Contents
What is tropical ulcer
Tropical ulcer also called phagedenic ulcer is a painful, rapidly enlarging ulcer that is usually found on legs of an individual living in a hot, humid tropical region caused by bacteria that is transmitted by mosquitoes and flies in tropical and subtropical countries 1, 2, 3, 4, 5, 6, 7, 8, 9, 10, 11. A high prevalence of tropical ulcer is found in Africa, South-East Asia and South America 1. A variety of bacteria are found to be present in the tropical ulcer; Fusobacterium species are almost always present in the early stages; anaerobic microorganisms (Bacillus fusiformis) and spirochetes (Treponema vincenti) aggravates these ulcers and delays healing 12, 13, 1, 8. Other bacteria such as Escherichia coli and Enterococcus species may be present 8.
Tropical ulcer is initially circular, superficial, very painful, and has purple edges. It becomes big rapidly across your skin and down into deeper tissues such as your muscle or even the periosteum (the fibrous membrane covering the surface of bones). Tropical ulcer may reach several centimeters in diameter after a couple of weeks. The edges become thickened and raised and the central crater may become necrotic (blackened due to death of tissue) and foul-smelling. Complications include septicemia, osteomyelitis, contractures and squamous cell carcinoma development.
Multiple predisposing factors play a role in causing tropical ulcers. There is initially some form of trauma or injury to the skin, often as minor as a scratch or an insect bite. Rural laborers who do not wear adequate protective clothing and footwear are at increased risk of developing tropical ulcer. Poor nutrition, poor hygiene, low socioeconomic conditions, poverty, lack of protection from insect bites, exposure to muddy water, and chronic diseases such as malaria and intestinal parasites also increase the risk of a tropical ulcer developing.
To diagnose a tropical ulcer, it is important to rule out other causes of leg ulcers such as cutaneous leishmaniasis, atypical mycobacteria, pyoderma gangrenosum, arterial ulcers, diabetes, pressure ulcer and venous disease. As tropical ulcers may mimic many other causes of skin ulceration and nodules, a history of recent travel should arouse clinical suspicion. The time frame since exposure to the causative organism is an important feature in the diagnostic process. For example, pyodermas and cutaneous larva migrans present a few days after contact with the causative agents, whereas leishmaniasis, cutaneous tuberculosis, atypical mycobacterial diseases (swimming pool granulomas) and tropical mycosis take weeks to months to appear. Swabs can be taken from the base and edges of the ulcer to determine the type of bacteria present.
Tropical ulcers are relatively rare in United States and can be challenging to diagnose 14. Tropical ulcers are best managed in collaboration with a dermatologist or infectious diseases physician.
Tropical ulcer is treated with local cleaning with soap and water or hydrogen peroxide, nonadherent antiseptic dressings and antibiotics such as penicillin or macrolide antibiotics (tetracycline) and metronidazole. Surgical debridement (removal of dead tissue) and skin grafting may be necessary.
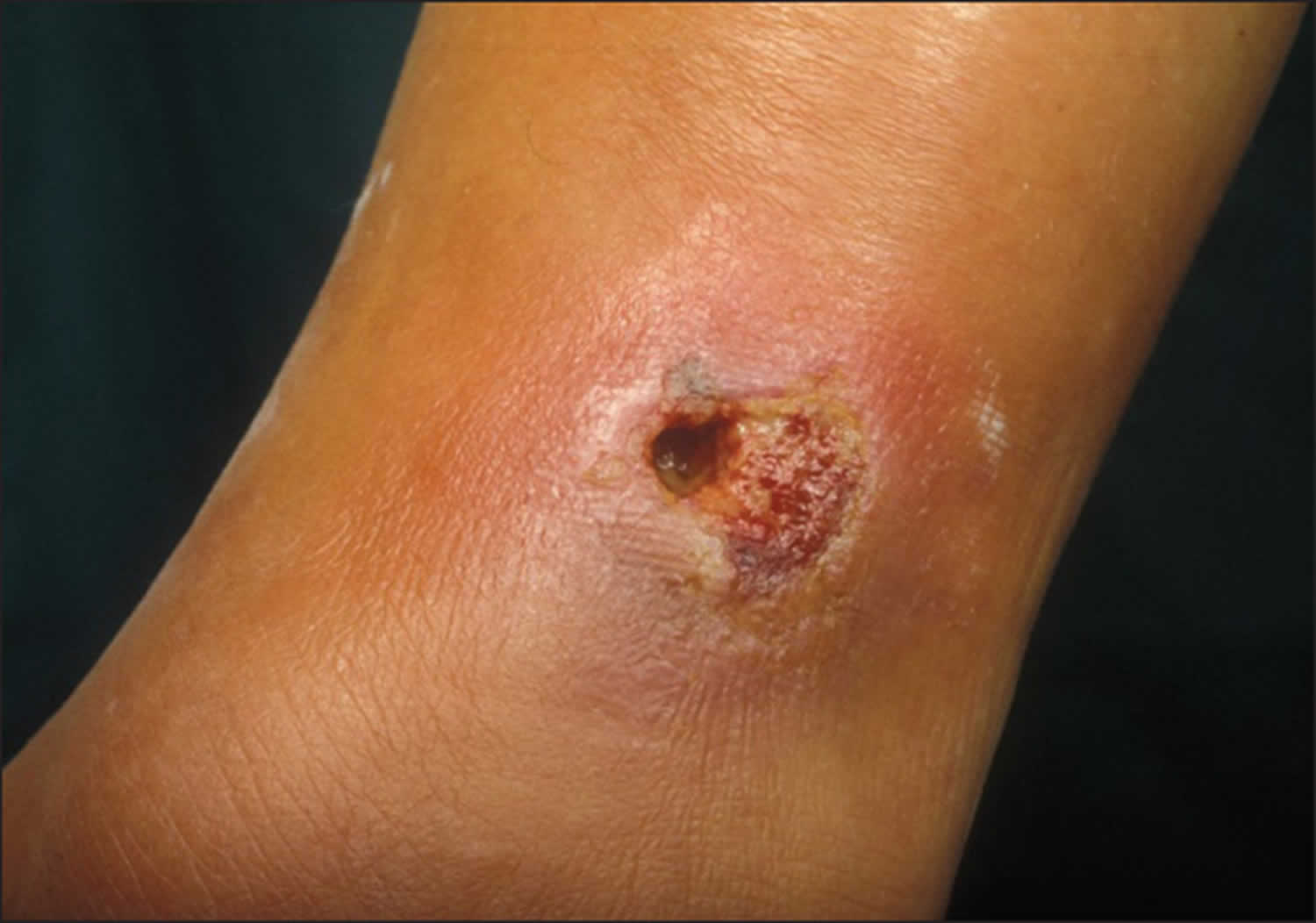
Figure 1. Tropical ulcer leg
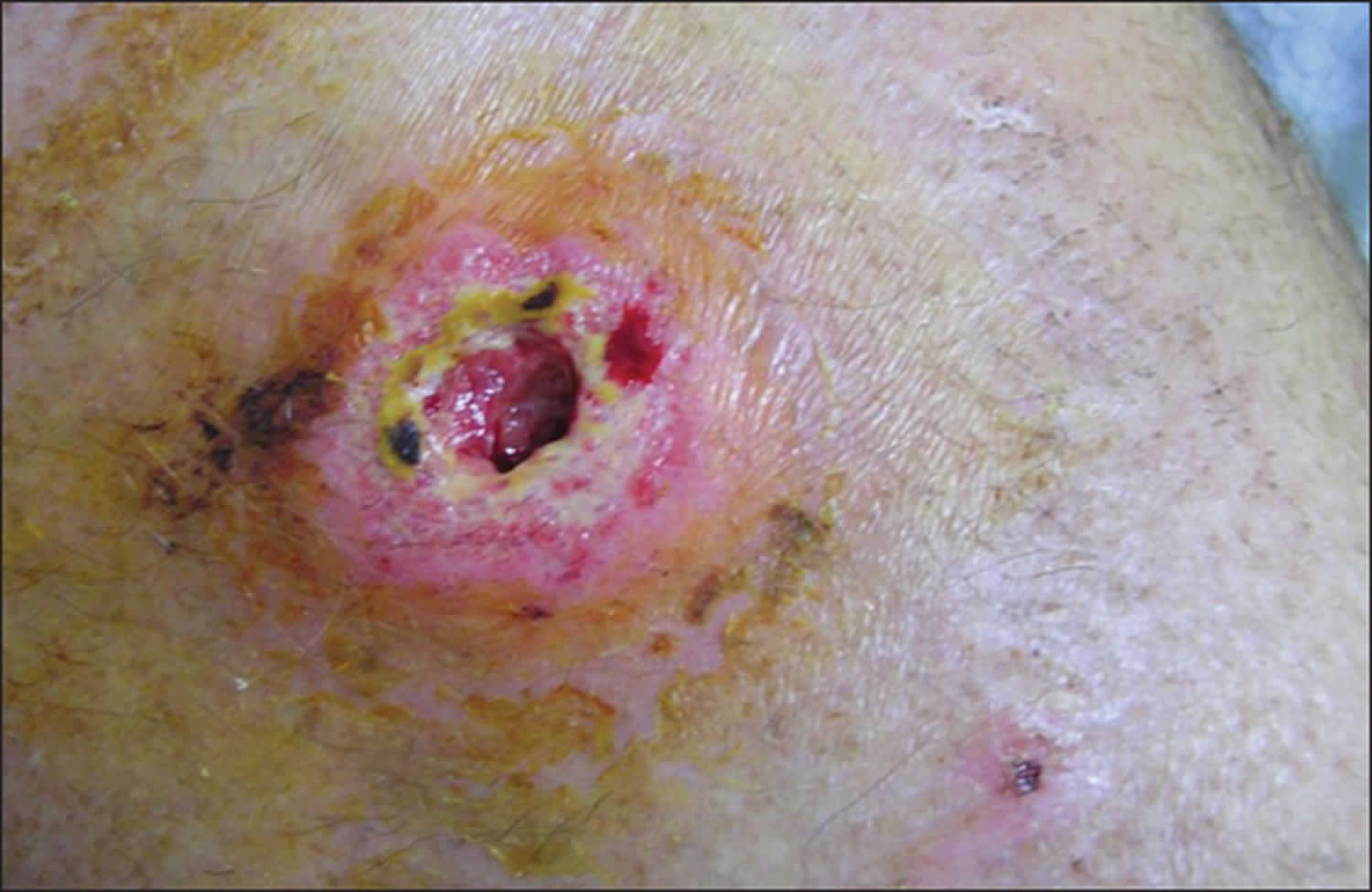
[Source 2 ]Figure 2. Tropical ulcer leg
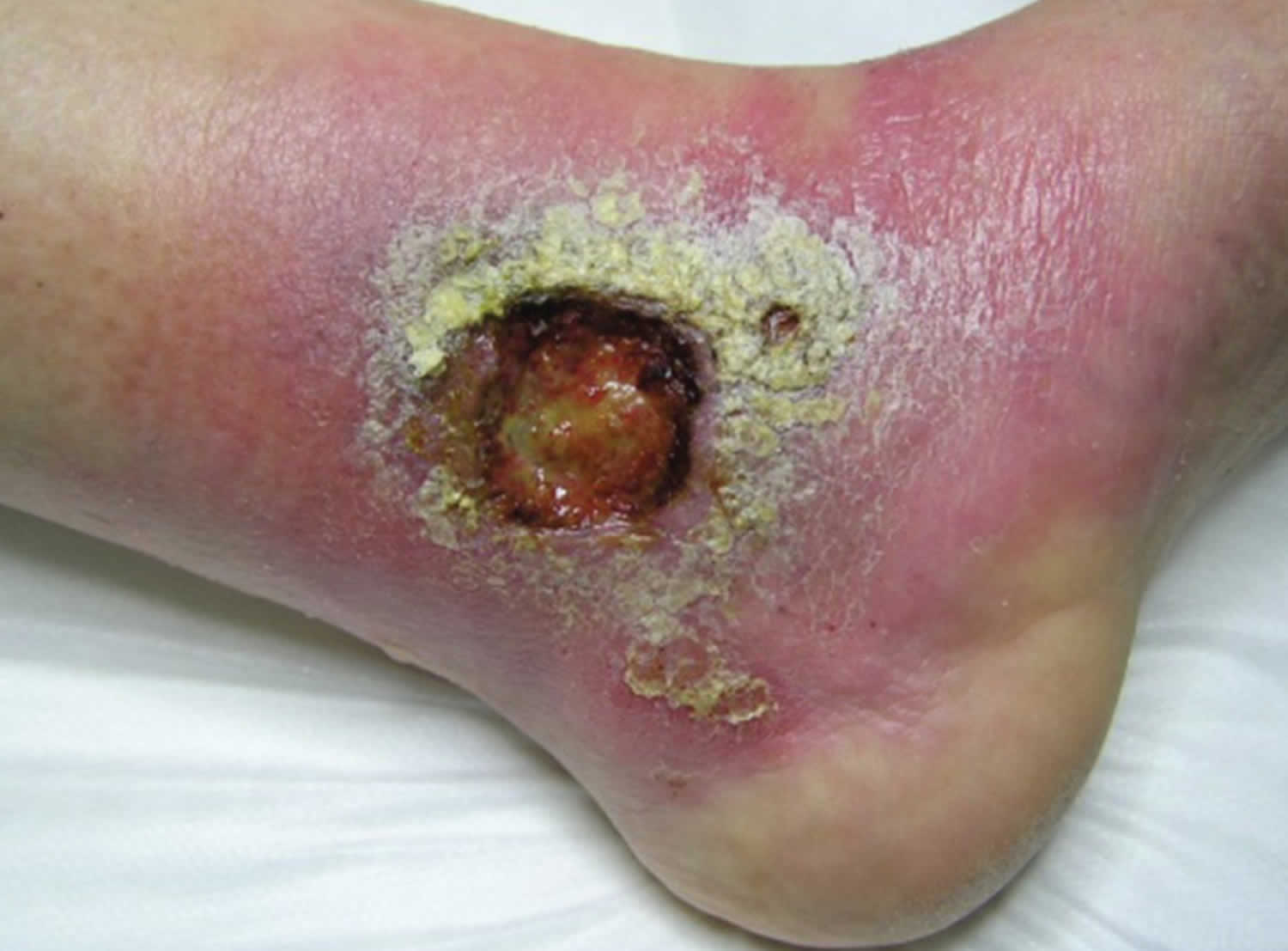
[Source 2 ]Figure 3. Tropical ulcer ankle
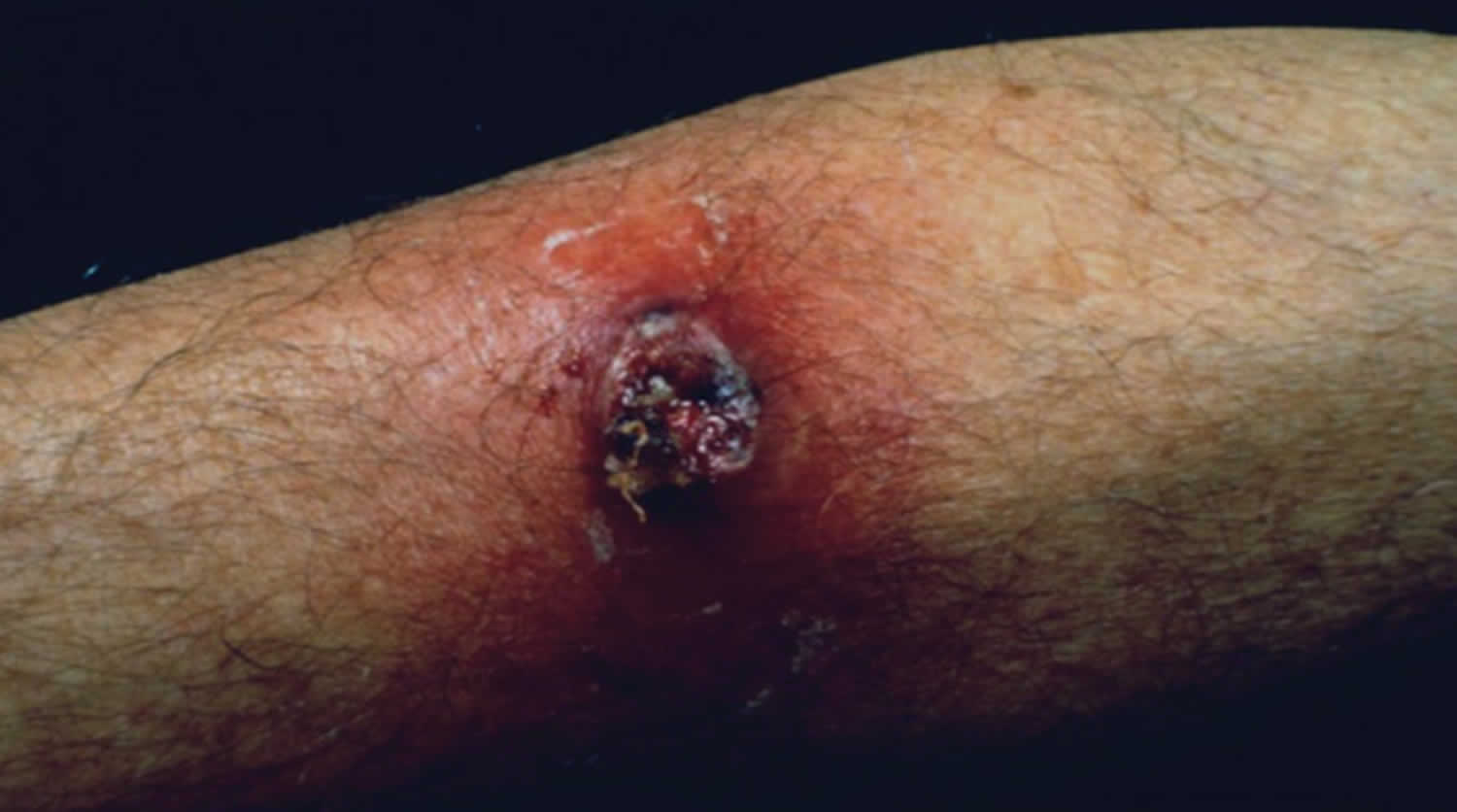
[Source 2 ]Figure 4. Tropical ulcer forearm
[Source 2 ]Tropical ulcer causes
Multiple predisposing factors play a role in causing tropical ulcers. There is initially some form of superficial trauma or injury to the skin, often as minor as a scratch or an insect bite. Rural laborers who do not wear adequate protective clothing and footwear are at increased risk of developing tropical ulcer. Poor nutrition, poor hygiene, low socioeconomic conditions, poverty, lack of protection from insect bites, exposure to muddy water, and chronic diseases such as malaria and intestinal parasites also increase the risk of a tropical ulcer developing.
Attempts to isolate the causative pathogen(s) have yielded Treponema spp., fusiform bacteria such as Fusobacterium ulcerans, Staphylococcus aureus, Corynebacterium haemolyticum and more recently Haemophilus ducreyi suggesting some or all of these organisms are involved in the pathogenesis 15, 16, 17, 7.
Tropical ulcer signs and symptoms
Clinically tropical ulcer begins as a vesicle (small blister less than 5 mm in diameter) or pustule (pus filled blister smaller than 5–10 mm in diameter) at the site of trauma most occur on the lower leg followed by ulceration with perilesional edema, purulent discharge and pain. Untreated, the ulcer shows necrotic slough and invasion of deeper subcutaneous tissues, fascia and bone. Histopathology is necessary to exclude malignancy in the chronic stage.
The lesion first appears as a small papule on the lower leg, usually at the site of trauma. The ulcer then spreads rapidly, forms a blister and undergoes necrosis, which is associated with pain, fever and malaise. Within a few weeks the ulcer enlarges to 10–12 cm and a superficial, necrotic, malodorous, purulent, hemorrhagic black coating develops. After 3–4 weeks, the edge becomes flatter, and the swelling and pain decrease 17.
Tropical ulcer diagnosis
Tropical ulcers are relatively rare in United States and can be challenging to diagnose 14. To diagnose a tropical ulcer, it is important to rule out other causes of leg ulcers such as cutaneous leishmaniasis, atypical mycobacteria, pyoderma gangrenosum, arterial ulcers, diabetes, pressure ulcer and venous disease. As tropical ulcers may mimic many other causes of skin ulceration and nodules, a history of recent travel should arouse clinical suspicion. The time frame since exposure to the causative organism is an important feature in the diagnostic process. For example, pyodermas and cutaneous larva migrans present a few days after contact with the causative agents, whereas leishmaniasis, cutaneous tuberculosis, atypical mycobacterial diseases (swimming pool granulomas) and tropical mycosis take weeks to months to appear. Swabs can be taken from the base and edges of the ulcer to determine the type of bacteria present.
Tropical ulcer differential diagnosis
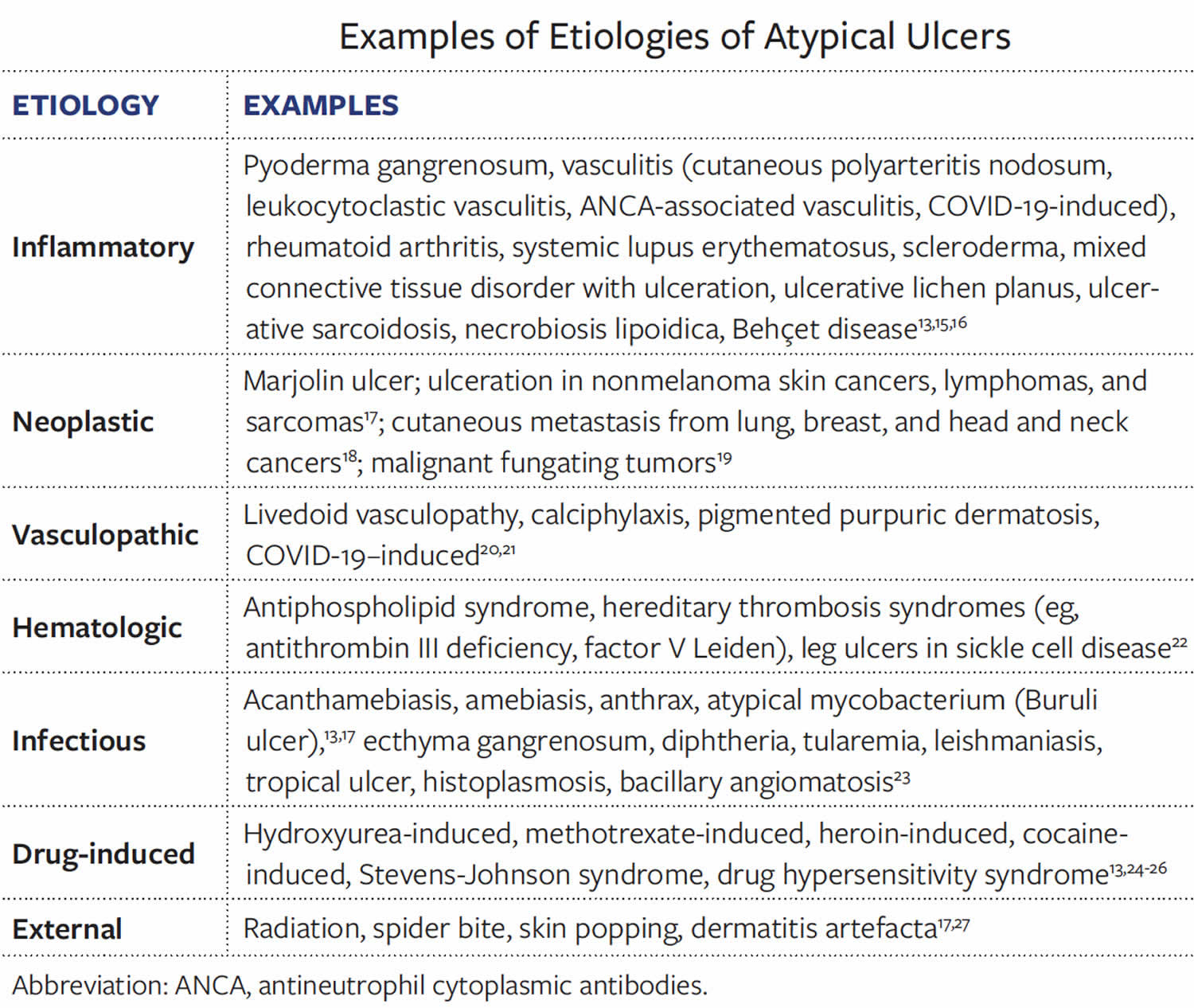
Simple tropical ulcers should be differentiated from other causes of leg ulceration that may be seen in the tropics. In contrast to buruli ulcers, for example, tropical ulcers show little undermining, whereas ulcers of cutaneous leishmaniasis are not usually painful. Appropriate investigations and skin biopsies may be needed to differentiate a tropical ulcer from other causes of chronic leg ulceration such as syphilitic gumma, pyoderma gangrenosum, venous ulcers, diabetic, vasculitic, ischemic and neoplastic ulcers 18.
Buruli ulcer also called Bairnsdale ulcer is caused by Mycobacterium ulcerans, an organism from the same family of bacteria that causes tuberculosis (Mycobacterium tuberculosis) and leprosy (Mycobacterium leprae). Buruli ulcer bacteria, Mycobacterium ulcerans, grows best at low oxygen concentrations and is found in muddy or marshy ground. It causes necrotizing ulcers in otherwise healthy people. Buruli ulcer is found in many parts of Africa – the name is derived from Buruli, a province in Uganda. It has been also reported in other parts of the world including Papua New Guinea, Australia, China, India and South America 19. Buruli ulcer can lead to massive skin ulceration, usually on the legs or arms. If untreated, the disease can spread to the bones and cause long-term disability.
Leishmaniasis is caused by the parasitic protozoan Leishmania, which is transmitted by sandflies, a tiny sand-colored blood-feeding fly called Phlebotomus papatasi sand fly that breeds in forest areas, caves and burrows in tropical and subtropical regions. There are several clinical variants of leishmaniasis, caused by different species of Leishmania. Cutaneous leishmaniasis is the most common form of the disease and is commonly seen in Iran, Afghanistan, Syria, Saudi Arabia, Peru, Brazil, the Middle East, North Africa and Asia. Leishmania tropica, Leishmania major, Leishmania infantum and Leishmania aethiopica cause old world cutaneous leishmaniasis, and Leishmania tropica mexicana, Leishmania braziliensis and Leishmania amazonensis cause new world leismaniasis. Cutaneous leishmaniasis is a common cause of skin ulceration in travellers returning from these countries. Clinical features of cutaneous leishmaniasis can vary. Typically, the lesion starts as a small red asymptomatic papule, which grows slowly into a plaque or nodule and ulcerates. There is a central crater covered with a dry scab with raised edges. There may be a halo around the lesion. In endemic areas, diagnosis of cutaneous leishmaniasis is usually made on clinical grounds alone. Microscopy of a slit skin smear or skin biopsy shows organisms within macrophages (dot and dash appearance). PCR and parasitic culture can be used to confirm the clinical diagnosis.
Venous ulcers that result from venous hypertension are the most common type of leg ulcer, affecting 1% to 3% of the US population 20. These ulcers are typically shallow, irregularly shaped wounds in the gaiter area with heavy drainage. Other symptoms suggestive of venous ulcers include varicose veins, edema, hemosiderosis, and stasis dermatitis 20.
Ischemic or arterial ulcers occur in response to an acute or chronic peripheral arterial decrease in circulation and are most commonly due to atherosclerosis 21. These ulcers tend to present as an extremely painful so-called punched-out lesions, and they are associated with signs of ischemia, described below. Risk factors for ischemic ulcers include age, smoking, diabetes, hypertension, dyslipidemia, family history, obesity, and sedentary lifestyle 21.
Diabetic foot ulcers are one of the most common complications of poorly controlled diabetes, with 5% of individuals with diabetes developing foot ulcers and 1% requiring amputation 22. The cause is multifold and includes poor blood sugar control, peripheral nerve damage, atherosclerosis, and poor foot care 22.
Pressure injuries are defined as localized damage to the skin and underlying soft tissue over a bony prominence or related to a medical device 23. These ulcers occur due to pressure, shearing forces, friction, and moisture beneath bony prominences; high-risk populations include the elderly and those bedbound with spinal cord injuries, traumatic brain injuries, or neuromuscular disorders 24.
Table 1. Tropical ulcer differential diagnosis
[Source 18 ]Tropical ulcer treatment
Tropical ulcers are best managed in collaboration with a dermatologist or infectious diseases physician. First-line treatment for tropical ulcers is a combination of penicillin (500 mg every 6 hours for 1 week) and metronidazole (250 mg every 8 hours for 10 days) 25. For patients who are allergic to penicillin, tetracycline (minocycline 100 mg twice daily or doxycycline 100 mg twice daily) can be given instead. Antibiotic treatment should be combined with proper would care and cleansing, immobilization and nutritional support. Large ulcers (>5 cm) require wound debridement and skin grafting 25.
- Mendiratta, V. and Agarwal, S. (2019). Tropical Ulcer. In Harper’s Textbook of Pediatric Dermatology (eds P. Hoeger, V. Kinsler, A. Yan, J. Harper, A. Oranje, C. Bodemer, M. Larralde, D. Luk, V. Mendiratta and D. Purvis). https://doi.org/10.1002/9781119142812.ch45[↩][↩][↩]
- Veraldi S, Faraci AG, Valentini D, Bottini S. Tropical ulcers: the first imported cases and review of the literature. Eur J Dermatol. 2021 Feb 1;31(1):75-80. doi: 10.1684/ejd.2021.3968[↩][↩][↩][↩][↩]
- Gear JH. Aetiology of tropical ulcer. Trans R Soc Trop Med Hyg. 1990 Sep-Oct;84(5):753. doi: 10.1016/0035-9203(90)90178-h[↩]
- Falkler WA Jr, Montgomery J, Nauman RK, Alpers M. Isolation of Fusobacterium nucleatum and electron microscopic observations of spirochetes from tropical skin ulcers in Papua New Guinea. Am J Trop Med Hyg. 1989 Apr;40(4):390-8. doi: 10.4269/ajtmh.1989.40.390[↩]
- Adriaans B. Tropical ulcer–a reappraisal based on recent work. Trans R Soc Trop Med Hyg. 1988;82(2):185-9. doi: 10.1016/0035-9203(88)90402-[↩]
- Smith CG. Tropical ulcer. Trans R Soc Trop Med Hyg. 1990 Jan-Feb;84(1):175-6. doi: 10.1016/0035-9203(90)90425-e[↩]
- Prescott TAK, Homot P, Lundy FT, Fang R, Patrick S, Cámara-Leret R, Kiapranis R. Tropical ulcer plant treatments used by Papua New Guinea’s Apsokok nomads. J Ethnopharmacol. 2017 Jun 9;205:240-245. doi: 10.1016/j.jep.2017.05.001[↩][↩]
- Tropical ulcer. https://dermnetnz.org/topics/tropical-ulcer[↩][↩][↩]
- Lupi O, Madkan V, Tyring SK. Tropical dermatology: bacterial tropical diseases. J Am Acad Dermatol. 2006 Apr;54(4):559-78; quiz 578-80. https://doi.org/10.1016/j.jaad.2005.03.066[↩]
- Giacani L, Lukehart SA. The endemic treponematoses. Clin Microbiol Rev. 2014 Jan;27(1):89-115. doi: 10.1128/CMR.00070-13[↩]
- Kazadi WM, Asiedu KB, Agana N, Mitjà O. Epidemiology of yaws: an update. Clin Epidemiol. 2014 Apr 2;6:119-28. doi: 10.2147/CLEP.S44553[↩]
- Adriaans B, Drasar BS. The isolation of fusobacteria from tropical ulcers. Epidemiol Infect. 1987 Oct;99(2):361-72. doi: 10.1017/s0950268800067844[↩]
- Tropical and exotic dermatoses and ulcers . https://www.racgp.org.au/afp/2014/september/tropical-and-exotic-dermatoses-and-ulcers[↩]
- Zeegelaar JE, Faber WR. Imported tropical infectious ulcers in travelers. Am J Clin Dermatol. 2008;9(4):219-32. doi: 10.2165/00128071-200809040-00002[↩][↩]
- Adriaans B, Shah H. Fusobacterium ulcerans sp. nov. from tropical ulcers. Int J Syst Bacteriol 1988; 38: 447–8. https://doi.org/10.1099/00207713-38-4-447[↩]
- Adriaans B. Tropical ulcer–a reappraisal based on recent work. Trans R Soc Trop Med Hyg. 1988;82(2):185-9. doi: 10.1016/0035-9203(88)90402-6[↩]
- Lupi O, Madkan V, Tyring SK. Tropical dermatology: bacterial tropical diseases. J Am Acad Dermatol. 2006 Apr;54(4):559-78; quiz 578-80. doi: 10.1016/j.jaad.2005.03.066[↩][↩]
- Nickles MA, Tsoukas MM, Sweiss N, Ennis W, Altman IA. Atypical ulcers: a stepwise approach for clinicians. Wounds. 2022 Oct;34(10):236-244. https://www.hmpgloballearningnetwork.com/site/wounds/review/atypical-ulcers-stepwise-approach-clinicians[↩][↩]
- Thangaraj HS, Evans MR, Wansbrough-Jones MH. Mycobacterium ulcerans disease; Buruli ulcer. Trans R Soc Trop Med Hyg. 1999 Jul-Aug;93(4):337-40. doi: 10.1016/s0035-9203(99)90104-9[↩]
- Bonkemeyer Millan S, Gan R, Townsend PE. Venous ulcers: diagnosis and treatment. Am Fam Physician. 2019;100(5):298–305. https://www.aafp.org/pubs/afp/issues/2019/0901/p298.html[↩][↩]
- Hess CT. Arterial ulcer checklist. Adv Skin Wound Care. 2010 Sep;23(9):432. doi: 10.1097/01.ASW.0000383218.26406.4b[↩][↩]
- Oliver TI, Mutluoglu M. Diabetic Foot Ulcer. [Updated 2023 Aug 8]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2023 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK537328[↩][↩]
- Pressure Injury and Stages. https://cdn.ymaws.com/npiap.com/resource/resmgr/NPIAP-Staging-Poster.pdf[↩]
- Evans JM, Andrews KL, Chutka DS, Fleming KC, Garness SL. Pressure ulcers: prevention and management. Mayo Clin Proc. 1995 Aug;70(8):789-99. doi: 10.4065/70.8.789[↩]
- Tropical and exotic dermatoses and ulcers. https://www.racgp.org.au/afp/2014/september/tropical-and-exotic-dermatoses-and-ulcers[↩][↩]