Contents
- What is colon pain?
- Colon pain causes
- How is the cause of colon pain diagnosed?
- How is colon pain treated?
- Constipation
- What is fecal impaction?
- What is intestinal obstruction?
- What is chronic constipation?
- Constipation causes
- Risk factors for constipation
- Constipation prevention
- Constipation signs and symptoms
- Constipation complications
- Constipation diagnosis
- Constipation treatment
- Home remedies for constipation
- Increase your dietary fiber intake
- Exercise
- Don’t ignore the urge to have a bowel movement
- Stress management
- Table 1. Putting positive thinking into practice
- Types of laxatives
- How laxatives relieve constipation
- Table 2. Laxatives for Chronic Constipation
- Prescription medicines
- Training your pelvic muscles
- Surgery
- Alternative medicine
- Irritable bowel syndrome
- Bowel obstruction
- Perforated bowel
- Colon cancer
What is colon pain?
Colon pain is a general term to describe abdominal pain, stomach pain, belly ache, tummy pain, stomach ache, stomach cramps or sore stomach. Colon pain is usually describes as pain or discomfort between your chest and hips, including areas from your mouth to your rectum which includes your esophagus, stomach, small intestine, large intestine, pancreas, liver, gallbladder, kidneys, spleen and other organs in your abdomen. In other words, many different conditions ranging from benign (less serious) to life-threatening conditions can cause abdominal pain. Colon pain can be in different areas of your abdomen and can move or radiate to other areas. Colon pain can be mild or severe. However, how bad your pain is does not always reflect the seriousness of the condition causing the pain. Colon pain may be constant or come and go (recurrent pain). Colon pain can be short-lived also known as acute abdominal pain. It also may occur over weeks, months or years, also known as chronic abdominal pain. Colon pain can feel like cramping, bloating, or constipation pain in your abdomen. Because colon pain is non-specific term to describe anything that can cause abdominal pain, you’ll need to see your doctor right away if you have abdominal pain so severe that you can’t move without causing more pain. Also see your doctor if you can’t sit still or find a comfortable position.
Colon pain may also be accompanied by other symptoms, such as:
- bloating, belching and burping
- loss of appetite
- heartburn
- nausea and vomiting
- a change in bowel habits (doing a poop) including diarrhea or constipation
- problems with urinating (doing a wee)
- fever
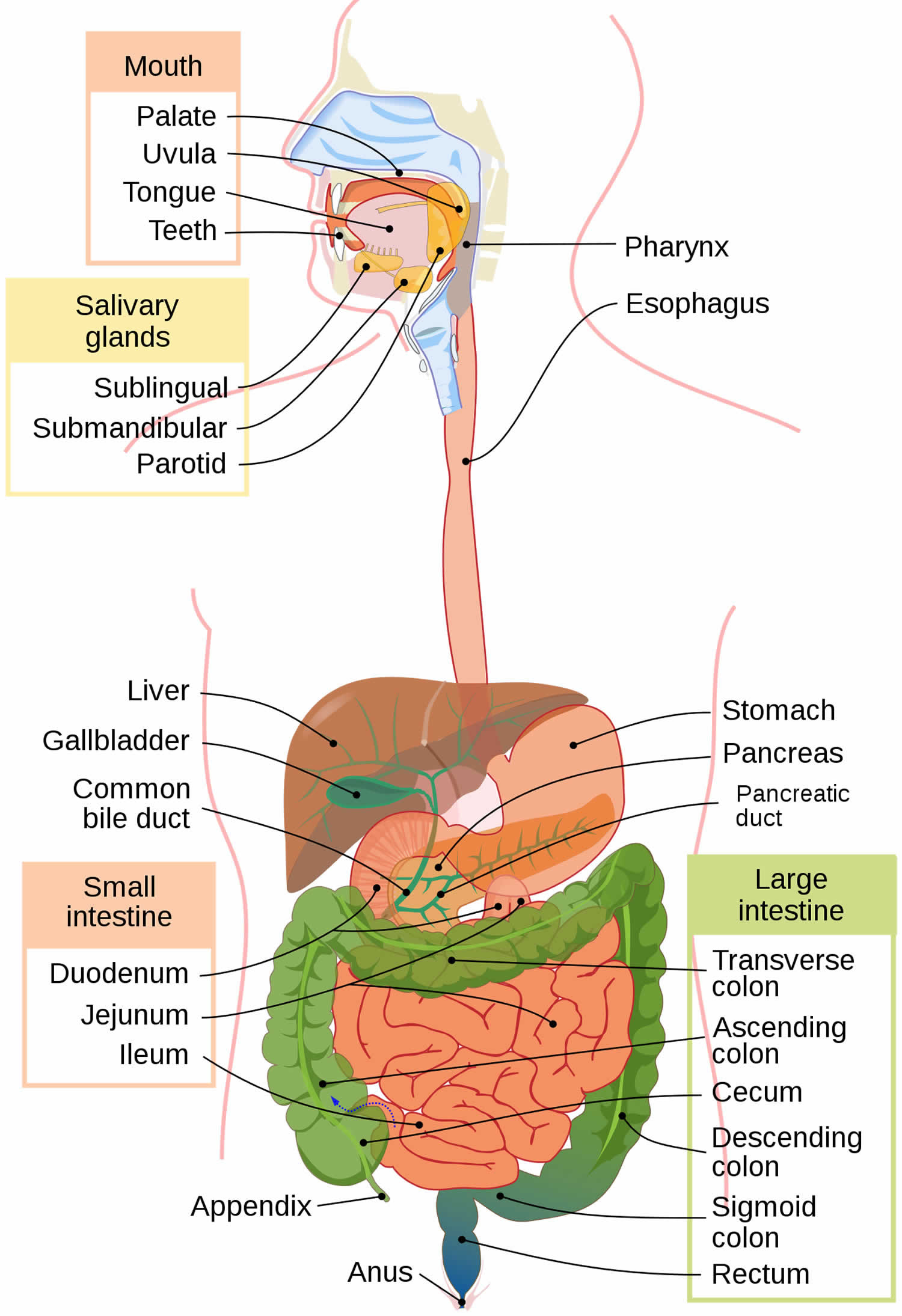
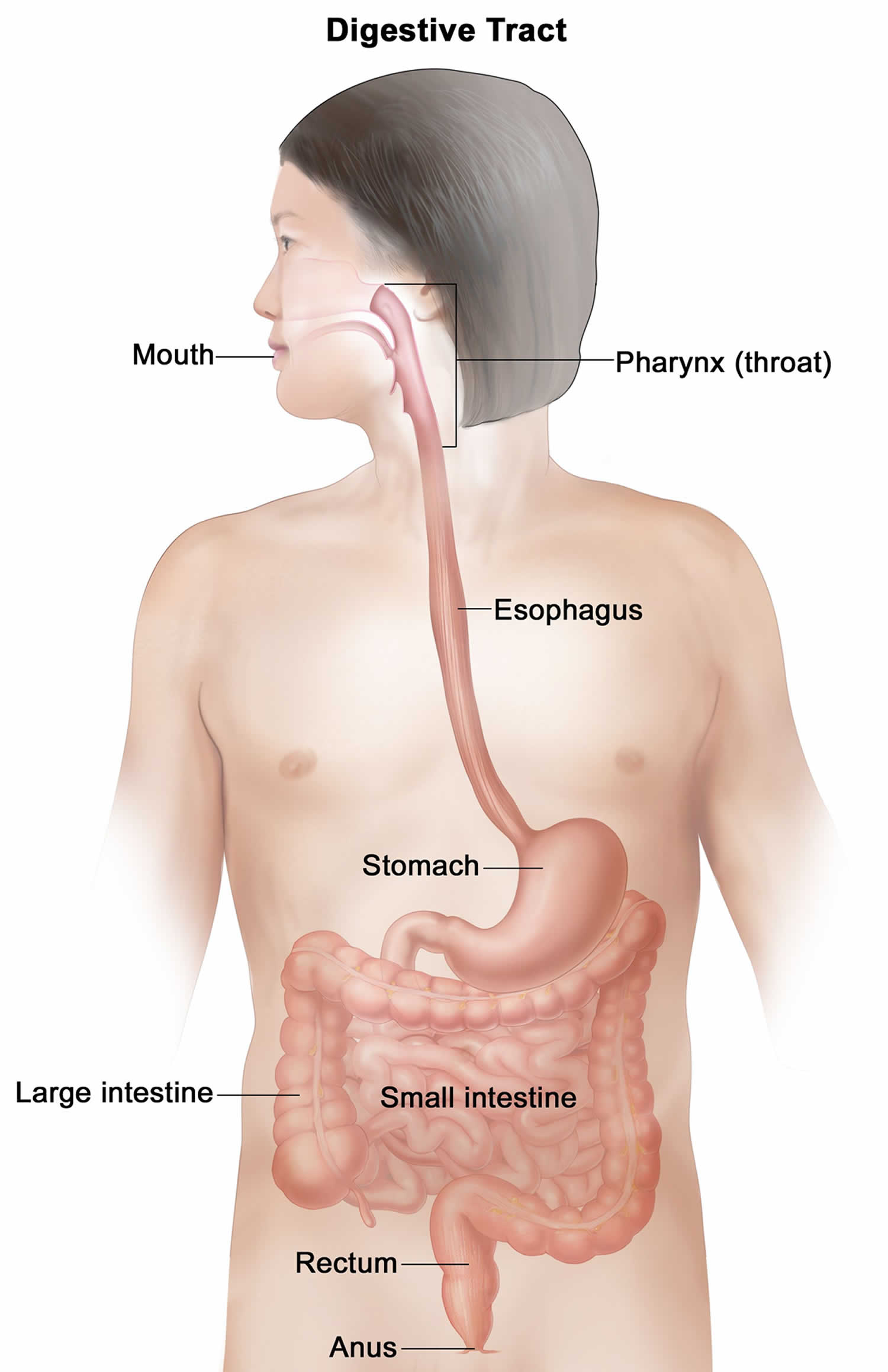
Figure 1. Gastrointestinal tract (human digestive system)
Figure 2. Gastrointestinal tract anatomy
See a doctor or seek immediate medical attention if your abdominal pain is severe and is associated with:
- Recent trauma, such as an accident or injury.
- Difficulty breathing.
- Sudden, sharp abdominal pain.
- Pain in, or between, your shoulder blades with nausea.
- Cancer treatment.
- Pain lasting for several hours.
- Pain and vomiting or shortness of breath.
- Pain and vomiting blood.
- Blood in your bowel motions (especially if bright red, maroon or dark, tarry black)
- Blood in your urine.
- Pain that spreads to your chest, neck or shoulder.
- Fever and sweats.
- Bloody stools.
- Inability to pass stool.
- Persistent nausea and vomiting.
- Weight loss.
- Skin that appears discolored.
- Severe tenderness when you touch your abdomen or your belly is rigid and hard to the touch.
- Swelling of your abdomen.
- You are pregnant or could be pregnant.
Call an ambulance or have someone drive you to the nearest emergency room.
See your doctor if you have:
- Abdominal discomfort that lasts 1 week or longer
- Abdominal pain that does not improve in 24 to 48 hours, or becomes more severe and frequent and occurs with nausea and vomiting
- Bloating that persists for more than 2 days
- Burning sensation when you urinate or frequent urination
- Diarrhea for more than 5 days
- Fever, over 100°F (37.7°C) for adults or 100.4°F (38°C) for children, with pain
- Prolonged poor appetite
- Prolonged vaginal bleeding
- Unexplained weight loss
- Unable to keep down any foods or liquids
Colon pain causes
Colon pain can have many causes ranging from benign (less serious) to life-threatening conditions. The most common causes usually aren’t serious, such as gas pains, indigestion or a pulled abdominal muscle. Other conditions may need urgent medical attention. The location and pattern of your abdominal pain can provide important clues, but how long it lasts is especially useful when figuring out its cause. For example, colon pain that is short-lived develops and often goes away over a few hours to a few days. On the other hand, long term or chronic abdominal pain may come and go over a few weeks to a few months or even years. Some chronic conditions cause progressive pain, which steadily gets worse over time.
Colon pain causes may include:
- Appendicitis
- Abdominal aortic aneurysm (bulging and weakening of the major artery in the body)
- Bowel blockage or obstruction
- Constipation
- Irritable bowel syndrome (IBS)
- Inflammatory bowel disease (IBD)
- Stomach cancer
- Colorectal cancer
- Gastroenteritis – a short-term illness triggered by the infection and inflammation of your digestive system. Some of the causes of gastroenteritis include viruses, bacteria, bacterial toxins, parasites, particular chemicals and some drugs. Symptoms can include abdominal cramps, diarrhea and vomiting.
- Colon spasms
- Stomach ulcer
- Heartburn and acid reflux
- Gastritis (inflammation of the stomach lining)
- Cholecystitis (inflammation of the gallbladder) with or without gallstones
- Decreased blood supply to the intestines (ischemic bowel)
- Diverticulitis (inflammation and infection of the pouches or diverticula in the colon [large intestine])
- Endometriosis – a chronic condition that occurs when tissue similar to the uterine lining grows outside of the uterus. It can cause pain, heavy periods, and infertility.
- Heartburn, indigestion, or gastroesophageal reflux disease (GERD)
- Hernia – a hernia is a bulge or lump that occurs when an organ or tissue pushes through a weakened area in the abdominal wall. Hernias can occur in the groin, abdomen, or other areas.
- Inflammatory bowel disease (Crohn disease or ulcerative colitis)
- Kidney stones
- Muscle strain
- Pancreatitis (inflammation or infection of the pancreas)
- Pelvic inflammatory disease (PID)
- Ruptured ovarian cyst
- Severe menstrual cramps
- Ectopic pregnancy
- Stomach ulcers
- Urinary tract infection (UTI)
Less serious causes of abdominal pain include:
- Constipation
- Irritable bowel syndrome (IBS)
- Food allergies or food intolerance such as lactose intolerance
- Food poisoning
- Stomach flu
Acute colon pain
Conditions that cause acute abdominal pain usually happen at the same time as other symptoms that develop over hours to days. Causes can range from minor conditions that go away without any treatment to serious medical emergencies, including:
- Abdominal aortic aneurysm (AAA)
- Appendicitis is when the appendix becomes inflamed and infected.
- Cholangitis, which is inflammation of the bile duct.
- Cholecystitis, which is inflammation of the gallbladder.
- Cystitis (irritation of the urine bladder)
- Diabetic ketoacidosis (in which the body has high levels of blood acids called ketones)
- Diverticulitis which is inflamed or infected pouches (diverticula) in the tissue lining the large intestines.
- Duodenitis, which is inflammation of the duodenum, the first part of the small intestine.
- Ectopic pregnancy occurs when the fertilized egg implants and grows outside of the uterus, such as in a fallopian tube.
- Fecal impaction, which is hardened stool that can’t be passed.
- Heart attack, also known as a myocardial infarction (MI), occurs when blood flow to the heart is reduced or stopped. This can happen when a coronary artery becomes blocked by a buildup of plaque.
- Abdominal injury
- Intestinal obstruction — when something blocks food or liquid from moving through the small or large intestine.
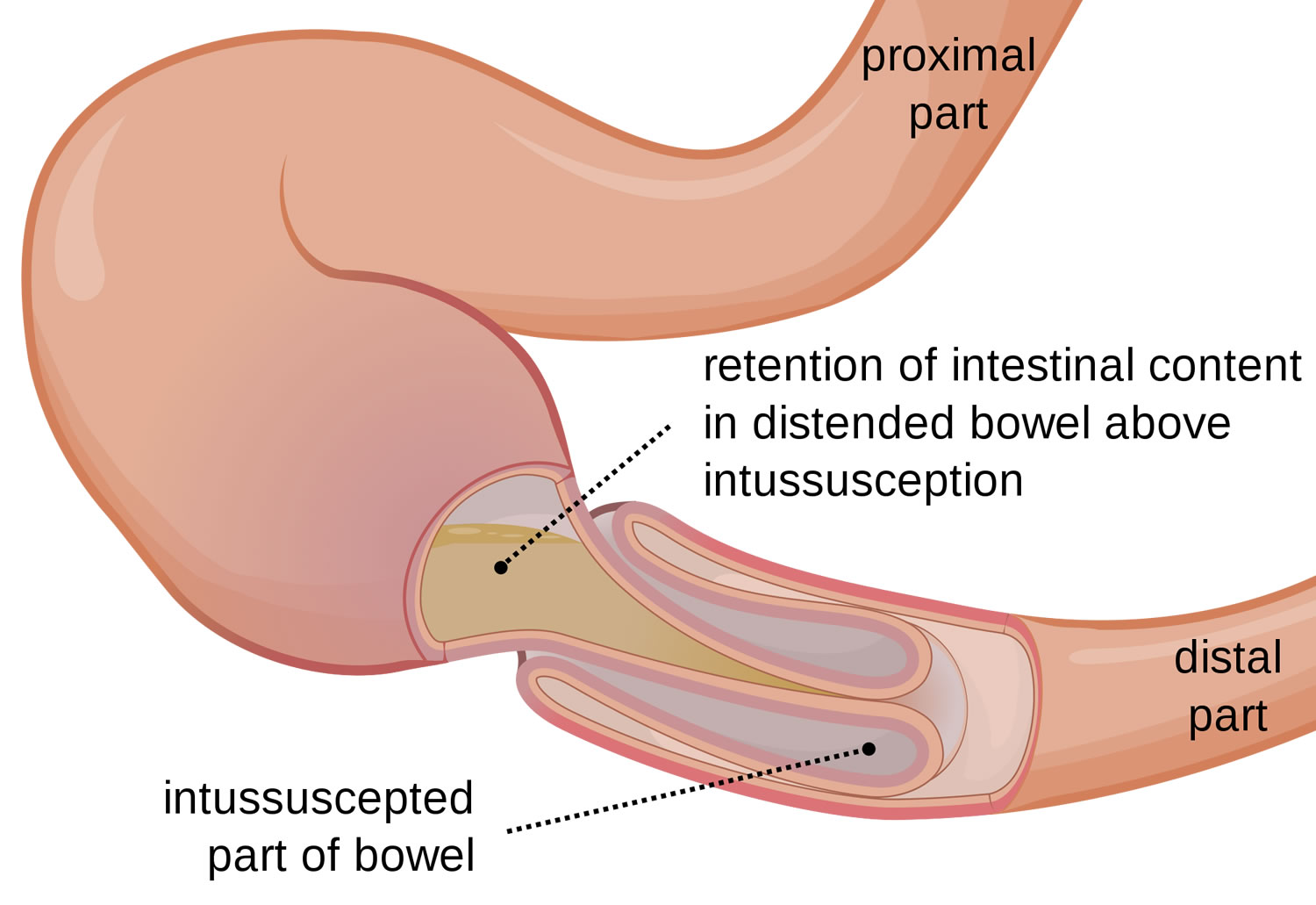
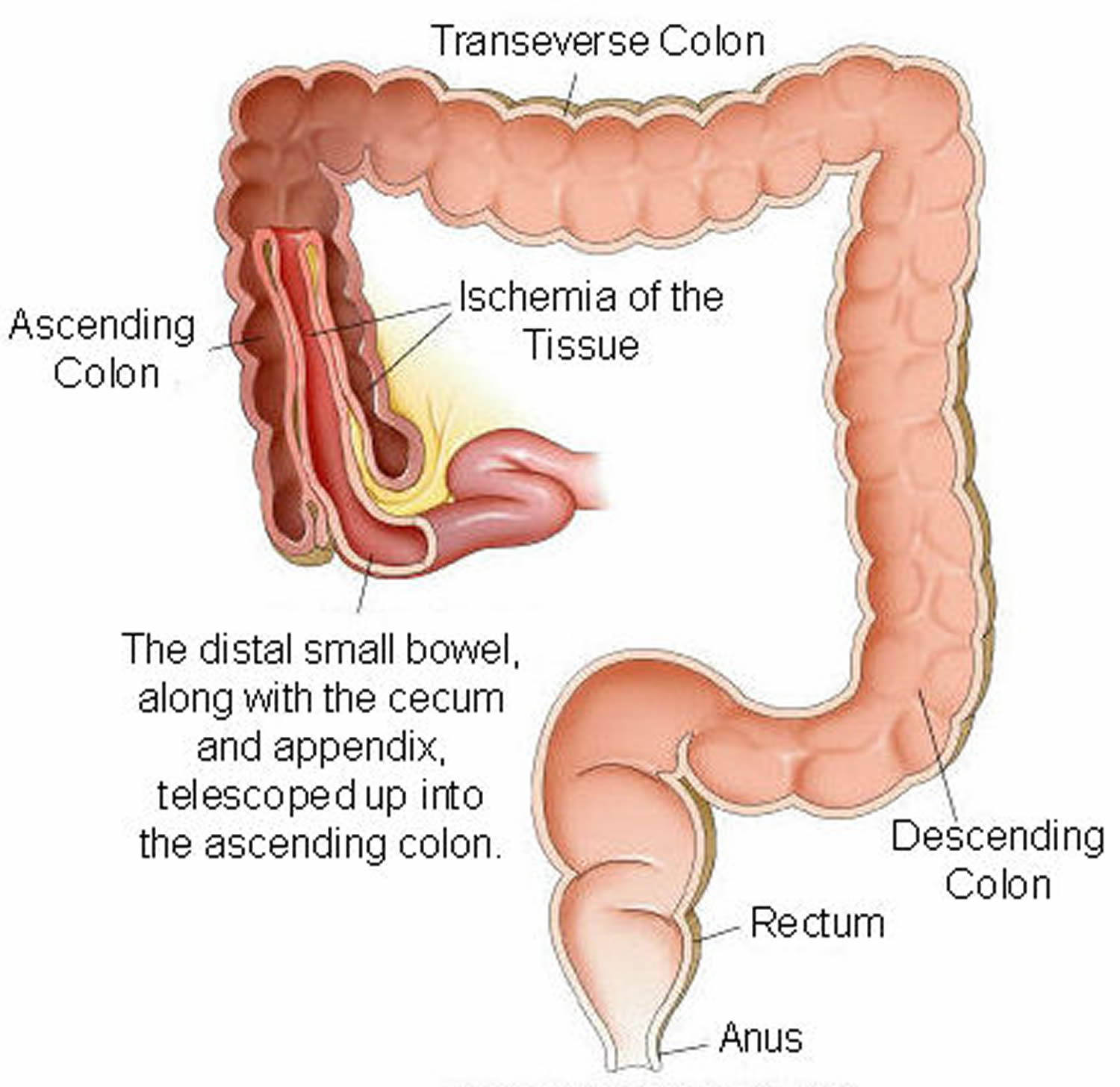
- Intussusception (in children), a life-threatening condition that occurs when part of the intestine folds into another part, blocking food and blood flow. It’s the most common cause of intestinal obstruction in children between the ages of three months and six years.
- Kidney infection, also called pyelonephritis, is a bacterial infection that causes inflammation of the kidney. It’s a type of urinary tract infection (UTI) that usually starts in your urine bladder and spreads to your kidneys.
- Kidney stones also called renal calculi, nephrolithiasis or urolithiasis are hard buildups of minerals and salt that form inside your kidneys.
- Liver abscess also called hepatic abscess is a pus-filled mass in your liver that can be caused by bacteria, parasites, or fungi.
- Mesenteric ischemia is a condition that occurs when blood flow to the intestines is reduced or blocked. It can be acute or chronic.
- Mesenteric lymphadenitis also known as mesenteric adenitis, is swelling of the lymph nodes in your abdomen. It’s a common cause of abdominal pain in children and young adults.
- Mesenteric thrombosis, a blood clot in a vein carrying blood away from your intestines.
- Pancreatitis is inflammation of your pancreas, a large organ that produces digestive enzymes and hormones. Pancreatitis can be acute pancreatitis (sudden and severe pancreatitis) or chronic pancreatitis (ongoing pancreatitis).
- Pericarditis is inflammation of the pericardium, the sac that surrounds the heart. Symptoms include chest pain, shortness of breath, and palpitations.
- Peritonitis is inflammation of the lining of your belly or abdomen called the peritoneum. It is often caused by an infection from a hole in the bowel or a burst appendix.
- Pleurisy is inflammation of the tissue that surrounds your lungs and lines your chest cavity. It can cause sharp chest pain, especially when breathing, coughing, or sneezing.
- Pneumonia is a lung infection that can be caused by bacteria, viruses, or fungi. It can range from mild to life-threatening.
- Pulmonary infarction is a condition that occurs when lung tissue dies due to a lack of blood supply. It’s usually caused by a pulmonary embolism (PE), which is a blood clot that blocks an artery in the lung.
- Ruptured spleen also called broken spleen is a medical emergency that occurs when the spleen bursts or tears. It can cause life-threatening internal bleeding.
- Salpingitis is an inflammation of the fallopian tubes caused by a bacterial infection. It’s a type of pelvic inflammatory disease (PID)
- Sclerosing mesenteritis is a rare disease that causes inflammation and scarring in the small intestine. Sclerosing mesenteritis can cause abdominal pain, bloating, nausea, vomiting, diarrhea, fever and weight loss.
- Shingles is a painful rash caused by the varicella-zoster virus (VZV), the same virus that causes chickenpox. It usually appears on one side of the body, often on the chest or abdomen.
- Spleen infections – spleen infections can occur due to a number of bacterial, viral, and parasitic infections. People with a non-functioning spleen or spleen disorders are at an increased risk of infection
- Splenic abscess is a pus-filled pocket in your spleen. Splenic abscess can be life-threatening if not treated promptly. It’s usually caused by bacteria, such as staphylococci, streptococci, salmonella, or E. coli
- Perforated bowel also known as torn colon or perforated intestine, is a hole in your colon (large intestine) that can be life-threatening. Symptoms include severe abdominal pain or cramping, bloating or a swollen abdomen, fever or chills, nausea and vomiting, and pain or tenderness when you touch your abdomen.
- Urinary tract infection (UTI) is a common bacterial infection that occurs when bacteria enter your urinary tract. Symptoms include a burning sensation when urinating, frequent urination, and pain in the lower abdomen or back.
- Viral gastroenteritis (stomach flu), is a common infection of your stomach and intestines that causes vomiting and diarrhea. It’s usually a mild illness that lasts a few days.
Progressive colon pain
Abdominal pain that steadily worsens over time is usually serious. Abdominal pain that steadily worsens over time often leads to the development of other symptoms.
Progressive abdominal pain causes include:
- Esophageal cancer
- Crohn’s disease — a chronic inflammatory bowel disease (IBD) that causes inflammation in your digestive tract. It’s an autoimmune disorder, which means the body’s immune system attacks healthy tissue.
- Enlarged spleen (splenomegaly)
- Gallbladder cancer
- Hepatitis – is a liver inflammation that can be caused by viruses, chemicals, drugs, alcohol, or autoimmune conditions. Hepatitis can be acute, meaning it flares up and then goes away, or chronic, meaning it’s a long-term condition.
- Kidney cancer
- Lead poisoning
- Liver cancer
- Non-Hodgkin lymphoma (NHL) – non-Hodgkin lymphoma (NHL) is a type of cancer that affects the lymphatic system. It’s a group of blood cancers that includes all lymphomas except Hodgkin lymphomas.
- Pancreatic cancer
- Stomach cancer
- Tubo-ovarian abscess is a pus-filled pocket involving a fallopian tube and an ovary and can be life-threatening.
- Uremia is buildup of waste products in your blood caused by kidney failure and can be life-threatening if left untreated.
Chronic colon pain
Chronic abdominal pain or long term abdominal pain may come and go over a few weeks to a few months or even years. The specific cause of chronic abdominal pain is often difficult to determine. Symptoms may range from mild to severe, coming and going but not necessarily getting worse over time.
Conditions that may cause chronic abdominal pain include:.
- Angina also called angina pectoris is chest pain or discomfort that occurs when the heart muscle doesn’t receive enough oxygen and blood. It’s a symptom of coronary artery disease, which is caused by a buildup of plaque in the heart’s coronary arteries.
- Celiac disease is a chronic digestive disease that damages the small intestine and prevents the body from absorbing nutrients. It’s caused by an immune system reaction to gluten, a protein found in wheat, rye, barley, and some oats.
- Endometriosis is a chronic condition that occurs when tissue similar to the uterine lining grows outside of the uterus. It can cause pain, heavy periods, and infertility.
- Functional dyspepsia also known as nonulcer dyspepsia is a chronic condition that causes pain or discomfort in your upper abdomen.
- Gallstones also called cholelithiasis are hardened deposits of cholesterol, bile salts, and calcium salts that form in your gallbladder. They can range in size from a grain of sand to a golf ball
- Gastritis is inflammation of your stomach lining. Causes include infection, injury, regular use of pain pills called non-steroidal anti-inflammatory drugs (NSAIDs) and too much alcohol.
- Gastroesophageal reflux disease (GERD) is a chronic condition that occurs when stomach contents flow into the esophagus. It can cause heartburn, chest pain, and difficulty swallowing.
- Hiatal hernia – a hiatal hernia occurs when part of your stomach pushes up into your chest through the diaphragm. This can cause heartburn, chest pain, and other symptoms.
- Inguinal hernia also known as a groin hernia, occurs when tissue from the abdomen bulges through a weak spot in the muscles of your lower abdominal wall and can descend into your scrotum. This creates a bulge or lump in the groin area.
- Irritable bowel syndrome (IBS) is a common digestive condition that causes abdominal pain and changes in your bowel movements.
- Mittelschmerz also called ovulation pain, is pain that occurs in your lower abdomen during ovulation. It can feel sharp or dull, and usually affects one side of the body. Mittelschmerz can last from minutes to several days.
- Ovarian cysts are fluid-filled sacs that form in or on your ovaries and aren’t cancer.
- Pelvic inflammatory disease (PID) is a bacterial infection of the female reproductive system. It can affect the uterus, fallopian tubes, and ovaries.
- Peptic ulcer is a sore in your stomach or duodenum (the first part of the small intestine).
- Sickle cell anemia is a blood disorder that causes red blood cells to become misshapen and break down more quickly than normal. This can lead to anemia, pain crises, infections, and organ damage.
- Strained or pulled abdominal muscle.
- Ulcerative colitis (UC) is a chronic inflammatory bowel disease (IBD) that causes ulcers and inflammation in your colon (large intestine) and rectum. It’s the most common type of inflammatory bowel disease (IBD).
How is the cause of colon pain diagnosed?
Abdominal pain is a common symptom. Your doctor will ask you about your pain and any other symptoms you have. Your doctor will also consider your past medical history, age, sex, recent travel and medicines you are taking when working out the cause of your pain. Your doctor will also do a physical examination.
Your doctor may suggest you have tests, such as:
- Blood tests
- Urine tests
- Stool tests
- An ultrasound scan, x-ray, CT scan or MRI scan of your abdomen
- Endoscopy or colonoscopy — where a long, flexible tube with a camera is used to examine your stomach or bowel while you are under sedation
- Electrocardiogram (ECG)
Your doctor may refer you to a specialist doctor for some tests and treatments.
How is colon pain treated?
The treatment of abdominal pain will depend on its underlying cause.
Some conditions can benefit from dietary changes. But always check with your doctor or dietitian before making major changes to your diet.
In some cases, such as appendicitis or bowel obstruction, you may need emergency surgery.
Some lifestyle measures can help keep you and your gut healthy. These include:
- Eating enough fiber, including from fruit and vegetables.
- Eat a well-balanced diet to give yourself the key nutrients your body needs to strengthen your immune system and give you energy.
- Getting regular physical activity.
- Drinking plenty of plain water.
- Limiting how much alcohol you drink.
Following a specific diet can help reduce abdominal pain due to some conditions, such as lactose intolerance or celiac disease. But always ask your doctor or dietitian before restricting foods from your diet.
Constipation
Constipation is when you have infrequent bowel movements or your stool may be hard, dry and difficult to pass. Constipation could also mean that you have 3 or fewer bowel movements in a week. The American College of Gastroenterology defines constipation based upon symptoms including unsatisfactory defecation with either infrequent stools, difficulty in passing stool or both 1. But if there is a new change in bowel habits, people should consult with their doctor 2. You may also have stomach pain, stomach cramps, bloating, and nausea when you are constipated 3. A bowel movement occurs when the food you eat passes through your digestive system. Your body takes the nutrients it needs from that food. What’s left over is called stool or feces. Your stool can be soft or hard. Bowel movements usually happen on a regular basis.
Constipation is a condition in which you typically have 4:
- Fewer than 3 bowel movements a week,
- Bowel movements with stools that are hard, dry, and small, making them painful or difficult to pass.
Symptoms of constipation:
- Feeling like you still need to have a bowel movement, even after you’ve had one.
- Feeling like your intestines or rectum (bottom) are blocked.
- Having hard, dry stool that is difficult to pass.
- Having fewer than 3 bowel movements in a week.
- Straining to have a bowel movement.
More serious symptoms of constipation include:
- Constipation that is new and unusual for you.
- You have been constipated for 3 weeks or more despite dietary changes to help.
- You have abdominal (stomach) pain.
- You lose weight without trying.
- You notice blood or white mucous in your stool.
- You cannot pass the stool on your own.
Some people think they are constipated if they don’t have a bowel movement every day. However, people can have different bowel movement patterns (how often, how consistent, and what time of day it occurs). Some people may have three bowel movements a day. Other people may only have three bowel movements a week 5. However, if your bowel movements become less frequent (based on your bowel movement patterns), are hard (and difficult to pass), and you are physically uncomfortable, you may be constipated.
Constipation is the slow movement of feces through your large intestine (bowel or colon) that results in the passage of dry, hard stool. This can result in discomfort or pain 6. The longer the transit time of stool in your large intestine, the greater the fluid absorption and the drier and harder the stool becomes.
People of all ages experience constipation occasionally. It is estimated that in the United States, constipation is one of the most common gastrointestinal (GI) problems affecting about 42 million people 7. About 33 out of 100 adults ages 60 and older have symptoms of constipation 8.
Constipation is common among all ages and populations in the United States, yet certain people are more likely to become constipated, including 9:
- Being dehydrated
- Eating a diet that’s low in fiber
- Getting little or no physical activity
- Having a mental health condition such as depression or an eating disorder
- Women, especially during pregnancy or after giving birth
- Older adults
- Non-Caucasians
- People with lower incomes
- People who just had surgery
- People taking medicines to treat depression or to relieve pain from things such as a broken bone, a pulled tooth, or back pain – certain medications, including sedatives, narcotics, some antidepressants or medications to lower blood pressure.
- People with certain health problems, including functional gastrointestinal disorders
You might become constipated because there is not enough fluid in your digestive system or not enough movement in your large intestine (bowel or colon) where stool is formed and pushed through to be passed from the body. Lack of physical activity, changes in food intake, or poor fluid intake add to the problem. And people who take certain kinds of pain medicine, especially opioids, are more at risk of constipation. Certain people with cancer might have an increased risk for constipation if they have a tumor in the belly or pelvis or get certain types of cancer treatment.
Usually, constipation goes away and is not serious. See your doctor if your constipation is chronic or frequent. Also see your doctor if your bowel habits change. It may be a problem with your diet or another health problem.
Most cases of constipation are easy to treat at home with diet and exercise. However, some cases require doctor recommendations, prescription medicine, or a medical procedure.
Home remedies for constipation includes:
- Eating high fiber diet. Eating a healthy diet with fiber and drinking plenty of fluids (water is the most helpful) can usually clear up constipation. High fiber foods include beans, dried fruits, fresh fruits and vegetables, whole-grain foods (choose brown rice or whole wheat bread instead of white), flaxseed meal, bran and powdered products containing psyllium. For example, 3 cups of popped popcorn has a little more than 3 grams of fiber. One cup of oatmeal has 4 grams of fiber. Adding fiber to each meal and snack will help you reach your goal for the day. Fiber supplements are helpful. Processed foods, such as desserts and sugary drinks, only make constipation worse.
- Men over the age of 50 should get at least 38 grams of fiber per day.
- Women over the age of 50 should get 25 grams per day.
- Children ages 1 to 3 should get 19 grams of fiber per day.
- Children between 4 and 8 years old should get 25 grams per day.
- Girls between 9 and 18 should get 26 grams of fiber each day. Boys of the same age range should get between 31 and 38 grams of fiber per day.
- Drinking plenty of water. Being dehydrated causes your stool to dry out. This makes having a bowel movement more difficult and painful. Most people need to drink at least 8 cups of liquid each day. You may need more based on your treatment, medications you are taking, or other health factors. Drinking warm or hot liquids may also help.
- Don’t ignore the urge to pass stool. When you have the urge to have a bowel movement, don’t hold it in. This causes the stool to build up.
- Exercise. Exercise is helpful in keeping your bowel movements regular. Ask your health care team about exercises that you can do. Most people can do light exercise, even in a bed or chair. Other people choose to walk or ride an exercise bike for 15 to 30 minutes each day.
- Beware of medicines. Certain prescription medicines (especially pain medicines) can slow your digestive system. This causes constipation. Talk to your doctor about how to prepare for this if you need these medicines.
- Try to create a regular schedule for bowel movements, especially after a meal.
- Make sure children who begin to eat solid foods get plenty of fiber in their diets.
- Try to manage stress.
- Bowel training. Teach your children to go to the bathroom when they have to. Holding it can lead to constipation. This also may be necessary for your elderly parents, if you are caring for them.
- Laxatives. This is over-the-counter medicine that helps you have a bowel movement. Laxatives should only be used in rare instances. Do not use them on a regular basis. If you have to use a laxative, bulk-forming laxatives are best (two brands: Metamucil and Benefiber). These work naturally to add bulk and water to your stools so they can pass easily. Bulk-forming laxatives can cause some bloating (when your stomach feels full) and gas.
Doctor recommended treatments for constipation:
- Mineral oil. Do not use this without your doctor’s recommendation. Your doctor may recommend using it if you recently had surgery and should not strain for a bowel movement. Do not use it regularly. It causes your body to lose important vitamins: A, D, E and K.
- Enema. This is a liquid medicine. It is inserted into your anus to help with constipation. It is often used after a surgery or before some medical procedures.
- Prescription medicine. Your doctor will prescribe a medicine based on the reason for your constipation.
- Medical procedures. This is done to help remove stool from the intestine.
- Surgery. This is rare. It might involve removing a damaged intestine for serious reasons.
What is fecal impaction?
A fecal impaction also known as stool impaction, is a large lump of dry, hard stool that stays stuck in the rectum. Fecal impaction is defined as a large mass of compacted feces at any intestinal level that cannot be evacuated spontaneously 10. Fecal impaction occurs because of hardened fecal matter retained in the large bowel which cannot be evacuated by regular peristaltic activity. Patients with fecal impaction often give a history of inability to evacuate stools spontaneously and complain of total constipation. In most instances, an associated history of progressive abdominal distension with increasing abdominal discomfort or pain is present. Occasionally, patients may also present with a spurious or overflow diarrhea. If fecal impaction is not recognized and treated early, it can give rise to the formation of fecoliths or stone-like feces. Fecal impaction can be life-threatening, patient with a fecal impaction may present with circulatory, cardiac, or respiratory symptoms rather than with gastrointestinal symptoms 11. If the fecal impaction is not recognized, the signs and symptoms may progress and resulting in death 12.
Fecal impaction is most often seen in people who are constipated for a long time (chronic constipation). Constipation is when you are not passing stool as often or as easily as is normal for you. Your stool becomes hard and dry. This makes it difficult to pass.
Fecal impaction commonly occurs among elderly individuals and other at-risk groups, such as children and patients with a neuro-psychiatric disease 13, rarely presenting as an acute emergency to a hospital. Severe constipation is a significant problem that affects almost 70% of elderly people who are under care in nursing homes 14. Among those affected, about 7% will have the condition detected during a digital rectal examination. Fecal impaction is more common among older women who are in institutional care and have associated neuropsychiatric disorders. It is a cause for increased morbidity among the elderly, and if allowed to progress, this can lead to complications causing mortality in the older age group 15.
Fecal impaction is a cause for increased morbidity and a significant cause of a decrease in quality of life among the elderly 16.
Physical examination findings often reveal a distended abdomen. In thinly built or emaciated individuals, hard fecal mass masses may be palpable along the colon. The diagnosis of fecal impaction is primarily based on clinical signs. A detailed history of bowel habits and a full physical examination which includes a digital rectal exam is mandatory.
Treatment for fecal impaction starts with removal of the impacted stool. After that, steps are taken to prevent future fecal impactions.
A warm mineral oil enema is often used to soften and lubricate the stool. However, enemas alone are not enough to remove a large, hardened impaction in most cases.
The fecal mass may have to be broken up by hand. This is called manual removal:
- Your doctor or nurse will need to insert one or two fingers into the rectum and slowly break up the mass into smaller pieces so that it can come out.
- This process must be done in small steps to avoid causing injury to the rectum.
- Suppositories inserted into the rectum may be given between attempts to help clear the stool.
Surgery is rarely needed to treat a fecal impaction. An overly widened colon (megacolon) or complete blockage of the bowel may require emergency removal of the impaction.
Most people who have had a fecal impaction will need a bowel retraining program. Your doctor and a specially trained nurse or therapist will:
- Take a detailed history of your diet, bowel patterns, laxative use, medicines, and medical problems
- Examine you carefully.
- Recommend changes in your diet, how to use laxatives and stool softeners, special exercises, lifestyle changes, and other special techniques to retrain your bowel.
- Follow you closely to make sure the program works for you.
What is intestinal obstruction?
Unlike constipation or fecal impaction, an intestinal obstruction is a partial or complete blockage of the bowel lumen by a process other than fecal impaction. Intestinal obstructions can be classified by the following three means:
- The type of obstruction.
- The obstructing mechanism.
- The part of the bowel involved.
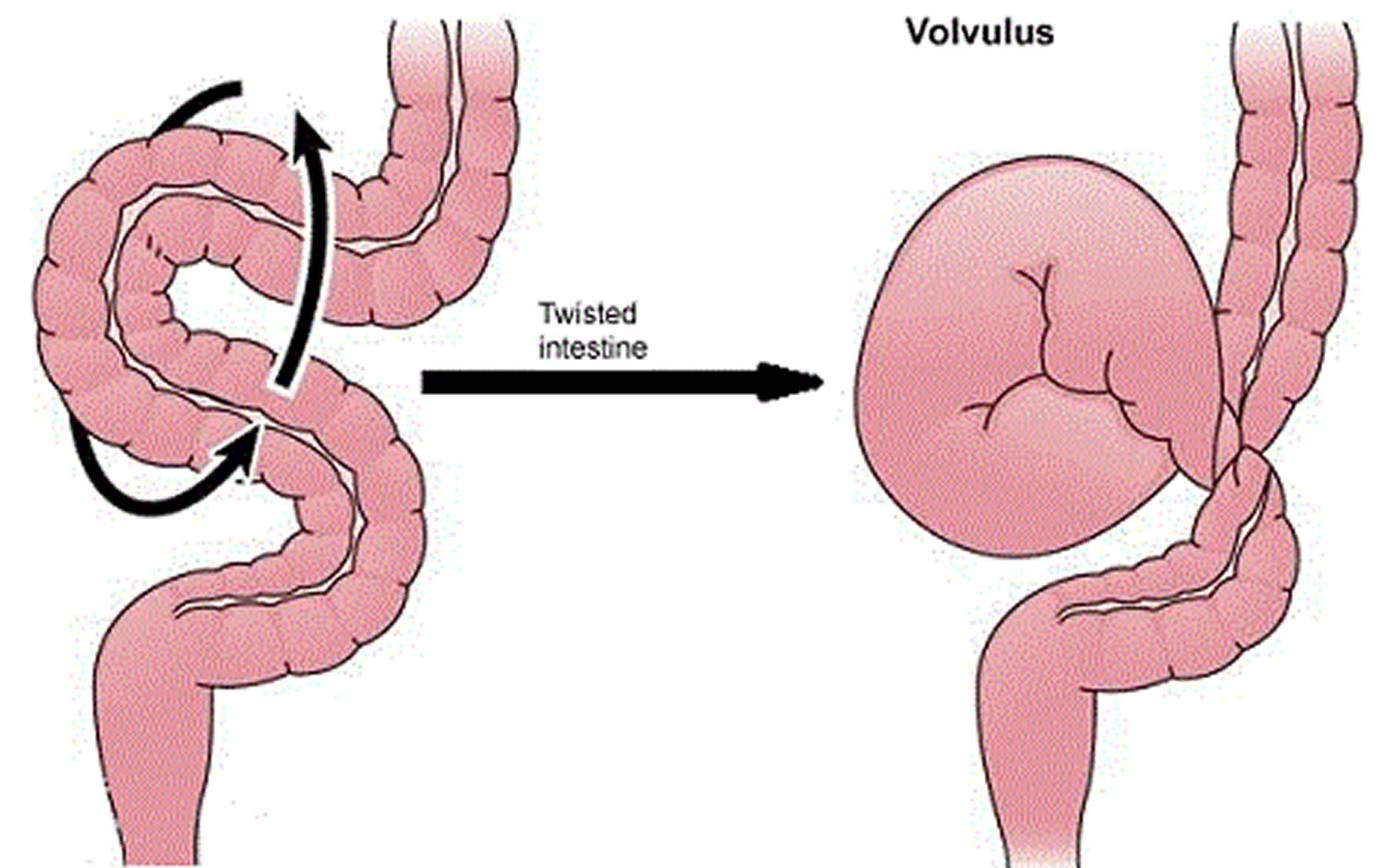
Structural disorders, such as intraluminal and extraluminal bowel lesions caused by primary or metastatic tumor, postoperative adhesions, volvulus of the bowel, or incarcerated hernia, affect peristalsis and the maintenance of normal bowel function. These disorders can lead to total or partial obstruction of the bowel.
Patients who have colostomies are at special risk of developing constipation. If stool is not passed on a regular basis (once a day to several times a day), further investigation is warranted. A partial or complete blockage may have occurred, particularly if no flatus has been passed 17.
What is chronic constipation?
Constipation most often lasts for only a short time (hours to days) and is not dangerous. You can take steps to prevent or relieve constipation.
However with chronic constipation, the infrequent bowel movements or difficult passage of stools can persists for several weeks or longer 18.
People who experience chronic constipation often find it can interfere with their ability to go about their daily tasks. Chronic constipation may also cause excessive straining to have a bowel movement and other signs and symptoms.
Treatment for chronic constipation depends in part on the underlying cause. However, in some cases, a cause is never found 18.
Constipation causes
You may be constipated for many reasons and constipation may have more than one cause at a time (multifactorial) 19, 20, 21. Constipation can be caused by your diet (too many processed foods and not enough fiber), certain medicines (opioid medicines given for pain and even too many laxatives, which usually help you have a bowel movement), dehydration (especially not enough water), too little physical activity, intestinal problems, immobility, or physical and social impediments (particularly inconvenient bathroom availability) and major life changes, such as pregnancy. Depression and anxiety caused by cancer treatment or cancer pain can lead to constipation. Constipation becomes more common as you age. Certain diseases and disabilities also can cause constipation. These include multiple sclerosis, stroke, diabetes, hypothyroidism (underactive thyroid) and lupus.
Dehydration (not enough fluids) and dietary changes are the most common causes of constipation in babies. For example, changing from breast milk to cow’s milk or from baby food to solids can cause constipation.
Constipation most commonly occurs when waste or stool moves too slowly through the digestive tract or cannot be eliminated effectively from the rectum, which may cause the stool to become hard and dry. Chronic constipation has many possible causes.
Blockages in the colon or rectum
Blockages in the colon or rectum may slow or stop stool movement. Causes include:
- Tiny tears in the skin around the anus (anal fissure)
- A blockage in the intestines (bowel obstruction)
- Colon cancer
- Narrowing of the colon (bowel stricture)
- Other abdominal cancer that presses on the colon
- Rectal cancer
- Rectum bulge through the back wall of the vagina (rectocele)
Problems with the nerves around the colon and rectum
Neurological problems can affect the nerves that cause muscles in the colon and rectum to contract and move stool through the intestines. Causes include:
- Damage to the nerves that control bodily functions (autonomic neuropathy)
- Multiple sclerosis
- Parkinson’s disease
- Spinal cord injury
- Stroke.
Difficulty with the muscles involved in elimination
Problems with the pelvic muscles involved in having a bowel movement may cause chronic constipation. These problems may include:
- Inability to relax the pelvic muscles to allow for a bowel movement (anismus)
- Pelvic muscles don’t coordinate relaxation and contraction correctly (dyssynergia)
- Weakened pelvic muscles
Conditions that affect hormones in the body
Hormones help balance fluids in your body. Diseases and conditions that upset the balance of hormones may lead to constipation, including:
- Diabetes
- Overactive parathyroid gland (hyperparathyroidism)
- Pregnancy
- Underactive thyroid (hypothyroidism).
Certain medicines and dietary supplements
Medicines and dietary supplements that can make constipation worse include:
- Antacids that contain aluminum and calcium
- Anticholinergics and antispasmodics
- Anticonvulsants—used to prevent seizures
- Calcium channel blockers
- Diuretics (fluid tablets)
- Iron supplements
- Medicines used to treat Parkinson’s disease
- Narcotic pain medicines
- Medicines used to treat depression
Life changes or daily routine changes
Constipation can happen when your life or daily routine changes. For example, your bowel movements can change:
- if you become pregnant
- as you get older
- when you travel
- when you ignore the urge to have a bowel movement
- if you change your medicines
- if you change how much and what you eat
Certain health and nutrition problems
Certain health and nutrition problems can cause constipation:
- not eating enough fiber
- not drinking enough liquids, or dehydration
- not getting enough physical activity
- celiac disease
- disorders that affect your brain and spine, such as Parkinson’s disease
- spinal cord or brain injuries
- conditions that affect your metabolism, such as diabetes
- conditions that affect your hormones, such as hypothyroidism
- inflammation linked to diverticular disease or proctitis
- intestinal obstructions, including anorectal blockage and tumors
- anatomic problems of your digestive tract
Risk factors for constipation
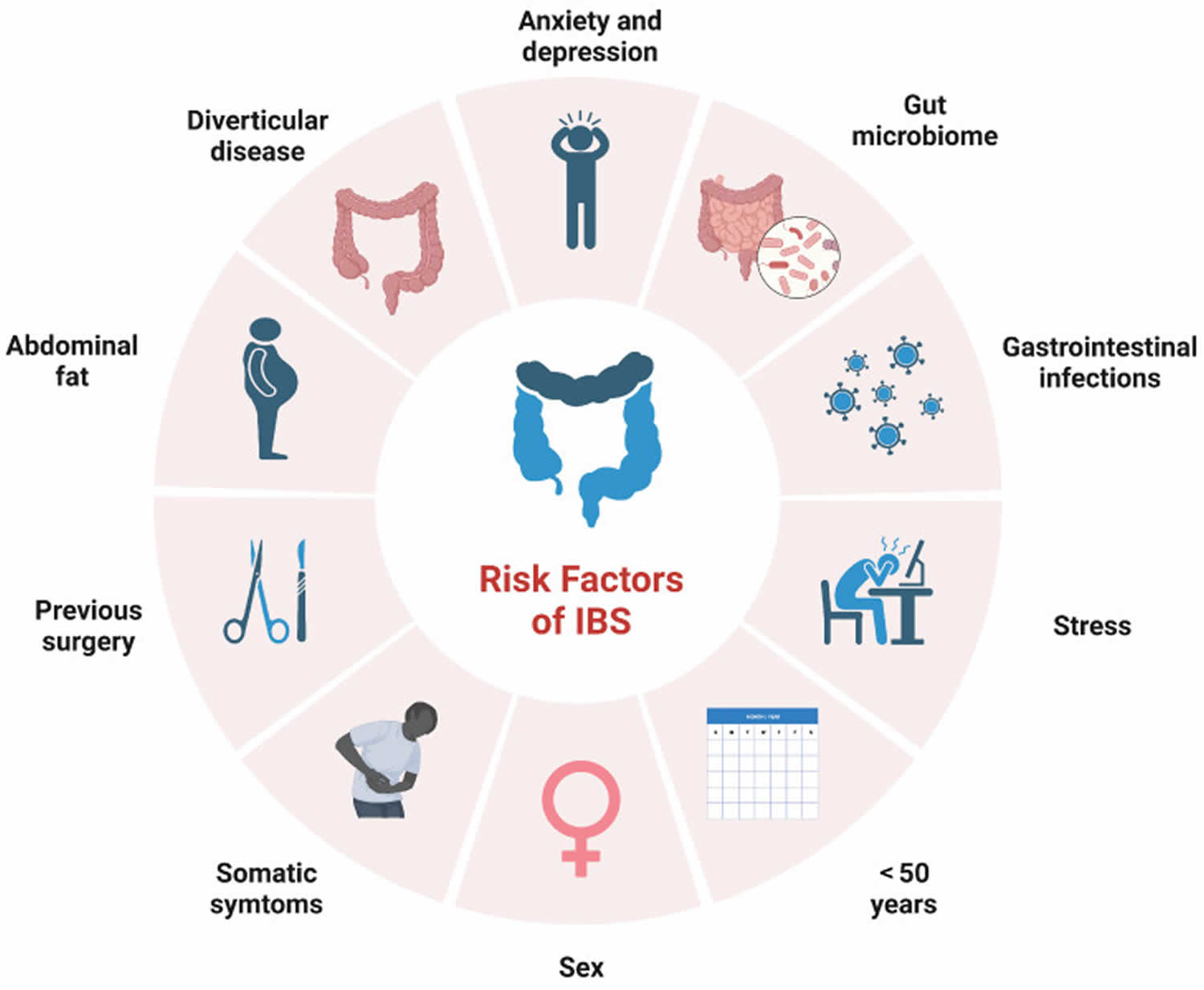
Factors that may increase your risk of chronic constipation include 22, 20, 23, 24:
- Being an older adult
- Being a woman
- Being dehydrated
- Eating a diet that’s low in fiber
- Getting little or no physical activity
- Taking certain medications, including sedatives, opioid pain medications, some antidepressants or medications to lower blood pressure
- Having a mental health condition such as depression or an eating disorder
- Stressful life events
- Physical and sexual abuse
Constipation prevention
There are things you can do to reduce constipation. Take these steps to help you avoid developing chronic constipation:
- Add more fiber to your diet. Adults should eat between 20-35 grams of fiber each day. Foods, such as beans, whole grains, bran, fruits, and vegetables are high in fiber. Adding bran to foods such as cereals or smoothies is an easy way to get more fiber in your diet. If you have had an intestinal obstruction or intestinal surgery, you should not eat a high-fiber diet. Ask your health care team how many grams of fiber you should have each day.
- Eat fewer foods with low amounts of fiber such as processed foods, and dairy and meat products.
- Drink more water. Being dehydrated causes your stool to dry out. This makes having a bowel movement more difficult and painful. Most people need to drink at least 8 cups of liquid each day. You may need more based on your treatment, medications you are taking, or other health factors. Drinking warm or hot liquids may also help.
- Don’t ignore the urge to pass stool. When you have the urge to have a bowel movement, don’t hold it in. This causes the stool to build up.
- Exercise. Exercise is helpful in keeping your bowel movements regular. Ask your health care team about exercises that you can do. Most people can do light exercise, even in a bed or chair. Other people choose to walk or ride an exercise bike for 15 to 30 minutes each day.
- Beware of medicines. Certain prescription medicines (especially pain medicines) can slow your digestive system. This causes constipation. Talk to your doctor about how to prepare for this if you need these medicines.
- Try to create a regular schedule for bowel movements, especially after a meal.
- Make sure children who begin to eat solid foods get plenty of fiber in their diets.
- Try to manage stress.
- See your doctor if you are being treated for certain diseases that are related to constipation. He or she may have additional guidance for lowering your risks.
Constipation signs and symptoms
Signs and symptoms of constipation include:
- Passing fewer than three stools a week or not having regular bowel movements within the past 3 days
- Having lumpy or small hard stools (sometimes described as “pellets”)
- Straining to have bowel movements
- Feeling as though there’s a blockage in your rectum that prevents bowel movements
- Feeling as though you can’t completely empty the stool from your rectum
- Stomachache or cramps
- Passing a lot of gas or frequent belching
- Belly looks blown up or puffy
- Leakage of soft, liquid stool that looks like diarrhea
- Vomiting or nausea
- Needing help to empty your rectum, such as using your hands to press on your abdomen and using a finger to remove stool from your rectum.
Constipation may be considered chronic if you’ve experienced two or more of these symptoms for the last three months.
- When to see a doctor: Make an appointment with your doctor if you experience unexplained and persistent changes in your bowel habits.
- Call your doctor immediately if you have:
- Bloody stools
- Severe cramps or pain
- Weakness or unusual tiredness
- Dizziness
- Rectal bleeding
- Unexplained changes in bowel patterns
- Constipation that lasts longer than seven days despite laxative use.
Constipation complications
Complications of chronic constipation include:
- Anal fissure (a tear in the skin around your anus). A large or hard stool can cause tiny tears in the anus.
- Stool impaction or fecal impaction (when your stool becomes too large to pass on your own). Chronic constipation may cause an accumulation of hardened stool that gets stuck in your intestines.
- Hemorrhoids (swollen veins in your anus). Straining to have a bowel movement may cause swelling in the veins in and around your anus.
- Rectal prolapse (when a small piece of your rectum comes out of your anus from straining to have a bowel movement). Straining to have a bowel movement can cause a small amount of the rectum to stretch and protrude from the anus.
- Encopresis (when your bowels are so backed up that only liquid can pass through). Many people mistake this for diarrhea take anti-diarrheal medicine, making constipation even worse.
Complications of constipation can become serious if left untreated. They may require surgery.
Constipation diagnosis
Doctors use your medical and family history, a physical exam, or medical tests to diagnose and find the cause of your constipation. Your doctor will ask you about your symptoms and medical history. This will include asking you about any medicines you take. Your doctor also will ask when you had your last bowel movement and how often you have them. Think about that before you see your doctor. It might be helpful to write it down for yourself or a child before your appointment. During the visit, your doctor may examine your rectum (the end of your large intestine near your anus), this is called digital rectal exam. During the digital rectal exam, your doctor will insert his or her finger (while wearing rubber gloves) into your rectum to feel for blockages.
Depending on your symptoms and health, your doctor may first try a treatment to improve your symptoms before ordering additional tests and procedures.
Your doctor may order additional tests and procedures, including a blood test and X-ray, to diagnose constipation and try to find the cause. A more thorough test is a colonoscopy. This is an invasive procedure done with anesthesia. During this test, your doctor will examine your colon with a long, flexible scope attached to a camera.
- Blood tests. Your doctor will look for a systemic condition such as low thyroid (hypothyroidism).
- Examination of the rectum and lower, or sigmoid, colon (sigmoidoscopy). In this procedure, your doctor inserts a lighted, flexible tube into your anus to examine your rectum and the lower portion of your colon.
- Examination of the rectum and entire colon (colonoscopy). This diagnostic procedure allows your doctor to examine the entire colon with a flexible, camera-equipped tube.
- Evaluation of anal sphincter muscle function (anorectal manometry). In this procedure, your doctor inserts a narrow, flexible tube into your anus and rectum and then inflates a small balloon at the tip of the tube. The device is then pulled back through the sphincter muscle. This procedure allows your doctor to measure the coordination of the muscles you use to move your bowels 25.
- Evaluation of anal sphincter muscle speed (balloon expulsion test). Often used along with anorectal manometry, this test measures the amount of time it takes for you to push out a balloon that has been filled with water and placed in your rectum 25.
- Evaluation of how well food moves through the colon (colonic transit study). In this procedure, you may swallow a capsule that contains either a radiopaque marker or a wireless recording device. The progress of the capsule through your colon will be recorded over several days and be visible on X-rays. In some cases, you may eat radiocarbon-activated food and a special camera will record its progress (scintigraphy). Your doctor will look for signs of intestinal muscle dysfunction and how well food moves through your colon.
- An X-ray of the rectum during defecation (defecography) 25. During this procedure, your doctor inserts a soft paste made of barium into your rectum. You then pass the barium paste as you would stool. The barium shows up on X-rays and may reveal a prolapse or problems with muscle function and muscle coordination.
- MRI defecography. During this procedure, as in barium defecography, a doctor will insert contrast gel into your rectum. You then pass the gel. The MRI scanner can visualize and assess the function of the defecation muscles. This test also can diagnose problems that can cause constipation, such as rectocele or rectal prolapse 25.
Medical and family history
Your doctor will ask you questions about your medical history, such as:
- whether you have ever had surgery to your digestive tract
- if you have recently lost or gained weight
- if you have a history of anemia
Your doctor also is likely to ask questions about your symptoms, such as:
- How often do you have a bowel movement?
- How long have you had symptoms?
- What do your stools look like?
- Do your stools have red streaks in them?
- Are there streaks of blood on your toilet paper when you wipe?
Your doctor is likely to ask questions about your routines, such as:
- What are your eating habits?
- What is your level of physical activity?
- What medicines, including supplements, and complementary and alternative medicines, do you take?
You may want to track your bowel movements and what your stools look like for several days or weeks before your doctor’s visit. Write down or record the information so you can share it with your doctor.
If you’ve been constipated a long time, your health care professional may ask whether anyone in your family has a history of conditions that may cause long-lasting constipation, such as:
- anatomic problems of the digestive tract
- intestinal obstruction
- diverticular disease
- colon or rectal cancer
Physical exam
During a physical exam, a health care professional may:
- check your blood pressure, temperature, and heart rate
- check for dehydration
- use a stethoscope to listen to sounds in your abdomen
- check your abdomen for:
- swelling
- tenderness or pain
- masses, or lumps
- perform a rectal exam
Lab tests
Your doctor may use one or more of the following lab tests to look for signs of certain diseases and conditions that may be causing your constipation:
- Blood tests can show signs of anemia, hypothyroidism, and celiac disease.
- Stool tests can show the presence of blood and signs of infection and inflammation.
- Urine tests can show signs of diseases such as diabetes.
Endoscopy
Your doctor may perform an endoscopy to look inside your anus, rectum, and colon for signs of problems in your lower digestive tract. Endoscopies for constipation include:
During these two tests, your doctor may also perform a biopsy. A biopsy is a procedure that involves taking small pieces of tissue and examining them under a microscope. A doctor can use a biopsy to look for signs of cancer or other problems.
Colorectal transit studies
Your doctor may use bowel function tests called colorectal transit studies to see how well your stool moves through your colon.
- Radiopaque markers—an x-ray that tracks radioactive markers while they pass through your digestive system. You swallow capsules with the markers, which take about 3 to 7 days to come out with a bowel movement.
- Scintigraphy—a test that involves eating a meal with a small dose of a radioactive substance. Your doctor tracks the substance using special computers and cameras as the substance passes through your intestines.
Other bowel function tests
Your doctor may also use one or more of the following tests to look for signs of certain diseases and conditions that may be causing your constipation:
- Defecography—an x-ray of the area around the anus and rectum to see how well you can hold and release stool
- Anorectal manometry—a test to check how sensitive your rectum is, how well it works, and how well the anal sphincters work
- Balloon expulsion test—a test that involves pushing a small water balloon from your rectum to see if you have a problem pushing out stool
Imaging tests
To look for other problems that may be causing your constipation, your doctor may perform an imaging test such as:
- Lower gastrointestinal (GI) series
- Magnetic resonance imaging (MRI)
- Computed tomography (CT) scan
Constipation treatment
Treatment for constipation depends in part on the underlying cause. Most cases of constipation are easy to treat at home with high fiber diet, plenty of water and exercise. If these changes don’t help, your doctor may recommend prescription medicine, or a medical procedure and rarely surgery.
Home remedies for constipation
Your doctor may recommend the following changes to relieve your constipation:
- Increase your fiber intake. Adding fiber to your diet increases the weight of your stool and speeds its passage through your intestines. Slowly begin to eat more fresh fruits and vegetables each day. Choose whole-grain breads and cereals. Your doctor may recommend a specific number of grams of fiber to consume each day. In general, adults should get 22 to 34 grams of fiber a day 26. A sudden increase in the amount of fiber you eat can cause bloating and gas, so start slowly and work your way up to your goal over a few weeks.
- Talk with a dietitian, to plan meals with the right amount of fiber for you. Be sure to add fiber to your diet a little at a time so your body gets used to the change. Good sources of fiber are:
- whole grains, such as whole wheat bread and pasta, oatmeal, and bran flake cereals
- legumes, such as lentils, black beans, kidney beans, soybeans, and chickpeas
- fruits, such as berries, apples with the skin on, oranges, and pears
- vegetables, such as carrots, broccoli, green peas, and collard greens
- nuts, such as almonds, peanuts, and pecans
- To help prevent or relieve constipation, AVOID foods with little to no fiber, such as:
- chips
- fast food
- meat
- prepared foods, such as some frozen meals and snack foods
- processed foods, such as hot dogs or some microwavable dinners
- Talk with a dietitian, to plan meals with the right amount of fiber for you. Be sure to add fiber to your diet a little at a time so your body gets used to the change. Good sources of fiber are:
- Drink plenty of water and other liquids if you eat more fiber or take a fiber supplement. Water is a good choice. Fruit juice — especially prune juice — also can help.
- Drinking enough water and other liquids is also a good way to avoid dehydration. Staying hydrated is good for your overall health and can help you avoid getting constipated. Ask a health care professional how much liquid you should drink each day based on your size, health, activity level, and where you live.
- Exercise most days of the week. Physical activity increases muscle activity in your intestines. Try to fit in exercise most days of the week. If you do not already exercise, talk to your doctor about whether you are healthy enough to start an exercise program.
- Don’t ignore the urge to have a bowel movement. Take your time in the bathroom, allowing yourself enough time to have a bowel movement without distractions and without feeling rushed.
Increase your dietary fiber intake
Today more than 80 percent of the U.S. population eats less than the recommended amount of vegetables, about 70 percent of the population eats more saturated fat, sodium and added sugar than is recommended. That is because the top three sources of calories in the U.S. are burgers, sandwiches and tacos; followed by desserts, sweet snacks and sugar-sweetened beverages, according to the most recent data from the National Health and Nutrition Examination Survey 27.
Adding fiber to your diet increases the weight of your stool and speeds its passage through your intestines. Slowly begin to eat more fresh fruits and vegetables each day. Choose whole-grain breads and cereals.
Adding fiber to the diet can have some side effects, such as abdominal bloating and/or gas, so start slowly and work your way up to your goal over a few weeks, until stools become softer and more frequent 28.
However, many people, including those with irritable bowel syndrome, cannot tolerate fiber supplements and do better by not increasing fiber in their diet
Your doctor may recommend a specific number of grams of fiber to consume each day. In general, aim for 22 to 34 grams of fiber per day in your daily diet 26.
Exercise
Exercise most days of the week. Physical activity increases muscle activity in your intestines. Try to fit in exercise most days of the week. If you do not already exercise, talk to your doctor about whether you are healthy enough to start an exercise program.
Don’t ignore the urge to have a bowel movement
Take your time in the bathroom, allowing yourself enough time to have a bowel movement without distractions and without feeling rushed.
Stress management
Stress is a normal psychological and physical reaction to the demands of life. A small amount of stress can be good, motivating you to perform well. But multiple challenges daily, such as sitting in traffic, meeting deadlines and paying bills, can push you beyond your ability to cope.
Stress has a way of becoming chronic as the worries of everyday living weigh us down. Or perhaps you’ve become accustomed to stress in your life, and you allow whatever is currently the most stressful problem to dictate what you will do each day. Everyone needs pleasure, productivity and creativity in their lives and chronic stress robs us of these.

Where do you put yourself on this stress chart?
To monitor your stress, first identify your triggers. What makes you feel angry, tense, worried or irritable ? Do you often get headaches or an upset stomach with no medical cause ?
Relaxation techniques are an essential part of stress management. Because of your busy life, relaxation might be low on your priority list. Don’t shortchange yourself. Everyone needs to relax and recharge to repair the toll stress takes on your mind and body.
Almost everyone can benefit from relaxation techniques, which can help slow your breathing and focus your attention. Common relaxation techniques include meditation, progressive muscle relaxation, tai chi and yoga. More-active ways of achieving relaxation include walking outdoors or participating in sports 30.
It doesn’t matter which relaxation technique you choose. Select a technique that works for you and practice it regularly.
Positive thinking helps with stress management also and can even improve your health 31. Practice overcoming negative self-talk with examples provided.
Some studies show that personality traits such as optimism and pessimism can affect many areas of your health and well-being. The positive thinking that usually comes with optimism is a key part of effective stress management. And effective stress management is associated with many health benefits. If you tend to be pessimistic, don’t despair — you can learn positive thinking skills.
Positive thinking doesn’t mean that you keep your head in the sand and ignore life’s less pleasant situations. Positive thinking just means that you approach unpleasantness in a more positive and productive way. You think the best is going to happen, not the worst.
Positive thinking often starts with self-talk. Self-talk is the endless stream of unspoken thoughts that run through your head. These automatic thoughts can be positive or negative. Some of your self-talk comes from logic and reason. Other self-talk may arise from misconceptions that you create because of lack of information.
If the thoughts that run through your head are mostly negative, your outlook on life is more likely pessimistic. If your thoughts are mostly positive, you’re likely an optimist — someone who practices positive thinking.
Researchers continue to explore the effects of positive thinking and optimism on health. Health benefits that positive thinking may provide include:
- Increased life span
- Lower rates of depression
- Lower levels of distress
- Greater resistance to the common cold
- Better psychological and physical well-being
- Better cardiovascular health and reduced risk of death from cardiovascular disease
- Better coping skills during hardships and times of stress.
It’s unclear why people who engage in positive thinking experience these health benefits. One theory is that having a positive outlook enables you to cope better with stressful situations, which reduces the harmful health effects of stress on your body.
It’s also thought that positive and optimistic people tend to live healthier lifestyles — they get more physical activity, follow a healthier diet, and don’t smoke or drink alcohol in excess.
Not sure if your self-talk is positive or negative?
Some common forms of negative self-talk include:
- Filtering. You magnify the negative aspects of a situation and filter out all of the positive ones. For example, you had a great day at work. You completed your tasks ahead of time and were complimented for doing a speedy and thorough job. That evening, you focus only on your plan to do even more tasks and forget about the compliments you received.
- Personalizing. When something bad occurs, you automatically blame yourself. For example, you hear that an evening out with friends is canceled, and you assume that the change in plans is because no one wanted to be around you.
- Catastrophizing. You automatically anticipate the worst. The drive-through coffee shop gets your order wrong and you automatically think that the rest of your day will be a disaster.
- Polarizing. You see things only as either good or bad. There is no middle ground. You feel that you have to be perfect or you’re a total failure.
You can learn to turn negative thinking into positive thinking. The process is simple, but it does take time and practice — you’re creating a new habit, after all. Here are some ways to think and behave in a more positive and optimistic way:
- Identify areas to change. If you want to become more optimistic and engage in more positive thinking, first identify areas of your life that you usually think negatively about, whether it’s work, your daily commute or a relationship. You can start small by focusing on one area to approach in a more positive way.
- Check yourself. Periodically during the day, stop and evaluate what you’re thinking. If you find that your thoughts are mainly negative, try to find a way to put a positive spin on them.
- Be open to humor. Give yourself permission to smile or laugh, especially during difficult times. Seek humor in everyday happenings. When you can laugh at life, you feel less stressed.
- Follow a healthy lifestyle. Aim to exercise for about 30 minutes on most days of the week. You can also break it up into 10-minute chunks of time during the day. Exercise can positively affect mood and reduce stress. Follow a healthy diet to fuel your mind and body. And learn techniques to manage stress.
- Surround yourself with positive people. Make sure those in your life are positive, supportive people you can depend on to give helpful advice and feedback. Negative people may increase your stress level and make you doubt your ability to manage stress in healthy ways.
- Practice positive self-talk. Start by following one simple rule: Don’t say anything to yourself that you wouldn’t say to anyone else. Be gentle and encouraging with yourself. If a negative thought enters your mind, evaluate it rationally and respond with affirmations of what is good about you. Think about things you’re thankful for in your life.
Here are some examples of negative self-talk and how you can apply a positive thinking twist to them:
If you tend to have a negative outlook, don’t expect to become an optimist overnight. But with practice, eventually your self-talk will contain less self-criticism and more self-acceptance. You may also become less critical of the world around you.
When your state of mind is generally optimistic, you’re better able to handle everyday stress in a more constructive way. That ability may contribute to the widely observed health benefits of positive thinking.
Table 1. Putting positive thinking into practice
| Negative self-talk | Positive thinking |
|---|---|
| I’ve never done it before. | It’s an opportunity to learn something new. |
| It’s too complicated. | I’ll tackle it from a different angle. |
| I don’t have the resources. | Necessity is the mother of invention. |
| I’m too lazy to get this done. | I wasn’t able to fit it into my schedule, but I can re-examine some priorities. |
| There’s no way it will work. | I can try to make it work. |
| It’s too radical a change. | Let’s take a chance. |
| No one bothers to communicate with me. | I’ll see if I can open the channels of communication. |
| I’m not going to get any better at this. | I’ll give it another try. |
Types of laxatives
Several types of laxatives exist. Each works somewhat differently to make it easier to have a bowel movement. The following are available over the counter:
- Fiber supplements. Fiber supplements add bulk to your stool. These include psyllium (Metamucil, Konsyl), calcium polycarbophil (FiberCon) and methylcellulose fiber (Citrucel). Taken with plenty of water or fruit juice, they are usually effective in 24 hours, but may take 2-3 days of regular treatment.
- Stimulants. Stimulants including Correctol, bisacodyl (Ducodyl), Dulcolax and senna-sennosides oral (Senokot) cause your intestines to contract. Stimulants are best taken at bedtime. Stimulant laxatives (senna, bisacodyl, cascara) act locally to stimulate the gut, and should be effective in 6-12 hours. These should not be used on a regular basis but are fine for one-off or occasional use.
- Osmotics. Osmotics are laxatives that work by pulling water into the intestines. Examples include oral magnesium hydroxide (Phillips Milk of Magnesia), magnesium citrate, lactulose (Kristalose), polyethylene glycol (Miralax). In addition, polyethylene glycol (PEG) (Golytely, Nulytely) is available by prescription. When taken on an empty stomach, they are effective in 2–48 hours.
- Lubricants. Lubricants such as mineral oil enable stool to move through your colon more easily.
- Stool softeners. Stool softeners such as docusate sodium (Colace) and docusate calcium (Surfak) moisten the stool by drawing water from the intestines. Stool softener laxatives (docusate) are often ineffective unless combined with an osmotic or stimulant laxative.
- Enemas and suppositories. Sodium phosphate (Fleet), soapsuds or tap water enemas can be useful to soften stool and produce a bowel movement. Glycerin or bisacodyl suppositories also can soften stool.
- Products such as liquid paraffin, magnesium salts, suppositories and enemas may be used occasionally to treat fecal impaction, but are not for regular use.
How laxatives relieve constipation
Laxatives work in different ways, and the effectiveness of each laxative type varies from person to person 32. In general, bulk-forming laxatives, also referred to as fiber supplements, are the gentlest on your body and safest to use long term. Metamucil and Citrucel fall into this category.
Oral laxatives may interfere with your body’s absorption of some medications and nutrients. Some laxatives can lead to an electrolyte imbalance, especially after prolonged use. Electrolytes — which include calcium, chloride, potassium, magnesium and sodium — regulate a number of body functions. An electrolyte imbalance can cause abnormal heart rhythms, weakness, confusion and seizures.
Here are some examples of types of laxatives. Even though many laxatives are available over-the-counter, it’s best to talk to your doctor about laxative use and which kind may be best for you.
Table 2. Laxatives for Chronic Constipation
| Type of laxative (brand examples) | How they work | Side effects |
|---|---|---|
| Oral osmotics (Phillips’ Milk of Magnesia, Miralax) | Draw water into the colon to allow easier passage of stool | Bloating, cramping, diarrhea, nausea, gas, increased thirst |
| Oral bulk formers (Benefiber, Citrucel, FiberCon, Metamucil) | Absorb water to form soft, bulky stool, prompting normal contraction of intestinal muscles | Bloating, gas, cramping or increased constipation if not taken with enough water |
| Oral stool softeners (Colace, Surfak) | Add moisture to stool to allow strain-free bowel movements | Electrolyte imbalance with prolonged use |
| Oral stimulants (Dulcolax, Senokot) | Trigger rhythmic contractions of intestinal muscles to eliminate stool | Belching, cramping, diarrhea, nausea, urine discoloration with senna and cascara derivatives |
| Rectal suppositories (Dulcolax, Pedia-Lax) | Trigger rhythmic contractions of intestinal muscles and soften stool | Rectal irritation, diarrhea, cramping |
Footnotes:
- Precautions for pregnant women and children. Don’t give children under age 6 laxatives without a doctor’s recommendation. If you’re pregnant, ask your doctor before using laxatives. Bulk-forming laxatives and stool softeners are generally safe to use during pregnancy, but stimulant laxatives may be harmful.
- If you’ve recently given birth, consult your doctor before using laxatives. Although they’re usually safe to use during breast-feeding, some ingredients may pass into breast milk and cause diarrhea in nursing infants.
Prescription medicines
If over-the-counter laxatives don’t help your chronic constipation, your doctor may recommend a prescription medication, especially if you have irritable bowel syndrome (IBS).
- Medications that draw water into your intestines. A number of prescription medications are available to treat chronic constipation. Lubiprostone (Amitiza), linaclotide (Linzess) and plecanatide (Trulance) work by drawing water into your intestines and speeding up the movement of stool.
- Serotonin 5-hydroxytryptamine 4 receptors. Prucalopride (Motegrity) helps move stool through the colon.
- Peripherally acting mu-opioid receptor antagonists (PAMORAs). If constipation is caused by opioid pain medications, PAMORAs such as naloxegol (Movantik) and methylnaltrexone (Relistor) reverse the effect of opioids on the intestine to keep the bowel moving.
- Other types of medications. Misoprostol (Cytotec), colchicine/probenecid (Col-Probenecid) and onabotulinumtoxinA (also called botulinum toxin type A or Botox) all work in different ways and may be used to treat chronic constipation.
Training your pelvic muscles
During a biofeedback session, a special tube (catheter) to measure muscle tension is inserted into your rectum. The therapist guides you through exercises to alternately relax and tighten your pelvic muscles. A machine will gauge your muscle tension and use sounds or lights to help you understand when you’ve relaxed your muscles.
Surgery
Surgery may be an option if you have tried other treatments and your chronic constipation is caused by a blockage, rectocele or stricture.
For people who have tried other treatments without success and who have abnormally slow movement of stool through the colon, surgical removal of part of the colon may be an option. Surgery to remove the entire colon is rarely necessary.
Alternative medicine
Many people use alternative and complementary medicine to treat constipation, but these approaches have not been well-studied. Using a probiotic such as bifidobacterium or lactobacillus may be helpful, but more studies are needed. Fructooligosaccharide, a sugar that occurs naturally in many fruits and vegetables, may be helpful as well. Researchers currently are evaluating the usefulness of acupuncture.
Irritable bowel syndrome
Irritable bowel syndrome also called IBS is a common, long-term condition that affects the functioning of your large intestine 33, 34, 35, 36, 37, 38, 39, 40, 41, 42, 43. Irritable bowel syndrome (IBS) is a functional disorder of the intestine but is now called disorder of gut–brain interaction (DGBI), because there is no sign of the disease that can be seen or measured, but the large intestine is not functioning normally 44. The main symptoms of irritable bowel syndrome (IBS) are abdominal pain, stomach cramps or discomfort that is often relieved by passing wind or feces, stomach bloating and chronic diarrhea or constipation. Some people go back and forth between diarrhea and constipation 44. In addition, IBS is often associated with other somatic comorbidities such as pain syndromes, overactive bladder and migraine; psychiatric conditions including depression and anxiety and visceral sensitivity 45. Although IBS can cause a great deal of discomfort, it does not harm the intestines.
IBS symptoms vary between individuals and affect some people more severely than others. They tend to come and go in periods lasting a few days to a few months at a time, often during times of stress or after eating certain foods.
These symptoms can be embarrassing, inconvenient and distressing. Fortunately, IBS does not cause permanent damage to your bowel and it does not cause other serious diseases like bowel cancer.
Irritable bowel syndrome (IBS) is common, occurring in about one in five Americans and up to 8–12% of the population worldwide 40, 46, 47, 48. Studies have estimated the prevalence in the United States is somewhere between 15% and 20% of the entire population. IBS is seen in similar frequencies in other countries around the world. Irritable bowel syndrome (IBS) affects about twice as many women as men and is most often found in people younger than 45 years. It usually begins in late adolescence or early adult life between 20 and 30 years of age and rarely appears for the first time after the age of 50.
Based on questionnaire data, women are 1.5 to 3.0 times more likely to have IBS, reflecting a prevalence in women of 14% and in men of 8.9% 45, 46. However, based on healthcare system utilization, women are up to 2 to 2.5 times more likely to see a healthcare provider for their symptoms 49. The reason why women are more commonly affected by irritable bowel syndrome is not completely understood. It does not seem to be merely due to hormonal differences between men and women. Rather it seems to be due to differences in how women and men process sensations from the intestines, both in the intestinal nervous system ( “enteric nervous system”) as well as the brain and spinal cord (“central nervous system”) 50. The frequency of IBS seems to be the same across racial, ethnic and national boundaries.
Despite the fact that irritable bowel syndrome is so common, most people with IBS do not see a doctor for their symptoms 50. It is estimated that only 1 in 4 people with IBS see a doctor (and thus become a patient with IBS). Reasons why some people chose to see a doctor and others do not are not completely understood. Interestingly severity of gastrointestinal symptoms from IBS alone does not seem to be the major driving factor. Rather the impact of IBS on the patient’s ability to function on a day-to-day basis while having IBS symptoms, the stress from having IBS, and concerns about other diseases that they might have are some of the more frequent reasons patients see their doctor for IBS like symptoms.
Studies have shown that that when compared to patients with no medical problems, patients with diabetes, gastroesophageal reflux disease (GERD), as well as individuals who have no gastro intestinal disorders, patients with IBS had significantly higher degrees of impairment in their quality of life. By this is meant their physical functioning, their ability to participate in the activities of daily living, their level of emotional distress, their sexual functioning and all the other components that go into a happy and healthy normal life without disease. This is the true impact of IBS and is an important reason that it deserves serious attention from the medical community. IBS is also a costly disease, not only in terms of money spent for health care but also money lost because patients cannot work while they have symptoms. It is estimated that IBS patients because of their inability to participate in work activities, school activities, etc. lose $30 to $90 billion per year in productivity. After the common cold, IBS is the second most frequent reason people take days off from work in the United States. This makes IBS a very important issue for public health and the society in general, which clearly needs to be addressed by the medical community.
The exact cause of irritable bowel syndrome (IBS) remains incompletely understood, but is probably multifactorial and complex 46. A unifying theme is that the symptoms of IBS result from disordered communication between your gut and your brain, which clinically presents as increased internal organ perception and altered bowel habits 46. Scientific evidence has identified alterations in central (brain) and peripheral (gut) mechanisms in IBS and the bidirectional communication between the brain and the gut. Significant mechanisms linked to IBS include a gut motility disturbance, visceral hypersensitivity, altered mucosal and immune function, altered gut microbiota, and altered central nervous system (brain and spinal cord) processing 46. Other less reproducible mechanisms may include genetic associations, alterations in gastrointestinal microbiota, and disturbances in mucosal and immune function 51.
Irritable bowel syndrome (IBS) is best defined by what it is NOT!
- IBS is NOT an anatomical or structural defect.
- IBS is NOT an identifiable physical or chemical disorder.
- IBS is NOT a cancer and will not cause cancer.
- IBS will NOT cause other gastrointestinal diseases.
Patients suffering from IBS should not be worried about it leading to other serious diseases. The major problem with IBS is not because it causes death or serious disease, but because it changes the quality of life for the patient.
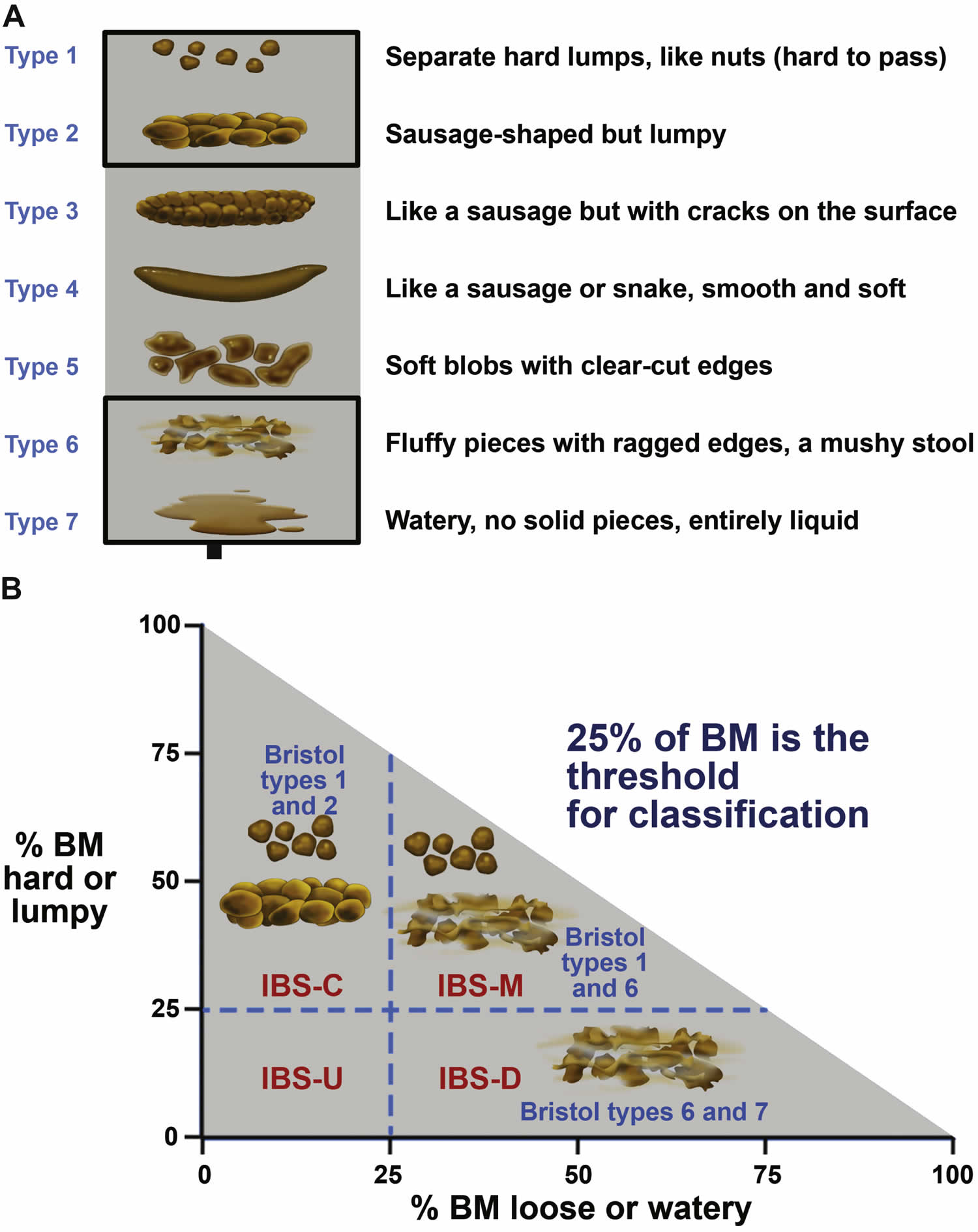
IBS is diagnosed based on symptoms, and a distinction is made between the following subtypes of IBS:
- IBS-D: Diarrhea predominant
- IBS-C: Constipation predominant
- IBS with mixed bowel habits (IBS-M): Alternating, or mixed, between constipation and diarrhea
- IBS-PI: Post Infectious IBS
- PDV-IBS: Post Diverticulitis IBS
- IBS unclassified (IBS-U): Patients who meet diagnostic criteria for IBS but whose bowel habits cannot be accurately categorized into 1 of the 3 groups above should be categorized as having IBS unclassified.
Classifying patients with IBS into specific subtypes based on predominant bowel habits is useful as it helps focus treatment on the predominant, and often, the most bothersome symptom. For clinical trials, or when appropriate in clinical settings, subjects should complete a 14-day bowel diary to most accurately categorize IBS subtypes. Bristol stool types 1 and 2 or types 6 and 7 are considered abnormal 52.
The diagnosis of IBS is based on symptoms ranging from the Manning criteria to the Rome criteria, and the most widely used diagnostic criteria are the Rome IV 53. Rome IV diagnostic criteria defined irritable bowel syndrome (IBS) as a functional bowel disorder in which recurrent abdominal pain is associated with defecation or a change in bowel habits. Disordered bowel habits are typically present (i.e., constipation, diarrhea or a mix of constipation and diarrhea), as are symptoms of abdominal bloating or distension. Symptom onset should occur at least 6 months prior to diagnosis and symptoms should be present during the last 3 months 54.
IBS Rome IV Diagnostic Criteria – recurrent abdominal pain, on average, at least 1 day per week in the last 3 months, associated with 2 or more of the following criteria 54:
- Related to defecation.
- Associated with a change in the frequency of stool.
- Associated with a change in the form (appearance) of stool.
These criteria fulfilled for the last 3 months with symptom onset at least 6 months before diagnosis.
According to Vijayvargiya et al 55, fecal bile acids and fecal fat are potential biomarkers for IBS-D (IBS with diarrhea predominant) and IBS-C (IBS with constipation predominant). Total fecal bile acids, chenodeoxycholic acid, cholic acid, and primary bile acids were significantly higher in patients with IBS-D (IBS with diarrhea predominant) than in healthy patients or patients with IBS-C (IBS with constipation predominant). In contrast, deoxycholic acid and combined deoxycholic acid and chenodeoxycholic acid (secretory) bile acids were significantly lower in patients with IBS-C than in healthy control and patients with IBS-D. Combining fasting serum 7α-hydroxy-4-cholesten-3-one and primary bile acids or fecal bile acid concentrations in stool samples is a simple, low-cost diagnostic for bile acid diarrhea. Circulating resolvin D1 (RvD1) and C-reactive protein (CRP) are inflammatory markers in patients with IBS-C; patients with IBS-C have higher CRP and lower resolvin D1 (RvD1) concentrations than healthy control 56. Furthermore, radiopaque markers and radionuclide scanning can be used to assess transit function, and rectal sensation to balloon distension can be used to assess visceral hypersensitivity 57. All of the ancillary tests listed above can be used to further identify the cause and guide medication use if the first-line medication is ineffective.
Irritable bowel syndrome is not associated with serious medical consequences. People with IBS tend to live long and in some studies, somewhat longer than individuals who do not have IBS. IBS is not associated with other serious GI diseases, such as inflammatory bowel disease (Crohn’s disease or ulcerative colitis) or colon cancer. The presence of IBS does not put extra stress on the other organs in the body such as the heart, liver or kidneys. Overall the prognosis for irritable bowel syndrome is excellent.
A subset of irritable bowel syndrome (IBS) sufferers may have co-morbidities with other digestive health disorders namely; GERD (gastroesophageal reflux disease) / Heartburn, Dyspepsia, Chronic Constipation, Chronic Abdominal Pain, Fibromyalgia, Pelvic pain or perhaps Crohn’s Disease and Ulcerative Colitis, known collectively as Inflammatory Bowel Disease (IBD). For instance, 29% of gastroesophageal reflux disease (GERD) patients have Chronic Constipation. Diagnosis can shift from one motility disorder to another over time; however, co-morbidity in IBS may be due to a general amplification of symptom reporting and physician consultation rather than a direct association.
Doctors may treat irritable bowel syndrome (IBS) by recommending changes in what you eat and other lifestyle changes, medicines, probiotics, and mental health therapies. You may have to try a few treatments to see what works best for you. Your doctor can help you find the right treatment plan. A research study illustrated that patient education in diet, exercise, and stress management showed significant improvement in pain and symptoms at 1 and 6 months of treatment. An educational approach and appropriate use of medications should be components of a physician-based IBS treatment plan.
Who is more likely to develop IBS?
Women are up to two times more likely than men to develop IBS 58. People younger than age 50 are more likely to develop IBS than people older than age 50 59.
Factors that can increase your chance of having IBS include:
- having a family member with IBS
- a history of stressful or difficult life events, such as abuse, in childhood
- having a severe infection in your digestive tract.
What other health problems do people with IBS have?
People with IBS often have other health problems, including 58, 45, 33, 34, 60:
- certain conditions that involve chronic pain, such as fibromyalgia, chronic fatigue syndrome and chronic pelvic pain
- certain digestive diseases, such as dyspepsia and gastroesophageal reflux disease
- certain mental disorders, such as anxiety, depression, and somatic symptom disorder.
Is there a cure for IBS?
At the present time there isn’t a cure for IBS. But, most people manage symptoms by avoiding triggers and taking medications when necessary.
What are there different types of IBS?
According to the Rome IV criteria, there are 4 main types of IBS are based on different patterns of changes in your bowel movements or abnormal bowel movements 61. Sometimes, it is important for your doctor to know which type of IBS you have. Some medicines work only for some types of IBS or make other types worse. Your doctor might diagnose IBS even if your bowel movement pattern does not fit one particular type.
Many people with IBS have normal bowel movements on some days and abnormal bowel movements on other days.
- IBS with constipation (IBS-C). With IBS-C, on days when you have at least one abnormal bowel movement more than a quarter (>25%) of your stools are hard or lumpy and less than a quarter (<25%) of your stools are loose or watery.
- IBS with diarrhea (IBS-D). In IBS-D, on days when you have at least one abnormal bowel movement more than a quarter (>25%) of your stools are loose or watery and less than a quarter (<25%) of your stools are hard or lumpy.
- IBS with mixed bowel habits (IBS-M). In IBS-M, on days when you have at least one abnormal bowel movement more than a quarter (>25%) of your stools are hard or lumpy and more than a quarter (>25%) of your stools are loose or watery.
- IBS unclassified (IBS-U): Patients who meet diagnostic criteria for IBS but whose bowel habits cannot be accurately categorized into 1 of the 3 groups above should be categorized as having IBS unclassified.
Irritable bowel syndrome causes
The exact cause of irritable bowel syndrome is not known. However, tremendous advances in our understanding of this common and disabling disorder have been made in the last 10 years. Abnormal motility in terms of the bowel moving too fast (which causes diarrhea) or too slow (which causes constipation) is certainly part of this syndrome. However, this represents only one part of a complicated disease. The symptoms of pain, incomplete emptying of the bowels, and bloating cannot be blamed only on abnormal gastrointestinal motility. Over the last 20 years a number of very well done scientific studies have demonstrated that individuals with IBS tend to have higher levels of sensitivity in the intestines compared to individuals who do not have IBS.
In the last 10 years, we found and identified certain chemicals present in the intestines, which send signals from nerve endings from the intestines to the brain, and also from the brain to the intestines. These chemicals are called “neuro transmitters” and work as messengers between nerve endings to carry signals in both directions between the brain and gut. This is very important because it has led to the development of new drugs. Some of these drugs are currently available. Others are being developed, as we better understand how these chemical ‘neuro transmitters’ work. One of the major neuro transmitters involved in sensation of pain in the gut as well as playing a key role in motility activity of the gut is serotonin. This chemical also known by its chemical abbreviation 5-HT. However, serotonin is only one of a large number of neuro transmitters that are present in the gut. As scientists identify more and more of these substances and better understand their actions, they may be able to further supplement the arsenal of medications that will influence these neuro transmitters and thus help relieve the symptoms of IBS. Clearly the future is quite bright both for better understanding this perplexing and disabling disorder as well as using this knowledge to make newer and better treatments for IBS.
The precise cause of IBS isn’t known. Certain problems are more common in people with IBS. Experts think these problems may play a role in causing IBS. These problems include 62, 63, 64, 65, 66, 67, 68, 69:
- Muscle contractions in the intestine. The walls of the intestines are lined with layers of muscle that contract as they move food through your digestive tract. Contractions that are stronger and last longer than normal can cause gas, bloating and diarrhea. Weak intestinal contractions can slow food passage and lead to hard, dry stools.
- Nervous system. Abnormalities in the nerves in your digestive system may cause you to experience greater than normal discomfort when your abdomen stretches from gas or stool. Poorly coordinated signals between the brain and the intestines can cause your body to overreact to changes that normally occur in the digestive process, resulting in pain, diarrhea or constipation.
- Inflammation in the intestines. Some people with IBS have an increased number of immune-system cells in their intestines. This immune-system response is associated with pain and diarrhea.
- Severe infection. IBS can develop after a severe bout of diarrhea (gastroenteritis) caused by bacteria or a virus. IBS might also be associated with a surplus of bacteria in the intestines (bacterial overgrowth).
- Changes in bacteria in the gut (microflora). Microflora are the “good” bacteria that reside in the intestines and play a key role in health. Research indicates that microflora in people with IBS might differ from microflora in healthy people.
- Early-life stress. People exposed to stressful events such as physical or sexual abuse, especially in childhood, tend to have more symptoms of IBS.
- Certain mental disorders, such as depression, anxiety, and somatic symptom disorder.
- Food intolerances or food sensitivities, in which certain foods cause digestive symptoms
Research suggests that genes may make some people more likely to develop IBS.
Triggers for Irritable bowel syndrome (IBS)
Symptoms of IBS can be triggered by:
- Food. The role of food allergy or intolerance in IBS isn’t fully understood. A true food allergy rarely causes IBS. But many people have worse IBS symptoms when they eat or drink certain foods or beverages, including wheat, dairy products, citrus fruits, beans, cabbage, milk and carbonated drinks.
- Stress. Most people with IBS experience worse or more frequent signs and symptoms during periods of increased stress. But while stress may aggravate symptoms, it doesn’t cause them.
- Hormones. Women are twice as likely to have IBS, which might indicate that hormonal changes play a role. Many women find that signs and symptoms are worse during or around their menstrual periods.
Risk factors for Irritable bowel syndrome (IBS)
Many people have occasional signs and symptoms of IBS. But you’re more likely to have IBS if you 70, 71, 72:
- Are young. IBS occurs more frequently in people under age 50.
- Are female. In the United States, IBS is more common among women. Estrogen therapy before or after menopause also is a risk factor for IBS.
- Have a family history of IBS. Genes may play a role, as may shared factors in a family’s environment or a combination of genes and environment.
- Have anxiety, depression or other mental health issues. Anxiety, depression and other mental health issues are associated with IBS. A history of sexual, physical or emotional abuse also might be a risk factor.
Figure 3. Risk factors in irritable bowel syndrome (IBS)
Irritable bowel syndrome symptoms
The most common symptoms of irritable bowel syndrome (IBS) are pain in your abdomen, often related to your bowel movements, and changes in your bowel movements. These changes may be diarrhea, constipation, or both, depending on what type of IBS you have.
The signs and symptoms of IBS include:
- Abdominal pain, cramping or bloating that is usually worse after eating and typically relieved or partially relieved by passing a bowel movement
- Excess gas
- Diarrhea or constipation — sometimes alternating bouts of diarrhea and constipation
- Mucus in the stool
IBS symptoms can include:
- sensation of incomplete evacuation
- farting (flatulence)
- passing mucus in the stool
- tiredness and a lack of energy
- feeling sick (nausea)
- backache
- problems peeing, like needing to pee often, sudden urges to pee, and feeling like you cannot fully empty your bladder
- not always being able to control when you poop (bowel incontinence)
Most people with IBS experience times when the signs and symptoms are worse (flare-ups) and times when they improve or even disappear completely.
Women with IBS often have more symptoms during their periods.
The signs and symptoms may be triggered by food or drink such as alcohol, caffeine, certain foods, such as spicy or fatty food, stress and anxiety.
Irritable bowel syndrome (IBS) complications
Chronic constipation or diarrhea can cause hemorrhoids.
In addition, IBS is associated with:
- Poor quality of life. Many people with moderate to severe IBS report poor quality of life. Research indicates that people with IBS miss three times as many days from work as do those without bowel symptoms.
- Mood disorders. Experiencing the signs and symptoms of IBS can lead to depression or anxiety. Depression and anxiety also can make IBS worse.
Irritable bowel syndrome (IBS) Diagnosis
There’s no test to definitively diagnose IBS. Your doctor is likely to start with a complete medical history, physical exam and tests to rule out other conditions. If you have IBS with diarrhea, you likely will be tested for gluten intolerance (celiac disease).
After other conditions have been ruled out, your doctor is likely to use one of these sets of diagnostic criteria for IBS:
- Rome criteria. These criteria include abdominal pain and discomfort lasting on average at least one day a week in the last three months, associated with at least two of these factors: Pain and discomfort are related to defecation, the frequency of defecation is altered, or stool consistency is altered.
- Manning criteria. These criteria focus on pain relieved by passing stool and on having incomplete bowel movements, mucus in the stool and changes in stool consistency. The more symptoms you have, the greater the likelihood of IBS.
- Type of IBS. For the purpose of treatment, IBS can be divided into three types, based on your symptoms: constipation-predominant, diarrhea-predominant or mixed.
Your doctor will also likely assess whether you have other signs or symptoms that might suggest another, more serious, condition. These signs and symptoms include:
- Onset of signs and symptoms after age 50
- Weight loss
- Rectal bleeding
- Fever
- Nausea or recurrent vomiting
- Abdominal pain, especially if it’s not completely relieved by a bowel movement, or occurs at night
- Diarrhea that is persistent or awakens you from sleep
- Anemia related to low iron
If you have these signs or symptoms, or if an initial treatment for IBS doesn’t work, you’ll likely need additional tests.
What tests do doctors use to diagnose IBS?
Your doctor may recommend several tests, including stool studies to check for infection or problems with your intestine’s ability to take in the nutrients from food (malabsorption). You may also have a number of other tests to rule out other causes for your symptoms.
Diagnostic procedures and imaging tests can include:
- Flexible sigmoidoscopy. Your doctor examines the lower part of your colon (sigmoid) with a flexible, lighted tube (sigmoidoscope).
- Colonoscopy. Your doctor uses a small, flexible tube to examine the entire length of your colon.
- Upper endoscopy. A long, flexible tube is inserted down your throat and into your esophagus, which is the tube connecting your mouth and stomach. A camera on the end of the tube provides a view of your upper digestive tract. During an endoscopy, a tissue sample called a biopsy may be collected. A sample of fluid may be collected to look for overgrowth of bacteria. This test may be recommended if celiac disease is suspected.
- X-ray or CT scan. These tests produce images of your abdomen and pelvis that might allow your doctor to rule out other causes of your symptoms, especially if you have abdominal pain. Your doctor might fill your large intestine with a liquid (barium) to make any problems more visible on X-ray. This barium test is sometimes called a lower GI series.
Laboratory tests can include:
- Lactose intolerance tests. Lactase is an enzyme you need to digest the sugar found in dairy products. If you don’t produce lactase, you may have problems similar to those caused by IBS, including abdominal pain, gas and diarrhea. Your doctor may order a breath test or ask you to remove milk and milk products from your diet for several weeks.
- Breath test for bacterial overgrowth. A breath test also can determine if you have bacterial overgrowth in your small intestine. Bacterial overgrowth is more common among people who have had bowel surgery or who have diabetes or some other disease that slows down digestion.
- Upper endoscopy. A long, flexible tube is inserted down your throat and into the tube connecting your mouth and stomach (esophagus). A camera on the end of the tube allows the doctor to inspect your upper digestive tract and obtain a tissue sample (biopsy) from your small intestine and fluid to look for overgrowth of bacteria. Your doctor might recommend endoscopy if celiac disease is suspected.
- Stool tests. Your stool might be examined for bacteria or parasites, or a digestive liquid produced in your liver (bile acid), if you have chronic diarrhea. Bile acid is a digestive liquid produced in the liver. Stool studies also can check to see if the intestine has trouble taking in nutrients. This is a condition known as malabsorption.
IBS Rome IV Diagnostic Criteria
Recurrent abdominal pain, on average, at least 1 day per week in the last 3 months, associated with 2 or more of the following criteria 54:
- Related to defecation.
- Associated with a change in the frequency of stool.
- Associated with a change in the form (appearance) of stool.
These criteria fulfilled for the last 3 months with symptom onset at least 6 months before diagnosis.
IBS subtypes diagnostic criteria
Predominant bowel habits are based on stool form on days with at least one abnormal bowel movement 54:
- IBS with constipation predominant (IBS-C): More than one-fourth (25%) of bowel movements with Bristol stool form types 1 or 2 and less than one-fourth (25%) of bowel movements with Bristol stool form types 6 or 7. Alternative for epidemiology or clinical practice: Patient reports that abnormal bowel movements are usually constipation (like type 1 or 2 in the picture of Bristol Stool Form Scale [BSFS] below).
- IBS with diarrhea predominant (IBS-D): more than one-fourth (25%) of bowel movements with Bristol stool form types 6 or 7 and less than one-fourth (25%) of bowel movements with Bristol stool form types 1 or 2. Alternative for epidemiology or clinical practice: Patient reports that abnormal bowel movements are usually diarrhea (like type 6 or 7 in the picture of Bristol Stool Form Scale [BSFS] below).
- IBS with mixed bowel habits (IBS-M): more than one-fourth (25%) of bowel movements with Bristol stool form types 1 or 2 and more than one-fourth (25%) of bowel movements with Bristol stool form types 6 or 7. Alternative for epidemiology or clinical practice: Patient reports that abnormal bowel movements are usually both constipation and diarrhea (more than one-fourth of all the abnormal bowel movements were constipation and more than one-fourth were diarrhea, using picture of Bristol Stool Form Scale [BSFS] below).
- IBS unclassified (IBS-U): Patients who meet diagnostic criteria for IBS but whose bowel habits cannot be accurately categorized into 1 of the 3 groups above should be categorized as having IBS unclassified.
The Bristol stool form scale (BSFS) was developed in the 1990s in the Bristol Royal Infirmary in England 52. The authors described 7 types of stool (see Figure 4 below):
- Type 1: Separate hard lumps, like nuts (hard to pass)
- Type 2: Sausage-shaped, but lumpy
- Type 3: Like a sausage but with cracks on its surface
- Type 4: Like a sausage or snake, smooth and soft
- Type 5: Soft blobs with clear cut edges (passed easily)
- Type 6: Fluffy pieces with ragged edges, a mushy stool
- Type 7: Watery, no solid pieces, entirely liquid
The authors classified stool types 1 and 2 as being associated with constipation, while stool types 6 and 7 were associated with diarrhea and stool type 5 to some degree 52. Stool types 3 and 4 were considered normal stools. The BSFS is a convenient way for patients to describe their bowel habits, and is routinely used in clinical trials. In addition, at the two extremes (Bristol stool types 1 and 2 or types 6 and 7), the stool form serves as a rough surrogate marker of colon transit 52. Patients with IBS with constipation predominant (IBS-C) have >25% of their bowel movements associated with BSFS 1 or 2, while those with IBS with diarrhea predominant (IBS-D) have >25% of their bowel movements associated with BSFS 6 or 7. Those with the mixed subtype of alternating constipation and diarrhea (IBS-M) have >25% of their bowel movements associated with BSFS 1 or 2 and >25% of their bowel movements associated with BSFS 6 or 7.
For clinical trials, or when appropriate in clinical settings, subjects should complete a 14-day bowel diary to most accurately categorize IBS subtypes. Bristol stool types 1 and 2 or types 6 and 7 are considered abnormal 52.
IBS subtypes related to bowel habit abnormalities (IBS-C, IBS-D, and IBS-M) can only be confidently established when the patient is evaluated off medications used to treat bowel habit abnormalities.
Figure 4. Bristol Stool Form Scale
Footnotes: (A) The Bristol Stool Form Scale (BSFS) is a useful tool to evaluate bowel habit. The Bristol Stool Form Scale (BSFS) has been shown to be a reliable surrogate marker for colonic transit 73. (B) IBS subtypes should be established according to stool consistency, using the Bristol Stool Form Scale (BSFS). IBS subtyping is more accurate when patients have at least 4 days of abnormal bowel habits per month. Bowel habit subtypes should be based on Bristol Stool Form Scale (BSFS) for days with abnormal bowel habits.
[Source 54 ]Irritable bowel syndrome treatment
Treatment of IBS focuses on relieving symptoms so that you can live as normally as possible.
Stressful life experiences can worsen IBS symptoms and it is important you seek advise for stress reduction from your primary care clinician if you are having difficulty dealing with the stress.
Mild signs and symptoms can often be controlled by managing stress and by making changes in your diet and lifestyle. Try to:
- Avoid foods that trigger your symptoms
- Eat high-fiber foods. Fiber may improve constipation in IBS because it makes stool soft and easier to pass. The Dietary Guidelines for Americans recommends that adults should get 22 to 34 grams of fiber a day 74. To help your body get used to more fiber, add foods with fiber to your diet a little at a time. Too much fiber at once can cause gas, which can trigger IBS symptoms. Adding fiber to your diet slowly, by 2 to 3 grams a day, may help prevent gas and bloating.
- Two types of fiber are:
- Soluble fiber, which is found in beans, fruit, and oat products. Research suggests that soluble fiber is more helpful in relieving IBS symptoms.
- Insoluble fiber, which is found in whole-grain products and vegetables
- Two types of fiber are:
- Drink plenty of fluids
- Exercise regularly
- Get enough sleep.
Your doctor might suggest that you ELIMINATE or AVOID from your diet:
- High-gas foods. If you experience bloating or gas, you might avoid items such as carbonated and alcoholic beverages, caffeine, raw fruit, and certain vegetables, such as cabbage, broccoli and cauliflower.
- Gluten. Research shows that some people with IBS report improvement in diarrhea symptoms if they stop eating gluten (wheat, barley and rye) even if they don’t have celiac disease.
- FODMAPs. Some people are sensitive to certain carbohydrates such as fructose, fructans, lactose and others, known as FODMAPs — fermentable oligo-, di-, and monosaccharides and polyols. FODMAPs are found in certain grains, vegetables, fruits and dairy products. Your IBS symptoms might ease if you follow a strict low-FODMAP diet and then reintroduce foods one at a time. Examples of foods that contain FODMAPs include:
- fruits such as apples, apricots, blackberries, cherries, mango, nectarines, pears, plums, and watermelon, or juice containing any of these fruits.
- canned fruit in natural fruit juice, or large amounts of fruit juice or dried fruit.
- vegetables such as artichokes, asparagus, beans, cabbage, cauliflower, garlic and garlic salts, lentils, mushrooms, onions, and sugar snap or snow peas.
- dairy products such as milk, milk products, soft cheeses, yogurt, custard, and ice cream.
- wheat and rye products.
- honey and foods with high-fructose corn syrup.
- products, including candy and gum, with sweeteners ending in “–ol,” such as sorbitol, mannitol, xylitol, and maltitol.
Your doctor may suggest that you try the low FODMAP diet for a few weeks to see if it helps with your symptoms. If your symptoms improve, your doctor may recommend slowly adding foods that contain FODMAPs back into your diet. You may be able to eat some foods with FODMAPs without having IBS symptoms.
A dietitian can help you with these diet changes.
If your problems are moderate or severe, your doctor might suggest counseling — especially if you have depression or if stress tends to worsen your symptoms.
In addition, based on your symptoms your doctor might suggest medications such as:
- Fiber supplements. Taking a supplement such as psyllium (Metamucil) with fluids may help control constipation.
- Laxatives. If fiber doesn’t help constipation, nonprescription laxatives, such as magnesium hydroxide oral (Milk of Magnesia) or polyethylene glycol (Miralax), may be recommended.
- Anti-diarrheal medications. Over-the-counter medications, such as loperamide (Imodium), can help control diarrhea. Your doctor might also prescribe a bile acid binder, such as cholestyramine (Prevalite), colestipol (Colestid) or colesevelam (Welchol). Bile acid binders can cause bloating.
- Anticholinergic medications. Medications such as dicyclomine (Bentyl) can help relieve painful bowel spasms. They are sometimes prescribed for people who have bouts of diarrhea. These medications are generally safe but can cause constipation, dry mouth and blurred vision.
- Tricyclic antidepressants. This type of medication can help relieve depression as well as inhibit the activity of neurons that control the intestines to help reduce pain. If you have diarrhea and abdominal pain without depression, your doctor may suggest a lower than normal dose of imipramine (Tofranil), desipramine (Norpramine) or nortriptyline (Pamelor). Side effects — which might be reduced if you take the medication at bedtime — can include drowsiness, blurred vision, dizziness and dry mouth.
- SSRI antidepressants. Selective serotonin reuptake inhibitor (SSRI) antidepressants, such as fluoxetine (Prozac, Sarafem) or paroxetine (Paxil), may help if you’re depressed and have pain and constipation.
- Pain medications. Pregabalin (Lyrica) or gabapentin (Neurontin) might ease severe pain or bloating.
IBS medication
Medications approved for certain people with IBS include:
- Alosetron (Lotronex). Alosetron is designed to relax the colon and slow the movement of waste through the lower bowel. Alosetron can be prescribed only by doctors enrolled in a special program, is intended for severe cases of diarrhea-predominant IBS in women who haven’t responded to other treatments, and isn’t approved for use by men. It has been linked to rare but important side effects, so it should only be considered when other treatments aren’t successful.
- Eluxadoline (Viberzi). Eluxadoline can ease diarrhea by reducing muscle contractions and fluid secretion in the intestine, and increasing muscle tone in the rectum. Side effects can include nausea, abdominal pain and mild constipation. Eluxadoline has also been associated with pancreatitis, which can be serious and more common in certain individuals.
- Rifaximin (Xifaxan). This antibiotic can decrease bacterial overgrowth and diarrhea.
- Lubiprostone (Amitiza). Lubiprostone can increase fluid secretion in your small intestine to help with the passage of stool. It’s approved for women who have IBS with constipation, and is generally prescribed only for women with severe symptoms that haven’t responded to other treatments.
- Linaclotide (Linzess). Linaclotide also can increase fluid secretion in your small intestine to help you pass stool. Linaclotide can cause diarrhea, but taking the medication 30 to 60 minutes before eating might help.
Lifestyle and home remedies
Simple changes in your diet and lifestyle often provide relief from IBS. Your body will need time to respond to these changes. Try to:
- Experiment with fiber. Fiber helps reduce constipation but also can worsen gas and cramping. Try slowly increasing the amount of fiber in your diet over a period of weeks with foods such as whole grains, fruits, vegetables and beans. A fiber supplement might cause less gas and bloating than fiber-rich foods.
- Avoid problem foods. Eliminate foods that trigger your symptoms.
- Drink plenty of water. Drink at least eight 8-ounce glasses of water a day (2 liters). Water keeps your gastrointestinal tract lubricated and can help treat or prevent constipation.
- Limit dairy products, like cheese and milk. Lactose intolerance is more common in people with IBS. If you cut back on dairy, make sure to eat nondairy foods rich in calcium, like broccoli, spinach or salmon.
- Limit foods that can make you gassy. Foods like beans, brussels sprouts and cabbage are notorious for causing gas, but carbonated sodas and even chewing gum can make you gassy. Reduce these foods to go easier on your gut.
- Avoid gluten. People with IBS — even those without celiac disease — tend to be more sensitive to gluten. If you opt for a gluten-free diet, work with your doctor and dietitian to ensure you’re getting enough of the key vitamins and minerals (like fiber, iron and calcium) often found in foods with gluten.
- Eat at regular times. Don’t skip meals, and try to eat at about the same time each day to help regulate bowel function. If you have diarrhea, you may find that eating small, frequent meals makes you feel better. But if you’re constipated, eating larger amounts of high-fiber foods may help move food through your intestines.
- Exercise regularly. Exercise helps relieve depression and stress, stimulates normal contractions of your intestines, and can help you feel better about yourself. Aim for 150 minutes of moderate exercise weekly. This is about 30 minutes a day, five days a week.
- Try relaxation techniques. Daily yoga, meditation and other de-stressing techniques can help calm an overtaxed nervous system and a “nervous gut”. Sometimes, a behavioral therapist can help.
- Get enough sleep. Aim for seven to nine hours of quality sleep each night. Go to bed at the same time each night. A good night’s rest is one of the most powerful de-stressors available. Reach out to your doctor if you’re having trouble sleeping.
Many people with IBS benefit from seeing a therapist. Therapy can help you get a handle on stress and conditions such as anxiety and depression that contribute to IBS. Some people find relief through:
- Cognitive behavioral therapy (CBT). Cognitive behavioral therapy (CBT) is a type of psychotherapy (talk therapy) that helps people learn to challenge negative thoughts and behaviors. It can help with a variety of mental health conditions such as depression and anxiety, and emotional concerns, and PTSD. CBT can also help manage nonpsychological health conditions, such as insomnia and chronic pain. Mental health professionals, including psychologists, therapists and counselors, use CBT to treat or manage mental health conditions and emotional concerns. It’s one of the most common and best-studied forms of psychotherapy.
- Hypnotherapy. Hypnotherapy is a psychological therapy that uses hypnosis to treat mental and physical health conditions. Hypnosis allows you to be more open to suggestions about making healthful changes in your perceptions, sensations, emotions, memories, thoughts or behaviors. It can also help change habits. A trained, certified hypnotist or hypnotherapist will guide you.
- Biofeedback. Biofeedback is a type of mind-body technique that helps you take control of certain involuntary bodily functions, such as your heart rate, breathing patterns and muscle responses. There are several types of biofeedback therapy. It can help manage conditions like chronic pain, anxiety and incontinence. During biofeedback, you’re connected to electrical pads and a healthcare provider uses noninvasive monitoring equipment and instruments to measure your body’s involuntary functions. Based on feedback from the instruments, your healthcare provider suggests how you can create voluntary (conscious) changes for these mostly involuntary functions. With education and practice, you can learn to make those bodily changes without equipment.
Bloating, cramps and farting remedies
- eat oats (such as porridge) regularly
- eat up to 1 tablespoon of linseeds (whole or ground) a day
- avoid foods that are hard to digest (like cabbage, broccoli, cauliflower, brussels sprouts, beans, onions and dried fruit)
- avoid products containing a sweetener called sorbitol
- ask your pharmacist about medicines that can help, like Buscopan or peppermint oil
Diarrhea remedies
- cut down on high-fiber foods like wholegrain foods (such as brown bread and brown rice), nuts and seeds
- avoid products containing a sweetener called sorbitol
- ask your pharmacist about medicines that can help, like Imodium (loperamide)
Constipation remedies
- drink plenty of water to help make your stool softer
- increase how much soluble fiber you eat – good foods include oats, pulses, carrots, peeled potatoes and linseeds (whole or ground)
- ask your pharmacist about medicines that can help (laxatives), like Metamucil or Citrucel.
Alternative medicine
The role of alternative therapies in relieving IBS symptoms is unclear. Ask your doctor before starting any of these treatments. Alternative therapies include:
- Hypnosis. A trained professional teaches you how to enter a relaxed state and then guides you in relaxing your abdominal muscles. Hypnosis may reduce abdominal pain and bloating. Several studies support the long-term effectiveness of hypnosis for IBS.
- Mindfulness training. Mindfulness is the act of being intensely aware of what you’re sensing and feeling at every moment, without interpretation or judgment. Research indicates that mindfulness can ease symptoms of IBS.
- Acupuncture. Researchers have found that acupuncture may help improve symptoms for people with IBS.
- Peppermint. Peppermint is a natural antispasmodic that relaxes smooth muscles in the intestines. It might provide short-term relief of IBS symptoms, but study results have been inconsistent.
- Probiotics. Probiotics are “good” bacteria that normally live in your intestines and are found in certain foods, such as yogurt, and in dietary supplements. Recent studies suggest that certain probiotics may relieve IBS symptoms, such as abdominal pain, bloating and diarrhea.
- Stress reduction. Yoga or meditation can help relieve stress. You can take classes or practice at home using books or videos.
IBS Diet
There is no ‘one size fits all’ diet for IBS. However, dietary changes can often relieve IBS symptoms.
It may help to keep a food diary so you can identify any foods that make your symptoms worse.
It can also help to modify the amount and type of fiber in your diet:
- If you have IBS with constipation, it can help to eat more soluble fiber and drink more water
- If you have IBS with diarrhea, it can help to cut down on insoluble fiber.
In some cases, avoiding a particular food or food group might help – examples include gluten, caffeine, alcohol, spicy foods, high fat foods or foods that cause excessive bloating such as beans, lentils or certain vegetables.
In past years IBS was treated from the perspective that it was a “motility disorder”. The use of fiber supplementation to improve intestinal motility or movement was a common recommendation. While some studies have questioned whether fiber supplementation alone is helpful for the treatment of IBS and its symptoms, there are other good reasons to consume a high fiber diet. High fiber diets are associated with lower blood sugar, lower cholesterol as well as a lower tendency to form diverticula or outpouchings of the colon. Moreover, some patients with IBS report having a good result with a high fiber diet. Certainly every patient should include at least 25 grams of fiber in their diet every day.
What is FODMAP?
Australian researchers have recently developed a special diet that may help control IBS symptoms in some people. It’s called the FODMAP diet, and it involves restricting your intake of certain dietary carbohydrates (sugars) that are poorly absorbed by the bowel.
Before making any major changes to your diet it is a good idea to talk to your doctor or a dietitian.
FODMAP stands for “Fermentable Oligosaccharides, Disaccharides, Monosaccharides And Polyols“. A diet low in fermentable oligosaccharides, disaccharides, monosaccharides, and polyols (FODMAPs) – low FODMAP diet. Since ingestion of FODMAPs increases the delivery of readily fermentable substrates and water to the distal small intestine and colon—which results in luminal distention and gas—the reduction of FODMAPs in a patient’s diet may improve functional gastrointestinal symptoms 75.
These fermentable short-chain carbohydrates are prevalent in the diet.
- Oligosaccharides: fructans and galactooligosaccharides (GOS)
- Disaccharides: lactose
- Monosaccharides: fructose
- Polyols: sorbitol and mannitol
Researchers suggest that the small intestine does not absorb FODMAPs very well. They increase the amount of fluid in the bowel. They also create more gas. That’s because bacteria in the colon they are easily fermented by colonic bacteria. The increased fluid and gas in the bowel leads to bloating and changes in the speed with which food is digested. This results in gas, pain and diarrhea. Eating less of these types of carbohydrates should decrease these symptoms.
As FODMAPs are poorly absorbed during the digestive process, they may pass to the large intestine (colon), where they are rapidly fermented by the bacteria that normally live in the colon. This makes chemicals called short chain fatty acids, as well as gas. This, in turn, leads to changes in the acidity and types of bacteria in the colon. The colon expands, which can lead to pain, bloating, and changes in bowel habits.
- Diets rich in FODMAPs may increase symptoms in patients with functional gut disorders (FGD) or irritable bowel syndrome (IBS). However, the FODMAPs themselves are not the root of the problem. For that reason, patients may need to include other options to treat their symptoms. This may include medicine, exercise, meditation, hypnotherapy, etc.
So far, studies have shown that a low FODMAP diet has a beneficial effect in a majority of patients with Irritable Bowel Syndrome (IBS) symptoms 76. One study even found that 76% of Irritable Bowel Syndrome (IBS) patients following the diet reported improvement with their symptoms. Probiotics also have great potential in the management of Irritable Bowel Syndrome (IBS); however, it is still unclear which strains and doses are the most beneficial. Further research is needed on the effect of different fibers or combinations of fibers, in Irritable Bowel Syndrome (IBS).
Low Fodmap Diet
FODMAP stands for Fermentable, Oligo-, Di-, Mono-saccharides And Polyols. FODMAPs are short-chain carbohydrates (sugars) that are highly fermentable (to ferment, is to go through a chemical change that results in alcohol) and poorly absorbed during digestion 77. The acronym FODMAPs was created to describe poorly absorbed, short-chain carbohydrates that can lead to excessive fluid and gas accumulation, resulting in bloating, abdominal pain, and distention (Figure 4).
The Low FODMAP diet was developed by researchers at Monash University more than five years ago, in Australia, by Susan Shepherd and Peter Gibson. This diet eliminates certain foods to improve the symptoms of functional gut disorders (FGD). Irritable bowel syndrome (IBS), a type of FGD, may be helped by this diet. IBS is the most commonly diagnosed gastrointestinal condition and over half of patients with IBS associate a trigger in their symptoms with eating a meal 78. The Monash team, led by Professor Peter Gibson, provided the first evidence that a Low FODMAP diet improves IBS symptoms. Irritable bowel syndrome (IBS) is a common functional gastrointestinal disorder affecting one in seven Australian adults and approximately 35 million Americans are impacted by IBS including many in Europe and many in Asian countries. IBS is characterised by chronic and relapsing symptoms; lower abdominal pain and discomfort, bloating, wind, distension and altered bowel habit (ranging from diarrhoea to constipation) but with no abnormal pathology. The diagnosis of IBS should be made by a medical practitioner.
FODMAPs are found in a wide variety of foods, including those containing lactose, fructose in excess of glucose, fructans, galacto-oligosaccharides, and polyols (sorbitol, mannitol, xylitol, and maltitol). All FODMAPs have poor absorption and rapid fermentation, and they are comprised of small, osmotically active molecules. FODMAPs are poorly absorbed for a number of reasons, including the absence of luminal enzymes capable of hydrolyzing the glycosidic bonds contained in carbohydrates, the absence or low activity of brush border enzymes (eg, lactase), or the presence of low-capacity epithelial transporters (fructose, glucose transporter 2 [GLUT-2], and glucose transporter 5 [GLUT-5]). Fructose, which is an important FODMAP in the Western diet, is absorbed across villous epithelium through low-capacity, carrier-mediated diffusion involving GLUT-5. The absorption of free fructose is markedly enhanced in the presence of glucose via GLUT-2. Therefore, if fructose is present in excess of glucose, the risk of fructose malabsorption is increased. In addition, some molecules, such as polyols, are too large for simple diffusion. The fermentation rate is determined by the chain length of the carbohydrate 79.
For example, oligosaccharides are rapidly fermented, compared to polysaccharides. Fermentation results in the production of carbon dioxide, hydrogen, and/or methane gas. Finally, small, osmotically active molecules draw more water and other liquid into the small bowel. Given these properties, a diet low in FODMAPs has become a potential therapy for IBS patients.
When FODMAPs reach the colon (large intestine), bacteria ferment these sugars, turning them into gas and chemicals. This stretches the walls of the colon, causing abdominal bloating, distension, and pain or cramping in many people. Other symptoms, such as diarrhea, constipation, and nausea, are also common side effects of FODMAP carbohydrates. Not everyone has the same reaction to FODMAPs. Ethnicity, genetics, and environmental factors (such as an individual’s microbiome, motility, immune system, and sensory system) may play a part in your body’s ability to tolerate these carbohydrates.
Figure 5. FODMAPs in your gut
Note: Ingested fermentable oligosaccharides, disaccharides, monosaccharides, and polyols (FODMAPs) are poorly absorbed in the small intestine. Their small molecular size results in an osmotic effect, drawing water (H20) through to the large intestine. FODMAPs are then fermented by colonic microflora, producing hydrogen (H2) and/or methane gas (CH4). The increase in fluid and gas leads to diarrhea, bloating, flatulence, abdominal pain, and distension.
[Source 75]Bowel obstruction
Bowel obstruction is a blockage that keeps food or liquid from passing through your small intestine or large intestine (colon). This interruption can occur at any point along the length of the gastrointestinal tract and clinical symptoms often vary based on the level of obstruction, the nature, severity, location and etiology. Bowel obstruction may be functional, due to bowel wall or splanchnic nerve dysfunction (pseudo-bowel obstruction), or mechanical, due to a mechanical barrier. Intestinal obstruction is most commonly caused by intra-abdominal adhesions, malignancy, or intestinal herniation.
Obstruction may occur in the small bowel (small bowel obstruction) or large bowel (large bowel obstruction). Large bowel obstruction or disease states may be associated with or masquerade as small bowel obstruction. Acute functional dilatation of the colon is referred to as “colonic pseudo-obstruction”. Acute functional small bowel dilatation is referred to as “adynamic or paralytic ileus”.
Bowel obstruction may be partial or complete, simple or complicated. Partial bowel obstruction allows some liquid contents and gas to pass through the point of obstruction, whereas complete bowel obstruction impedes passage of all bowel contents. Unlike simple bowel obstruction, complicated bowel obstruction indicates compromise of the circulation to a segment of bowel with resultant ischemia, infarction, and perforation.
Intestinal obstruction accounts for approximately 15 percent of all emergency department visits for acute abdominal pain 80.
Causes of bowel obstruction may include fibrous bands of tissue (adhesions) in the abdomen that form after surgery, an inflamed intestine (Crohn’s disease), infected pouches in your intestine (diverticulitis), hernias and colon cancer.
Complications of intestinal obstruction include bowel ischemia and perforation. Morbidity and mortality associated with intestinal obstruction have declined since the advent of more sophisticated diagnostic tests, but the condition remains a challenging surgical diagnosis.
Without treatment, the blocked parts of the intestine can die, leading to serious problems. However, with prompt medical care, intestinal obstruction often can be successfully treated. Physicians who are treating patients with intestinal obstruction must weigh the risks of surgery with the consequences of inappropriate conservative management.
Because of the serious complications that can develop from intestinal obstruction, seek immediate medical care if you have severe abdominal pain or other symptoms of bowel obstruction.
Bowel obstruction causes
The most common causes of intestinal obstruction include adhesions, neoplasms (tumors) and herniation (Table 1).
The most common causes of intestinal obstruction in adults are:
- Intestinal adhesions (60 percent) — bands of fibrous tissue in the abdominal cavity that can form after abdominal or pelvic surgery
- Colon cancer (20 percent)
Adhesions resulting from prior abdominal surgery are the predominant cause of small bowel obstruction, accounting for approximately 60 percent of cases 81. Lower abdominal surgeries, including appendectomies, colorectal surgery, gynecologic procedures, and hernia repairs, confer a greater risk of adhesive small bowel obstruction. Less common causes of obstruction include intestinal intussusception, volvulus, intra-abdominal abscesses, gallstones, and foreign bodies.
In children, the most common cause of intestinal obstruction is telescoping of the intestine (intussusception) (see Figures 2 and 3).
Other possible causes of intestinal obstruction include:
- Hernias — portions of intestine that protrude into another part of your body
- Inflammatory bowel diseases, such as Crohn’s disease
- Diverticulitis — a condition in which small, bulging pouches (diverticula) in the digestive tract become inflamed or infected
- Twisting of the colon (volvulus)
- Impacted feces
Table 3. Bowel obstruction causes
| Adhesive disease (60 percent) |
| Neoplasm (20 percent) |
| Herniation (10 percent) |
| Inflammatory bowel disease (5 percent) |
| Intussusception (< 5 percent) |
| Volvulus (< 5 percent) |
| Other (< 5 percent) |
Intussusception
Intussusception is a unique type of bowel obstruction that results from invagination of a segment of bowel into another (see Figures 2 and 3). It may occur anywhere along the gastrointestinal tract distal to the gastric cardia. Intussusception may occur in a downward direction or may be retrograde, and is classified into enteric. The exact mechanism colic and enterocolic of itussuception is not known but an organic lesion, diseased segment of bowel, or an adjacent area of normal bowel may serve as a lead point in initiating the process. Accordingly, intussusception is classified into idiopathic, postoperative, and intussusception due to an organic lesion. In adults, a tumor is the lead point in 80–90% of cases. A Meckel’s diverticulum (see Figure 5) may invaginate into the ileum and sometimes, thence, into the colon 82.
Malignant tumors are being recognized with increasing frequency. A recently recognized subtype is postoperative intussusception. The point of origin of the intussusception is the small bowel and more specifically, the jejunum, particularly proximal jejunum, and dense desmoplastic inflammatory reaction within the mesentery may be the underlying mechanism precipitating the intussusception.
Figure 6. Intussusception
Figure 7. Intussusception of distal small intestine into the cecum (large intestine)
Volvulus
Volvulus is axial twist of the gastrointestinal tract around its mesentery resulting in partial or complete luminal obstruction (closed loop) of the bowel and a variable degree of arterial or venous obstruction (Figure 8). Volvulus commonly occurs in the colon (large intestine) and may affect the stomach or small bowel. Volvulus occurs when the small bowel twists around a Meckel’s diverticulum that is attached by a fibrous cord to the umbilicus 82, or when a closed loop obstruction twists along its long axis. Gallstone ileus is a mechanical bowel obstruction caused by migration of gallstones from the biliary system through a biliary-enteric fistula with impaction within lumen of the bowel. Littre’s hernia is incarcerated Meckel’s diverticulum in an external hernia.
Figure 8. Volvulus
Figure 9. Meckel’s diverticulum
Intestinal Pseudo-obstruction
Intestinal pseudo-obstruction (paralytic ileus) can cause signs and symptoms of bowel obstruction, but doesn’t involve a physical blockage 83. Intestinal pseudo-obstruction is a rare condition with symptoms that resemble those caused by a blockage, or obstruction, of the intestines. In paralytic ileus, muscle or nerve problems disrupt the normal coordinated muscle contractions of the intestines, slowing or stopping the movement of food and fluid through the digestive system.
This condition can occur in people of any age. Some infants are born with congenital intestinal pseudo-obstruction, and some people develop this condition as adults. Intestinal pseudo-obstruction may be acute, occurring suddenly and lasting a short time, or it may be chronic, or long lasting.
Acute colonic pseudo-obstruction, also called Ogilvie syndrome or acute colonic ileus, mostly affects older adults. In this condition, the colon becomes distended, or enlarged, after
- surgery, such as operations to open the abdomen or replace a hip or knee
- injury, such as a hip fracture
- illness, such as a serious infection
Acute large bowel pseudo-obstruction can lead to serious complications. However, people with the condition usually get better with treatment.
What causes intestinal pseudo-obstruction?
Problems with nerves, muscles, or interstitial cells of Cajal cause intestinal pseudo-obstruction. Interstitial cells of Cajal are called “pacemaker” cells because they set the pace of intestinal contractions. These cells convey messages from nerves to muscles.
Problems with nerves, muscles, or interstitial cells of Cajal prevent normal contractions of the intestines and cause problems with the movement of food, fluid, and air through the intestines.
Primary or idiopathic intestinal pseudo-obstruction is intestinal pseudo-obstruction that occurs by itself. In some people with primary intestinal pseudo-obstruction, mutations, or changes, in genes—traits passed from parent to child—cause the condition. However, health care providers do not typically order genetic testing for an intestinal pseudo-obstruction, as they don’t commonly recognize gene mutations as a cause.
Some people have duplications or deletions of genetic material in the FLNA gene. Researchers believe that these genetic changes may impair the function of a protein, causing problems with the nerve cells in the intestines.1 As a result, the nerves cannot work with the intestinal muscles to produce normal contractions that move food, fluid, and air through the digestive tract. Also, these genetic changes may account for some of the other signs and symptoms that can occur with intestinal pseudo-obstruction, such as bladder symptoms and muscle weakness.
A condition called mitochondrial neurogastrointestinal encephalopathy may also cause primary intestinal pseudo-obstruction. In people with this condition, mitochondria—structures in cells that produce energy—do not function normally. Mitochondrial neurogastrointestinal encephalopathy can also cause other symptoms, such as problems with nerves in the limbs and changes in the brain.
Secondary intestinal pseudo-obstruction develops as a complication of another medical condition. Causes of secondary intestinal pseudo-obstruction include:
- Abdominal or pelvic surgery
- Diseases that affect muscles and nerves, such as lupus erythematosus, scleroderma, and Parkinson’s disease
- Infections
- Certain medications that affect muscles and nerves, including tricyclic antidepressants, such as amitriptyline and imipramine (Tofranil), and opioid pain medications, such as those containing hydrocodone (Vicodin) and oxycodone (Oxycontin)
- Radiation to the abdomen
- Certain cancers, including lung cancer
What are the symptoms of intestinal pseudo-obstruction?
Intestinal pseudo-obstruction symptoms may include:
- abdominal swelling or bloating, also called distension
- abdominal pain
- nausea
- vomiting
- constipation
- diarrhea
Over time, the condition can cause malnutrition, bacterial overgrowth in the intestines, and weight loss. Malnutrition is a condition that develops when the body does not get the right amount of the vitamins, minerals, and other nutrients it needs to maintain healthy tissues and organ function.
Some people develop problems with their esophagus, stomach, or bladder.
How is intestinal pseudo-obstruction diagnosed?
To diagnose intestinal pseudo-obstruction, a health care provider may suggest the person consult a gastroenterologist—a doctor who specializes in digestive diseases. A health care provider will perform a physical exam; take a complete medical history, imaging studies, and a biopsy; and perform blood tests. A health care provider may order other tests to confirm the diagnosis. The health care provider also will look for the cause of the condition, such as an underlying illness.
Intestinal pseudo-obstruction can be difficult to diagnose, especially primary intestinal pseudo-obstruction. As a result, a correct diagnosis may take a long time.
Physical Exam
A physical exam is one of the first things a health care provider may do to help diagnose intestinal pseudo-obstruction. During a physical exam, a health care provider usually:
- examines a person’s body
- uses a stethoscope to listen to bodily sounds
- taps on specific areas of the person’s body
Medical History
The health care provider will ask a person to provide a medical and family history to help diagnose intestinal pseudo-obstruction.
A health care provider may order the following imaging studies:
- Abdominal x-ray. An x-ray is a picture recorded on film or a computer that a technician takes using low-level radiation.
- Upper GI series. A health care provider may order an upper GI series to look at the small intestine. A person should not eat or drink for 8 hours before the procedure, if possible. During the procedure, the person will stand or sit in front of an x-ray machine and drink barium, a chalky liquid. Infants lie on a table and the technician will give them barium through a tiny tube placed in the nose that runs into the stomach. Barium coats the lining of the small intestine, making signs of obstruction show up more clearly on x-rays.
- Lower GI series. A health care provider may order a lower GI series, an x-ray exam to look at the large intestine. For the test, the person will lie on a table while the health care provider inserts a flexible tube into the person’s anus. The health care provider will fill the large intestine with barium, making signs of underlying problems show up more clearly on x-rays. The test can show problems with the large intestine that are causing the person’s symptoms. The health care provider may ask the person to follow a clear liquid diet for 1 to 3 days before the procedure. A person may need to use a laxative or an enema before the test. A laxative is medication that loosens stool and increases bowel movements. An enema involves flushing water or laxative into the anus using a special squirt bottle.
- Computerized tomography (CT) scan. CT scans use a combination of x-rays and computer technology to create images.
- Upper GI endoscopy. This procedure involves using an endoscope—a small, flexible tube with a light—to see the upper GI tract, which includes the esophagus, stomach, and duodenum. A gastroenterologist performs the test at a hospital or an outpatient center. The gastroenterologist carefully feeds the endoscope down the esophagus and into the stomach and duodenum. A small camera mounted on the endoscope transmits a video image to a monitor, allowing close examination of the intestinal lining. A health care provider may give a person a liquid anesthetic to gargle or may spray anesthetic on the back of the person’s throat. A health care provider will place an intravenous (IV) needle in a vein in the arm to administer sedation. Sedatives help patients stay relaxed and comfortable. This test can show blockages or other conditions in the upper small intestine. A gastroenterologist may obtain a biopsy of the lining of the small intestine during an upper GI endoscopy.
Biopsy
A gastroenterologist can obtain a biopsy of the intestinal wall during endoscopy or during surgery, if the person has surgery for intestinal pseudo-obstruction and the cause is unknown. If the health care provider needs to examine the nerves in the intestinal wall, a deeper biopsy, which a gastroenterologist can typically obtain only during surgery, is necessary.
A biopsy is a procedure that involves taking a piece of the intestinal wall tissue for examination with a microscope. A health care provider performs the biopsy in a hospital and uses light sedation and local anesthetic; the health care provider uses general anesthesia if performing the biopsy during surgery. A pathologist—a doctor who specializes in diagnosing diseases—examines the intestinal tissue in a lab. Diagnosing problems in the nerve pathways of the intestinal tissue requires special techniques that are not widely available.
A health care provider can also use a biopsy obtained during endoscopy to rule out celiac disease. Celiac disease is an autoimmune disorder in which people cannot tolerate gluten because it damages the lining of their small intestine and prevents absorption of nutrients. Gluten is a protein found in wheat, rye, and barley and in products such as vitamin and nutrient supplements, lip balms, and certain medications.
Blood Tests
A blood test involves drawing blood at a health care provider’s office or a commercial facility and sending the sample to a lab for analysis. The blood test can show the presence of other diseases or conditions that may be causing a person’s symptoms. The blood test also can show levels of essential vitamins and minerals to help detect malnutrition.
Manometry
Manometry is a test that measures muscle pressure and movements in the GI tract, such as how well the smooth muscles of the stomach and small intestine contract and relax. A gastroenterologist performs the test at a hospital or an outpatient center. While the person is under sedation, a health care provider places a thin tube, or manometry tube, into the stomach and moves it down into the small intestine. A gastroenterologist may use an endoscope to place this tube. A health care provider will move the person to a manometry room and connect the manometry tube to a computer. When the person wakes up from sedation, the computer records the pressure inside the intestine while the person is fasting and after the person has eaten a meal. Manometry can confirm the diagnosis of intestinal pseudo-obstruction and show the extent of the condition.
Gastric Emptying Tests
Gastric emptying tests can show if a disorder called gastroparesis is causing a person’s symptoms. People with gastroparesis, which literally refers to a paralyzed stomach, have severely delayed gastric emptying, or the delayed movement of food from the stomach to the small intestine. Some patients with intestinal pseudo-obstruction also have gastroparesis.
Types of gastric emptying tests include the following:
- Gastric emptying scintigraphy. This test involves eating a bland meal—such as eggs or an egg substitute—that contains a small amount of radioactive material. A specially trained technician performs the test in a radiology center or hospital, and a radiologist interprets the results; the person does not need anesthesia. An external camera scans the abdomen to show where the radioactive material is located. The radiologist is then able to measure the rate of gastric emptying at 1, 2, 3, and 4 hours after the meal. Normal values depend on the composition of the meal. With some meals, if more than 10 percent of the meal is still in the stomach at 4 hours, a health care provider confirms the diagnosis of gastroparesis. Obtaining scans for 4 hours after the meal is essential. When the technician only obtains scans 1 to 2 hours after the meal, the results are often unreliable.
- Breath test. With this test, the person eats a meal containing a small amount of nonradioactive material. Then, the health care provider takes breath samples over a period of several hours to measure the amount of nonradioactive material in the exhaled breath. The results allow the health care provider to calculate how fast the stomach is emptying.
- SmartPill. The SmartPill is a small electronic device in capsule form. The SmartPill test is available at specialized outpatient centers. The person swallows the device so that it can move through the entire digestive tract and send information to a cell-phone-sized receiver worn around the person’s waist or neck. The recorded information provides details about how quickly food travels through each part of the digestive tract.
Intestinal pseudo-obstruction treatment
A health care provider will treat intestinal pseudo-obstruction with nutritional support, medications, and, in some cases, decompression. Rarely, a person will need surgery. If an illness, a medication, or both cause intestinal pseudo-obstruction, a health care provider will treat the underlying illness, stop the medication, or do both.
Nutritional Support
People with intestinal pseudo-obstruction often need nutritional support to prevent malnutrition and weight loss. Enteral nutrition provides liquid food through a feeding tube inserted through the nose into the stomach or placed directly into the stomach or small intestine. A health care provider inserts the feeding tube, sometimes using x-ray or endoscopy for guidance, and teaches the person how to care for the tube after returning home. Enteral nutrition is sufficient for most people with intestinal pseudo-obstruction. In a severe case, a person may need IV feeding, also called parenteral nutrition, which provides liquid food through a tube placed in a vein.
Enteral nutrition is possible because the intestinal lining is normal in most people with intestinal pseudo-obstruction. Enteral nutrition is preferred over parenteral nutrition because it has a much lower risk of complications.
Medications
A health care provider prescribes medications to treat the different symptoms and complications of intestinal pseudo-obstruction, such as
- antibiotics to treat bacterial infections
- pain medication, which should be used sparingly, if at all, because most pain medications delay intestinal transit
- medication to make intestinal muscles contract
- antinausea medications
- antidiarrheal medications
- laxatives
Decompression
A person with acute colonic pseudo-obstruction and a greatly enlarged colon who does not respond to medications may need a procedure, called decompression, to remove gas from the colon. A gastroenterologist can perform the procedure in a hospital or an outpatient center. The gastroenterologist may choose to decompress the colon by using colonoscopy. During colonoscopy, the gastroenterologist inserts a flexible tube into the colon through the anus. A health care provider gives the person a light sedative, and possibly pain medication, to relax. If the person requires long-term decompression, the gastroenterologist also can decompress the colon through a surgical opening in the cecum. In this case, the health care provider gives the person local anesthesia.
Surgery
In severe cases of intestinal pseudo-obstruction, a person may need surgery to remove part of the intestine. However, surgery should be performed rarely, if at all, because intestinal pseudo-obstruction is a generalized disorder that typically affects the entire intestine. Removing part of the intestine cannot cure the disease.
A surgeon—a doctor who specializes in surgery—will perform the surgery at a hospital; a person will need general anesthesia. A few highly specialized treatment centers offer small intestine transplantation. A health care provider may recommend small intestine transplantation when all other treatments have failed.
Eating, Diet, and Nutrition
Researchers have not found that eating, diet, and nutrition play a role in causing or preventing intestinal pseudo-obstruction. Following special diets usually does not help improve the disorder. However, eating frequent, small meals with pureed foods or liquids may ease digestion. Vitamin and trace mineral supplements may help a person who is malnourished.
Risk factors for bowel obstruction
Diseases and conditions that can increase your risk of intestinal obstruction include:
- Abdominal or pelvic surgery, which often causes adhesions — a common intestinal obstruction
- Crohn’s disease, which can cause the intestine’s walls to thicken, narrowing the passageway
- Cancer in your abdomen, especially if you’ve had surgery to remove an abdominal tumor or radiation therapy.
Bowel obstruction pathophysiology
The fundamental concerns about intestinal obstruction are its effect on whole body fluid/electrolyte balances and the mechanical effect that increased pressure has on intestinal perfusion. Proximal to the point of obstruction, the intestinal tract dilates as it fills with intestinal secretions and swallowed air 84. Failure of intestinal contents to pass through the intestinal tract leads to a cessation of flatus and bowel movements. Intestinal obstruction can be broadly differentiated into small bowel and large bowel obstruction.
Fluid loss from vomiting (emesis), bowel edema, and loss of absorptive capacity leads to dehydration. Vomiting leads to loss of gastric potassium, hydrogen, and chloride ions, and significant dehydration stimulates renal proximal tubule reabsorption of bicarbonate and loss of chloride, perpetuating the metabolic alkalosis 85. In addition to derangements in fluid and electrolyte balance, intestinal stasis leads to overgrowth of intestinal flora, which may lead to the development of feculent emesis. Additionally, overgrowth of intestinal flora in the small bowel leads to bacterial translocation across the bowel wall 86.
Ongoing dilation of the intestine increases luminal pressures. When luminal pressures exceed venous pressures, loss of venous drainage causes increasing edema and hyperemia of the bowel. This may eventually lead to compromised arterial flow to the bowel, causing ischemia, necrosis, and perforation. A closed-loop obstruction, in which a section of bowel is obstructed proximally and distally, may undergo this process rapidly, with few presenting symptoms. Intestinal volvulus, the prototypical closed-loop obstruction, causes torsion of arterial inflow and venous drainage, and is a surgical emergency.
Bowel obstruction signs and symptoms
Signs and symptoms of intestinal obstruction include:
- Crampy or colicky abdominal pain that comes and goes
- Loss of appetite
- Constipation
- Nausea and Vomiting
- Inability to have a bowel movement or pass gas
- Swelling of the abdomen.
Bowel obstruction complications
Untreated, intestinal obstruction can cause serious, life-threatening complications, including:
- Tissue death. Intestinal obstruction can cut off the blood supply to part of your intestine. Lack of blood causes the intestinal wall to die. Tissue death can result in a tear (perforation) in the intestinal wall, which can lead to infection.
- Infection. Peritonitis is the medical term for infection in the abdominal cavity. It’s a life-threatening condition that requires immediate medical and often surgical attention.
Small Intestine
Most digestion and absorption of nutrients occur in the small intestine. Because of this, its structure is specially adapted for these functions. Its length alone provides a large surface area for digestion and absorption, and that area is further increased by circular folds, villi, and microvilli. The small intestine begins at the pyloric sphincter of the stomach, coils through the central and inferior part of the abdominal cavity, and eventually opens into the large intestine. It averages 2.5 cm (1 in.) in diameter; its length is about 3 m (10 ft ) in a living person.
The small intestine is divided into three regions. The first part of the small intestine is the duodenum, the shortest region, and is retroperitoneal. It starts at
the pyloric sphincter of the stomach and is in the form of a C-shaped tube that extends about 25 cm (10 in.) until it merges with the jejunum. The jejunum is the next portion and is about 1 m (3 ft ) long and extends to the ileum. The final and longest region of the small intestine, the ileum, measures about 2 m (6 ft ) and joins the large intestine at a smooth muscle sphincter called the ileocecal sphincter (valve).
Large Intestine
The large intestine is the last major organ in the alimentary canal (Figure 1). The material that reaches it is a largely digested residue that contains few nutrients. During the 12–24 hours that this residue remains in the large intestine, little additional breakdown of food occurs, except for the small amount of digestion performed by the many bacteria living there. Even though the large intestine absorbs these few remaining nutrients, its main function is to absorb water and electrolytes from the digested mass, resulting in semisolid feces. Propulsion through the large intestine is sluggish and weak, except for mass peristaltic movements, which pass over the colon a few times a day to force the feces powerfully toward the rectum.
The large intestine frames the small intestine on 3½ sides, forming an open rectangle (Figure 1). This organ, which is wider than the small intestine but less than half as long (1.5 meters), has the following subdivisions: cecum, appendix, colon, rectum, and anal canal. Over most of its length, the large intestine exhibits three
special features: teniae coli, haustra, and epiploic appendages. Teniae (taeniae) coli are three longitudinal strips, spaced at equal intervals around the circumference of the cecum and colon. They are thickenings of the longitudinal layer of the muscularis externa, which is thin except at these sites. Because the teniae maintain muscle tone, they cause the large intestine to pucker into sacs, or haustra. Epiploic appendages, also called omental appendices, are fat-filled pouches of visceral peritoneum that hang from the intestine. Their significance is unknown.
The large intestine begins with the saclike cecum (blind pouch) in the right iliac fossa. The opening of the ileum of the small intestine into the cecum’s medial wall is surrounded internally by the ileocecal valve, which is formed by two raised edges of the mucosa. A sphincter in the distal ileum keeps the valve closed until there is food in the stomach, at which time the sphincter reflexively relaxes, opening the valve. As the cecum fills, its walls stretch, pulling the edges of the ileocecal valve together and closing the opening. This action prevents reflux of feces from the cecum back into the ileum.
The appendix is a blind tube that opens into the posteromedial wall of the cecum. Although almost always illustrated as hanging inferiorly, it more often lies “tucked up” posterior to the cecum in the right iliac fossa. The appendix has large masses of lymphoid tissue in its wall. Commonly considered a vestigial organ, current research proposes that the appendix functions as a safe haven for the beneficial bacteria that inhabit the large intestine. According to this theory, beneficial bacteria from the appendix can repopulate the gut following an infectious disease that causes diarrhea and flushes out the intestinal flora.
The colon has several distinct segments. From the cecum, the ascending colon ascends along the right side of the posterior abdominal wall in a secondarily retroperitoneal position and reaches the level of the right kidney, where it makes a rightangle turn, the right colic flexure (also called the hepatic flexure because the liver lies directly superior to it). From this flexure, the transverse colon extends intraperitoneal to the left across the peritoneal cavity. Directly anterior to the spleen, it bends acutely downward at the left colic (splenic) flexure and descends along the left side of the posterior abdominal wall again in a secondarily retroperitoneal position as the descending colon. Inferiorly, the colon becomes intraperitoneal and enters the true pelvis as the S-shaped sigmoid colon.
In the pelvis, the sigmoid colon joins the rectum, which descends along the inferior half of the sacrum in a secondarily retroperitoneal position. The rectum has no teniae coli; its longitudinal muscle layer is complete and well developed, so that it can generate strong contractions for defecation. Even though the word rectum means “straight,” the rectum actually has several tight bends. Internally, these bends are represented as three transverse folds of the rectum, or rectal valves, which prevent feces from being passed along with flatus (gas).
The last subdivision of the large intestine is the anal canal. About 3 cm long, it begins where the rectum passes through the levator ani, the muscle that forms the pelvic floor. A portion of the levator ani is responsible for maintaining the anorectal angle, an acute angle between the anus and the rectum that contributes to fecal continence. The anal canal lies entirely external to the abdominopelvic cavity in the perineum. Internally, the superior half of the anal canal contains longitudinal folds of mucosa, the anal columns. These columns contain the terminal portions of the superior rectal artery and vein (the hemorrhoidal vessels). Neighboring anal columns join each other inferiorly at crescent-shaped transverse folds called anal valves. The pockets just superior to these valves are anal sinuses, which release mucus when they are compressed by feces, providing lubrication that eases fecal passage during defecation. The horizontal line along which the anal valves lie is called the pectinate (“comb-shaped”) line. Because the mucosa superior to this line is innervated by visceral sensory fibers, it is relatively insensitive to pain. Inferior to the pectinate line, however, the mucosa is sensitive to pain because it is innervated by somatic nerves. The wall of the anal canal contains two sphincter muscles: an internal anal sphincter of smooth muscle and an external anal sphincter of skeletal muscle. The former is a thickening of the circular layer of the muscularis, whereas the latter is a distinct muscle. The external sphincter contracts voluntarily to inhibit defecation, whereas the internal sphincter contracts involuntarily, both to prevent feces from leaking from the anus between defecations and to inhibit defecation during emotional stress. During toilet training, children learn to control the external anal sphincter.
Bowel obstruction diagnosis
Patients should be asked about their history of abdominal neoplasia (cancer), hernia or hernia repair, and inflammatory bowel disease, because these conditions increase the risk of bowel obstruction. The hallmarks of bowel obstruction include colicky abdominal pain, nausea and vomiting, abdominal distension, and a cessation of flatus and bowel movements. It is important to differentiate between true mechanical obstruction and other causes of these symptoms (Table 2). Distal obstructions allow for a greater intestinal reservoir, with pain and distension more marked than emesis, whereas patients with proximal obstructions may have minimal abdominal distension but marked emesis. The presence of hypotension and tachycardia is an indication of severe dehydration. Abdominal palpation may reveal a distended, tympanitic abdomen; however, this finding may not be present in patients with early or proximal obstruction. Auscultation in patients with early obstruction reveals high-pitched bowel sounds, whereas those with late obstruction may present with minimal bowel sounds as the intestinal tract becomes hypotonic.
Table 4. Differential Diagnosis of Abdominal Pain, Distension, Nausea, and Cessation of Flatus and Bowel Movements
| Alternate diagnosis | Clues |
|---|---|
| Ascites | Acute liver failure, history of hepatitis or alcoholism |
| Medications (e.g., tricyclic antidepressants, narcotics) | Review of medications; diagnosis of exclusion |
| Mesenteric ischemia | History of peripheral vascular disease, hypercoagulable state, or postprandial abdominal angina; recent use of vasopressors |
| Perforated viscus/intra-abdominal sepsis | Fever, leukocytosis, acute abdomen, free air on imaging |
| Postoperative paralytic ileus | Recent abdominal surgery with no postoperative flatus or bowel movement |
| Pseudo-obstruction (Ogilvie syndrome) | Acutely dilated large intestine, history of intestinal dysmotility, diabetes mellitus, scleroderma |
Tests and procedures used to diagnose bowel obstruction include:
- Physical exam. Your doctor will ask about your medical history and your symptoms. He or she will also do a physical exam to assess your situation. The doctor may suspect intestinal obstruction if your abdomen is swollen or tender or if there’s a lump in your abdomen. He or she may listen for bowel sounds with a stethoscope.
- Laboratory tests. Laboratory evaluation of patients with suspected bowel obstruction should include a complete blood count and metabolic panel. Hypokalemic, hypochloremic metabolic alkalosis may be noted in patients with severe emesis. Elevated blood urea nitrogen levels are consistent with dehydration, and hemoglobin and hematocrit levels may be increased. The white blood cell count may be elevated if intestinal bacteria translocate into the bloodstream, causing the systemic inflammatory response syndrome or sepsis. The development of metabolic acidosis, especially in a patient with an increasing serum lactate level, may signal bowel ischemia.
- X-ray. To confirm a diagnosis of intestinal obstruction, your doctor may recommend an abdominal X-ray. However, some intestinal obstructions can’t be seen using standard X-rays.
- Computerized tomography (CT). A CT scan combines a series of X-ray images taken from different angles to produce cross-sectional images. These images are more detailed than a standard X-ray, and are more likely to show an intestinal obstruction.
- Ultrasound. When an intestinal obstruction occurs in children, ultrasound is often the preferred type of imaging. In youngsters with an intussusception, an ultrasound will typically show a “bull’s-eye,” representing the intestine coiled within the intestine.
- Air or barium enema. An air or barium enema is basically enhanced imaging of the colon that may be done for certain suspected causes of obstruction. During the procedure, the doctor will insert air or liquid barium into the colon through the rectum. For intussusception in children, an air or barium enema can actually fix the problem most of the time, and no further treatment is needed.
Imaging Tests
The initial evaluation of patients with clinical signs and symptoms of intestinal obstruction should include plain upright abdominal radiography. Radiography can quickly determine if intestinal perforation has occurred; free air can be seen above the liver in upright films or left lateral decubitus films. Radiography accurately diagnoses intestinal obstruction in approximately 60 percent of cases and its positive predictive value approaches 80 percent in patients with high-grade intestinal obstruction. However, plain abdominal films can appear normal in early obstruction and in high jejunal or duodenal obstruction. Therefore, when clinical suspicion for obstruction is high or persists despite negative initial radiography, non-contrast computed tomography (CT) should be ordered.
In patients with small bowel obstruction, supine views show dilation of multiple loops of small bowel, with a paucity of air in the large bowel (Figure 10). Those with large bowel obstruction may have dilation of the colon, with decompressed small bowel in the setting of a competent ileocecal valve. Upright or lateral decubitus films may show laddering air fluid levels (Figure 7). These findings, in conjunction with a lack of air and stool in the distal colon and rectum, are highly suggestive of mechanical intestinal obstruction.
Figure 10. X-ray abdomen – Supine view of the abdomen in a patient with small bowel obstruction. Dilated loops of small bowel are visible (arrows).
Figure 11. X-ray abdomen – Lateral decubitus view of the abdomen, showing air-fluid levels consistent with large bowel obstruction (arrows).
CT Scan
Computed Tomography is appropriate for further evaluation of patients with suspected intestinal obstruction in whom clinical examination and radiography do not yield a definitive diagnosis. CT is sensitive for detection of high-grade obstruction (up to 90 percent in some series) 87 and has the additional benefit of defining the cause and level of obstruction in most patients 88. In addition, CT can identify emergent causes of intestinal obstruction, such as volvulus or intestinal strangulation.
CT findings in patients with bowel obstruction include dilated loops of bowel proximal to the site of obstruction, with distally decompressed bowel. The presence of a discrete transition point helps guide operative planning (Figure 12). Absence of contrast material in the rectum is also an important sign of complete obstruction. For this reason, rectal administration of contrast material should be avoided. A C-loop of distended bowel with radial mesenteric vessels with medial conversion is highly suspicious for intestinal volvulus. Thickened intestinal walls and poor flow of contrast material into a section of bowel suggests ischemia, whereas pneumatosis intestinalis, free intra-peritoneal air, and mesenteric fat stranding suggest necrosis and perforation.
Although CT is highly sensitive and specific for high-grade bowel obstruction, its value diminishes in patients with partial obstruction. In these patients, oral contrast material may be seen traversing the length of the intestine to the rectum, with no discrete area of transition. Fluoroscopy may be of greater value in confirming the diagnosis.
The American College of Radiology recommends non-contrast CT as the initial imaging modality of choice 89. However, because most causes of small bowel obstruction will have systemic manifestations or fail to resolve—necessitating operative intervention—the additional diagnostic value of CT compared with radiography is limited. Radiation exposure is also significant. Therefore, in most patients, CT should be ordered when the diagnosis is in doubt, when there is no surgical history or hernias to explain the etiology, or when there is a high index of suspicion for complete or high-grade obstruction.
Figure 12. CT scan bowel obstruction
Note: Axial computed tomography scan showing dilated, contrast-filled loops of bowel on the patient’s left (yellow arrows), with decompressed distal small bowel on the patient’s right (red arrows). The cause of obstruction, an incarcerated umbilical hernia, can also be seen (green arrow), with proximally dilated bowel entering the hernia and decompressed bowel exiting the hernia.
Contrast fluoroscopy
Contrast studies, such as a small bowel follow-through, can be helpful in the diagnosis of a partial intestinal obstruction in patients with high clinical suspicion and in clinically stable patients in whom initial conservative management was not effective 90. The use of water-soluble contrast material is not only diagnostic, but may also be therapeutic in patients with partial small-bowel obstruction. A randomized controlled trial of 124 patients showed a 74 percent reduction in the need for surgical intervention in patients receiving gastrografin fluoroscopy within 24 hours of initial presentation 91. Contrast fluoroscopy may also be useful in determining the need for surgery; the presence of contrast material in the rectum within 24 hours of administration has a 97 percent sensitivity for spontaneous resolution of intestinal obstruction 92.
There are several variations of contrast fluoroscopy. In the small-bowel follow-through study, the patient drinks contrast material, then serial abdominal radiographs are taken to visualize the passage of contrast through the intestinal tract. Enteroclysis involves naso- or oro-duodenal intubation, followed by the instillation of contrast material directly into the small bowel. Although this study has superior sensitivity compared with small-bowel follow-through 93, it is more labor-intensive and is rarely performed. Rectal fluoroscopy can be helpful in determining the site of a suspected large bowel obstruction.
Ultrasound
In patients with high-grade obstruction, ultrasound evaluation of the abdomen has high sensitivity for intestinal obstruction, approaching 85 percent 94. However, because of the wide availability of CT, it has largely replaced ultrasonography as the first-line investigation in stable patients with suspected intestinal obstruction. Ultrasonography remains a valuable investigation for unstable patients with an ambiguous diagnosis and in patients for whom radiation exposure is contraindicated, such as pregnant women.
Magnetic resonance imaging (MRI)
Magnetic resonance imaging (MRI) may be more sensitive than CT in the evaluation of bowel obstruction 95. MRI enteroclysis, which involves intubation of the duodenum and infusion of contrast material directly into the small bowel, can more reliably determine the location and cause of obstruction 96. However, because of the ease and cost-effectiveness of abdominal CT, MRI remains an investigational or adjunctive imaging modality for intestinal obstruction.
Bowel obstruction treatment
Treatment for intestinal obstruction depends on the cause of your condition, but generally requires hospitalization.
Management of intestinal obstruction is directed at correcting physiologic derangements caused by the obstruction, bowel rest, and removing the source of obstruction. The former is addressed by intravenous fluid resuscitation with isotonic fluid. The use of a bladder catheter to closely monitor urine output is the minimum requirement for gauging the adequacy of resuscitation; other invasive measures, such as arterial canalization or central venous pressure monitoring, can be used as the clinical situation warrants. Antibiotics are used to treat intestinal overgrowth of bacteria and translocation across the bowel wall 97. The presence of fever and leukocytosis should prompt inclusion of antibiotics in the initial treatment regimen. Antibiotics should have coverage against gram-negative organisms and anaerobes, and the choice of a specific agent should be determined by local susceptibility and availability. Aggressive replacement of electrolytes is recommended after adequate renal function is confirmed.
Hospitalization to stabilize your condition
When you arrive at the hospital, the doctors will first work to stabilize you so that you can undergo treatment. This process may include:
- Placing an intravenous (IV) line into a vein in your arm so that fluids can be given
- Putting a nasogastric tube through your nose and into your stomach to suck out air and fluid and relieve abdominal swelling
- Placing a thin, flexible tube (catheter) into your bladder to drain urine and collect it for testing.
Treatment of stable patients with bowel obstruction and a history of abdominal surgery presents a challenge. Conservative management of a high-grade bowel obstruction should be attempted initially, using intestinal intubation and decompression, aggressive intravenous rehydration, and antibiotics.
Caution should be used when clinical and radiologic evidence suggest complete obstruction, because the use of intestinal stimulation can exacerbate the obstruction and precipitate intestinal ischemia.
Conservative management is successful in 40 to 70 percent of clinically stable patients, with a higher success rate in those with partial obstruction 98. Although conservative management is associated with shorter initial hospitalization (4.9 versus 12 days), there is also a higher rate of eventual recurrence (40.5 versus 26.8 percent) 99. With conservative management, resolution generally occurs within 24 to 48 hours. Beyond this time frame, the risk of complications, including vascular compromise, increases. If intestinal obstruction is not resolved with conservative management, surgical evaluation is required 100.
Treating intussusception
A barium or air enema is used both as a diagnostic procedure and a treatment for children with intussusception. If an enema works, further treatment is usually not necessary.
Due to tumors accounting for majority of cases of adults with intussusception, treatment of intussusception in adults is surgical without attempts at hydrostatic reduction. Optimal surgical procedure depends on the anatomic location, present of a lead point, and local factors, such as edema, inflammation, and ischemia of involved bowel. While resection is the treatment of colic andenterocolic intussusception, the choice in enteric type i.e. attempt at operative reduction vs. resection without attempt at reduction, depends on presence of underlying lesion, chances the lesion is malignant, and viability of involved bowel.
Treatment for partial obstruction
If you have an obstruction in which some food and fluid can still get through (partial obstruction), you may not need further treatment after you’ve been stabilized. Your doctor may recommend a special low-fiber diet that is easier for your partially blocked intestine to process. If the obstruction does not clear on its own, you may need surgery to relieve the obstruction.
The inclusion of oral magnesium hydroxide, simethicone, and probiotics decreased the length of hospitalization in a randomized controlled trial of 144 patients with partial small bowel obstructions (number needed to treat = 7) 101.
Treatment for complete obstruction
If nothing is able to pass through your intestine, you’ll usually need surgery to relieve the blockage. The procedure you have will depend on what’s causing the obstruction and which part of your intestine is affected. Surgery typically involves removing the obstruction, as well as any section of your intestine that has died or is damaged.
Alternatively, your doctor may recommend treating the obstruction with a self-expanding metal stent. The wire mesh tube is inserted into your colon via an endoscope passed through your mouth or colon. It forces open the colon so that the obstruction can clear.
Stents are generally used to treat people with colon cancer or to provide temporary relief in people for whom emergency surgery is too risky. You may still need surgery, once your condition is stable.
Treatment for pseudo-obstruction
If your doctor determines that your signs and symptoms are caused by pseudo-obstruction (paralytic ileus), he or she may monitor your condition for a day or two in the hospital, and treat the cause if it’s known. Paralytic ileus can get better on its own. In the meantime, you’ll likely be given food through a nasal tube or an IV to prevent malnutrition.
If paralytic ileus doesn’t improve on its own, your doctor may prescribe medication that causes muscle contractions, which can help move food and fluids through your intestines. If paralytic ileus is caused by an illness or medication, the doctor will treat the underlying illness or stop the medication. Rarely, surgery may be needed to remove part of the intestine.
In cases where the colon is enlarged, a treatment called decompression may provide relief. Decompression can be done with colonoscopy, a procedure in which a thin tube is inserted into your anus and guided into the colon. Decompression can also be done through surgery.
Bowel obstruction surgery
The decision to perform surgery for intestinal obstruction can be difficult. Peritonitis, clinical instability, or unexplained leukocytosis or acidosis are concerning for abdominal sepsis, intestinal ischemia, or perforation; these findings mandate immediate surgical exploration. Patients with an obstruction that resolves after reduction of a hernia should be scheduled for elective hernia repair, whereas immediate surgery is required in patients with an irreducible or strangulated hernia. Stable patients with a history of abdominal malignancy or high suspicion for malignancy should be thoroughly evaluated for optimal surgical planning. Abdominal malignancy can be treated with primary resection and reconstruction or palliative diversion, or placement of venting and feeding tubes.
Perforated bowel
Perforated bowel is a hole in the wall of the small intestine (small bowel perforation) or large intestine (large bowel perforation), which is a life-threatening condition associated with mortality ranging from 30 to 50% 102, 103, 104, 105, 106. Perforation of the small intestine or large intestine causes the intestinal contents to leak into your abdomen. These contents can range from highly acidic gastric contents in more proximal bowel perforation, to fecal material from a more distal area of perforation. These contents can cause a severe infection called peritonitis, which is a life-threatening emergency that needs emergency surgery to repair the hole, stop the bleeding, remove the obstruction, infection, or ischemia. Symptoms of perforated bowel may include sudden and severe constant abdominal pain, nausea and vomiting, fever or chills, swelling and bloating of the abdomen, and inability to pass wind or stool and in severe cases sepsis (a life-threatening emergency that happens when your body’s response to an infection damages vital organs) and shock (a life-threatening condition that occurs when your body doesn’t get enough blood flow).
Your intestines can be damaged and perforated by a range of conditions, including 102, 103, 107, 108, 109, 110, 111, 112, 113, 114, 115:
- trauma, injury (e.g., blunt force trauma such as from a car accident or penetrating injuries such as from a knife or gunshot wound) or swallowing a foreign object
- bowel obstruction
- severe constipation or fecal impaction (e.g., stercoral perforation)
- medical procedures (e.g., after digestive surgery, colonoscopy or endoscopy). The overall incidence of perforation from colonoscopy has been reported, on average, around 2% with higher rates during colonoscopy requiring therapeutic interventions 116
- diverticulitis and inflammatory bowel disease such as Crohn’s disease or ulcerative colitis
- burst appendix or appendicitis
- a tumor that grows through the wall of your intestine (e.g., colorectal cancer or colon perforation from obstruction by distal colon cancer or extracolonic tumor)
- vascular disorders e.g., mesenteric ischemia, ischemic colitis or connective tissue disorders
- chemotherapy drugs
- radiation therapy to your pelvis or abdomen
- ingestion of caustic substances
- drug-induced ulcers (e.g., non-steroidal anti-inflammatory drugs (NSAIDs) and corticosteroids are the most common)
- forceful vomiting
- bowel perforation in neonates is often due to necrotizing enterocolitis
In children, bowel perforation is most likely to follow abdominal trauma 102. The incidence of bowel perforation is 1% to 7% in pediatric trauma patients 102.
In adults, ulcerative disease represents the most common cause of bowel perforation, with duodenal ulcers causing 2- to 3-times the rate of perforation than gastric ulcers do 102. Perforation secondary to diverticular disease represents up to 15% of cases. In the elderly population, perforated appendicitis represents the most common cause of perforation 102.
It’s important to get treatment fast for perforated bowel. To diagnose a perforated bowel, a doctor talks with you about your medical history and gives you a physical exam. Your symptoms alone may be enough for your doctor to diagnose a perforated bowel.
If more tests are needed to confirm a diagnosis, your doctor may suggest:
- Abdominal and upright chest x-rays are quick and cheap and can identify even small amounts of pneumoperitoneum. X-rays of the chest or abdomen which may show air in your abdominal cavity. This is called free air. It is a sign of a perforation. If the esophagus is perforated free air can be seen in the mediastinum (the space between your lungs in the chest that contains the heart, trachea and esophagus) around your heart and in your chest. You also may have a test that uses sound waves to make images inside your body, called ultrasound.
- Colonic perforation tends to result in a greater amount of pneumoperitoneum than free fluid 117
- Upper gastrointestinal tract perforation tends to present with a relatively large volume of free fluid and less pneumoperitoneum 117
- The presence of pneumoperitoneum in the periportal region is also suggestive of upper gastrointestinal perforation 118
- CT scan of the abdomen and pelvis is the most sensitive and specific test to diagnose a perforation and ascertain the most likely cause 119. Disease processes such as diverticulitis, appendicitis, and bowel obstructions can be readily identified on CT scan. The use of intravenous contrast is recommended to aid in visualizing potential areas of ischemia. Complications from a perforation such as an abscess and secondary bowel obstruction can also be identified with CT scan and guide management accordingly.
- Blood tests. A sample of your blood may be taken to see if you have an increase in disease-fighting white blood cells. This is usually a sign of an infection or inflammation. You also might have a blood culture test to find out if bacteria are in your blood.
- Peritoneal fluid analysis. In this test, a thin needle is used to take a sample of the fluid in your peritoneum. You’re more likely to have this test if you get peritoneal dialysis or if you have fluid in your abdomen from liver disease. An increased white blood cell count in this fluid usually points to an infection or inflammation. A culture of the fluid may be used to spot bacteria.
- A procedure may help find the area of the perforation, such as an upper endoscopy (EGD) or a colonoscopy.
- In children, the preferred primary test is ultrasound given its ease and lack of radiation exposure. However, ultrasound is especially dependent on the experience level of the operator. If necessary, secondary testing such as x-ray, MRI, and CT are reasonable options 120.
Perforated bowel treatment most often involves emergency surgery to repair the hole 121. Sometimes, a small part of the intestine must be removed. One end of the intestine may be brought out through an opening called stoma made in your abdominal wall. This is called a colostomy or ileostomy. A drain from the abdomen or other organ may also be needed. In rare cases, people can be treated with antibiotics alone if the perforation has closed. Antibiotics clear out the infection and keep it from spreading. The type of antibiotic you’ll need and how long you’ll have to take it will vary. It depends on how serious your condition is and the kind of peritonitis you have. This can be confirmed by a physical exam, blood tests, CT scan, and x-rays.
A perforation from a colonoscopy may sometimes be closed during the procedure without surgery.
Contained or controlled bowel perforations can be managed conservatively with interventional radiology guided drainage of fluid collections 122. However, the failure of conservative management with persistence of symptoms and/or development of sepsis necessitate surgical intervention.
Historically, laparotomy has been the intervention of choice for acute abdomen; recently, however, laparoscopic exploration has emerged as a viable option to identify and treat the source of perforation 123. Resection or repair of the perforated site with or without drainage and diversion is usually undertaken. Duodenal perforations, on the other hand, are generally treated with omental patch repair without resection. Risks and benefits of surgery, particularly amongst elderly patient and those with medical conditions, should be thoroughly discussed before offering surgical intervention 124.
Surgery is successful most of the time. Your health status before the perforation occurs best predicts your outcome (prognosis). However, the outcome (prognosis) will depend on how severe the perforation is, and for how long it was present before treatment. The presence of other illnesses, septic shock and your age can also affect how well you will do after treatment.
Figure 13. Bowel perforation with massive pneumoperitoneum
Footnotes: Bowel perforation with massive pneumoperitoneum evident by the excessive free gas in the abdominal cavity, including the bilateral subphrenic spaces and surrounding the edges of the liver (hepatic edge sign). Bowel double wall sign or Rigler sign is well-demonstrated. Some of the bowel loops are significantly dilated. Gas-fluid levels are seen in the dilated lower abdominal loops. No rectal gas is seen.
[Source 125 ]Figure 14. Small bowel perforation
Footnotes: Traumatic small bowel perforation in a construction worker where a metal bar fell on his abdomen 10 days prior. Initial CT was reported to be normal. Now peritonitic. 12 cm gas and fluid-filled walled-off collection in the midline of the abdomen largely occupying the small bowel mesentery. Suspicion of occasional bleb of intraperitoneal gas adjacent to the collection. Dilated fluid-filled small bowel distally in the pelvis. Small volume pelvic free fluid. Small bowel loops laterally in the left side of the abdomen indicating an element of malrotation. The solid organs are normal. Normal large bowel.
Comment: Enlarged intra-abdominal fluid collection, appears related to the mesentery and small bowel.
[Source 126 ]Figure 15. Large bowel obstruction and perforation
Footnotes: 75 year old male with short history of abdominal distension and no motion passed for 2 days. (Top image) Abdominal X-ray showing the large bowel is grossly dilated down to the level of a cut-off at the junction of the distal descending and sigmoid colon. The small bowel is moderately dilated. (Bottom image) Non contrast CT scan due to renal impairment showing 4.5cm stenosing tumor at the junction of the sigmoid and descending colon with resultant dilatation of the large bowel upto 9cm. Blebs of intramural gas throughout the colon. The distal small bowel is dilated due to a incompetent ileocecal valve. Multiple foci of pneumoperitoneum in the mid and upper abdomen. No overt infradiaphrgamatic nodes. At least two right lower lobe lung nodules, the largest 8mm.
[Source 127 ]Perforated bowel can be life-threatening if you don’t get medical treatment quickly. See a doctor right away if you have severe pain or tenderness of your abdomen, bloating or a feeling of fullness along with:
- Fever.
- Upset stomach and vomiting.
- Reduced urine.
- Thirst.
- Not able to pass stool or gas.
Perforated bowel also might happen after a burst appendix or a serious injury to your abdomen.
- Get medical help right away if you have severe abdominal pain. Your abdominal pain may feel so bad that you can’t sit still or find a comfortable position.
- Call your local emergency number or get emergency medical care if you have severe belly pain after an accident or injury.
Perforated bowel causes
Bowel perforation results from a destruction of the mucosal layers of the intestinal tract resulting in the spilling of air and digestive contents into the peritoneal cavity. Your intestines can be damaged and perforated by a range of conditions, including 128, 107, 108, 109, 110, 111, 112, 113, 114, 115:
- Bowel obstruction (both small and large intestine)
- Bowel ischemia e.g., mesenteric ischemia, ischemic colitis or connective tissue disorders
- Severe ulcer disease
- Trauma, injury (e.g., blunt force trauma such as from a car accident or penetrating injuries such as from a knife or gunshot wound) or swallowing a foreign object
- Severe constipation or fecal impaction
- Medical procedures (e.g., after digestive surgery, colonoscopy or endoscopy). The overall incidence of perforation from colonoscopy has been reported, on average, around 2% with higher rates during colonoscopy requiring therapeutic interventions 116
- Diverticulitis and inflammatory bowel disease such as Crohn’s disease or ulcerative colitis
- Burst appendix or appendicitis
- Gastrointestinal tumors that grow through the wall of your intestine (e.g., colorectal cancer or colon perforation from obstruction by distal colon cancer or extracolonic tumor)
- Chemotherapy drugs
- Radiation therapy to your pelvis or abdomen
- Ingestion of caustic substances
- Drug-induced ulcers (e.g., non-steroidal anti-inflammatory drugs (NSAIDs) and corticosteroids are the most common)
- Forceful vomiting
- Bowel perforation in neonates is often due to necrotizing enterocolitis
Upper gastrointestinal perforation (stomach and duodenum) is most commonly caused by peptic ulcer disease with severe epigastric or back pain, with acute onset 102, 103. Sometimes there are chronic symptoms leading up to the perforation event, such as dyspepsia, bloating, nausea, and early satiety 112. Less commonly, cancer or traumatic perforation are possibilities. Imaging usually shows upper abdominal free air and possible leakage of contents into the peritoneal cavity. Usage of oral contrast can be seen extravasating soon after ingestion. Acute onset of periumbilical pain, nausea, vomiting, and decreased bowel function are symptoms of bowel obstruction 103. Imaging suggesting free intraperitoneal air with dilated small or large bowel can signify this as a source of perforation 103. Presence of an incarcerated hernia, history of abdominal surgery, or findings of intussusception on imaging sometimes is present in these cases 129.
Large intestine perforation should be considered with a history of left lower quadrant or history of diverticulitis also usually with decreased stool output 102, 103. Colon cancer is a consideration also, especially with lack of endoscopy screening history. Imaging typically shows free air located near the area of perforation with possible abscess formation present due to the leakage of stool into the peritoneal cavity 111. Rarely, free intraperitoneal air can be caused by benign pneumatosis intestinalis (a very rare condition where multiple gaseous cysts form in the wall of the small or large intestines) unrelated to ischemia and can be managed without surgical intervention 130.
In children, bowel perforation is most likely to follow abdominal trauma 102. The incidence of bowel perforation is 1% to 7% in pediatric trauma patients 102.
In adults, ulcerative disease represents the most common cause of bowel perforation, with duodenal ulcers causing 2- to 3-times the rate of perforation than gastric ulcers do 102. Perforation secondary to diverticular disease represents up to 15% of cases. In the elderly population, perforated appendicitis represents the most common cause of perforation 102.
Perforated bowel pathophysiology
There are 4 mechanisms that can lead to a intestinal tract perforation. A thorough understanding of these mechanisms is critical to guide the appropriate workup and management 103:
- Ischemia (bowel obstruction, necrosis)
- Numerous causes can lead to ischemia and perforation. In the case of bowel obstruction (small or large intestine), the physical distention of the bowel wall results in decreased perfusion 109. This ultimately leads to full thickness wall necrosis and subsequent perforation. Bowel obstruction due to adhesions is more common in patients with a prior history of surgery, but can also result from herniation and strangulation, inflammation, tumors, and foreign bodies. Decreased end-organ perfusion secondary to thrombotic or embolic disease can also result in full-thickness ischemia and perforation. This is more common in older patients, particularly those with a history of smoking, coronary artery disease, or clotting disorders 131.
- Infection (appendicitis, diverticulitis)
- The most common infectious causes of perforation are appendicitis and diverticulitis. Appendicitis can be considered at any age, whereas diverticulitis is more common beyond middle age 111. Both disease processes are usually presumed to be the result of entrapped fecal material in a blind ending structure, leading to increased intraluminal pressure, stasis, and infection leading to a localized abscess or frank perforation. Inflammatory diseases of the bowel, such as Crohn disease and ulcerative colitis can also lead to perforation, especially Crohn’s, which is characterized by full thickness inflammation of the bowel wall 132.
- Erosion (cancer, ulcerative disease)
- Erosive diseases, such as the local invasion of the wall of a viscus by a tumor or ulcerative disease, can also cause perforation. Stercoral perforation is a rare tear in the colon wall caused by hardened feces that is increasingly being recognized as a complication of severe constipation. In peptic ulcer disease, there is direct erosion through the layers of the bowel wall by the ulcer itself, usually due to Helicobacter pylori infection, acid overproduction, or lack of acid protective mechanisms 112. Tumors of the gastrointestinal (GI) tract are most commonly adenocarcinomas, which arise from the mucosa and, in advanced stages, can result in transmural invasion and perforation 133.
- Physical disruption (trauma, iatrogenic injury)
In addition to the mechanisms that can lead to a intestinal tract perforation, the variation in bacterial flora between the upper and lower intestinal tract must also be considered. For example, upper intestinal perforations proximal to the ligament of Trietz result in significantly less bacterial contamination than distal colonic perforations. In the treatment of distal perforations, antibiotics must include gram-negative and anaerobic coverage 135.
Perforated bowel prevention
People will often have a few days of pain before the intestinal perforation occurs. If you have pain in the abdomen, see your doctor right away. Treatment is much simpler and safer when it is started before the perforation occurs.
Perforated bowel signs and symptoms
Perforation of the intestine or other organs causes the intestinal contents to leak into your abdomen. This can lead to peritonitis and eventually sepsis if left untreated.
Perforated bowel symptoms may include:
- Severe abdominal pain
- Chills
- Fever
- Nausea
- Vomiting
- Shock
Perforated bowel signs and symptoms varies: esophageal perforations can present with non-specific symptoms such as acute chest pain, painful swallowing (odynophagia) and vomiting 106, gastroduodenal perforations typically present with acute abdominal pain 105, 136, whereas colonic perforations tend to follow a slower progression course, presenting with secondary bacterial peritonitis or localised abscess formation 105, 137. A subset of patients exhibits delayed symptoms, abscess formation that mimics an abdominal mass, or with sepsis 136.
Almost all patients with bowel perforation experience some element of abdominal pain, and this is usually accompanied by nausea, vomiting, decreased bowel function, or fever 103. Details about the symptoms including the length of time, prior episodes, recent procedures such as endoscopic retrograde cholangiopancreatography (ERCP) and colonoscopy and exacerbating and relieving factors can be crucial in determining the cause of the perforation 138, 139. A family history of cancer and a personal history of colonoscopy can be important to determine the likelihood of occult cancer or inflammatory bowel disease (IBD).
Perforated bowel complications
Complications caused by an intestinal perforation can be related to the disease process that caused it or the treatments given. Even after surgery for perforated bowel, infection is the most common complication. Infections can be either inside the abdomen such as abdominal abscess (a collection of pus and infected fluid in the abdomen) or peritonitis (inflammation of the lining of your belly or abdomen called the peritoneum), or throughout your whole body. Body-wide infection is called sepsis. Sepsis can be very serious and can lead to shock, organ failure and death.
Early complications
- Hemodynamic instability leading to hypoperfusion, shock, and multi-organ system failure, infection (whether local abscess formation, peritonitis, or systemic bacteremia)
Late complications
- Delayed wound healing, postoperative adhesions leading to bowel obstruction, fistula formation, and hernias 121.
Perforated bowel diagnosis
To diagnose a perforated bowel, a doctor talks with you about your medical history and gives you a physical exam. Your symptoms alone may be enough for your doctor to diagnose a perforated bowel.
If more tests are needed to confirm a diagnosis, your doctor may suggest:
- Abdominal and upright chest x-rays are quick and cheap and can identify even small amounts of pneumoperitoneum. X-rays of the chest or abdomen which may show air in your abdominal cavity. This is called free air. It is a sign of a perforation. If the esophagus is perforated free air can be seen in the mediastinum (the space between your lungs in the chest that contains the heart, trachea and esophagus) around your heart and in your chest. You also may have a test that uses sound waves to make images inside your body, called ultrasound.
- Upright chest radiography (50% to 70% sensitive) can help detect free intraperitoneal air below the diaphragm suggestive of bowel perforation 102. The likelihood of diagnosing free air is higher if the patient has been sitting upright for at least 15 minutes prior to the chest radiography 102. Lateral decubitus films can be used if the patient is unable to sit upright.
- Colonic perforation tends to result in a greater amount of pneumoperitoneum than free fluid 117.
- Upper gastrointestinal tract perforation tends to present with a relatively large volume of free fluid and less pneumoperitoneum 117.
- The presence of pneumoperitoneum in the periportal region is also suggestive of upper gastrointestinal perforation 118.
- Up to 40 percent of patients will demonstrate greater than 2 cm of free gas at 24 hours post laparoscopy, without any clinical evidence of bowel perforation 102. After laparotomy, free intra-abdominal gas often may be present for a longer duration postoperatively (up to one week), but the volume should be gradually decreased 102.
- CT scan of the abdomen and pelvis is the most sensitive and specific test to diagnose a perforation and ascertain the most likely cause 119. Disease processes such as diverticulitis, appendicitis, and bowel obstructions can be readily identified on CT scan. The use of intravenous contrast is recommended to aid in visualizing potential areas of ischemia. Complications from a perforation such as an abscess and secondary bowel obstruction can also be identified with CT scan and guide management accordingly.
- Blood tests. A sample of your blood may be taken to see if you have an increase in disease-fighting white blood cells. This is usually a sign of an infection or inflammation. You also might have a blood culture test to find out if bacteria are in your blood.
- Peritoneal fluid analysis. In this test, a thin needle is used to take a sample of the fluid in your peritoneum. You’re more likely to have this test if you get peritoneal dialysis or if you have fluid in your abdomen from liver disease. An increased white blood cell count in this fluid usually points to an infection or inflammation. A culture of the fluid may be used to spot bacteria.
- A procedure may help find the area of the perforation, such as an upper endoscopy (EGD) or a colonoscopy.
- In children, the preferred primary test is ultrasound given its ease and lack of radiation exposure. However, ultrasound is especially dependent on the experience level of the operator. If necessary, secondary testing such as x-ray, MRI, and CT are reasonable options 120.
Perforated bowel treatment
Once the initial assessment is complete and bowel perforation is suspected, management can ensue. Many, but not all causes of perforated bowel, require surgery to repair the hole 121. However, all cases should be evaluated by a surgeon 107. Sometimes, a small part of the intestine must be removed. One end of the intestine may be brought out through an opening called stoma made in your abdominal wall. This is called a colostomy or ileostomy. A drain from the abdomen or other organ may also be needed. In rare cases, people can be treated with antibiotics alone if the perforation has closed. Antibiotics clear out the infection and keep it from spreading. The type of antibiotic you’ll need and how long you’ll have to take it will vary. It depends on how serious your condition is and the kind of peritonitis you have. This can be confirmed by a physical exam, blood tests, CT scan, and x-rays.
A perforation from a colonoscopy may sometimes be closed during the procedure without surgery.
Other treatments depend on your symptoms and may include:
- Pain medications.
- Intravenous fluids given through your vein.
- Oxygen.
- In some cases, a blood transfusion.
For both operative and nonoperative patients, initial treatment includes bowel rest, intravenous fluids, intravenous broad-spectrum antibiotics, and frequent abdominal examinations. Instances that are accompanied by sepsis and peritonitis are more likely to require surgery, whereas those that do not need surgery may be amenable to conservative management 140, 141.
Contained or controlled bowel perforations can be managed conservatively with interventional radiology guided drainage of fluid collections 122. However, the failure of conservative management with persistence of symptoms and/or development of sepsis necessitate surgical intervention.
Historically, laparotomy has been the intervention of choice for acute abdomen; recently, however, laparoscopic exploration has emerged as a viable option to identify and treat the source of perforation 123. Resection or repair of the perforated site with or without drainage and diversion is usually undertaken. Duodenal perforations, on the other hand, are generally treated with omental patch repair without resection. Risks and benefits of surgery, particularly amongst elderly patient and those with medical conditions, should be thoroughly discussed before offering surgical intervention 124.
Perforated bowel prognosis
Short- and long-term prognoses of a patient with bowel perforation depend on multiple factors. For instance, your age, medical conditions, benign or malignant cause, and tolerance to treatment are important considerations when discussing prognosis 103, 142. Since surgery is commonly necessary, patients who are unable to tolerate or choose not to undergo surgery when it is required may have a worse prognosis 142.
Risks of abdominal infection, bleeding, potential anastomotic leakage (a serious complication that occurs when the ends of a surgically connected intestines leak), hernia formation from surgical healing 103. Other risks include heart and lung (cardiopulmonary) complications, thromboembolic events (a condition in which a blood clot breaks off from its original site and travels through the bloodstream to obstruct a blood vessel, causing tissue ischemia and organ damage), cardiovascular events, and possible prolonged need for ventilator support must also be discussed as well as expected recovery and possible level of function.
Nationwide mortality (dying) from emergency general surgery cases is 5.0% for patients 65–69 years of age, but increases steadily to 20.4% for patients aged 90 and older 143. Serious morbidity (illness) for this patient group is also high, with a reported range from 17–83% 144, 145, 146, 147. These factors must be discussed candidly with patients and families before surgery, in the elderly especially, to determine their expectations and desires 148.
Colon cancer
Colon cancer also known as bowel cancer or colorectal cancer (a term that combines colon cancer and rectal cancer which begins in the rectum), is cancer of the large intestine (colon or large bowel), which is the final part of your digestive tract. The colon (large bowel) is the main part of the large intestine and is about 5 feet long. The rectum and anal canal make up the last part of the large intestine and are about 6 to 8 inches long. The anal canal ends at the anus (the opening of the large intestine to the outside of the body). Cancer that begins in the colon is called colon cancer, and cancer that begins in the rectum is called rectal cancer. Cancer that starts in either of these organs may also be called colorectal cancer. Depending on where the cancer starts, colon cancer is sometimes called colon or rectal cancer or colorectal cancer. Colon cancer and rectal cancer are often grouped together because they have many features in common. The large intestine (colon) extends from the distal end of the ileum to the anus, a distance of approximately 1.5 m in adults (5 ft) long and 6.5 cm (2.5 in.) in diameter. Together, the rectum and anal canal make up the last part of the large intestine and are about 6-8 inches long. The anal canal ends at the anus (the opening of the large intestine to the outside of the body). Most cases of colon cancer begin as small, noncancerous (benign) clumps of cells called adenomatous polyps. Over time some of these polyps can become colon cancers. Polyps may be small and produce few, if any, symptoms. For this reason, doctors recommend regular screening tests to help prevent colon cancer by identifying and removing polyps before they turn into cancer.
The chance of changing into a cancer depends on the kind of polyp. The 2 main types of polyps are:
- Adenomatous polyps (adenomas): These polyps sometimes change into cancer. Because of this, adenomas are called a pre-cancerous condition.
- Hyperplastic polyps and inflammatory polyps: These polyps are more common, but in general they are not pre-cancerous.
Other polyp characteristics that can increase the chances a polyp may contain cancer or increase someone’s risk of developing colorectal cancer besides the type include the size (larger than 1 cm), the number found (more than two), and if dysplasia is seen in the polyp after it is removed.
Dysplasia, another pre-cancerous condition, is an area in a polyp or in the lining of the colon or rectum where the cells look abnormal (but not like true cancer cells).
If cancer forms in a polyp, it can eventually begin to grow into the wall of the colon or rectum.
The wall of the colon and rectum is made up of several layers. Colorectal cancer starts in the innermost layer (the mucosa) and can grow outward through some or all of the other layers. When cancer cells are in the wall, they can then grow into blood vessels or lymph vessels (tiny channels that carry away waste and fluid). From there, they can travel to nearby lymph nodes or to distant parts of the body.
The stage (extent of spread) of a colorectal cancer depends on how deeply it grows into the wall and if it has spread outside the colon or rectum.
It can take as many as 10 to 15 years for a polyp to develop into colorectal cancer. Regular screening can often prevent colorectal cancer by finding and removing polyps before they have the chance to turn into cancer. Screening can also often find colorectal cancer early, when it might be easier to treat.
Excluding skin cancers, colorectal cancer is the third most common cancer diagnosed in both men and women in the United States. The American Cancer Society’s estimates for the number of colorectal cancer cases in the United States for 2025 are 149, 150:
- About 107,320 new cases of colon cancer (54,510 in men and 52,810 in women)
- About 46,950 new cases of rectal cancer (27,950 in men and 19,000 in women)
- The rate of people being diagnosed with colon or rectal cancer each year has dropped overall since the mid-1980s, mainly because more people are getting screened and changing their lifestyle-related risk factors. From 2012 to 2021, incidence rates dropped by about 1% each year. But this downward trend is mostly in older adults. In people younger than 50 years of age, rates have increased by 2.4% per year from 2012 to 2021.
- In the United States, colorectal cancer is the third-leading cause of cancer-related deaths in men and the fourth leading cause in women, but it’s the second most common cause of cancer deaths when numbers for men and women are combined. .
- Deaths: Colorectal cancer is expected to cause about 52,900 deaths during 2025 (colon and rectal cancers combined)
- Overall, the lifetime risk of developing colorectal cancer is about 1 in 24 for men (4.2%) and 1 in 26 (3.8%) for women. However, each person’s risk might be higher or lower than this, depending on their risk factors for colorectal cancer.
- About 4.2% of Americans are expected to develop colorectal cancer within their lifetime, and the lifetime risk of dying from colorectal cancer is 1.7% 151. Age-specific incidence and mortality rates show that most colorectal cancer cases are diagnosed after age 54 years and 78% of cases occur in patients aged 55 years and older; about 15% of colorectal cancer cases occur in patients aged 45 to 54 years 150, 152.
- Colorectal cancer is the second leading cause of cancer death in the United States. The death rate was 13.4 per 100,000 men and women per year based on 2015–2019 deaths, age-adjusted.
- Colorectal cancer represents 7.9% of all new cancer cases in the U.S.
- Colorectal cancer deaths represents 8.6% of all cancer deaths in the U.S.
- Rate of New Cases and Deaths per 100,000: The rate of new cases of colorectal cancer was 36.5 per 100,000 men and women per year. The death rate was 12.9 per 100,000 men and women per year. These rates are age-adjusted and based on 2017–2021 cases and 2018–2022 deaths.
- Lifetime Risk of Developing colorectal cancer: Approximately 4.0 percent of men and women will be diagnosed with colorectal cancer at some point during their lifetime, based on 2018–2021 data.
- In 2021, there were an estimated 1,392,445 people living with colorectal cancer in the United States.
- 5-Year Relative Survival is 65%. Relative survival is an estimate of the percentage of patients who would be expected to survive the effects of their cancer. It excludes the risk of dying from other causes. Because survival statistics are based on large groups of people, they cannot be used to predict exactly what will happen to an individual patient. No two patients are entirely alike, and treatment and responses to treatment can vary greatly.
Overall, the lifetime risk of developing colorectal cancer is about 1 in 24 (4.2%) for men and 1 in 26 (3.8%) for women. This risk is slightly lower in women than in men. A number of other factors (described in Colorectal Cancer Risk Factors) can also affect your risk for developing colorectal cancer.
Colorectal cancer is the second leading cause of cancer death when numbers for both men and women are combined. The death rate (the number of deaths per 100,000 people per year) from colorectal cancer has been dropping in older adults for several decades. It is expected to cause about 52,900 deaths during 2025. One reason for this is that colorectal polyps are now more often found by screening and removed before they can develop into cancers. Screening also results in many colorectal cancers being found earlier, when they are likely to be easier to treat. In addition, treatments for colorectal cancer have improved over the last few decades. In people under 55, however, death rates have been increasing about 1% per year since the mid-2000s.
When colorectal cancer is found at an early stage before it has spread, the 5-year relative survival rate is about 90%. But only about 4 out of 10 colorectal cancers are found at this early stage. When cancer has spread outside the colon or rectum, survival rates are lower.
Unfortunately, only a little more than half of people who should get tested for colorectal cancer get the tests that they should. This may be due to things like lack of public and health care provider awareness of screening options, costs, and health insurance coverage issues.
Cancer of the colon is a highly treatable and often curable disease when localized to the bowel. Surgery is the primary form of treatment and results in cure in approximately 50% of the patients. Recurrence following surgery is a major problem and is often the ultimate cause of death.
Colon cancer signs and symptoms
Many people with colon cancer experience no symptoms in the early stages of the disease. When symptoms appear, they’ll likely vary, depending on the cancer’s size and location in your large intestine. Many of the symptoms of colon cancer can also be caused by something that isn’t cancer, such as infection, hemorrhoids, irritable bowel syndrome, or inflammatory bowel disease.
Colorectal cancer might not cause symptoms right away, but if it does, it may cause one or more of these symptoms:
- A change in bowel habits, such as diarrhea, constipation, or narrowing of the stool, that lasts for more than a few days
- A feeling that you need to have a bowel movement that’s not relieved by having one
- Rectal bleeding with bright red blood
- Blood in the stool, which might make the stool look dark brown or black
- Persistent abdominal discomfort, such as cramps, gas or pain
- A feeling that your bowel doesn’t empty completely
- Weakness or fatigue
- Unexplained weight loss
Signs of colon cancer include blood in the stool or a change in bowel habits.
These and other signs and symptoms may be caused by colon cancer or by other conditions. Check with your doctor if you have any of the following:
- A change in bowel habits.
- Blood (either bright red or very dark) in the stool.
- Diarrhea, constipation, or feeling that the bowel does not empty all the way.
- Stools that are narrower than usual.
- Frequent gas pains, bloating, fullness, or cramps.
- Weight loss for no known reason.
- Feeling very tired.
- Vomiting.
Colorectal cancers can often bleed into the digestive tract. Sometimes the blood can be seen in the stool or make it look darker, but often the stool looks normal. But over time, the blood loss can build up and can lead to low red blood cell counts (anemia). Sometimes the first sign of colorectal cancer is a blood test showing a low red blood cell count.
Some people may have signs that the cancer has spread to the liver with a large liver felt on exam, jaundice (yellowing of the skin or whites of the eyes), or trouble breathing from cancer spread to the lungs.
Many of these symptoms can be caused by conditions other than colorectal cancer, such as infection, hemorrhoids, or irritable bowel syndrome. Still, if you have any of these problems, it’s important to see your doctor right away so the cause can be found and treated, if needed.
If you notice any persistent symptoms that worry you, make an appointment with your doctor.
Talk with your doctor about when to begin colon cancer screening. Guidelines generally recommend that colon cancer screenings begin around 50. Your doctor may recommend more frequent or earlier screening if you have other risk factors, such as a family history of the disease.
Colon cancer causes
In most cases, it’s not clear what causes colon cancer. Doctors know that colon cancer occurs when healthy cells in the colon develop errors in their genetic blueprint, the DNA. A cell’s DNA contains a set of instructions that tell a cell what to do.
Healthy cells grow and divide in an orderly way to keep your body functioning normally. But when a cell’s DNA is damaged and becomes cancerous, cells continue to divide — even when new cells aren’t needed. As the cells accumulate, they form a tumor.
With time, the cancer cells can grow to invade and destroy normal tissue nearby. And cancerous cells can travel to other parts of the body to form deposits there (metastasis).
Inherited gene mutations that increase the risk of colon cancer
Inherited gene mutations that increase the risk of colon cancer can be passed through families, but these inherited genes are linked to only a small percentage of colon cancers. Inherited gene mutations don’t make cancer inevitable, but they can increase an individual’s risk of cancer significantly.
The most common forms of inherited colon cancer syndromes are:
- Hereditary nonpolyposis colorectal cancer (HNPCC) also called Lynch syndrome. Hereditary nonpolyposis colorectal cancer increases the risk of colon cancer and other cancers. People with hereditary nonpolyposis colorectal cancer tend to develop colon cancer before age 50. Lynch syndrome (hereditary non-polyposis colon cancer or HNPCC) is caused by changes in genes that normally help a cell repair damaged DNA. A mutation in one of the DNA repair genes like MLH1, MSH2, MSH6, PMS2, and EPCAM, can allow DNA errors to go unfixed. These errors will sometimes affect growth-regulating genes, which may lead to the development of cancer.
- Familial adenomatous polyposis (FAP). About 1% of all colorectal cancers are caused by familial adenomatous polyposis (FAP). Familial adenomatous polyposis (FAP) is caused by inherited changes in the APC gene. The APC gene is a tumor suppressor gene; it normally helps keep cell growth in check. In people with inherited changes in the APC gene, this “brake” on cell growth is turned off, causing hundreds of polyps to form in the colon. Over time, cancer will nearly always develop in one or more of these polyps. Familial adenomatous polyposis (FAP) is a rare disorder that causes you to develop thousands of polyps in the lining of your colon and rectum. In the most common type of FAP, hundreds or thousands of polyps develop in a person’s colon and rectum, often starting at ages 10 to 12 years. Cancer usually develops in 1 or more of these polyps as early as age 20. By age 40, almost all people with FAP will have colon cancer if their colon hasn’t been removed to prevent it. People with FAP also have an increased risk for cancers of the stomach, small intestines, pancreas, liver, and some other organs. There are 3 sub-types of familial adenomatous polyposis (FAP):
- In attenuated FAP (AFAP), patients have fewer polyps (less than 100), and colorectal cancer tends to occur at a later age (40s and 50s).
- Gardner syndrome is a type of FAP that also causes non-cancer tumors of the skin, soft tissue, and bones.
- Turcot syndrome is a rare inherited condition in which people have a higher risk of many adenomatous polyps and colorectal cancer. People with Turcot syndrome who have the APC gene are also at risk of a specific type of brain cancer called medulloblastoma.
- Peutz-Jeghers syndrome is caused by inherited changes in the STK11 (LKB1) gene, a tumor suppressor gene. People with Peutz-Jeghers syndrome tend to have freckles around the mouth (and sometimes on their hands and feet) and a special type of polyp called hamartomas in their digestive tracts. These people are at a much higher risk for colorectal cancer, as well as other cancers, such as breast, ovary, and pancreas. They usually are diagnosed at a younger than usual age.
- MUTYH-associated polyposis (MAP) is caused by mutations in the MUTYH gene, which is involved in how the cell “proofreads” or checks the DNA and fixes errors when cells divide. People with MUTYH-associated polyposis (MAP) develop many colon polyps. These will almost always become cancer if not watched closely with regular colonoscopies. These people also have an increased risk of other cancers of the GI (gastrointestinal) tract and thyroid.
Familial adenomatous polyposis, hereditary nonpolyposis colorectal cancer and other, rarer inherited colon cancer syndromes can be detected through genetic testing. If you’re concerned about your family’s history of colon cancer, talk to your doctor about whether your family history suggests you have a risk of these conditions. You may want to ask your doctor about genetic counseling and genetic testing.
Association between diet and increased colon cancer risk
Studies of large groups of people have shown an association between a typical Western diet and an increased risk of colon cancer. A typical Western diet is high in fat and low in fiber.
A diet that’s high in red meats (such as beef, pork, lamb, or liver) and processed meats (like hot dogs and some luncheon meats) raises your colorectal cancer risk.
Cooking meats at very high temperatures (frying, broiling, or grilling) creates chemicals that might raise your cancer risk. It’s not clear how much this might increase your colorectal cancer risk.
Having a low blood level of vitamin D may also increase your risk.
When people move from areas where the typical diet is low in fat and high in fiber to areas where the typical Western diet is most common, the risk of colon cancer in these people increases significantly. It’s not clear why this occurs, but researchers are studying whether a high-fat, low-fiber diet affects the microbes that live in the colon or causes underlying inflammation that may contribute to cancer risk. This is an area of active investigation and research is ongoing.
Following a healthy eating pattern that includes plenty of fruits, vegetables, and whole grains, and that limits or avoids red and processed meats and sugary drinks probably lowers risk.
Risk factors for colon cancer
Anything that increases your chance of getting a disease is called a risk factor. Having a risk factor does not mean that you will get cancer; not having risk factors doesn’t mean that you will not get cancer. Talk to your doctor if you think you may be at risk for colorectal cancer.
Factors that may increase your risk of colon cancer include:
- Older age. The great majority of people diagnosed with colon cancer are older than 50. Colon cancer can occur in younger people, but it occurs much less frequently.
- African-American race. African-Americans have a greater risk of colon cancer than do people of other races in the US.
- Jews of Eastern European descent (Ashkenazi Jews) have one of the highest colorectal cancer risks of any ethnic group in the world.
- Having a personal history of cancer of the colon, rectum, or ovary.
- Having a personal history of high-risk adenomas (colorectal polyps that are 1 centimeter or larger in size or that have cells that look abnormal under a microscope).
- Having a personal history of inflammatory intestinal conditions for 8 years or more. Chronic inflammatory diseases of the colon, such as ulcerative colitis and Crohn’s disease, can increase your risk of colon cancer.
- Having inherited syndromes that increase colon cancer risk. Genetic syndromes passed through generations of your family can increase your risk of colon cancer. These syndromes include familial adenomatous polyposis (FAP) and hereditary nonpolyposis colorectal cancer, which is also known as Lynch syndrome.
- Family history of colon or rectal cancer. You’re more likely to develop colon cancer if you have a parent, sibling or child with the disease (first-degree relative). If more than one family member has colon cancer or rectal cancer, your risk is even greater.
- Low-fiber, high-fat diet. Colon cancer and rectal cancer may be associated with a diet low in fiber and high in fat and calories. Research in this area has had mixed results. Some studies have found an increased risk of colon cancer in people who eat diets high in red meat and processed meat.
- A sedentary lifestyle. If you’re inactive, you’re more likely to develop colon cancer. Getting regular physical activity may reduce your risk of colon cancer.
- Diabetes. People with diabetes and insulin resistance have an increased risk of colon cancer. Both type 2 diabetes and colorectal cancer share some of the same risk factors (such as being overweight and physical inactivity). But even after taking these factors into account, people with type 2 diabetes still have an increased risk. They also tend to have a less favorable prognosis (outlook) after diagnosis.
- Obesity. People who are obese have an increased risk of colon cancer and an increased risk of dying of colon cancer when compared with people considered normal weight.
- Smoking. People who smoke may have an increased risk of colon cancer.
- Alcohol. Having three or more alcoholic drinks per day increases your risk of colon cancer.
- Radiation therapy for cancer. Radiation therapy directed at the abdomen to treat previous cancers increases the risk of colon and rectal cancer.
Colon cancer prevention
Get screened for colon cancer
People with an average risk of colon cancer can consider screening beginning at age 50. The American Cancer Society recommends that people at average risk of colorectal cancer start regular screening at age 45 153. But people with an increased risk, such as those with a family history of colon cancer, should consider screening sooner.
People who are in good health and with a life expectancy of more than 10 years should continue regular colorectal cancer screening through the age of 75.
For people ages 76 through 85, the decision to be screened should be based on a person’s preferences, life expectancy, overall health, and prior screening history.
People over 85 should no longer get colorectal cancer screening.
*For screening, people are considered to be at average risk if they do NOT have:
- A personal history of colorectal cancer or certain types of polyps
- A family history of colorectal cancer
- A personal history of inflammatory bowel disease (ulcerative colitis or Crohn’s disease)
- A confirmed or suspected hereditary colorectal cancer syndrome, such as familial adenomatous polyposis (FAP) or Lynch syndrome (hereditary non-polyposis colon cancer or HNPCC)
- A personal history of getting radiation to the abdomen (belly) or pelvic area to treat a prior cancer
Several screening options exist — each with its own benefits and drawbacks. Talk about your options with your doctor, and together you can decide which tests are appropriate for you. The most important thing is to get screened, no matter which test you choose.
Several screening tests can be divided into 2 main groups:
- Stool-based tests: These tests check the stool (feces) for signs of cancer. These tests are less invasive and easier to have done, but they need to be done more often.
- Visual (structural) exams: These tests look at the structure of the colon and rectum for any abnormal areas. This is done either with a scope (a tube-like instrument with a light and tiny video camera on the end) put into the rectum, or with special imaging (x-ray) tests.
These tests each have different risks and benefits (see below), and some of them might be better options for you than others.
Make lifestyle changes to reduce your risk
You can take steps to reduce your risk of colon cancer by making changes in your everyday life. Take steps to:
- Eat a variety of fruits, vegetables and whole grains. Fruits, vegetables and whole grains contain vitamins, minerals, fiber and antioxidants, which may play a role in cancer prevention. Choose a variety of fruits and vegetables so that you get an array of vitamins and nutrients.
- Drink alcohol in moderation, if at all. If you choose to drink alcohol, limit the amount of alcohol you drink to no more than one drink a day for women and two for men.
- Stop smoking. Talk to your doctor about ways to quit that may work for you.
- Exercise most days of the week. Try to get at least 30 minutes of exercise on most days. If you’ve been inactive, start slowly and build up gradually to 30 minutes. Also, talk to your doctor before starting any exercise program.
- Maintain a healthy weight. If you are at a healthy weight, work to maintain your weight by combining a healthy diet with daily exercise. If you need to lose weight, ask your doctor about healthy ways to achieve your goal. Aim to lose weight slowly by increasing the amount of exercise you get and reducing the number of calories you eat.
Colon cancer prevention for people with a high risk
Some medications have been found to reduce the risk of precancerous polyps or colon cancer. However, not enough evidence exists to recommend these medications to people who have an average risk of colon cancer. These options are generally reserved for people with a high risk of colon cancer.
For instance, some evidence links a reduced risk of polyps and colon cancer to regular use of aspirin or aspirin-like drugs. But it’s not clear what dose and what length of time would be needed to reduce the risk of colon cancer. Taking aspirin daily has some risks, including gastrointestinal bleeding and ulcers, so doctors typically don’t recommend this as a prevention strategy unless you have an increased risk of colon cancer.
Screening Tests for Colorectal Cancer
Doctors recommend certain screening tests for healthy people with no signs or symptoms in order to look for early colon cancer. Finding colon cancer at its earliest stage provides the greatest chance for a cure. Screening (which is a process of looking for cancer in people who have no symptoms) has been shown to reduce your risk of dying of colon cancer.
People with an average risk of colon cancer can consider screening beginning at age 45. But people with an increased risk, such as those with a family history of colon cancer, should consider screening sooner. African-Americans and American Indians may consider beginning colon cancer screening at age 45.
Both men and women should have a colon cancer screening test starting at age 45 (if following the American Cancer Society Guideline). Some doctors recommend that African Americans begin screening at age 45.
With a recent increase in colon cancer in people in their 40s, the American Cancer Society recommends that healthy men and women start screening at age 45. Talk to your doctor if you’re concerned.
Several screening options exist — each with its own benefits and drawbacks. Talk about your options with your doctor, and together you can decide which tests are appropriate for you. If a colonoscopy is used for screening, polyps can be removed during the procedure before they turn into cancer.
There are 3 main types of colorectal cancer screening tests 154:
- Blood-based tests: These tests check a person’s blood for signs of colorectal cancer.
- Stool-based tests: These tests check the stool (feces) for signs of colon cancer. These tests are less invasive and easier to have done, but they need to be done more often.
- Visual (structural) exams: These tests look at the structure of the colon and rectum for any abnormal areas. They are done either with a scope (a tube-like instrument with a light and tiny video camera on the end) put into the rectum, or with special imaging (x-ray) tests.
These tests each have different risks and benefits and some of them might be better options for you than others.
If you choose to be screened with a test other than colonoscopy, any abnormal test result should be followed up with a timely colonoscopy.
Some of these tests might also be used if you have symptoms of colorectal cancer or other digestive diseases such as inflammatory bowel disease.
The American Cancer Society believes that preventing colorectal cancer (and not just finding it early) should be a major reason for getting tested. Having polyps found and removed keeps some people from getting colorectal cancer. You are encouraged to have tests that have the best chance of finding both polyps and cancer if these tests are available to you and you are willing to have them. But the most important thing is to get tested, no matter which test you choose.
For screening, people are considered to be at AVERAGE risk if they DO NOT have:
- A personal history of colorectal cancer or certain types of polyps
- A family history of colorectal cancer
- A personal history of inflammatory bowel disease (ulcerative colitis or Crohn’s disease)
- A confirmed or suspected hereditary colorectal cancer syndrome, such as familial adenomatous polyposis (FAP) or Lynch syndrome (hereditary non-polyposis colon cancer or HNPCC)
- A personal history of getting radiation to the abdomen (belly) or pelvic area to treat a prior cancer
People who are in good health and with a life expectancy of more than 10 years should continue regular colorectal cancer screening through the age of 75.
For people ages 76 through 85, the decision to be screened should be based on a person’s preferences, life expectancy, overall health, and prior screening history.
People over 85 should no longer get colorectal cancer screening.
When colon cancer is found early, before it has spread, the 5-year relative survival rate is 90%. This means 9 out of 10 people with early-stage cancer survive at least 5 years. But if the cancer has had a chance to spread outside the colon, survival rates are lower.
Starting at age 45, men and women at average risk for developing colorectal cancer should use one of the screening tests below:
Screening is the process of looking for cancer in people who have no symptoms. Several tests can be used to screen for colorectal cancers. These tests can be divided into 153:
Visual (structural) exams of the colon and rectum
- Colonoscopy every 10 years
- CT colonography (virtual colonoscopy) every 5 years
- Sigmoidoscopy every 5 years
Stool-based tests
- Highly sensitive fecal immunochemical test (FIT) every year
- Highly sensitive guaiac-based fecal occult blood test (gFOBT) every year
- Multi-targeted stool DNA test with fecal immunochemical testing (MT-sDNA or sDNA-FIT or FIT-DNA)) every 3 years
Tests that can find both colorectal polyps and cancer are encouraged if they are available and you are willing to have them. But the most important thing is to get tested, no matter which test you choose.
These tests, as well as others, can also be used when people have symptoms of colorectal cancer and other digestive diseases such as inflammatory bowel disease.
People at increased or high risk
If you are at an increased or high risk of colorectal cancer, you might need to start colorectal cancer screening before age 45 and/or be screened more often. The following conditions make your risk higher than average:
- A personal history of colorectal cancer or adenomatous polyps
- A personal history of inflammatory bowel disease (ulcerative colitis or Crohn’s disease)
- A personal history of radiation to the abdomen (belly) or pelvic area to treat a prior cancer
- A strong family history of colorectal cancer or polyps
- A known family history of a hereditary colorectal cancer syndrome such as familial adenomatous polyposis (FAP) or Lynch syndrome (hereditary non-polyposis colon cancer or HNPCC)
The tables below suggest screening guidelines for people with increased or high risk of colorectal cancer based on specific risk factors. Some people may have more than one risk factor. Refer to the tables below and discuss these recommendations with your doctor. Your doctor can suggest the best screening option for you, as well as any changes in the schedule based on your individual risk.
People at increased risk for colorectal cancer
- People with one or more family members who have had colon or rectal cancer. Screening recommendations for these people depend on who in the family had cancer and how old they were when it was diagnosed. Some people with a family history will be able to follow the recommendations for average risk adults, but others might need to get a colonoscopy (and not any other type of test) more often, and possibly starting before age 45.
- People who have had certain types of polyps removed during a colonoscopy. Most of these people will need to get a colonoscopy again after 3 years, but some people might need to get one earlier (or later) than 3 years, depending on the type, size, and number of polyps.
- People who have had colon or rectal cancer. Most of these people will need to start having colonoscopies regularly about one year after surgery to remove the cancer. Other procedures like MRI or proctoscopy with ultrasound might also be recommended for some people with rectal cancer, depending on the type of surgery they had.
- People who have had radiation to the abdomen (belly) or pelvic area to treat a prior cancer. Most of these people will need to start having colorectal screening (colonoscopy or stool based testing) at an earlier age (depending on how old they were when they got the radiation). Screening often begins 5 years after the radiation was given or at age 30, whichever comes last. These people might also need to be screened more often than normal (such as at least every 3 to 5 years).
People at high risk for colorectal cancer
- People with inflammatory bowel disease (Crohn’s disease or ulcerative colitis). These people generally need to get colonoscopies (not any other type of test) starting at least 8 years after they are diagnosed with inflammatory bowel disease. Follow-up colonoscopies should be done every 1 to 3 years, depending on the person’s risk factors for colorectal cancer and the findings on the previous colonoscopy.
- People known or suspected to have certain genetic syndromes. These people generally need to have colonoscopy (not any of the other tests). Screening is often recommended to begin at a young age, possibly as early as the teenage years for some syndromes – and needs to be done much more frequently. Specifics depend on which genetic syndrome you have, and other factors. If you’re at increased or high risk of colorectal cancer (or think you might be), talk to your doctor to learn more. Your doctor can suggest the best screening option for you, as well as determine what type of screening schedule you should follow, based on your individual risk.
Note: As of 2022, the American Cancer Society no longer have screening guidelines specifically for people at increased or high risk of colorectal cancer. The tables below were from American Cancer Society prior to them removing their screening guidelines for people at increased or high risk of colorectal cancer. But we have decided to leave them here for your reference.
Table 5. Professional society recommendations on when to start and when to stop colorectal cancer screening
| Colorectal cancer screening start age | Colorectal cancer screening stop age | |
|---|---|---|
| Multi-Society Task Force, 2021 | “We suggest that clinicians offer colorectal cancer screening to all average-risk individuals age 45-49 (weak recommendation; low-quality evidence).” | “We suggest that individuals who are up to date with screening and have negative prior screening tests, particularly high-quality colonoscopy, consider stopping screening at age 75 years or when life expectancy is less than 10 years (weak recommendation, low-quality evidence).” |
| “For average-risk individuals who have not initiated screening before age 50, we recommend that clinicians offer colorectal cancer screening to all average-risk individuals beginning at age 50 (strong recommendation, high-quality evidence).” | “We suggest that persons without prior screening should be considered for screening up to age 85, depending on consideration of their age and comorbidities (weak recommendation, low-quality evidence).” | |
| National Comprehensive Cancer Network, 2021 155 | “Average risk: age ≥45. The panel has reviewed existing data for beginning screening of average-risk individuals at age <50 years. Based on their assessment, the panel agrees that the data are stronger to support beginning screening at 50 years but acknowledges that lower-level evidence supports a benefit for screening earlier. When initiating screening for all eligible individuals, the panel recommends a discussion of potential harms/risks and benefits, and the consideration of all recommended colorectal cancer screening options.” | Not provided |
| American College of Gastroenterology, 2021 156 | “We recommend colorectal cancer screening in average-risk individuals between ages 50 and 75 years to reduce incidence of advanced adenoma, colorectal cancer, and mortality from colorectal cancer.” Strong recommendation; moderate-quality evidence “We suggest colorectal cancer screening in average-risk individuals between ages 45 and 49 years to reduce incidence of advanced adenoma, colorectal cancer, and mortality from colorectal cancer.” Conditional recommendation; very low-quality evidence | “We suggest that a decision to continue screening beyond age 75 years be individualized (conditional recommendation strength, very low-Grading of Recommendations Assessment, Development and Evaluation quality of evidence).” |
| U.S. Preventative Services Task Force, 2021 157 | Grade A: “The U.S. Preventative Services Task Force recommends screening for colorectal cancer in all adults ages 50 to 75 years.” Grade B: “The U.S. Preventative Services Task Force recommends screening for colorectal cancer in adults aged 45 to 49 years.” | Grade C: “The U.S. Preventative Services Task Force recommends that clinicians selectively offer screening for colorectal cancer in adults aged 76 to 85 years. Evidence indicates that the net benefit of screening all persons in this age group is small. In determining whether this service is appropriate in individual cases, patients and clinicians should consider the patient’s overall health, prior screening history, and preferences.” |
| American College of Physicians, 2019 158 | “Clinicians should screen for colorectal cancer in average-risk adults between the ages of 50 and 75 years.” | “Clinicians should discontinue screening for colorectal cancer in average-risk adults older than 75 years or in adults with a life expectancy of 10 years or less.” |
| American Cancer Society, 2018 159 | “The American Cancer Society recommends that adults aged 45 and older with an average risk of colorectal cancer undergo regular screening with either a high-sensitivity stool-based test or a structural (visual) examination, depending on patient preference and test availability. As a part of the screening process, all positive results on non-colonoscopy screening tests should be followed up with timely colonoscopy.” | “Average-risk adults in good health with a life expectancy of greater than 10 years continue colorectal cancer screening through the age of 75 years (qualified recommendation).” |
| “The recommendation to begin screening at age 45 is a qualified recommendation.” | Clinicians should “individualize colorectal cancer screening decisions for individuals aged 76 through 85 years based on patient preferences, life expectancy, health status, and prior screening history (qualified recommendation).” | |
| “The recommendation for regular screening in adults aged 50 y and older is a strong recommendation.” | Clinicians should “discourage individuals over age 85 years from continuing colorectal cancer screening (qualified recommendation).” |
Colon cancer Diagnosis
If you have symptoms that might be from colorectal cancer, or if a screening test shows something abnormal, your doctor will recommend one or more of the exams and tests below to find the cause.
Your doctor will also ask about your medical history to learn about possible risk factors, including your family history. You will also be asked if you’re having any symptoms and, if so, when they started and how long you’ve had them.
As part of a physical exam, your doctor will feel your abdomen for masses or enlarged organs, and also examine the rest of your body. You may also have a digital rectal exam (DRE). During this test, the doctor inserts a lubricated, gloved finger into your rectum to feel for any abnormal areas.
If your signs and symptoms indicate that you could have colon cancer, your doctor may recommend one or more tests and procedures, including:
Using a scope to examine the inside of your colon. Colonoscopy uses a long, flexible and slender tube attached to a video camera and monitor to view your entire colon and rectum. If any suspicious areas are found, your doctor can pass surgical tools through the tube to take tissue samples (biopsies) for analysis and remove polyps.
Virtual colonoscopy: A procedure that uses a series of x-rays called computed tomography to make a series of pictures of the colon. A computer puts the pictures together to create detailed images that may show polyps and anything else that seems unusual on the inside surface of the colon. This test is also called colonography or CT colonography.
Sigmoidoscopy: A procedure to look inside the rectum and sigmoid (lower) colon for polyps (small areas of bulging tissue), other abnormal areas, or cancer. A sigmoidoscope is inserted through the rectum into the sigmoid colon. A sigmoidoscope is a thin, tube-like instrument with a light and a lens for viewing. It may also have a tool to remove polyps or tissue samples, which are checked under a microscope for signs of cancer.
Biopsy: The removal of cells or tissues so they can be viewed under a microscope by a pathologist to check for signs of cancer.
Biopsy samples (from colonoscopy or surgery) are sent to the lab where they are looked at closely. Other tests may suggest that colorectal cancer is present, but the only way to be sure is to look at the biopsy samples under a microscope.
If cancer is found, other lab tests may also be done on the biopsy specimens to help better classify the cancer.
- Gene tests: Doctors may look for specific gene changes in the cancer cells that might affect how the cancer is best treated especially if the cancer has spread (metastasized). For example, doctors now typically test the cells for changes in the KRAS and NRAS and BRAF genes. Some doctors may also test for changes in the BRAF gene. Patients whose cancers have mutations in these genes typically do not benefit from treatment with certain targeted anti-cancer drugs.
- MSI and MMR testing: Colorectal cancer cells are typically tested to see if they show high levels of gene changes called microsatellite instability (MSI). Testing might also be done to see if the cancer cells have changes in any of the mismatch repair (MMR) genes (MLH1, MSH2, MSH6, and PMS2).
Changes in MSI or in MMR genes (or both) are often seen in people with Lynch syndrome (HNPCC). Most colorectal cancers do not have high levels of MSI or changes in MMR genes. But most colorectal cancers that are linked to Lynch syndrome do.
There are 2 possible reasons to test colorectal cancers for MSI or for MMR gene changes:
- To identify patients who should be tested for Lynch syndrome. A diagnosis of Lynch syndrome can help plan other cancer screenings for the patient (for example, women with Lynch syndrome may need to be screened for uterine cancer). Also, if a patient has Lynch syndrome, their relatives could also have it, and may want to be tested for it.
- To determine treatment options for colorectal cancer, where MSI or MMR results could change the way it is treated.
Blood tests. No blood test can tell you if you have colon cancer. But your doctor may test your blood for clues about your overall health, such as kidney and liver function tests.
Your doctor may also test your blood for a chemical sometimes produced by colon cancers called tumor markers that can be found in the blood. The most common tumor markers for colorectal cancer are carcinoembryonic antigen (CEA) and CA 19-9. Tracked over time, the level of CEA (carcinoembryonic antigen) in your blood may help your doctor understand your prognosis and whether your cancer is responding to treatment.
Blood tests for these tumor markers can sometimes suggest someone might have colorectal cancer, but they can’t be used alone to screen for or diagnose cancer. This is because tumor marker levels can sometimes be normal in someone who has cancer and can be abnormal for reasons other than cancer.
Tumor markers are used most often along with other tests to monitor patients who already have been diagnosed with colorectal cancer. They may help show how well treatment is working or provide an early warning that a cancer has returned.
If symptoms or the results of the physical exam or blood tests suggest that you might have colorectal cancer, your doctor could recommend more tests. This most often is colonoscopy, but sometimes other tests may be done first.
Barium enema: A series of x-rays of the lower gastrointestinal tract. A liquid that contains barium (a silver-white metallic compound) is put into the rectum. The barium coats the colon and x-rays are taken. This procedure is also called a lower GI series.
Colon cancer treatment
The type of treatment your doctor recommends will depend largely on the location of your cancer, its stage and your other health concerns. Treatment for colon cancer usually involves surgery to remove the cancer. Other treatments, such as radiation therapy and chemotherapy, might also be recommended.
Colon cancer main treatments are:
- Surgery – the cancerous section of bowel is removed; it’s the most effective way of curing bowel cancer and in many cases is all you need
- Chemotherapy – where medicine is used to kill cancer cells
- Radiotherapy – where radiation is used to kill cancer cells
- Radiation therapy and/or chemotherapy may be given before surgery to shrink the tumor, make it easier to remove the cancer, and help with bowel control after surgery. Treatment given before surgery is called neoadjuvant therapy. After all the cancer that can be seen at the time of the surgery is removed, some patients may be given radiation therapy and/or chemotherapy after surgery to kill any cancer cells that are left. Treatment given after the surgery, to lower the risk that the cancer will come back, is called adjuvant therapy.
- Radiofrequency ablation: The use of a special probe with tiny electrodes that kill cancer cells. Sometimes, the probe is inserted directly through the skin, and only local anesthesia is needed. In other cases, the probe is inserted through an incision in the abdomen. This is done in the hospital with general anesthesia.
- Cryosurgery: A treatment that uses an instrument to freeze and destroy abnormal tissue. This type of treatment is also called cryotherapy.
- Targeted therapies – a newer group of medicines that increases the effectiveness of chemotherapy and prevents the cancer spreading
- Immunotherapy. Immunotherapy is the use of medicines to help a person’s own immune system better recognize and destroy cancer cells. Immunotherapy can be used to treat some people with advanced colorectal cancer.
- Ablation and embolization therapy. When colon or rectal cancer has spread and there are a few small tumors in the liver or lungs, these metastases can sometimes be removed by surgery or destroyed by other techniques, such as ablation or embolization.
As with most types of cancer, the chance of a complete cure depends on how far your cancer spread by the time it’s diagnosed. If your cancer is confined to the bowel, surgery is usually able to completely remove it.
Keyhole or robotic surgery is being used more often, which allows surgery to be performed with less pain and a quicker recovery.
Surgery for early-stage colon cancer
If your colon cancer is very small, your doctor may recommend a minimally invasive approach to surgery, such as:
- Removing polyps (polypectomy) during a colonoscopy. If your cancer is small, localized and completely contained within a polyp and in a very early stage, your doctor may be able to remove it completely during a colonoscopy. This is usually done by passing a wire loop through the colonoscope to cut the polyp off the wall of the colon with an electric current.
- Endoscopic mucosal resection. Removing larger polyps may require also taking a small amount of the lining of the colon or rectum in a procedure called an endoscopic mucosal resection.
- Minimally invasive surgery. Polyps that can’t be removed during a colonoscopy may be removed using laparoscopic surgery. In this procedure, your surgeon performs the operation through several small incisions in your abdominal wall, inserting instruments with attached cameras that display your colon on a video monitor. The surgeon may also take samples from lymph nodes in the area where the cancer is located.
Surgery for invasive colon cancer
If the cancer has grown into or through your colon, your surgeon may recommend:
- Partial colectomy also called hemicolectomy or segmental resection. During this procedure, the surgeon removes the part of your colon that contains the cancer, along with a margin of normal tissue on either side of the cancer. Your surgeon is often able to reconnect the healthy portions of your colon or rectum. This procedure can commonly be done by a minimally invasive approach (laparoscopy).
- Surgery to create a way for waste to leave your body. When it’s not possible to reconnect the healthy portions of your colon or rectum, you may need an ostomy. This involves creating an opening in the wall of your abdomen from a portion of the remaining bowel for the elimination of stool into a bag that fits securely over the opening. Sometimes the ostomy is only temporary, allowing your colon or rectum time to heal after surgery. In some cases, however, the colostomy may be permanent. Sometimes the end of the small intestine (the ileum) instead of the colon is connected to a stoma in the skin. This is called an ileostomy.
- Lymph node removal. Nearby lymph nodes are usually also removed during colon cancer surgery and tested for cancer. At least 12 nearby lymph nodes are also removed so they can be checked for cancer.
- If all of the colon is removed, it’s called a total colectomy. Total colectomy isn’t often needed to remove colon cancer. It’s mostly used only if there’s another problem in the part of the colon without cancer, such as hundreds of polyps (in someone with familial adenomatous polyposis) or, sometimes, inflammatory bowel disease.
Surgery for advanced cancer
If your cancer is very advanced or your overall health very poor, your surgeon may recommend an operation to relieve a blockage of your colon or other conditions in order to improve your symptoms. This surgery isn’t done to cure cancer, but instead to relieve signs and symptoms, such as bleeding and pain.
Some patients have colon cancer that has spread to other parts of the body and also have tumors blocking the colon. In this case, surgery may be done to relieve the blockage without removing the part of the colon containing the cancer. Instead, the colon is cut above the tumor and attached to a stoma (an opening in the skin of the abdomen) to allow stool to come out. This is called a diverting colostomy. It can often help the patient recover enough to start other treatments (such as chemotherapy). It might also be done in cases where the cancer has not spread to distant areas.
If the cancer has spread to only one or a few spots (nodules) in the lungs or liver (and apparently nowhere else), surgery may be used to remove it. In most cases, this is only done if the cancer in the colon is also being removed (or was already removed). Depending on the extent of the cancer, this might help the patient live longer, or it could even cure the cancer. Deciding if surgery is an option to remove areas of cancer spread depends on their size, number, and location.
Chemotherapy
Chemotherapy uses drugs to destroy cancer cells. Chemotherapy for colon cancer is usually given after surgery (adjuvant chemo) if the cancer has spread to lymph nodes. In this way, chemotherapy may help reduce the risk of cancer recurrence and death from cancer. Sometimes chemotherapy may be used before surgery (neoadjuvant chemo) as well, with the goal of shrinking the cancer before an operation. Chemotherapy before surgery is more common in rectal cancer than in colon cancer.
Chemotherapy can also be given to relieve symptoms of colon cancer that has spread to other areas of the body.
Chemotherapy (chemo) may be used at different times during treatment for colorectal cancer:
- Adjuvant chemo is given after surgery. The goal is to kill cancer cells that might have been left behind at surgery because they were too small to see, as well as cancer cells that might have escaped from the main colon or rectal cancer to settle in other parts of the body but are too small to see on imaging tests. This helps lower the chance that the cancer will come back.
- Neoadjuvant chemo is given (sometimes with radiation) before surgery to try to shrink the cancer and make it easier to remove. This is often done for rectal cancer.
- For advanced cancers that have spread to other organs like the liver, chemo can be used to help shrink tumors and ease problems they’re causing. While it’s not likely to cure the cancer, this often helps people feel better and live longer.
Chemotherapy drugs used to treat colorectal cancer include:
- 5-Fluorouracil (5-FU)
- Capecitabine (Xeloda), a pill that is changed into 5-FU once it gets to the tumor.
- Irinotecan (Camptosar)
- Oxaliplatin (Eloxatin)
- Trifluridine and tipiracil (Lonsurf), a combination drug in pill form
- Leucovorin (a vitamin that improves the effectiveness of 5-FU).
- Other chemotherapy drugs not listed here may also be used.
Most often, combinations of 2 or 3 of these drugs are used. Sometimes, chemo drugs are given along with a targeted therapy drug bevacizumab, cetuximab, or panitumumab.
Chemo drugs attack cells that are dividing quickly, which is why they work against cancer cells. But other cells in the body, such as those in hair follicles and in the lining of the mouth and intestines, are also dividing quickly. These cells can be affected by chemo too, which can lead to side effects.
Radiation therapy
Radiation therapy uses powerful energy sources, such as X-rays, to kill cancer cells, to shrink large tumors before an operation so that they can be removed more easily, or to relieve symptoms of colon cancer and rectal cancer. Radiation therapy either alone or combined with chemotherapy (chemoradiation) is one of the standard treatment options for the initial management of rectal cancer followed by surgery.
Different types of radiation therapy can be used to treat colon and rectal cancers.
- External-beam radiation therapy (EBRT). External-beam radiation therapy (EBRT) is the type of radiation therapy used most often for people with colon or rectal cancer. The radiation is focused on the cancer from a machine outside the body. It’s a lot like getting an x-ray, but the radiation is more intense. How often and how long a person gets radiation treatments depends on the reason the radiation is being given and other factors. Treatments might be given over the course of a few days or several weeks. Newer EBRT techniques, such as three-dimensional conformal radiation therapy (3D-CRT), intensity modulated radiation therapy (IMRT), and stereotactic body radiation therapy (SBRT), have been shown to help doctors treat colorectal cancers that have spread to the lungs or liver more accurately while lowering the radiation exposure to nearby healthy tissues. They are typically used if there is only a small number of tumors and if the tumor is causing symptoms and surgery is not an option.
- Internal radiation therapy (brachytherapy). Brachytherapy might be used to treat some rectal cancers, but more research is needed to understand how to best use and when to use brachytherapy. For this treatment, a radioactive source is put inside your rectum next to or into the tumor. This allows the radiation to reach the rectum without passing through the skin and other tissues of the belly (abdomen), so it’s less likely to damage nearby tissues.
- Endocavitary radiation therapy: For this treatment, a small balloon-like device is placed into the rectum to deliver high-intensity radiation for a few minutes. This is typically done in 4 treatments (or less), with about 2 weeks between each treatment. This can let some patients, particularly elderly patients, avoid major surgery and a colostomy. This type of treatment is used for some small rectal cancers or in cases where radiation was already given in the pelvic area and the rectal cancer has come back. Sometimes external-beam radiation therapy is also given.
- Interstitial brachytherapy: For this treatment, a tube is placed into the rectum and right into the tumor. Small pellets of radioactive material are then put into the tube for several minutes. The radiation travels only a short distance, limiting the harmful effects on nearby healthy tissues. It’s sometimes used to treat people with rectal cancer who are not healthy enough for surgery or have cancer that has come back in the rectum. This can be done a few times a week for a couple of weeks, but it can also be just a one-time procedure.
- Radioembolization. Radiation can also be given during an embolization procedure.
Targeted drug therapy
Targeted therapy is a type of cancer treatment that targets proteins that control how cancer cells grow, divide, and spread. As researchers learn more about the DNA changes and proteins that drive cancer, they are better able to design treatments that target these proteins. Most targeted therapies are either small-molecule drugs or monoclonal antibodies.
- Small-molecule drugs are small enough to enter cells easily, so they are used for targets that are inside cells.
- Monoclonal antibodies also known as therapeutic antibodies, are proteins produced in the lab. These proteins are designed to attach to specific targets found on cancer cells. Some monoclonal antibodies mark cancer cells so that they will be better seen and destroyed by the immune system. Other monoclonal antibodies directly stop cancer cells from growing or cause them to self-destruct. Still others carry toxins to cancer cells.
Your doctor may suggest biomarker tests to help predict your response to certain targeted therapy drugs.
Targeted therapies used to treat colon cancer include:
- Bevacizumab (Avastin)
- Cetuximab (Erbitux)
- Encorafenib (Braftovi)
- Fruquintinib (Fruzaqla)
- Panitumumab (Vectibix)
- Ramucirumab (Cyramza)
- Regorafenib (Stivarga)
- Ziv-aflibercept (Zaltrap)
Targeted drugs can be given along with chemotherapy or alone. Targeted drugs are typically reserved for people with advanced colon cancer.
Some people are helped by targeted drugs, while others are not. Researchers have recently made progress in determining who is most likely to benefit from specific targeted drugs. Until more is known, doctors carefully weigh the possible benefit of targeted drugs against the risk of side effects and the cost when deciding whether to use these treatments.
Colon cancer survival rate
Remember, these survival rates are only estimates – they can’t predict what will happen to any individual person. We understand that these statistics can be confusing and may lead you to have more questions. Talk to your doctor to better understand your specific situation.
Table 6. 5-year relative survival rates for colon cancer
| National Cancer Institute’s SEER (Surveillance, Epidemiology, and End Results) stage | 5-year relative survival rate |
|---|---|
| Localized | 91% |
| Regional | 73% |
| Distant | 13% |
| All SEER stages combined | 63% |
Footnote: SEER 2014 to 2020, All Races, Both Sexes by SEER Combined Summary Stage
Table 7. 5-year relative survival rates for rectal cancer
| National Cancer Institute’s SEER (Surveillance, Epidemiology, and End Results) stage | 5-year relative survival rate |
|---|---|
| Localized | 90% |
| Regional | 74% |
| Distant | 18% |
| All SEER stages combined | 67% |
Footnotes:
- These numbers apply only to the stage of the cancer when it is first diagnosed. They do not apply later on if the cancer grows, spreads, or comes back after treatment.
- These numbers don’t take everything into account. Survival rates are grouped based on how far the cancer has spread, but your age, overall health, how well the cancer responds to treatment, whether the cancer started on the left or right side of the colon, and other factors can also affect your outlook.
- People now being diagnosed with colon or rectal cancer may have a better outlook than these numbers show. Treatments improve over time, and these numbers are based on people who were diagnosed and treated at least five years earlier.
These survival rates are only estimates – they can’t predict what will happen to any individual person. We understand that these statistics can be confusing and may lead you to have more questions. Talk to your doctor to better understand your specific situation.
[Source 161 ]- Bharucha AE, Dorn SD, Lembo A, Pressman A. American Gastroenterological Association medical position statement on constipation. Gastroenterology. 2013. January;144(1): 211–7. 10.1053/j.gastro.2012.10.029[↩]
- Constipation and Defecation Problems. https://gi.org/topics/constipation-and-defection-problems/[↩]
- National Cancer Institute at the National Institutes of Health. Constipation. https://www.cancer.gov/about-cancer/treatment/side-effects/constipation[↩]
- Pare P, Ferrazzi S, Thompson WG, Irvine EJ, Rance L. An epidemiological survey of constipation in canada: definitions, rates, demographics, and predictors of health care seeking. Am J Gastroenterol. 2001 Nov;96(11):3130-7. doi: 10.1111/j.1572-0241.2001.05259.x[↩]
- The National Institute of Diabetes and Digestive and Kidney Diseases Health Information Center. Definition & Facts for Constipation. https://www.niddk.nih.gov/health-information/digestive-diseases/constipation/definition-facts[↩]
- Culhane B: Constipation. In: Yasko J, ed.: Guidelines for Cancer Care: Symptom Management. Reston, Va: Reston Publishing Company, Inc., 1983, pp 184-7.[↩]
- Higgins PD, Johanson JF. Epidemiology of constipation in North America: a systematic review. American Journal of Gastroenterology. 2004;99:750–759[↩]
- American Gastroenterological Association; Bharucha AE, Dorn SD, Lembo A, Pressman A. American Gastroenterological Association medical position statement on constipation. Gastroenterology. 2013 Jan;144(1):211-7. doi: 10.1053/j.gastro.2012.10.029[↩]
- Rose S, ed. Constipation: A Practical Approach to Diagnosis and Treatment. New York, NY: Springer Science and Business Media; 2014.[↩]
- Report of an unusual case with severe fecal impaction responding to medication therapy. Zhao W, Ke M. J Neurogastroenterol Motil. 2010 Apr; 16(2):199-202.[↩]
- Serrano Falcón B, Barceló López M, Mateos Muñoz B, Álvarez Sánchez A, Rey E. Fecal impaction: a systematic review of its medical complications. BMC Geriatr. 2016;16:4. Published 2016 Jan 11. doi:10.1186/s12877-015-0162-5 https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4709889/[↩]
- Wright BA, Staats DO: The geriatric implications of fecal impaction. Nurse Pract 11 (10): 53-8, 60, 64-6, 1986. https://www.ncbi.nlm.nih.gov/pubmed/3785769?dopt=Abstract[↩]
- Management and prevention of fecal impaction. Wald A. Curr Gastroenterol Rep. 2008 Oct; 10(5):499-501.[↩]
- Mathew G, Cagir B. Fecal Impaction. [Updated 2018 Nov 26]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2018 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK448094[↩]
- Serrano Falcón B, Álvarez Sánchez Á, Diaz-Rubio M, Rey E. Prevalence and factors associated with faecal impaction in the Spanish old population. Age Ageing. 2017 Jan 12;46(1):119-124.[↩]
- García Cabrera AM, Jiménez Rodríguez RM, Reyes Díaz ML, Vázquez Monchul JM, Ramos Fernández M, Díaz Pavón JM, Palacios González C, Padillo Ruiz FJ, de la Portilla de Juan F. Fecal incontinence in older patients. A narrative review. Cir Esp. 2018 Mar;96(3):131-137.[↩]
- Hampton BG, Bryant RA, eds.: Ostomies and Continent Diversions: Nursing Management. St. Louis, Mo: Mosby Year Book, Inc., 1992.[↩]
- Mayo Foundation for Medical Education and Research. Constipation. http://www.mayoclinic.org/diseases-conditions/constipation/home/ovc-20252671[↩][↩]
- Forootan M, Bagheri N, Darvishi M. Chronic constipation: A review of literature. Medicine (Baltimore). 2018 May;97(20):e10631. doi: 10.1097/MD.0000000000010631[↩]
- Bharucha AE, Wald A. Chronic Constipation. Mayo Clin Proc. 2019 Nov;94(11):2340-2357. doi: 10.1016/j.mayocp.2019.01.031[↩][↩]
- Bharucha AE, Lacy BE. Mechanisms, Evaluation, and Management of Chronic Constipation. Gastroenterology. 2020 Apr;158(5):1232-1249.e3. doi: 10.1053/j.gastro.2019.12.034[↩]
- Werth BL, Christopher SA. Potential risk factors for constipation in the community. World J Gastroenterol. 2021 Jun 7;27(21):2795-2817. doi: 10.3748/wjg.v27.i21.2795[↩]
- Bharucha AE, Pemberton JH, Locke GR 3rd. American Gastroenterological Association technical review on constipation. Gastroenterology. 2013 Jan;144(1):218-38. doi: 10.1053/j.gastro.2012.10.028[↩]
- van Dijk KN, de Vries CS, van den Berg PB, Dijkema AM, Brouwers JR, de Jong-van den Berg LT. Constipation as an adverse effect of drug use in nursing home patients: an overestimated risk. Br J Clin Pharmacol. 1998 Sep;46(3):255-61. doi: 10.1046/j.1365-2125.1998.00777.x[↩]
- Mayo Foundation for Medical Education and Research. Constipation Diagnosis. http://www.mayoclinic.org/diseases-conditions/constipation/diagnosis-treatment/diagnosis/dxc-20252753[↩][↩][↩][↩]
- Dietary Guidelines for Americans. https://www.dietaryguidelines.gov[↩][↩]
- American Heart Association Scientific Statement October 27, 2016 – Statement provides blueprint for healthcare providers to translate nutrition recommendations into practical food choices – http://newsroom.heart.org/news/statement-provides-blueprint-for-healthcare-providers-to-translate-nutrition-recommendations-into-practical-food-choices[↩]
- UpToDate. Patient education: High-fiber diet (Beyond the Basics). https://www.uptodate.com/contents/high-fiber-diet-beyond-the-basics[↩]
- The American Heart Association. What Is Stress Management ? http://www.heart.org/HEARTORG/HealthyLiving/StressManagement/FightStressWithHealthyHabits/What-Is-Stress-Management_UCM_321076_Article.jsp#.V6Ot_2dTEqw[↩]
- Mayo Foundation for Medical Education and Research. Relaxation techniques. http://www.mayoclinic.org/healthy-lifestyle/stress-management/basics/relaxation-techniques/hlv-20049495[↩]
- Mayo Foundation for Medical Education and Research. Stress management. http://www.mayoclinic.org/healthy-lifestyle/stress-management/in-depth/positive-thinking/art-20043950?p=1[↩][↩]
- Mayo Foundation for Medical Education and Research. Over-the-counter laxatives for constipation: Use with caution. http://www.mayoclinic.org/diseases-conditions/constipation/in-depth/laxatives/art-20045906[↩][↩]
- Napolitano M, Fasulo E, Ungaro F, Massimino L, Sinagra E, Danese S, Mandarino FV. Gut Dysbiosis in Irritable Bowel Syndrome: A Narrative Review on Correlation with Disease Subtypes and Novel Therapeutic Implications. Microorganisms. 2023 Sep 22;11(10):2369. doi: 10.3390/microorganisms11102369[↩][↩][↩]
- Staudacher HM, Black CJ, Teasdale SB, Mikocka-Walus A, Keefer L. Irritable bowel syndrome and mental health comorbidity – approach to multidisciplinary management. Nat Rev Gastroenterol Hepatol. 2023 Sep;20(9):582-596. doi: 10.1038/s41575-023-00794-z[↩][↩]
- Nabi MY, Nauhria S, Reel M, Londono S, Vasireddi A, Elmiry M, Ramdass PVAK. Endometriosis and irritable bowel syndrome: A systematic review and meta-analyses. Front Med (Lausanne). 2022 Jul 25;9:914356. doi: 10.3389/fmed.2022.914356[↩]
- Chlebicz-Wójcik A, Śliżewska K. Probiotics, Prebiotics, and Synbiotics in the Irritable Bowel Syndrome Treatment: A Review. Biomolecules. 2021 Aug 4;11(8):1154. doi: 10.3390/biom11081154[↩]
- Shin A, Kashyap PC. Multi-omics for biomarker approaches in the diagnostic evaluation and management of abdominal pain and irritable bowel syndrome: what lies ahead. Gut Microbes. 2023 Jan-Dec;15(1):2195792. doi: 10.1080/19490976.2023.2195792[↩]
- Wu Y, Li Y, Zheng Q, Li L. The Efficacy of Probiotics, Prebiotics, Synbiotics, and Fecal Microbiota Transplantation in Irritable Bowel Syndrome: A Systematic Review and Network Meta-Analysis. Nutrients. 2024 Jul 2;16(13):2114. doi: 10.3390/nu16132114[↩]
- Ghoshal UC, Sachdeva S, Pratap N, Karyampudi A, Mustafa U, Abraham P, Bhatt CB, Chakravartty K, Chaudhuri S, Goyal O, Makharia GK, Panigrahi MK, Parida PK, Patwari S, Sainani R, Sadasivan S, Srinivas M, Upadhyay R, Venkataraman J. Indian consensus statements on irritable bowel syndrome in adults: A guideline by the Indian Neurogastroenterology and Motility Association and jointly supported by the Indian Society of Gastroenterology. Indian J Gastroenterol. 2023 Apr;42(2):249-273. doi: 10.1007/s12664-022-01333-5[↩]
- Huang KY, Wang FY, Lv M, Ma XX, Tang XD, Lv L. Irritable bowel syndrome: Epidemiology, overlap disorders, pathophysiology and treatment. World J Gastroenterol. 2023 Jul 14;29(26):4120-4135. doi: 10.3748/wjg.v29.i26.4120[↩][↩]
- García Mansilla MJ, Rodríguez Sojo MJ, Lista AR, Ayala Mosqueda CV, Ruiz Malagón AJ, Gálvez J, Rodríguez Nogales A, Rodríguez Sánchez MJ. Exploring Gut Microbiota Imbalance in Irritable Bowel Syndrome: Potential Therapeutic Effects of Probiotics and Their Metabolites. Nutrients. 2024 Dec 31;17(1):155. doi: 10.3390/nu17010155[↩]
- Gwee KA, Ghoshal UC, Chen M. Irritable bowel syndrome in Asia: pathogenesis, natural history, epidemiology, and management. J Gastroenterol Hepatol. 2018;33:99–110. doi: 10.1111/jgh.13987[↩]
- Sperber AD, Bangdiwala SI, Drossman DA, et al. Worldwide Prevalence and Burden of Functional Gastrointestinal Disorders, Results of Rome Foundation Global Study. Gastroenterology. 2021 Jan;160(1):99-114.e3. https://www.gastrojournal.org/article/S0016-5085(20)30487-X/fulltext[↩]
- Irritable Bowel Syndrome. http://s3.gi.org/patients/cgp/pdf/ibs.pdf[↩][↩]
- Enck P, Aziz Q, Barbara G, Farmer AD, Fukudo S, Mayer EA, Niesler B, Quigley EM, Rajilić-Stojanović M, Schemann M, Schwille-Kiuntke J, Simren M, Zipfel S, Spiller RC. Irritable bowel syndrome. Nat Rev Dis Primers. 2016 Mar 24;2:16014. doi: 10.1038/nrdp.2016.14[↩][↩][↩]
- Ford AC, Sperber AD, Corsetti M, Camilleri M. Irritable bowel syndrome. Lancet. 2020 Nov 21;396(10263):1675-1688. https://eprints.whiterose.ac.uk/166983/3/THELANCET-D-20-00123R3%20CLEAN.pdf[↩][↩][↩][↩][↩]
- Lacy BE, Patel NK. Rome Criteria and a Diagnostic Approach to Irritable Bowel Syndrome. J Clin Med. 2017 Oct 26;6(11):99. doi: 10.3390/jcm6110099[↩]
- Sperber AD, Dumitrascu D, Fukudo S, Gerson C, Ghoshal UC, Gwee KA, Hungin APS, Kang JY, Minhu C, Schmulson M, Bolotin A, Friger M, Freud T, Whitehead W. The global prevalence of IBS in adults remains elusive due to the heterogeneity of studies: a Rome Foundation working team literature review. Gut. 2017 Jun;66(6):1075-1082. doi: 10.1136/gutjnl-2015-311240[↩]
- Drossman DA, Li Z, Andruzzi E, Temple RD, Talley NJ, Grant Thompson W, et al. U. S. Householder survey of functional gastrointestinal disorders. Dig Dis Sci. 1993;38:1569–80. doi: 10.1007/BF01303162[↩]
- IRRITABLE BOWEL SYNDROME. http://s3.gi.org/patients/gihealth/pdf/ibs.pdf[↩][↩]
- Eijsbouts C, Zheng T, Kennedy NA, Bonfiglio F, Anderson CA, Moutsianas L, et al. Genome-wide analysis of 53,400 people with irritable bowel syndrome highlights shared genetic pathways with mood and anxiety disorders. Nat Genet. 2021;53:1543–52. doi: 10.1038/s41588-021-00950-8[↩]
- Lewis S.J., Heaton K.W. Stool form scale as a useful guide to intestinal transit time. Scand. J. Gastroenterol. 1997;32:920–924. doi: 10.3109/00365529709011203[↩][↩][↩][↩][↩]
- Mearin F, Lacy BE, Chang L, Chey WD, Lembo AJ, Simren M, Spiller R. Bowel Disorders. Gastroenterology. 2016 doi: 10.1053/j.gastro.2016.02.031[↩]
- Mearin F, Lacy BE, Chang L, Chey WD, Lembo AJ, Simren M, Spiller R. Bowel Disorders. Gastroenterology. 2016 Feb 18:S0016-5085(16)00222-5. https://www.gastrojournal.org/article/S0016-5085(16)00222-5/fulltext[↩][↩][↩][↩][↩]
- Vijayvargiya P, Camilleri M, Burton D, Busciglio I, Lueke A, Donato LJ. Bile and fat excretion are biomarkers of clinically significant diarrhoea and constipation in irritable bowel syndrome. Aliment Pharmacol Ther. 2019;49:744–758. doi: 10.1111/apt.15106[↩]
- Karatay E, Utku ÖG. Serum resolvin D1 levels as a marker of inflammation in constipation dominant irritable bowel syndrome. Turk J Gastroenterol. 2020;31:113–119. doi: 10.5152/tjg.2020.19751[↩]
- Camilleri M, Boeckxstaens G. Irritable bowel syndrome: treatment based on pathophysiology and biomarkers. Gut. 2023;72:590–599. doi: 10.1136/gutjnl-2022-328515[↩]
- Chey WD, Kurlander J, Eswaran S. Irritable bowel syndrome: a clinical review. JAMA. 2015 Mar 3;313(9):949-58. doi: 10.1001/jama.2015.0954[↩][↩]
- Mearin F, Lacy BE, Chang L, Chey WD, Lembo AJ, Simren M, Spiller R. Bowel Disorders. Gastroenterology. 2016 Feb 18:S0016-5085(16)00222-5. doi: 10.1053/j.gastro.2016.02.031[↩]
- Mayer EA, Ryu HJ, Bhatt RR. The neurobiology of irritable bowel syndrome. Mol Psychiatry. 2023 Apr;28(4):1451-1465. doi: 10.1038/s41380-023-01972-w[↩]
- Drossman DA, Hasler WL. Rome IV-Functional GI Disorders: Disorders of Gut-Brain Interaction. Gastroenterology. 2016 May;150(6):1257-61. https://www.gastrojournal.org/article/S0016-5085(16)30048-8/fulltext[↩]
- Ford A.C., Sperber A.D., Corsetti M., Camilleri M. Irritable Bowel Syndrome. Lancet. 2020;396:1675–1688. doi: 10.1016/S0140-6736(20)31548-8[↩]
- Enck P., Aziz Q., Barbara G., Farmer A.D., Fukudo S., Mayer E.A., Niesler B., Quigley E.M.M., Rajilić-Stojanović M., Schemann M., et al. Irritable Bowel Syndrome. Nat. Rev. Dis. Primers. 2016;2:16014. doi: 10.1038/nrdp.2016.14[↩]
- Osadchiy V., Martin C.R., Mayer E.A. The Gut-Brain Axis and the Microbiome: Mechanisms and Clinical Implications. Clin. Gastroenterol. Hepatol. 2019;17:322–332. doi: 10.1016/j.cgh.2018.10.002[↩]
- Zamani M., Alizadeh-Tabari S., Zamani V. Systematic Review with Meta-Analysis: The Prevalence of Anxiety and Depression in Patients with Irritable Bowel Syndrome. Aliment. Pharmacol. Ther. 2019;50:132–143. doi: 10.1111/apt.15325[↩]
- Erdrich S., Hawrelak J.A., Myers S.P., Harnett J.E. A Systematic Review of the Association between Fibromyalgia and Functional Gastrointestinal Disorders. Ther. Adv. Gastroenterol. 2020;13:175628482097740. doi: 10.1177/1756284820977402[↩]
- Kleykamp B.A., Ferguson M.C., McNicol E., Bixho I., Arnold L.M., Edwards R.R., Fillingim R., Grol-Prokopczyk H., Turk D.C., Dworkin R.H. The Prevalence of Psychiatric and Chronic Pain Comorbidities in Fibromyalgia: An ACTTION Systematic Review. Semin. Arthritis Rheum. 2021;51:166–174. doi: 10.1016/j.semarthrit.2020.10.006[↩]
- Gholamnezhad F., Qeisari A., Shahriarirad R. Gastroesophageal Reflux Disease Incidence among Male Patients with Irritable Bowel Syndrome: A Cross-sectional Study in Southern Iran. JGH Open. 2023;7:152–156. doi: 10.1002/jgh3.12867[↩]
- Ng Q.X., Soh A.Y.S., Loke W., Lim D.Y., Yeo W.-S. The Role of Inflammation in Irritable Bowel Syndrome (IBS) J. Inflamm. Res. 2018;11:345–349. doi: 10.2147/JIR.S174982[↩]
- Lovell R.M., Ford A.C. Global Prevalence of and Risk Factors for Irritable Bowel Syndrome: A Meta-Analysis. Clin. Gastroenterol. Hepatol. 2012;10:712–721.e4. doi: 10.1016/j.cgh.2012.02.029[↩]
- Zia J.K., Lenhart A., Yang P.-L., Heitkemper M.M., Baker J., Keefer L., Saps M., Cuff C., Hungria G., Videlock E.J., et al. Risk Factors for Abdominal Pain-Related Disorders of Gut-Brain Interaction in Adults and Children: A Systematic Review. Gastroenterology. 2022;163:995–1023.e3. doi: 10.1053/j.gastro.2022.06.028[↩]
- Agnello M., Carroll L.N., Imam N., Pino R., Palmer C., Varas I., Greene C., Hitschfeld M., Gupta S., Almonacid D.E., et al. Gut Microbiome Composition and Risk Factors in a Large Cross-Sectional IBS Cohort. BMJ Open Gastroenterol. 2020;7:e000345. doi: 10.1136/bmjgast-2019-000345[↩]
- Patel P, Bercik P, Morgan DG, Bolino C, Pintos-Sanchez MI, Moayyedi P, Ford AC. Prevalence of organic disease at colonoscopy in patients with symptoms compatible with irritable bowel syndrome: cross-sectional survey. Scand J Gastroenterol. 2015 Jul;50(7):816-23. doi: 10.3109/00365521.2015.1007079[↩]
- Dietary Guidelines for Americans. https://www.dietaryguidelines.gov/[↩]
- Magge S, Lembo A. Low-FODMAP Diet for Treatment of Irritable Bowel Syndrome. Gastroenterology & Hepatology. 2012;8(11):739-745. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3966170/[↩][↩]
- Irritable bowel syndrome and diet: where are we in 2018 ? Current Opinion in Clinical Nutrition & Metabolic Care: November 2017 – Volume 20 – Issue 6 – p 456–463. http://journals.lww.com/co-clinicalnutrition/Abstract/2017/11000/Irritable_bowel_syndrome_and_diet___where_are_we.6.aspx[↩]
- Low-FODMAP Diet. American College of Gastroenterology. http://patients.gi.org/topics/low-fodmap-diet/[↩]
- Low FODMAP diet for Irritable Bowel Syndrome. Monash University. https://www.monash.edu/medicine/ccs/gastroenterology/fodmap[↩]
- Evidence-based dietary management of functional gastrointestinal symptoms: The FODMAP approach. Gibson PR, Shepherd SJ. J Gastroenterol Hepatol. 2010 Feb; 25(2):252-8. https://www.ncbi.nlm.nih.gov/pubmed/20136989/[↩]
- Irvin TT. Abdominal pain: a surgical audit of 1190 emergency admissions. Br J Surg. 1989;76(11):1121–1125.[↩]
- Shelton BK. Intestinal obstruction [published correction appears in AACN Clin Issues. 2000;11(1):following table of contents]. AACN Clin Issues. 1999;10(4):478–491.[↩]
- Cullen J J, Kelly K A. Current management of Meckel’s diverticulum. Advances Surg. (1996);9:207–214. https://www.ncbi.nlm.nih.gov/pubmed/8720004[↩][↩]
- Intestinal Pseudo-obstruction. https://www.niddk.nih.gov/health-information/digestive-diseases/intestinal-pseudo-obstruction[↩]
- Wright HK, O’Brien JJ, Tilson MD. Water absorption in experimental closed segment obstruction of the ileum in man. Am J Surg. 1971;121(1):96–99.[↩]
- Wangensteen OH. Understanding the bowel obstruction problem. Am J Surg. 1978;135(2):131–149.[↩]
- Rana SV, Bhardwaj SB. Small intestinal bacterial overgrowth. Scand J Gastroenterol. 2008;43(9):1030–1037.[↩]
- Suri S, Gupta S, Sudhakar PJ, Venkataramu NK, Sood B, Wig JD. Comparative evaluation of plain films, ultrasound and CT in the diagnosis of intestinal obstruction. Acta Radiol. 1999;40(4):422–428.[↩]
- Furukawa A, Yamasaki M, Furuichi K, et al. Helical CT in the diagnosis of small bowel obstruction. Radiographics. 2001;21(2):341–355.[↩]
- Ros PR, Huprich JE. ACR Appropriateness Criteria on suspected small-bowel obstruction. J Am Coll Radiol. 2006;3(11):838–841.[↩]
- Hayanga AJ, Bass-Wilkins K, Bulkley GB. Current management of small-bowel obstruction. Adv Surg. 2005;39:1–33.[↩]
- Choi HK, Chu KW, Law WL. Therapeutic value of gastrografin in adhesive small bowel obstruction after unsuccessful conservative treatment: a prospective randomized trial. Ann Surg. 2002;236(1):1–6.[↩]
- Abbas S, Bissett IP, Parry BR. Oral water soluble contrast for the management of adhesive small bowel obstruction. Cochrane Database Syst Rev. 2007;(3):CD004651[↩]
- Dunn JT, Halls JM, Berne TV. Roentgenographic contrast studies in acute small-bowel obstruction. Arch Surg. 1984;119(11):1305–1308.[↩]
- Lim JH, Ko YT, Lee DH, Lee HW, Lim JW. Determining the site and causes of colonic obstruction with sonography. AJR Am J Roentgenol. 1994;163(5):1113–1117.[↩]
- Matsuoka H, Takahara T, Masaki T, Sugiyama M, Hachiya J, Atomi Y. Preoperative evaluation by magnetic resonance imaging in patients with bowel obstruction. Am J Surg. 2002;183(6):614–617.[↩]
- Wiarda BM, Horsthuis K, Dobben AC, et al. Magnetic resonance imaging of the small bowel with the true FISP sequence: intra- and interobserver agreement of enteroclysis and imaging without contrast material. Clin Imaging. 2009;33(4):267–273.[↩]
- Sagar PM, MacFie J, Sedman P, May J, Mancey-Jones B, Johnstone D. Intestinal obstruction promotes gut translocation of bacteria. Dis Colon Rectum. 1995;38(6):640–644.[↩]
- Williams SB, Greenspon J, Young HA, Orkin BA. Small bowel obstruction: conservative vs. surgical management. Dis Colon Rectum. 2005;48(6):1140–1146.[↩]
- Cox MR, Gunn IF, Eastman MC, Hunt RF, Heinz AW. The safety and duration of non-operative treatment for adhesive small bowel obstruction. Aust N Z J Surg. 1993;63(5):367–371.[↩]
- Fevang BT, Jensen D, Svanes K, Viste A. Early operation or conservative management of patients with small bowel obstruction? Eur J Surg. 2002;168(8–9):475–481.[↩]
- Chen SC, Yen ZS, Lee CC, et al. Nonsurgical management of partial adhesive small-bowel obstruction with oral therapy: a randomized controlled trial. CMAJ. 2005;173(10):1165–1169.[↩]
- Jones MW, Kashyap S, Zabbo CP. Bowel Perforation. [Updated 2023 Apr 24]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2025 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK537224[↩][↩][↩][↩][↩][↩][↩][↩][↩][↩][↩][↩][↩][↩][↩][↩]
- Hafner J, Tuma F, Hoilat GJ, et al. Intestinal Perforation. [Updated 2023 Aug 8]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2025 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK538191[↩][↩][↩][↩][↩][↩][↩][↩][↩][↩]
- Pouli, S., Kozana, A., Papakitsou, I. et al. Gastrointestinal perforation: clinical and MDCT clues for identification of aetiology. Insights Imaging 11, 31 (2020). https://doi.org/10.1186/s13244-019-0823-6[↩]
- Langell JT, Mulvihill SJ. Gastrointestinal perforation and the acute abdomen. Med Clin North Am. 2008 May;92(3):599-625, viii-ix. doi: 10.1016/j.mcna.2007.12.004[↩][↩][↩]
- Del Gaizo AJ, Lall C, Allen BC, Leyendecker JR. From esophagus to rectum: a comprehensive review of alimentary tract perforations at computed tomography. Abdom Imaging. 2014 Aug;39(4):802-23. doi: 10.1007/s00261-014-0110-4[↩][↩]
- Tanner TN, Hall BR, Oran J. Pneumoperitoneum. Surg Clin North Am. 2018 Oct;98(5):915-932. doi: 10.1016/j.suc.2018.06.004[↩][↩][↩]
- Grotelüschen R, Bergmann W, Welte MN, Reeh M, Izbicki JR, Bachmann K. What predicts the outcome in patients with intestinal ischemia? A single center experience. J Visc Surg. 2019 Oct;156(5):405-411. doi: 10.1016/j.jviscsurg.2019.01.007[↩][↩]
- Long B, Robertson J, Koyfman A. Emergency Medicine Evaluation and Management of Small Bowel Obstruction: Evidence-Based Recommendations. J Emerg Med. 2019 Feb;56(2):166-176. doi: 10.1016/j.jemermed.2018.10.024[↩][↩][↩]
- Low ZX, Bonney GK, So JBY, Loh DL, Ng JJ. Laparoscopic versus open appendectomy in pediatric patients with complicated appendicitis: a meta-analysis. Surg Endosc. 2019 Dec;33(12):4066-4077. doi: 10.1007/s00464-019-06709-x[↩][↩]
- Špičák J, Kučera M, Suchánková G. Divertikulární choroba: diagnostika a léčba [Diverticular disease: diagnosis and treatment]. Vnitr Lek. 2018 Summer;64(6):621-634. Czech.[↩][↩][↩][↩]
- Kavitt RT, Lipowska AM, Anyane-Yeboa A, Gralnek IM. Diagnosis and Treatment of Peptic Ulcer Disease. Am J Med. 2019 Apr;132(4):447-456. doi: 10.1016/j.amjmed.2018.12.009[↩][↩][↩][↩]
- Zhang L, Wang H. [Imaging characteristics of gastrointestinal neoplastic acute abdomen]. Zhonghua Wei Chang Wai Ke Za Zhi. 2018 Nov 25;21(11):1223-1229. Chinese.[↩][↩]
- Biffl WL, Leppaniemi A. Management guidelines for penetrating abdominal trauma. World J Surg. 2015 Jun;39(6):1373-80. doi: 10.1007/s00268-014-2793-7[↩][↩][↩]
- Song WC, Lv WW, Gao XZ. Iatrogenic Gastrointestinal Perforation Following Therapeutic Endoscopic Procedures: Management and Outcome. J Coll Physicians Surg Pak. 2017 Sep;27(9):563-565.[↩][↩][↩]
- Garrido Serrano A, Fernández Álvarez P. A foreign body in the small bowel: a rare entity of acute abdomen. Rev Esp Enferm Dig. 2019 Jan;111(1):84. doi: 10.17235/reed.2018.5783/2018[↩][↩]
- Bowel perforation. https://radiopaedia.org/articles/bowel-perforation-1[↩][↩][↩][↩]
- Cho HS, Yoon SE, Park SH, Kim H, Lee YH, Yoon KH. Distinction between upper and lower gastrointestinal perforation: usefulness of the periportal free air sign on computed tomography. Eur J Radiol. 2009 Jan;69(1):108-13. doi: 10.1016/j.ejrad.2007.08.024[↩][↩]
- Paolantonio P, Rengo M, Ferrari R, Laghi A. Multidetector CT in emergency radiology: acute and generalized non-traumatic abdominal pain. Br J Radiol. 2016;89(1061):20150859. doi: 10.1259/bjr.20150859[↩][↩]
- Krüger PC, Mentzel HJ. Radiologische Abklärung des akuten Abdomens im Kindesalter [Radiological evaluation of acute abdomen in children]. Radiologe. 2019 Feb;59(2):146-153. German. doi: 10.1007/s00117-018-0464-7[↩][↩]
- Ruscelli P, Renzi C, Polistena A, Sanguinetti A, Avenia N, Popivanov G, Cirocchi R, Lancia M, Gioia S, Tabola R. Clinical signs of retroperitoneal abscess from colonic perforation: Two case reports and literature review. Medicine (Baltimore). 2018 Nov;97(45):e13176. doi: 10.1097/MD.0000000000013176[↩][↩][↩]
- Zhao N, Li Q, Cui J, Yang Z, Peng T. CT-guided special approaches of drainage for intraabdominal and pelvic abscesses: One single center’s experience and review of literature. Medicine (Baltimore). 2018 Oct;97(42):e12905. doi: 10.1097/MD.0000000000012905[↩][↩]
- Siragusa G, Gelarda E, Epifanio E, Geraci F, Geraci G. La videolaparoscopia nelle urgenze addominali [Video laparoscopy in abdominal emergencies]. Minerva Chir. 1999 Apr;54(4):199-204. Italian.[↩][↩]
- Tengberg LT. Perioperative treatment of patients undergoing acute high-risk abdominal surgery . Dan Med J. 2018 Feb;65(2):B5442. https://ugeskriftet.dk/dmj/perioperative-treatment-patients-undergoing-acute-high-risk-abdominal-surgery[↩][↩]
- Pneumoperitoneum. https://radiopaedia.org/cases/pneumoperitoneum-42[↩]
- Traumatic small bowel perforation. https://radiopaedia.org/cases/traumatic-small-bowel-perforation-1[↩]
- Tumoral large bowel obstruction and perforation. https://radiopaedia.org/cases/tumoral-large-bowel-obstruction-and-perforation[↩]
- Ugwu AU, Kerins N, Malik M. Traumatic small bowel perforation in a case of a perineal hernia. J Surg Case Rep. 2018 Dec 12;2018(12):rjy330. doi: 10.1093/jscr/rjy330[↩]
- Bower KL, Lollar DI, Williams SL, Adkins FC, Luyimbazi DT, Bower CE. Small Bowel Obstruction. Surg Clin North Am. 2018 Oct;98(5):945-971. doi: 10.1016/j.suc.2018.05.007[↩]
- Wada K, Takeuchi N, Emori M, Takada M, Nomura Y, Otsuka A. Two Cases of Pneumatosis Cystoides Intestinalis With Intraperitoneal Free Air. Gastroenterology Res. 2017 Jun;10(3):208-211. doi: 10.14740/gr834w[↩]
- Lim S, Halandras PM, Bechara C, Aulivola B, Crisostomo P. Contemporary Management of Acute Mesenteric Ischemia in the Endovascular Era. Vasc Endovascular Surg. 2019 Jan;53(1):42-50. doi: 10.1177/1538574418805228[↩]
- Pavlović-Calić N. Ulcerozni kolitis i Kronova bolest [Ulcerative colitis and Crohn’s disease]. Med Arh. 2003;57(1 Suppl 2):85-6. Bosnian.[↩]
- Ko BM. [Small Bowel Tumors and Polyposis: How to Approach and Manage?]. Korean J Gastroenterol. 2018 Dec 25;72(6):277-280. Korean. doi: 10.4166/kjg.2018.72.6.277[↩]
- Vanaclocha-Espi M, Ibáñez J, Molina-Barceló A, Valverde-Roig MJ, Pérez E, Nolasco A, de la Vega M, de la Lastra-Bosch ID, Oceja ME, Espinàs JA, Font R, Pérez-Riquelme F, Arana-Arri E, Portillo I, Salas D; CRIBEA Group. Risk factors for severe complications of colonoscopy in screening programs. Prev Med. 2019 Jan;118:304-308. doi: 10.1016/j.ypmed.2018.11.010[↩]
- Fan YC, Peery AF. Therapeutic management of acute uncomplicated diverticulitis. Minerva Gastroenterol Dietol. 2017 Jun;63(2):143-151. doi: 10.23736/S1121-421X.16.02361-8[↩]
- Picone D, Rusignuolo R, Midiri F, Lo Casto A, Vernuccio F, Pinto F, Lo Re G. Imaging Assessment of Gastroduodenal Perforations. Semin Ultrasound CT MR. 2016 Feb;37(1):16-22. doi: 10.1053/j.sult.2015.10.006[↩][↩]
- Saturnino PP, Pinto A, Liguori C, Ponticiello G, Romano L. Role of Multidetector Computed Tomography in the Diagnosis of Colorectal Perforations. Semin Ultrasound CT MR. 2016 Feb;37(1):49-53. doi: 10.1053/j.sult.2015.10.007[↩]
- Bill JG, Smith Z, Brancheck J, Elsner J, Hobbs P, Lang GD, Early DS, Das K, Hollander T, Doyle MBM, Fields RC, Hawkins WG, Strasberg SM, Hammill C, Chapman WC, Edmundowicz S, Mullady DK, Kushnir VM. The importance of early recognition in management of ERCP-related perforations. Surg Endosc. 2018 Dec;32(12):4841-4849. doi: 10.1007/s00464-018-6235-8[↩]
- Wang H, Li A, Shi X, Xu X, Wang H, Wang H, Yu E. [Diagnosis and treatment of iatrogenic colonoscopic perforation]. Zhonghua Wei Chang Wai Ke Za Zhi. 2018 Jun 25;21(6):660-665. Chinese.[↩]
- Titos-García A, Aranda-Narváez JM, Romacho-López L, González-Sánchez AJ, Cabrera-Serna I, Santoyo-Santoyo J. Nonoperative management of perforated acute diverticulitis with extraluminal air: results and risk factors of failure. Int J Colorectal Dis. 2017 Oct;32(10):1503-1507. doi: 10.1007/s00384-017-2852-2[↩]
- Nimmagadda N, Matsushima K, Piccinini A, Park C, Strumwasser A, Lam L, Inaba K, Demetriades D. Complicated appendicitis: Immediate operation or trial of nonoperative management? Am J Surg. 2019 Apr;217(4):713-717. doi: 10.1016/j.amjsurg.2018.12.061[↩]
- Ho VP, Schiltz NK, Reimer AP, Madigan EA, Koroukian SM. High-Risk Comorbidity Combinations in Older Patients Undergoing Emergency General Surgery. J Am Geriatr Soc. 2019 Mar;67(3):503-510. doi: 10.1111/jgs.15682[↩][↩]
- Massarweh NN, Legner VJ, Symons RG, McCormick WC, Flum DR. Impact of advancing age on abdominal surgical outcomes. Arch Surg. 2009 Dec;144(12):1108-14. doi: 10.1001/archsurg.2009.204[↩]
- Shah AA, Haider AH, Zogg CK, Schwartz DA, Haut ER, Zafar SN, Schneider EB, Velopulos CG, Shafi S, Zafar H, Efron DT. National estimates of predictors of outcomes for emergency general surgery. J Trauma Acute Care Surg. 2015 Mar;78(3):482-90; discussion 490-1. doi: 10.1097/TA.0000000000000555[↩]
- Healthcare Cost and Utilization Project (HCUP) Statistical Briefs [Internet]. Rockville (MD): Agency for Healthcare Research and Quality (US); 2006 Feb-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK52651[↩]
- Southern DA, Quan H, Ghali WA. Comparison of the Elixhauser and Charlson/Deyo methods of comorbidity measurement in administrative data. Med Care. 2004 Apr;42(4):355-60. doi: 10.1097/01.mlr.0000118861.56848.ee[↩]
- Elixhauser A, Steiner C, Harris DR, Coffey RM. Comorbidity measures for use with administrative data. Med Care. 1998 Jan;36(1):8-27. doi: 10.1097/00005650-199801000-00004[↩]
- Cooper Z, Lilley EJ, Bollens-Lund E, Mitchell SL, Ritchie CS, Lipstiz SR, Kelley AS. High Burden of Palliative Care Needs of Older Adults During Emergency Major Abdominal Surgery. J Am Geriatr Soc. 2018 Nov;66(11):2072-2078. doi: 10.1111/jgs.15516[↩]
- Key Statistics for Colorectal Cancer. https://www.cancer.org/cancer/types/colon-rectal-cancer/about/key-statistics.html[↩]
- Cancer Stat Facts: Colorectal Cancer. https://seer.cancer.gov/statfacts/html/colorect.html[↩][↩]
- SEER Cancer Statistics Review (CSR) 1975-2017. https://seer.cancer.gov/archive/csr/1975_2017[↩]
- Imperiale TF, Wagner DR, Lin CY, Larkin GN, Rogge JD, Ransohoff DF. Results of screening colonoscopy among persons 40 to 49 years of age. N Engl J Med. 2002 Jun 6;346(23):1781-5. doi: 10.1056/NEJM200206063462304[↩]
- American Cancer Society Guideline for Colorectal Cancer Screening. https://www.cancer.org/cancer/colon-rectal-cancer/detection-diagnosis-staging/acs-recommendations.html[↩][↩]
- Colorectal Cancer Screening Tests. https://www.cancer.org/cancer/types/colon-rectal-cancer/detection-diagnosis-staging/screening-tests-used.html[↩]
- NCCN. Colorectal cancer screening guidelines. https://www.nccn.org/professionals/physician_gls/pdf/colorectal_screening.pdf[↩]
- Shaukat A, Kahi CJ, Burke CA, Rabeneck L, Sauer BG, Rex DK. ACG Clinical Guidelines: Colorectal Cancer Screening 2021. Am J Gastroenterol. 2021 Mar 1;116(3):458-479. doi: 10.14309/ajg.0000000000001122[↩]
- US Preventive Services Task Force. Screening for Colorectal Cancer: US Preventive Services Task Force Recommendation Statement. JAMA. 2021;325(19):1965–1977. doi:10.1001/jama.2021.6238[↩]
- Qaseem, A., Crandall, C. J., Mustafa, R. A., Hicks, L. A., Wilt, T. J., Clinical Guidelines Committee of the American College of Physicians, Forciea, M. A., Fitterman, N., Horwitch, C. A., Kansagara, D., Maroto, M., McLean, R. M., Roa, J., & Tufte, J. (2019). Screening for Colorectal Cancer in Asymptomatic Average-Risk Adults: A Guidance Statement From the American College of Physicians. Annals of internal medicine, 171(9), 643–654. https://doi.org/10.7326/M19-0642[↩]
- Wolf, A.M., et al. Colorectal cancer screening for average-risk adults: 2018 guideline update from the American Cancer Society. CA: A Cancer Journal for Clinicians, 68: 250-281. https://doi.org/10.3322/caac.21457[↩]
- Updates on age to start and stop colorectal cancer screening: recommendations from the U.S. Multi-Society Task Force on Colorectal Cancer. Patel, Swati G. et al. Gastrointestinal Endoscopy, Volume 95, Issue 1, 1-15, November 15, 2021. https://doi.org/10.1016/j.gie.2021.06.012[↩]
- Survival Rates for Colorectal Cancer. https://www.cancer.org/cancer/colon-rectal-cancer/detection-diagnosis-staging/survival-rates.html[↩]