open sores may include:
- Burning sensation or pain
- Sensitivity to hot, acidic or spicy foods
- Bleeding and irritation with tooth brushing
- Inflammation of the gums (gingivitis)
- Painful, thickened patches on the tongue
- Discomfort when speaking, chewing or swallowing
Oral lichen planus diagnosis
The diagnosis of oral lichen planus can be made from the clinical features if they are sufficiently characteristic, particularly if typical skin lesions are also present, but biopsy is recommended to confirm the diagnosis. Biopsy is often performed to rule out oral cancer.
Other more specialized microscopic tests may be needed to identify immune system proteins commonly associated with oral lichen planus. Under the microscope, the pathologist may observe a characteristic lichenoid reaction. Direct immunofluorescence may reveal positive staining for fibrinogen, immunoglobulins and complement.
You doctor may also request lab tests such as:
- Cultures. A sample of cells is taken from your mouth using a cotton swab. The sample is examined under a microscope to determine whether you have a secondary fungal, bacterial or viral infection.
- Blood tests. These may be done to identify conditions such as hepatitis C, which may rarely be associated with oral lichen planus, and lupus, which may look similar to oral lichen planus.
Oral lichen planus treatment
Oral lichen planus is a chronic condition. There is no cure, so the treatment focuses on helping severe lesions heal and reducing pain or other discomfort. Your doctor will monitor your condition to determine the appropriate treatment or stop treatment as necessary.
Dealing with triggers
It is important to identify and remove or avoid any potential agent that might have caused a lichenoid reaction, such as drugs that have been started in recent months and contact allergens identified by patch testing.
If your doctor suspects that oral lichen planus may be related to a trigger, such as a drug, an allergen or stress, he or she can recommend how to address the trigger. For example, you may be advised to try another drug instead, to see an allergist or dermatologist for additional testing, or to learn stress management techniques.
Most people get satisfactory control of symptoms with the following measures.
- Meticulous oral hygiene: brushing teeth and gums, regular visits to dentist, once-weekly mouthwash with diluted chlorhexidine
- If standard toothpaste irritates, try products that do not contain sodium lauryl sulfate
- Stop smoking
- Topical numbing agents can be used to provide temporary relief for areas that are particularly painful.
- Topical chamomile gel
- Topical retinoid, for example tretinoin or isotretinoin gel
- Topical steroids as drops, pastes, gels or sprays, for example, triamcinolone in an emollient dental paste, fluticasone nasal preparations, and clobetasol propionate in various forms.
- Steroid injections (intralesional triamcinolone)
- Mouth rinse containing a calcineurin inhibitor: ciclosporin or tacrolimus
Corticosteroids
In severe cases systemic corticosteroids may be used.
Corticosteroids may reduce inflammation related to oral lichen planus. One of these forms may be recommended:
- Topical. Mouthwash, ointment or gel is applied directly to the mucous membrane — the preferred method.
- Oral. Corticosteroids are taken as a pill for a limited amount of time.
- Injection. The medication is injected directly into the lesion.
Topical corticosteroids are the mainstay of treatment of oral lichen planus with 65% to 100% responding at least partially 8. Generally, higher potency preparations appear to be most effective, achieving a rapid response; one should lower the strength of the steroid as soon as erosions heal and erythematous lesions become asymptomatic. Once the disease becomes inactive with only white reticular lesions present, therapy may be temporarily discontinued.
A potent topical steroid gel or ointment applied 3-5 times a day is a simple first-line intervention. Dexamethasone 0.5 mg/5 mL sipped 1 teaspoon orally and held in the mouth for several minutes (swish and spit) has been used. Fluticasone propionate spray (50 ug aqueous solution-nasal spray 2 puffs four times daily) was helpful 9. Adverse effects included bad taste and smell, difficulty in application, sore throat, red, painful tongue, swollen mouth, nausea and candidiasis.
For intractable erosive oral lichen planus lesions, intralesional triamcinolone (10-20 mg/ml) injections can be highly effective and repeated every several weeks.
Immune response medicines
Other possible therapeutic agents may include:
- Thalidomide
- Systemic retinoids (acitretin or isotretinoin)
- Griseofulvin
- Azathioprine
- Cyclophosphamide
- Methotrexate
- Dapsone
- Metronidazole
- Low molecular weight heparin.
Medications that suppress or modify your body’s immune response may be used to improve more-severe lesions and lessen pain. They come in these forms:
- Topical ointments or gels. Calcineurin inhibitors, similar to oral drugs used to prevent rejection of transplanted organs, may be effective for treating oral lichen planus. But these medications have a Food and Drug Administration warning because of an unclear association with cancer. Examples include tacrolimus (Protopic) and pimecrolimus (Elidel).
- Systemic medication. For severe cases where oral lichen planus also involves other areas — such as the scalp, genitalia or esophagus — systemic medications that suppress the immune system may be used.
Potent topical immunosuppressants such as cyclosporine, tacrolimus, and pimecrolimus are beneficial for oral lichen planus 10. Tacrolimus 0.03-0.1% twice daily has been reported effective for erosive oral lichen planus 11. The main side effect is burning. Oral cyclosporin (e.g. as an oral rinse, or by applying several drops of 100 mg/mL of Sandimmun oral solution using the fingers twice daily) may be tried. An oral prosthesis has been used to occlude cyclosporin. For significant gingival involvement, brushing should be very gentle, and a sponge may be substituted for a brush. The high cost of cyclosporine precludes its routine use although utilizing a small quantity of drug reduces the cost. In small controlled studies, both pimecrolimus and tacrolimus reduced the symptoms and signs of oral lichen planus. Burning was the most common side effect of each. Tacrolimus may be at least as equally effective or more effective than potent topical steroids. However, relapses of oral lichen planus after cessation of therapy is expected with calcineurin inhibitors. Use the use one of these agents is combined with a topical steroid both twice daily. Given the Food and Drugs Administration (FDA) warning about calcineurin inhibitors and the potential association with an increased risk of cancer, the long-term use of these drugs for this chronic disease may be limited.
Retinoic acid has been used for thick lesions. Oral alitretinoin was effective for oral lichen planus in a study of 10 patients 12. Oral mycophenolate mofetil 500-1000 twice daily can be beneficial 13.
A number of systemic immunosuppressive agents have been anecdotally reported to be beneficial in the treatment of oral lichen planus 14. It was found that methotrexate (12.5-20 mg/week), azathioprine (100-150 mg/day), mycophenolate mofetil (1-2 g/day), and hydroxychloroquine (200-400 mg/day) are the most useful systemic agents. Some doctors have also been using thalidomide and tumor necrosis factor (TNF)-alpha inhibitors for refractory cases. Although none of these agents provide long-term remission, significant clinical benefits are achieved and maintained with long term administration. It is unclear whether reducing inflammation by aggressive therapy influences the malignant transformation of the disease.
Targeted molecular medicines are under investigation for the treatment or recalcitrant disease, with apremilast reported effective in a few patients. Apremilast has been used 3 patients with success 15.
- A biopsy to rule out squamous cell carcinoma should be done of unresponsive or suspicious lesions as squamous cell carcinoma develops in about 1% of patients.
Oral lichen planus home remedies
In addition to regular medical and dental treatment, self-care measures may help improve your oral lichen planus symptoms or help prevent recurring episodes of severe symptoms:
- Practice good oral hygiene. Keep your mouth clean to reduce your symptoms and help prevent infection. Gently brush your teeth at least twice a day using a bland toothpaste, and floss daily.
- Also avoid habits that can injure the inside of your mouth, such as chewing on your lip or cheek.
- Learn to manage stress. Because stress may complicate symptoms or trigger symptom recurrence, you may need to develop skills to avoid or manage stress. Your doctor may refer you to a mental health specialist who can help you identify stressors, develop stress management strategies or address other mental health concerns.
- See your doctor or dentist regularly. See your dentist twice a year for checkups and cleanings, or more often as directed by your dentist. Because long-term treatment is often required, talk to your doctor or dentist about how often you should be seen to evaluate how your treatment is working and for cancer screening.
Oral lichen planus diet
- Adjust your diet. Cut out spicy, salty or acidic foods if they seem to trigger or worsen your symptoms. Choose foods that are soft to help limit discomfort. And reduce or eliminate the use of caffeine.
- Avoid irritants. Avoid alcohol or tobacco.
- Scully C, Beyli M, Ferreiro MC, et al. Update on oral lichen planus; etiopathogenesis and management. Crit Rev Oral Biol Med. 1998;9:86-122.[↩]
- Eisen D. The clinical features, malignant potential, and systemic associations of oral lichen planus: a study of 723 patients. J Am Acad Dermatol. 2002;46:207-214.[↩]
- Eisen D. The evaluation of cutaneous, genital, scalp, nail, esophageal, and ocular involvement in patients with oral lichen planus. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 1999;88:431-436.[↩]
- Boyd As, Neldner KH. Lichen planus. J Am Acad Dermatol. 1991;25:593-619.[↩]
- Helander, SD, Rogers RS 3rd. The sensitivity and specificity of direct immunofluorescence testing in disorders of mucous membranes. J Am Acad Dermatol. 1994;30:65-75.[↩]
- Carrozzo M, Brancatello F, Dametto E, et al. Hepatitis C virus-associated oral lichen planus: is the geographical heterogeneity related to HLA-DR6? J Oral Pathol Med. 2005;34:204-208.[↩]
- Gonzalez-Moles MA, Scully C, Gil-Montoya JA. Oral lichen planus: controversies surrounding malignant transformation. Oral Dis. 2008;14:229-243.[↩]
- Eisen D. The clinical manifestations and treatment of oral lichen planus. Dermatol Clin. 2003;21:79-89.[↩]
- JAAD 2002;47;271[↩]
- Corrocher G, Di Lorenzo G, Martinelli N, et al. Comparative effect of tacrolimus 0.1% ointment and clobetasol 0.05% ointment in patients with oral lichen planus. J Clin Periodontol. 2008;35:244-249.[↩]
- BJD 1999;140;338[↩]
- JEADV 2016;30;293[↩]
- JAAD 2016;74;1073[↩]
- Scully C, Eisen D, Carrozzo M. Management of Oral Lichen Planus. Am J Clin Dermatol.2 000;5:287-306.[↩]
- J Drugs Dermatol 2016;15;1026[↩]