Contents
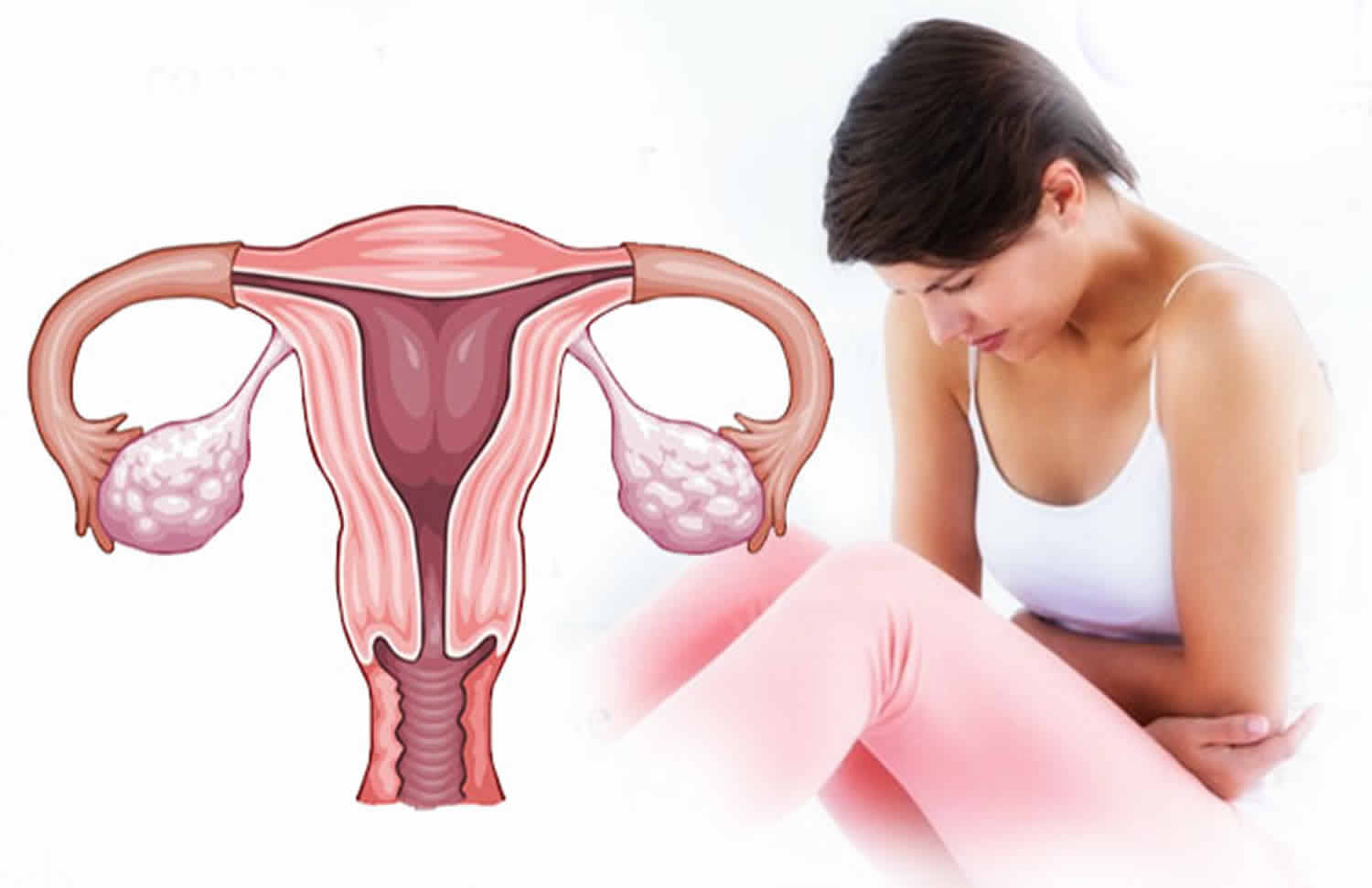
What is abnormal uterine bleeding
Abnormal uterine bleeding is more commonly referred to as “abnormal vaginal bleeding”, which is any heavy or unusual bleeding from the uterus through your vagina 1, 2. Abnormal uterine bleeding may include spotting of small amounts of blood between periods — often seen on toilet tissue after wiping — or extremely heavy periods in which you soak a pad or tampon every one to two hours for two or more hours. Abnormal uterine bleeding can occur at any time during your monthly cycle, including during your normal menstrual period.
In most women, abnormal uterine bleeding is caused by a hormone imbalance. When hormones are the problem, doctors call the problem dysfunctional uterine bleeding. Abnormal bleeding caused by hormone imbalance is more common in teenagers or in women who are approaching menopause.
Vaginal bleeding between periods is one symptom of abnormal uterine bleeding. Having extremely heavy bleeding during your period can also be considered abnormal uterine bleeding. Very heavy bleeding during a period and/or bleeding that lasts more than 7 days is called menorrhagia. For example, women may bleed enough to soak through 1 or more tampons or sanitary pads every hour.
Normal vaginal bleeding occurs with the female ovulatory cycle beginning with the menarche, or onset of menses, which generally occurs at 10 to 15 years of age. Normal vaginal bleeding or menstruation, occurs every 21 to 35 days when the uterus sheds its lining, marking the start of a new reproductive cycle. A menstrual period may last for just a few days or up to a week. Your flow may be heavy or light and still considered normal. Menstrual cycles tend to be longer for teens and for women nearing menopause, and menstrual flow may also be heavier at those ages. Menstrual period ends with the menopause, or cessation of menses, generally between age 45 and 50 years 3.
Many women have abnormal uterine bleeding between their periods at some point in their lives. Abnormal uterine bleeding occurs when you have:
- Heavier bleeding than usual
- Bleeding for more days than normal (menorrhagia)
- Spotting or bleeding between periods
- Bleeding after sex
- Bleeding after menopause
- Bleeding while pregnant
- Bleeding before age 9
- Menstrual cycles longer than 35 days or shorter than 21 days
- No period for 3 to 6 months (amenorrhea)
A variety of things can cause abnormal uterine bleeding. Pregnancy is a common cause. Polyps or uterine fibroids (small and large growths) in the uterus can also cause bleeding. Rarely, a thyroid problem, infection of the cervix, or cancer of the uterus can cause abnormal uterine bleeding.
These are just a few of the problems that can cause abnormal uterine bleeding. These problems can occur at any age, but the likely cause of abnormal uterine bleeding usually depends on your age.
Women in their teens, 20s, and 30s
A common cause of abnormal bleeding in young women and teenagers is pregnancy. Many women have abnormal bleeding in the first few months of a normal pregnancy. Some birth control pills or the intrauterine device (IUD) can also cause abnormal bleeding.
Some young women who have abnormal uterine bleeding do not release an egg from their ovaries (called ovulation) during their menstrual cycle. This is common for teenagers who have just started getting their periods. This causes a hormone imbalance where the estrogen in your body makes the lining of your uterus (called the endometrium) grow until it gets too thick. When your body gets rid of this lining during your period, the bleeding will be very heavy. A hormone imbalance may also cause your body not to know when to shed the lining. This can cause irregular bleeding (“spotting”) between your periods.
Women in their 40s and early 50s
In the years before menopause and when menopause begins, women have months when they don’t ovulate. This can cause abnormal uterine bleeding, including heavy periods and lighter, irregular bleeding.
Thickening of the lining of the uterus is another cause of bleeding in women in their 40s and 50s. This thickening can be a warning of uterine cancer. If you have abnormal uterine bleeding and you’re in this age group, you need to tell your doctor about it. It may be a normal part of getting older, but it’s important to make sure uterine cancer isn’t the cause.
Women after menopause
Hormone replacement therapy is a common cause of uterine bleeding after menopause. Other causes include endometrial and uterine cancer. These cancers are more common in older women than in younger women. But cancer is not always the cause of abnormal uterine bleeding. Many other problems can cause bleeding after menopause. For this reason, it’s important to talk to your doctor if you have any bleeding after menopause.
The history should determine the following information:
- Premenarchal bleeding, which may be associated with precocious puberty (bleeding before the age of 9 years)
- Onset and cessation of menses
- The characteristics of the menstrual cycle: interval, duration, amount of flow, last monthly period
- Postcoital bleeding (any bleeding after intercourse or in association with douching)
- Postmenopausal bleeding (any bleeding occurring in the postmenopausal female)
If you’re pregnant, see your doctor immediately if you notice vaginal bleeding.
In general, anytime you experience unexpected vaginal or uterine bleeding, consult your doctor. Whether or not uterine bleeding is normal depends on your age and the circumstances.
See your doctor in the following situations:
- Postmenopausal women not taking hormone therapy should see a doctor if they experience uterine bleeding.
- Postmenopausal women taking cyclic hormone therapy may experience some uterine bleeding. A cyclic hormone therapy regimen — oral estrogen daily plus oral progestin for 10 to 12 days a month — can lead to uterine bleeding that resembles a period (withdrawal bleeding) for a few days out of the month. If you have uterine bleeding other than expected withdrawal bleeding, contact your doctor.
- Postmenopausal women taking continuous hormone therapy — a low-dose combination of estrogen and progestin daily — may experience light, irregular uterine bleeding for the first six months. If uterine bleeding persists longer or heavy uterine bleeding begins, see your doctor.
- Girls who don’t have any other signs of puberty or are younger than age 8 should have any uterine bleeding investigated.
- You have soaked through a pad or tampon every hour for 2 to 3 hours.
- Your bleeding lasts longer than 1 week.
- You have vaginal bleeding and you are pregnant or could be pregnant.
- You have severe pain, especially if you also have pain when not menstruating.
- Your periods have been heavy or prolonged for three or more cycles, compared to what is normal for you.
- You have bleeding or spotting after reaching menopause.
- You have bleeding or spotting between periods or caused by having sex.
- Abnormal bleeding returns.
- Bleeding increases or becomes severe enough to cause weakness or lightheadedness.
- You have fever or pain in the lower abdomen
- Your symptoms become more severe or frequent.
The following situations are likely normal, but talk to your doctor if you’re concerned:
- Newborn girls may have some vaginal bleeding during the first month of life. Bleeding that’s excessive or lasts longer should be checked out.
- Teenagers who have just begun having periods may experience irregular cycles during the first few years. In addition, many girls and women have light spotting for a few days before menstruating.
- Women starting birth control pills may experience occasional spotting the first few months.
- Women nearing menopause (perimenopause) may experience increasingly heavy or irregular periods. Ask your doctor about possible treatments to minimize your symptoms.
Dysfunctional uterine bleeding symptoms
Symptoms of abnormal vaginal bleeding include:
- Bleeding or spotting between periods
- Bleeding after sex
- Bleeding more heavily (passing large clots, needing to change protection during the night, soaking through a sanitary pad or tampon every hour for 2 to 3 hours in a row)
- Bleeding for more days than normal or for more than 7 days
- Menstrual cycle less than 28 days (more common) or more than 35 days apart
- Bleeding after you have gone through menopause
- Heavy bleeding associated with anemia (low blood count, low iron)
Bleeding from the rectum or blood in the urine may be mistaken for vaginal bleeding. To know for certain, insert a tampon into the vagina and check for bleeding.
Keep a record of your symptoms and bring these notes to your doctor. Your record should include:
- When menstruation begins and ends
- How much flow you have (count numbers of pads and tampons used, noting whether they are soaked)
- Bleeding between periods and after sex
- Any other symptoms you have
Dysfunctional uterine bleeding causes
There are many causes of dysfunctional uterine bleeding or vaginal bleeding. Dysfunctional uterine bleeding can relate to an issue with your reproductive system (a gynecologic condition) or to other medical problems or certain medications. If you have reached menopause — defined as 12 consecutive months, give or take, without a menstrual period — subsequent vaginal bleeding may be a cause for concern and should be evaluated.
Most conditions that cause abnormal uterine bleeding can occur at any age, but some are more likely to occur at a particular time in a woman’s life.
Abnormal uterine bleeding in young girls
Bleeding before menarche (the first period in a girl’s life) is always abnormal. It may be caused by trauma, a foreign body (such as toys, coins, or toilet tissue), irritation of the genital area (due to bubble bath, soaps, lotions, or infection), or urinary tract problems. Bleeding can also occur as a result of sexual abuse.
Abnormal uterine bleeding in adolescents
Many girls have episodes of irregular bleeding during the first few months after their first menstrual period. This usually resolves without treatment when the girl’s hormonal cycle and ovulation normalizes. If irregular bleeding persists beyond this time, or if the bleeding is heavy, further evaluation is needed.
Abnormal bleeding in teens can also be caused by any of the conditions that cause bleeding in all premenopausal women, including: pregnancy, infection, and bleeding disorder or other medical illnesses. These and other causes are discussed in the next section.
Abnormal uterine bleeding in premenopausal women
Many different conditions can cause abnormal bleeding in women between adolescence and menopause. Abrupt changes in hormone levels at the time of ovulation can cause vaginal spotting, or small amounts of bleeding. Breakthrough bleeding can also occur in premenopausal women who use hormonal birth control methods.
Some women do not ovulate regularly and may experience unpredictable light or heavy vaginal bleeding. Although irregular ovulation is most common when periods first begin and during perimenopause, it can occur at any time during the reproductive years.
Some women who ovulate regularly experience excessive blood loss during their periods or bleed between periods. The most common causes of such bleeding are uterine fibroids, uterine adenomyosis, or endometrial polyps. Fibroids are benign masses in the muscle layer of the uterus (myometrium), while adenomyosis is a condition in which the lining of the uterus (endometrium) grows into the myometrium. Endometrial polyps are fleshy (usually benign) growths of tissue which project into the uterine cavity. These conditions are common causes of abnormal uterine bleeding. Fibroids, adenomyosis and polyps can also occur in anovulatory women.
Other causes of abnormal uterine bleeding in premenopausal women include:
- Pregnancy
- Cancer or precancer of the cervix or the endometrium (lining of the uterus)
- Infection or inflammation of the cervix or endometrium
- Clotting disorders such as von Willebrand disease, platelet abnormalities, or problems with clotting factors
- Medical illnesses such as hypothyroidism, liver disease, or chronic renal disease
Abnormal uterine bleeding when using hormonal birth control
Girls and women who use hormonal birth control (e.g., pills, ring, patch) may experience “breakthrough” bleeding between periods. If this occurs during the first few months, it may be due to changes in the lining of the uterus. If it persists for more than a few months, evaluation may be needed and/or a different birth control pill may be recommended. Initially, women using injectable contraception often experience irregular bleeding; over time, bleeding stops occurring in such women. Irregular bleeding is common in women using the contraceptive implant. In women using progestin-releasing intrauterine devices (IUDs), bleeding is often irregular at first. Over time, bleeding becomes lighter; long-term, such women often experience scant bleeding spotting or no bleeding.
Breakthrough bleeding can also happen if a hormonal birth control method is forgotten or taken late. In this situation, there is a risk that the woman could become pregnant if she has sex. An alternate or “back-up” form of birth control (e.g., condoms) is recommended if the pill/patch/shot is not taken on time.
Abnormal uterine bleeding in women in perimenopause
Before menstrual periods end, a woman passes through a period called the menopausal transition or perimenopause. During the menopausal transition, the timing of periods begins to change as ovulation becomes less regular. While ovaries in perimenopausal women continue to make estrogen, progesterone secretion declines. These hormonal changes can cause the endometrium to grow and produce excess tissue, increasing the chances that polyps or endometrial hyperplasia (thickened lining of the uterus that can progress to cancer) will develop and potentially cause abnormal bleeding. The menopausal transition is a time when women are more likely to experience abnormal uterine bleeding.
Women in the menopausal transition are also at risk for other conditions that cause abnormal bleeding, including cancer, infection, and body-wide (systemic) illnesses. Further evaluation is needed in women with persistent irregular menstrual cycles or an episode of profuse bleeding.
Women in the menopausal transition still ovulate some of the time and can become pregnant; pregnancy itself can cause abnormal bleeding. In addition, women in perimenopause may use hormonal birth control medications, which can cause breakthrough bleeding.
Abnormal uterine bleeding in menopausal women
A number of conditions can cause abnormal bleeding during the menopause. Women who take hormone therapy may experience cyclical bleeding. Any other bleeding that occurs during menopause is abnormal and should be investigated. Causes of abnormal bleeding during menopause include:
- Atrophy or excessive thinning of the tissue lining the vagina and uterus, caused by low hormone levels
- Cancer or precancerous changes (hyperplasia) of the uterine lining (endometrium)
- Polyps or fibroids
- Infection of the uterus
- Use of blood thinners or anticoagulants
- Side effects of radiation therapy
Possible causes of dysfunctional uterine bleeding
- Cancers and precancerous conditions
- Cervical cancer
- Endometrial cancer (uterine cancer)
- Endometrial hyperplasia
- Ovarian cancer
- Uterine sarcoma
- Vaginal cancer
- Endocrine system factors
- Hyperthyroidism (overactive thyroid)
- Hypothyroidism (underactive thyroid)
- Polycystic ovary syndrome (PCOS)
- Stopping or changing birth control pills or menopausal hormone therapy (withdrawal bleeding)
- Fertility and reproduction factors
- Ectopic pregnancy
- Fluctuating hormone levels
- Miscarriage (before the 20th week of pregnancy)
- Pregnancy
- Random ovulatory cycles
- Sexual intercourse
- Perimenopause (the transition time before menopause)
- Vaginal atrophy (genitourinary syndrome of menopause)
- Infections
- Cervicitis (an inflammation of the cervix)
- Chlamydia trachomatis
- Endometritis
- Gonorrhea
- Pelvic inflammatory disease (PID) — infection of the female reproductive organs
- Ureaplasma vaginitis
- Vaginitis (bacterial vaginosis)
- Medical conditions
- Celiac disease
- Severe systemic disease, such as kidney or liver disease
- Thrombocytopenia
- Von Willebrand disease (and other blood clotting disorders)
- Diabetes
- Cirrhosis of the liver
- Lupus erythematosus
- Bleeding disorders
- Medications and devices
- Forgotten (retained) tampon
- Use of an intrauterine device (IUD) for birth control (may cause spotting)
- Stopping or changing birth control pills or menopausal hormone therapy (withdrawal bleeding)
- Tamoxifen side effect
- Noncancerous growths and other uterine conditions
- Adenomyosis
- Cervical polyps — noncancerous (benign) growths on your cervix
- Uterine fibroids
- Uterine polyps (endometrial polyps)
- Trauma
- Blunt trauma or penetrating injury to the vagina or cervix
- Sexual abuse
- Other causes may include:
- Cervical or endometrial biopsy or other procedures
- Changes in exercise routine
- Diet changes
- Recent weight loss or gain
- Stress
- Use of certain drugs such as blood thinners (warfarin or Coumadin)
- An object in the vagina.
Can abnormal uterine bleeding be prevented or avoided?
If your abnormal uterine bleeding is caused by hormonal changes, you will not be able to prevent it. But if your hormonal changes are caused by being overweight, losing weight could help. Your weight affects your hormone production. Maintaining a healthy weight can help prevent abnormal uterine bleeding.
Dysfunctional uterine bleeding diagnosis
While taking your medical history, a clinician will review the duration and amount of bleeding; factors that seem to bring the bleeding on; symptoms that occur along with the bleeding such as pain, fever, or vaginal odor; if bleeding occurs after sexual intercourse; whether there is a personal or family history of bleeding disorders; the woman’s medical history and medications she is taking; recent weight changes, stress, a new exercise program, or underlying medical problems.
Exams and Tests
A doctor will perform a physical examination to evaluate the woman’s overall health, and a pelvic examination to confirm that the bleeding is from the uterus and not from another site (e.g, the external genitals or rectum). During the pelvic exam, the clinician will look for any obvious lesions (cuts, sores, or tumors) and will examine the size and shape of the uterus. He or she will examine the cervix to look for signs of cervical bleeding, and a Pap smear/human papillomavirus (HPV) test may be obtained to screen for cervical cancer (the cervix is at the lower end of the uterus, where it opens to the vagina).
You may have certain tests, including:
- Pap test
- Urinalysis
- Thyroid functioning tests
- Complete blood count (CBC)
- Iron count
- Pregnancy test
Based on your symptoms, other tests may be needed. Some can be done in your provider’s office. Others may be done at a hospital or surgical center:
Endometrial assessment
Tests that assess the endometrium (lining of the uterus) may be performed to rule out endometrial cancer and structural abnormalities such as uterine fibroids or polyps. Such tests include:
Endometrial biopsy — An endometrial biopsy is often performed in women age 45 or older to rule out endometrial cancer or abnormal endometrial growths. A biopsy may also be performed in women younger than 45 years if they have risk factors for endometrial cancer or are felt to be at increased risk for an infection of the endometrium. Risks for endometrial cancer include obesity, chronic anovulation, history of breast cancer, tamoxifen use or a family history of breast cancer or colon cancer.
During the biopsy, a thin instrument is inserted through the vagina and cervix into the uterus to obtain a small sample of endometrial tissue. The biopsy (which often causes temporary severe uterine cramping) can be performed in a healthcare provider’s office without anesthesia. Because only a small portion of the endometrium is sampled, the biopsy may miss some causes of bleeding and other tests are sometimes necessary.
Transvaginal ultrasound — An ultrasound uses sound waves to measure an organ’s shape and structure. In a transvaginal ultrasound, an ultrasound probe is inserted into the vagina so that it is closer to the uterus and can provide a clear image of the uterus. The lining of the uterus is evaluated and measured; postmenopausal women normally have a thin endometrial lining; in postmenopausal women with uterine bleeding, if the lining is thicker than 4 or 5 mm, additional evaluation with an endometrial biopsy may be appropriate. Ultrasound cannot distinguish between different types of abnormalities (eg, polyp versus cancer) and further testing may be necessary.
Saline infusion sonography (sonohysterography) — In this test, a transvaginal ultrasound is performed after sterile saline is infused into the uterus. This procedure gives a better picture of the inside of the uterus, and small lesions can be more easily detected. However, because tissue samples cannot be obtained during the procedure, a final diagnosis is not always possible and additional evaluation, often hysteroscopy or dilation and curettage (D&C), may be necessary.
Hysteroscopy — During hysteroscopy, a small scope is inserted through the cervix and into the uterus. Air or fluid is injected to expand the uterus and to allow the physician to see the inside of the uterus. Tissue samples may be taken. Anesthesia may be used to minimize discomfort during the procedure. Hysteroscopy may be performed in the office or in a same-day surgery in an operating room.
Dilation and curettage (D&C) — In a D&C, the cervix or opening of the uterus is dilated and instruments are inserted and used to remove endometrial or uterine tissue. A D&C usually requires anesthesia.
Magnetic resonance imaging (MRI) — In this imaging test, powerful magnets are used to create images of internal organs.
Dysfunctional uterine bleeding treatment
There are several treatment options for abnormal bleeding. Your treatment will depend on the cause of your bleeding, your age, and whether you want to get pregnant in the future. Your doctor will help you decide which treatment is right for you. Or, if your doctor decides that a hormone imbalance is causing your abnormal bleeding, you and your doctor may decide to wait and see if the bleeding improves on its own. Some treatment options include the following:
Treatment depends on the specific cause of the vaginal bleeding, including:
- Hormonal changes
- Endometriosis
- Uterine fibroids
- Ectopic pregnancy
- Polycystic ovary syndrome (PCOS)
Treatment may include hormonal medicines, pain relievers, and possibly surgery.
Medication to stop uterine bleeding
The type of hormone you take will depend on whether you want to get pregnant as well as your age:
- Birth control pills can help make your periods more regular.
- Hormones also can be given as an injection, a skin patch, a vaginal cream, or through an intrauterine contraceptive device (IUD) that releases hormones.
- An intrauterine contraceptive device (IUD) is a birth control device that is inserted in the uterus. The hormones in the IUD are released slowly and may control abnormal bleeding.
Other medicines given for abnormal uterine bleeding may include:
- Nonsteroidal anti-inflammatory drugs (ibuprofen or naproxen) to help control bleeding and reduce menstrual cramps. If you have heavy menstrual bleeding, try taking ibuprofen (Advil, Motrin) during your period (or a few days before you expect your period, if you know). Ibuprofen is a nonsteroidal anti-inflammatory drug (NSAID). NSAIDs can work to reduce the bleeding during your period.
- Tranexamic acid to help treat heavy menstrual bleeding
- Antibiotics to treat infections
- Gonadotropin-releasing hormone (GnRH) agonists—These drugs can stop the menstrual cycle and reduce the size of fibroids.
- Special medications—If you have a bleeding disorder, your treatment may include medication to help your blood clot.
- You also should make sure that you are getting enough iron in your diet. Your doctor may prescribe an iron supplement to ensure that you don’t become anemic.
Birth control pills
Birth control pills are often used to treat uterine bleeding that is due to hormonal changes or hormonal irregularities. Birth control pills may be used in women who do not ovulate regularly to establish regular bleeding cycles and prevent excessive growth of the endometrium. In women who do ovulate, they may be used to treat excessive menstrual bleeding. Nonsteroidal anti-inflammatory drugs (NSAIDS, e.g., ibuprofen, naproxen sodium) may also be helpful in reducing blood loss and cramping in these women.
During the menopausal transition, birth control pills or other hormonal therapy may be used to regulate the menstrual cycle and prevent excessive growth of the endometrium.
Progesterone
Progesterone is a hormone made by the ovary that is effective in preventing or treating excessive bleeding in women who do not ovulate regularly. A synthetic form of progesterone, called progestin, may be recommended to treat abnormal bleeding. Progestins are usually given as pills (eg, medroxyprogesterone acetate, norethindrone acetate), and are taken once a day for 10 to 12 days each month or taken continuously (every day). In women taking monthly cyclical progestin therapy, vaginal bleeding may occur cyclically. Cyclical progestin therapy does not provide consistent contraception. In women using cyclical progestin therapy and experiencing cyclical bleeding, if the expected bleeding does not occur, the possibility of pregnancy should be explored.
Progestins may also be given in other ways, such as in an injection, an implant, or an intrauterine device. These treatments are discussed in detail in a separate topic review.
Intrauterine device (IUD)
An intrauterine contraceptive device (IUD) that secretes progestin (e.g., Mirena, Liletta, Kyleena, or Skyla) may be recommended for women who have abnormal uterine bleeding. IUDs are T-shaped devices inserted by a healthcare provider through the vagina and cervix into the uterus. IUDs include an attached plastic string that projects through the cervix, enabling the woman to check that the device remains in place.
Progestin-releasing IUDs decrease menstrual blood loss by more than 50 percent and decrease pain associated with periods. Some women completely stop having menstrual bleeding as a result of the IUD, which is reversible when the IUD is removed.
Dilatation and curettage (D&C)
A D&C is a procedure in which the opening of your cervix is stretched just enough so a surgical tool can be put into your uterus. Your doctor uses this tool to scrape away the lining of your uterus. The removed lining is checked in a lab for abnormal tissue. A D&C is done under general anesthesia (while you’re in a sleep-like state).
If you’re having heavy bleeding, your doctor may perform a D&C both to find out the problem and to treat the bleeding. The D&C itself often makes heavy bleeding stop. Your doctor will decide if this procedure is necessary.
Surgery
Surgery may be necessary to remove abnormal uterine structures (e.g, fibroids, polyps). Women who have completed childbearing and have heavy menstrual bleeding can consider a surgical procedure such as endometrial ablation. This procedure may be performed in a gynecologist’s office or in an operating room as a same-day surgery, and uses heat, cold, electrical energy, or a laser to destroy the lining of the uterus.
Women with fibroids can have surgical treatment of their fibroids, either by removing the fibroid(s) (e.g., myomectomy) or by reducing the blood supply of the fibroids (e.g., uterine artery embolization). The most definitive surgical treatment for abnormal uterine bleeding is hysterectomy, or removal of the entire uterus. At the time of hysterectomy, the ovaries may be left in place or removed. Hysterectomy may be performed by conventional laparoscopy or robotic laparoscopy (“belly button surgery”), through the vagina, or by an open incision on the abdomen.
- Abnormal Uterine Bleeding. https://familydoctor.org/condition/abnormal-uterine-bleeding[↩]
- Vaginal bleeding. https://www.mayoclinic.org/symptoms/vaginal-bleeding/basics/definition/sym-20050756[↩]
- Chapter 173Abnormal Vaginal Bleeding. Clinical Methods: The History, Physical, and Laboratory Examinations. 3rd edition. https://www.ncbi.nlm.nih.gov/books/NBK282/[↩]